Pulmonary Hypertension PH By Ahmad AlMasri Definition defined

Pulmonary Hypertension (PH) By: Ahmad Al-Masri

Definition • defined as mean pulmonary artery pressure of ≥ 25 mm. Hg at rest, as measured at right heart catheterisation. • Normal mean pulmonary artery pressure? ! 15 mm Hg

Classifications 1) Pulmonary arterial hypertension 2) Pulmonary venous hypertension 3) PH caused by respiratory disorders & /or hypoxaemia 4) PH caused by chronic thromboembolic disease 5) Miscellaneous

Pulmonary arterial hypertension • Primary (Idiopathic) : sporadic & familial… (BMPR 2 gene)!! Typically young female (20 -30) • - found in: 75% of the familial cases 25% of sporadic cases Secondary: connective tissue disease (systemic sclerosis) congenital systemic to pulmonary (left to right) shunts (VSD, ASD, PDA) portal hypertension HIV infection various drugs or toxins persistent pulmonary hypertension of the newborn
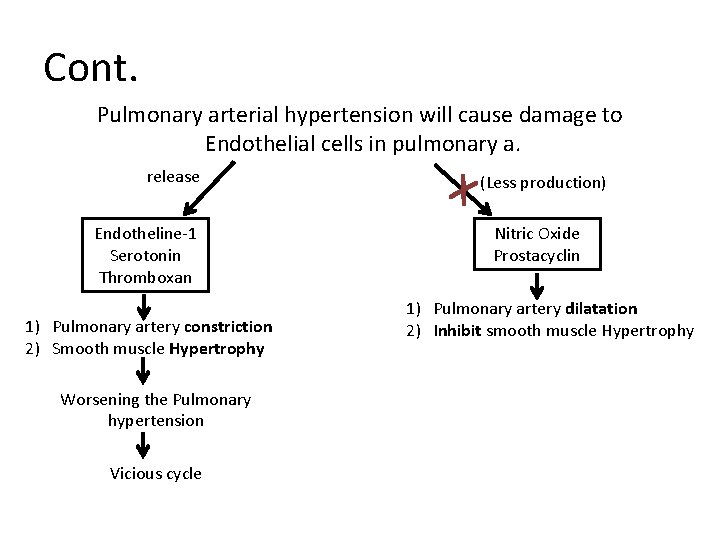
Cont. Pulmonary arterial hypertension will cause damage to Endothelial cells in pulmonary a. release Endotheline-1 Serotonin Thromboxan 1) Pulmonary artery constriction 2) Smooth muscle Hypertrophy Worsening the Pulmonary hypertension Vicious cycle (Less production) Nitric Oxide Prostacyclin 1) Pulmonary artery dilatation 2) Inhibit smooth muscle Hypertrophy
Pulmonary venous hypertension 1. Left-sided atrial or ventricular heart disease (eg. hypertrophy, atrial myxoma , etc. . ) 2. Left-sided valvular heart disease (eg. Mirtal stenosis) 3. Pulmonary veno-occlusive disease 4. Pulmonary capillary haemangiomatosis (very rare)
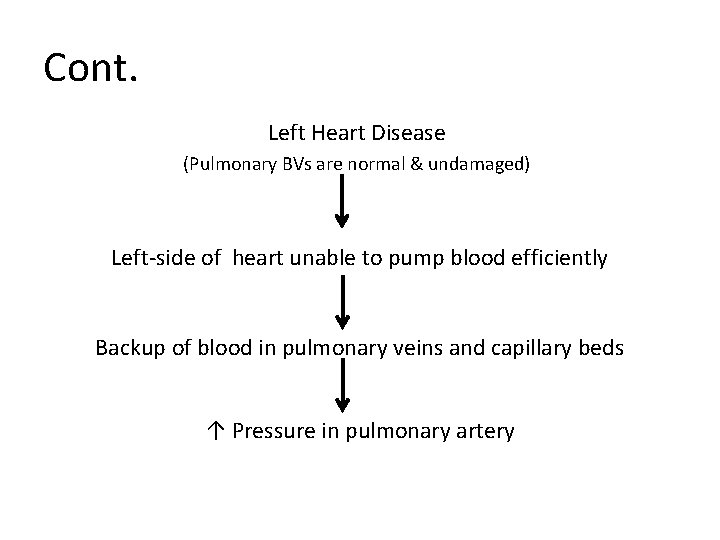
Cont. Left Heart Disease (Pulmonary BVs are normal & undamaged) Left-side of heart unable to pump blood efficiently Backup of blood in pulmonary veins and capillary beds ↑ Pressure in pulmonary artery

PH caused by respiratory disorders & /or hypoxaemia • • COPD Diffuse parenchymal lung disease Sleep-disordered breathing Alveolar hypoventilation disorders Chronic exposure to high altitude Neonatal lung disease Alveolar capillary dysplasia Severe kyphoscoliosis

Cont. respiratory disorders & /or hypoxaemia Hypoxic vasoconstriction of pulmonary arterioles ↑ Pulmonary vascular resistance (harder for Rt. Ventricle to pump blood)
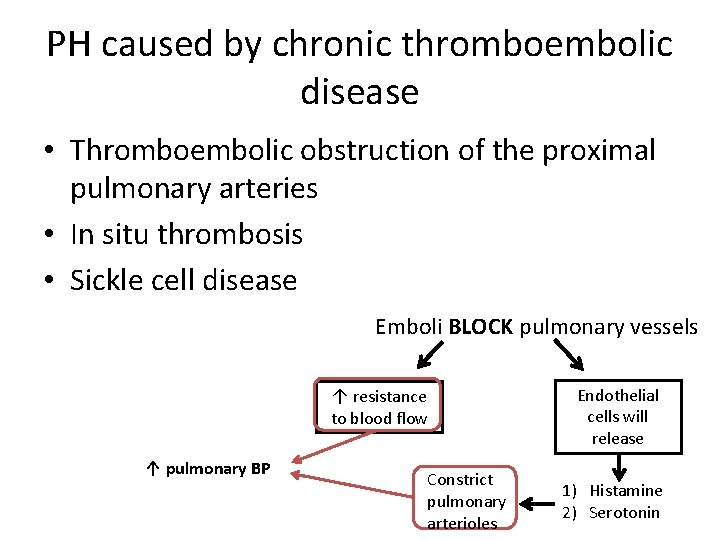
PH caused by chronic thromboembolic disease • Thromboembolic obstruction of the proximal pulmonary arteries • In situ thrombosis • Sickle cell disease Emboli BLOCK pulmonary vessels ↑ resistance to blood flow ↑ pulmonary BP Constrict pulmonary arterioles Endothelial cells will release 1) Histamine 2) Serotonin

Miscellaneous • Inflammatory conditions • Extrinsic compression of central pulmonary veins… eg. Tumour
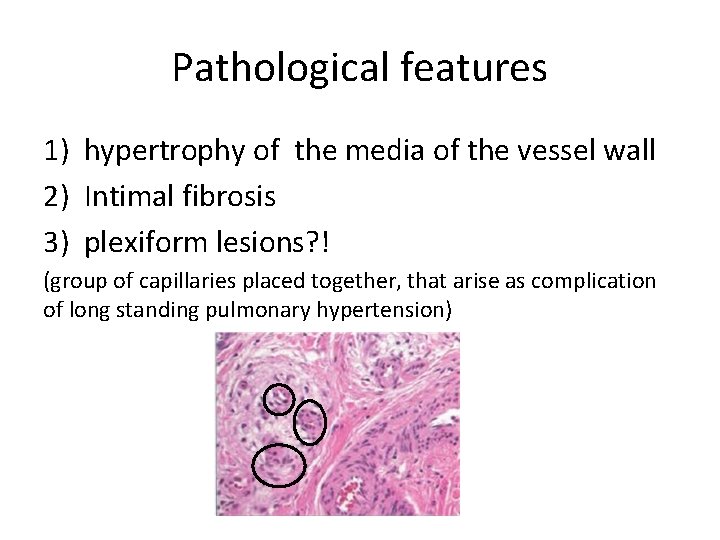
Pathological features 1) hypertrophy of the media of the vessel wall 2) Intimal fibrosis 3) plexiform lesions? ! (group of capillaries placed together, that arise as complication of long standing pulmonary hypertension)
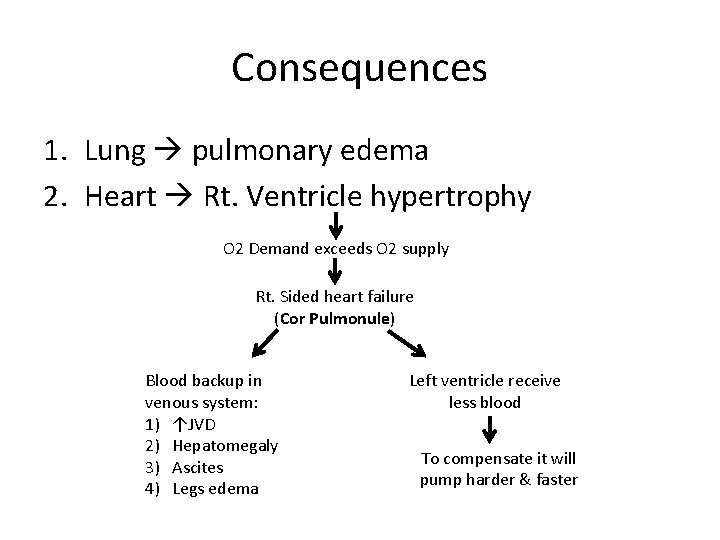
Consequences 1. Lung pulmonary edema 2. Heart Rt. Ventricle hypertrophy O 2 Demand exceeds O 2 supply Rt. Sided heart failure (Cor Pulmonule) Blood backup in venous system: 1) ↑JVD 2) Hepatomegaly 3) Ascites 4) Legs edema Left ventricle receive less blood To compensate it will pump harder & faster

Clinical features • Symptoms: - Breathlessness - chest pain - Fatigue - palpitation - Syncope (with severe disease) • Signs: - accentuation of pulmonary component of the second heart sound (S 2) m. c. - Right ventrical heave (right ventricular hypertrophy) - elevation of the jugular venous pulse (prominent ‘a’ wave if in sinus rhythm) - right ventricular third heart sound. - Tricuspid regurgitation

Investigations • CXR? ! Enlarged pulmonary arteries • ECG? ! right axis deviation due to Rt. Ventricle hypertrophy • Echocardiogram? ! 1) Dilated pulmonary artery 2) Dilatation/hypertrophy of RA and RV 3) Abnormal movement of IV septum (due to increased right ventricular volume) • Right heart catheterization? ! increased pulmonary artery pressure • V/Q scan… when? ! If the cause is not revealed (neither heart nor lung), to know is it due PE or is it primary pulmonary hypertension

Cont. • PFT? ! most pulmonary function parameters are normal in PH (if it’s not caused by respiratory disorders) , but the DLCO (Diffusing capacity of the lungs for carbon monoxide) decreases. Know that a very low DLCO is associated with a poor prognosis in patients with PH. • What are the 1 st tests you order when you suspect PH? ! ECG & an echocardiogram. • What follow-up test is done if the 1 st tests are suggestive? ! Right heart catheterization to confirm the diagnose

Management 1) Exercise : improve the functional class of patients greatly but does not change the hemodynamics. 2) Unless there is an increased risk of bleeding anticoagulants mainly warfarin. Our goal is to reach INR of 2. 0. 3) Diuretics are recommended for fluid retention. 4) Oxygen for those with chronic hypoxaemia. 5) Vasodilators 6) Lung transplantation

Vasodilator agents 1) Oral Calcium Channel Blockers. . vasodilators of choice (eg. ifedipine, amlodipine & diltiazem) 2) Oral Endothelin Receptor Antagonists (eg. Bosentan) 3)IV Prostacyclin (eg. Epoprostenol) 4) Inhaled PDE (phosphodiesterase) Inhibitors type 5

• Questions ? ?
- Slides: 19