Pulmonary function test Evaluation of pulmonary function is































- Slides: 47

Pulmonary function test

Evaluation of pulmonary function is important in many clinical situations evaluation of a variety of forms of lung disease assessing the presence of disease in a patient with known risk factors

Indications Risk evaluation of patients prior to thoracic or upper abdominal surgery Objective assessment of impairment or disability

Indications Evaluation of symptoms such as chronic persistent cough, wheezing, dyspnea and exertional cough or chest pain Objective assessment of bronchodilator therapy. Evaluation of effects of exposure to dusts or chemicals at work

Contraindications Hemoptysis of unknown origin Unstable angina pectoris Pneumothorax Thoracic aneurysms Recent myocardial infarction

Contraindications Recent abdominal or thoracic surgical procedures History of syncope associated with forced exhalation Recent eye surgery (increased intraocular pressure during forced expiration) Cerebral aneurysms Abdominal aneurysms

The major types of pulmonary function tests • spirometry • flow-volume loops • measurement of lung volumes • quantitation of diffusing capacity • Measurements of maximal respiratory pressures

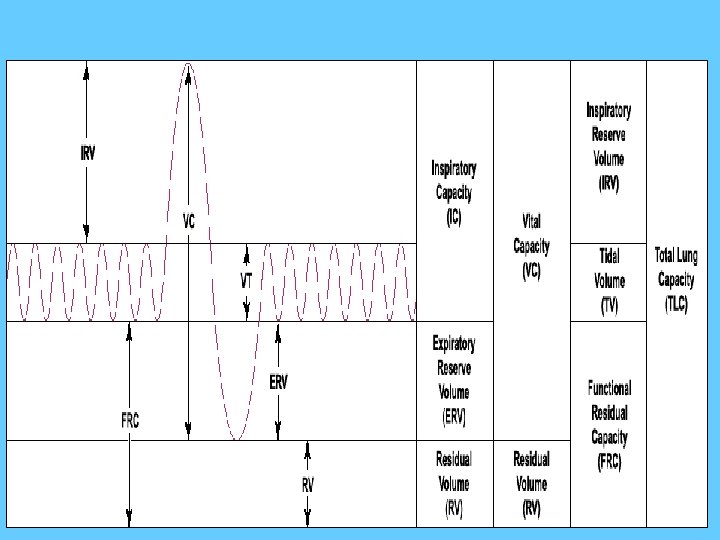
The predicted values of Lung volumes and Lung Capacities


Spirometry Check recovery from exacerbation of asthma, COPD Evaluate dyspnea Smokers over age 45 to detect COPD

Spirometry with bronchodilator Chronic cough or chest tightness Suspect asthma or COPD Determine response to specific bronchodilator therapy

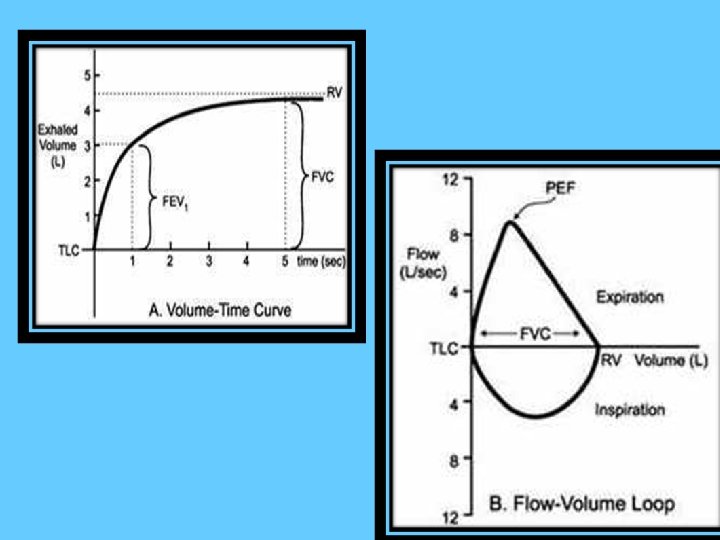
What is a spirometry ? ? Spirometry is a measure of airflow and lung volumes during a forced expiratory maneuver from full inspiration Spirometry is one of the most widely used lung function tests

How to do it ? ? 1. 2. 3. 4. 5. Stand or sit up straight (The patient places a clip over the nose ) Inhale maximally Get a good seal around mouthpiece of the spirometer Blow out as hard as fast as possible and count for at least 6 seconds. Record the best of three trial

• The basic values to interpret Spirometry are: 1. 2. 3. 4. 5. FVC FEV 1/FVC ratio FEV 1/FEV 6 FEF 25– 75%


Forced Vital Capacity (FVC) The FVC is the maximal amount of air that the patient can forcibly exhale after taking a maximal inhalation

FEV 1 Volume of air which can be forcibly exhaled from the lungs in the first second of a forced vital capicity maneuver. The FEV 1 is the most important spirometric variable for assessment of airflow obstruction

FEV 1 It declines in direct and linear proportion with clinical worsening of airways obstruction It increases with successful treatment of airways obstruction The FEV 1 should be used for determining the degree of obstruction (mild, moderate, or severe) Serial comparisons is important when following patients with asthma or COPD

FEV 1/FVC Ratio of FEV 1 to FVC : It indicates what percentage of the total FVC was expelled from the lungs during the first second of forced exhalation This value is critically important in the diagnosis of obstructive and restrictive diseases

FEF 25% Amount of air that was forcibly expelled in the first 25% of the total forced vital capacity test.

FEF 75% The amount of air expelled from the lungs during the first (75%) of the forced vital capacity test.

FEF 25%-75% • The amount of air expelled from the lungs during the middle half of the forced vital capacity test. More sensitive marker of mild small airway obstruction than the FEV 1 But reproducibility is poor

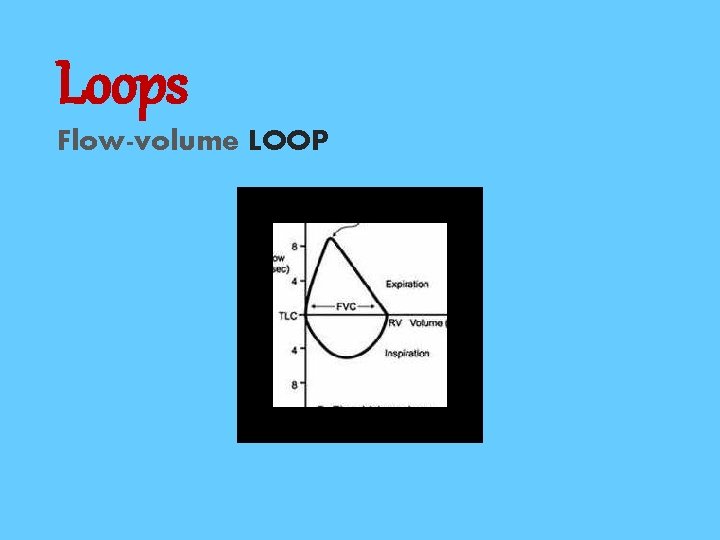
Loops Flow-volume LOOP

Residual Volume (RV) The amount of air left in the lungs after a maximal exhalation The amount of air that is always in the lungs and can never be expired

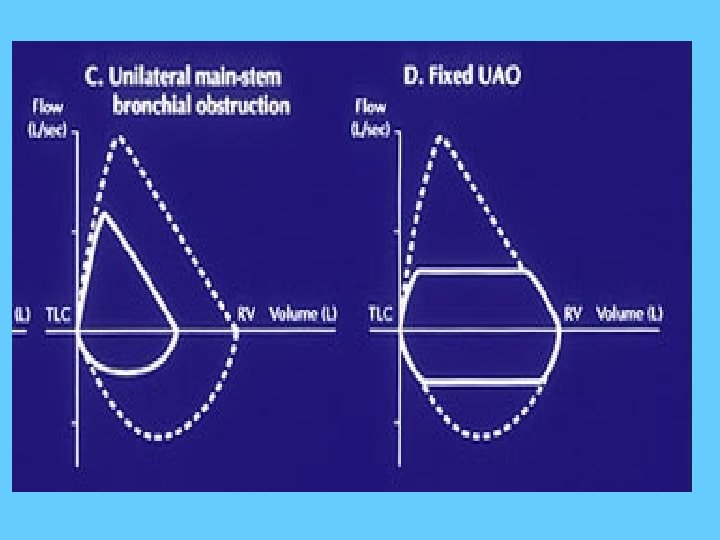
• The contour of the loop assists in the diagnosis and localization of airway obstruction as different lung disorders produce distinct , easily recognized pattern




Interpretation of PFTs Step 1. Look at the Flow-Volume loop to determine acceptability of the test, and look for upper airway obstruction pattern. Step 2. Look at the FEV 1 to determine if it is normal (≥ 80% predicted). Step 3. Look at FVC to determine if it is within normal limits (≥ 80%). Step 4. Look at the FEV 1/FVC ratio to determine if it is within normal limits (≥ 70%).

Step 5. Look at FEF 25 -75% (Normal (≥ 60%) • If FEV 1, FEV 1/FVC ratio, and FEF 25 -75% all are normal, the patient has a normal PFT. • If both FEV 1 and FEV 1/FVC are normal, but FEF 25 -75% is ≤ 60% , then think about early obstruction or small airways obstruction.

• If FEV 1 ≤ 80% and FEV 1/FVC ≤ 70%, there is obstructive defect, if FVC is normal, it is pure obstruction. If FVC ≤ 80% , possibility of additional restriction is there. • If FEV 1 ≤ 80% , FVC ≤ 80% and FEV 1/FVC ≥ 70% , there is restrictive defect, get lung volumes to confirm.

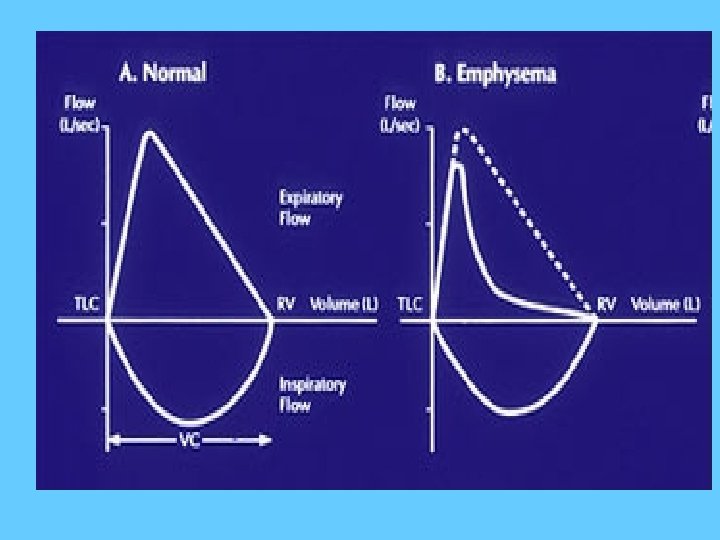
Obstructive Lung Diseases • Asthma • COPD (chronic bronchitis, emphysema and the overlap between them). • Cystic fibrosis

• Airflow is reduced because the airways narrow and the FEV 1 is reduced

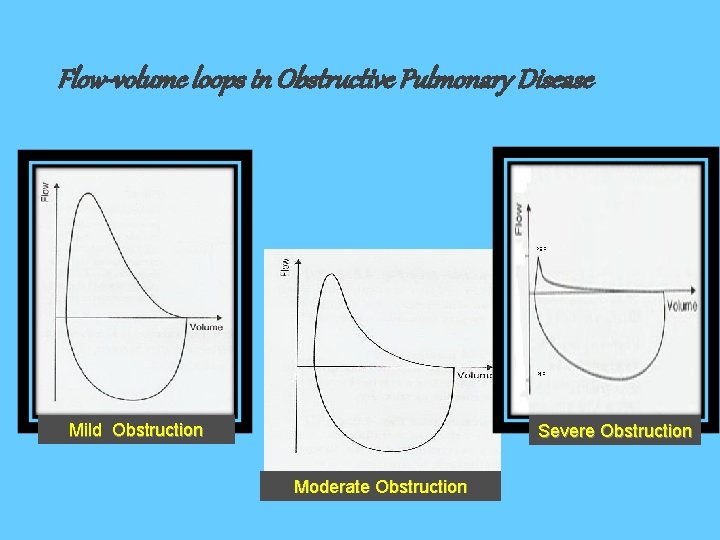
Flow-volume loops in Obstructive Pulmonary Disease PEF PIF Mild Obstruction Severe Obstruction Moderate Obstruction

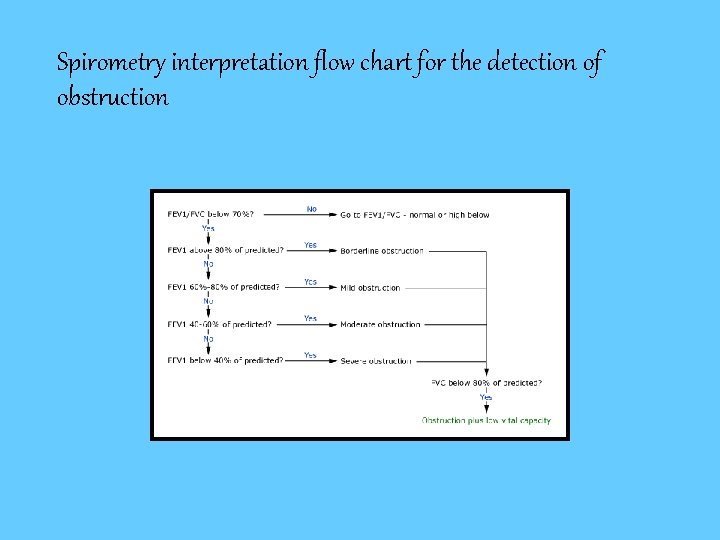
Spirometry interpretation flow chart for the detection of obstruction

Restrictive Lung Diseases

A. Intrinsic Restrictive Lung Disorders Sarcoidosis 2. Idiopathic pulmonary fibrosis 3. Interstitial pneumonitis 4. Tuberculosis 5. Pnuemonectomy (loss of lung) 6. Pneumonia 1.

B. Extrinsic Restrictive Lung Disorders Scoliosis, Kyphosis 2. Ankylosing Spondylitis 3. Pleural Effusion 4. Pregnancy 5. Gross Obesity 6. Tumors 7. Ascites Pain on inspiration - pleurisy, rib fractures 1. 8.

C. Neuromuscular Restrictive Lung Disorders 1. Generalized Weakness – 2. 3. 4. 5. 6. malnutrition Paralysis of the diaphragm Myasthenia Gravis Muscular Dystrophy Poliomyelitis Amyotrophic Lateral Sclerosis

Full expantion of the lung is limited and therefore the FVC is reduced FEV 1 may be reduced because the stiffness of fibrotic lungs increases the expiratory pressure FEV 1/FVC will be Normal or Increased

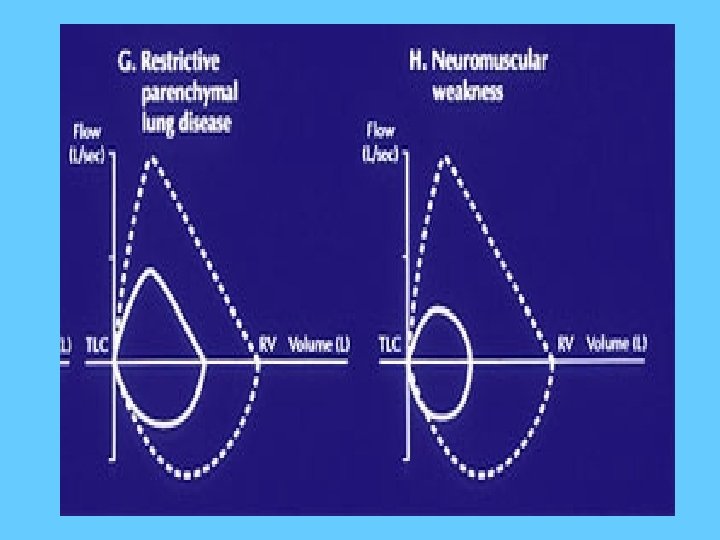
Flow volume loop in Restrictive lung disease

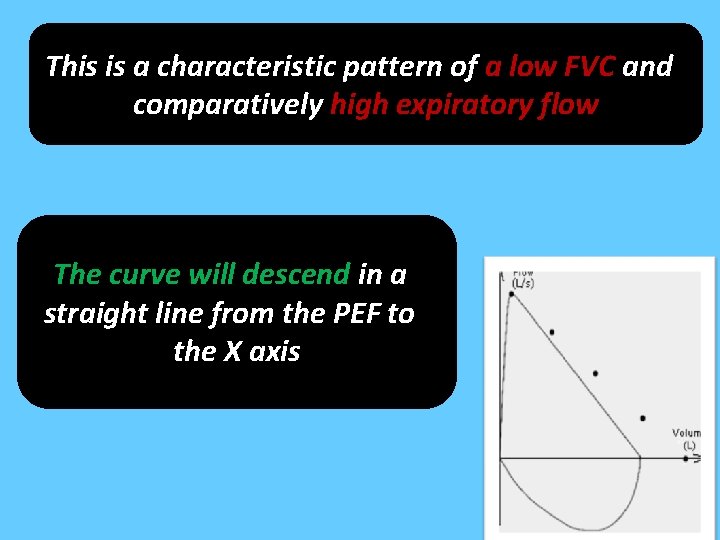
This is a characteristic pattern of a low FVC and comparatively high expiratory flow The curve will descend in a straight line from the PEF to the X axis

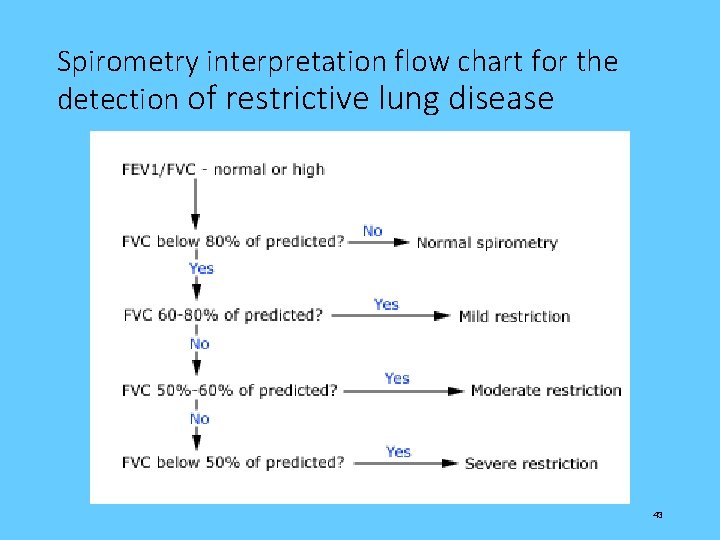
Spirometry interpretation flow chart for the detection of restrictive lung disease 43

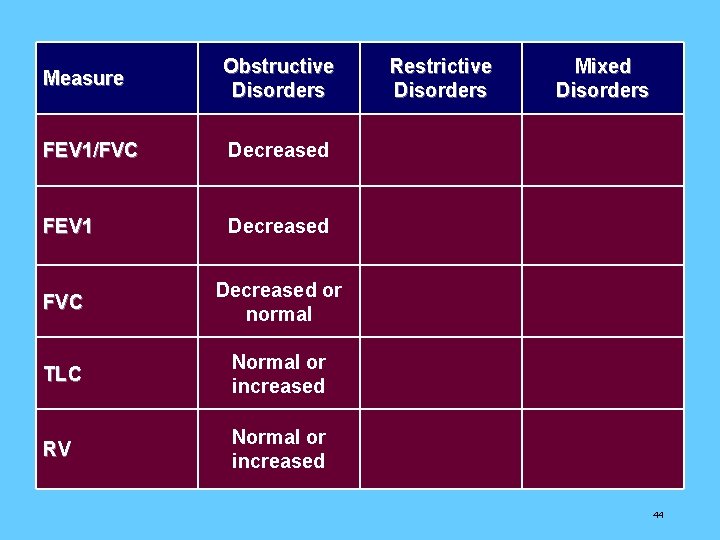
Measure Obstructive Disorders Restrictive Disorders Mixed Disorders FEV 1/FVC Decreased Normal or increased Decreased FEV 1 Decreased, normal, or increased FVC Decreased or normal Decreased TLC Normal or increased Decreased RV Normal or increased Decreased, normal, or increased Decreased 44

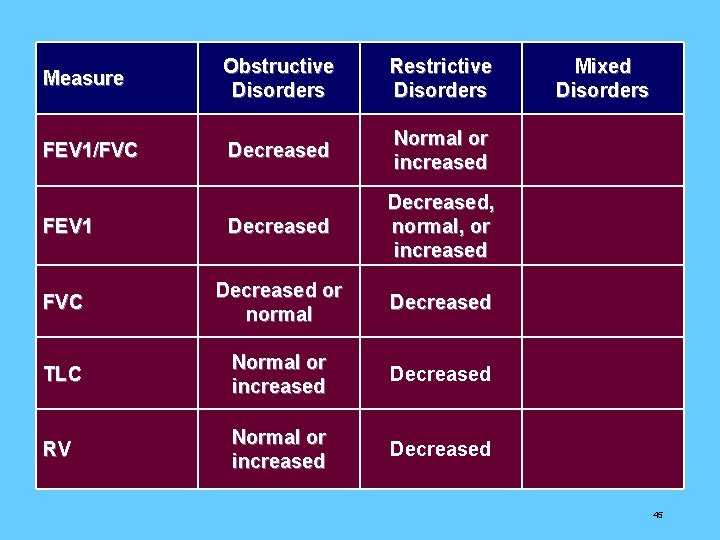
Measure Obstructive Disorders Restrictive Disorders Mixed Disorders FEV 1/FVC Decreased Normal or increased Decreased FEV 1 Decreased, normal, or increased Decreased FVC Decreased or normal Decreased TLC Normal or increased Decreased RV Normal or increased Decreased, normal, or increased 45

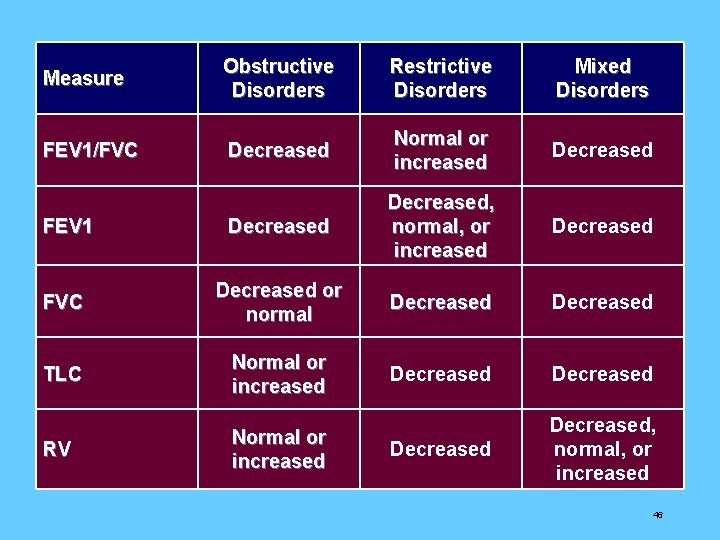
Measure Obstructive Disorders Restrictive Disorders Mixed Disorders FEV 1/FVC Decreased Normal or increased Decreased FEV 1 Decreased, normal, or increased Decreased FVC Decreased or normal Decreased TLC Normal or increased Decreased RV Normal or increased Decreased, normal, or increased 46

47