RAPID RESPONSE BPAS MEWS AND SIRS MAKING SENSE

RAPID RESPONSE, BPA’S, MEWS AND SIRS MAKING SENSE OF EARLY IDENTIFICATION OF THE DETERIORATING PATIENT WILLIAM SHEPPARD MD Covenant Healthcare Section of Hospital Medicine

DISCLOSURES NO CONFLICTS NO INDUSTRY SUPPORT NO SPECIAL CERTIFICATION

GOALS REVIEW THE HISTORY OF RAPID RESPONSE IN THE PATIENT WITH CHANGING VITALS USING SEPSIS CARE MODEL IMPROVE UNDERSTANDING OF BPA FIRING’S AND MEWS SCORE IMPROVE COORDINATION BETWEEN NURSING EVALUATION AND PHYSICIAN CARE

EVALUATION OF STUDIES CAN THEY SAY WHAT THEY SAY IS IT CLINICALLY USEFUL DOES IT APPLY TO MY PATIENT POPULATION CAN I REPLICATE THE STUDY DESIGN IN MY PRACTICE SETTING

HISTORY

INSTITUTE OF MEDICINE 1999 TO ERR IS HUMAN 2001 CROSSING THE QUALITY CHASM LATER 2001 AGENCY FOR HEALTHCARE RESEARCH AND QUALITY FORMED/FUNDED BY CONGRESS 2005 10, 000 LIVES CAMPAIGN ON INSTITUTE FOR HEALTHCARE IMPROVEMENT

THE PROBLEM PREVENTABLE ADVERESE OUTCOMES-17% OF INPATIENTS WITH 70% PREVENTABLE DETERIORATION NOT RECOGNIZED HIGH PATIENT TO NURSE RATIOS BACK UP OFTEN JUNIOR PHYSICIANS IN TRAINING EXPERIANCED CLINICIANS IN SEPERATE HOSPITAL “SILOS”

SOLUTIONS OUT REACH OF CLINICAL EXPERTS APPLICATION OF TECHNOLOGY

SPECIFIC SOLUTIONS EVOLUTION OF EARLY INTERVENTION IN DETERIORATING PATIENTS RAPID RESPONSE MEWS ELECTRONIC BOARDS / COLOR CODES CONTINUE TO DEVELOP

RAPID RESPONSE AND CLINICAL OUTREACH

RAPID RESPONSE FIRST MEDICAL EMERGENCY TEAM - SYDNEY AUSTRALIA 1989 AT LIVERPOOL HOSPITAL INSTITUE OF HEALTHCARE IMPROVEMENT STARTING 2005 GOAL TO REDUCE CARDIAC AND RESPIRATORY ARREST ON GMF’S PATTERNED ON PALS CONTINUE TO EVOLVE (TRIGGERS AND COMPOSITION)

RAPID RESPONSE VARIES BY INSTITUTION TEAM RESPONSE TRIGGERED BY …. RESEARCH INDICATED 80% OF CARDIAC ARREST PRECEDED BY ABNORMAL VITAL SIGNS FOR 8 HOURS MORE EXPERIANCED CLINICIAN EVALUATION-NURSE, ADVANCED PRACTICE NURSE OR PHYSICIAN ADVANCED INTERVENTION PRIOR TO TRANSFER TO ICU SETTING

RAPID RESPONSE MODELS MODEL MEDICAL EMERGENCY CRITICAL CARE OUTREACH RAPID RESPONSE PERSONAL DUTIES PHYSICIAN, RESPOND TO CRITICAL CARE EMERGENCIES NURSE CRITICAL CARE FOLLOW PATIENTS PHYSICIANS AND DISCHARGED NURSES FROM ICU PROACTIVE PHYSICIAN, EVALUATION OF CRITICAL CARE HIGH RISK PATIENT NURSE AND RT

RAPID RESPONSE TEAM Medical Rapid Response System Calling Criteria Any staff member may call the team if one of the following criteria is met: Heart rate over 140/min or less than 40/min Respiratory rate over 28/min or less than 8/min Systolic blood pressure greater than 180 mm. Hg or less than 90 mm. Hg Oxygen saturation less than 90% despite supplementation Acute change in mental status Urine output less than 50 cc over 4 hours Staff member has significant concern about the patient's condition Additional criteria used at some institutions: Chest pain unrelieved by nitroglycerin Threatened airway Seizure

DATA MULTIPLE STUDIES 2003 -4 SINGLE SITES REDUCTION IN ICU READMISSION AND IN HOSPITAL MORTALITY MOST LOOKED AT OUT REACH TEAMS FOLLOWING ICU GRADUATES

MERIT STUDY 23 HOSPITALS IN AUSTRALIA CLUSTER RANDOMIZED TRIAL MEDICAL EMERGENCY RESPONSE TEAM VS USUAL CARE FAILED TO DEMONSTRATE BENIFIT FELT TO BE UNDER POWERED TOO MANY VARIABLES TO CONTROL FOR

PATIENT AT RISK TEAM OUT REACH THAT SUPPLEMENTS USUAL CARE

RAPID RESPONSE MODEST IMPROVEMENT CARDIAC ARREST MORTALITY NO REDUCTION IN UNPLANNED ICU ADMISSIONS MUCH OF RESEARCH NOW FOCUSED ON ICU GRADUATE FOLLOW UP

EXPANDED RESPONIBILTIES REPLACE IV TEAM STAFFING SUPPORT EXPAND TO CRITICAL CARE OUT REACH

MEWS

MEWS- MODIFIED EARLY WARNING SCORE 0 TO 3 RATING SCALE, EVALUATING DEVIATION FROM NORMAL, BOTH HIGH AND LOW EVALUATES HEART RATE, RESPIRATORY RATE, SYSTOLIC BP, TEMPERATURE, URINE OUTPUT, LEVEL OF CONCIOUSNESS

MEWS SEEK TO STANDARDIZE INDICATION TO CALL RAPID RESPONSE REMOVE BARRIERS “WHY DID YOU CALL”


MEWS VALIDATION UK STAGED RESPONSE INCREASED FREQUENCY OF MONITOR FOLLOWED BY ADVANCED PRACTICE PROVIDER EVALUATION VALIDATED IN STUDIES ON UK SURGICAL WARDS : > 4 RESIDENT SURGEON EVALUATED REDUCED TRANSFER TO ICU

WHATS NEW AND NEXT FAMILY AND PATIENT INITIATED RAPID RESPONSE- SOCIETY OF CRITICAL CARE MEDICINE 2011

BPA’S

BPA’s AT COVENANT BEST PRACTICE ALERT TRIGGERED BY DATA INPUT CLINICAL DECISION ALGORITHM OR NOTIFICATION IN EPIC THE ALGORITHM CAN FUNCTION AS A EWS

BEST PRACTICE EVIDENCE BASED PROTOCOL DRIVEN CMS CORE MEASURES

EXAMPLE SEPSIS


WHY SEPSIS

sepsis leading cause of non cardiac death 8% annual incidence 650, 000 -750, 000 case per year in US increased incidence in age> 65 and non white population

SEPSIS EXPENSIVE A LEADING CAUSE OF INPATIENT MORTALITY NEW RESEARCH SUGGEST WE CAN IMPROVE CARE AND REDUCE MORTALITY CMS QUALITY MEASURE (2016)

SYSTEMIC INFLAMMATORY RESPONSE SYNDROME CONCEPT AND NAME ADOPTED IN 1992 GOAL TO STANDARDIZE DIAGNOSIS FOR PUPOSE OF RESEARCH CLINICAL SIGNS AND SYMPTOMS DRIVEN BY THE COMMON PATHOPHYSIOLOGY OF MICROVASCULAR DIC INFLAMMATORY RESPONSE TRIGGERS COAGULATION CASCADE
SIRS AND SEPSIS SUPECTED INFECTION CLINICAL FINDINGS SUGGESTIVE OF SIRS + INFECITON = SEPSIS + ORGAN DYSFUNCTION = SEVERE SEPSIS + HYPOTENSION AFTER 30 CC/KG FLUID BOLUS = SEPTIC SHOCK

SIRS CRITERIA TEMPERATURE >100. 9 OR < 96. 8 HEART RATE >90 RESPIRATORY RATE >20 OR PCO 2 < 32 mm. Hg WBC’s >12000 OR <4000 OR BANDS > 10%

WHY REDUCE MORTALITY AND MORBIDITY RESEARCH THAT DEFINED “EARLY GOAL DIRECTED THERAPY"

SURVIVING SEPSIS BEGAN 2002 FIRST GUIDELINES 2004 GUIDELINES REVISED 2008 AND 2012 NOW 30 SPONSORING ORGANIZATIONS


EARLY GOAL DIRECTED THERAPY MICHIGAN BORN AND BRED - DMC Rivers 2001 SIGNIFICANT MORTALITY REDUCTIONS EARLY IDENTIFICATION OF AT RISK PATIENT (LACTATE >2. 5 -4) SOMEWHAT STANDARDIZED DEFINITION OF SEPSIS

RIVERS 2001 EGDT randomly assigned patients who arrived at an urban emergency department with severe sepsis or septic shock to receive either six hours of early goal-directed therapy or standard therapy (as a control) before admission to the intensive care unit. Clinicians who subsequently assumed the care of the patients were blinded to the treatment assignment. In-hospital mortality (the primary efficacy outcome), end points with respect to resuscitation Acute Physiology and Chronic Health Evaluation (APACHE II) scores were obtained serially for 72 hours and compared between the study groups.

RIVERS 2001 EGDT Of the 263 enrolled patients, 130 were randomly assigned to early goal-directed therapy and 133 to standard therapy no significant differences between the groups with respect to base-line characteristics. In-hospital mortality was 30. 5 percent in the group assigned to early goal-directed therapy, as compared with 46. 5 percent in the group assigned to standard therapy (P=0. 009). During the interval from 7 to 72 hours, the patients assigned to early goal-directed therapy had a significantly higher mean (±SD) central venous oxygen saturation (70. a lower lactate concentration, a lower base deficit, and a higher p. H than the patients assigned to standard therapy (P≤ 0. 02 for all comparisons). 7 to 72 hour mean APACHE II scores were significantly lower, indicating less severe organ dysfunction, in the patients assigned to early goal-directed therapy than in those in standard therapy(13. 0± 6. 3 vs. 15. 9± 6. 4, P<0. 001).

EARLY GOAL DIRECTED THERAPY (PART 2) CV SO 2% CV ACCESS AND MONITORING AGRESSIVE CORRECTION OF INTRAVASCULAR VOLUME DEFICITS BROAD SPECTRUM ANTIBIOTICS BASED ON SUSPECTED SITE

CONFIRMATION OF EGDT PROMISE ARISE PROCESS

PROMISE TRIAL 51 CENTERS IN UK COMPARED EGDT WITH USUAL CARE END POINT ALL CAUSE 90 DAY MORTALITY

PROMISE RESULTS EGDT HAD MORE: FLUIDS, PRESSORS, PRBC TRANSFUSIONS, CV CATHETERS, ARTERIAL CATHETERS 90 DAY ALL CAUSE MORTALITY : EGDT- 29. 5 USUAL CARE- 29. 2

ARISE TRIAL 51 EMERGENCY ROOMS IN AUSTRALIA AND NEW ZELAND RANDOMIZED TO EGD THERAPY OR USUAL CARE 1600 PATIENTS

ARISE RESULTS EGD THERAPY RECIEVED MORE FLUIDS AND PRESSORS NO DIFFERENCE IN END POINT OF ALL CAUSE MORTALITY AT 90 DAYS

process trial In 31 emergency departments in the United States, septic shock to one of three groups for 6 hours of resuscitation: protocol-based EGDT; protocol-based standard therapy that did not require the placement of a central venous catheter, administration of inotropes, or blood transfusions; or usual care. end point was 60 -day in-hospital mortality. Secondary outcomes included longer-term mortality and the need for organ support.

process results 1341 patients, of whom 439 were randomly assigned to protocolbased EGDT, 446 to protocol-based standard therapy, and 456 to usual care. Resuscitation strategies differed significantly with respect to the monitoring of central venous pressure and oxygen and the use of intravenous fluids, vasopressors, inotropes, and blood transfusions. By 60 days, there were 92 deaths in the protocol-based EGDT group (21. 0%), 81 in the protocol-based standard-therapy group (18. 2%), and 86 in the usual-care group (18. 9%) There were no significant differences in 90 -day mortality, 1 -year mortality, or the need for organ support.

EGDT (PART 3) FANCY CATHETER NOT NEEDED CV ACCESS +/BENIFIT ONLY IN SHOCK PATIENT ANTIBIOTICS OUT TO 3 HOURS

EGDT (PART 3) ALL PATIENTS ARE ER ALL SUSPECTED SEPIS ON ARRIVAL ALL HYPOTENSIVE

FOR NOW
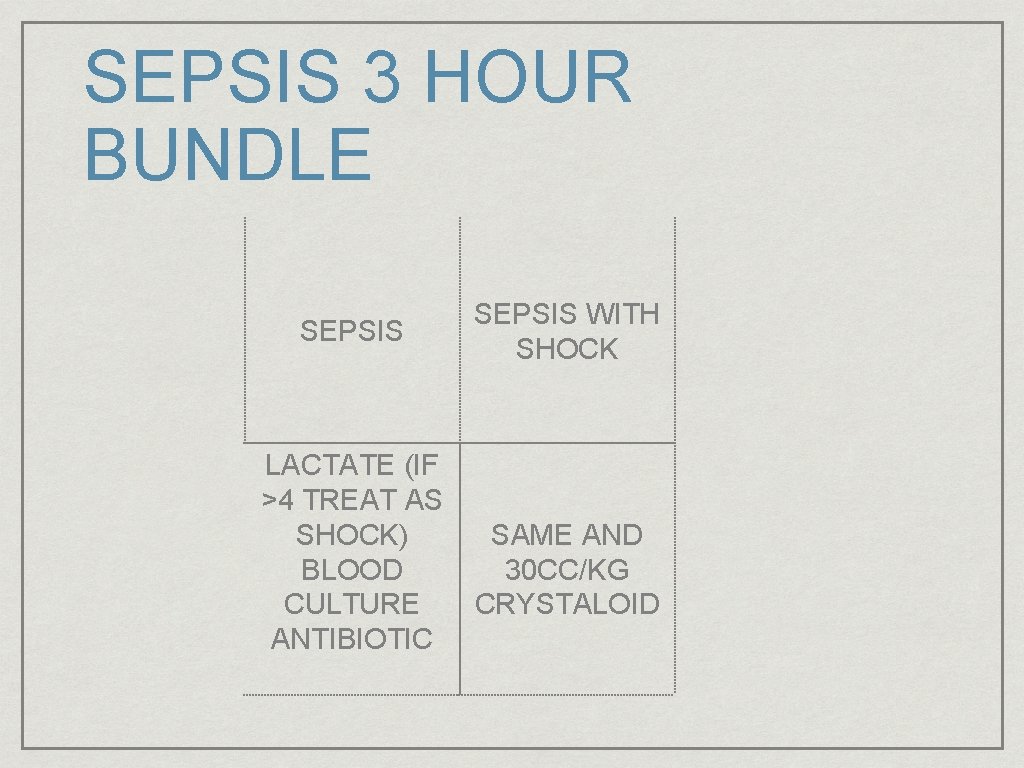
SEPSIS 3 HOUR BUNDLE SEPSIS LACTATE (IF >4 TREAT AS SHOCK) BLOOD CULTURE ANTIBIOTIC SEPSIS WITH SHOCK SAME AND 30 CC/KG CRYSTALOID

SEPIS 6 HOUR BUNDLE SEPIS WITH SHOCK REPEAT LACTATE PRESSORS TISSUE PERFUSIONN EXAM CVP, Scv. O 2, other
SURVIVING SEPSIS CVP > 8 CONSIDER TRANSFUSION OF HCT < 30 AND HYPO-PERFUSION SCVO 2> 70 MAP > 65 URINE OUT > 0. 5 CC/KG/HR

APPROPRIATE ANTIBIOTICS 1 -4 HOURS THEN MORTALITY INCREASES INSTITUTION SPECIFIC BASED ON LIKELY SOURCE CONTROL LESS THAN 6 HOURS

CENTRAL VENOUS ACCESS HYPOTENSION PERSISTS AFTER FLUID BOLUS (ie use of pressors) NO CONTRA-INDICATION

SEVERE SEPIS SIRS/SEPIS WITH END ORGAN HYPOPERFUSIOIN LACTATE > 2 NEW ELEVATION OF CREAT > 2 ARDS U out <0. 5 ml/kg/hr MAP <65 / BP < 90/60 HEPATIC DYSFUNCTION: INR > 1. 5 OR BILI > 2 DIC, PLTS < 100, 000 CARDIAC DYSFUNCTION

SHOCK HYPOTENSION PERSISTING AFTER 30 CC/KG CRYSTALOID BOLUS ( NS, LR, NORMOSOL) PRESSORS : first choice is norepinephrine
Svc. O 2 IS A MEASURE OF ADEQUACY OF TISSUE PERFUSION MEASURING CATHETER, BLOOD GAS VIA SVC LINE ADD HB IF PERSISTS < 70%

MAYO CLINIC ICU PROTOCOL LACTATE LEVEL X 2 3 HOURS APART IF NORMAL- STOP IF SUSPECT SEPIS ANTIBIOTIC, 30 ML/KG BALANCED OR CHLORIDE RESTRICED FLUIDS MAP >65 AND 50% REDUCTION LACTATE LEVEL BY 6 HOURS DE-EMPHASIZED CVP, SCVO 2 AND RBC TRANSFUSION

BUT REMEMBER INTERVENTIONS (LARGE VOLUME FLUID AND LARGE SALT LOAD OF ANTIBIOTICS) ARE NOT BENIGN NOT ALL SIRS IS SEPSIS


SEPSIS MIMICS ITS NOT JUST AN NUMBER

SEPSIS MIMICS NON INFECTIOUS SIRS CARDIAC PATIENTS- TACHICARDIC DYSRYTHMIAS, TAMPONADE AKI AND DEHYDRATION ADRENAL CRISIS OCCULT BLEED

NON SEPSIS CAUSES OF ELEVATED LACTATE HYPOXIA REGIONAL OR GENERAL HYPOPERFUSION DECREASED CLEARANCE RENAL OR HEPATIC DYSFUNCTION MEDICATIONS OR TOXINS DECREASING OXIDATIVE PHOSPORYLATION -antiviral, diabetic, anticonvulsant, antibiotic, beta agonist, propofol …. KETOSIS- ETOH AND DIABETIC SEIZURE

DISTRIBUTIVE SHOCK WARM AT START INCREASED PULSE PRESSURE INCREASED CARDIAC OUTPUT AND DECREASED SYSTEMIC VASCULAR RESISTANCE SEPSIS ONE OF 5 SUBTYPES OF DISTRIBUTIVE SHOCK

SHOCK CARDIOGENIC SHOCK #1 CAUSE DEATH IN US HEMORRHAGIC SHOCK #1 CAUSE DEATH UNDER AGE 45 SEPTIC SHOCK #13 CAUSE DEATH IN US

HOW WELL DO ALERTS WORK WHAT PATIENT POPULATION IT IS APPLIED TO SELECTION BIAS: ER, ICU TELE FLOOR

CHALLENGES “GARBAGE IN GARBAGE OUT” - QUALITY OF DATA INPUT INTO EHR THAT TRIGGERS RESPONSE REPLICATION OF ROBUST TEAMS THAT ALLOW EXPERIENCED CLINICIANS TO EVALUATE EARLY ALARM BIAS ALARM FATIGUE

FAILURE TO DUPLICATE STUDY DESIGN SEPSIS MODEL DATA FEED IDENTIFY AT RISK INCREASED MONITOR CLINICAL DECISON BEGIN AN EVIDENCED BASED CARE PLAN VS RETURN TO DATA FEED

OPINION

OPINIONS START WITH THE HIGH RISK PATIENTS MISSED DIAGNOSIS (LESS THAN 24 HOURS ADMISSION) RECENTLY OUT OF ICU AGE > 65 INTRA ABDOMINAL PATHOLOGY

OPINIONS YOU SHOULD BE THINKING INFECTION BEFORE YOUR GO DOWN THE SEPSIS PATH CONFIRM CHANGE IN VITALS AND TRY OBTAIN ORTHOSTATIC BP IDENTIFY ALL POSSIBLE REASONS FOR CHANGE IN VITALS DO YOU THINK THE PATIENT IS THIRD SPACING-THE BASE PHYSIOLOGY OF SIRS IF SEPSIS WITH SHOCK VOLUME-VOLUME

JUST OPINIONS IF YOU OBTAIN BLOOD CULTURES YOU SHOULD START OR ALTER ANTIBIOTICS IF YOU START A 30 CC/KG BOLUS YOU SHOULD TRANSFER TO ICU

QUESTIONS
- Slides: 77