Quality Medical Documentation The Key to Evidencing Quality

















- Slides: 22

Quality Medical Documentation: The Key to Evidencing Quality Care § From a risk-management perspective, understand how local, state, and federal regulations govern DMC-ODS services. § Identify the DMC-ODS timeliness and documentation requirements for critical components of the treatment process. § Understand the value a well documented treatment plan has on billing.

Admission to Treatment Eligibility *This is an Admission Work Flow Task What Eligibility for SUD benefits must be verified by the provider. This includes: • Validating Residency (I. D. Card; Utility Bill, etc. ) • Validating Medi-Cal Eligibility: MEDS file; My Health participation • Assisting individuals without current Los Angeles residency or current Medi-Cal eligibility When- At Intake Who- Provider Staff DOCUMENTATION: Notes documenting intake/admission information should be maintained in the Client Record using the “Miscellaneous Notes”

Admission to Treatment INTAKE/ASSESSMENT *This is an Admission Work Flow Task What ASAM Criteria Assessment (Full ASAM- Youth or Adult): 6 dimensions with risk ratings and appropriate level of care [LOC] determination Who- LPHA or Counselor When- Within 7 days from admission Date Note: Assessments need to be reviewed, and updated on a regular basis, including at every care transition

Admission to Treatment Physical Exam *This is an Admission Work Flow Task For Admission into a DMC SUD Treatment Program a When- Within 30 days from admission Date physical Exam is required in one of the following ways: a. They have had a Physical Exam within the past 12 months. Obtain copy and place in patient record; or b. Perform a new physical exam (by a physician, PA, or LNP) OR, if neither (a) or (b) has been performed, c. Include the goal of obtaining a physical exam in the Treatment Plan Perinatal Treatment is limited to pregnant and post partum women; medical documentation of pregnancy

*This is an Admission to Treatment Work INTAKE – Diagnosis and Medical Necessity Admission Flow Task What Review of Intake information and Evaluation of patient for SUD Diagnosis How The evaluation must be performed through a face-to-face review When- Within 7 days from admission Date DOCUMENTATION- The basis for the SUD diagnosis must be documented to include the specifier(s) and basis for each specifier. . . Who- LPHA, review with Counselor

Some Notes on MEDICAL NECESSITY The CORNERSTONE of Admission A simple way to look at when services are MEDICALLY NECESSARY. . 1. There is a SUD diagnosis (DSM-V diagnosed, must have at least one diagnosis; youth <21 years may be “at risk” by ASAM Criteria) 2. There are impairments—functional and diagnostically related (ASAM- Treatment services are consistent with standard treatment of the condition; meet ASAM Criteria) 3. It can be reasonably expected that treatment will improve functioning (ASAM- Services are required for other than convenience) See 22 CCR § 51303; 42 CFR § 438. 210(a)(4) and, ASAM Criteria (2013)

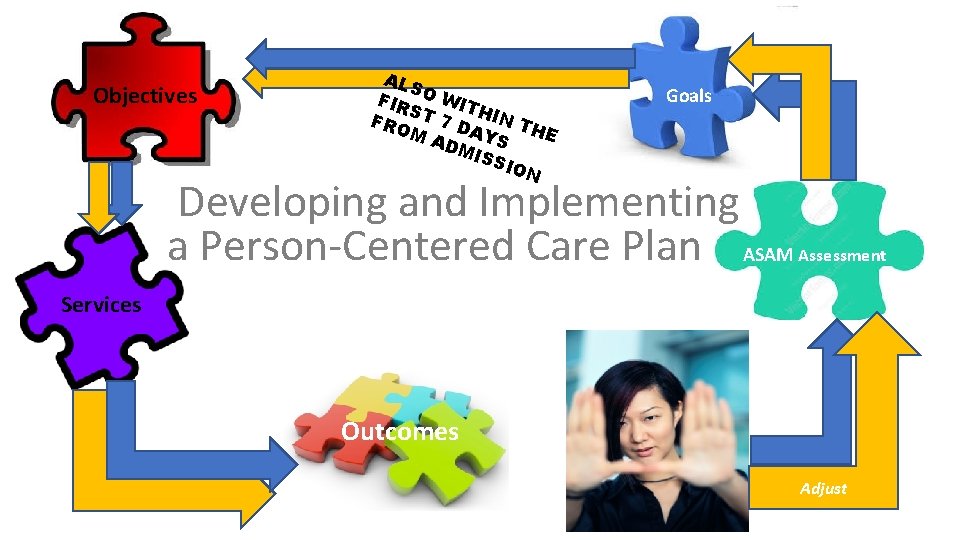
Objectives ALS FIR O WIT S H FRO T 7 D IN TH M A AYS E DM ISS ION Goals Developing and Implementing a Person-Centered Care Plan ASAM Assessment Services Outcomes Adjust

• In a PATIENT-CENTERED CARE ASSESSMENT the social and environmental factors that interfere with a patient’s usual care and decision-making are addressed as part of the patient’s care plan, but more importantly… • The ASAM 6 dimension is the tool we use to organize our assessment of the biopsychosocial factors, examining the challenges revealed in the context of the patient’s strengths, abilities, and preferences Patient Centered means Patient Goals are most important

Treatment Plan –Requirements Patient-Centered and with all the right stuff. . . 1. Statement of problem(s) clearly linked to issues identified in the assessment (ASAM) 2. Goals to be reached that address each problem Complete 3. Action steps- Specific activities and interventions and signed 4. Target dates to complete action steps/interventions within 7 days of 5. Description of services- type and frequency admit 6. Assignment of Primary counselor- name 7. DSM diagnosis 8. Signatures- counselor, patient, and LPHA (Typed/Printed names) and date(s) signed.

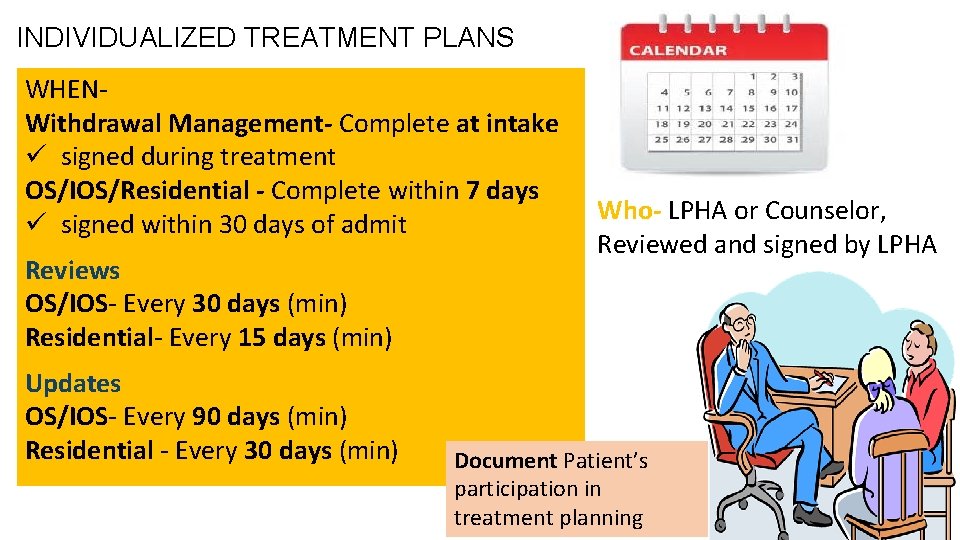
INDIVIDUALIZED TREATMENT PLANS WHENWithdrawal Management- Complete at intake ü signed during treatment OS/IOS/Residential - Complete within 7 days ü signed within 30 days of admit Reviews OS/IOS- Every 30 days (min) Residential- Every 15 days (min) Updates OS/IOS- Every 90 days (min) Residential - Every 30 days (min) Who- LPHA or Counselor, Reviewed and signed by LPHA Document Patient’s participation in treatment planning

PROBLEM STATEMENTS. . and GOALS Getting to “Good Problem Statements and Goals” • Start with a Therapeutic Alliance--3 CRITICAL ELEMENTS • Shared Goals • Consensus on methods and tasks of Treatment • An emotional bond • The ASAM assessment must be brought into the “Alliance” • Medical Necessity must be addressed • “Identified problems” must be addressed q There is no agreed upon standard for how to conduct the Treatment Planning session however a review of the ASAM (Risk ratings and rational) and a discussion on the patient’s vision for “DESIRED RESULTS” is recommended.

SHORT TERM GOALS- Big Goals Take Many Smaller Steps Short Term Goal are the manageable steps leading to goal attainment PROBLEM- Homelessness is a personal stressor and continuing drug use risk factor GOAL- Find recovery supporting, secure housing • Short-Term Goal 1: Resolve ambivalence about drug use and committing to abstinence-based housing • Short-Term Goal 2: Use problem solving format to identify possible shelter/housing options • Short-Term Goal 3: Complete applications and interviews for housing

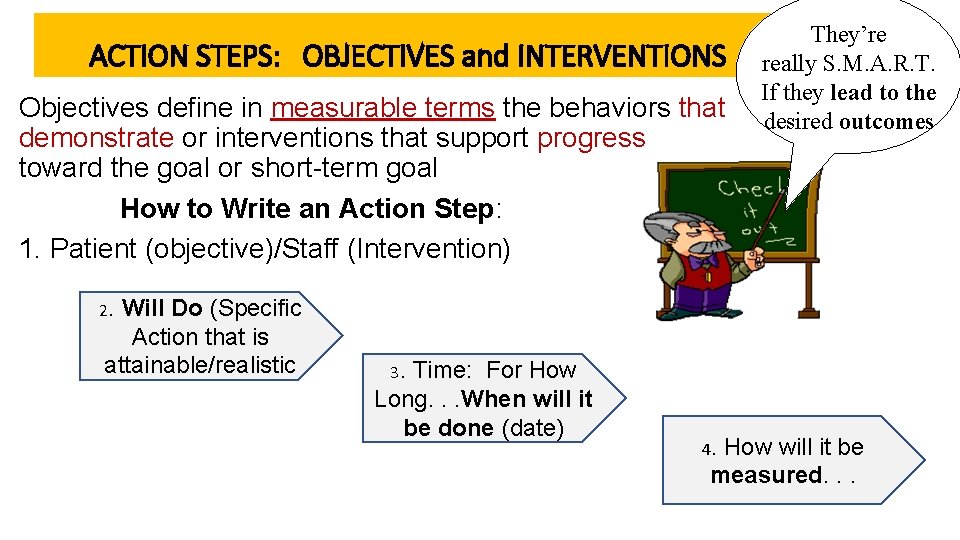
ACTION STEPS: OBJECTIVES and INTERVENTIONS Objectives define in measurable terms the behaviors that demonstrate or interventions that support progress toward the goal or short-term goal How to Write an Action Step: 1. Patient (objective)/Staff (Intervention) Will Do (Specific Action that is attainable/realistic They’re really S. M. A. R. T. If they lead to the desired outcomes 2. 3. Time: For How Long. . . When will it be done (date) 4. How will it be measured. . .

Look at Patient X’s needs—what she says and what is evidenced in her ASAM assessment (risk ratings and their rational) Practice Using the SMART format : 1) Chose one area and write a Problem Statement 2) For that “Problem”, write a Goal 3) List at least Three Action Steps and One Intervention • Do you feel this problem/goal and the objectives meet “medical necessity? ” Why, or how? • What else do you need to do to complete this treatment plan?

Case Notes Progress notes serve three major functions: 1. Document all services rendered during the course of treatment (ARE THE BASIS FOR BILLING); 2. Provide a record of all significant clinical data experienced during the treatment episode 3. Describe response to treatment—how services provided impacted impairments and functioning They are critical basis for reviewing and adjusting treatment plans. SAPC requires that progress notes for group & individual sessions follow 1 of 4 formats: SOAP; GIRP; SIRP; or BIRP

S. O. A. P. Method of Documentation Subjective - client’s observations or thoughts, client statement Objective – counselor’s observations during session Assessment - counselor’s understanding of problems and test results Plan – goals, objectives, and interventions reflecting identified needs 16

Documentation- Progress Notes IOP, Outpatient, NTP, Residential and Recovery Services For each individual or group session, the counselor who conducted that session shall record a progress note for each participant. Must be a legible, individual narrative summary and include the following information: Topic of Session Description of progress toward goals Date, Start, and End Time of each Service Document location of service and if in community, how confidentiality was ensured Remember to chart to your billable session Typed/Printed Name of LPHA or Counselor, signature, and date note written – MUST BE WITHIN 7 DAYS OF THE SESSION

Documentation- Progress Notes Intensive Outpatient Treatment and Residential Treatment The counselor shall record one progress note (at a minimum) per calendar week for each participant. Must be an individual narrative summary and include the following information: Topic of each Session Description of progress toward goals Remember to chart to your billable session Date, Start, and End Time of each Service; Record of participants attendance Document location of service and if in community, how confidentiality was ensured Typed/Printed Name of LPHA or Counselor, signature, and date note written – MUST BE WITHIN 7 DAYS of the summary period

DON’T FORGET GROUP SIGN IN SHEETS!!!! Date, Start, and End Time of the session Topic of each Session Typed/printed patient identifier, patient signature Description of progress toward goals Typed/Printed Name of LPHA or Counselor with signature

Let’s talk about writing chart notes. …. . How do we consistently chart PROGRESS TOWARD TREATMENT PLAN GOALS AND OBJECTIVES?

Continuing Services- Authorizations Continuing Service Justification- Medical Necessity qualification for ongoing receipt of DMC-ODS services is determined at least every six months (annually for NTP’s). This is accomplished through the reauthorization process by the LPHA Review by: LPHA What must be Documented before Continuing Services can be authorized: A Review of, • Beneficiary’s personal, medical & SU history • Most recent physical exam • Progress notes and TP Goals • Counselor’s recommendation • Beneficiary’s prognosis

Discharge/Transfer Planning It is said that “discharge planning begins at admit”—that means we should always be planning for the continuing care of our patients. A thorough discharge plan should include: • Narrative summary of the treatment episode. Describe services received and the patient’s response by ASAM Dimensions • Indicate patient’s prognosis: “Good”, “Fair”, or “Poor”, and provide an explanation. • Describe relapse triggers; the patient’s plan to avoid relapse when confronted with each trigger; and, the patient’s recovery support plan. • List all patient’s medications. Include dosage and response. • Indicate the reason for the discharge/referral or level of care transferred to if appropriate--Describe recommendations for follow up. Transition to and appropriate higher/lower level of care including Recovery Support Services needs to be a part of each Discharge Planning process and should be done as a WARM HAND-OFF!