Rebekah Vukovich CASE STUDY Dietetic Intern OUTLINE Introduction

Rebekah Vukovich CASE STUDY Dietetic Intern

OUTLINE Introduction to patient Past medical history Primary diseases/conditions Short bowel syndrome Patient’s current hospital admissions Nutrition Care Process

INTRODUCTION Female Age: 63 Weight: § First admission: 44 kg § Second admission: 49 kg § 28% wt. loss in past 10 months Height: 152. 4 cm BMI: 18. 9 (first admission) Social history: Married, retired, previously residing in extended care facility, home health care Primary problem: Multiple abdominal surgeries with complications, malnutrition, long-term TPN

PAST MEDICAL HISTORY Partial gastrectomy RNY gastrojejunostomy Colostomy G-tube GI bleed GERD Ulcers HTN Tracheostomy (December) MI COPD Depression CAD TIA Cardiac stents Rheumatoid arthritis

PREVIOUS HOSPITAL ADMISSIONS 3/2011 § Cardiac arrest, myocardial infarction 6/2012 § Perforated duodenal ulcer, peritonitis, graham patch over ulcer 7/2012 § Small bowel obstruction 3/2014 § Hematemesis, hiatal hernia, chronic gastritis, gastric ulcer 5/2014 § GI bleed, hiatal hernia, gastric ulcer 7/2014 § Upper GI bleed, peptic ulcer, anemia, partial gastrectomy, RNY gastrojejunostomy, G-tube placed 10/2014 § Chronic antral ulcer, gangrene, colectomy, ileostomy 12/2014 § Hyperkalemia, dehydration, AKI

PEPTIC ULCER Open sores or lesions, disrupt mucosal integrity § Gastric ulcer § Esophageal ulcer § Duodenal ulcer Causes: § Stomach acid § Helicobacter pylori infection § Long-term NSAIDs use Symptoms: § § Burning stomach pain Starts between meals or during the night May come and go, duration varies Less common: N/V, belching, poor appetite, weight loss

PEPTIC ULCERS Complications § Bleeding § Perforation § Obstruction Treatment § Worsen if not treated § Acid-suppressing medication § Antibiotics § Surgery Nutrition Therapy § Alcohol § Coffee and caffeine § Spices § Probiotics § Omega 3, 6

GASTRECTOMY WITH RNY GASTROJEJUNOSTOMY Billroth II Due to recurrent GI bleeds Chronic antral ulcer Procedure Nutritional complications § Obstruction, dumping, abdominal discomfort, diarrhea, weight loss, impaired digestion and absorption Micronutrient deficiencies: iron, calcium, Vit. D, riboflavin, folate, Vit. B 12 Diet § § § Avoid: concentrated sweets Lactose Small, frequent meals Lying down after meals Emphasize protein and fat Fiber

ILEOSTOMY Anatomy Diet recommendations: § § High-calorie high-protein Low residue Foods that cause gas and odor Malabsorption § Bile acid § Fat § Vitamin B 12 Increased loss § Fluid § Sodium § Potassium

SHORT BOWEL SYNDROME >40 -50% small intestine removed Particularly ileum and ileocecal valve Loss of small bowel absorptive area Complications § Diarrhea, dehydration, steatorrhea, weight loss, muscle wasting, bone disease Malabsorption with loss of absorptive area Prognosis: § § Adaption of remaining bowel Length of residual bowel Ileocecal valve Small and large bowel continuity

SHORT BOWEL SYNDROME Post-op feedings § If >1/2 removed, start TPN § Elemental formula § MCT triglycerides § 6 -10 small meals/day Supplements/Medications Initially, control hydroelectrolitic disturbances/rehydrate PN started early PN essential for long-term survival

DIET AND SHORT BOWEL SYNDROME Long-term TPN Complications § Systemic recurrent infections (vein catheter contamination), thrombosis of two or more central veins, and hepatic malfunction Satisfactory results with the use of EN § To reduce/eliminate PN Antimotility agents Oral diet: iso-osmolar, hypercaloric, fractionated form, addition of soluble fibers § Restriction of lipids, lactose, and calcium oxalate. § Oral rehydration § Vitamin/mineral supplement

RESEARCH STUDY Long-term retrospective clinical study 10 patients with severe SBS after intestinal surgery resection No chronic conditions Examined every 12 months Measured: body weight, height, BMI, basal energy expenditure, percentage of involuntary loss of usual body weight (%UWL), fat-free mass, fat mass, total protein, albumin, total lymphocyte count Calculated home parenteral nutrition (HPN) and home enteral nutrition (HEN) provided

RESULTS Significant and progressive increase in %UWL 20% of body weight loss by the end FFM and FM significant decrease Serum albumin, total protein, and total lymphocyte count did NOT change significantly HPN withdrawn in 8 patients (permanently in 5, and temporarily in 3) Most frequent complications: infection from central venous catheter (at least 1 x in each patient, 30 total instances) Bone disease in 7 pt. , deep vein thrombosis in 3 pt. , chronic calculous cholelithiasis in 5 pt. § Bone disease: use of cyclic HPN, may contribute to urinary calcium loss All patients survived for 2 years, seven for 5 yrs. , and six for 7 years of more

RESULTS References a study of 124 patients with SBS, survival of 94% at 1 year, 86% at 2 years, and 75% at 5 years § Death rate: 22% r/t HPN Duration of PN correlates significantly with length of RSB (length of the residual small bowel after the Treitz angle) Long-term Enteral Nutrition + Oral Intake achieved the minimal energy requirement at only 2 periods of the study Inability to use EN exclusively in severe SBS Patients who reduced PN, survived for longer periods Use of HEN + OI reduced complications of prolonged PN

NUTRITION RECOMMENDATIONS FROM STUDY Slow and progressive introduction of oral diet Control electrolytes No benefit to restricting lipids and oxalate if there is no colon Intestinal absorption up to 50% in SBS Hypercaloric: 1. 5 -2. 0 of BEE § Factors impairing intake: bacterial overgrowth, nausea, flatulence, poor appetite, fear of eating outside the home Consider intermittent use of PN throughout the year.
ADMISSION 1 MEDICATIONS IV fluids TPN M/V Lasix Novolog Lipitor Fiber. Con Lomotil Imodium Protonix Zofran Codeine Sulfate
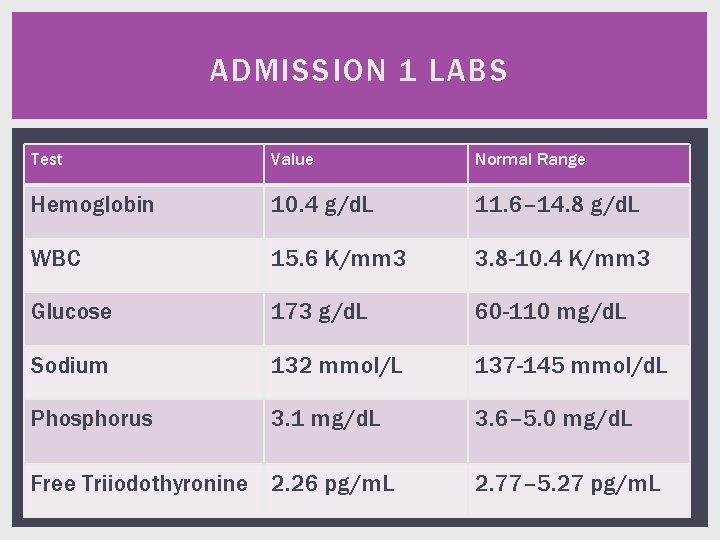
ADMISSION 1 LABS Test Value Normal Range Hemoglobin 10. 4 g/d. L 11. 6– 14. 8 g/d. L WBC 15. 6 K/mm 3 3. 8 -10. 4 K/mm 3 Glucose 173 g/d. L 60 -110 mg/d. L Sodium 132 mmol/L 137 -145 mmol/d. L Phosphorus 3. 1 mg/d. L 3. 6– 5. 0 mg/d. L Free Triiodothyronine 2. 26 pg/m. L 2. 77– 5. 27 pg/m. L

PRESENT MEDICAL STATUS AND TREATMENT ADMISSION 1 Severe sepsis due to abdominal abscess, complicated by septic shock § r/t recent removal of duodenostomy tube Advanced COPD Right lower quadrant fluid collection Acute abdominal pain r/t mesenteric edema Peritonitis Leukocytosis Hypertension Treatment: § § Guided drainage IV fluids IV antibiotics Oxygen

ADMISSION 1 NUTRITION ASSESSMENT Surgeon recommends complete bowel shut down and rest with minimum 2 weeks of TPN for malnutrition and duodenal leak. Diet History: soft diet at nursing home Weight History: Admission 44 kg (22% in <3 months; severe) § 12/2/14 41. 8 kg § 10/23/14 56. 5 kg § 3/8/14 61. 3 kg Nutrition-Focused Physical Assessment: § § § § Orbital Triceps Temporal Clavicle Shoulders Interosseous Hand-grip strength

ADMISSION 1 NUTRITION ASSESSMENT Diet order: Clear Liquids, NPO, TPN Nutrition Needs: § Calories: BMR = 917; stress factor 1. 4 (sepsis) = 1375 § Protein: 1. 2 -2. 0 g/kg (sepsis, catabolic) = 52 -88 § Fluid: 30 ml/kg = 1200 ml/d TPN: Clinimix 5/15 § 2 L w/ 500 ml 20% lipids providing 1920 kcal and 100 gm protein § 1320 m. L w/ 250 ml 20% fat emulsion, providing 1437 kcal (104%) and 66 g protein (75 -127%) Nutrition Diagnosis: Malnutrition r/t chronic illness of sepsis and altered GI function as evidenced by 22% wt. loss past 3 months, poor grip strength, subcutaneous fat loss, muscle atrophy and poor po intake for 3 days which meets the parameters for severe protein-calorie malnutrition (PCM).

PRESENT MEDICAL STATUS AND TREATMENT ADMISSION 2 Weakness Hyponatremia Acute respiratory failure Leukocytosis UTI Sepsis § Polymicrobial septicemia § Fungal septicemia Short bowel syndrome Treatment § Normal saline § Antibiotic § 2 units packed red blood cells

ADMISSION 2 NUTRITION ASSESSMENT Fatigue and weakness past 2 weeks Trigger: poor po >5 days and 10# wt. loss in past 6 months Weight: admission 49 kg, Discharge 62. 2 kg I>O Diet history: since previous discharge § Regular diet: 2 -3 meals/day § Steak, potatoes, chicken, fish, mac & cheese, hamburger, yogurt, oatmeal, pudding. No cottage cheese. Denies GI discomfort. § Eating less past 2 weeks § Stated she was drinking adequate fluids (ginger-ale, Pedialyte, Powerade, popsicles) § TPN: 1320 ml with 250 ml 20% lipids

NUTRITION ASSESSMENT Nutritional Needs: § Calories: RMR = 971, stress factor 1. 3 (infection, hx COPD) = 1262 § Protein: 1 -1. 3 g/kg (potential malabsorption, infection, chronic illness) = 49 -74 g § Fluid: 30 ml/kg = 1470 ml Current diet: Purred diet, Clear Liquids, Full Liquids TPN: Clinimix 5/15 1320 ml w/ 250 ml 20% lipids, which provides: 1437 kcal (114% of estimated needs) and 66 g protein (90 -135% of estimated needs).

ADMISSION 2 NUTRITION CARE PROCESS Diagnosis § Inadequate oral intake r/t poor appetite and fatigue as evidenced by reported poor po intake >5 days. Intervention § Meals and Snacks: Encourage small, frequent meals. Decrease amount of fluid consumption with meals, have fluids between meals. § Nutrition Support: Continue TPN § Supplement: Place order for Ensure TID. Monitoring and Evaluation § Meals and Snacks: Monitor for intake and tolerance. § Nutrition Support: Monitor for tolerance and order change. § Supplement: Monitor for consumption and need for lower-sugar formula § Anthropometrics: Maintain wt. +/-. 5 to 1 kg of admission wt. § Biochemical: Monitor Hgb, Hct, sodium, BUN, glucose, and iron.

DISCHARGE Two weeks of therapy for bacteremia and fungemia. Long-term TPN Home health care

THANK-YOU! Questions?
- Slides: 27