RABIES Dr Arvind Natarajan Professor Dept of Microbiology

RABIES Dr. Arvind Natarajan Professor Dept of Microbiology SDUMC

Family : Rhabdoviridae Genera : Lyssa virus RABIES VIRUS • • Rhabdos - means Bullet or Rod shaped Lyssa virus - means Madness
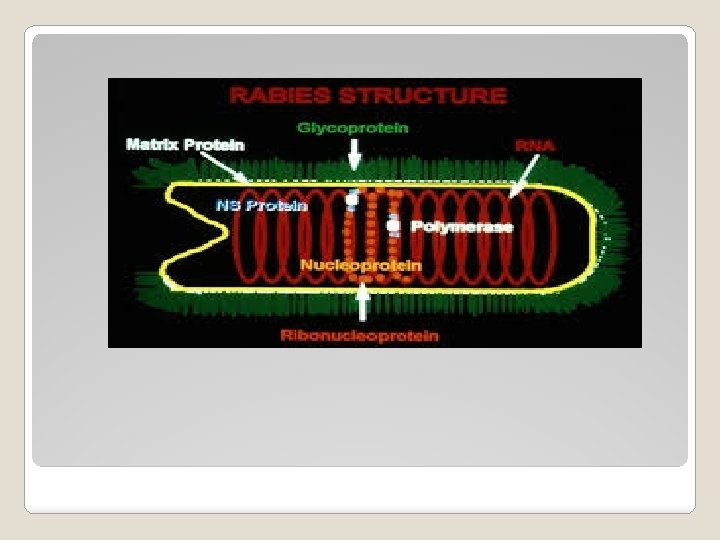

Morphology of Virus Bullet Shaped virus : 180 × 75 nm One end round & other end concave Enveloped virus - Spikes (GP) Matrix protein Nucleocapsid : helical symmetry : ss. RNA, Nucleoprotein Antigen Role Glycoprotein Pathogenesis : Binds to Ach receptors in neural tissues Immunity : neutralizing antibodies Diagnostic : Haemagglutination test Immunization : Protective Purified form of antigen used in the subunit vaccine Nucleoprotein Diagnostic : Direct immunofluorescence test
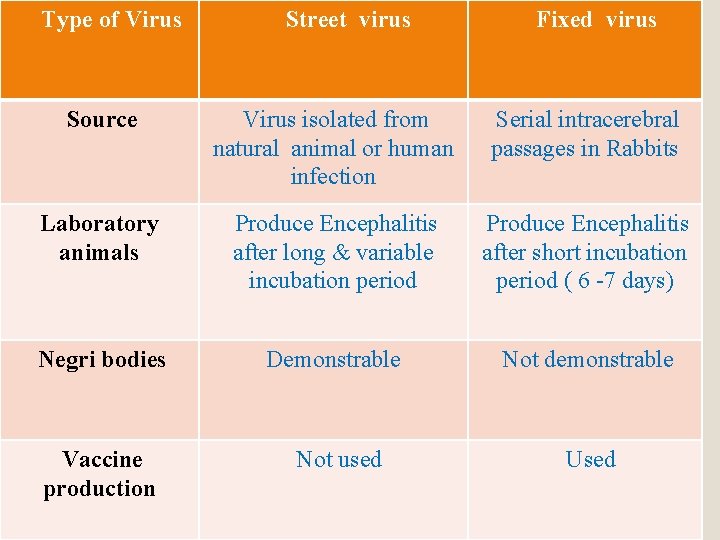
Type of Virus Street virus Fixed virus Source Virus isolated from natural animal or human infection Serial intracerebral passages in Rabbits Laboratory animals Produce Encephalitis after long & variable incubation period Produce Encephalitis after short incubation period ( 6 -7 days) Negri bodies Demonstrable Not demonstrable Vaccine production Not used Used

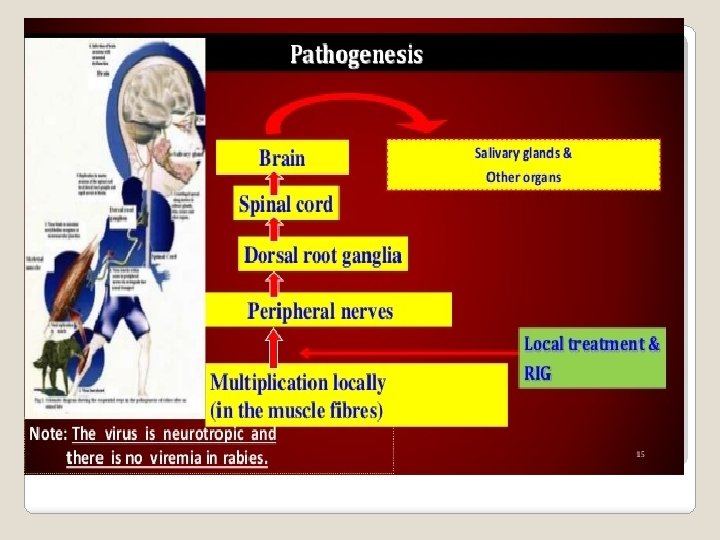
Pathogenesis Definition : Rabies is a fatal zoonotic , rapidly progressive disease of the CNS in humans and animals Source of infection : Animals : wide host range Highly susceptible : Foxes, Jackals, wolves, cattle, cats, bats Moderately susceptible : Dogs, goats, sheep, horses Reservoir of Infection : Jackals, fox, hyena

Modes of transmission : Contact with infected animals Saliva Mucosa or Non intact skin • Mainly by Infected animal Bite, Licks or Scratch • Inhalation of virus-containing aerosol • Organ transplantation - Cornea
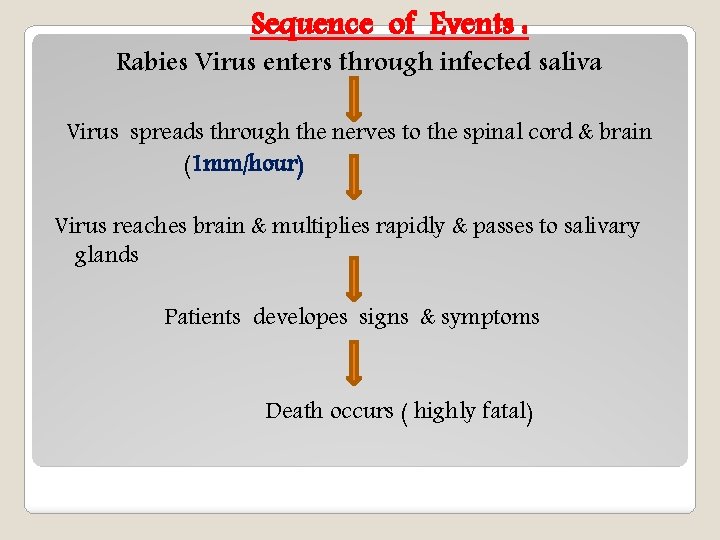
Sequence of Events : Rabies Virus enters through infected saliva Virus spreads through the nerves to the spinal cord & brain (1 mm/hour) Virus reaches brain & multiplies rapidly & passes to salivary glands Patients developes signs & symptoms Death occurs ( highly fatal)

Clinical Manifestations : Incubation period : Variable Typically 1 – 3 months Varies from <1 week to >1 year. Inversely related to the distance from the bite site to CNS 1. 2. 3. Short Prodromal period Acute Neurologic phase Coma & Death

Clinical manifestations 1. Short Prodromal period : Non specific symptoms : fever, malaise, anorexia Pain/unusual/ unexplained tingling, pricking or burning sensation (paraesthesia) at the wound site. 2. Acute Neurologic phase : • Encephalitic Rabies • Paralytic / Dumb rabies Encephalitic Rabies Hyperexcitability : anxiety, agitation, hyperactivity lucid interval : Autonomic ( sympathetic) lacrimation, salivation, cardiac arrhythmia Hydrophobia / Aerophobia

Paralytic / Dumb Rabies : ( 20% of cases) Partially vaccinated or infected with bat rabies virus • Flaccid paralysis • bitten limb progresses to quadiparesis 3. Coma & Death is almost certain

Rabies in Animals : Furious Rabies : The animal becomes aggressive, runs amok, bites people coming on its way Dumb Rabies : The animals withdraws itself from surroundings Remains silent

Laboratory Diagnosis : Diagnosis in Animals Diagnosis in Humans • • Antemortem diagnosis Postmortem diagnosis

Laboratory diagnosis Detection of Antigen : Direct IF Virus Isolation : Cell line : BHK , Mouse neuroblastoma Mouse inoculation Detection of Antibodies : CSF, Serum RRFIT, IFA Detection of nucleic acid – RT PCR Microscopy : Negri bodies

Diagnosis of Animals : Specimen Collection : • Brain tissue (especially hippocampus , cerebellum & spinal cord) • Salivary glands 1 part is preserved in 50% glycerol saline – Virus isolation Other part in Zenkers fixative – Negri bodies demonstration Methods : • Fluorescent antibody test : detects Rabies antigen • Demonstration of Negri bodies by Sellers stain • Immuno histo chemistry (IHC) – formalin fixed tissues • Virus Isolation : Mouse neuroblastoma cells (MNA) Baby Hamster Kidney (BHK) • Animal Inoculation test : Intra cerebral inoculation into mouse • •

DIAGNOSIS IN HUMANS Antemortem Diagnosis Specimen Collection � Saliva � CSF � Skin biopsies of hair follicles at the nape of the neck � Corneal Impression smear � Serum Saliva : virus isolation & RT-PCR. Serum and CSF : Detection of antibodies to rabies virus. Skin biopsy specimens & Corneal impression smear are examined for rabies antigen : : Direct IF

DIAGNOSIS IN HUMANS Postmortem Diagnosis Specimen Collection : • Brain tissue (especially hippocampus , cerebellum & spinal cord) • Salivary glands Methods : Fluorescent antibody test : detects Rabies antigen Demonstration of Negri bodies by Sellers stain Immuno histo chemistry (IHC) – formalin fixed tissues Virus Isolation : Mouse neuroblastoma cells (MNA) Baby Hamster Kidney (BHK) • Animal Inoculation test : Intra cerebral inoculation into mouse • • •
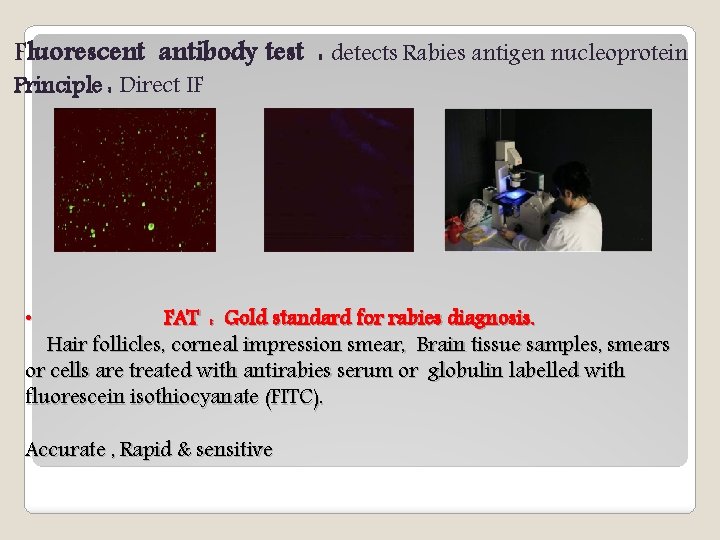
Fluorescent antibody test : detects Rabies antigen nucleoprotein Principle : Direct IF FAT : Gold standard for rabies diagnosis. Hair follicles, corneal impression smear, Brain tissue samples, smears or cells are treated with antirabies serum or globulin labelled with fluorescein isothiocyanate (FITC). • Accurate , Rapid & sensitive
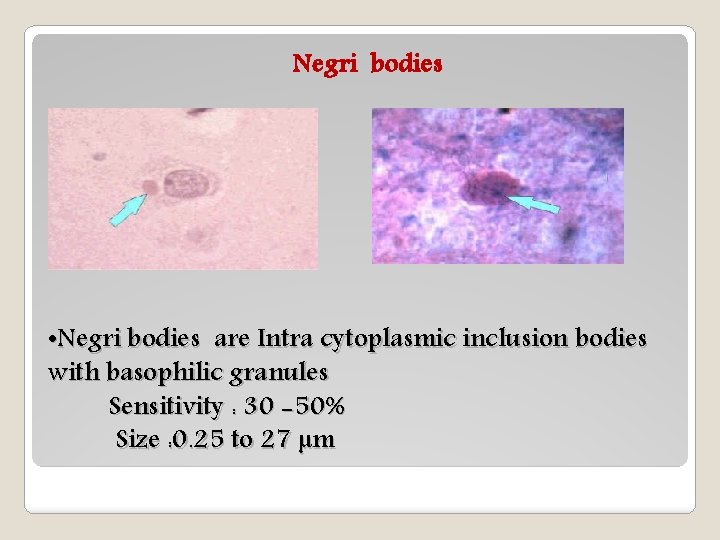
Negri bodies • Negri bodies are Intra cytoplasmic inclusion bodies with basophilic granules Sensitivity : 30 -50% Size : 0. 25 to 27 µm
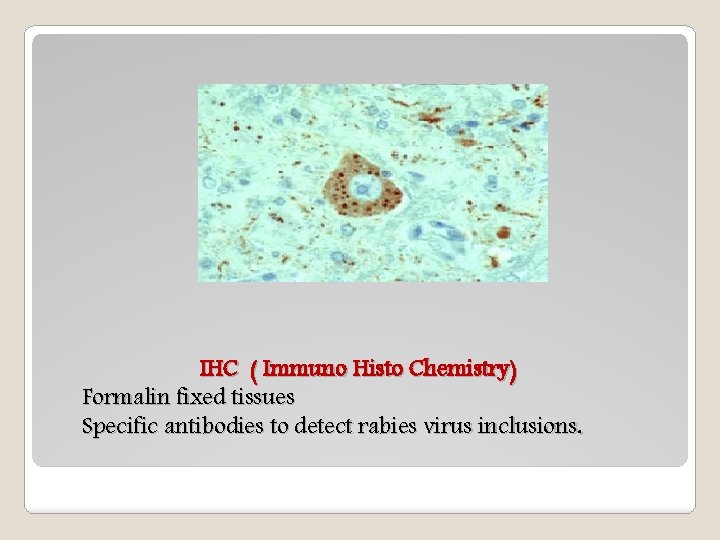
IHC ( Immuno Histo Chemistry) Formalin fixed tissues Specific antibodies to detect rabies virus inclusions.

Electron Microscopy : Bullet shaped virus
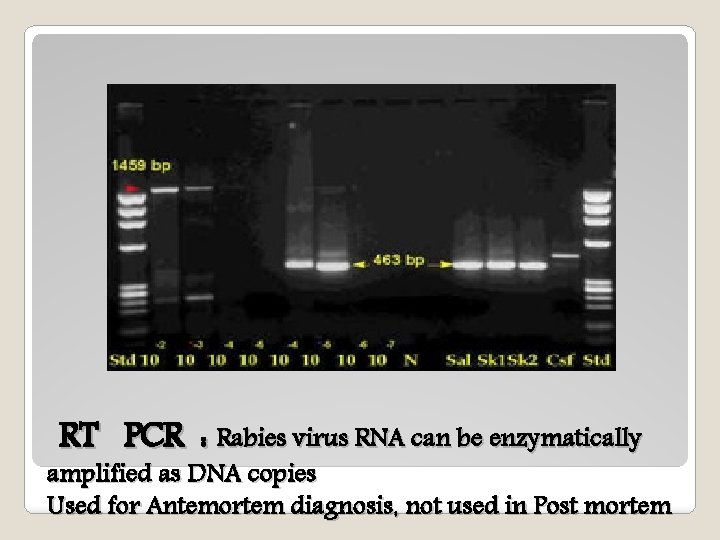
RT PCR : Rabies virus RNA can be enzymatically amplified as DNA copies Used for Antemortem diagnosis, not used in Post mortem

Antibody detection : Detection of CSF antibodies is more significant than serum antibodies CSF antibodies : • Appear early • definitive diagnosis Various antibody test : • • • MNT : Mouse neutralisation test FAVN Fluorescent Antibody Neutralization Test RFFIT : Rapid Fluorescent Focus Inhibition Test

Prophylaxis Pre exposure Prophylaxis : • Veterinarians • Health care workers • Laboratory workers • Forest explorers Vaccine Schedule: 3 doses on days 0, 7 & 21 Booster dose: after 1 yr & then after 5 yrs

Post exposure Prophylaxis Local Treatment • Hyper Immune serum/ Rabies Immunoglobulin • Vaccines • Local Treatment : The wound should be thoroughly washed with Soap & water IMMEDIATELY. After washing, treated with quartenary ammonium compound/ tincture iodine/alcohol Antibiotics & TT should be given SUTURING - CONTRAINDICATED


Hyper Immune serum/ Rabies Immunoglobulin : Anti Rabies Immunoglobulin : Human Anti Rabies Immunoglobulin • Horse Anti Rabies Immunoglobulin • Dose : 20 IU/kg body weight Given to high Risk groups Half dose is given – infilteration into the wound locally Other half is administered Intra muscularly Human Antisera – Safe , Preferred Horse antisera – Risk of Hypersensitivity

Rabies Vaccine : • Neural vaccines • Non neural vaccines Neural Vaccines : 1. Semple vaccine 2. Beta propiolactone vaccine 3. Infant Brain vaccine Neural Vaccines are associated with serious risk of neurological complications due to myelin (MBP) Neural vaccines are discontinued Subcutaneous route on the anterior abdominal wall

Non neural vaccines 1. Egg vaccines 2. Cell culture vaccines 3. Sub unit vaccines Egg Vaccines : • Duck egg vaccine • Live attenuated chick embryo vaccine. 2 types • Low egg passage: 40 -50 passage …Dogs • High egg passage: 180 passage … Cats/ Cattle

Cell culture vaccines : • Human diploid Cell Strain vaccine (HDCS) • Purified Chick Embryo Cell culture vaccine (PCEC) • Purified Vero Cell vaccine ( PVC) Vaccines are highly immunogenic not associated with neurological complications Vaccines which are widely used now a days Sub unit vaccines: Recombinant vaccine with Surface Glycoprotein ( Protective antigen) cloned Still in experimental stage – Orally

Post Exposure Prophylaxis Schedule : 0, 3, 7, 14 & 28 with booster dose on day 90 Protection : Upto 5 yrs Further exposure : 2 or 3 booster dose ( day 0, 3 & 7) After 5 years : full 5 doses Dose : 1 ml intramuscular 0. 1 ml intradermal Observe the animal for 10 days, if animal is healthy. . Discontinue PEP Animal is observed for 10 days bcoz the virus may be present in the saliva 3 -4 days before onset of symptoms & the animal dies with in 5 -6 days after developing the disease

Treatment: No specific treatment Supportive treatment: Intensive care, Management of complications, IFN may be used • • Prevention & Control : Elimination of stray dogs Vaccination of animals Registration & licensing of all domestic measures Control measures on wild life

THANK YOU DEAR STUDENTS
- Slides: 34