Quantitative validation of central lineassociated bloodstream infections CLABSI

Quantitative validation of central lineassociated bloodstream infections (CLABSI) in Oregon intensive care units (ICU) 2009 Zintars Beldavs Manager HAI Program, Acute and Communicable Disease Section, Oregon Public Health Division, Oregon Health Authority June, 2012

Central Line-Associated Bloodstream Infection (CLABSI) Deadly: 18% mortality 14, 000 deaths/ year in ICU patients Prolong hospitalization by mean of 7 days Expensive: $3, 700 - $29, 000/episode Preventable: hand hygiene, barrier precautions, skin antisepsis, catheter site selection Pittet D, Tarara D, Wenzel RP. Nosocomial bloodstream infection in critically ill patients. Excess length of stay, extra costs, and attributable mortality. JAMA. 1994; 271: 1598 -1601. Soufir L et al. Infect Control Hosp Epidemiol 1999 Jun; 20(6): 396 -401.

Mandated Reporting in Oregon Reportable as of 1/1/2009 • CLABSIs in ICU • SSI knee prostheses and coronary artery bypass grafts More reportable surgical site infections as of 1/1/11 • Colon surgery • Hip prosthesis • Laminectomy • Abdominal hysterectomy
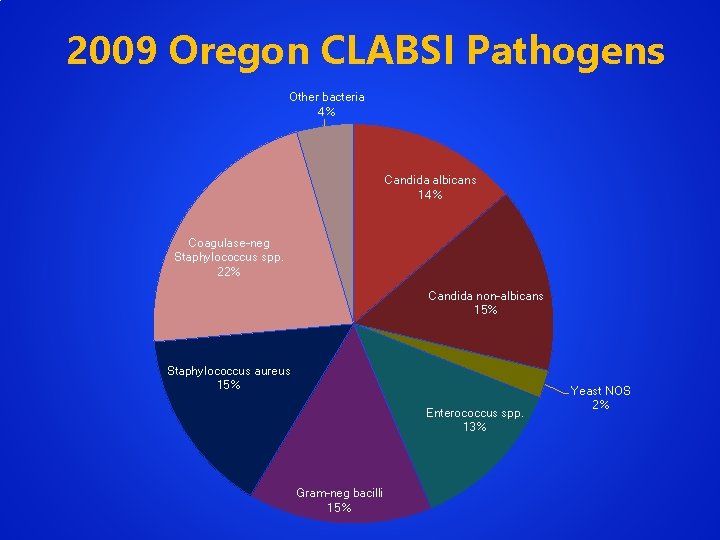
2009 Oregon CLABSI Pathogens Other bacteria 4% Candida albicans 14% Coagulase-neg Staphylococcus spp. 22% Candida non-albicans 15% Staphylococcus aureus 15% Enterococcus spp. 13% Gram-neg bacilli 15% Yeast NOS 2%
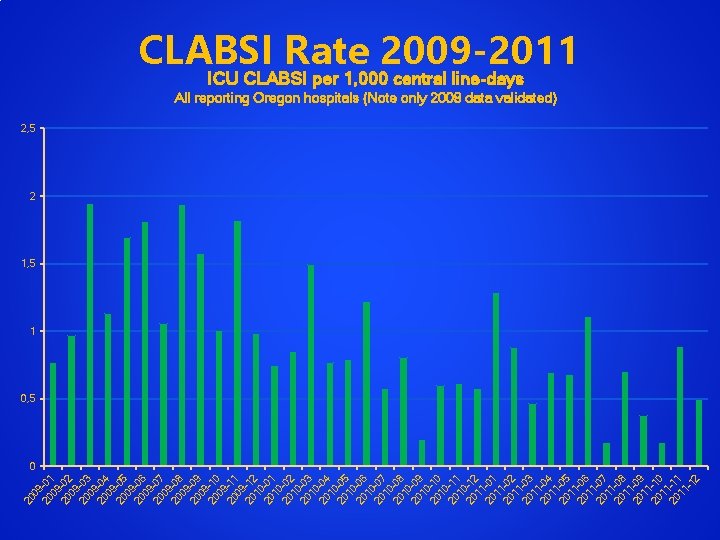
09 20 -01 09 20 -02 09 20 -03 09 20 -04 09 20 -05 09 20 -06 09 20 -07 09 20 -08 09 20 -09 09 20 -10 09 20 -11 09 20 -12 10 20 -01 10 20 -02 10 20 -03 10 20 -04 10 20 -05 10 20 -06 10 20 -07 10 20 -08 10 20 -09 10 20 -10 10 20 -11 10 20 -12 11 20 -01 11 20 -02 11 20 -03 11 20 -04 11 20 -05 11 20 -06 11 20 -07 11 20 -08 11 20 -09 11 20 -10 11 20 -11 11 -1 2 20 CLABSI Rate 2009 -2011 ICU CLABSI per 1, 000 central line-days All reporting Oregon hospitals (Note only 2009 data validated) 2, 5 2 1, 5 1 0, 5 0
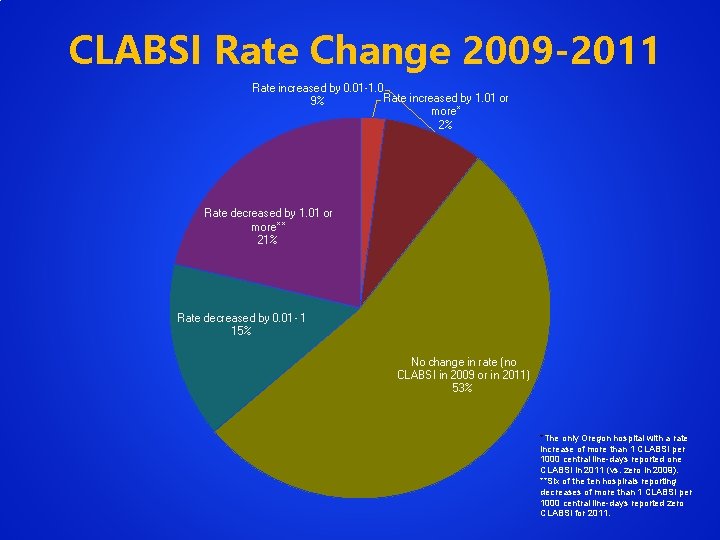
CLABSI Rate Change 2009 -2011 Rate increased by 0. 01 -1. 0 Rate increased by 1. 01 or 9% more* 2% Rate decreased by 1. 01 or more** 21% Rate decreased by 0. 01 - 1 15% No change in rate (no CLABSI in 2009 or in 2011) 53% *The only Oregon hospital with a rate increase of more than 1 CLABSI per 1000 central line-days reported one CLABSI in 2011 (vs. zero in 2009). **Six of the ten hospirals reporting decreases of more than 1 CLABSI per 1000 central line-days reported zero CLABSI for 2011.
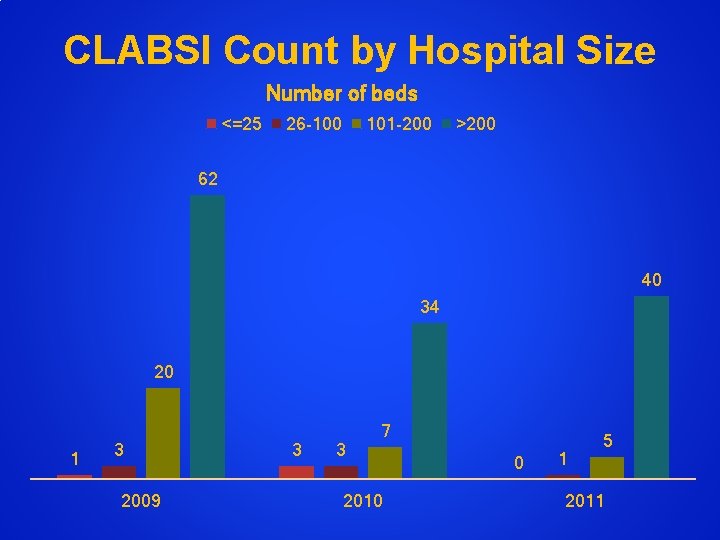
CLABSI Count by Hospital Size Number of beds <=25 26 -100 101 -200 >200 62 40 34 20 1 3 2009 3 3 7 2010 0 1 5 2011

Validation for Accurate Data • Concern: surveillance definitions applied inconsistently by IPs • Poor inter-rater reliability: kappas. 30 to. 58 • Previous validation studies: potentially > half of cases not reported (Connecticut)

Objectives • Evaluate quality of reported data – Assess under- and over-reporting – Gauge the reliability and consistency of surveillance case definitions • Provide feedback to facilities on surveillance case definitions and reporting methods

Methods • Study period: 2009 • Included: 44 acute care hospitals – 28 with < 50 beds – 10 with > 200 beds – Median central line days 210, range 4 -4956 • OPHD validation team: – – HAI Program Manager Epidemiologist EIS Officer/Physician 3 public health nurses Map: Oregon Association of Hospitals and Healthcare Systems, oahhs. org

Methods All blood culture (+) Drawn in ICU or up to 48 hours after and Organism not isolated in 14 days before admit

Methods Unit of analysis: Single bacteremia episode More than one CLABSI/patient possible

Methods 37 Hospitals All (+) culture reviewed 7 Hospitals All reported CLABSI and random sample 60 (+) culture not reported as CLABSI Reviewers blind as to reported CLABSI status
Methods Hospital Determination Validator Determination Adjudication Discussion NHSN

Methods 1926 (+) cultures received on line lists 1204 from 7 highest volume facilities 722 from 41 facilities < than 60 (+) cultures

Methods 1199 medical records reviewed 477 sampled at 7 highest-volume facilities 722 at small- and medium- volume facilities

Results 817 included in final analysis Hospitals included cultures not requested: (+) blood cultures obtained prior admit or > 48 hours after discharge from ICU 382 of 1199 reviewed censored

Results Discordant Cases • 35 records with disagreement – 18 (51%) adjudicated as CLABSI – 17 (49%) adjudicated as not CLABSI – Hospital correct in 13 (37%) – OPHD correct in 22 (63%) – 4 required NHSN consult (2 CLABSI)

Reasons for discrepancies Reason for discrepancy for under-reported CLABSI No. episodes % No clearly discernible reason determined 7 44 Misattributed CLABSI to other infection 7 44 Recognized CLABSI failed to attribute ICU 1 6 Misclassified CLABSI as present on admit 1 6 Total 44 100 No. episodes % Infection attributable to other site 2 33 Infection not attributable to ICU 2 33 Single blood culture for probable contaminant 1 16. 5 Unknown why reported CLABSI 1 16. 5 Total 6 100 Reason for discrepancy for over-reported CLABSI For CLABSI “just missed”: at some facilities, IP staff had changed since 2009 and current staff unaware of rationale for previous reporting decisions.
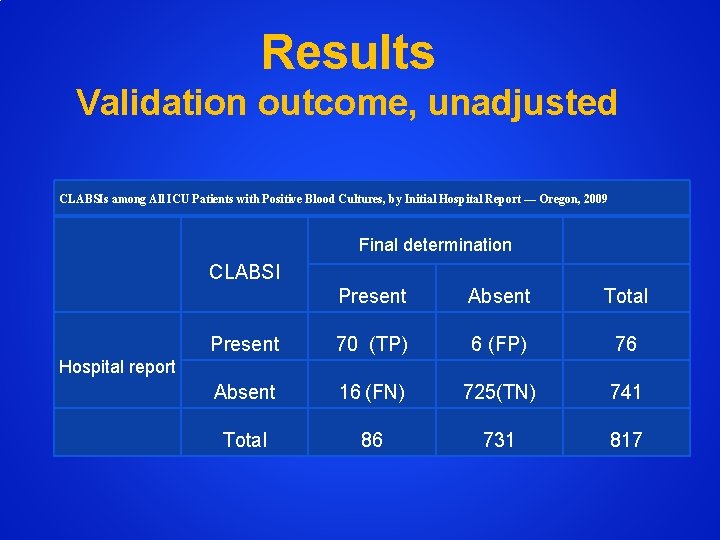
Results Validation outcome, unadjusted CLABSIs among All ICU Patients with Positive Blood Cultures, by Initial Hospital Report — Oregon, 2009 Final determination CLABSI Present Absent Total Present 70 (TP) 6 (FP) 76 Absent 16 (FN) 725(TN) 741 Total 86 731 817 Hospital report

Example Calculation to Adjust for Sampling Fraction • • • 60 Records sampled at hospital 142 Total BSI 2 BSI reported as CLABSI Sampling fraction: 60/140=. 43 True positive and false positive remain (all reported CLABSI reviewed) False negative and true negative results divided by sampling fraction Hospital CLABSI Present Hospital CLABSI Absent Final Determination CLABSI Present Final Determination CLABSI Absent 1 True Positive 1 False Positive “Overreport” 2 (Estimate: 2/. 43=4. 7) False Negative “Underreport” 42 (Estimate: 42/. 43=98) True Negative
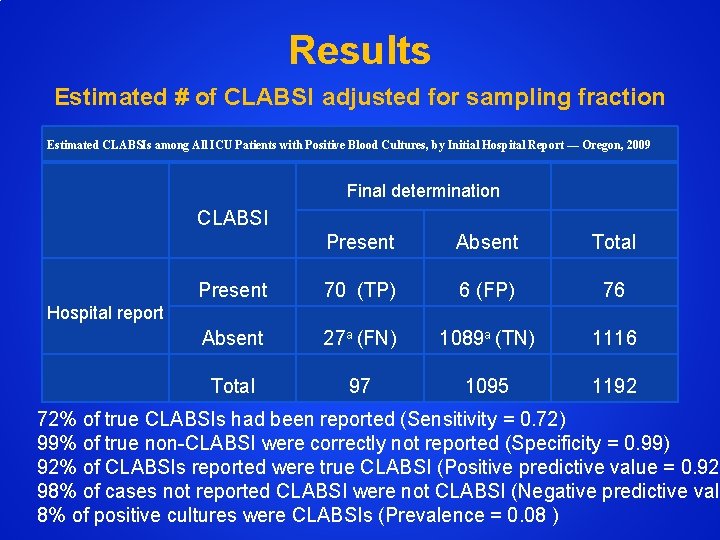

Results Estimated # of CLABSI adjusted for sampling fraction Estimated CLABSIs among All ICU Patients with Positive Blood Cultures, by Initial Hospital Report — Oregon, 2009 Final determination CLABSI Present Absent Total Present 70 (TP) 6 (FP) 76 Absent 27 a (FN) 1089 a (TN) 1116 Total 97 1095 1192 Hospital report 72% of true CLABSIs had been reported (Sensitivity = 0. 72) 99% of true non-CLABSI were correctly not reported (Specificity = 0. 99) 92% of CLABSIs reported were true CLABSI (Positive predictive value = 0. 92) 98% of cases not reported CLABSI were not CLABSI (Negative predictive valu 8% of positive cultures were CLABSIs (Prevalence = 0. 08 )
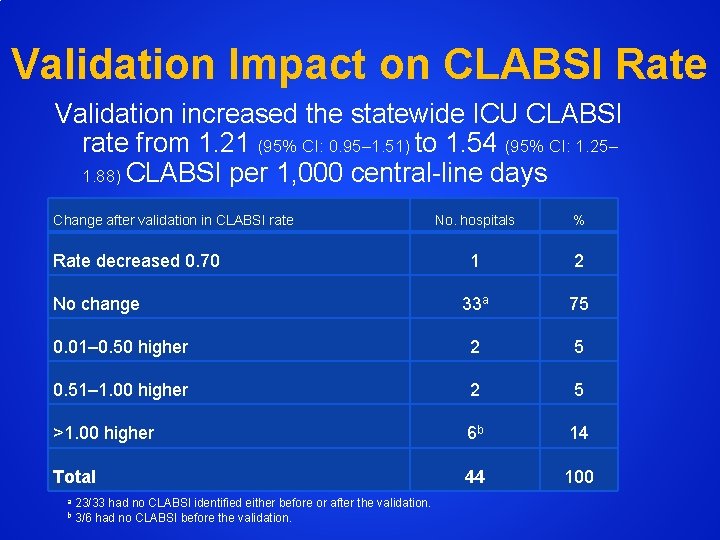
Validation Impact on CLABSI Rate Validation increased the statewide ICU CLABSI rate from 1. 21 (95% CI: 0. 95– 1. 51) to 1. 54 (95% CI: 1. 25– 1. 88) CLABSI per 1, 000 central-line days Change after validation in CLABSI rate No. hospitals % 1 2 33 a 75 0. 01– 0. 50 higher 2 5 0. 51– 1. 00 higher 2 5 >1. 00 higher 6 b 14 Total 44 100 Rate decreased 0. 70 No change a b 23/33 had no CLABSI identified either before or after the validation. 3/6 had no CLABSI before the validation.

Importance of Inter-Agency Follow-up Discussion • Of 27 unreported cases identified as CLABSI by OPHD, 16 (59%) true CLABSI • Sensitivity of reporting: – 72% based on follow-up adjudication – vs. 60% based on OPHD review alone (P= 0. 07), closer to some previous validation efforts

Limitations • Denominator data not rigorously assessed • Did not adjudicate cases when reviews concordant with reported data • Unbiased 3 rd party not involved in adjudication discussions

Conclusions • Validating hospital CLABSI reporting improves accuracy of hospital-based CLABSI surveillance • Discussing discordant findings improves the quality of validation

Future Work • Currently completing coronary artery bypass graft validation of all 14 hospitals – Similar adjudication procedure – Sampling higher duration procedures • Given funding: comprehensive baseline and yearly sampled validation other HAIs

Acknowledgments OPHD HAI program staff and others assisting • Paul Cieslak – Public Health Physician • Ann Thomas – Public Health Physician • Margaret Cunningham – HAI Epidemiologist • Diane Roy – HAI Administrative Assistant • John Oh – EIS Officer • Steve Moore – Public Health Nurse • Jennifer Tujo – Infection Preventionist • Valerie Ocampo – HAI Public Health Nurse Oregon Patient Safety Commission Office for Oregon Health Policy and Research Association of Professionals in Infection Control, Oregon-SW Washington Chapter Questions? 971 -673 -1111 zintars. g. beldavs@state. or. us

Questions?
- Slides: 29