Radiological Category OB Ultrasound Principal Modality 1 Ultrasound
Radiological Category: OB Ultrasound Principal Modality (1): Ultrasound Principal Modality (2): None Case Report # 764 Submitted by: Mary Kristen Jesse, M. D. Faculty reviewer: Venkateswar Surabhi, M. D, The University of Texas Medical School at Houston Date accepted: 15 February, 2011

Case History 28 -year-old, G 2 P 1 A 0 female at 21 weeks gestation presents to the emergency department with pelvic pain and vaginal bleeding.
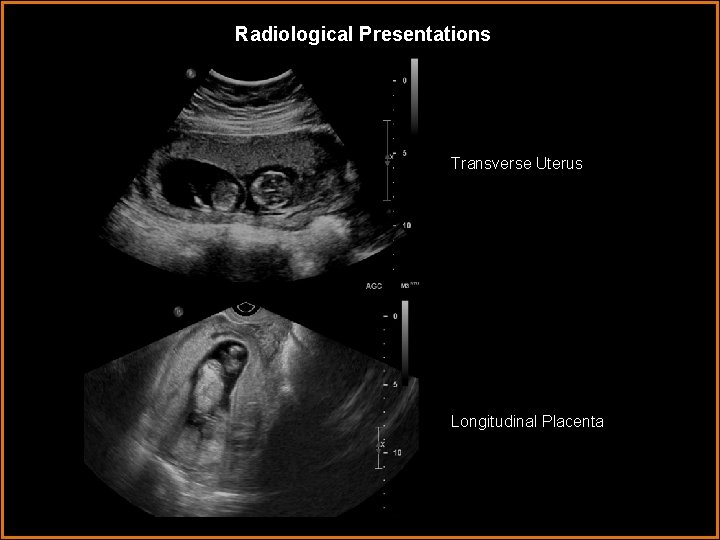
Radiological Presentations Transverse Uterus Longitudinal Placenta
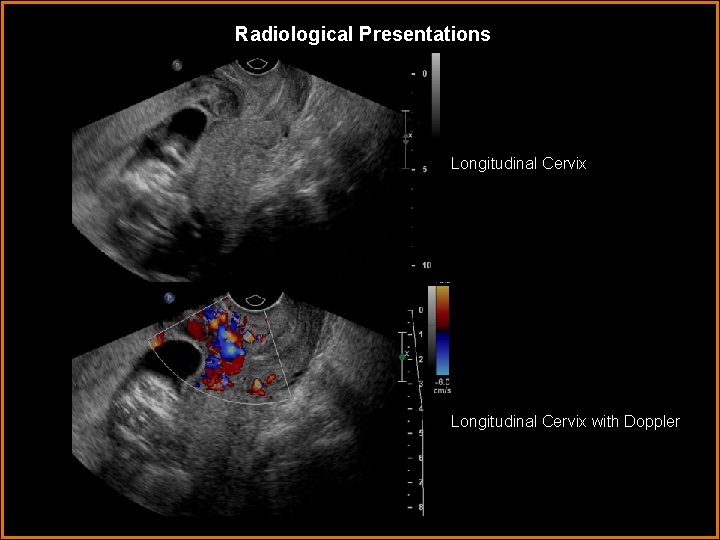
Radiological Presentations Longitudinal Cervix with Doppler

Test Your Diagnosis Which of the following is your choice for the appropriate diagnosis? After your selection, go to next page. A. Marginal sinus previa B. Cord presentation C. Placenta accreta D. Vasa previa E. Placenta increta

Findings and Differentials Findings: Transvaginal ultrasound demonstrates a viable monochorionic/diamniotic twin gestation. Placental tissue is present on either side of the cervix. Longitudinal views of the cervix demonstrate multiple anechoic structures within the gestational sac which cross midline in the region of the cervix. On Doppler interrogation, flow is demonstrated within these structures. Differentials: • Type I vasa previa • Type II vasa previa • Cord presentation • Marginal sinus previa
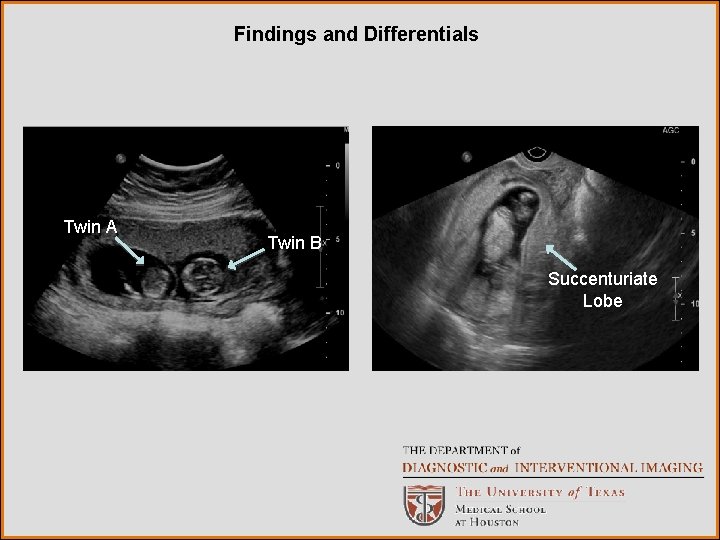
Findings and Differentials Twin A Twin B Succenturiate Lobe
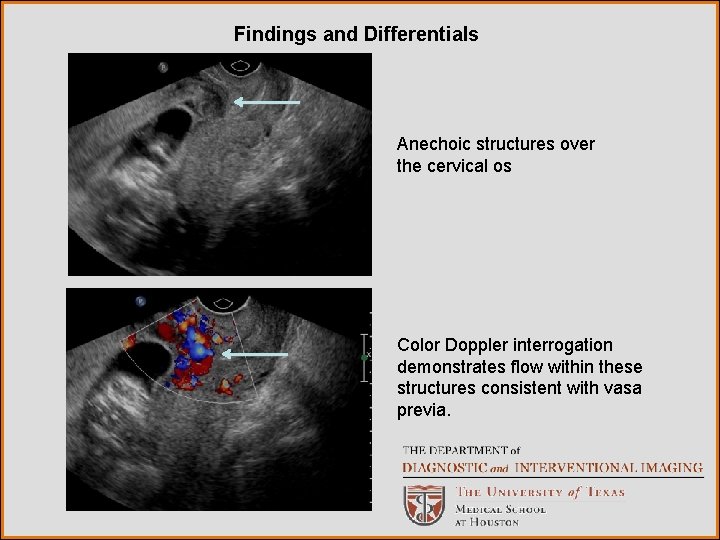
Findings and Differentials Anechoic structures over the cervical os Color Doppler interrogation demonstrates flow within these structures consistent with vasa previa.

Discussion Vasa previa occurs when submembranous fetal vessels cross or run in close proximity to the cervical os. This entity has been described in as many as 1: 3000 deliveries. Complications of vasa previa can be avoided by performing cesarian section at the time of delivery. According to the article by Gagnon et al, if vasa previa is undiagnosed at the time of delivery, the fetal survival rate is 44%, compared with 97% survival if the diagnosis is known. Complications of vasa previa include peripartum hemorrhage and prenatal venous compression and thrombosis. Type II vasa previa, the most common form, occurs in the presence of a succenturiate (accessory) lobe of the placenta. Two separate lobes of the placenta are connected by vessels which cross the cervical os. These abnormal vessels can be demonstrated using Doppler evaluation. Type I vasa previa occurs in the setting of villamentous insertion of the umbilical cord. In these cases, the umbilical cord inserts on the membranes adjacent to a low-lying placenta, near or over the cervical os.
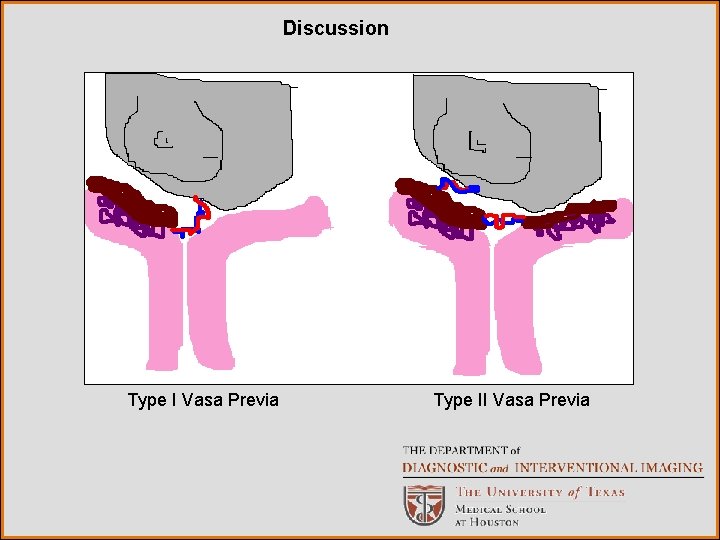
Discussion Type I Vasa Previa Type II Vasa Previa

Discussion A monochorionic twin gestation, as in this case, and uterine abnormalities increase the risk of vasa previa. Although this abnormality is usually detected during a third trimester ultrasound, vasa previa may be detected as early as the second trimester. In the article by Lee et al, the earliest detectable case of vasa previa occurred at 15 weeks gestation. Vasa previa is usually an incidental finding on prenatal ultrasound, but patients will occasionally present with abdominal pain and second- or thirdtrimester bleeding. It is important to maintain a high index of suspicion when performing obstetric ultrasounds, especially in the presence of monochorionic twin gestation or a succenturiate lobe of the placenta. Color Doppler evaluation of the cervix and cervical os should always be performed in these cases.

Discussion Marginal sinus previa occurs when maternal placental veins lie at or near the cervical os. These cases have normal placenta and cord insertion and occur in the setting of marginal placenta previa. Cord presentation describes the scenario in which an otherwise normal umbilical cord is the presenting structure at labor. These deliveries are at increased risk for cord accident or nuchal cord.

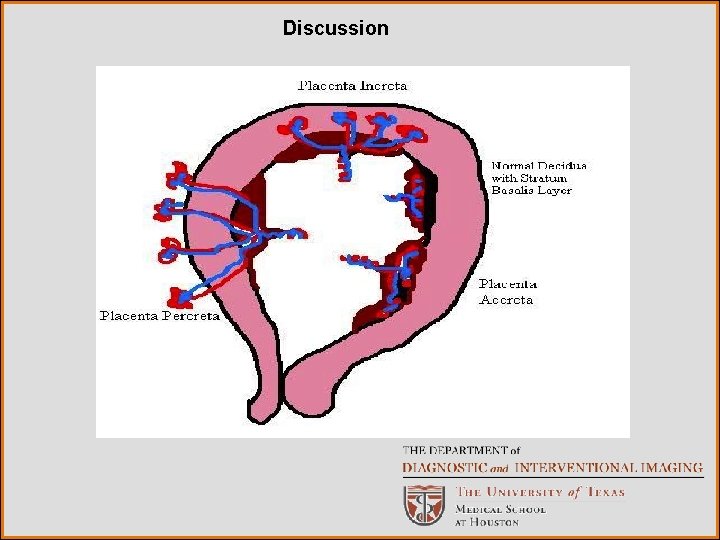
Discussion In some cases, the placenta may attach abnormally to the uterine wall, leading to an increased risk of hemorrhage. The spectrum of abnormal uterine attachment is described below. Placenta accreta: The placenta is abnormally adherent to the myometrium with partial or complete absence of the decidua basalis. This comprises the vast majority of cases of abnormal placental attachment. Placenta increta: The placenta is abnormally adherent to and invades the uterine myometrium. The placenta does not breach the external uterine wall. Placenta percreta: The rarest and most severe form of placental invasion, in which the placenta invades through both the myometrium and the uterine serosa (the outerine wall). In this form, the placenta can also invade adjacent structures such as the bladder.
Discussion

Diagnosis Type II vasa previa.

References Hasegawa J, Farina A, Nakamura M, Matsuoka R, Ichizuka K, Sekizawa A, Okai T. “Analysis of the ultrasonographic findings predictuve of vasa previa. ” Prenatal Diagnosis. 2010 Dec; 30(12 -13): 1121 -5. Gagon R, Morin L, Bly S, Butt K, Cargill Ym, Denis N, Hietala-Coyle MA, Lim KI. “Guidelines for the management of vasa previa. ” Obstetrics Gynaecology Canada. 2009 Aug; 31(8): 748 -60. Lee W, Lee VL, Kirk JS, Sloan CT, Smith RS, Comstock CH. “Vasa previa: prenatal diagnosis, natural evolution, and clinical outcome. ” Obstetrics Gynecology 2000 Apr; 95(4): 572 -6. Beale MH et al. “Umbilical cord complications. ” Emedicine 2009. Sohaey R. “Vasa previa. ” Stat. DX.
- Slides: 16