RASHTRIYA SWASTHYA BIMA YOJANA STRUCTURE OF THE PRESENTATION

RASHTRIYA SWASTHYA BIMA YOJANA

STRUCTURE OF THE PRESENTATION n n n Why Health Insurance? What is the Scheme? How is it different from the other schemes? What has happened so far? How has the scheme been perceived? What are the challenges for the future? 2
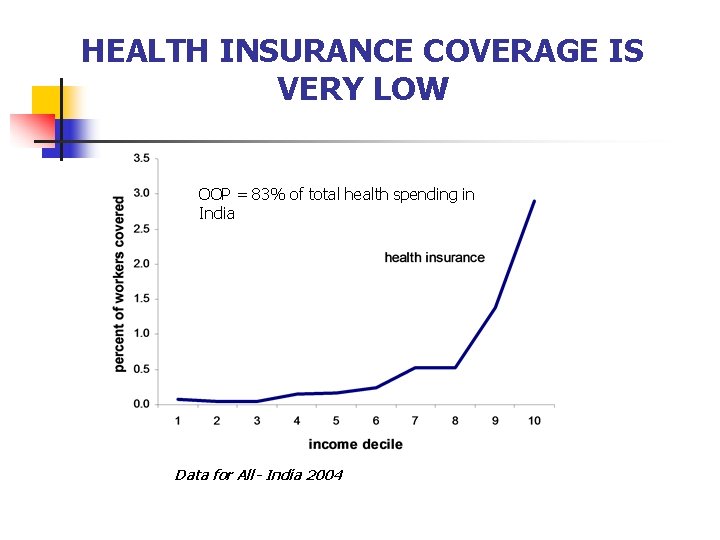
HEALTH INSURANCE COVERAGE IS VERY LOW OOP = 83% of total health spending in India Data for All- India 2004
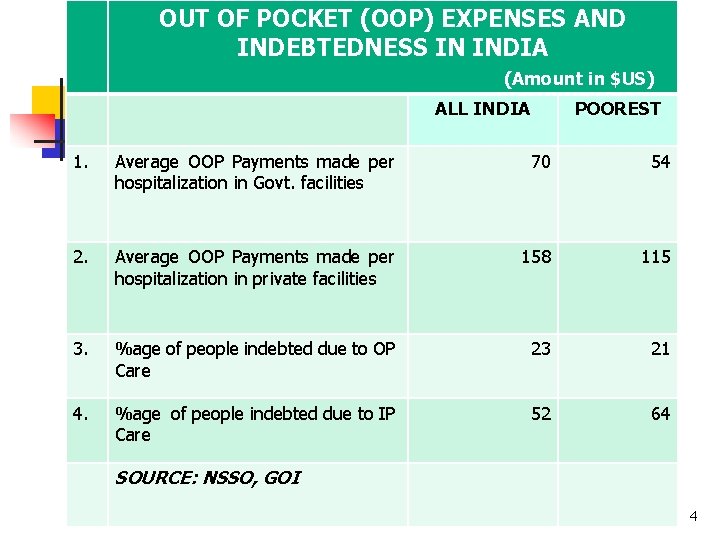
OUT OF POCKET (OOP) EXPENSES AND INDEBTEDNESS IN INDIA (Amount in $US) ALL INDIA POOREST 1. Average OOP Payments made per hospitalization in Govt. facilities 70 54 2. Average OOP Payments made per hospitalization in private facilities 158 115 3. %age of people indebted due to OP Care 23 21 4. %age of people indebted due to IP Care 52 64 SOURCE: NSSO, GOI 4

CHARACTERISTICS OF UNORGANIZED SECTOR WORKERS n n n Poor Self-Employed Illiterate Migratory Unskilled 5

RASHTRIYA SWASTHYA BIMA YOJANA The Scheme n n n Total sum Insured of Rs 30, 000 per BPL family (a unit of five) on a family floater basis Pre-existing diseases to be covered Coverage of health services related to hospitalization and certain procedures which can be provided on a day-care basis 6

RASHTRIYA SWASTHYA BIMA YOJANA Benefits n n Cashless coverage for hospitalization with few exceptions. Provision of Smart Card. Provision of pre and post hospitalization expenses. Transport allowance @ Rs. 100 per visit up to a ceiling of Rs. 1000 as part of the benefits. 7

FUNDING n n n Contribution by GOI : 75% of the estimated annual premium. Contribution by the State Governments: 25% of the annual premium. Additional benefits can be provided by the State Government but the cost has to be borne by the State. Beneficiary to pay Rs. 30 per annum as Registration Fee. Administrative cost to be borne by the State Government. Cost of Smart Card to be borne by the Central Government @ Rs. 60 per beneficiary 8
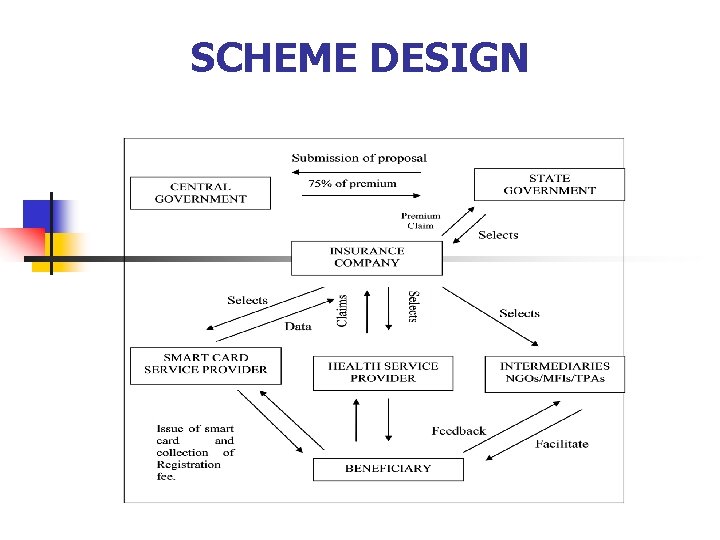
SCHEME DESIGN

HOW HAS RSBY EVOLVED AS A DIFFERENT SCHEME? n n n n IT used to reach the poor on a large scale. The BPL families are being empowered with a choice. They can choose from among several hospitals (both public and private) for treatment. A ‘business’ model for a social sector scheme. (Fortune at the bottom of the pyramid) Key Management System (KMS) to make the scheme foolproof. Simple front end but extremely complex back end. Paperless, cashless and ageless. IT and KMS has allowed to prevent leakages. Validity of the smart card throughout the country. 10

SMART CARD 11
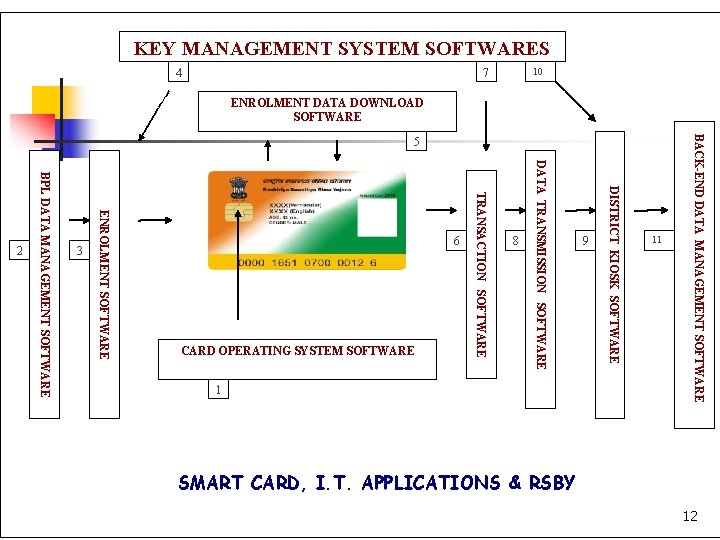
KEY MANAGEMENT SYSTEM SOFTWARES 5 BACK-END DATA MANAGEMENT SOFTWARE DISTRICT KIOSK SOFTWARE DATA TRANSMISSION SOFTWARE TRANSACTION SOFTWARE ENROLMENT SOFTWARE CARD OPERATING SYSTEM SOFTWARE BPL DATA MANAGEMENT SOFTWARE 1 11 9 8 6 3 2 10 7 4 ENROLMENT DATA DOWNLOAD SOFTWARE SMART CARD, I. T. APPLICATIONS & RSBY 12

WHAT WAS REQUIRED TO BE DONE DURING THE INITIAL PHASE? n n n Insurance related Tasks. Information Technology related Tasks. Marketing of the Scheme. 13

TASKS DURING THE INITIAL PHASE Insurance and Medical Services Related Activities n n n Issue of Guidelines. Preparing Tender Document template to be issued by the State Governments. Preparing Contract Document template between States and Insurance Companies. Standardizing Surgical Procedures and the Costs thereof. (States can revise the package rates) Preparing MOU template between Centre and the States. Guidelines for evaluating the process and the outputs. 14

TASKS DURING THE INITIAL PHASE Information Technology Related Issues n n n n Standardization of Smart Card specifications. Standardization of Smart Card Handling Devices specifications. Preparation of Enrolment software for issue of Smart Cards. Standardization of software specifications for transacting business with smart cards. Evolving IT package for settlement of claims. Evolving MIS for monitoring and evaluation. Evolving Key Management System (KMS) with a view to providing security. Putting in place a Software Certification System. 15

TASKS DURING THE INITIAL PHASE Marketing of the Scheme n Within the Central Government n State Governments n Insurance Companies n Health Service Providers n Smart Card Service Providers n Intermediaries 16

WHAT HAS HAPPENED SO FAR? …. since its roll out from 1. 4. 08 n n Twenty Five States have advertised. Approval has been given to 21 States and 18 of these have started issuing smart cards. Around 5. 5 million smart cards, covering around 20 million persons, have already been issued. Around 70, 000 persons have availed health care benefits in hospitals. 17
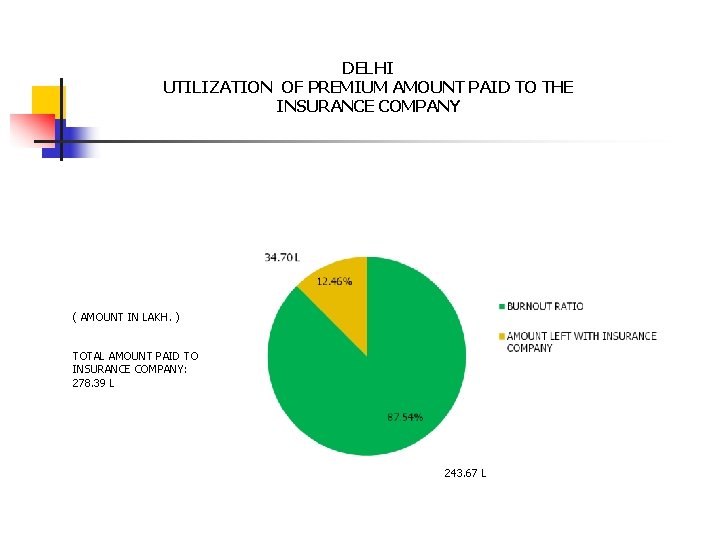
DELHI UTILIZATION OF PREMIUM AMOUNT PAID TO THE INSURANCE COMPANY ( AMOUNT IN LAKH. ) TOTAL AMOUNT PAID TO INSURANCE COMPANY: 278. 39 L 243. 67 L
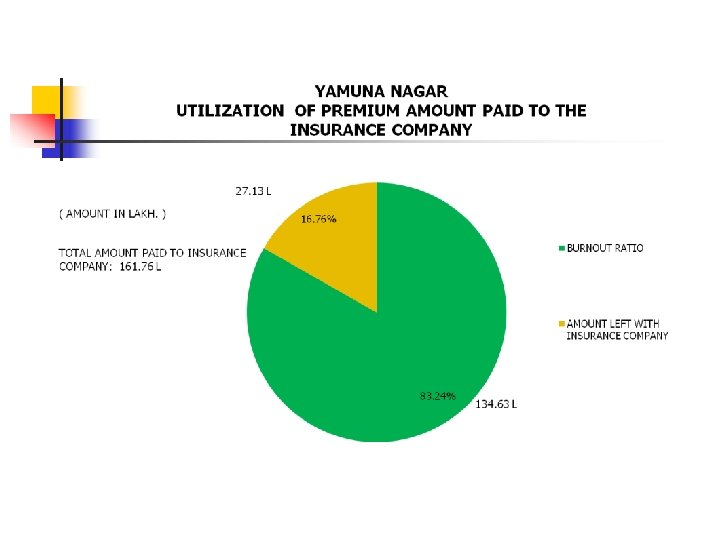
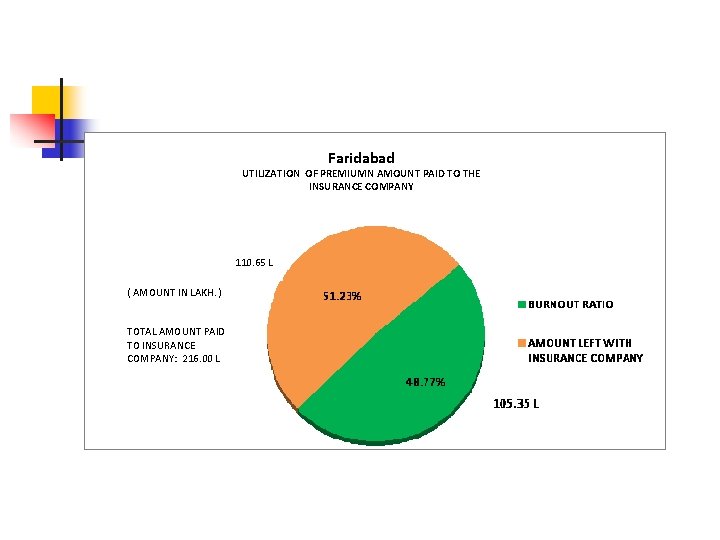
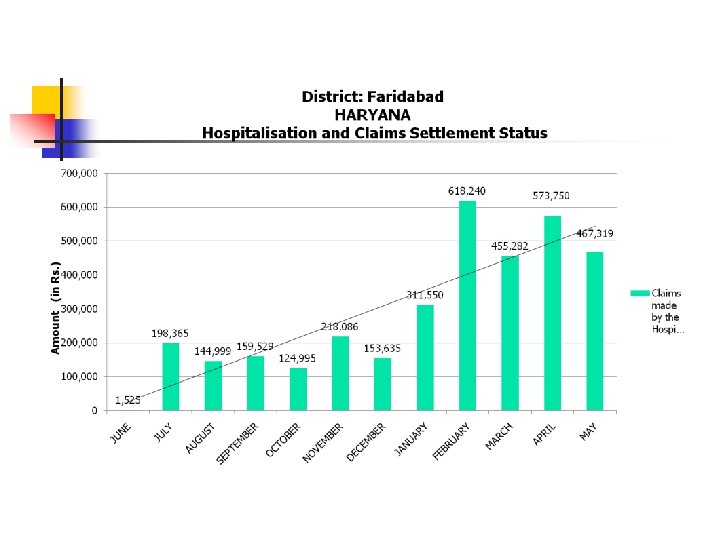
Faridabad UTILIZATION OF PREMIUMN AMOUNT PAID TO THE INSURANCE COMPANY 110. 65 L ( AMOUNT IN LAKH. ) TOTAL AMOUNT PAID TO INSURANCE COMPANY: 216. 00 L
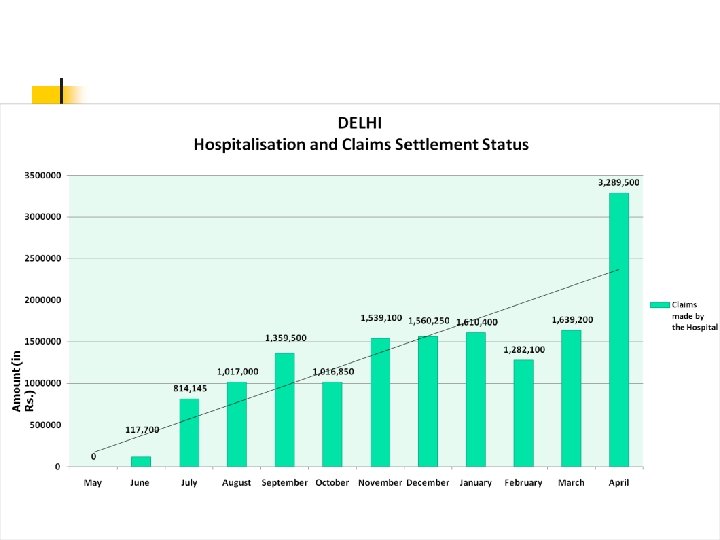

RSBY …………other incidental benefits. n n n Investment in health infrastructure by the private sector and inducing quality improvement in existing infrastructure Disease profiling in each District. Enabling zero-leakage and providing a platform for schemes like PDS. Creating opportunities for future penetration. Improving the BPL data-base 23

RSBY ……………. . as perceived by the media 24

“For the nation, it is the best Diwali present amidst all the gloom in the marketplace”






MAJOR PROBLEMS FACED IN THE INITIAL IMPLEMENTATION OF THE SCHEME n n n n Data relating to Below Poverty Line (BPL) families. Initial reluctance of the Sates to participate on account of the complexities of the scheme. Intricate Information Technology (IT) applications. Non-availability of requisite hardware at such a large scale. Ineffective communication strategy for this type of target segment. Poor conversion ratio in some of the States, like Delhi Poor burn-out ratio in some districts, like Faridabad (Haryana) 31

The Challenges Ahead n n n n n Sustaining the momentum and improving upon the numbers. Inducing increased commitment levels in some States. Getting medical departments of some of the States to see value in the scheme. Finding a lasting solution to the problems relating to BPL data. Evolving a robust back-end data base management. Ensuring quality. Convergence with the UId Project. Capacity building at each level, specially the State Nodal Agency and the hospitals. Evolving an institutional framework. 32

. . . the journey so far has been tough but enjoyable. However, there is still a long way to go.
- Slides: 33