Radiofrequency ablation HALO in the treatment of Oesophageal

Radiofrequency ablation (HALO) in the treatment of Oesophageal Dysplasia Bristol Royal Infirmary M. Boal, D. Titcomb 2/2/17
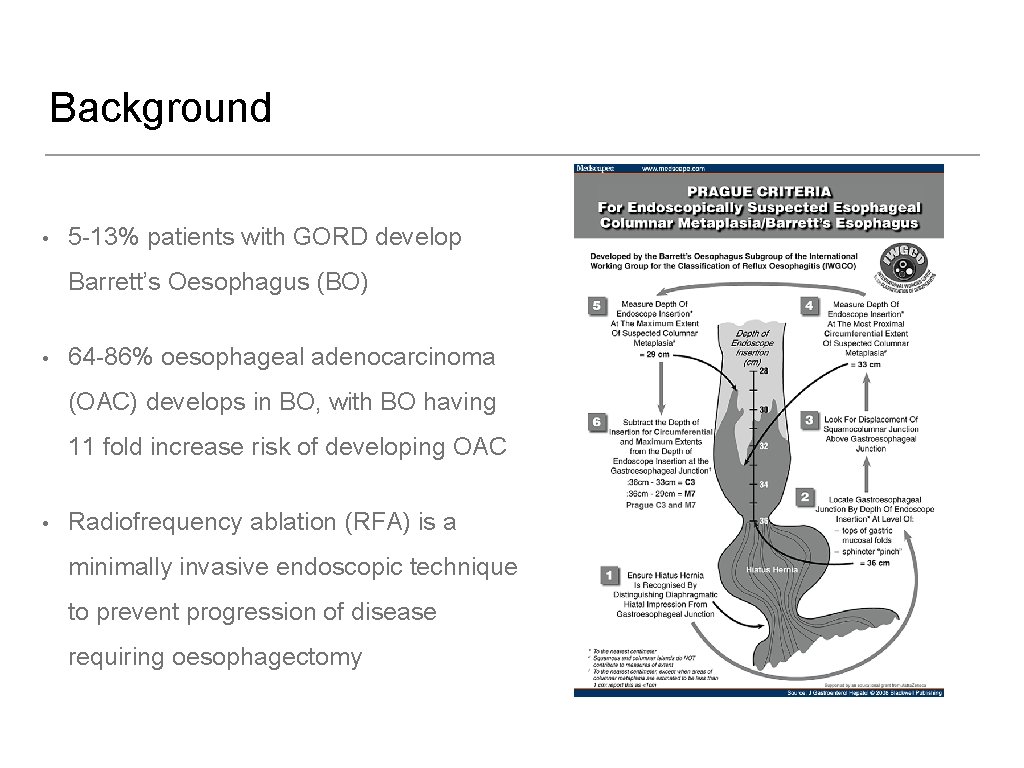
Background • 5 -13% patients with GORD develop Barrett’s Oesophagus (BO) • 64 -86% oesophageal adenocarcinoma (OAC) develops in BO, with BO having 11 fold increase risk of developing OAC • Radiofrequency ablation (RFA) is a minimally invasive endoscopic technique to prevent progression of disease requiring oesophagectomy
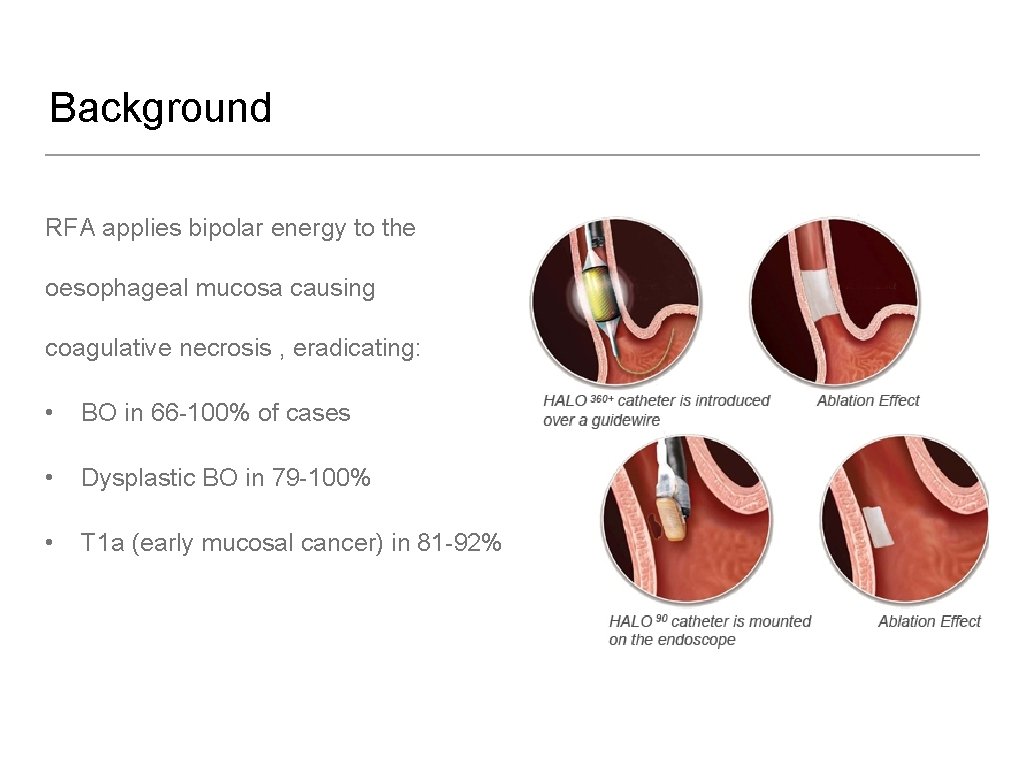
Background RFA applies bipolar energy to the oesophageal mucosa causing coagulative necrosis , eradicating: • BO in 66 -100% of cases • Dysplastic BO in 79 -100% • T 1 a (early mucosal cancer) in 81 -92%

NICE guidance 2010: • Recommend use in dysplastic BO • Use in non-dysplastic BO and squamous dysplasia for research purposes 2014: • Enough evidence for use in low grade dysplasia (LGD)

The British Society of Gastroenterologists guidance • RFA is preferred to oesophagectomy or surveillance in high grade dysplasia (HGD) and Barrett’s related OAC confined to mucosa (Grade B recommendation) • Post EMR visible flat lesions should be managed with RFA (Grade A recommendation) • Follow up endoscopy

NOGCA • Despite The BSG/ NICE recommendation that RFA should be offered to patients with HGD, Tis/T 1 a disease, NOGCA data suggests 29. 7% are still offered surveillance.

Aim: • Rates of dysplasia progression and regression for patients who underwent radiofrequency ablation (HALO/Barrx-Flex)

Primary outcome: • Assess rates of disease regression post index RFA intervention Secondary: • Assess rates of disease progression post RFA intervention and complication

Method: • Single centre • Retrospective data extracted from clinical/electronic notes • 1 st data set June 2011 - Oct 2014 • 2 nd data set Nov 2014 -Dec 2016
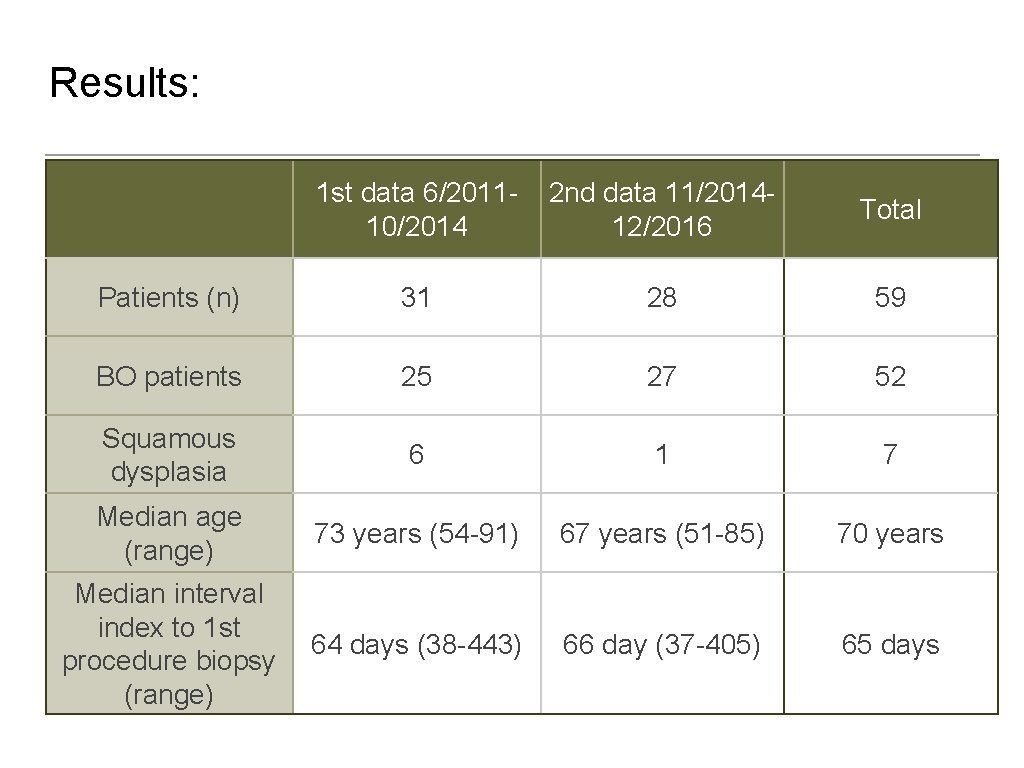
Results: 1 st data 6/201110/2014 2 nd data 11/201412/2016 Total Patients (n) 31 28 59 BO patients 25 27 52 Squamous dysplasia 6 1 7 Median age (range) 73 years (54 -91) 67 years (51 -85) 70 years Median interval index to 1 st procedure biopsy (range) 64 days (38 -443) 66 day (37 -405) 65 days
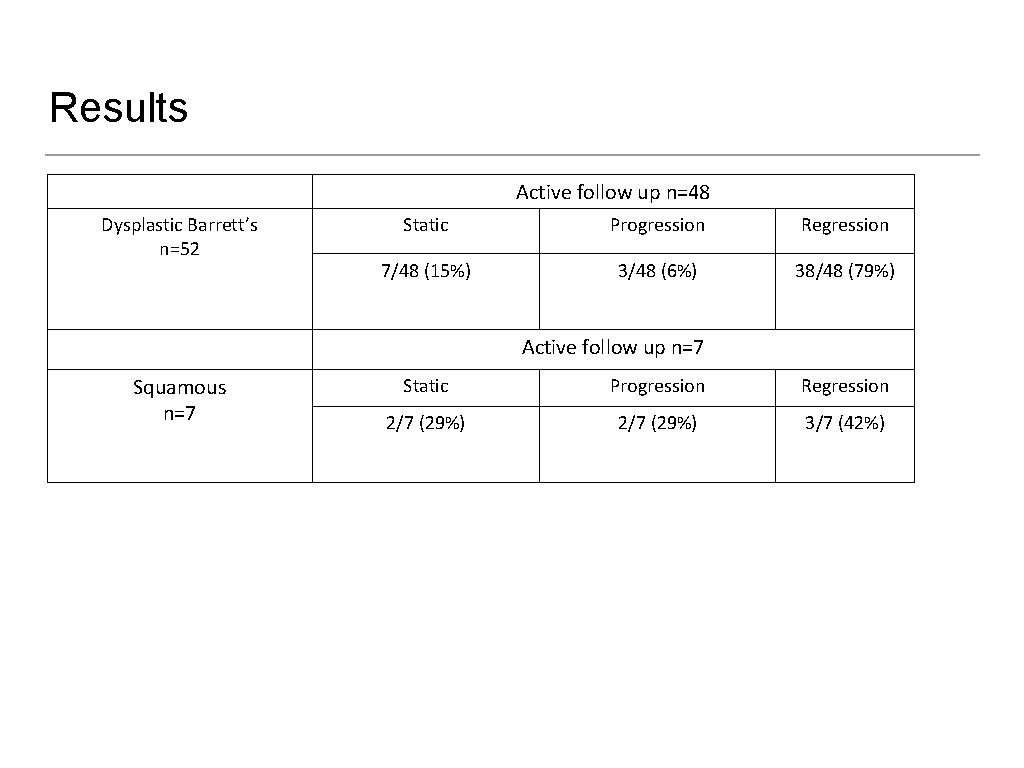
Results Active follow up n=48 Dysplastic Barrett’s n=52 Static Progression Regression 7/48 (15%) 3/48 (6%) 38/48 (79%) Active follow up n=7 Squamous n=7 Static Progression Regression 2/7 (29%) 3/7 (42%)

Conclusion • RFA is less invasive and cost effective compared to alternative treatment (surgery) and is associated with less morbidity and no mortality • RFA is effective, causing disease regression in most cases. • RFA may halt or slow progression
- Slides: 12