Randomized Embedded Multifactorial Adaptive Platform trial for Community

Randomized, Embedded, Multifactorial Adaptive Platform trial for Community. Acquired Pneumonia Background & Design

REMAP-CAP • Randomised • Rather than random clinician choice • Embedded • Recruitment by clinical staff (and / or research coordinators) • Deliver intervention using usual clinical processes • Multifactorial • Simultaneously assess different aspects of treatment • • • Therapeutic anticoagulation (ward and ICU) Antivirals Immunomodulation Immunoglobulin therapy Vitamin C & Statins (coming soon) • Adaptive
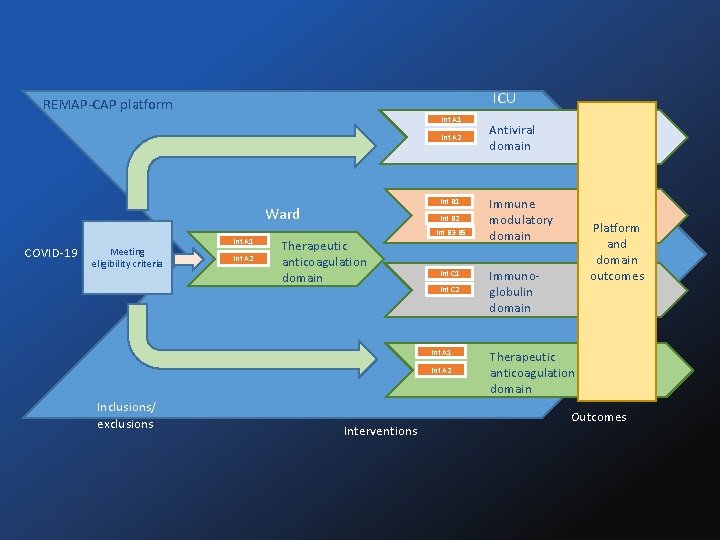
ICU REMAP-CAP platform Int A 1 Int A 2 Int B 1 Ward COVID-19 Meeting eligibility criteria Int A 1 Int A 2 Int B 2 Therapeutic anticoagulation domain Int B 3 -B 5 Int C 1 Int C 2 Int A 1 Int A 2 Inclusions/ exclusions Interventions Antiviral domain Immune modulatory domain Platform and domain outcomes Immunoglobulin domain Therapeutic anticoagulation domain Outcomes

REMAP-CAP • Randomised • Embedded • Multifactorial • Adaptive • Frequent Bayesian adaptive analyses • Response adaptive randomisation • Add / subtract domains and intervention • Platform Trial • All patients with COVID-19 included

Response Adaptive Randomisation • RAR varies randomisation proportions as trial data or interim analyses accrue • Higher probability an intervention is superior increases the proportion assigned for next week • Higher probability an intervention is inferior decreases the proportion assigned for next week • More likely to receive the most beneficial treatment in the trial vs outside trial • If an intervention is superior, trial saves lives

Analysis and RAR during pandemic • Statistical model evaluates all pandemic domains • Evaluates patients who are confirmed COVID-19 and not confirmed COVID 19 separately with borrowing between stratum, as appropriate • Reduction in statistical trigger from 0. 99 to 0. 95 probability of superiority • RAR driven off confirmed COVID-19 for future suspected and confirmed patients • Assesses safety in suspected patients

Primary end-point Days alive and not receiving organ support in ICU at Day 21 • Censored at hospital discharge (no need to follow-up after hospital discharge until usual D 90) • It is VITAL that D 21 endpoint is entered as soon as possible after the end of study day 21 • D 90 follow up still required • D 180 follow up not required for patients

Randomized, Embedded, Multifactorial Adaptive Platform trial for Community. Acquired Pneumonia Platform eligibility

Pandemic platform eligibility Platform inclusion criteria: 1. Adult patient admitted to hospital with acute illness due to suspected or proven pandemic infection Platform exclusion criteria: 1. Death is deemed to be imminent or inevitable during the next 24 hours AND one or more of the patient, substitute decision maker or attending physician are not committed to full active treatment 2. Patient expected to be discharged from hospital today or tomorrow 3. >14 days have elapsed while admitted to hospital with symptoms of acute illness due to suspected/proven pandemic infection 4. Previous participation in this REMAP within the last 90 days

Inclusion definitions Does the patient have clinically suspected or proven pandemic infection • Clinically suspected = treating clinician believes that pandemic infection is a likely diagnosis • That testing is being done is not sufficient, must think pandemic infection is likely • Suspected or proven hospital-acquired pandemic infection are eligible

Changes to eligibility The following platform eligibility criteria do not apply for patients with clinically suspected or proven pandemic infection: • Is the patient a resident of a nursing home or long-term care facility • Prior to this illness was the patient known to be an inpatient in any healthcare facility within the last 30 days • Does the patient have signs and/or symptoms that are consistent with lower respiratory tract infection • Does the patient have radiological evidence of new onset infiltrate of infective origin • Time window from hospital admission to ICU admission

Changes to eligibility Patients may now be eligible in both Moderate and Severe disease states: • Severe State = receiving organ support in ICU • Moderate State = • • In ICU but not receiving organ support Not in ICU Patients may receive allocations while in Moderate state and later receive an allocation to other domains if then progress to Severe state. Patients in Severe state cannot receive
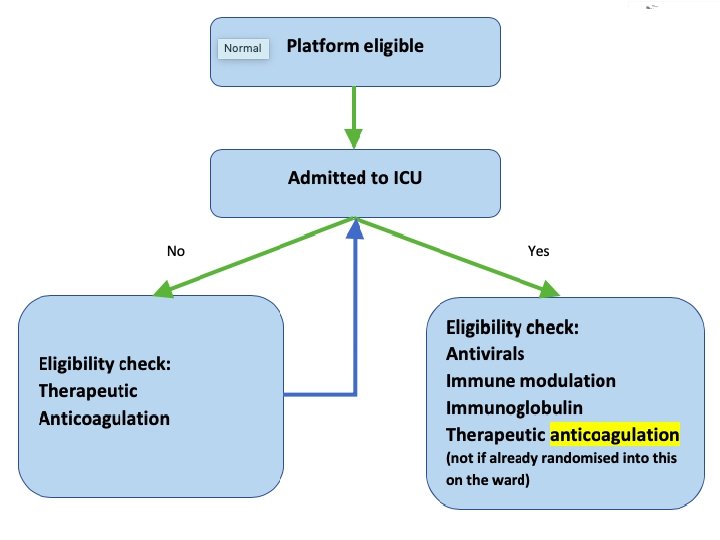
Definitions

Randomized, Embedded, Multifactorial Adaptive Platform trial for Community. Acquired Pneumonia Domain eligibility/intervent ions

Randomized, Embedded, Multifactorial Adaptive Platform trial for Community. Acquired Pneumonia Therapeutic Anticoagulation Domain

Interventions Available Interventions: • Local standard thromboprophylaxis • Using pharmacological agents • Therapeutic anticoagulation with unfractionated heparin (UFH) or subcutaneous low molecular weight heparin (LMWH) Available to patients in the following States: • Moderate (not in ICU or not receiving organ support in ICU)

Eligibility Inclusion Criteria: • Platform eligible

Eligibility Exclusion Criteria: • >48 hours since ICU admission • Note: >48 h since first organ support, if already randomised in Moderate State. • Clinical or laboratory bleeding risk sufficient to contraindicate therapeutic anticoagulation • Intention to continue or commence dual anti-platelet therapy • Therapeutic anticoagulation is already present, or decision to commence therapeutic anticoagulation

Eligibility Exclusion Criteria: • Enrolment in a trial evaluating anticoagulation for COVID-19 infection, where the protocol requires continuation of the treatment assignment • Known or suspected adverse reaction to UFH or LMWH, including HIT • Treating clinician believes that participation is not in the best

Local standard thromboprophylaxis • Standard venous thromboprophylaxis as per local guidelines • Dose of agent should not be sufficient to result in therapeutic anticoagulation • Administered for 14 days or hospital discharge, whichever occurs first • Administration after day study 14 is at the discretion of the treating clinician

Local standard thromboprophylaxis • Therapeutic anticoagulation can be commenced if patient develops an accepted clinical indication for anticoagulation • DVT, proven PE, acute coronary syndrome, systemic embolic event, intermittent haemodialysis, or SLED • Systemic therapeutic anticoagulation for c. RRT is not permitted, unless there is additional indication for anticoagulation. • Regional low-dose heparin permitted to prevent filter clotting, however dose of

Local standard thromboprophylaxis • If unfractionated heparin is used, doses should be below those expected to achieve therapeutic anticoagulation. • If LMWH is used, standard low dose is preferred, but intermediate thromboprophylaxis dose (e. g. no more than double standard low thromboprophylaxis dose) is acceptable if it has become standard practice at the site.

Therapeutic Anticoagulation • Administer UFH or LMWH to achieve systemic anticoagulation. • As per local hospital policy and guidelines for the treatment of VTE • Either agent may be used, and the same patient may be switched between UFH and LMWH • Cease (whichever occurs first): • On study day 15, • 24 hours after liberation from invasive mechanical ventilation, or • ICU or hospital discharge

Discontinuation of intervention • Study intervention should be discontinued if there is clinical bleeding or other complication • Anticoagulation or local standard venous thromboprophylaxis may be recommenced if deemed appropriate by the treating clinician. • Laboratory-proven HIT must result in cessation of UFH or LMWH without recommencement • Study interventions can be discontinued

Concomitant Care • Additional agents intended to modify the patient’s coagulation as a treatment for COVID-19 infection should not be administered • Commencement of any agent that inhibits platelet function is not permitted unless there is an accepted clinical indication • Patients who receive agent(s) which inhibit platelet function as a usual medication may have this medication continued

End-point Secondary endpoints • Serial detection of SARS-Co. V-2 in upper or lower respiratory tract specimens • using only specimens collected for routine clinically indicated testing • Confirmed VTE or PE • RBC transfused between randomization and end of study day 15

Randomized, Embedded, Multifactorial Adaptive Platform trial for Community. Acquired Pneumonia ICU Level Domains

Antiviral Domain Available Interventions: • No antiviral intended to be active against SARS-Co. V-2 infection (no placebo) • Lopinavir/ritonavir (‘Kaletra’) Available to patients in the following States: • Moderate (not receiving organ support in ICU) • Severe (receiving organ support in ICU)

Immune Modulator Domain Available Interventions: • No immune modulation therapy intended to be active against COVID-19 (no placebo) • Interferon-beta-1 a (IFN-β 1 a) • Anakinra (interleukin-1 receptor antagonist) • Tocilizumab (IL-6 inhibition) • Sarilumab (IL-6 inhibition) Available to patients in the following States: • Moderate (not receiving organ support in ICU)

Immunoglobulin Domain Available Interventions: • No immunoglobulin against COVID-19 (no placebo) • Convalescent plasma (standard or intensive sampling) Available to patients in the following States: • Moderate (not receiving organ support in ICU)

Vitamin C Domain Available Interventions: • No vitamin C (no placebo) • Vitamin C Available to patients in the following States: • Moderate (not receiving organ support in ICU) • Severe (receiving organ support in ICU)

Statin Domain Available Interventions: • No statins (no plcebo) • Simvastatin Available to patients in the following States: • Moderate (not receiving organ support in ICU) • Severe (receiving organ support in ICU)

Randomized, Embedded, Multifactorial Adaptive Platform trial for Community. Acquired Pneumonia Randomisation on ward

Login screen Generic login for site clinical users remapcapds 9+++ https: //remapcap. spinnakersoftw

e. CRF Eligibility Assess eligibility of a new patient
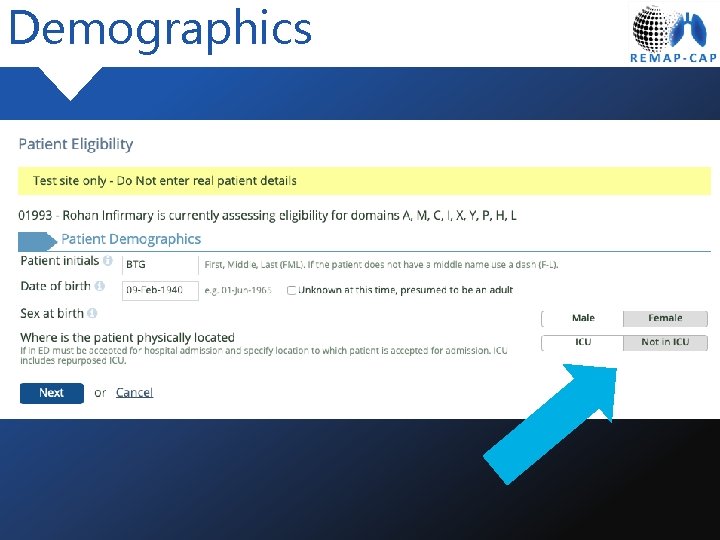
Demographics

Disease and Platform Eligibility

Disease and Platform Eligibility

Disease and Platform Eligibility

Domain and Intervention Eligibility

Domain and Intervention Eligibility
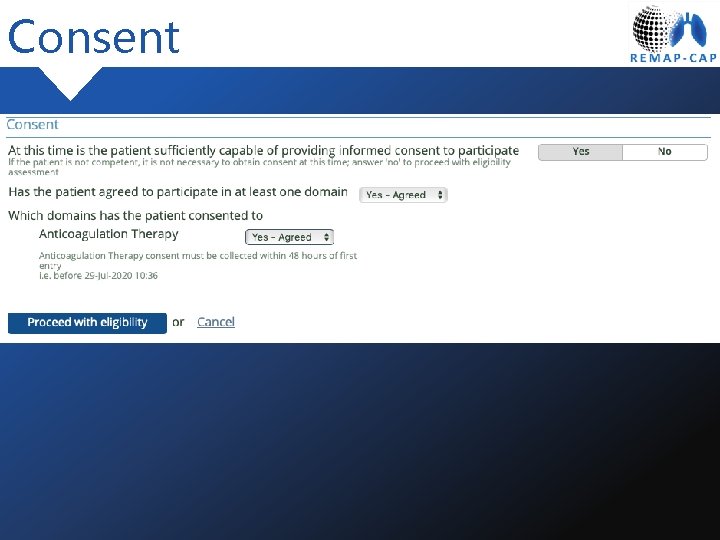
Consent
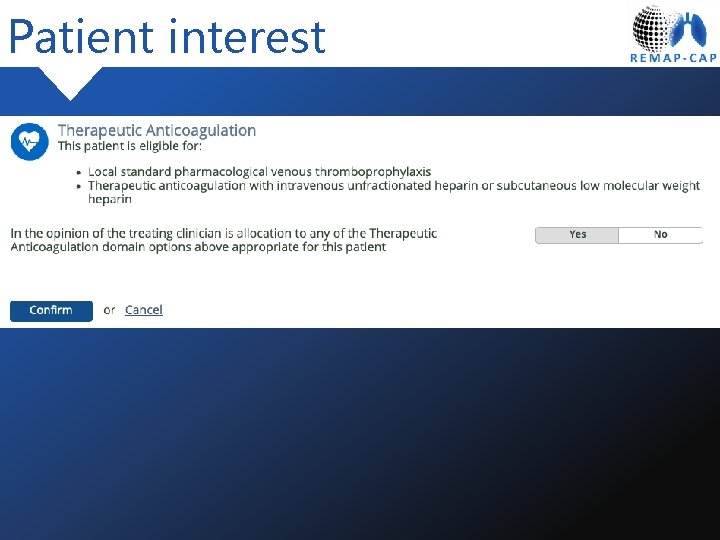
Patient interest

Randomisation
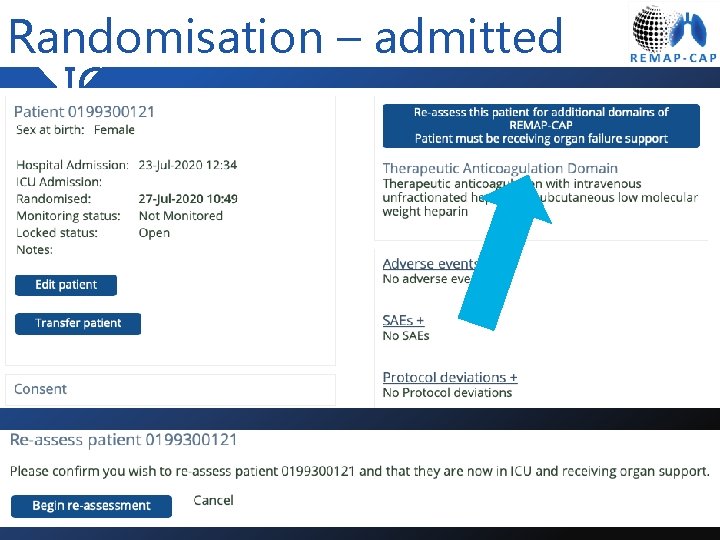
Randomisation – admitted to ICU
- Slides: 45