Pulmonary Thromboembolism 11162011 HPI 17 yo female developed

Pulmonary Thromboembolism 11_16_2011

HPI • 17 yo female developed shortness of breath while doing a mild run at school • O 2 sat 91% in nurse’s office – Sent to ED – Sat drops to 83% while running in place • ROS: – No cough, fever, wheeze, syncope, hemoptysis, chest pain – Completely negative • PMH: Hemolytic anemia as a child requiring blood transfusions until splenectomy

ED • Normal CXR, nl EKG • CT scan to evaluate for pulmonary embolus – negative • D-dimer – high normal – cannot rule out PE, but low probability

? ? ? • Why is she hypoxic? – No signs of V/Q mismatch – Shunt? • O 2 increases when she is given supplemental O 2 – This can be seen in hepatopuolmonary syndrome but she has no liver disease – Diffusion abnormality? • No evidence of pulmonary hypertension on echo – Negative cardiac workup including negative bubble study – Spirometry normal – Methemoglobin negative

Labs • • Hct 29. 1 ESR/CRP nl Negative hypercoag panel Ig. G to aspergillus elevated
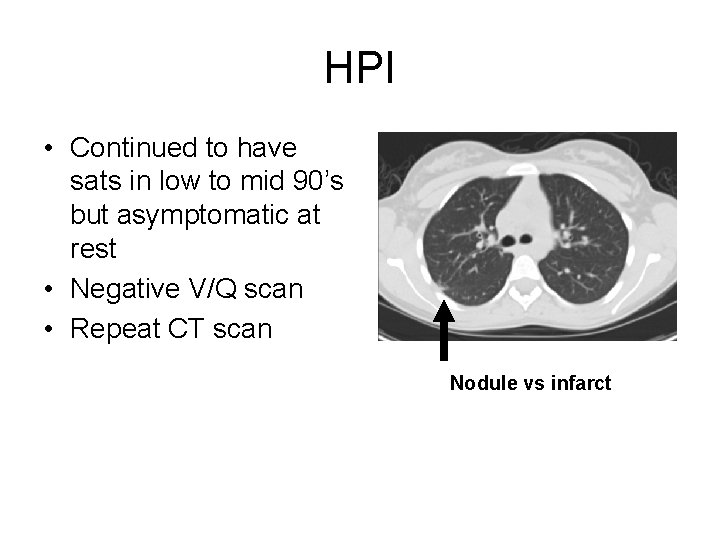
HPI • Continued to have sats in low to mid 90’s but asymptomatic at rest • Negative V/Q scan • Repeat CT scan Nodule vs infarct

What to do • 17 yo with hypoxia at rest who significantly desaturates with very mild exercise • Labs and physical examination unremarkable • Question of lung nodule on CT scan
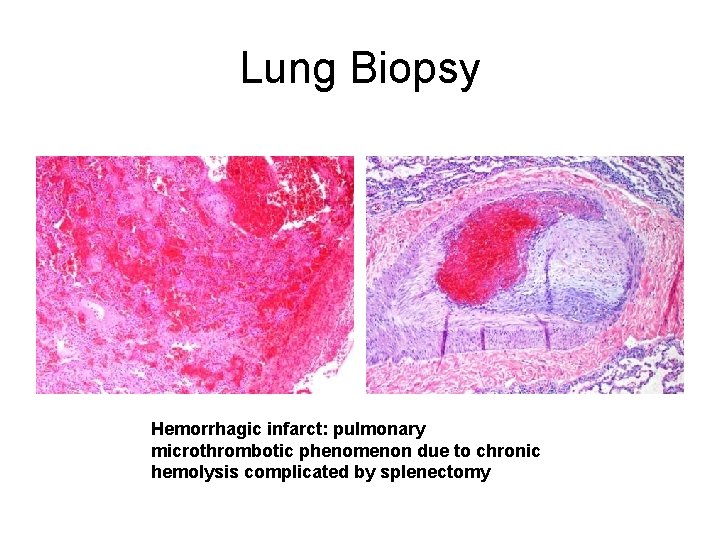
Lung Biopsy Hemorrhagic infarct: pulmonary microthrombotic phenomenon due to chronic hemolysis complicated by splenectomy

• Treated with lovenox and sats improved to 9798% • Chronic hemolysis causing micro thromboemboli which led to decreased diffusion and dec. sats. • Since lovenox helped, pt must have been continuously showering her lungs with thromboemboli… • Has subsequently been placed on coumadin and is doing well.
- Slides: 9