Radiological Category Neuroradiology Principal Modality 1 MRI brain

Radiological Category: Neuroradiology Principal Modality (1): MRI brain Principal Modality (2): CT brain Case Report # 760 Submitted by: Yueping Hou, M. D. Faculty reviewer: Emilio Supsupin Jr. , M. D. , The University of Texas Medical School at Houston Date accepted: 2 February, 2011

Case History 23 -year-old male presents to the ENT clinic with chronic nasal congestion and extensive polyposis filling the entire nasal cavity on clinical examination. This is painless and associated with halitosis. There are no other symptoms such as epistaxis, hemoptysis, fever, odynophagia, weight loss, or night sweats.
Radiological Presentations
Radiological Presentations
Radiological Presentations

Test Your Diagnosis Which one of the following is your choice for the appropriate diagnosis? After your selection, go to next page. • Fungal sinusitis • Neoplasm/lymphoma • Inverting Papilloma

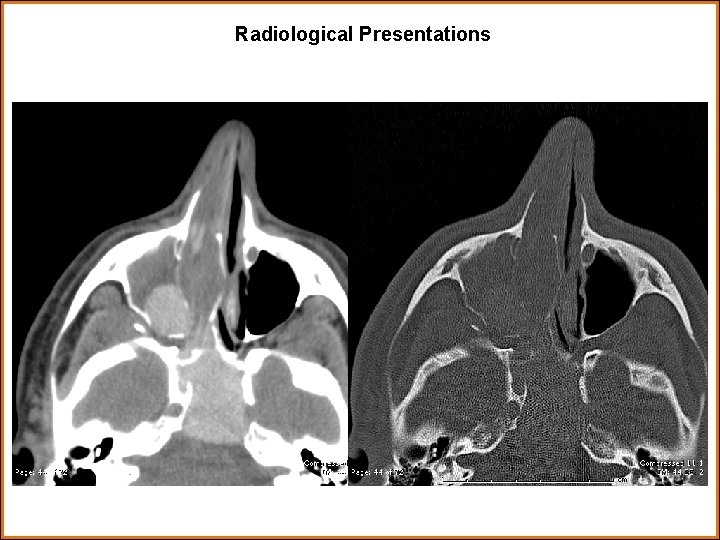
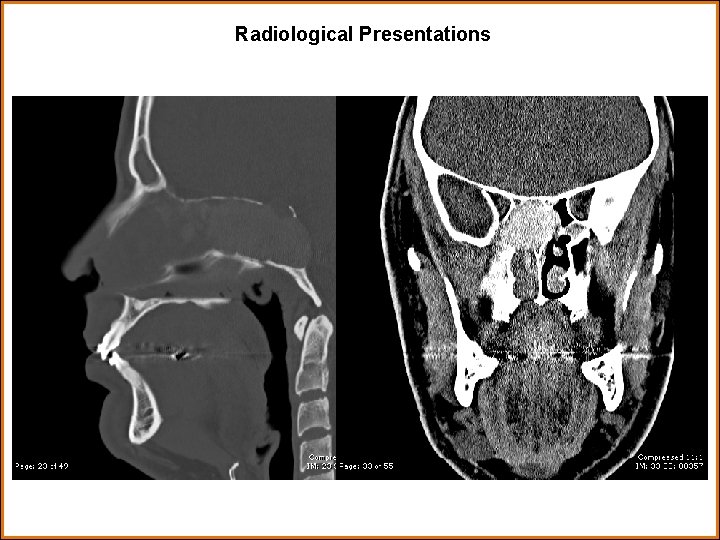
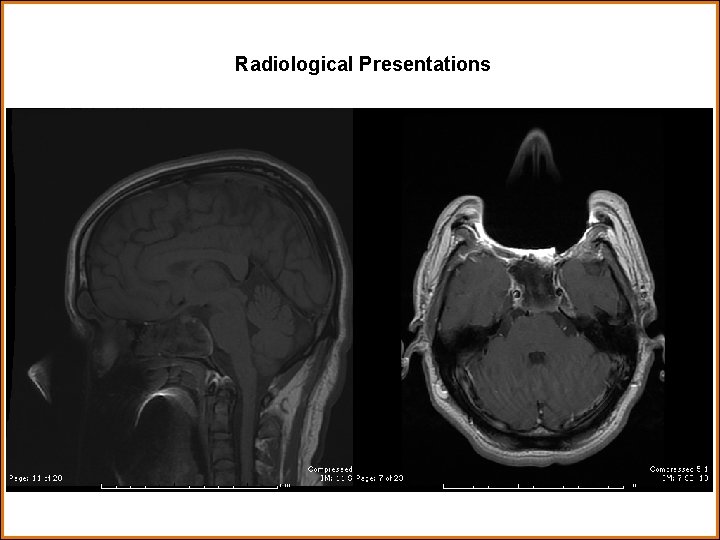
Findings and Differential Diagnosis Findings: CT brain: Expansile lesion centered in the sphenoid sinus with extension to the paranasal cavities and the skull base with bone remodeling and destruction. Resembles an aggressive infection such as fungal sinusitis. MRI brain: Large soft tissue mass with minimal heterogeneous enhancement centered at and occupies the sphenoid sinus/central skull base with extension into the posterior ethmoid air cells and superior nasopharynx. Internal susceptibility artifacts within the lesion noted. Does not appear to invade the cavernous carotid. Differentials: • Fungal sinusitis • Inverting papilloma • Lymphoma • Squamous cell carcinoma • Juvenile nasal angiofibroma

Diagnosis Right nasal endoscopy with frontal sinusotomy, sphenoidotomy, total ethmoidectomy, maxillary antrostomy, and removal of sinus contents. Pathology confirms the diagnosis of allergic fungal sinusitis.

Discussion Allergic fungal sinusitis (AFS) (sometimes called allergic sinonasal aspergillosis) is believed to be an allergic reaction to aerosolized environmental fungi. It presents clinically as a severe form of chronic rhinosinusitis with production of eosinophilic mucin containing noninvasive fungal hyphae. In contrast to invasive fungal infections that affect mostly immunocompromised hosts such as people with diabetes or AIDS, AFS happens primarily in immunocompetent patients. However, most of them do have a history of allergic rhinitis. About 40% of patients with AFS are also asthmatics. Clinical presentation of AFS patients include symptoms of chronic rhinosinusitis, such as nasal obstruction, purulent rhinorrhea, postnasal drainage, or headaches. More advanced cases may also develop facial deformity or diplopia. CT without contrast enhancement is considered the imaging modality of choice for the diagnosis of AFS by many. The nonenhancing CT typically shows material of increased attenuation causing opacification and expansion of the sinuses with bony remodeling/erosion. The increased attenuation of AFS is believed to be most likely related to the combined effects of heavy metals such as iron, manganese, and calcium, as well as inspissated mucosal secretion. CT is especially valuable in evaluating the bony changes. Peripheral mucosal enhancement can typically be seen in post contrast CT images. This is presumably secondary to the inflammatory reactions to the fungal invasion.
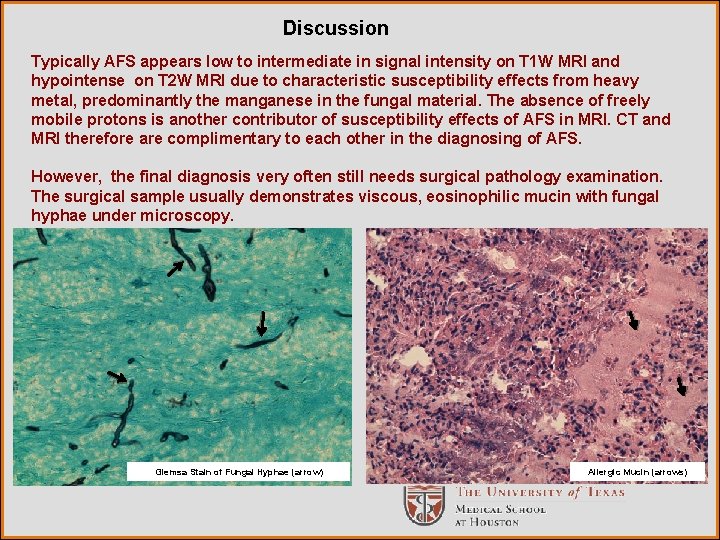
Discussion Typically AFS appears low to intermediate in signal intensity on T 1 W MRI and hypointense on T 2 W MRI due to characteristic susceptibility effects from heavy metal, predominantly the manganese in the fungal material. The absence of freely mobile protons is another contributor of susceptibility effects of AFS in MRI. CT and MRI therefore are complimentary to each other in the diagnosing of AFS. However, the final diagnosis very often still needs surgical pathology examination. The surgical sample usually demonstrates viscous, eosinophilic mucin with fungal hyphae under microscopy. Giemsa Stain of Fungal Hyphae (arrow) Allergic Mucin (arrows)

Discussion Differential diagnosis of Allergic fungal sinusitis (AFS) often include sinonasal polyposis, sinonasal mucocele, fibrous dysplasia, and ossifying fibroma. Inverted papilloma, squamous cell carcinoma, and non-Hodgkin lymphoma are less common. • Sinonasal polyposis: Homogeneous masses, low on T 1 and high on T 2 due to relatively high fluid content, more likely hypodense on noncontrast CT. • Sinonasal mucocele: Opacified, expanded sinus cavity with low density on noncontrast CT; generally low T 1 and high T 2 signal likely secondary to a relatively high fluid content. • Squamous cell carcinoma: Enhancing solid mass with bony destruction. Relatively hypointense on T 2. • Inverted papillomas: Nonspecific enhancing lobular mass on lateral nasal wall. Typically isodense to muscle on T 1 and iso- to hypointense on T 2 W MR. • Non-Hodgkin lymphoma: Soft tissue mass with bone remodeling/destruction; homogeneous with diffuse enhancement in MR.

References 1. Proc Am Thorac Soc. 2010 May; 7(3): 245 -52. Allergic fungal rhinitis and rhinosinusitis. Hamilos DL. 2. Radiographics. 2007 Sep-Oct; 27(5): 1283 -96. Imaging features of invasive and noninvasive fungal sinusitis: a review. Aribandi M, Mc. Coy VA, Bazan C 3 rd. 3. Curr Opin Otolaryngol Head Neck Surg. 2007 Feb; 15(1): 18 -22. Allergic fungal rhinosinusitis: diagnosis and management. Ryan MW, Marple BF. 4. Statdx. com.

Acknowledgment Special thanks to Dr. Ekene Okoye from the University of Texas Medical School at Houston, Department of Pathology for providing pathology microphotography.
- Slides: 13