Radiation Safety Training for Medical Imaging Students Deputy

























































- Slides: 82

Radiation Safety Training for Medical Imaging Students Deputy Radiation Safety Officer: Michael “Ike” Hall, CHP, CSP Emory University Hospital 404 -712 -7867

Topics n n n Fundamentals of Radiation Limits and Dosimetry Biological Effects of Radiation and Pregnancy Fluoroscopy and Patient Injuries Worker Protection

What is radiation? Radiation is energy emitted from unstable atoms. Radiation can be in the form of subatomic particles (alpha or beta particles) or electromagnetic radiation (X and gamma rays). Radiation that is energetic enough to change the chemistry of a target is called ionizing radiation, and that will be the focus of this training.

Ionizing Radiation n Ion: atom with a positive or negative charge (i. e. , too few or too many electrons) Radiation that is energetic enough can strip electrons and create ions Ionization can change molecular chemistry or break apart molecules

Radiation Biology in a nutshell Ionizing radiation harms biological systems by two means: v Indirectly - Production of Free Radicals v Directly - DNA damage

Four Possible Outcomes n n Cells are undamaged by the dose Cells are damaged, repair the damage and operate normally Cells are damaged, repair the damage and operate abnormally Cells die as a result of the damage

Measuring Radiation n Exposure: measure of ionization in air (roentgen, or R) Absorbed dose: energy deposited in material per unit mass (Gray or rad) 1 Gray = 1 Joule/kg = 100 rad

Measuring Radiation n Equivalent dose: measure of the biological effect of a specific kind of radiation on humans (Sieverts or rem) For x-rays, dose and dose equivalent are equal. Dose equivalence may be different for some radioactive particles. 1 Gray = 1 Sievert = 100 rem

How much radiation is harmful? Radiogenic health effects (primarily cancer) are observed in humans only at doses in excess of 10 rem delivered at high dose rates. Below this dose, estimation of adverse health effect is speculative. “Radiation Risk in Perspective” Health Physics Society

How much radiation is in the environment? n n n People are exposed to background radiation continuously. The average dose due to background exposure is around 350 millirem per year in the United States. Background exposure can vary with altitude, soil, and medical usage.

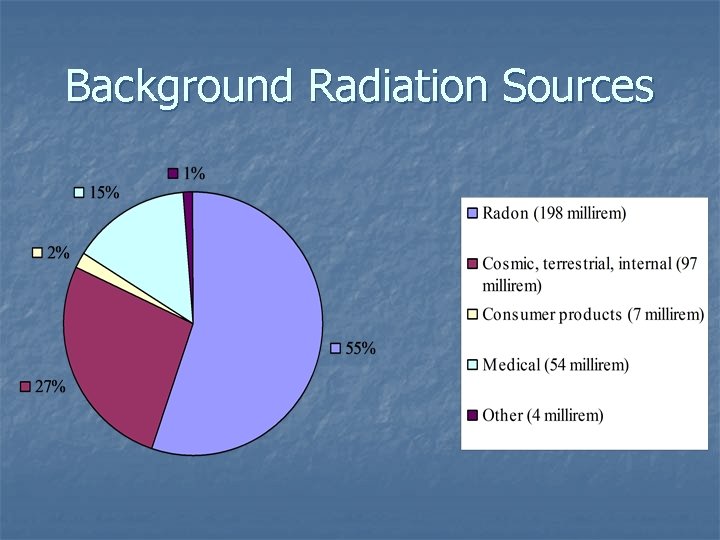
Background Radiation Sources

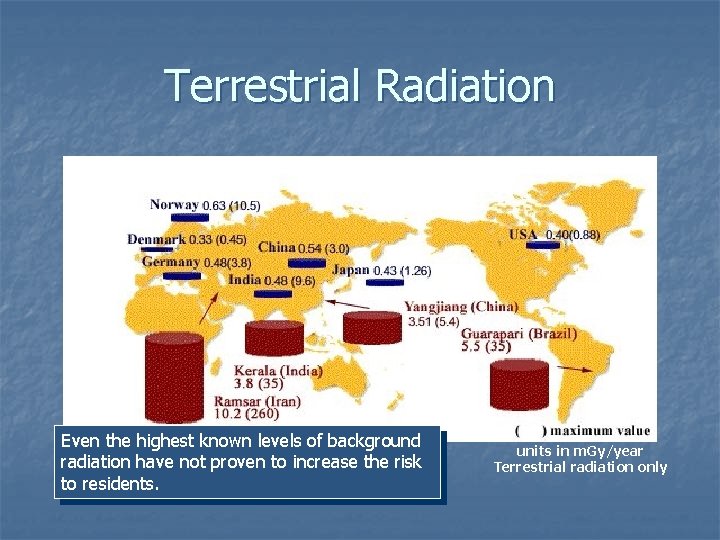
Terrestrial Radiation Even the highest known levels of background radiation have not proven to increase the risk to residents. units in m. Gy/year Terrestrial radiation only

Radiation Safety Principles The Radiation Safety program, including training, monitoring, and contamination control, is designed to ensure that no worker receives a radiation dose in excess of regulatory limits, and that each worker generally receives only as much exposure as necessary to do one's job.

Radiation Safety Principles n Time n Distance n Shielding n Containment

Time n n n Dose is directly proportional to the time spent near radiation and radioactive materials Minimize time near radiation producing machines and radioactive materials or patients whenever possible Plan work activities so as to spend less time handling radioactive material

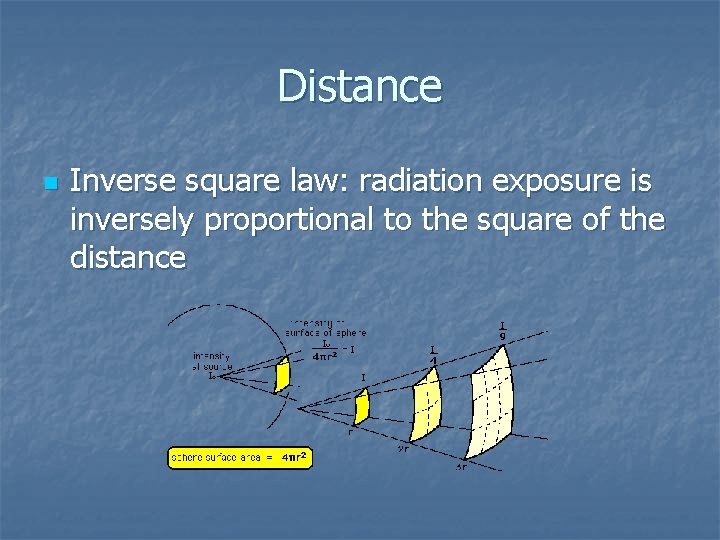
Distance n Inverse square law: radiation exposure is inversely proportional to the square of the distance

Distance n n n Maximize your distance from radiationproducing machines and radioactive materials or patients Use tongs or other tools to handle radioactive sources Move radioactive materials using a cart or portable lead “pig”

Shielding n Use the right kind of shielding for the radiation in question Beta radiation: Plexiglas n Gamma and x-ray: Lead or other high-density material n n Use sufficient shielding for the task

Shielding n n Engineering controls: leaded walls, windows, movable barriers, bricks, shipping and storage containers PPE: Lead aprons, thyroid collars, and glasses for radiation-producing equipment

Containment n n n Engineering controls: Sealed sources, syringe caps, ventilation PPE: Disposable gloves, lab coats, isolation gowns, booties, goggles, face shields, coveralls, respirators Routine contamination monitoring is essential to verify proper containment of radioactive materials

Annual Occupational Limits n 5000 mrem whole body n 15, 000 mrem to lens of eye n 50, 000 mrem to extremities n Set by federal government based on advice from scientific committees

Are these limits safe? The annual radiation limits have been established to ensure that the long-term risks of radiation exposure are minimized. There has been no evidence that occupational doses within these limits pose any risk. Due to potential uncertainties in dose measurement, the limits are set conservatively.

Other Dose Limits n n Members of public limited to 100 mrem per year from licensed activities, 500 mrem per year from exposure to Nuclear Medicine therapy patients Employees under 18 limited to 10% of permissible adult dose limit (500 mrem annually)

Declared Pregnant Workers n n 500 mrem/term limit to fetus (50 mrem/month) Limit is extremely conservative with respect to risk Contact supervisor and Radiation Safety Officer to declare pregnancy Monthly fetal badge assigned

Who gets radiation badges? Radiation badges are required for workers who are likely to receive more than 10% of the annual occupational radiation limits. In practice, almost everyone who routinely works with radioactive materials or radiation-producing machines gets one or more badges.

How do I request a badge? Ask your supervisor or the Radiation Safety Officer for a Personnel History Form. You may also find the form online. Radiation Safety Training is required to get a badge. Please ask your supervisor or the RSO. Training may be provided as an orientation packet, an inservice, or online.

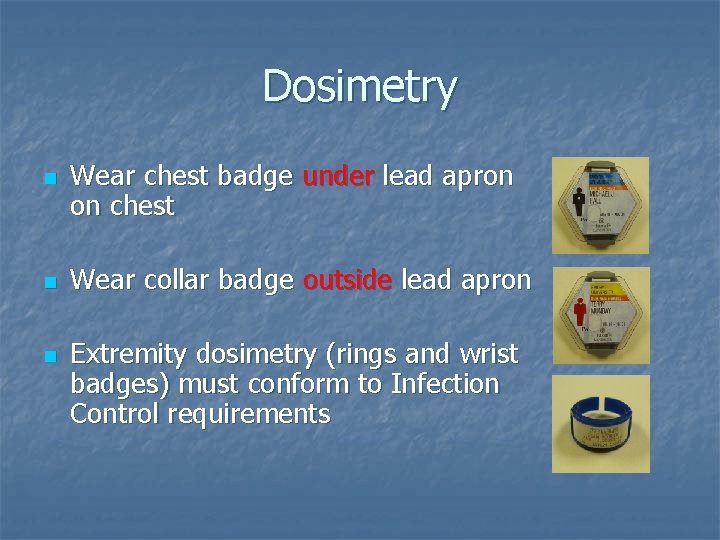
Dosimetry n n n Wear chest badge under lead apron on chest Wear collar badge outside lead apron Extremity dosimetry (rings and wrist badges) must conform to Infection Control requirements

Proper Care of Badges n n Actually take them out of the package and wear them Take care not to reverse chest and collar badges Do not leave badges on your apron or in the suite Exchange badges promptly at the beginning of each month or pay $20

How does the badge work? The Luxel dosimeter has a thin strip of specially formulated aluminum oxide (Al 2 O 3) crystalline material. Filters of various thickness simulate radiation doses to different tissues. During analysis, the strip is stimulated with laser light, causing it to luminesce in proportion to the amount of radiation exposure.

Annual Occupational Limits n 5000 mrem whole body n 15, 000 mrem to lens of eye n 50, 000 mrem to extremities n Set by federal government based on advice from scientific committees

Other Dose Limits n n Members of public limited to 100 mrem per year from licensed activities, 500 mrem per year from exposure to Nuclear Medicine therapy patients Employees under 18 limited to 10% of permissible adult dose limit (500 mrem annually)

Dosimetry Reports n n Dosimetry reports provided monthly to departmental contact Emory maintains permanent record, department maintains for 3 years Review and initial dosimetry reports Report dosimetry problems to supervisor or Radiation Safety Officer

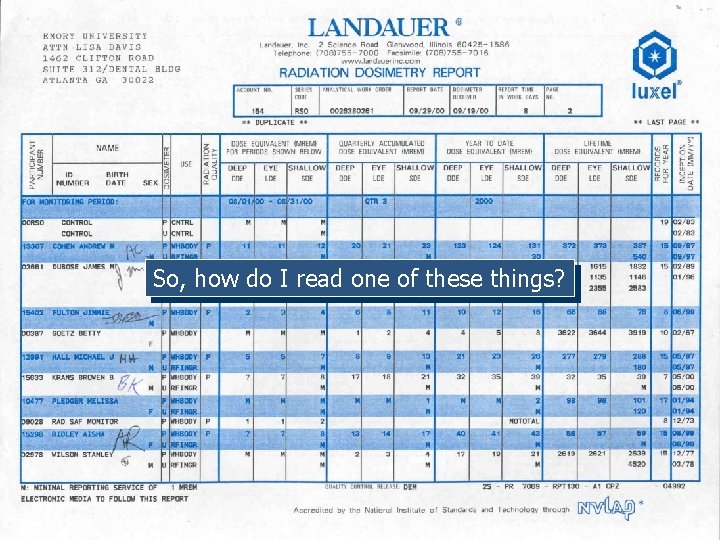
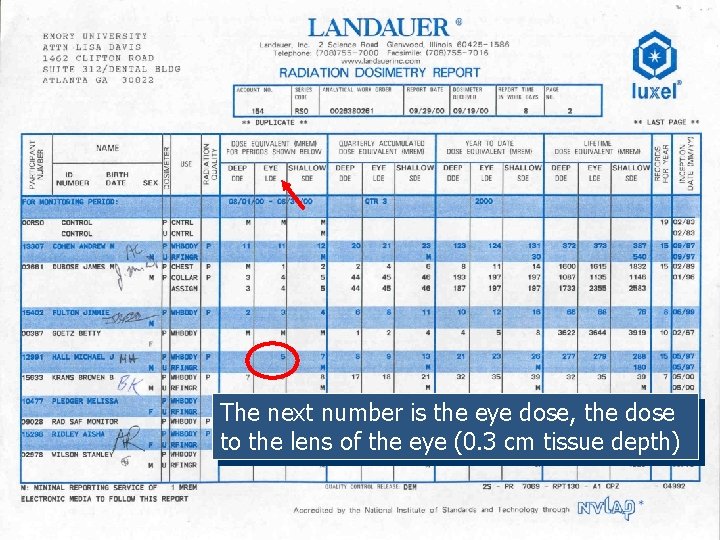
So, how do I read one of these things?

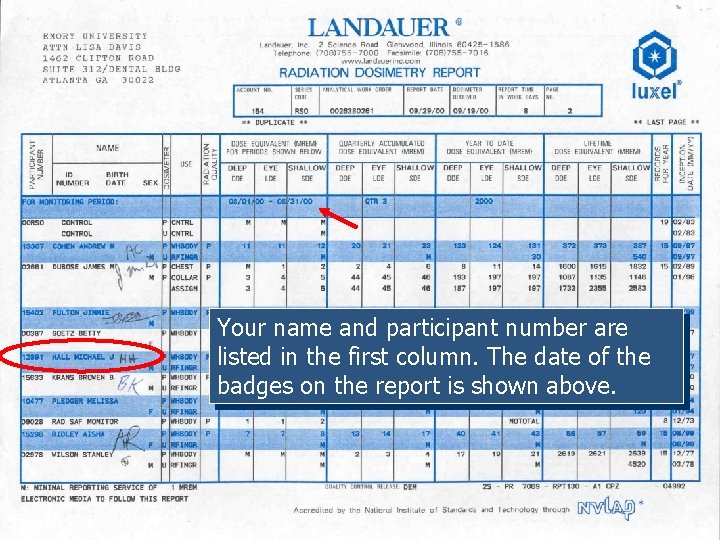
Your name and participant number are listed in the first column. The date of the badges on the report is shown above.

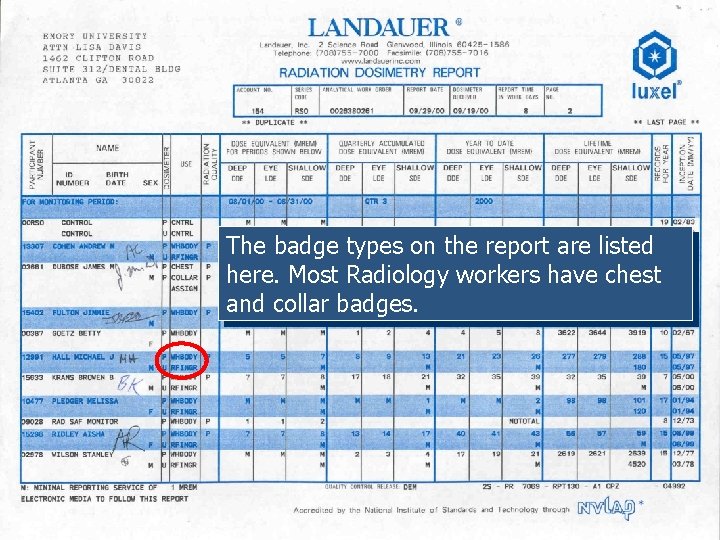
The badge types on the report are listed here. Most Radiology workers have chest and collar badges.

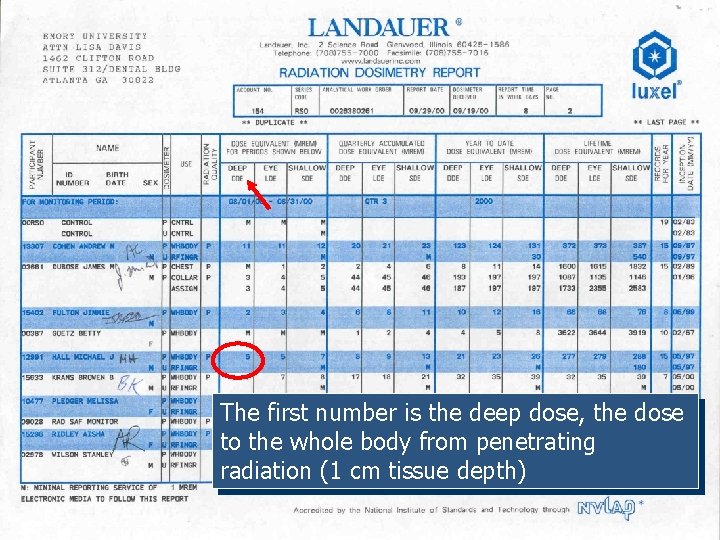
The first number is the deep dose, the dose to the whole body from penetrating radiation (1 cm tissue depth)

The next number is the eye dose, the dose to the lens of the eye (0. 3 cm tissue depth)

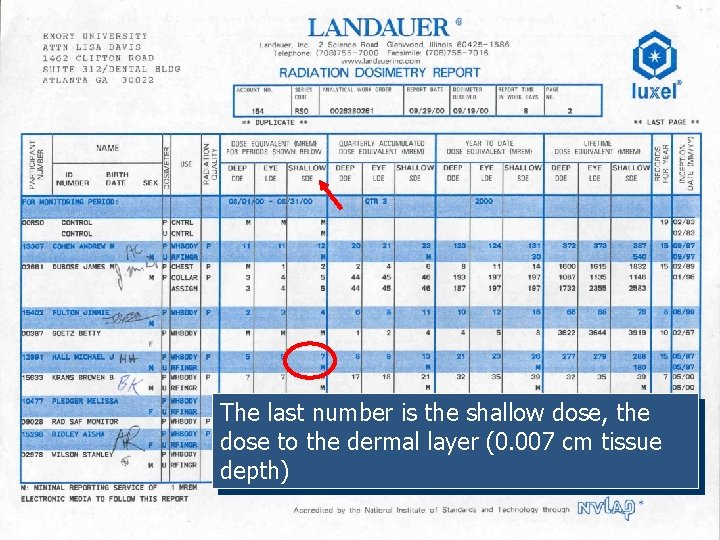
The last number is the shallow dose, the dose to the dermal layer (0. 007 cm tissue depth)

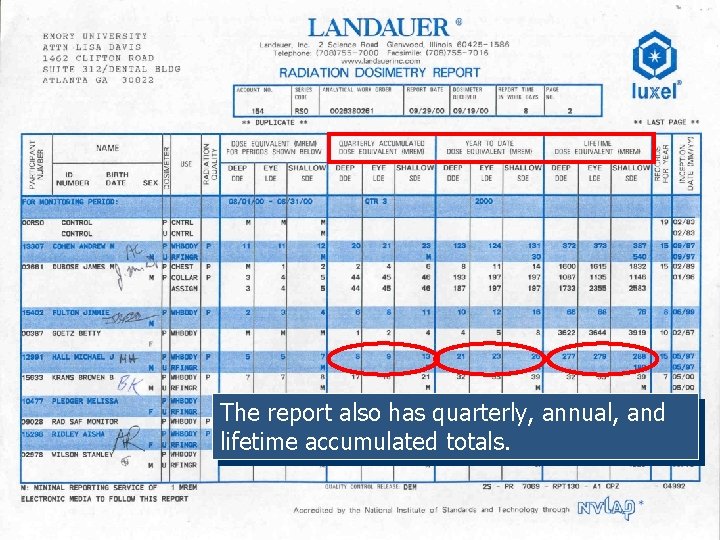
The report also has quarterly, annual, and lifetime accumulated totals.

Dose Determination n For workers with chest and collar badges, assigned dose is a combination of readings: Whole body dose from a combination of chest and collar badges n Eye dose from lens-equivalent area of collar badge n Shallow dose from skin-equivalent area of collar badge n

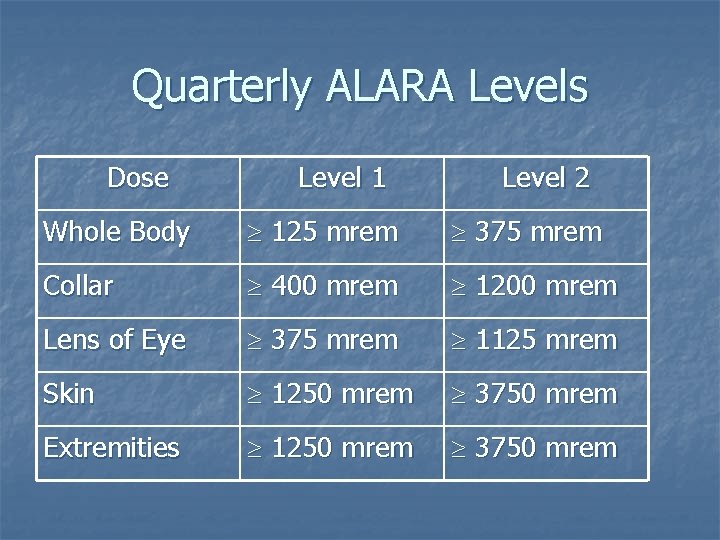
Quarterly ALARA Reports n n n Workers exceeding the doses on the following table are added to the ALARA report ALARA Level 2 doses are investigated by the Radiation Safety Officer Work activity may be restricted if corrective actions not taken

Quarterly ALARA Levels Dose Level 1 Level 2 Whole Body 125 mrem 375 mrem Collar 400 mrem 1200 mrem Lens of Eye 375 mrem 1125 mrem Skin 1250 mrem 3750 mrem Extremities 1250 mrem 3750 mrem

What are the effects of high doses of radiation? n Acute radiation exposure, however rare, may result in severe clinical effects or even death: n n Exposures of minutes to hours while handling highly radioactive sources Laboratory and manufacturing accidents Intentional and accidental high medical doses Radiation controls are in place to ensure that these kinds of exposures do not happen!

Category of Effects n Deterministic effects occur with acute doses and result from cell death n n Characterized by threshold dose (below a given dose, no effect) Stochastic effects may occur at chronic doses n n Affects the probability of all-or-none phenomena such as carcinogenesis Ill-defined threshold dose

Acute Radiation Syndrome n n Follows a predictable course over a period of time Characterized by the development of signs and symptoms Onset time of symptoms indicates dose Severity of effect increases as dose increases

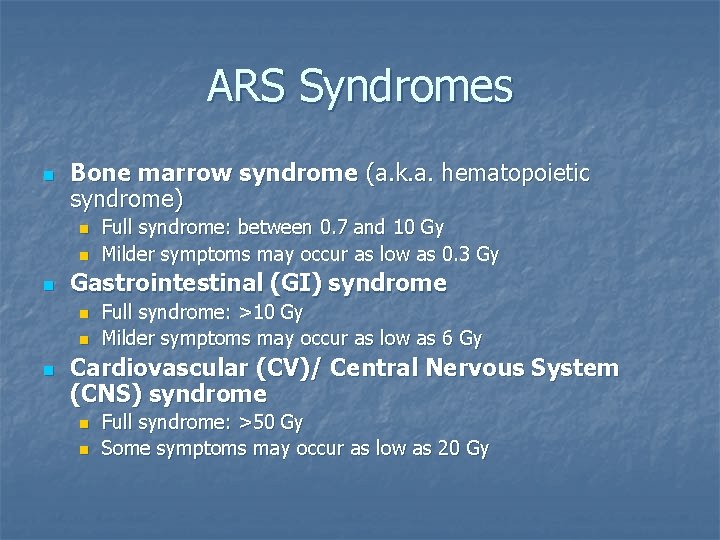
ARS Syndromes n Bone marrow syndrome (a. k. a. hematopoietic syndrome) n n n Gastrointestinal (GI) syndrome n n n Full syndrome: between 0. 7 and 10 Gy Milder symptoms may occur as low as 0. 3 Gy Full syndrome: >10 Gy Milder symptoms may occur as low as 6 Gy Cardiovascular (CV)/ Central Nervous System (CNS) syndrome n n Full syndrome: >50 Gy Some symptoms may occur as low as 20 Gy

Bone marrow syndrome n n n The survival rate of patients decreases with increasing dose Characterized by damage to cells that divide at the most rapid pace (such as bone marrow, the spleen and lymphatic tissue) The primary cause of death is the destruction of the bone marrow, resulting in infection and hemorrhage

Gastrointestinal (GI) syndrome n n n Survival is extremely unlikely with this syndrome Destructive and irreparable changes in the GI tract and bone marrow usually cause infection, dehydration, and electrolyte imbalance Death usually occurs within 2 weeks

Cardiovascular (CV) / Central Nervous System (CNS) syndrome n n Death typically occurs within 3 days Death likely is due to collapse of the circulatory system as well as increased pressure in the confining cranial vault as the result of increased fluid content caused by edema, vasculitis, and meningitis.

Four Stages of ARS n n Prodromal stage (N-V-D stage): Classic symptoms are nausea, vomiting, as well as anorexia and possibly diarrhea, which occur from minutes to days following exposure. The symptoms may last (episodically) for minutes up to several days. Latent stage: Patient looks and feels generally healthy for a few hours or even up to a few weeks.

Four Stages of ARS n n Manifest illness stage: Symptoms depend on the specific syndrome and last from hours up to several months. Recovery or death: Most patients who do not recover will die within several months of exposure. The recovery process lasts from several weeks up to two years.

Effects on Embryo / Fetus n n High acute doses may cause death or abnormalities Large doses between 4 – 11 weeks can cause severe abnormalities Doses as low as 25 rad may cause defects Doses less than 10 rad generally considered not to increase risk

Patients and Pregnancy n n Mandatory patient pregnancy testing for high dose procedures Screening permitted for low dose diagnostic procedures Report cases of fetal exposure to supervisor and Radiation Safety Officer IMMEDIATELY RSO will determine fetal dose and report to patient’s physician

Cutaneous Radiation Syndrome (CRS) n n Recently introduced to describe the complex pathological syndrome that results from acute radiation exposure to the skin. It is possible to receive a damaging dose to the skin without symptoms of ARS, especially with acute exposures to beta radiation or X-rays.

Cutaneous Radiation Syndrome (CRS) n n Cause of syndrome is radiation damage to basal cell layer of the skin Characterized by inflammation, erythema, epilation, and/or dry or moist desquamation Within a few hours after irradiation, a transient and inconsistent erythema (associated with itching) can occur A latent phase may occur and last from a few days up to several weeks, when intense reddening, blistering, and ulceration of the irradiated site are visible

Cutaneous Radiation Syndrome (CRS) n In most cases, healing occurs by regenerative means; however, very large skin doses can cause permanent hair loss, damaged sebaceous and sweat glands, atrophy, fibrosis, decreased or increased skin pigmentation, and ulceration or necrosis of the exposed tissue.

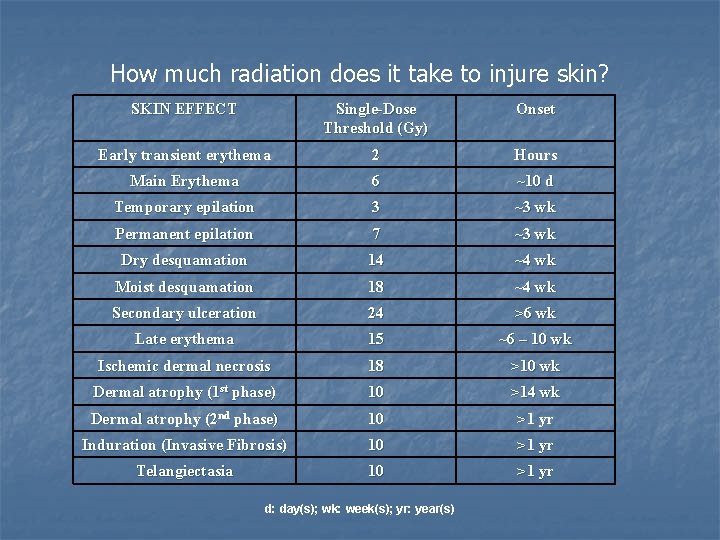
How much radiation does it take to injure skin? SKIN EFFECT Single-Dose Threshold (Gy) Onset Early transient erythema 2 Hours Main Erythema 6 ~10 d Temporary epilation 3 ~3 wk Permanent epilation 7 ~3 wk Dry desquamation 14 ~4 wk Moist desquamation 18 ~4 wk Secondary ulceration 24 >6 wk Late erythema 15 ~6 – 10 wk Ischemic dermal necrosis 18 >10 wk Dermal atrophy (1 st phase) 10 >14 wk Dermal atrophy (2 nd phase) 10 >1 yr Induration (Invasive Fibrosis) 10 >1 yr Telangiectasia 10 >1 yr d: day(s); wk: week(s); yr: year(s)

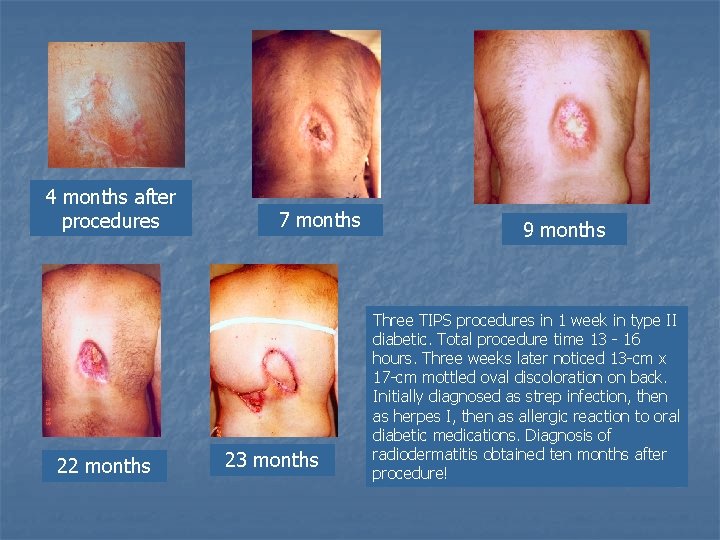
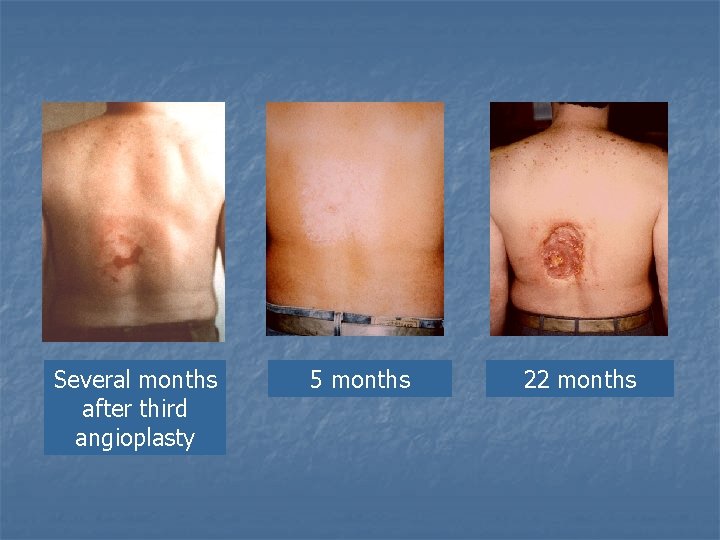
4 months after procedures 22 months 7 months 23 months 9 months Three TIPS procedures in 1 week in type II diabetic. Total procedure time 13 - 16 hours. Three weeks later noticed 13 -cm x 17 -cm mottled oval discoloration on back. Initially diagnosed as strep infection, then as herpes I, then as allergic reaction to oral diabetic medications. Diagnosis of radiodermatitis obtained ten months after procedure!

Several months after third angioplasty 5 months 22 months

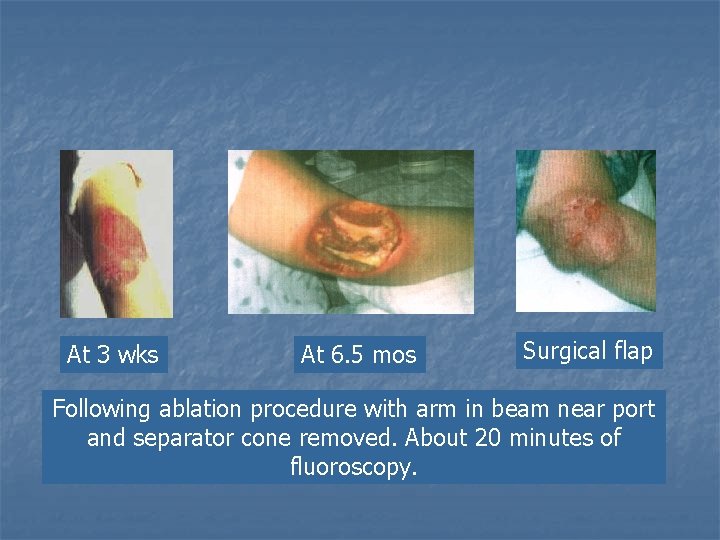
At 3 wks At 6. 5 mos Surgical flap Following ablation procedure with arm in beam near port and separator cone removed. About 20 minutes of fluoroscopy.

Stochastic Effects n n The effects of low levels of radiation are more difficult to determine because the deterministic effects described above do not occur at these levels. Studies of people who have received high doses have shown a link between radiation dose and some delayed, or latent effects, including some forms of cancer and genetic effects.

Stochastic Effects n To estimate the risks associated with low or chronic exposure, we create a model of the risk of occurrence of cancer at high doses to the risk of cancer at low doses, usually assuming no threshold. This type of risk model is called stochastic. The risk of a clinical effect increases with the dose, but the effect is the same.

Stochastic Effects n n This scaling or extrapolation is generally considered to be a conservative approach (may over-estimate the risk) to estimating low-dose risks. The risk of certain effects, including cancer, may be cumulative in patients with repeated examinations and higher in younger patients.

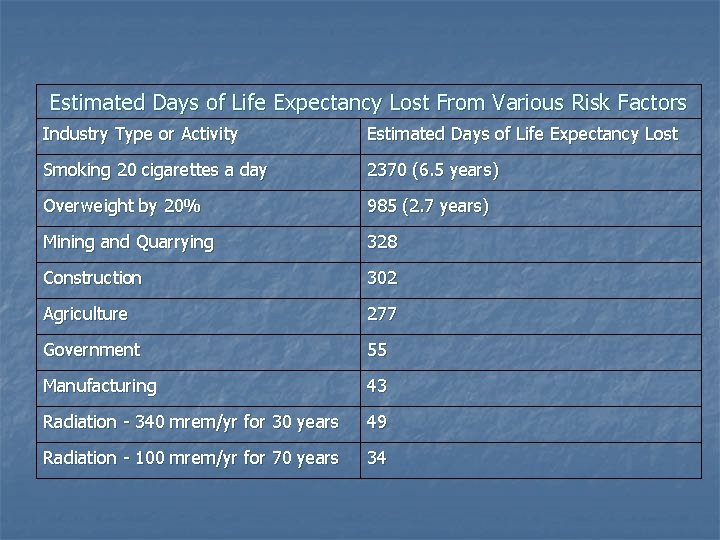
Estimated Days of Life Expectancy Lost From Various Risk Factors Industry Type or Activity Estimated Days of Life Expectancy Lost Smoking 20 cigarettes a day 2370 (6. 5 years) Overweight by 20% 985 (2. 7 years) Mining and Quarrying 328 Construction 302 Agriculture 277 Government 55 Manufacturing 43 Radiation - 340 mrem/yr for 30 years 49 Radiation - 100 mrem/yr for 70 years 34

Ionizing Radiation at EUH n n Radiography Fluoroscopy Computed Tomography (CT) Nuclear Medicine n n Diagnostic Therapeutic Radiation Oncology Blood Irradiation

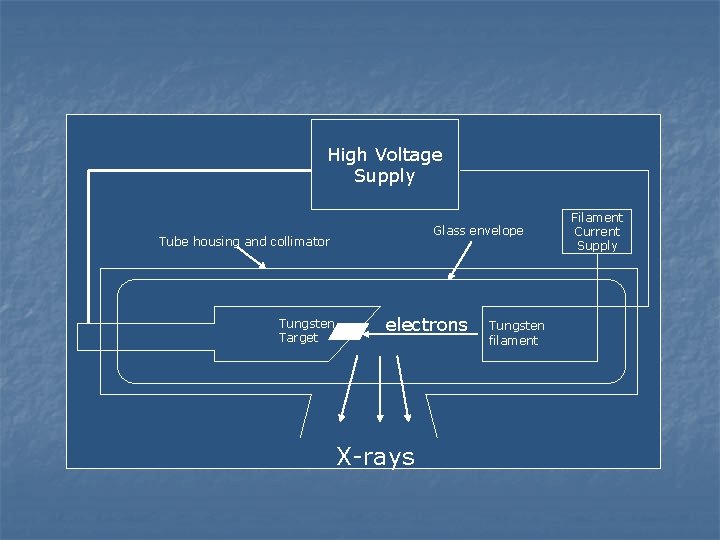
How are X-rays produced? n n n Electrons are fired at a target made of a heavy material, like tungsten The electrons are slowed down by the nuclei of the tungsten atoms Some of the electron energy is converted to electromagnetic radiation (x-rays)

High Voltage Supply Glass envelope Tube housing and collimator Tungsten Target electrons X-rays Tungsten filament Filament Current Supply

Diagnostic X-ray Techniques n Radiographs n Fluoroscopy n Computed Tomography (CT)

How do I reduce my exposure? Observe the following precautions: n n n Maximize your distance from radiation producing machines whenever practical Do not be in the suite longer than necessary Utilize available shielding

Use Available Shielding Leaded Goggles, if necessary Thyroid Shield Badges Lead vest & apron Wear dosimetry!

Use Available Shielding n n n Adjustable head/neck shields RADPAD patient drapes Leaded acrylic barriers and windows

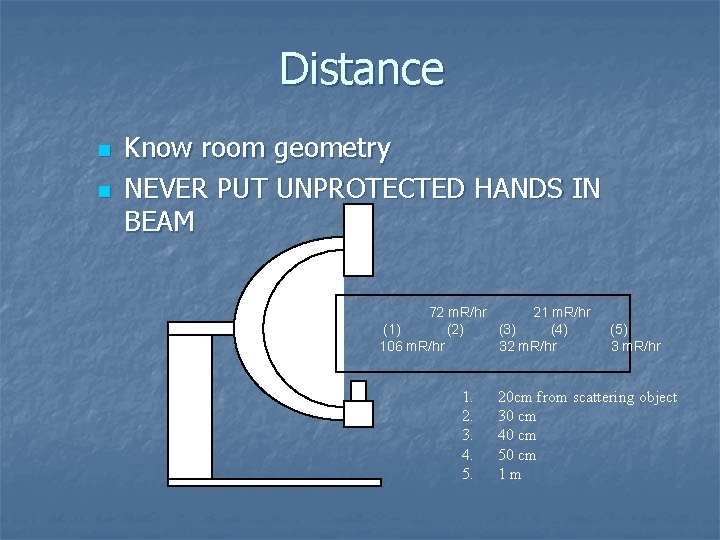
Distance n n Know room geometry NEVER PUT UNPROTECTED HANDS IN BEAM 72 m. R/hr 21 m. R/hr (1) (2) (3) (4) (5) 106 m. R/hr 32 m. R/hr 3 m. R/hr 1. 2. 3. 4. 5. 20 cm from scattering object 30 cm 40 cm 50 cm 1 m

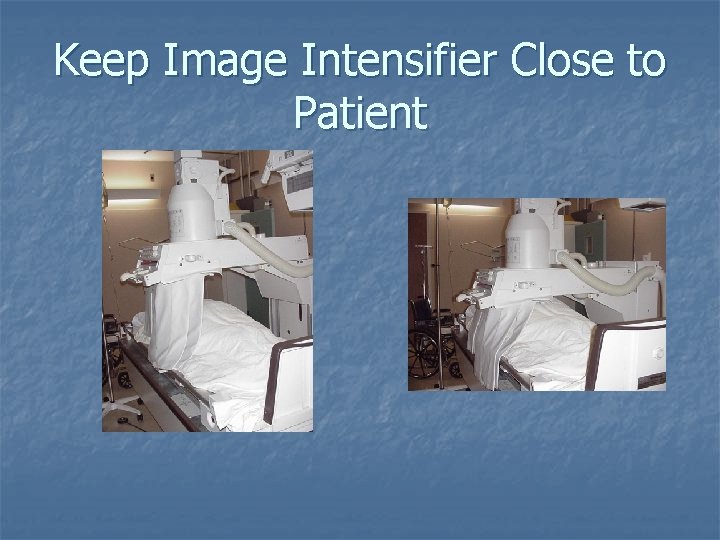
Keep Image Intensifier Close to Patient

Collimate to the Area of Interest Don’t catch the edge of the patient.

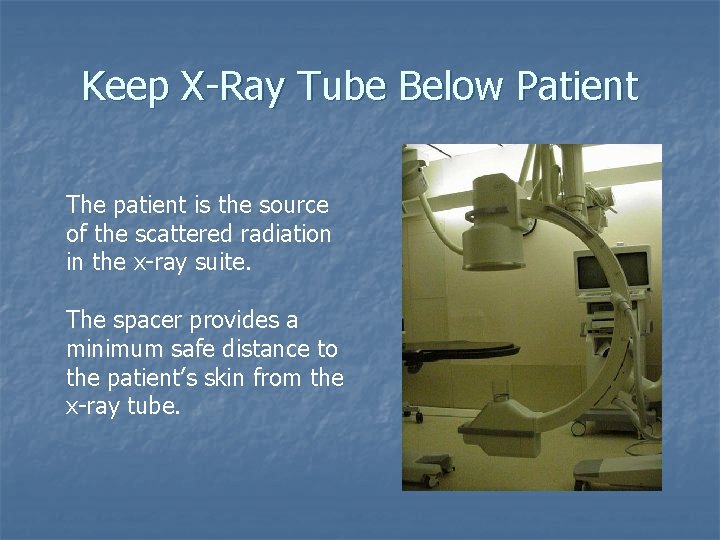
Keep X-Ray Tube Below Patient The patient is the source of the scattered radiation in the x-ray suite. The spacer provides a minimum safe distance to the patient’s skin from the x-ray tube.

Reduce Magnification when possible

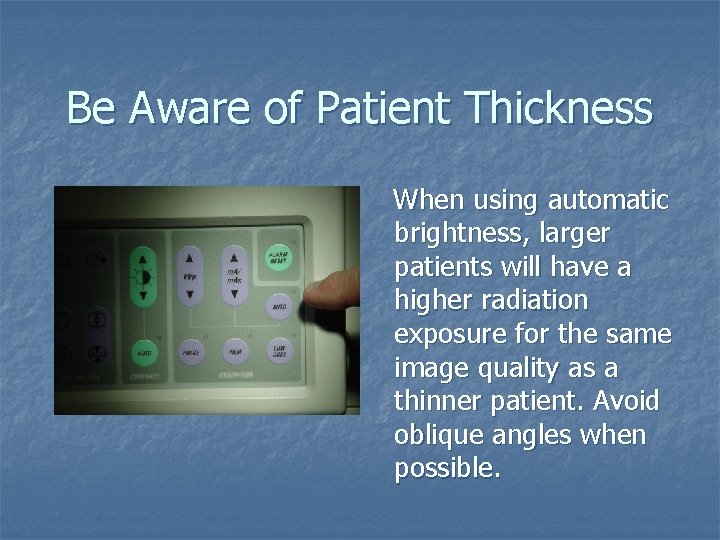
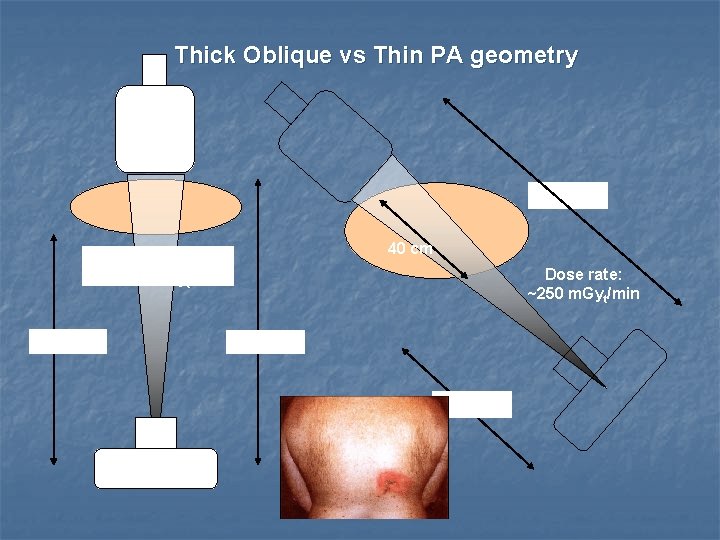
Be Aware of Patient Thickness When using automatic brightness, larger patients will have a higher radiation exposure for the same image quality as a thinner patient. Avoid oblique angles when possible.

Thick Oblique vs Thin PA geometry 100 cm 40 cm Dose rate: 20 – 40 m. Gyt/min 80 cm Dose rate: ~250 m. Gyt/min 100 cm 50 cm

Operator’s Responsibilities n n n Notifying the RSO when there is a new machine or any change in setup Keeping exposures to himself & staff ALARA Clearing the area of all nonessential personnel

Operator’s Responsibilities n n n Observing any restrictions Using minimum exposure factors Notifying your supervisor and the RSO immediately of any accidental exposure to radiation

FDA Recommendations n n n Establish standard procedures and protocols Determine dose rates for specific systems Assess each protocol for the potential for radiation injury to the patient Modify protocols to minimize cumulative absorbed dose to any skin area Appropriate training for all operators

After the Procedure n n n Record fluoro time and projection in patient chart, especially for interventional procedures with more than 30 minutes of beam-on time Indicate in which room procedure occurred Record any additional information on radiation output