RABIES PREVENTION AND CONTROL IN SIMCOE MUSKOKA Charles

RABIES PREVENTION AND CONTROL IN SIMCOE MUSKOKA Charles Gardner, MD, CCFP, MHSc, FRCPC June 4 th, 2015 Collingwood General and Marine Hospital

ACKNOWLEDGEMENTS Dr. Dean Middleton Veterinarian and Senior Public Health Epidemiologist, Enteric, Zoonotic and Vector-Borne Diseases Unit, Public Health Ontario Dr. Catherine Filejski Public Health Veterinarian Enteric and Zoonotic Diseases Unit Ontario Ministry of Health and Long Term Care

CLINICAL SCENARIOS • Case 1: Facial Bite by Dog in Guatemala § Dog unavailable § Dog known to be vaccinated § Victim previously immunized 5 years ago • Case 2: Bat Found in Bedroom § Husband awoke to something touching him, he grabbed bat and threw it across room § Wife reports not being touched by bat § Bat killed… awaiting testing for rabies
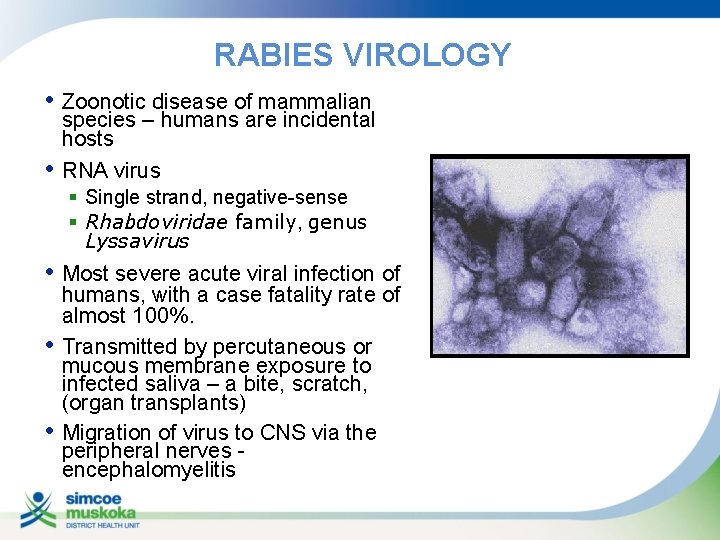
RABIES VIROLOGY • Zoonotic disease of mammalian • species – humans are incidental hosts RNA virus § Single strand, negative-sense § Rhabdoviridae family, genus Lyssavirus • Most severe acute viral infection of • • humans, with a case fatality rate of almost 100%. Transmitted by percutaneous or mucous membrane exposure to infected saliva – a bite, scratch, (organ transplants) Migration of virus to CNS via the peripheral nerves encephalomyelitis

RABIES TRANSMISSION CHARACTERISTICS • Likelihood of transmission post bite of a rabid animal is 15% (up to 60% with deep wounds) without rabies post exposure prophylaxis • Completely prevented with timely vaccination – pre or post exposure § failure rates (with a delay or breach in protocol) range from 1 in 80, 000 in developed countries to 1 in 12, 000 in developing countries • Incubation period 3 to 8 weeks after exposure – can range from a few days to several years § Depends on wound severity, innervation of location, distance from CNS • Period of communicability § Only known reliably for dogs, cats, ferrets • 3 -7 days before onset of clinical signs § Longer in other species (skunks, bats)

INTERNATIONAL AND HISTORICAL EPIDEMIOLOGY • History of significant burden of illness in humans in western society § 100 human cases per year in the USA, early 1900’s • Control measures succeeding in Ontario / Canada • human cases of canine rabies in Canada and the United States dramatically declined in the 1950 s with dog vaccination § bat-variant virus recently has become the dominant cause of rabies in humans • Continued heavy disease burden in developing countries § 55, 000 human cases / year globally § Would be much greater (est. of 327, 000 annually) without postexposure prophylactic vaccination – 15 million prophylaxed annually § WHO reports more deaths than from dengue fever, polio, meningococcal meningitis or Japanese encephalitis.

HUMAN CASES IN CANADA / ONTARIO • In Canada, 9 human cases occurred between 1960 and 2009 (NACI, 2012). • In Ontario, 1 human case occurred in 2012 that was acquired while travelling outside of Canada • The last case of human rabies that was acquired in Ontario occurred in 1967. • Historically, skunks, foxes and raccoons are the main reservoirs in Ontario. Arrival from northern Ontario in the 1950’s • In Ontario, bats currently pose the biggest threat of transmitting the virus to humans. • Dog exposures are the greatest risk for returning travelers – other mammalian species also a risk Source: Based on PHO Grand Rounds , Tuesday April 21, 2015
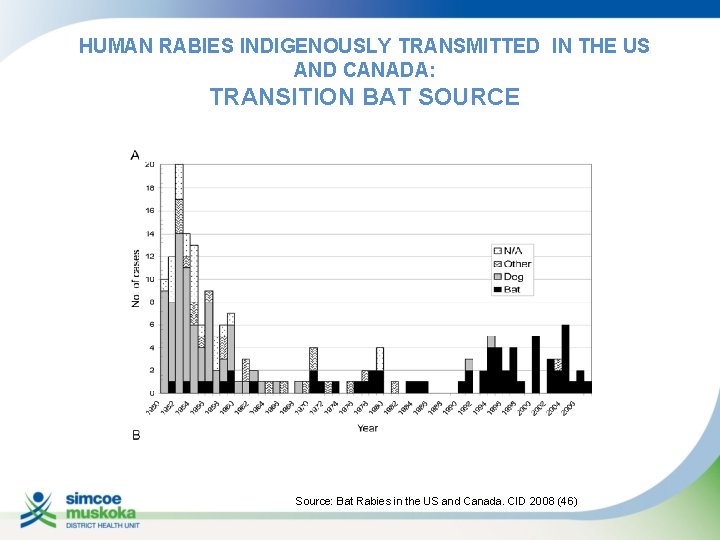
HUMAN RABIES INDIGENOUSLY TRANSMITTED IN THE US AND CANADA: TRANSITION BAT SOURCE Source: Bat Rabies in the US and Canada. CID 2008 (46)
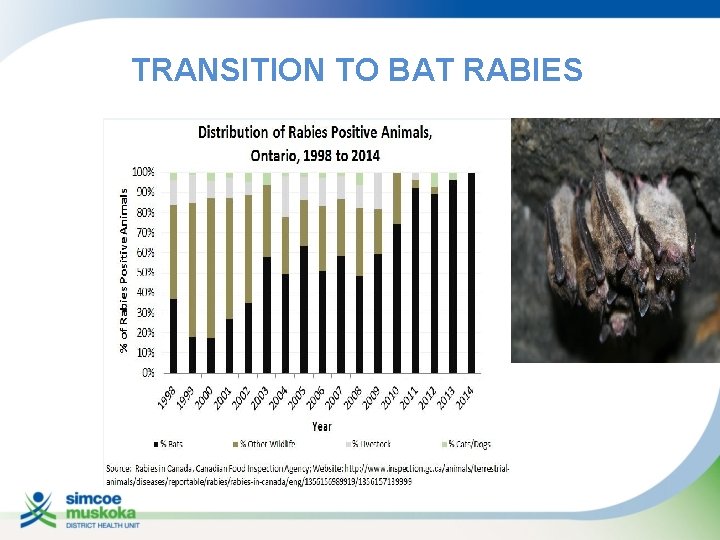
TRANSITION TO BAT RABIES

RABIES CONTROL STRATEGIES In Ontario, four main strategies have been used to prevent rabies cases in humans: 1. Public Health messaging informing people to avoid contact with wild animals. 2. Wildlife rabies control programs targeting skunks, raccoons and foxes. (note: no program for bat rabies) 3. Vaccinating bridge vectors such as dogs, cats, other pets, and farm animals. 4. Human Rabies Post-Exposure Prophylaxis (RPEP), and Pre. Exposure Prophylaxis Source: PHO Grand Rounds , Tuesday April 21, 2015

MANY PARTNERS TO CONTROL RABIES Hospitals/ ER Rooms Primary Care Providers Other Health Units Police Animal Control SMDHU MOHLTC Municipalities PHO Humane Society OAVT OMAFRA Veterinarians CFIA MNR
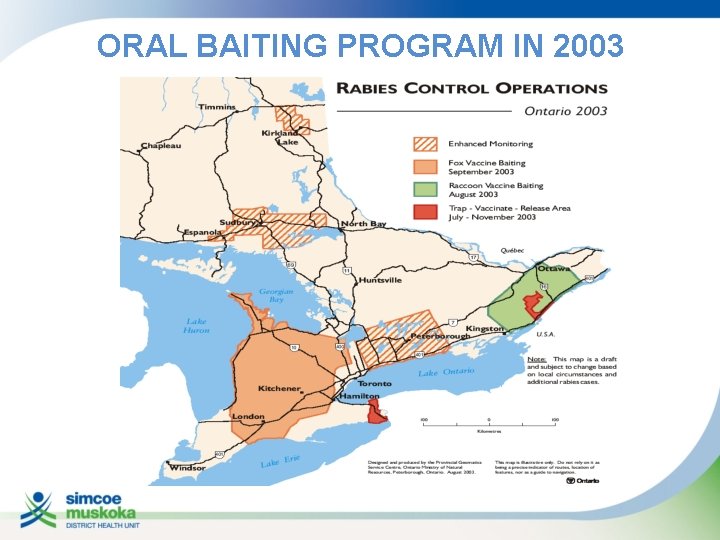
ORAL BAITING PROGRAM IN 2003
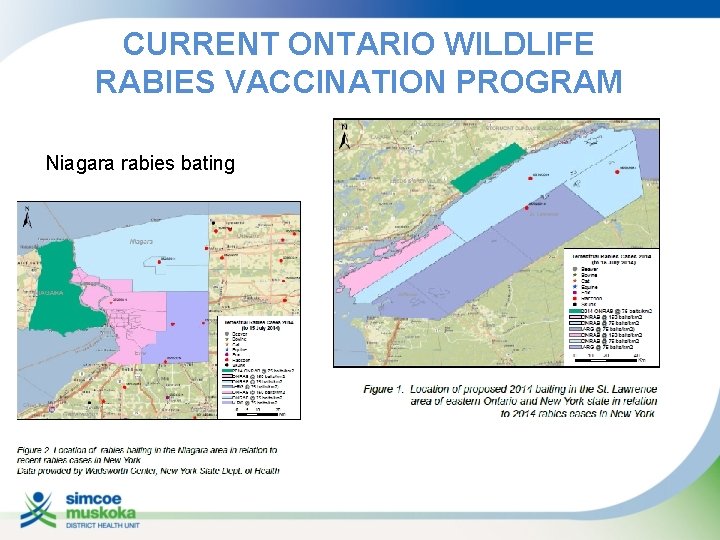
CURRENT ONTARIO WILDLIFE RABIES VACCINATION PROGRAM Niagara rabies bating St. Lawrence River rabies bating
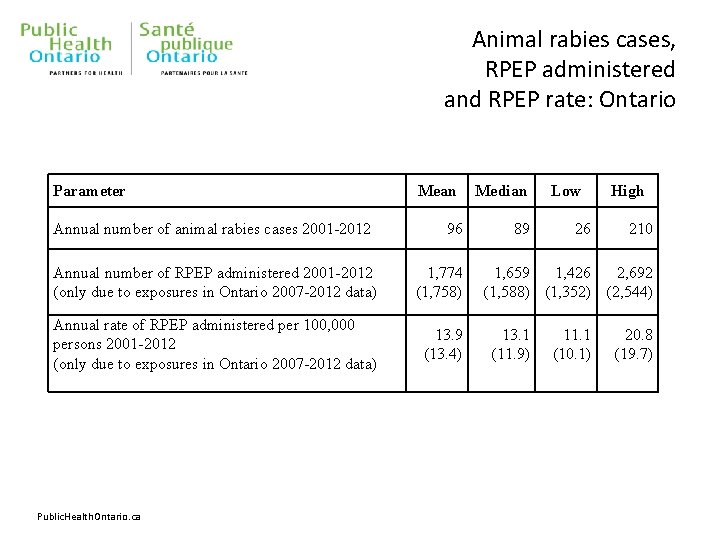
Animal rabies cases, RPEP administered and RPEP rate: Ontario Parameter Annual number of animal rabies cases 2001 -2012 Mean 96 Annual number of RPEP administered 2001 -2012 (only due to exposures in Ontario 2007 -2012 data) 1, 774 (1, 758) Annual rate of RPEP administered per 100, 000 persons 2001 -2012 (only due to exposures in Ontario 2007 -2012 data) 13. 9 (13. 4) Public. Health. Ontario. ca Median 89 Low 26 High 210 1, 659 1, 426 2, 692 (1, 588) (1, 352) (2, 544) 13. 1 (11. 9) 11. 1 (10. 1) 20. 8 (19. 7)
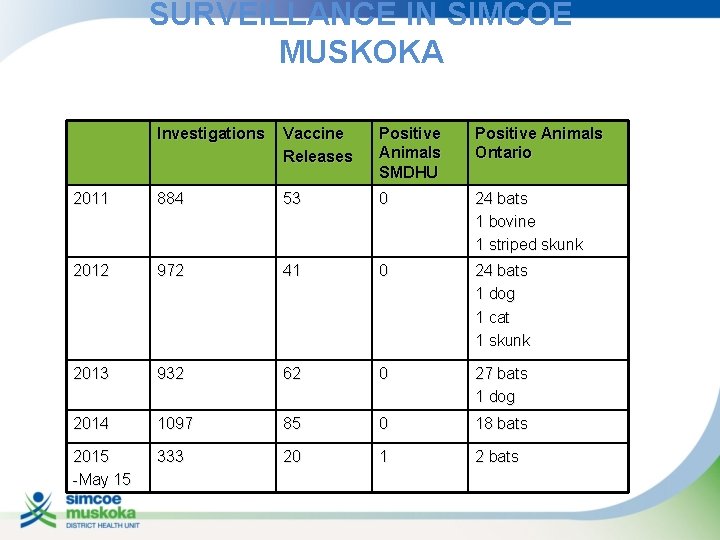
SURVEILLANCE IN SIMCOE MUSKOKA Investigations Vaccine Releases Positive Animals SMDHU Positive Animals Ontario 2011 884 53 0 24 bats 1 bovine 1 striped skunk 2012 972 41 0 24 bats 1 dog 1 cat 1 skunk 2013 932 62 0 27 bats 1 dog 2014 1097 85 0 18 bats 2015 -May 15 333 20 1 2 bats
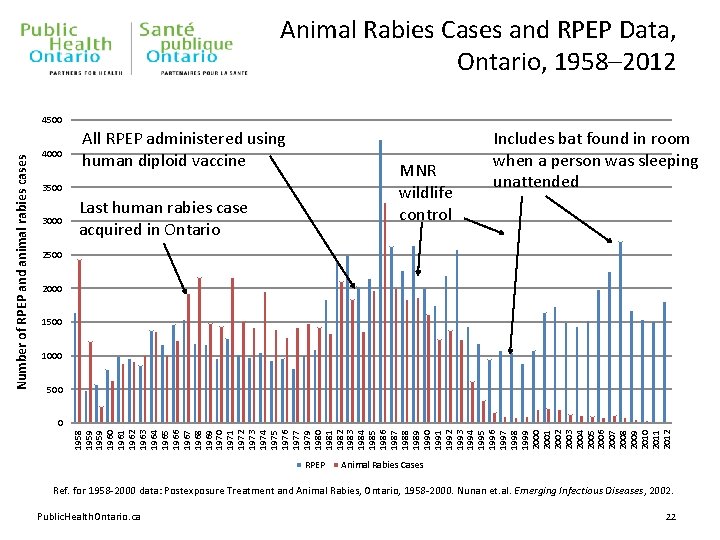
Animal Rabies Cases and RPEP Data, Ontario, 1958– 2012 4000 All RPEP administered using human diploid vaccine MNR wildlife control 3500 3000 Last human rabies case acquired in Ontario Includes bat found in room when a person was sleeping unattended 2500 2000 1500 1000 500 0 1958 1959 1960 1961 1962 1963 1964 1965 1966 1967 1968 1969 1970 1971 1972 1973 1974 1975 1976 1977 1979 1980 1981 1982 1983 1984 1985 1986 1987 1988 1989 1990 1991 1992 1993 1994 1995 1996 1997 1998 1999 2000 2001 2002 2003 2004 2005 2006 2007 2008 2009 2010 2011 2012 Number of RPEP and animal rabies cases 4500 RPEP Animal Rabies Cases Ref. for 1958 -2000 data: Postexposure Treatment and Animal Rabies, Ontario, 1958 -2000. Nunan et. al. Emerging Infectious Diseases, 2002. Public. Health. Ontario. ca 22

RABIES POST-EXPOSURE MANAGEMENT APPROACH 1. Wound care – irrigation (15 minutes), tetanus prophylaxis and antibiotics as appropriate, delayed wound closure 2. Report animal bites to local Public Health (requirement of the HPPA). § Public health staff role includes assessing human exposures to animals to advise on the need for RPEP. • Dogs, cats and ferrets may be observed for 10 days postexposure. • Testing of animals (wild or ill domestic) 3. A course of four rabies vaccines as well as rabies immune globulin (RIG). • Decision based on risk assessment – Canadian Immunization Guidelines, and the Guidance Document for the Management of Suspected Rabies Exposures (Public Health Division, MOHLTC 2013) Source: PHO Grand Rounds, Tuesday April 21, 2015

EXPOSURE INDICATIONS FOR VACCINATION • Species and local prevalence of rabies (exposing animal and in other species) • The type of exposure - bite, non-bite (e. g. salivary contact with open skin or mucous membrane, transplant of infected organs), or direct contact with a bat. • Provoked versus unprovoked bite (not helpful for wild animals) • The vaccination status and behaviour of a domestic animal. • The age of the exposed person (children higher risk) • The location and severity of the bite (hands and face) • Source animal for observation (cats, dogs, ferrets) or testing • Resources § Table 1: Risk Assessment Related to the Exposure to the Potentially Rabid Animal – Canadian Immunization Guide § Table 1: Summary of Post-Exposure Prophylaxis (PEP) for Persons Potentially Exposed to Rabies - Guidance Document for the Management of Suspected Rabies Exposures, MOHLTC

EXPOSURE RISK RECOMMENDATIONS: BATS • Current bat exposure recommendation: Post-exposure rabies prophylaxis following bat contact is recommended when: § There has been direct contact with a bat (touching or landing on a person), AND § A bite, scratch, or saliva exposure into a wound or mucous membrane cannot be ruled out. • Revision of NACI recommendation from 1998 to 2009, that people who may not be aware of or able to report a bat bite (e. g. , sleeping person, young child, cognitively impaired) receive vaccination : § expected to prevent a case in Canada once every 84 years § 314, 000 people would need to be treated (cost of $2 billion) to prevent 1 case § therefore revised recommendation in 2009

HISTORY OF CHANGES IN POST EXPOSURE PROPHYLAXIS • Number of doses of rabies vaccine has declined over time with its increase in potency • Reduction from a standard of 5 doses to 4 in 2010, bases on NACI and ACIP review, with the following rationale: § Protection is needed rapidly to prevent viral entry to CNS (therefore need RIG at the wound site) § Animal models of serological response and protection from rabies § Human immunogenicity studies with antibodies detected 14 days post vaccine initiation § No human cases attributed to failure to receive a fifth dose Source: MMWR, 19 Mar, 2010

POST-EXPOSURE PROPHYLAXIS PROTOCOL: RABIES VACCINE § Rabies vaccines (Rab) • Human Diploid Cell Rabies Vaccine). (HDCV) IMOVAX® Rabies • Purified Chick Embryo Cell Rabies Vaccine), (PCECV) Rab. Avert® § Not Previously Immunized • Immunocompetent – 4 doses (Day 0, 3, 7, 14) – 1 ml IM (never gluteal, as risking reduced immune response) • Immunocompromised (including corticosteroids, chloroquine) – 5 doses (Day 0, 3, 7, 14, 28) – 1 ml IM § Previously immunized • 2 doses – 1 ml IM (Day 0, 3) • 4 doses if previous vaccination was not with HDCV or PCECV

POST-EXPOSURE PROPHYLAXIS PROTOCOL: RABIES IMMUNE GLOBULIN • Post Exposure Prophylaxis § Rabies Immune Golbulin [Human] Hyper. Rab ® S/D § Human Rabies Immunoglobulin- Imo. Gam ® • Not Previously Immunized § To achieve prompt levels of neutralizing antibodies in the wound during the initial phase of management § 20 IU/kg - Day 0 (can be up to 7 days post onset of PEP series, if not immediately available) § If possible, entire volume to be given at the wound site(s) – remainder IM (away from first dose of rabies vaccine) • Previously Immunized - not indicated

PRE-EXPOSURE PROPHYLAXIS • Efficacy § Adequate antibody titres for up to 2 years after immunization – may wane after • 7 days after a booster dose 100% are adequately protected • Indications: § Laboratory workers who handle rabies virus. § Veterinarians, veterinary staff, animal control and wildlife workers. § Travelers to high risk locations – WHO (http: //www. who. int/rabies/Global_Rabies_ITH_2008. png ) § Hunter and trappers in areas with confirmed rabies. § Spelunkers (cavers). • Rabies Vaccine § 3 doses – 1 ml IM (days 0, 7 and 21 or 28) • Rabies Immune Globulin § Not indicated

VACCINATION SAFETY • HDCV risk is estimated to be minor; § Pain, erythema, swelling and itching at the injections site in 30% to 74%; § Headache, nausea, abdominal pain and dizziness in 20%. § Immune complex-like allergic reactions in up to 6% of persons receiving booster doses of HDCV. Few hospitalizations and no deaths. § Anaphylaxis in up to 1 in 10, 000 § In 2012 in Ontario, of the 9812 doses administered, there were 4 adverse events, none with serious outcomes (PHO) • RIG § Local pain, erythema and induration are common. Headache and low-grade fever may follow administration. § Made from human plasma – potential risk of undetected infectious agents (CDC)

CONTRAINDICATIONS AND PRECAUTIONS • No contraindications to the use of rabies vaccine or RIG after significant exposure to a proven rabid animal § Pregnancy not a contraindication for post exposure prophylaxis • Caution re compartment syndrome with wound infiltration • Seek expert consultation if hypersensitive to any ingredient in the formulation or container: § IMOVAX® Rabies: neomycin, phenol red § Rab. Avert®: amphotericin B, chick protein, chlortetracycline, neomycin, polygeline § (gelatin) § IMOGAM® Rabies: latex in vial stopper § HYPERRAB® S/D: • RIG: § Potential anaphylaxis with subsequent serum products for patients with specific Ig. A deficiency § Postpone live vaccinations 3 months afterward

POST VACCINATION SEROLOGIC TESTING • Serologic testing is not routinely indicated with vaccination (pre or post exposure prophylaxis) for healthy persons • Indications for serology testing: § Vaccination given by the ID route – check serology at least 2 weeks after completion of series. § Ongoing high risk of exposure to rabies (every 6 / 12 for continuous risk, to every 2 years for frequent risk). § Substantial deviation from the recommended postexposure schedule – check serology 7 to 14 days after completing the series. § Immunization with a vaccine other than HDCV or PCECV – check serology at least 7 to 14 days after completing the series – can be day 0, and discontinue RPEP after 2 doses HDCV or PCECV if sufficient titre § Immunocompromised persons, or if taking chloroquine check serology 7 to 14 days after completing the series. Revaccination with a second rabies vaccine series if unacceptable response, followed by serologic testing

PUBLIC HEALTH MANDATE / SERVICES • Animal Bite Investigation § Receive reports of all animal bites (1097 in 2014) § Animal Management • Specimen testing (102 in 2013; 13 in 2014) • Quarantine animal (dogs, cats, ferrets) – Normal 10 days – Follow up on animal vaccination • Companion animal vaccination § Low cost vaccination clinics § Animal vaccination enforcement (HPPA) • Vaccine consultation and provision (62 in 2013; 83 in 2014) • Public and health care provider communication
HEALTH UNIT WEBSITE RESOURCES Main SMDHU website http: //www. simcoemuskokahealth. org/ Home. aspx

HOW TO CONTACT US • Website resources – Primary Care Professionals’ Portal (Environmental Health) § http: //www. simcoemuskokahealth. org/JFY/PCPortal. aspx • Rabies email: rabies. program@smdhu. org • New Rabies Program Phone Line 705 -721 -7520 ext. 8894 § For physician consult and vaccine release • Animal exposure reporting § Rabies fax line 705 -725 -8132 § Reporting form: http: //www. simcoemuskokahealth. org/Libraries/JFY_Health_Care_Professio nals/150203 Rabies_and_Animal_Exposure_Report_Form. sflb. ashx • After Hours 1 -888 -225 -7851

CLINICAL SCENARIOS REVISITED • Case 1: Facial Bite by Dog in Guatemala § Dog unavailable § Dog known to be vaccinated § Victim previously immunized 5 years ago • Case 2: Bat Found in Bedroom § Husband awoke to something touching him, he grabbed bat and threw it across room § Wife reports not being touched by bat § Bat killed… awaiting testing for rabies
- Slides: 30