Radiculopathy symptoms Painnumbness in the skin innervated by
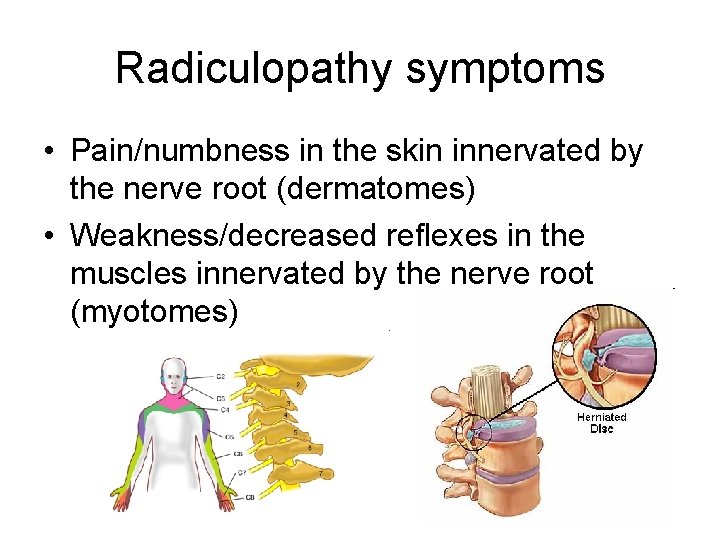
Radiculopathy symptoms • Pain/numbness in the skin innervated by the nerve root (dermatomes) • Weakness/decreased reflexes in the muscles innervated by the nerve root (myotomes)

Polyneuropathy • Mononeuropathy – Focal involovement of a single nerve, implying local pathology • Plexopathy – Damage to a nerve plexus • Radiculopathy: – Nerve root impingement or damage • Polyneuropathy – Symmetric distal sensory loss, burning or weakness
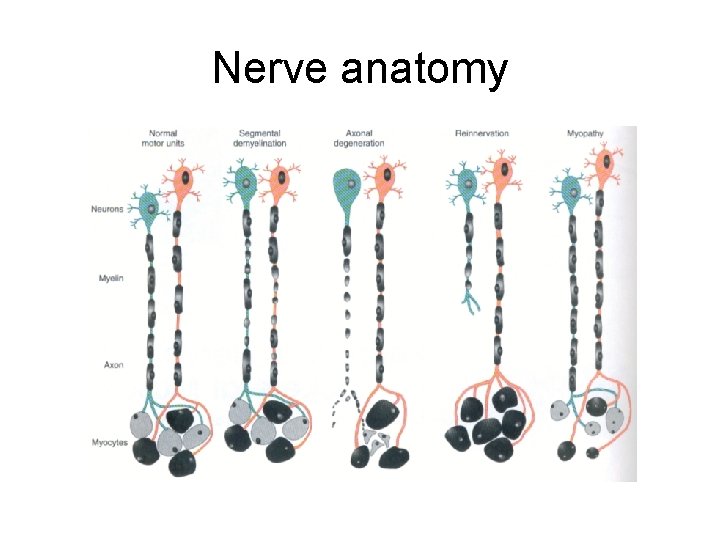
Nerve anatomy
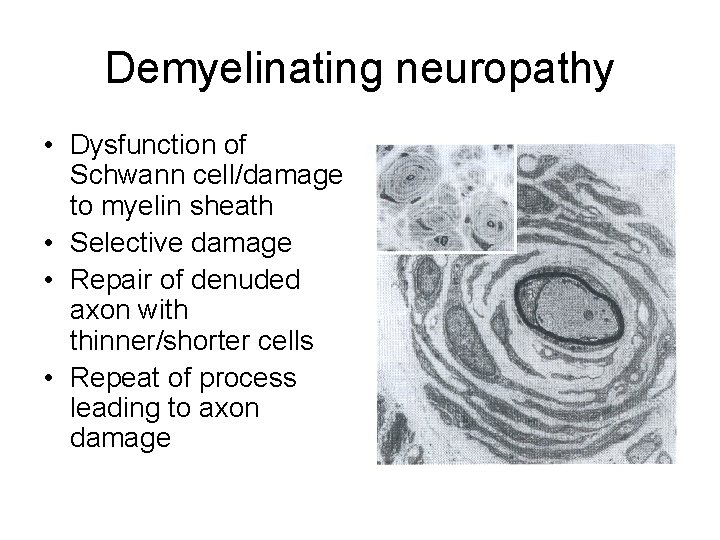
Demyelinating neuropathy • Dysfunction of Schwann cell/damage to myelin sheath • Selective damage • Repair of denuded axon with thinner/shorter cells • Repeat of process leading to axon damage

Inflammatory Causes • Acute Inflammatory Demyelinating Polyneuropathy (Guillian-Barre) – Progression of disease within 4 weeks – Starts distally, spreads proximally • Chronic Inflammatory Demyelinating Polyneuropathy – Progression of disease at or after 8 weeks – Relapsing and Remitting Course

Guillian-Barre Syndrome • Etiology: 1 to 3 cases per 100, 000 persons in the US • Pathophysiology – Antibodies attack the proteins in myelin • Clinical Course – 2/3’s with preceding viral illness followed by ascending paralysis, necessitating vent support in 30% and facial weakness in >50% – Paresthesias in hands and feet in 80% – CSF with high protein without increased WBC – Mortality is 2 -5%
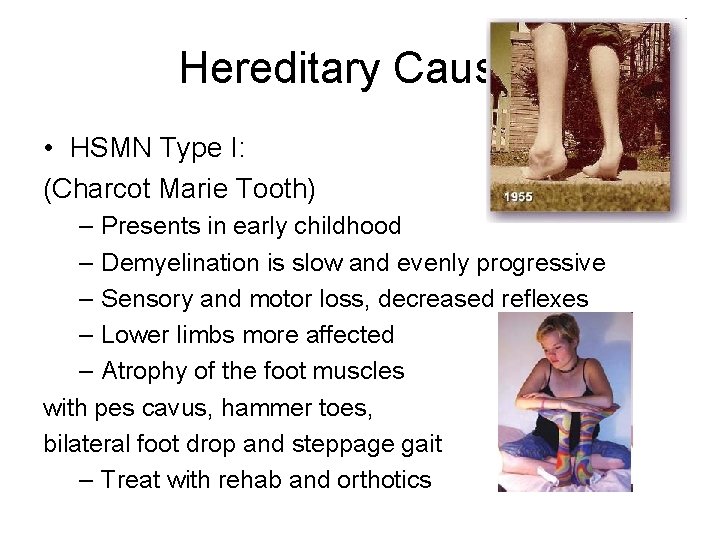
Hereditary Causes • HSMN Type I: (Charcot Marie Tooth) – Presents in early childhood – Demyelination is slow and evenly progressive – Sensory and motor loss, decreased reflexes – Lower limbs more affected – Atrophy of the foot muscles with pes cavus, hammer toes, bilateral foot drop and steppage gait – Treat with rehab and orthotics
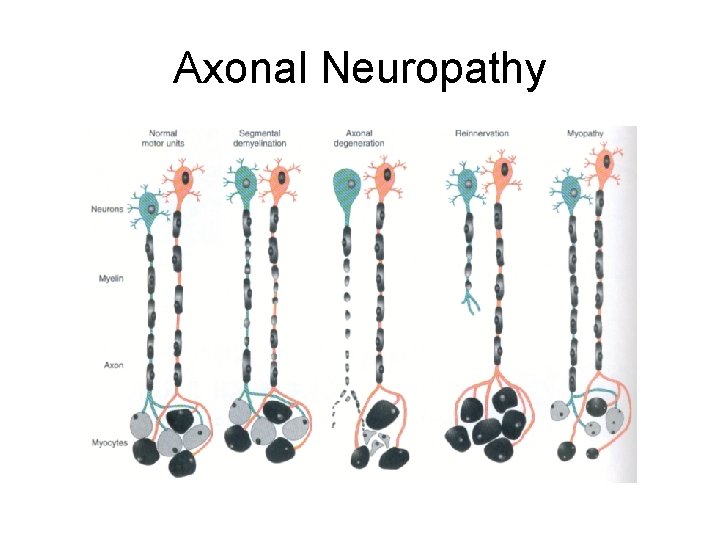
Axonal Neuropathy
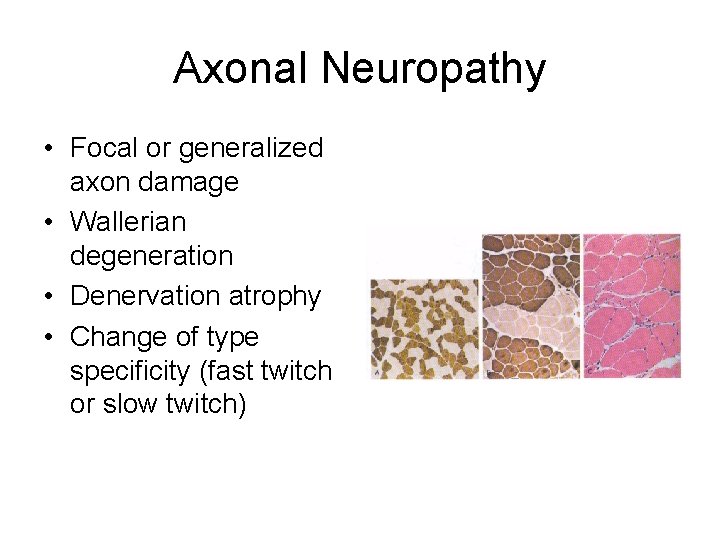
Axonal Neuropathy • Focal or generalized axon damage • Wallerian degeneration • Denervation atrophy • Change of type specificity (fast twitch or slow twitch)
Differential Diagnosis Guidelines • Metabolic/Toxic – – Diabetes Mellitus Renal failure Et. OH abuse Hypothyroidism • Infectious – HIV – Hepatitis C • Cancer – Treatment (chemo, radiation) – Tumor effects (lymphoma, leukemia) – Paraneoplastic syndromes • Critical Illness polyneuropathy • Nutrition – Vitamin B 12 deficiency – Vitamin B 6 deficiency

Diabetes Mellitus: Etiology • 50% of patients with Diabetes for 25 years have clinical signs of neuropathy • Complications: lower extremity infections, ulcerations, and subsequent amputations • Foot problems hospitalize more patients than any other diabetic complication • Cumulative risk of LE amputation in one report was 11 percent after 25 years of diagnosed diabetes

Diabetes Mellitus: Pathophysiology Vascular – The blood supply to the nerves decreases because the extra glucose attaches to the RBC’s and forms a complex that damages the blood vessels – Presence and severity of neuropathy connected to presence of cardiac risk factors such as HTN, smoking, triglycerides, BMI, and cardiovascular disease

Diabetes Mellitus: Clinical syndromes • Distal Symmetric polyneuropathy • Autonomic neuropathy – Ex postural hypotension, gastroparesis • Polyradiculopathies – Older pts with PN with weakness and atrophy in 1 or more contiguous nerve roots – Inflammatory etiology: possible vasculitis with immune complex and complement deposition • Focal Mononeuropathies – Cranial (esp III, VI, IV) – ¼-1/3 of patients will have median nerve damage

Critical Illness/ICU • Neuromuscular weakness occurs in 25% of patients vented in the ICU >7 days • Diff dx for patients with flaccid generalized weakness in the critically ill patient: – Critical Illness myopathy – Critical Illness polyneuropathy

Prognosis and Treatment • Reversible over weeks and months, occasionally permanent quadriparesis • Reduce/stop glucocorticoids or treat underlying sepsis • Aggressive medical management and avoidance of complications • Rehabilitation (ROM, prevent contractures, edema control, progressive activity)
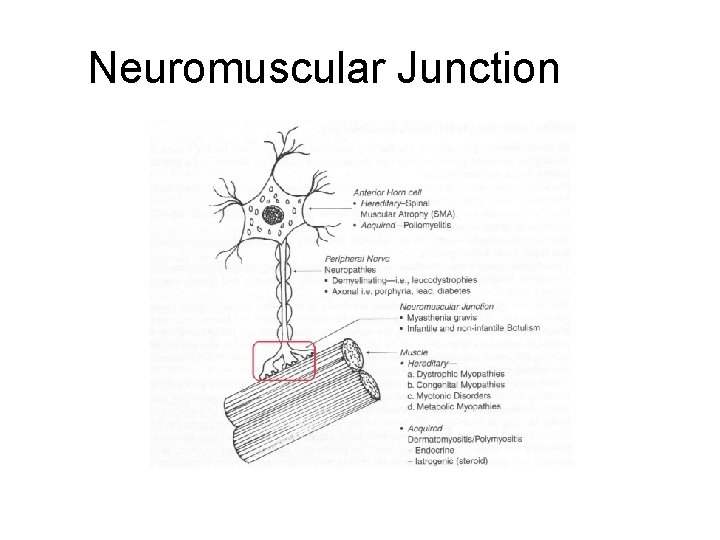
Neuromuscular Junction
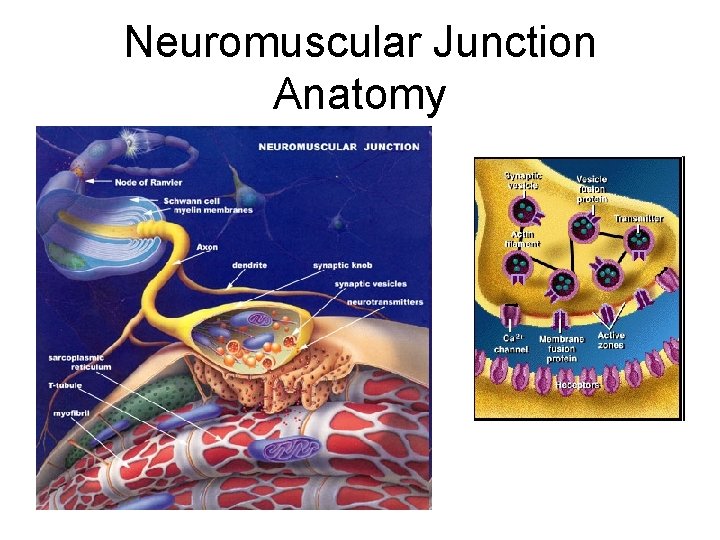
Neuromuscular Junction Anatomy

Myasthenia Gravis • Antibodies attack the acetylcholine receptors on the muscle membrane (post-synaptic) • Proximal fatigue and weakness, respiratory distress • Worse with exercise, heat, and by the end of the day, improves with rest • Facial and/or bulbar symptoms – Ptosis, diplopia, dysphagia, dysarthria • Treatment: anticholinesterase drugs (Mestinon), steroids, immunosuppression, plasmapheresis
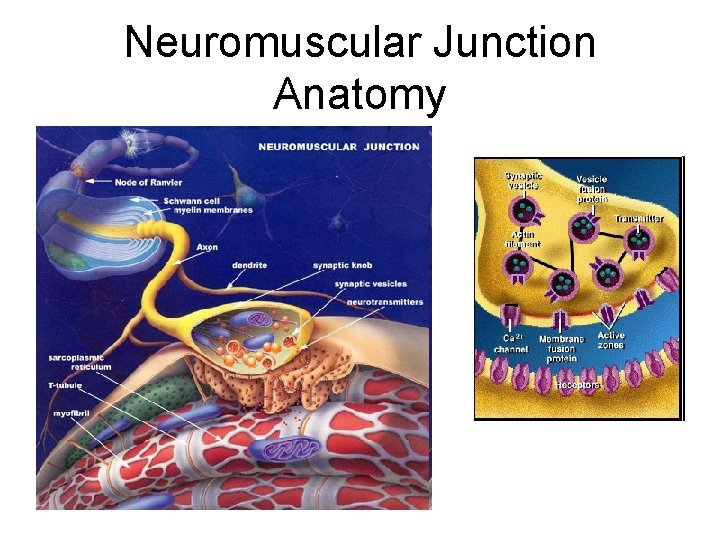
Neuromuscular Junction Anatomy

Lambert Eaton Syndrome • Autoimmune Antibodies attack the nerve terminal, decreasing calcium entry to the cell (pre-synaptic) • Associated with small cell lung cancer • Proximal fatigue and weakness, mainly in the lower limbs • Exacerbated with rest, improved with exercise • Rarely involves neck, face, and bulbar muscles • Treatment: treat cancer if present, steroids, immunosuppression, plasmapheresis
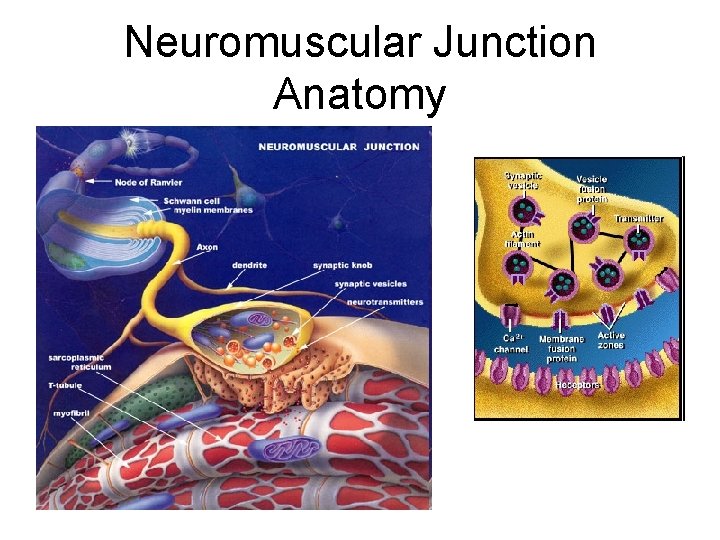
Neuromuscular Junction Anatomy

Botulism Toxin • Clostridium Botulinum toxin block release of acetylcholine from the nerve terminal (presynaptic) • Associated with contaminated raw meat, fish, canned vegetables, honey • Bulbar symptoms noted first (ptosis, dysphagia, dysarthria) • GI symptoms: diarrhea, nausea, vomiting • Widespread flaccid paralysis • Respiratory and cardiac problems • Treatment with antitoxin. The nerves have to sprout new terminal endings to reconnect to muscle fibers
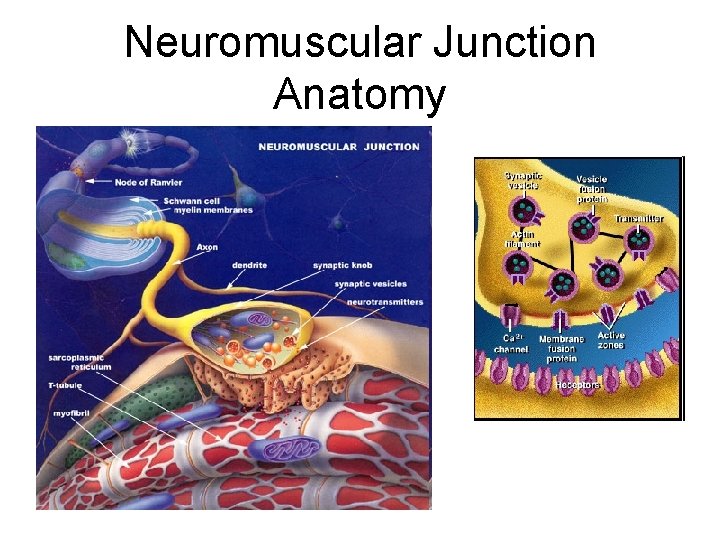
Neuromuscular Junction Anatomy
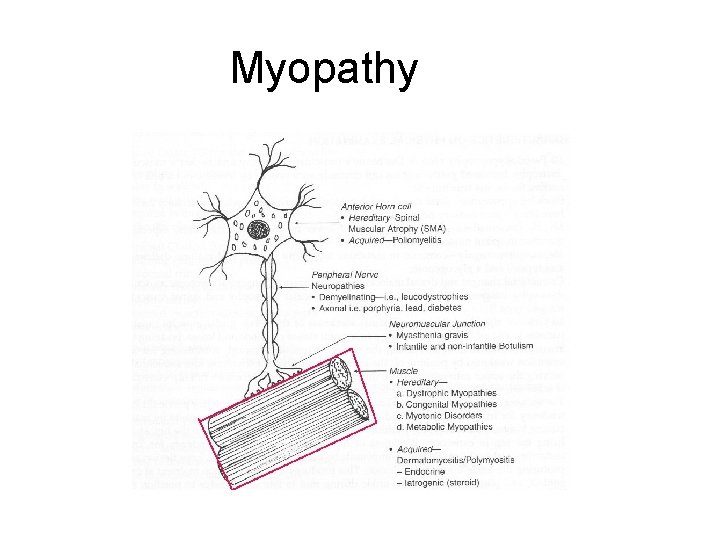
Myopathy

Types of myopathies • Dystrophic – Duchenne Muscular Dystrophy • Congenital • Metabolic • Inflammatory – Polymyositis – Dermatomyositis • Endocrine – Thyroid abnormalities – Adrenal abnormalities • Toxic – Chemotherapy – Alcohol • Medications – Statins (for cholesterol) – Steroids
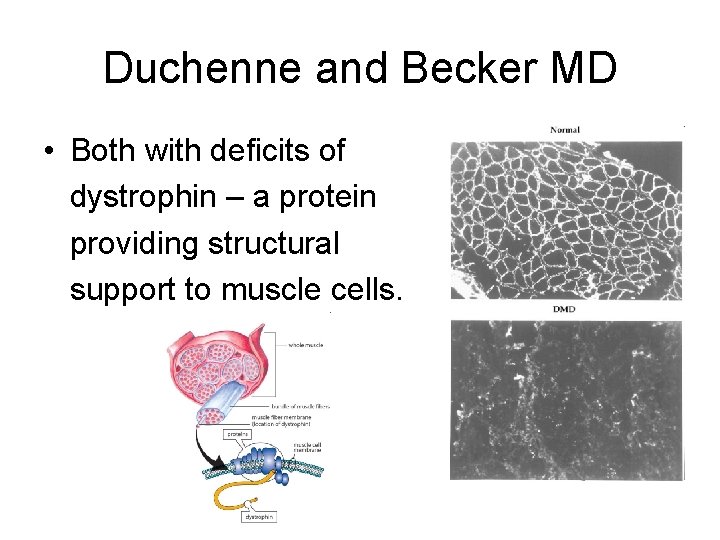
Duchenne and Becker MD • Both with deficits of dystrophin – a protein providing structural support to muscle cells.
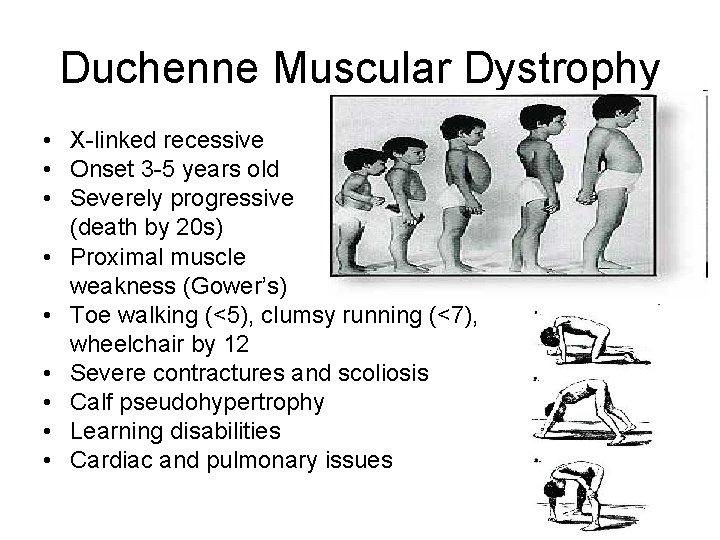
Duchenne Muscular Dystrophy • X-linked recessive • Onset 3 -5 years old • Severely progressive (death by 20 s) • Proximal muscle weakness (Gower’s) • Toe walking (<5), clumsy running (<7), wheelchair by 12 • Severe contractures and scoliosis • Calf pseudohypertrophy • Learning disabilities • Cardiac and pulmonary issues

Becker Muscular Dystrophy • • X-linked recessive Onset in adulthood Slowly progressive Proximal weakness Calf pseudohypertrophy Less learning difficulties Milder cardiac complications Rehab considerations: bracing, tendon lengthening, possible scoliosis surgery

Inflammatory myopathies: Polymyositis • Autoimmune disorder, can be associated with connective tissue disorders, infection, cancer • Symmetrical proximal weakness and atrophy (hips then shoulders) • Neck flexion weakness • Muscle pain, trouble swallowing, voice quality change • No facial or eye muscle weakness • Treatment with steroids, immunosuppression, plasmapheresis, rest
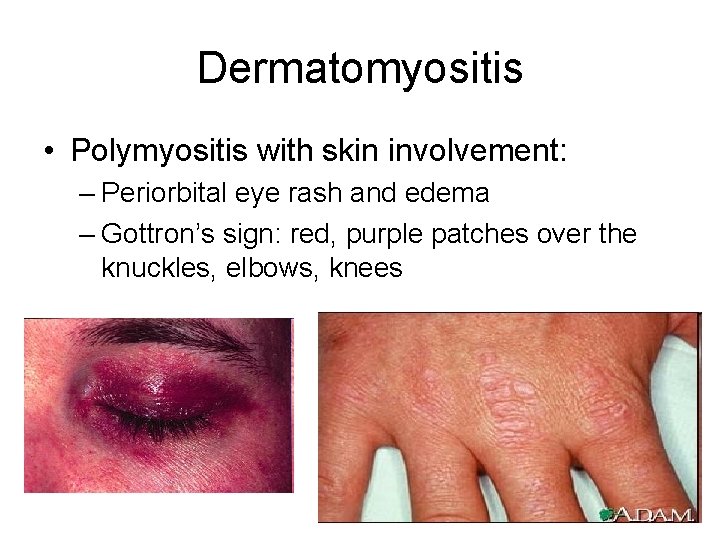
Dermatomyositis • Polymyositis with skin involvement: – Periorbital eye rash and edema – Gottron’s sign: red, purple patches over the knuckles, elbows, knees

Questions?
- Slides: 31