PYOGENIC INFECTIONS AND TYPHOID Dr Kiran H S































































- Slides: 88

PYOGENIC INFECTIONS AND TYPHOID Dr. Kiran H S Assistant Proffessor Dept of Pathology

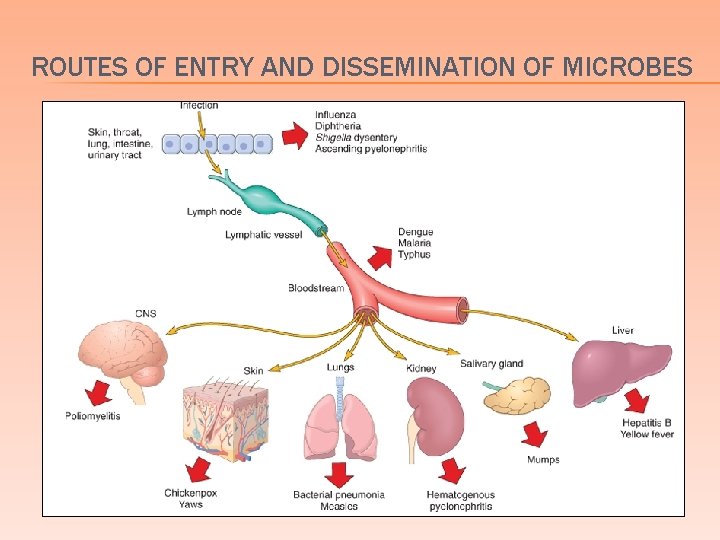
ROUTES OF ENTRY AND DISSEMINATION OF MICROBES

GRAM NEGATIVE AND POSITIVE BACTERIAL INFECTIONS 3

STAPHYLOCOCCUS AUREUS 4

TOXIN-RELATED DISEASES ASSOCIATED WITH STAPH. AUREUS � Toxic Shock syndrome � Scalded skin syndrome � Bullous impetigo � Food poisoning 5

1)TOXIC SHOCK SYNDROME (TSS) 6

TOXIC SHOCK SYNDROME � Caused by any of several related toxic exotoxins produced by S. aureus � TSST-1 � most frequently implicated exotoxin � staphylococcal enterotoxin B is 2 nd most frequently implicated � For illness to develop, an individual must be colonized or infected with a toxigenic strain of S. aureus and lack a protective level of antibody to the toxin 7

TOXIC SHOCK SYNDROME � Menstruation most common setting for TSS � May also be associated with barrier contraceptives, puerperium, septic abortion, non-obstetric gynecologic surgery and skin lesions � chemical or thermal burns, insect bites, varicella lesions and surgical wounds � Overt infection with S. aureus is not required for the development of TSS 8

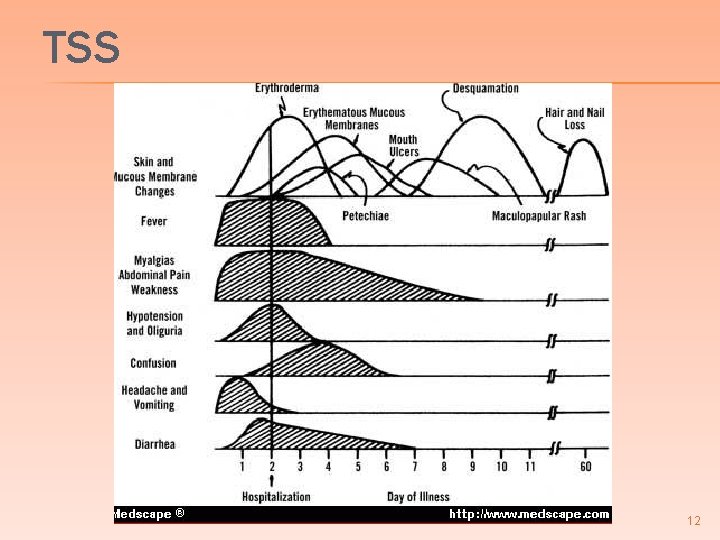
TOXIC SHOCK SYNDROME DIAGNOSTIC CRITERIA � Fever > 102 0 F � Rash; diffuse macular erythroderma “sunburn rash” � Desquamation: 1 -2 weeks after onset of illness typically on palms and soles � � Hypotension; systolic blood pressure of < 90 mm Hg or orthostatic syncope � S. aureus infection or mucosal colonization 9

TOXIC SHOCK SYNDROME DIAGNOSTIC CRITERIA � Involvement of at least three of the following organ systems � GI; vomiting or diarrhea � Muscular; severe myalgias or twice upper limit elevation of CK � Mucous membranes; hyperemia; vaginal, oropharyngeal, conjunctival � Renal; BUN or Creatinine level at least twice the upper limit of normal 10

TOXIC SHOCK SYNDROME DIAGNOSTIC CRITERIA � Involvement of at least three of the following organ systems (ctd) � Hepatic; total serum bilirubin or ALT or AST level at least twice the upper limit of normal � Hematopoietic; thrombocytopenia � CNS; disorientation or alteration in consciousness 11

TSS 12

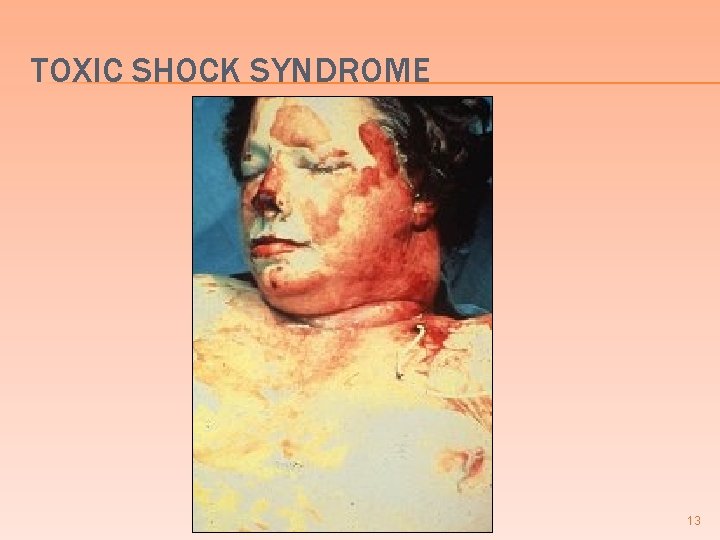
TOXIC SHOCK SYNDROME 13

2)SCALDED SKIN SYNDROME 14

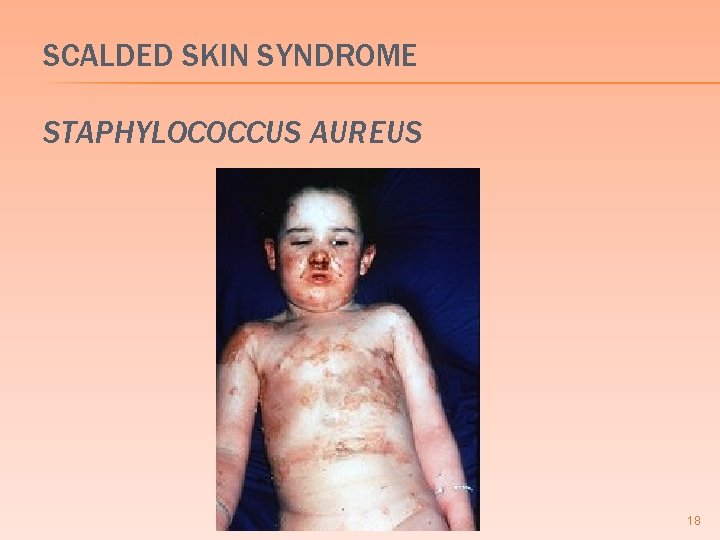
SCALDED SKIN SYNDROME Wide spread skin disease due to epidermolytic toxin � Separation of epidermis at stratum granulosum � Children and immunocompromised adults � � � rare in immunocompetent adults because of the presence of antibodies Begins with erythematous rash periorbital and perioral areas and spreads to the trunk and limbs generalized bulla formation 15

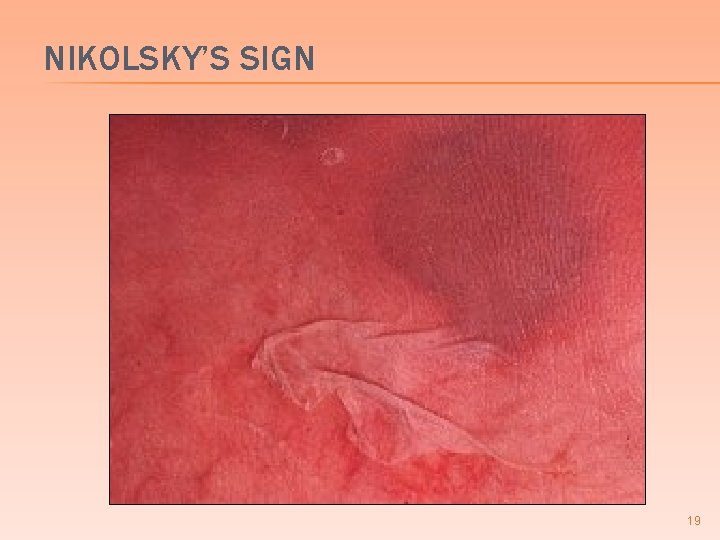
SCALDED SKIN SYNDROME � (+) Nikolsky sign � skin slides off when touched Bullae usually sterile � effects are due to exotoxin � Prodrome of fever and malaise with generalized erythema and profound skin tenderness � 16

SCALDED SKIN SYNDROME � Toxic Epidermal Necrolysis (TEN) � sloughing of the entire epidermis, resulting in very severe disease +/- death � usually immune mediated; drug associated (ampicillin, allopurinol) � less commonly assoc w/ Staph. � HIV infected patients 17

SCALDED SKIN SYNDROME STAPHYLOCOCCUS AUREUS 18

NIKOLSKY’S SIGN 19

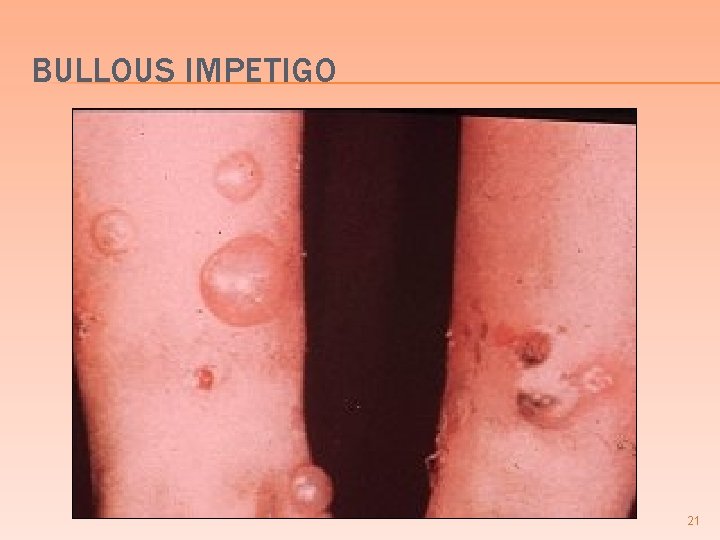
3) BULLOUS IMPETIGO � More localized & milder than scalded skin syndrome � Young children � Large friable clear to cloudy bulla honey yellow crusts � (+) Nikolsky sign � S. aureus can be recovered from lesions 20

BULLOUS IMPETIGO 21

4) STAPHYLOCOCCAL FOOD POISONING 22

STAPHYLOCOCCAL FOOD POISONING � Due to preformed heat-stable enterotoxin produced in foods prior to ingestion � Custard filled baked goods & processed meats � More common in summer months � Symptoms occur between 2 -6 hours after ingestion of contaminated food 23

STAPHYLOCOCCAL FOOD POISONING � Symptoms � nausea, begin abruptly vomiting, crampy abdominal pain, and diarrhea � Self limited � Culture food, not patient 24

STAPHYLOCOCCAL OSTEOMYELITIS 25

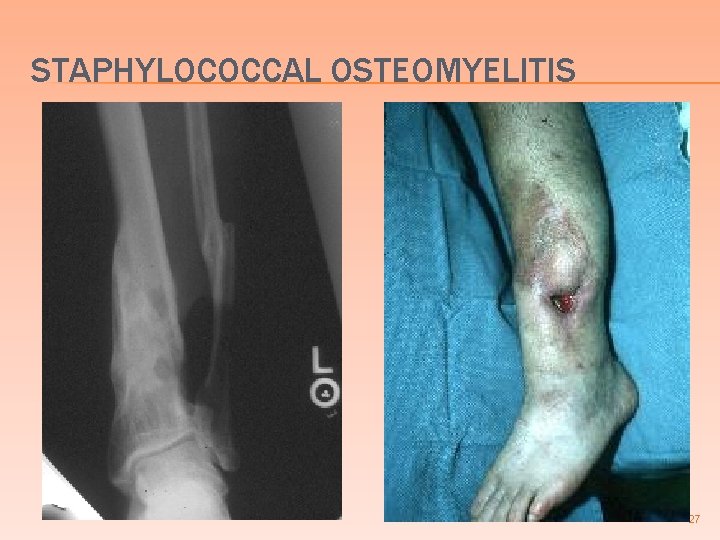
STAPHYLOCOCCAL OSTEOMYELITIS S. aureus the most common cause of osteomyelitis � Usually secondary to hematogenous spread to bone � � less commonly due to trauma (open fx) or extension from adjacent infected tissue Acute osteomyelitis may be cured by antibiotics alone � Chronic osteomyelitis requires surgical debridement of infected bone + antibiotics � 26

STAPHYLOCOCCAL OSTEOMYELITIS 27

CUTANEOUS STAPHYLOCOCCAL INFECTIONS 28

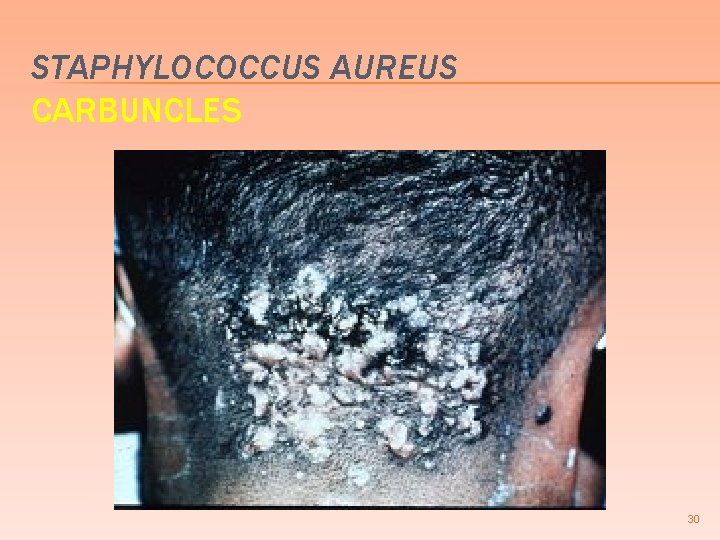
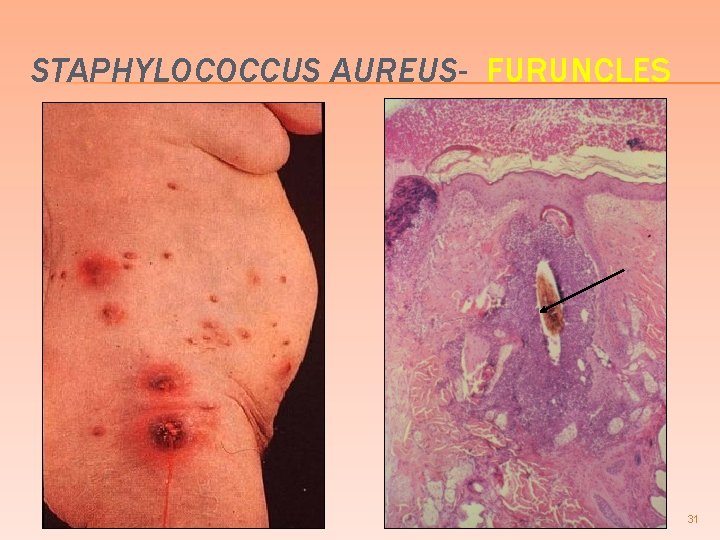
CUTANEOUS INFECTIONS DUE TO STAPHYLOCOCCUS AUREUS Bullous impetigo & scalded skin synd � Furuncles (boils) � � � deep infection of a single hair follicle Carbuncles � deep infection of a group of contiguous hair follicles Suppurative hidradenitis abscesses apocrine glands � Infection of the nail bed � Post-operative suture or wound abscess � Post-partum breast abscess � 29

STAPHYLOCOCCUS AUREUS CARBUNCLES 30

STAPHYLOCOCCUS AUREUS- FURUNCLES 31

STAPHYLOCOCCAL ENDOCARDITIS 32

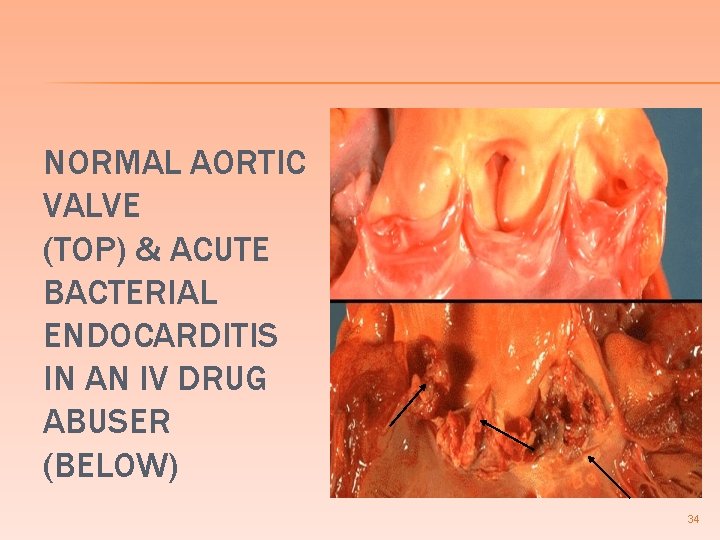
STAPH. AUREUS ENDOCARDITIS Staph. aureus is the most common cause of acute infective endocarditis in IV drug abusers � Infects normal and abnormal valves � Involves tricuspid valve in 50% of cases � Mortality is high in left-sided (mitral) endocarditis and low in right-sided (tricuspid or pulmonary) endocarditis � 33

NORMAL AORTIC VALVE (TOP) & ACUTE BACTERIAL ENDOCARDITIS IN AN IV DRUG ABUSER (BELOW) 34

RX OF STAPHYLOCOCCUS AUREUS INFECTIONS � 90% of hospital and community strains of S. aureus are resistant to penicillin due to production of -lactamase � MRSA (methicillin resistant S. aureus) � resistant to all beta-lactam antibiotics and to cephalosporins � treat with vancomycin 35

RX OF STAPHYLOCOCCUS AUREUS INFECTIONS � Vancomycin-resistant Staphylococcus aureus � Associated with transfer of resistance from enterococci � Treat with Synercid I. V. 36

STREPTOCOCCAL INFECTIONS 37

STREPTOCOCCAL IMPETIGO 38

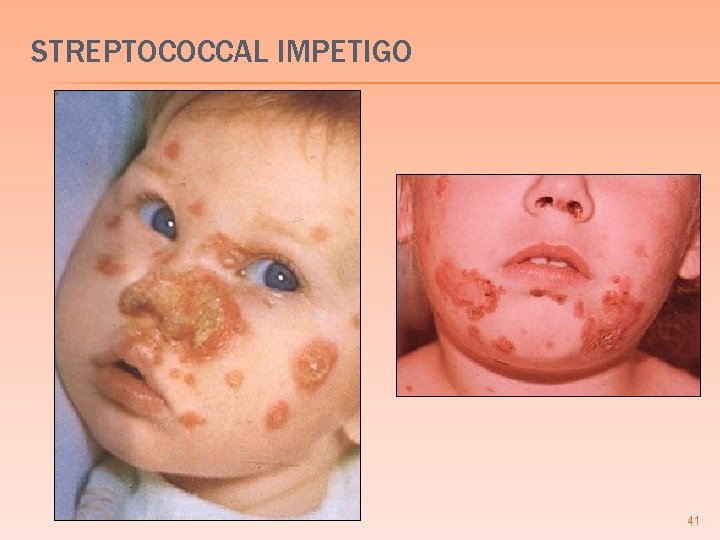
STREPTOCOCCAL IMPETIGO � Strep. � pyogenes most common cause of impetigo � Young children � Begins on face spreads to limbs � Erythematous macules vesicles & pustules honey colored crusts � Similar presentation as S. aureus � different from S. aureus � S. aureus; more likely to see bulla & + Nikolsky sign 39

STREPTOCOCCAL IMPETIGO � Highly contagious � avoid � Topical contact w/ other children antibiotics for localized infection � bacitracin, � Systemic mupirocin antibiotics for more generalized infection � penicillin, erythromycin, dicloxacillin 40

STREPTOCOCCAL IMPETIGO 41

STREPTOCOCCUS PYOGENES � Group A Beta-hemolytic � Most common cause of bacterial tonsillopharyngitis � Erythrogenic toxin � phage mediated � pyrogenic & cytotoxic � Also causes cellulitis, necrotizing fasciitis, streptococcal toxic shock syndrome, puerperal sepsis and endometritis 42

STREPTOCOCCAL CELLULITIS 43

PE; Labs: Temperature 39. 4; pulse 120; respirations 12; BP 130/80. Extremities: erythematous right leg, swollen and tender WBC 21, 000 (↑) with 80% neutrophils (↑) 44

CELLULITIS Infection of the subcutaneous tissue � Etiology � most commonly Strep. pyogenes & Staph. aureus � traumatic disruption of skin � +/- spontaneously (without obvious disruption) in very young elderly or immunocompromised patients � Strep. pyogens produces hyaluronidase, liquefies tissue, more likely to have diffuse spread rather than abscess formation � 45

STREPTOCOCCAL CELLULITIS � Clinical Area is acutely red, hot & tender/painful � leading edge is not raised but may be well defined � Rapid propagation centripetal from traumatic lesion � +/- lymphangitis lymphadenopathy � +/- desquamation of skin � � Tx; Erythromycin, cephalosporins, amoxicillin/clavulanate, azithromycin, clarithromycin, clindamycin 46

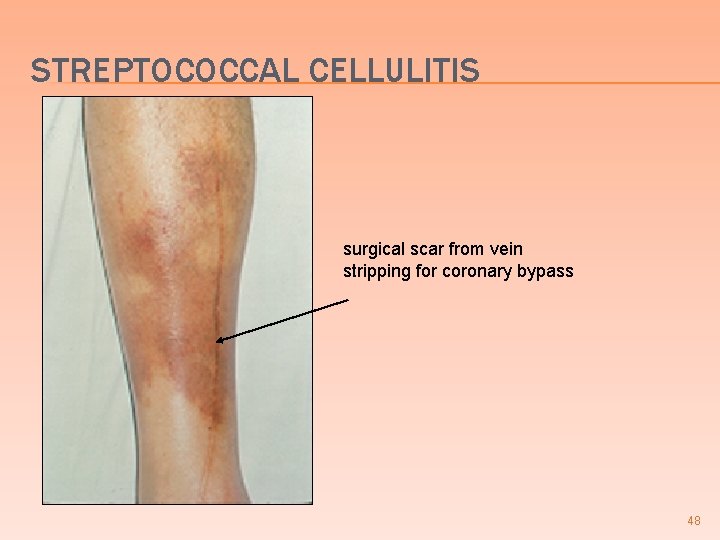
INFECTIOUS DISEASE PEARLS Recurrent streptococcal leg cellulitis may occur in patients after coronary bypass surgery if the saphenous vein was removed � Parenteral drug abusers have an increased risk of streptococcal cellulitis often associated with bacteremia, endocarditis, or septic thrombophlebitis � Patients with impaired lymphatic drainage may have recurrent cellulitis � Cellulitis of the foot or leg often co-exists with osteomyelitis in immunocompromised patients or diabetics � 47

STREPTOCOCCAL CELLULITIS surgical scar from vein stripping for coronary bypass 48

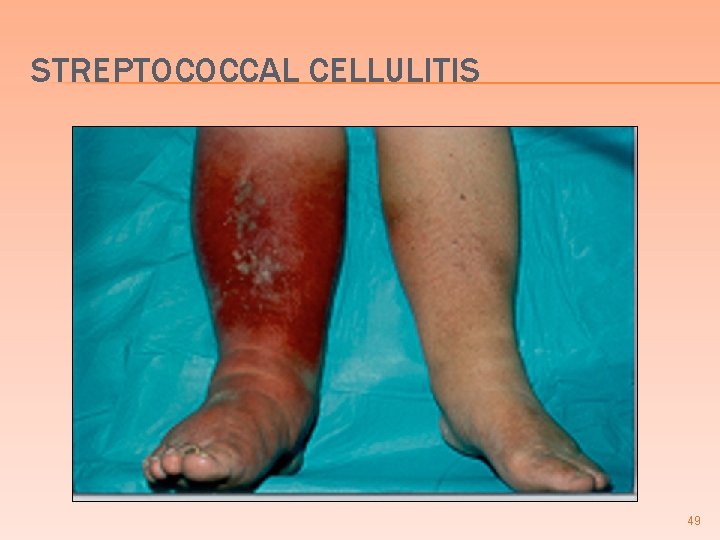
STREPTOCOCCAL CELLULITIS 49

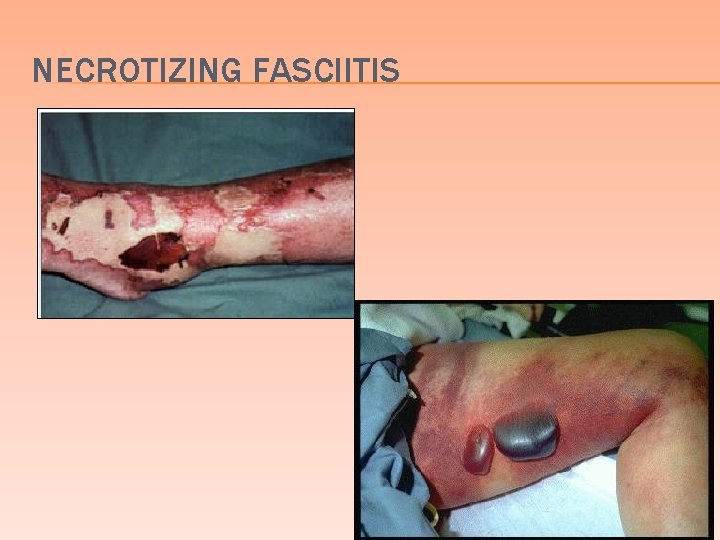
NECROTIZING FASCIITIS 50

NECROTIZING FASCIITIS �A life threatening infection � Involves deep soft (SQ) tissue, muscle and fascia � Develops at sites of wounds � Perineal infection in post partum diabetic & immunocompromised women (Fournier’s gangrene) � rarely healthy women 51

NECROTIZING FASCIITIS � Clinical � Severely painful cellulitis that may become bullous and/or gangrenous � Initially, the pain may be out of proportion to the severity of the cellulitis � Pure Streptococcal infection, � exudate is odorless, without gas � Mixed infections, streptococci + anaerobes + enterobacteriaceae � foul smelling exudate with gas 52

NECROTIZING FASCIITIS 53

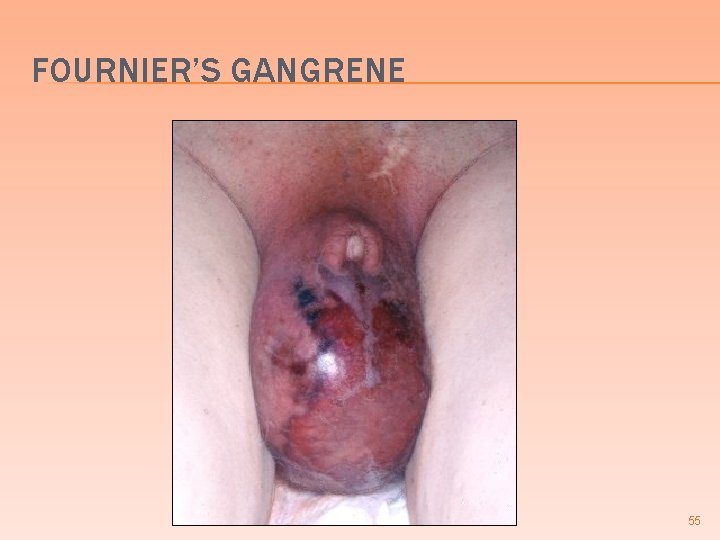
FOURNIER’S GANGRENE �A special case of necrotizing fasciitis involving the male or female genitalia � Usually associated with an underlying condition such as diabetes mellitus or immune compromised patients � Often involves mixed infections w/ Gram (+) and Gram (-), aerobic and anaerobic acting synergistically 54

FOURNIER’S GANGRENE 55

TREATMENT OF NECROTIZING FASCIITIS � Early surgical exploration and extensive debridement + antibiotics 56

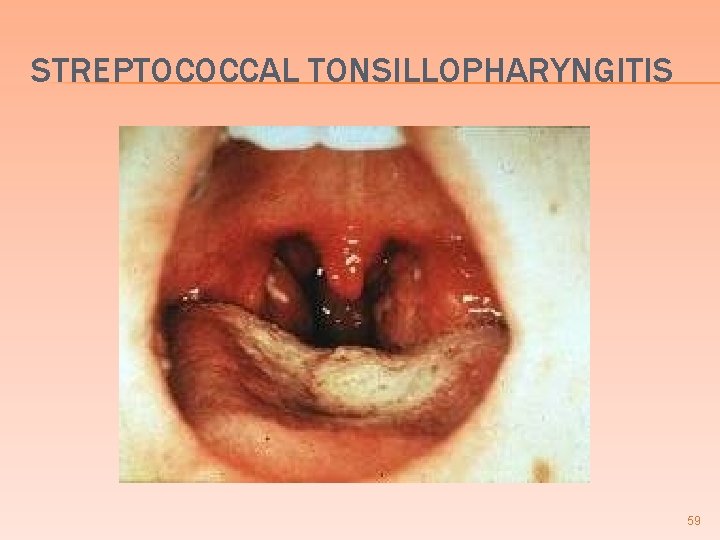
STREPTOCOCCUS PYOGENES TONSILLOPHARYNGITIS � MOST COMMON CAUSE of bacterial tonsillopharyngitis � Erythrogenic (scarletinal) toxin is elaborated by some strains of group A strep. infected by a temperate bacteriophage � Most frequently seen in children from 515 years of age 57

STREPTOCOCCUS PYOGENES TONSILLOPHARYNGITIS � Clinical � (can also be seen w/ Staph. ) Red swollen tonsils, severely painful � Increased � +/- # follicles Peritonsillar abscess � peritonsillar abscess will deviate the uvula away from the involved tonsil � +/- Ludwig’s angina � diffuse suppurative inflammation of SQ tissue of pharynx, gingiva, & neck 58

STREPTOCOCCAL TONSILLOPHARYNGITIS 59

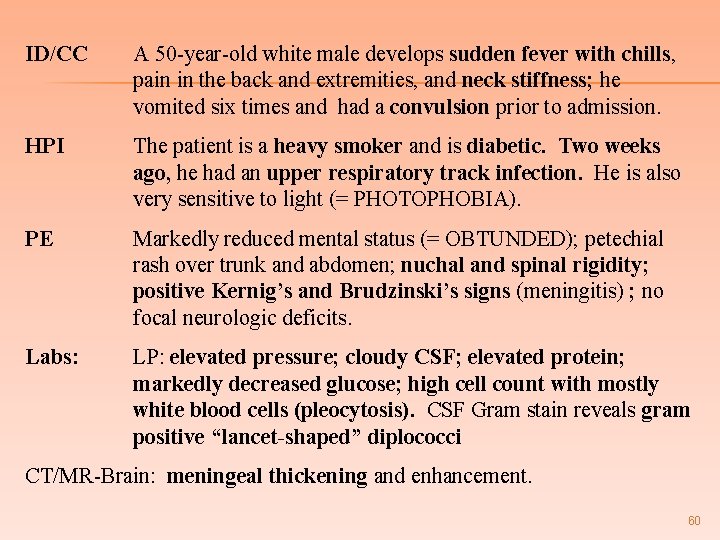
ID/CC A 50 -year-old white male develops sudden fever with chills, pain in the back and extremities, and neck stiffness; he vomited six times and had a convulsion prior to admission. HPI The patient is a heavy smoker and is diabetic. Two weeks ago, he had an upper respiratory track infection. He is also very sensitive to light (= PHOTOPHOBIA). PE Markedly reduced mental status (= OBTUNDED); petechial rash over trunk and abdomen; nuchal and spinal rigidity; positive Kernig’s and Brudzinski’s signs (meningitis) ; no focal neurologic deficits. Labs: LP: elevated pressure; cloudy CSF; elevated protein; markedly decreased glucose; high cell count with mostly white blood cells (pleocytosis). CSF Gram stain reveals gram positive “lancet-shaped” diplococci CT/MR-Brain: meningeal thickening and enhancement. 60

STREPTOCOCCAL MENINGITIS 61

STREPTOCOCCUS PNEUMONIAE Common cause of suppurative meningitis in children � r/o N. meningitidis � Most common cause of community-acquired bacterial pneumonia � > 20 years-old � empyema is the most common complication � Most common cause of otitis media, purulent sinusitis, and mastoiditis � Second most common cause of acute epiglottiditis 62

STREPTOCOCCUS PNEUMONIAE PEARLS � Pneumococcal meningitis is associated with sinusitis, otitis media, skull fractures, and CSF leaks � Pneumococcal endocarditis may result as a complication of pneumococcal meningitis � CSF in pneumococcal meningitis may have a greenish tint 63

� ID/CC � HPI few � PE A 35 year old woman complains of fever and pain in the face and upper teeth, especially upon leaning forward She has had a chronic cough for the past months as well as nasal congestion and discharge Fever. Halitosis; greenish-yellow postnasal discharge; bilateral boggy nasal mucosa; bilateral percussion tenderness and erythema over zygomatic arch; clouding of sinuses by transillumination; dental and cranial nerve exams normal 64

ACUTE SINUSITIS � DDX; � Streptococcus pneumoniae � Hemophilus influenzae � Moraxella catarrhalis 65

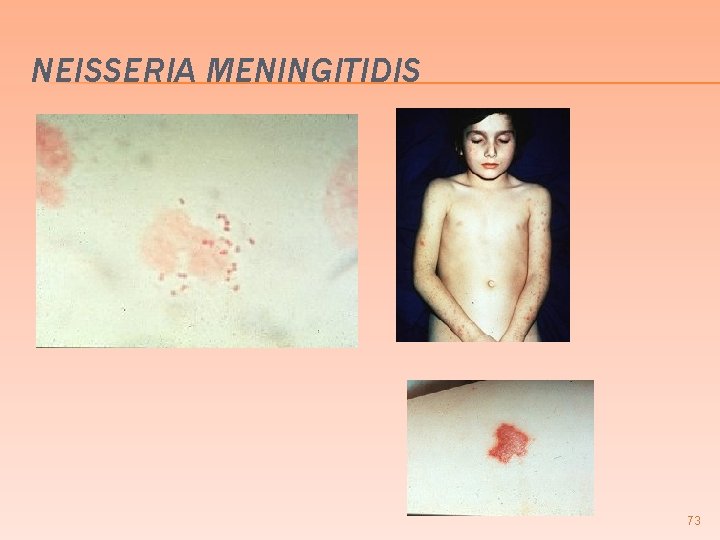
MENINGOCOCCEMIA NEISSERIA MENINGITIDIS 66

MENINGOCOCCEMIA NEISSERIA MENINGITIDIS Gram (-) diplococcus � Suppurative meningitis (+) Burdinski and Kernig signs � Small vessel vasculitis, capillary thrombosis & petechial hemorrhages purpura � Fulminating rapidly progressive septicemia with fever vascular collapse and DIC � induction of TNF & IL 1 & 6 cause the hypotension and vascular collapse � 67

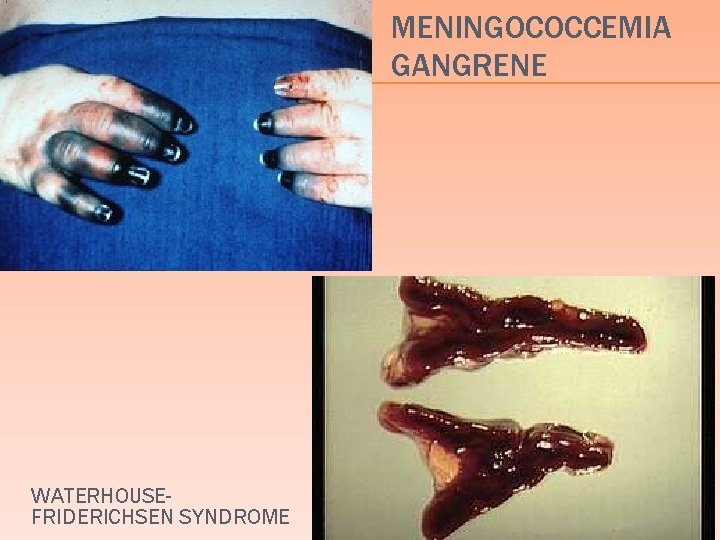
MENINGOCOCCEMIA NEISSERIA MENINGITIDIS � +/- Waterhouse-Friderichsen syndrome � overwhelming bacterial infection � most commonly N. meningitidis rapidly progressive hypotension � DIC & purpura � bilateral adrenal cortical hemorrhage � � insufficiency � +/- Purpura Fulminans � a catastrophic febrile illness with initial hemorrhagic skin lesions that progress to gangrene 68

MENINGOCOCCEMIA NEISSERIA MENINGITIDIS � N. meningitidis is the most common cause of suppurative meningitis in patients 1 -18 yrsold � particularly common in crowded conditions (dormitories, boot camps) 69

MENINGOCOCCEMIA NEISSERIA MENINGITIDIS � Clinical severity is measured by how rapidly naturally occurring anticoagulants (protein C and S) are depleted, the degree of thrombocytopenia, and the presence of fibrin split products � High levels of TNF- and IFN- are associated with a poor prognosis 70

MENINGOCOCCEMIA NEISSERIA MENINGITIDIS � Patients with deficiency of properdin (serum protein kills bacteria) and ineffective alternative complement pathway (both sexlinked) have a very high risk of fulminant meningococcemia � Tx: Penicillin G � Treat family/contacts with Rifampin � vaccinate contacts > 2 yrs-old 71

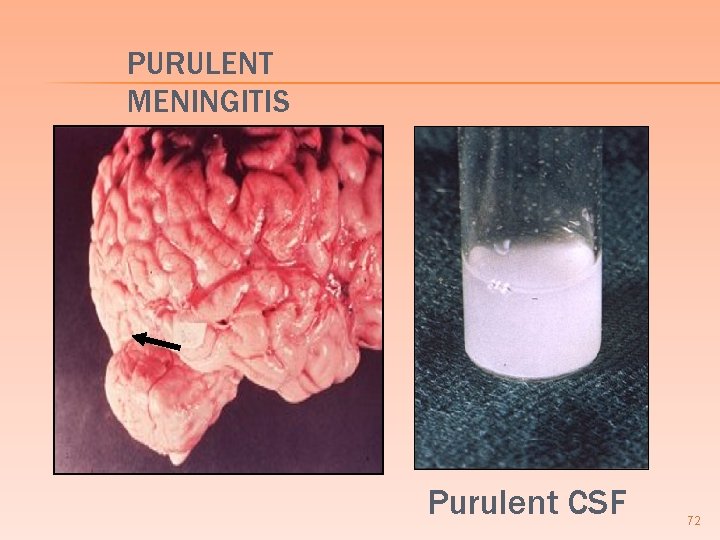
PURULENT MENINGITIS Purulent CSF 72

NEISSERIA MENINGITIDIS 73

MENINGOCOCCEMIA GANGRENE WATERHOUSEFRIDERICHSEN SYNDROME 74

NEISSERIA GONORRHEA 75

NEISSERIA. GONORRHEA � Women more likely to be asymptomatic carriers than men � Men more likely to transmit the disease than women after each sexual exposure � Purulent penile discharge (urethritis) 2 -5 d. after exposure � Cervicitis (cervical discharge) most common site in women +/- urethritis, Bartholins gland abscess, PID (10 -20 % of untreated women) � fever, pain subpubic region 76

NEISSERIA. GONORRHEA � R/O Chlamydia trichomatis � Gram stain urethral exudate/cervical smear � intracellular organism are diagnostic 77

NEISSERIA. GONORRHEA � Conjunctivitis in neonates (ophthalmia neonatorum) � bilateral � develops 2 -5 days old � r/o �Chlamydia trichomatis � develops 5 -7 days old � most common cause �S. aureus usually unilateral 78

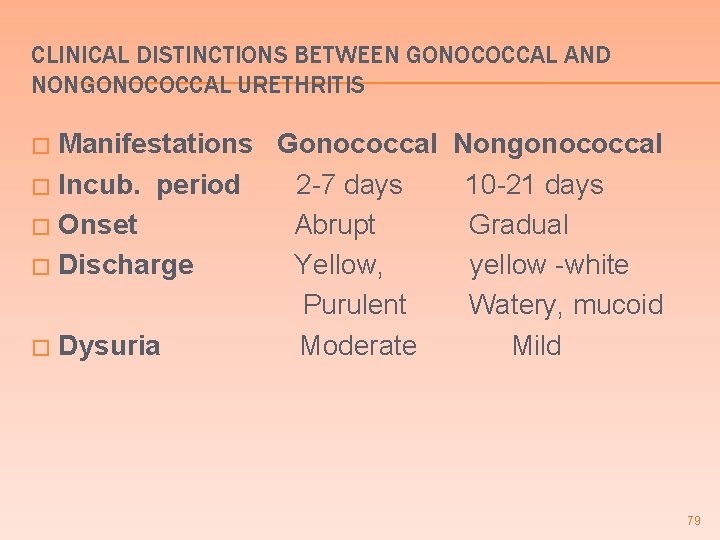
CLINICAL DISTINCTIONS BETWEEN GONOCOCCAL AND NONGONOCOCCAL URETHRITIS Manifestations Gonococcal Nongonococcal � Incub. period 2 -7 days 10 -21 days � Onset Abrupt Gradual � Discharge Yellow, yellow -white Purulent Watery, mucoid � Dysuria Moderate Mild � 79

NEISSERIA. GONORRHEA � Tx � All patients with gonorrhea should be treated simultaneously for chlamydia � ceftriaxone (gonorrhea) & doxycycline (Chlamydia) 80

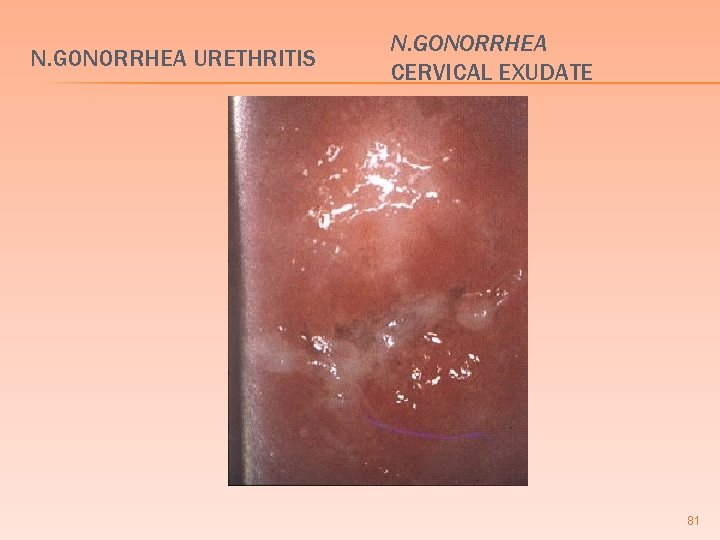
N. GONORRHEA URETHRITIS N. GONORRHEA CERVICAL EXUDATE 81

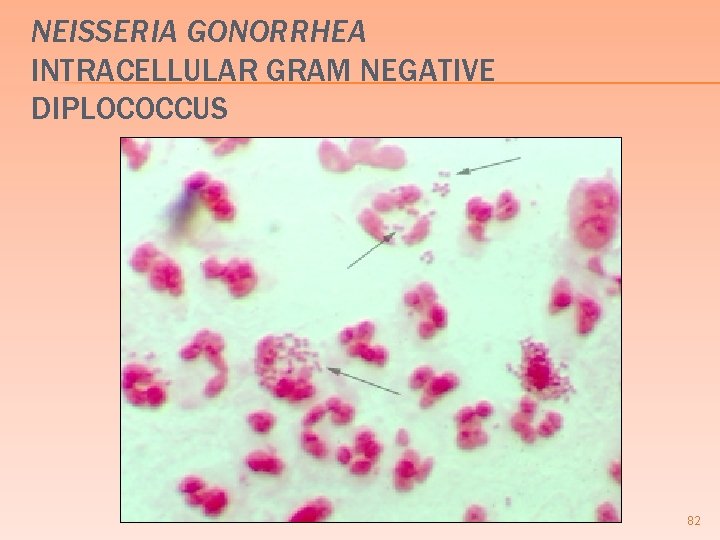
NEISSERIA GONORRHEA INTRACELLULAR GRAM NEGATIVE DIPLOCOCCUS 82

ID/CC: A 27 -year-old male is admitted to the hospital for evaluation of increasing fever of unknown origin along with malaise, headache, sore throat, cough, and constipation. HPI: He visited Southeast Asia three weeks ago but did not receive any prior vaccinations. PE: Bradycardia; fever charting reveals “stepladder” pattern. mild hepatosplenomegaly; faint erythematous macules seen over trunk (= “ROSE SPOTS”). Labs: CBC: neutropenia with relative lymphocytosis. Widal’s test positive in significant titers; blood and stool cultures reveal a non-lactose fermenting gram negative motile rods. 83

SALMONELLA TYPHI TYPHOID FEVER 84

SALMONELLA TYPHI TYPHOID FEVER Gram (-) rod, non-lactose fermenting, motile � Acquired by ingesting contaminated food or water � Carrier state: in gallbladder (up to 1 year) � DX: Blood culture (first week); stool and urine in third to fourth week � Widal’s test; agglutination test for S. typhi antibodies � � Vi antigens more sensitive & specific Only Salmonella w/ human reservoirs � RX: Fluoroquinolone; Ciprofloxacin � 85

SALMONELLA TYPHI TYPHOID FEVER � First week of infection � � Fever, malaise, constipation, & abdominal pain; positive blood cultures Second week of infection Sustained bacteremia, abdominal pain, diarrhea w/ occult blood, (+) stool culture � Rose spots; few 2 -4 mm erythmatous papules most common upper abdomen lower thorax, fade 2 -3 days � Hepatosplenomegaly, Absolute neutropenia, Bradycardia � “classic triad” � � Third week of infection; melena, ileus 86

SALMONELLOSIS � Four species: S. typhi, S. enteritidis, S. choleraesuis, and S. typhimurium � Diabetes predisposes to salmonella enteritis due to loss of gastric acidity and poor bowel motility � Septicemia can produce osteomyelitis � Second most common cause of osteomyelitis in sickle cell patients 87

SALMONELLA FOOD POISONING One of the most common causes of food poisoning � S. enteritidis, S. choleraesuis, and S. typhimurium � Fever, vomiting, diarrhea, abdominal pain � 8 -48 hours incubation � Self-limited diarrhea lasting 7 -10 days � Carried in nature by animal reservoirs � � � chickens, turtles, cattle, pigs, sheep, lizards, iguanas, snakes Any condition with hypochlorhydria predisposes to infection 88