Pulmonary Separation and Differential Lung Ventilation in Management
- Slides: 1

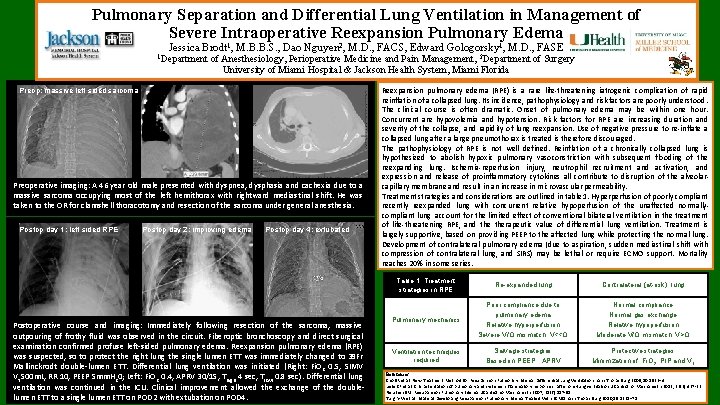
Pulmonary Separation and Differential Lung Ventilation in Management of Severe Intraoperative Reexpansion Pulmonary Edema Jessica Brodt 1, M. B. B. S. , Dao Nguyen 2, M. D. , FACS, Edward Gologorsky 1, M. D. , FASE 1 Department of Anesthesiology, Perioperative Medicine and Pain Management, 2 Department of Surgery University of Miami Hospital & Jackson Health System, Miami Florida Preop: massive left sided sarcoma Preoperative imaging: A 46 year old male presented with dyspnea, dysphasia and cachexia due to a massive sarcoma occupying most of the left hemithorax with rightward mediastinal shift. He was taken to the OR for clamshell thoracotomy and resection of the sarcoma under general anesthesia. Postop day 1: left sided RPE Postop day 2: improving edema Postop day 4: extubated Postoperative course and imaging: Immediately following resection of the sarcoma, massive outpouring of frothy fluid was observed in the circuit. Fiberoptic bronchoscopy and direct surgical examination confirmed profuse left-sided pulmonary edema. Reexpansion pulmonary edema (RPE) was suspected, so to protect the right lung the single lumen ETT was immediately changed to 39 Fr Mallinckrodt double-lumen ETT. Differential lung ventilation was initiated (Right: Fi. O 2 0. 5, SIMV VT 500 m. L, RR 10, PEEP 5 mm. H 20; Left: Fi. O 2 0. 4, APRV 30/15, Thigh 4 sec, Tlow 0. 8 sec). Differential lung ventilation was continued in the ICU. Clinical improvement allowed the exchange of the doublelumen ETT to a single lumen ETT on POD 2 with extubation on POD 4. Reexpansion pulmonary edema (RPE) is a rare life-threatening iatrogenic complication of rapid reinflation of a collapsed lung. Its incidence, pathophysiology and risk factors are poorly understood. The clinical course is often dramatic. Onset of pulmonary edema may be within one hour. Concurrent are hypovolemia and hypotension. Risk factors for RPE are increasing duration and severity of the collapse, and rapidity of lung reexpansion. Use of negative pressure to re-inflate a collapsed lung after a large pneumothorax is treated is therefore discouraged. The pathophysiology of RPE is not well defined. Reinflation of a chronically collapsed lung is hypothesized to abolish hypoxic pulmonary vasoconstriction with subsequent flooding of the reexpanding lung. Ischemia-reperfusion injury, neutrophil recruitment and activation, and expression and release of proinflammatory cytokines all contribute to disruption of the alveolarcapillary membrane and result in an increase in microvascular permeability. Treatment strategies and considerations are outlined in table 1. Hyperperfusion of poorly compliant recently reexpanded lung with concurrent relative hypoperfusion of the unaffected normallycompliant lung account for the limited effect of conventional bilateral ventilation in the treatment of life-threatening RPE, and therapeutic value of differential lung ventilation. Treatment is largely supportive, based on providing PEEP to the affected lung while protecting the normal lung. Development of contralateral pulmonary edema (due to aspiration, sudden mediastinal shift with compression of contralateral lung, and SIRS) may be lethal or require ECMO support. Mortality reaches 20% in some series. Table 1: Treatment strategies in RPE Re-expanded lung Contralateral (at-risk) lung Pulmonary mechanics Poor compliance due to pulmonary edema Relative hyperperfusion Severe V/Q mismatch, V<<Q Normal compliance Normal gas exchange Relative hypoperfusion Moderate V/Q mismatch, V>Q Ventilation techniques required Salvage strategies Based on PEEP, APRV Protective strategies Minimization of Fi. O 2, PIP and VT References Cho SR et al. New Treatment Method for Reexpansion Pulmonary Edema: Differential Lung Ventilation. Ann Thorac Surg 2005; 80: 1933– 4 Leite CF et al. Characterization of pulmonary and systemic inflammatory responses…after one-lung ventilation. J Cardiothor Vasc Anesth 2012; 26(3): 427 -32 Neustein SM. Reexpansion Pulmonary Edema. J Cardiothor Vasc Anesth 2007; 21(6): 887 -91 Tung Y-W et al. Bilateral Developing Reexpansion Pulmonary Edema Treated With ECMO. Ann Thorac Surg 2010; 89: 1268– 71