Pulmonary Hypertension I Abou Daya Pulmonary CCM 05242016

Pulmonary Hypertension I. Abou Daya Pulmonary CCM 05/24/2016 1

Pulmonary HTN : Definition Ø Pulmonary Hypertension : • Mean Pulmonary Artery Pressure MPAP > 25 mm. Hg at rest q Without treatment, it leads to progressive elevation of BP in the Pulmonary Vascular Bed and cause right heart Failure /Death 2
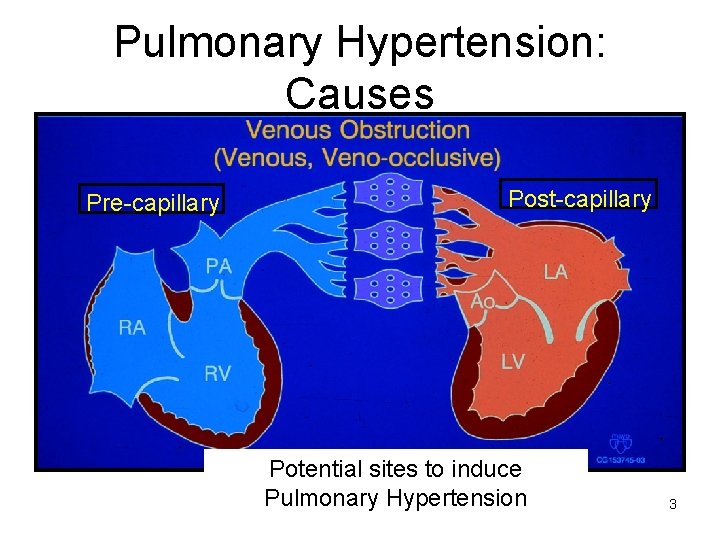
Pulmonary Hypertension: Causes Pre-capillary Post-capillary Potential sites to induce Pulmonary Hypertension 3

PHTN : • - PHTN affects : Breathing : Oxygenation / Diffusion Cardiac Output and BP : Hemodynamics Peripheral circulation : Leg edema Renal Function : Fluid and Electrolytes Liver/ GI : Venous stasis Daily Activity 4
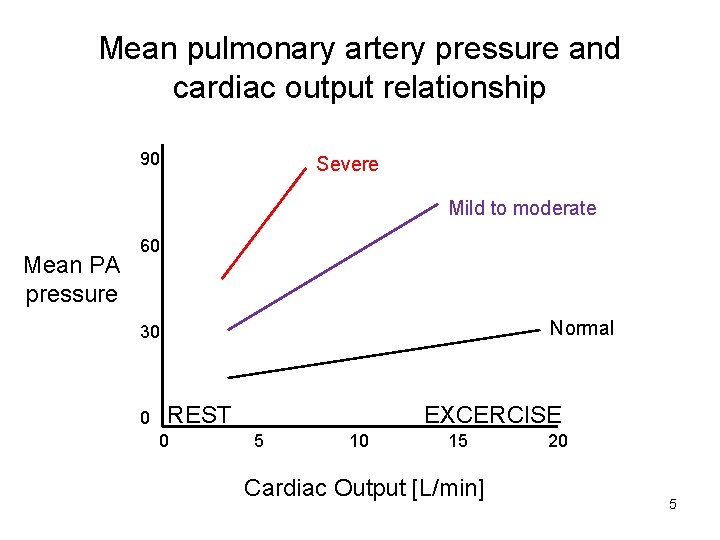
Mean pulmonary artery pressure and cardiac output relationship 90 Severe Mild to moderate Mean PA pressure 60 Normal 30 0 REST 0 EXCERCISE 5 10 15 Cardiac Output [L/min] 20 5

Pulmonary Hypertension: Classification 1. Pulmonary arterial hypertension (PAH) 1. idiopathic (“primary pulmonary hypertension”) 2. secondary to systemic disorders 2. Pulmonary hypertension due to left heart disease (pulmonary venous hypertension) 3. Pulmonary hypertension associated with respiratory disease and/or hypoxia 1. COPD, Interstitial lung disease, OSA 4. Chronic Thromboembolic/embolic pulmonary hypertension 5. Pulmonary hypertension from unclear mechanisms 6

Pulmonary HTN : Clinical Manifestations • Symptoms and signs are usually not specific; delay in diagnosis very common. • Early – dyspnea with activity ‘Most Common’ • Late symptoms: – – – Syncope/ Palpitations Fatigue /Lack of Energy Chest pain / chest pressure leg edema (signs of right heart failure) abnormal findings on chest X ray or ECG 7

Pulmonary HTN : Physical Exam Ø Ø Ø Ø Ø Accentuated intensity of pulmonary second heart sound Tricuspid murmur Pulmonary murmur Right ventricular S 3 or S 4 Parasternal heave or subxiphoid thrust Jugular venous distension Peripheral edema Hepatomegaly Ascites 8

What other tests should be ordered in the evaluation of PH? Ø Chest radiography; ECHO; EKG, BNP or N-Terminal BNP Ø CBC; electrolytes / creatinine Ø HIV serologic testing Ø Autoantibody testing for collagen vascular disease Ø Liver function testing Ø Pulmonary function testing Ø Polysomnography Ø Radionuclide ventilation-perfusion imaging Ø Right heart catheterization Ø Six-minute walking Test 9
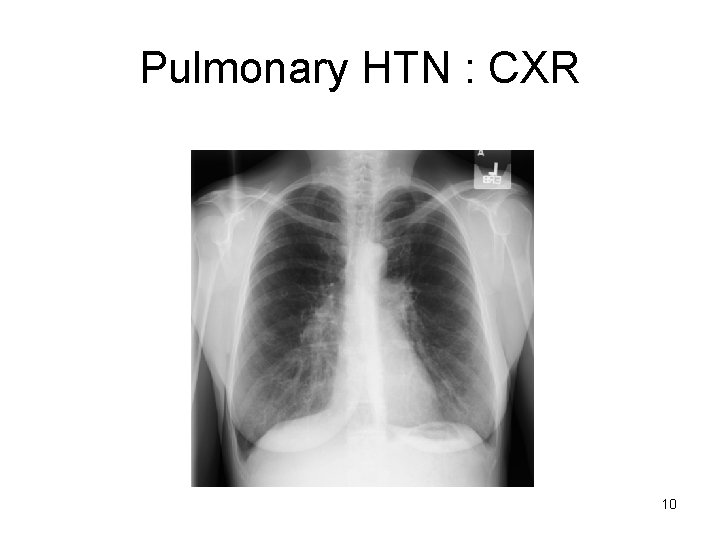
Pulmonary HTN : CXR 10

PHTN: EKG abnormalities • Right heart strain (RVH and RA enlargement) • Non-specific • Right axis deviation • ST depression and T wave inversion V 1 V 3 11

Pulmonary HTN : Screening • There is no perfect screening tool. • Transthoracic echocardiography • Goals: – 1. determine right ventricular size and systolic function – 2. estimate right ventricular systolic pressure 12

PHTN: Role of echocardiography Ø One of best tests to evaluate for possible PH q May report an estimate of systolic PAP q May provide information on cause of PH and symptoms q Underlying VHD if present Ø Indicators of more severe disease q Right atrial or ventricular enlargement q Hypertrophy; decreased right ventricular function q Severe elevations in right ventricular pressure may cause leftward deviation of interventricular septalum q Pericardial effusion 13
![PHTN: Echo PASP = (4 x [TRV]2) + RAP LA RA LV RV Echo PHTN: Echo PASP = (4 x [TRV]2) + RAP LA RA LV RV Echo](http://slidetodoc.com/presentation_image_h2/f3717635ff6c9c1c28a646031670b96d/image-14.jpg)
PHTN: Echo PASP = (4 x [TRV]2) + RAP LA RA LV RV Echo transducer 14 CP 900234 -1

PHTN: W/U • If the echocardiogram suggests the presence of pulmonary hypertension – 1. perform careful evaluation for secondary causes – 2. consider whether you should proceed to right heart catheterization 15
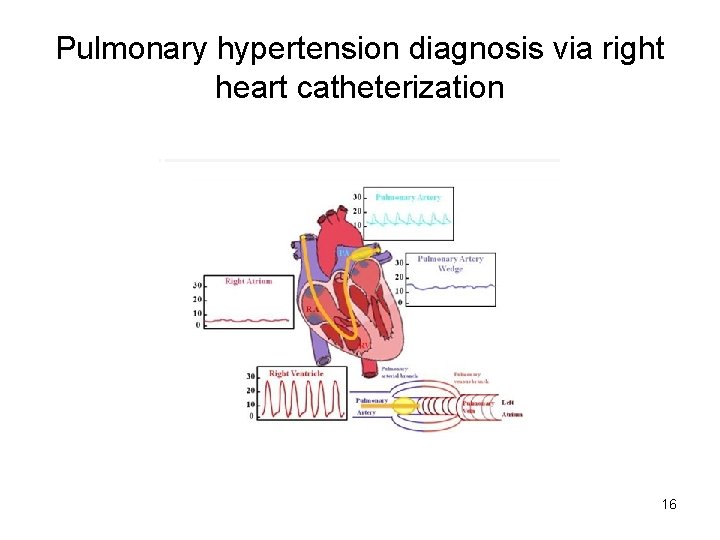
Pulmonary hypertension diagnosis via right heart catheterization 16

Is cardiac catheterization Necessary ? Ø Right heart catheterization q Required if PAH (Group I )suspected (before advanced medical Rx) q Also helps identify unrecognized left heart dysfunction and pulmonary venous hypertension Ø Left heart catheterization q Often done concurrently, particularly if risk for CAD Ø No right heart catheterization needed… q PH known to be due to left heart or chronic pulmonary disease AND and cath not needed to guide management

How should right heart catheterization be done when PH is a consideration? Ø Assess for possible left-to-right shunts Ø Measure hemodynamics accurately q Accurate Measure of PAP q Unsure of wedge? Measure left ventricular end-diastolic pressure simultaneously Ø Test Pulmonary Vasoreactivity in PAH 18

Once pulmonary hypertension is detected, look for causes! 19
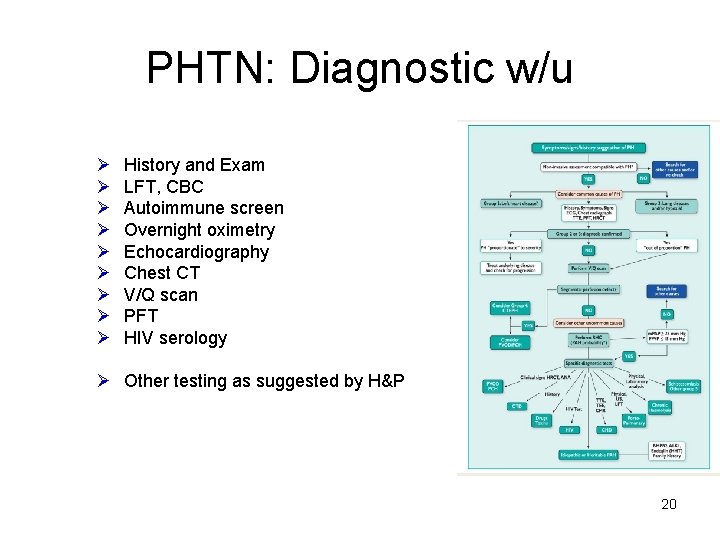
PHTN: Diagnostic w/u Ø Ø Ø Ø Ø History and Exam LFT, CBC Autoimmune screen Overnight oximetry Echocardiography Chest CT V/Q scan PFT HIV serology Ø Other testing as suggested by H&P 20

What are the requirements for the diagnosis of PAH Group I Ø Presence of PH q Mean PAP > 25 mm Hg Ø Absence of pulmonary venous hypertension q Left atrial or “wedge” pressure < 15 mm Hg Ø Exclusion of significant chronic hypoxemic lung disease Ø Exclusion of chronic thromboembolic disease Ø Elevated pulmonary vascular resistance q > 3 Wood units 21

Group 1: “Primary” pulmonary arterial hypertension • Remember PAH (Group 1) and PH (Groups 2 -5) are different entities • PAH is a progressive disease with a 50% survival at 2. 8 years • Can lead to sudden death • Often affects young adults: mean age 45 years • Rarely familial 22
Group 1: Secondary pulmonary artery hypertension • Collagen vascular disease • scleroderma • Systemic lupus erythematosus • Liver disease • Congenital heart • Drugs/toxins • HIV infection 23
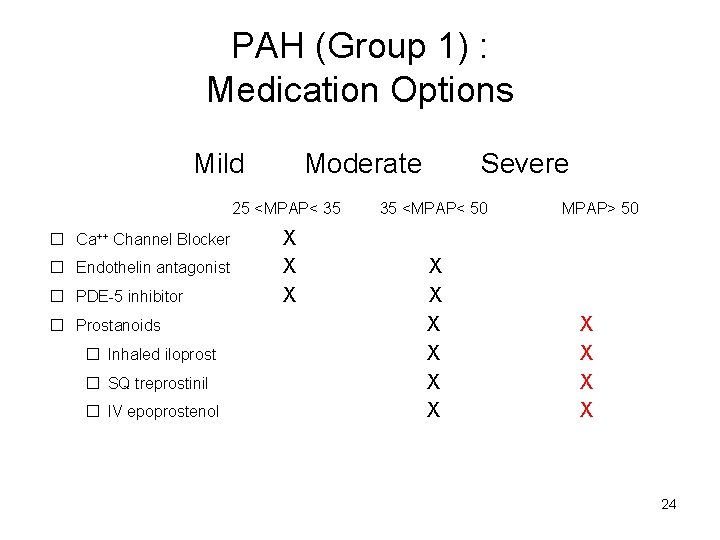
PAH (Group 1) : Medication Options Mild Moderate 25 <MPAP< 35 � Ca++ Channel Blocker � Endothelin antagonist � PDE-5 inhibitor � Prostanoids � Inhaled iloprost � SQ treprostinil � IV epoprostenol X X X Severe 35 <MPAP< 50 X X X MPAP> 50 X X 24
Drug of choice? • Right heart catheterization vasodilator “challenge” � 20% acute drop in MPAP and PVR? . . . begin with ca++ channel blocker 25

What drugs are available for the treatment of PAH? • Advanced therapies Ø Endothelin Antagonists (for lower risk patients) Ø Phosphodiesterase-5 Inhibitors (for lower risk patients) Ø Prostacyclins (for higher risk patients) 26
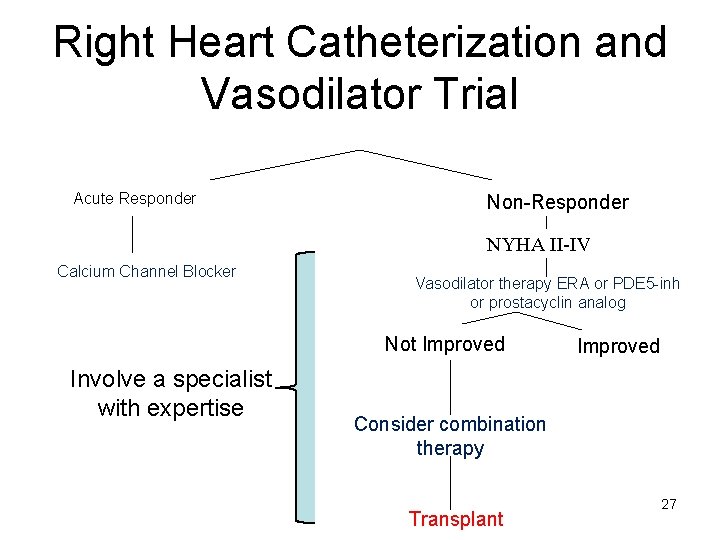
Right Heart Catheterization and Vasodilator Trial Acute Responder Non-Responder NYHA II-IV Calcium Channel Blocker Vasodilator therapy ERA or PDE 5 -inh or prostacyclin analog Not Improved Involve a specialist with expertise Improved Consider combination therapy Transplant 27
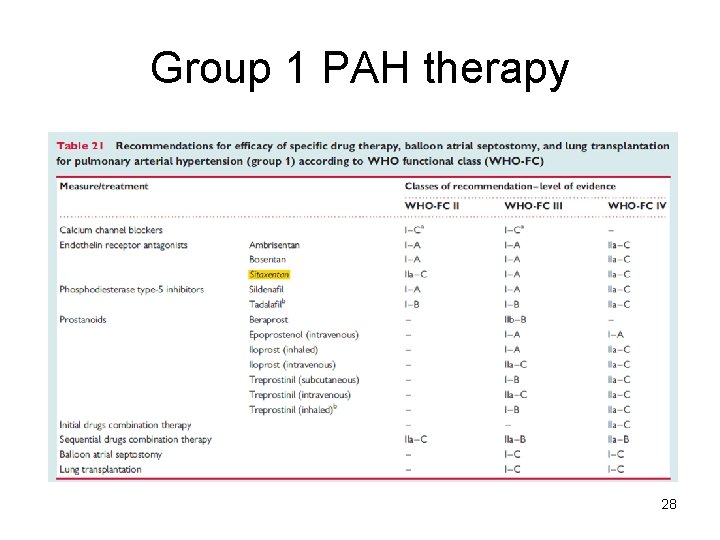
Group 1 PAH therapy 28

When should a clinician consider consultation with a specialist in diagnosing pulmonary hypertension? Ø Uncertainty regarding the diagnosis Ø Multiple comorbid conditions that may complicate diagnosis or treatment Ø High-risk features or NYHA functional class III or IV • Refer to a specialized center for evaluation 29

PHTN : Prognosis Ø Negative prognostic sign in many conditions (HF, COPD) Ø It increases Perioperative Mortality In particular, PAH prognosis q Worse in presence of advanced NYHA/WHO functional class, shorter 6 -min walking distance q Worse with connective tissue disease q Worse with portopulmonary hypertension q Untreated PAH: median survival 2. 8 years 30
CLINICAL BOTTOM LINE: Diagnosis and Screening… v Confirm elevated pulmonary pressures v Evaluate for potential causes § ECHO; chest X-ray § Ventilation-perfusion scanning § Pulmonary function and blood testing v Assess disease severity § Measure oxyhemoglobin saturation § 6 -minute walking distance § Blood BNP v Right heart catheterization § Mandatory if therapy directed at PH itself (e. g. , PAH) 31

PHTN Group (2 -5) : Management • • Treat any underlying disease. Treat cardiac disease (left sided). Treat lung disease and hypoxemia. Treat obstructive sleep apnea or any associated sleep disorder. • Treat Thromboembolic disease. • Remember: Groups 2 -5 are managed differently and vasodilator therapy is NOT recommended. 32

Adjunctive therapy • • • Salt restriction. Diuretics as needed. Oxygen at rest or with activity. Flu and pneumococcal vaccination. Digoxin ? Role if any. Anticoagulation ? 33

PHTN : Group 2 due to Cardiac Disease Ø Systolic HF q Use: ACE inhibitors; β-blockers; diuretics q Possibly: cardiac resynchronization, implantable cardioverter defibrillator placement, digitalis Ø HFp. EF q Control BP + heart rate with β-blockers, diuretics Ø Left HFr. EF q Differentiate from PAH q Don’t use prostacyclin analogues, endothelin antagonists Ø PH secondary to left valvular heart disease q Evaluation for correction of valvular disease 34

How should patients with PH due to lung disease be treated? Ø Optimize treatment of underlying cause q. Sleep apnea (minimize nocturnal desaturation) q. COPD q. Idiopathic lung disease Ø Use supplemental oxygen to avoid hypoxia Ø Enroll in pulmonary rehabilitation Ø Don’t use PAH therapy in PH due to lung disease 35

How should patients with chronic Thromboembolic PH be treated? Ø Prevention of recurrent clot / embolism (anticoagulation) Ø Pulmonary thromboendarterectomy (PTE) q Refer to center experienced in procedure and postop q Improves symptoms in most patients q Surgical mortality at experienced centers: <5% Ø Use medical therapy directed at PH only when… q PTE impossible due to distal location of disease within pulmonary vasculature q Therapeutic bridge needed until PTE performed q Patient decides not to have PTE 36

What drugs are available for the treatment of PAH? Ø Diuretics Ø Supplemental oxygen Ø Calcium-channel blockers (trial only if demonstrated vasoreactivity) Ø Anticoagulants Ø Digoxin 37

Is there a role for combination therapy in PAH? Ø Sequential addition of advanced therapies: current model q Initial therapy: based on illness severity + functional class q If PAH worsens: add therapies until treatment goals met q Approach shown to improve 6 -min walking distance and delay clinical worsening 38

What is the role of lung transplantation? Ø Treats underlying pulmonary condition in patients with… q Late-stage respiratory disease: severe PH + COPD or ILD q PAH: consider transplant when progressive disease requires parenteral therapy Ø Defer until deterioration occurs despite max medical Rx Ø Double lung transplantation: preferred procedure for PAH q Reduces right ventricular afterload: right heart often recovers q PAH: 23% unadjusted 3 -mo mortality after procedure Ø Heart-lung transplantation q For uncorrectable congenital heart lesions q For concomitant primary cardiac failure 39

What is the role of exercise? Ø Exercise improves exercise capacity and QOL q Important adjunct to medical therapy q Avoids deconditioning from being sedentary q PH isn’t a contraindication to judicious exercise Ø Encourage patients to remain active within symptom limits q Mild breathlessness is acceptable q Avoid severe breathlessness, exertional dizziness, near syncope, or chest pain q Isometric exercises discouraged due to exertional syncope 40

Conclusions v PAH § Perform right heart catheterization with vasodilator test § Don’t treat empirically with calcium-channel blockers § Advanced therapies: prostacyclins, endothelin-receptor antagonists, PDE 5 inhibitors v Right HF § Use diuretics, salt restriction v PH due to left heart or chronic hypoxemic lung disease § Treat underlying disorders (not PH per se) v Chronic Thromboembolic PH § Use anticoagulants + possible thromboendarterectomy v Evaluate need for supplemental oxygen v Lung transplantation: in nonresponsive advanced disease

Conclusion • • • New onset exertional dyspnea…think of pulmonary hypertension. Screen by Transthoracic Doppler Echo but make sure you tell the cardiologist that you are thinking of PH! Definitive diagnosis by right heart catheterization “Group 1”. Several pharmacologic options now available: selection a function of PAH severity, expertise, cost assessment, and other factors. Pregnancy may cause significant challenges. PH patients are increasingly older with potential multiple ongoing diagnoses. 42

Thank you 43
- Slides: 43