Pulmonary Pathology I Lab November 25 2013 Pulmonary

Pulmonary Pathology I Lab November 25, 2013

Pulmonary Pathology I Case 1

Q 1 Describe the gross findings Normal Fresh, unfixed specimen
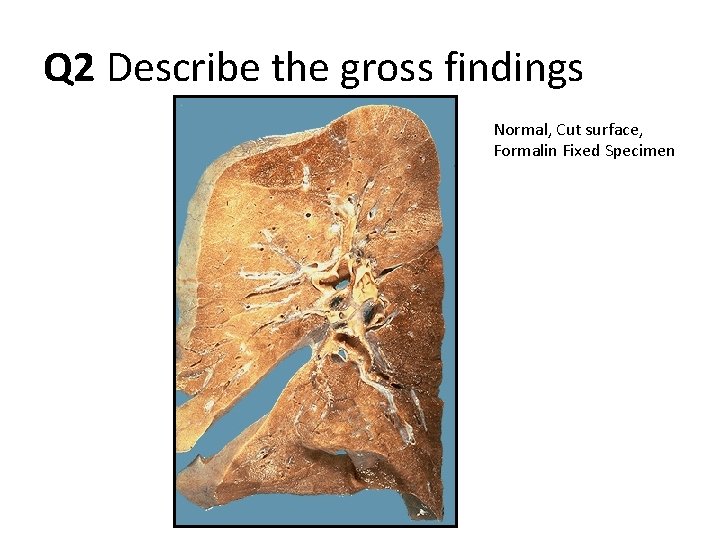
Q 2 Describe the gross findings Normal, Cut surface, Formalin Fixed Specimen
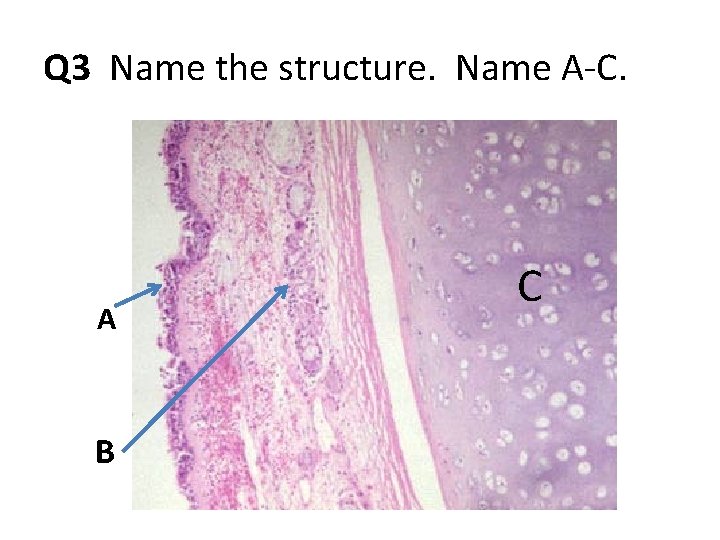
Q 3 Name the structure. Name A-C. A B C
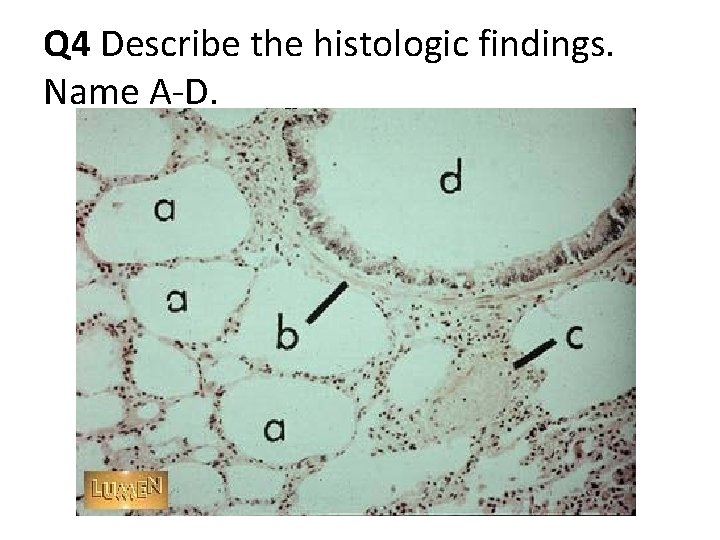
Q 4 Describe the histologic findings. Name A-D.
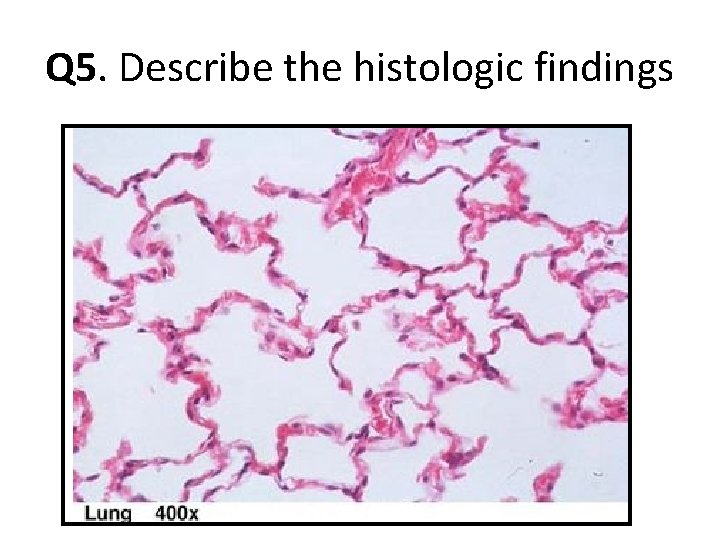
Q 5. Describe the histologic findings

Pulmonary Pathology 1 Case 2

Case History A 67 -year-old man presents with dyspnea. He also complains of cough, which is worse in the mornings, off and on for several years. There is no history of fever or purulent sputum or cyanosis. He smokes two packs of cigarettes/day for the last 50 years. On exam there is hyper-resonance of the chest by percussion and prolonged expiratory phase on auscultation.
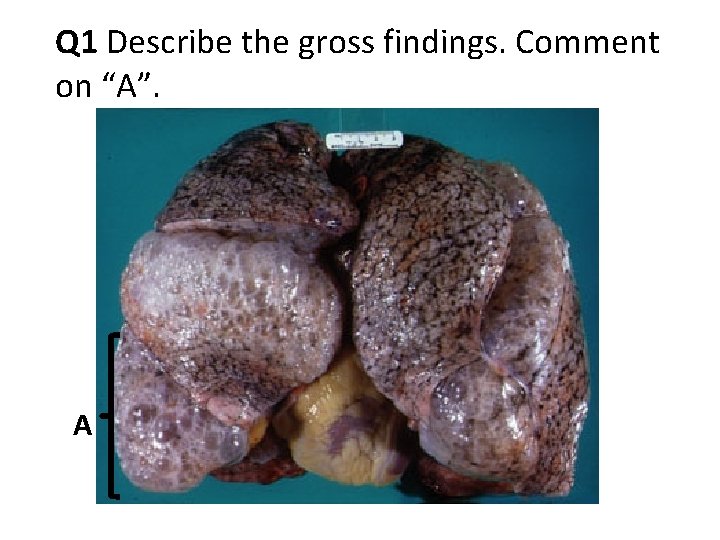
Q 1 Describe the gross findings. Comment on “A”. A
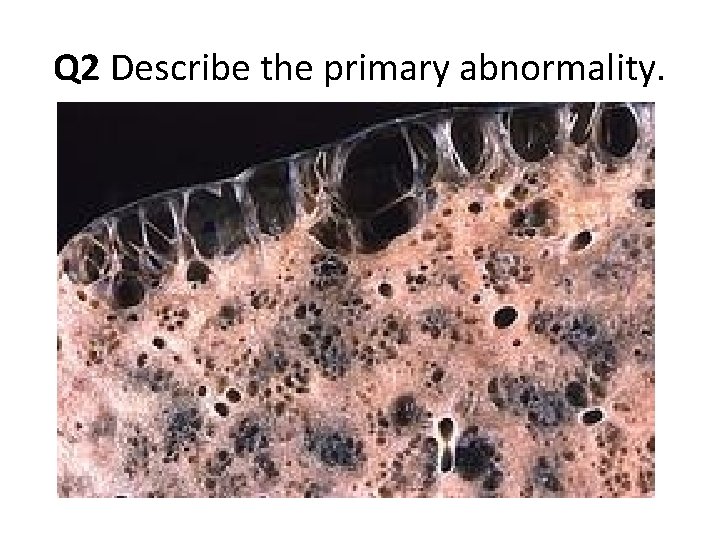
Q 2 Describe the primary abnormality.
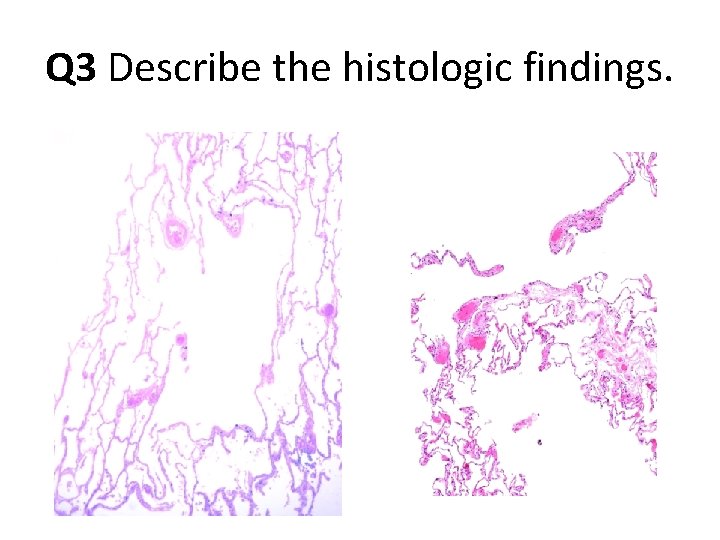
Q 3 Describe the histologic findings.
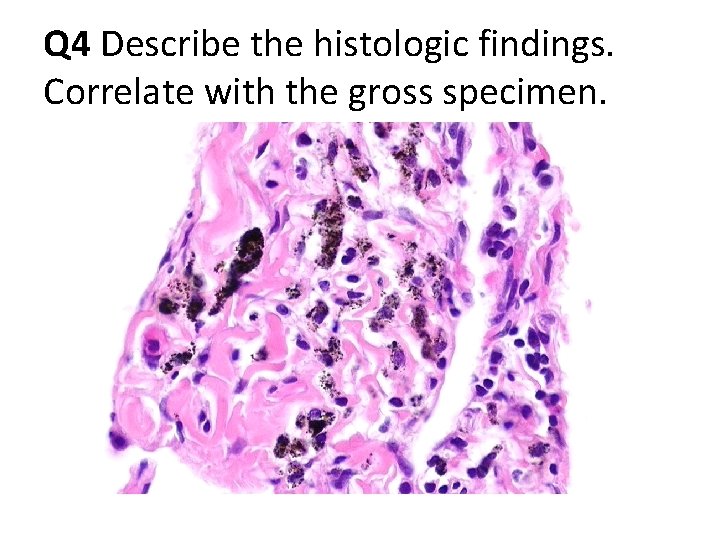
Q 4 Describe the histologic findings. Correlate with the gross specimen.

Q 5 What is your diagnosis? Q 6 What is the most common etiology of this disease process? Summarize the pathogenesis.

Q 7 What underlying genetic disorder(s) can contribute to the development of this disease process?
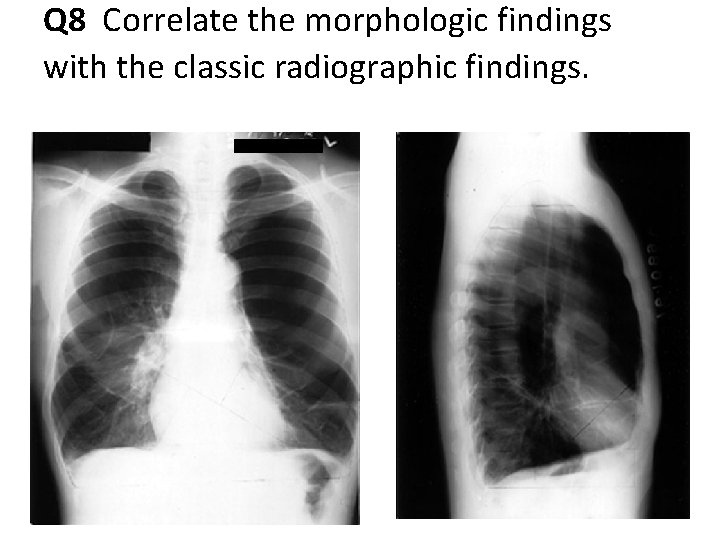
Q 8 Correlate the morphologic findings with the classic radiographic findings.

Pulmonary Pathology I Case 3

Case History A newborn develops respiratory insufficiency. He was born at 25 weeks gestation and weighed 500 gm at birth. The mother had fever for 3 days before delivery and the amniotic fluid was purulent. Surfactant and antibiotics were administered. The baby’s condition deteriorated rapidly and he died 8 hours later.
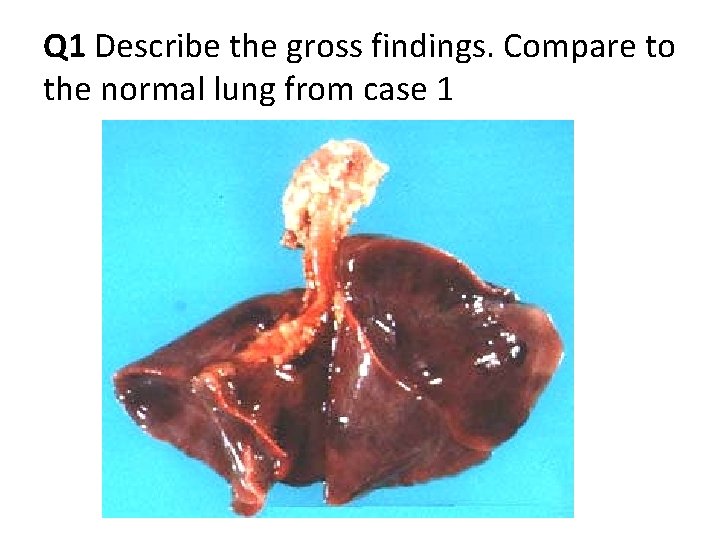
Q 1 Describe the gross findings. Compare to the normal lung from case 1
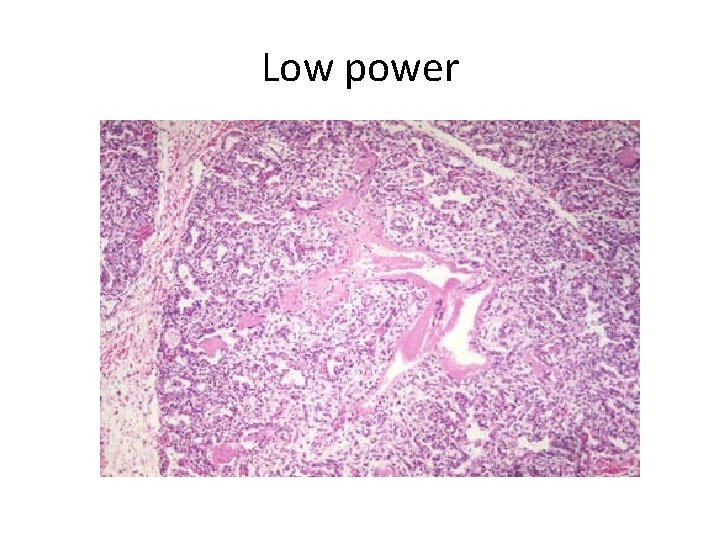
Low power
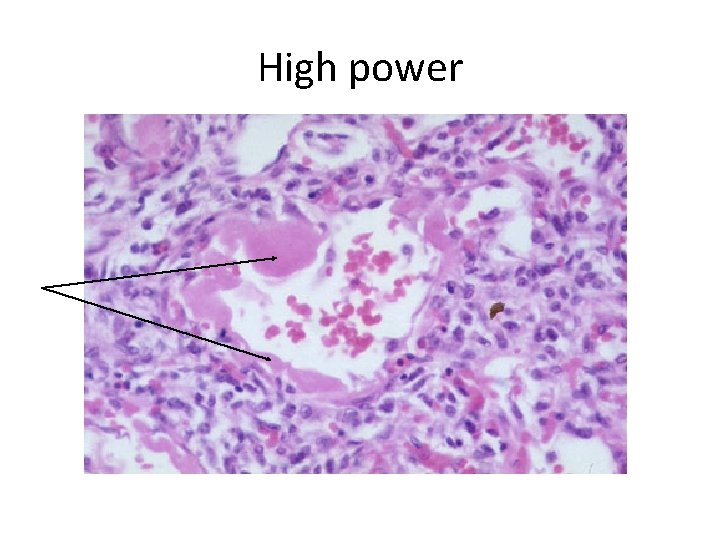
High power

Q 2 Describe the histologic findings. What is the structure highlighted by the arrows composed of? Q 3 Diagnosis? Q 4 Describe the pathogenesis of this disease process.

Q 5 Newborns who ultimately survive this disease process will have received high concentrations of ventilator-administered oxygen for prolonged periods: Name the two most common associated complications

Pulmonary Pathology 1 Case 4

Case History A 44 -year-old woman undergoing chemotherapy for metastatic ovarian cancer is admitted to the hospital with a severe infection and sepsis. Over the next 2 days she develops progressive dyspnea. She becomes hypoxic and cyanotic and requires increasing oxygen concentration. Chest X-ray shows diffuse bilateral infiltrates.
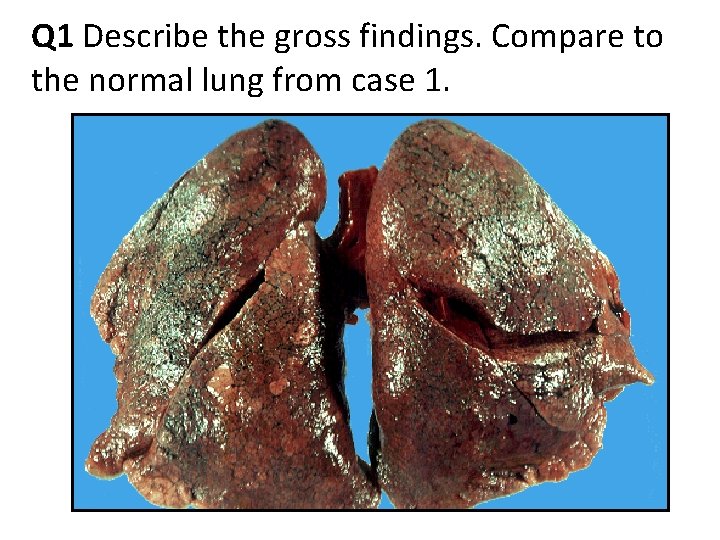
Q 1 Describe the gross findings. Compare to the normal lung from case 1.
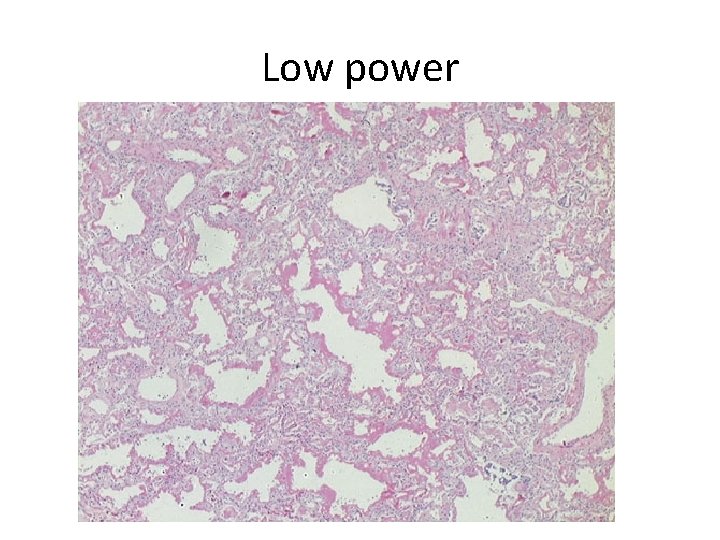
Low power
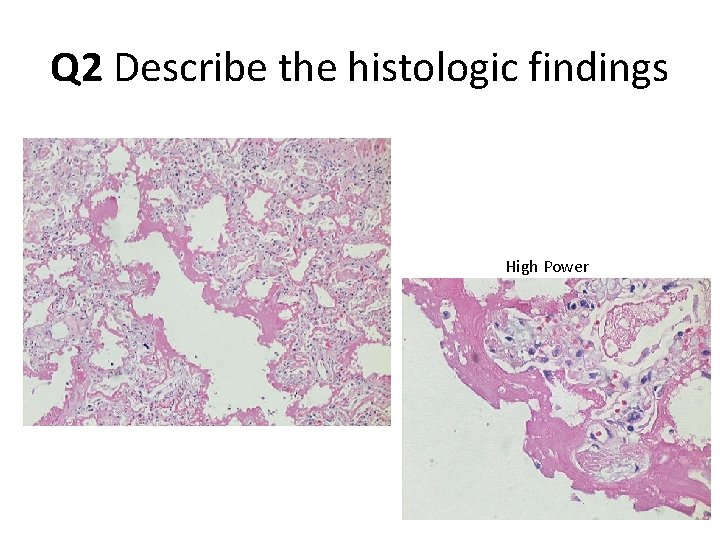
Q 2 Describe the histologic findings High Power

Q 3 Diagnosis? Q 4 List the most common etiologies of this condition. Q 5 Summarize the pathogenesis.

Pulmonary Pathology 1 Case 5

Case History A 56 year-old man develops progressive dyspnea over 6 -8 months. He denies fever, chest pain or hemoptysis. He has never smoked cigarettes. On physical exam he is hypoxemic. On chest auscultation there are fine bibasilar inspiratory crackles (sound like Velcro) Chest X-ray shows bilateral interstitial infiltrates with a peripheral distribution.
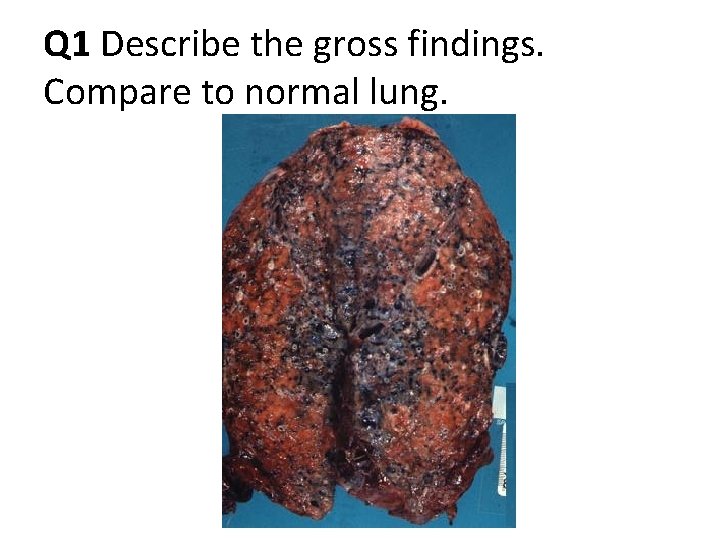
Q 1 Describe the gross findings. Compare to normal lung.
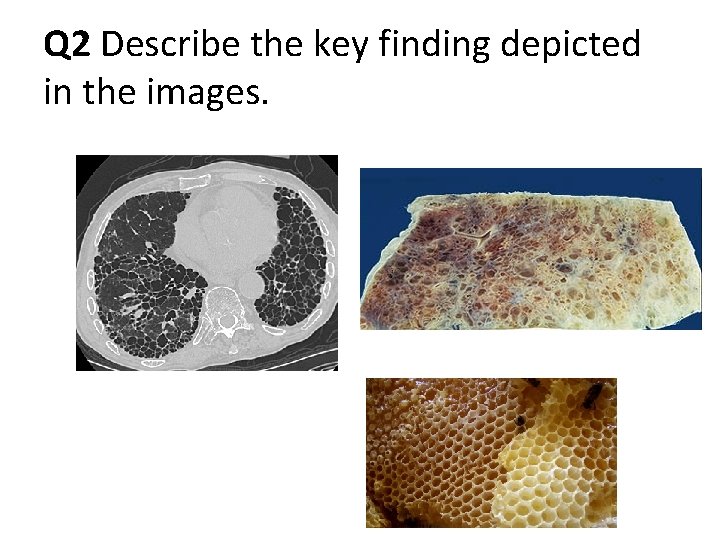
Q 2 Describe the key finding depicted in the images.
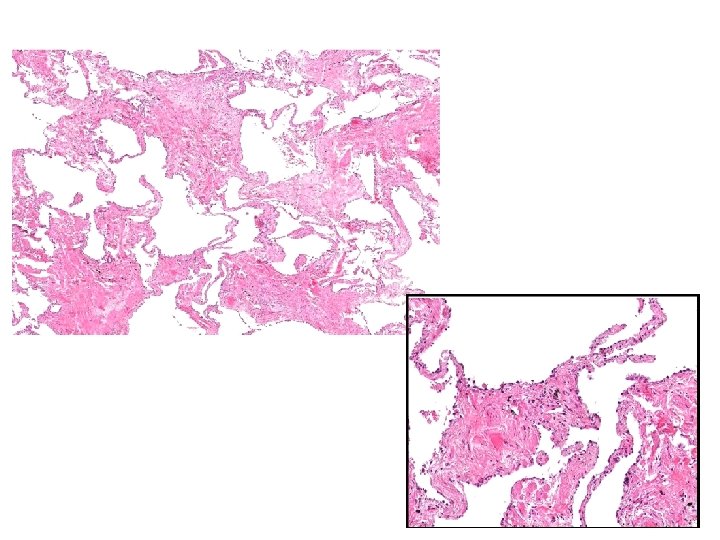

Q 3 Describe the histologic findings. Correlate the gross/radiographic images with the histology. Q 4 Diagnosis?

Q 5 List diseases that may result in this process.

Pulmonary Pathology 1 Case 6

Case History A 33 -year old African American woman is involved in a motor vehicle accident. She sustained minor chest and head trauma. The patient is healthy, works as a school-teacher, and has never smoked. She takes no prescription or over the counter medications. Physical exam is notable for a frontal head hematoma and is otherwise unremarkable. In the ED a head CT and chest-ray were performed.
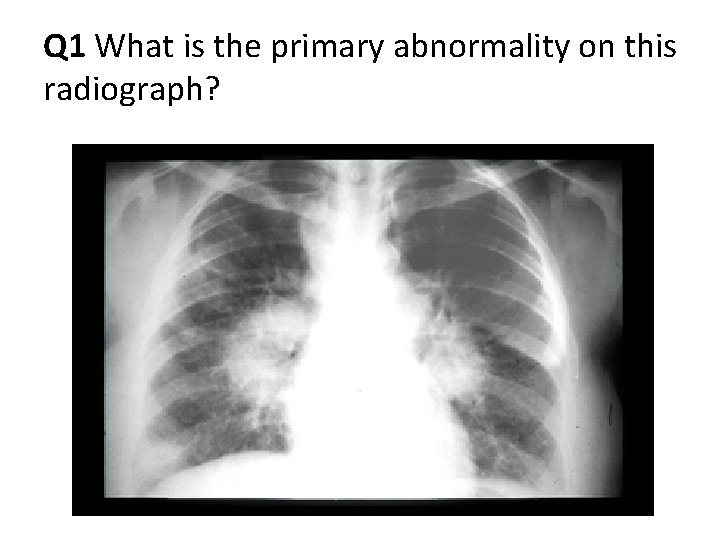
Q 1 What is the primary abnormality on this radiograph?
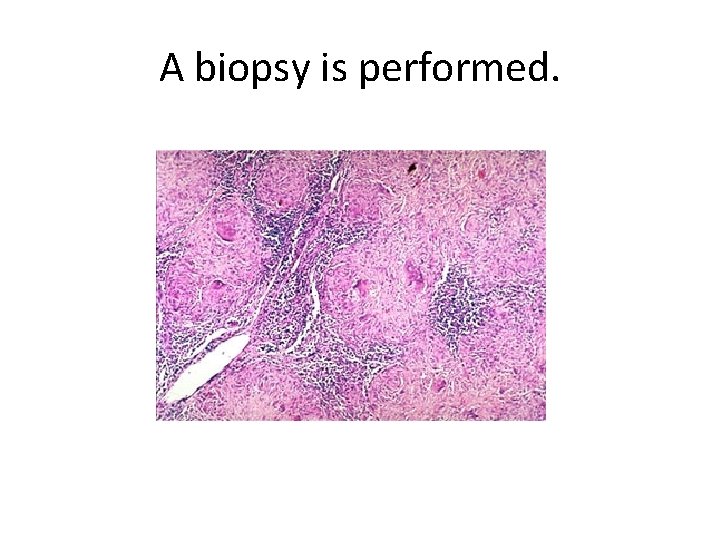
A biopsy is performed.
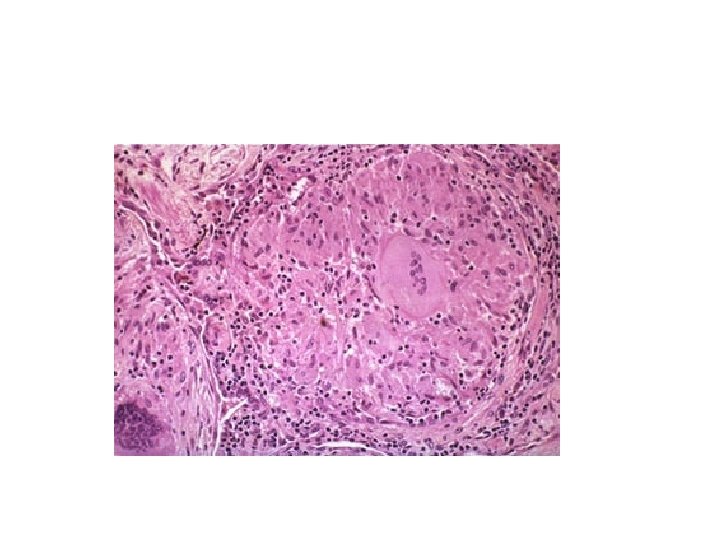

Q 3 Describe the histologic findings. Q 4 Are there any special stains that should be performed on the biopsied tissue before rendering a diagnosis?

Q 5 The stains ordered are negative. What is the most likely diagnosis? Q 6 Summarize the known or hypothesized elements of the pathophysiology of this disease process.

Q 7 Are there extrapulmonary/extrathoracic lesions in this disease process? If so, what organs are most commonly involved and what are the associated clinical manifestations?

End of Pulmonary Pathology I
- Slides: 45