Pulmonary embolism pulmonary hypertension cor pulmonale chronicum Attila

Pulmonary embolism, pulmonary hypertension, cor pulmonale chronicum Attila Somfay Dept. Pulmonology, University of Szeged, Deszk, Hungary

KEY POINTS • 1/1000/year • early treatment is highly effective, but is underdiagnosed, therefore, remains a major health problem • diagnostic strategy should be based on clinical evaluation (probability assessment) • value of PPV and NPV are high when concordant with clinical assessment • additional tetsting is neccessery when test result is inconsistent with clinical probability

Epidemiology • USA: 117 %000 VTE - 48 %000 DVT - 69 %000 PE (Arch Intern Med 1998; 158: 585 -593) • Europe: 183 %000 VTE - 124 %000 DVT - 60 %000 PE (Thromb Haemost 2000; 83: 657 -660)
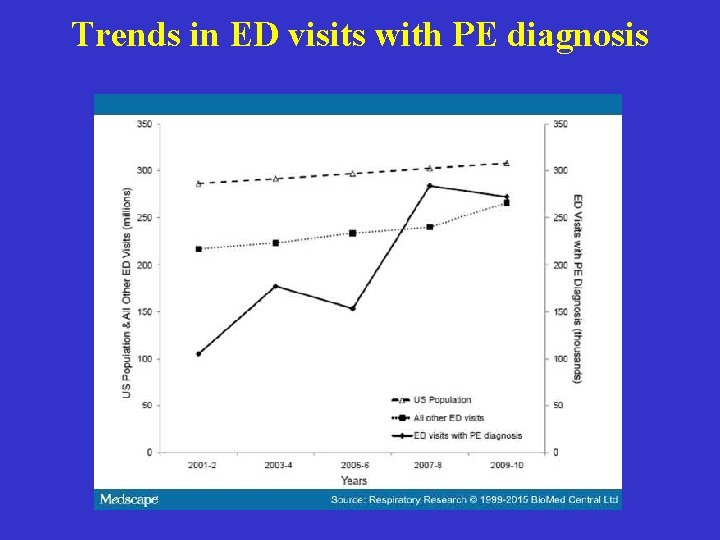
Trends in ED visits with PE diagnosis
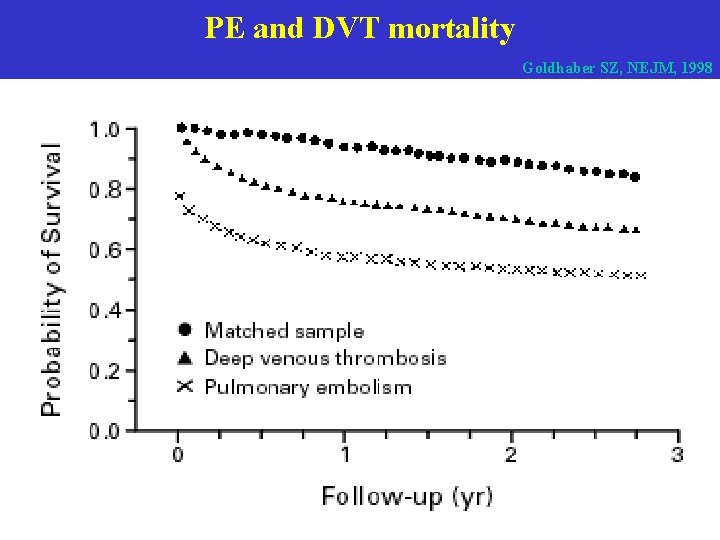
PE and DVT mortality Goldhaber SZ, NEJM, 1998

Pathogenesis of VTE 1. Venous stasis – immobility (hospitalization-DVT), CHF, gravidity, obesity, elderly patients 2. Intima injury– surgery (orthopedic, obstetrical), trauma venous lines, venography 3. Abnormalities of coagulation – fibrinolysis - malignancy - lupus anticoagulant - thrombophilias: AT III, protein S-, protein C deficiency - mutation (Factor VLeiden) - myeloproliferativ disorders, policythaemia - nephrosis sy - gravidity, contraceptive pills - colitis ulcerosa

Fedullo PF, Tapson VF NEJM 2003

Symptomes of PE 1. 2. 3. 4. 5. 6. 7. Dyspnoe with sudden onset Pleural chest pain Cough Hemoptoe Sweat Non-pleural chest pain Syncope 84% 74% 53% 30% 27% 14% 13%

Physical findings 1. Tachypnoe (>16/min) 2. Crackles, local wheeze 3. PII ! 4. Tachycardia (>100/min) 5. Fever 6. Sweating 7. Phlebitis 8. Anasarca 9. Cyanosis 10. Pleural friction rub, fluid 92% 58% 53% 44% 43% 36% 32% 24% 19% 11%

Fedullo PF, Tapson VF NEJM 2003
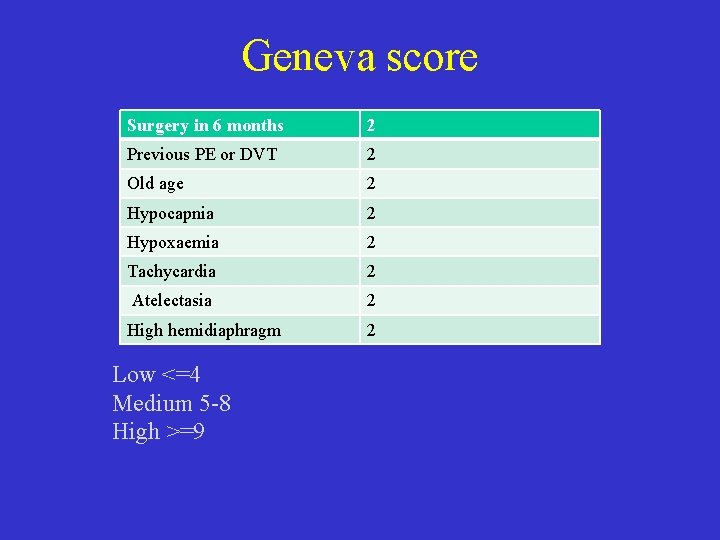

Geneva score Surgery in 6 months 2 Previous PE or DVT 2 Old age 2 Hypocapnia 2 Hypoxaemia 2 Tachycardia 2 Atelectasia 2 High hemidiaphragm 2 Low <=4 Medium 5 -8 High >=9

Goldhaber SZ, NEJM, 1998

Clinical classification Hemodynamics (mm. Hg): RA 1. Acute, massive 2. Acute, minor 3. Chronic, reccurant (CTEPH) 12 5 6 RV PA 45/0 -12 45/20 30/0 -5 30/15 90/0 -6 90/50

Acute, massiv PE • >50% obstruction (mechanic + humoral + neurogenic) • Heavy, retrosternal pain, panic • Pallor, cyanosis, sweating, strongs dyspnoe, tachycardia • Right heart failure, distended jugular veins Diff dg: AMI, dissecant aortic aneurysm, cardiac tamponade, pulmonary edema, ptx, shock

Acute, minor PE • • • Haemoptysis Pleural chest pain Mild dyspnoe Pa. O 2 normal Fever, tachycardia Diff dg: pleurisy, pneumonia, bronchial cc

Chronic, reccurant PE (CTEPH) • • Reccurant episodes for months - years Progression of effort dyspnea Cyanosis Angina-like chest pain (decreased myocardial perfusion pressure) • Tachycardia, PII !, systolic ejection click • Death: progression of right heart failure Diff dg: COPD, CHF, hyperventilation sy
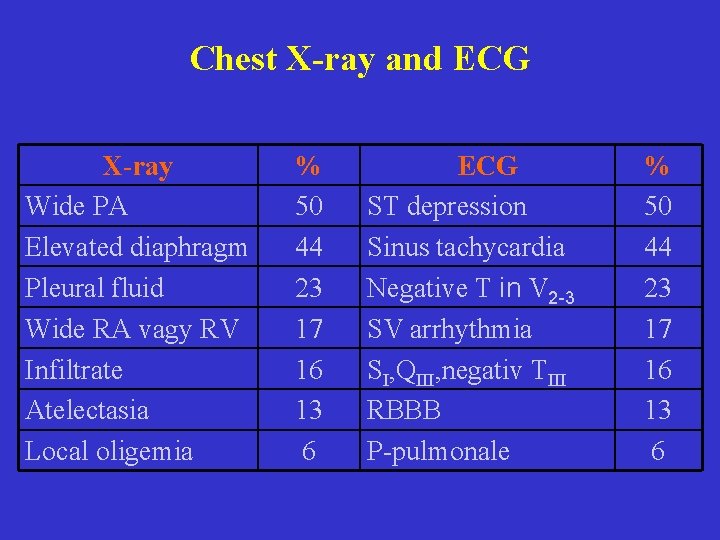
Chest X-ray and ECG X-ray Wide PA Elevated diaphragm Pleural fluid Wide RA vagy RV Infiltrate Atelectasia Local oligemia % 50 44 23 17 16 13 6 ECG ST depression Sinus tachycardia Negative T in V 2 -3 SV arrhythmia SI, QIII, negativ TIII RBBB P-pulmonale % 50 44 23 17 16 13 6

Acute, massive PE rs. R’

CTEPH

ABG • • Pa. O 2 Pa. CO 2 p. H ! P(A-a)O 2 Alveolar gas equation: PA (mm. Hg) = (PB-47) x FIO 2 – 1. 2 x Pa. CO 2 102 = 150 - 48

West JB, 1998
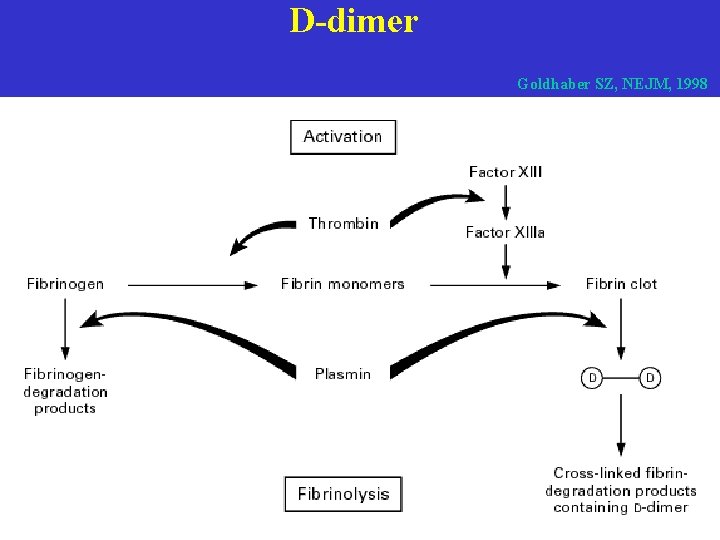
D-dimer Goldhaber SZ, NEJM, 1998

Blood chemistry - D-dimer (ELISA): sensitive, but not specific (AMI, pneumonia, CHF, cc, surgery) > 500 ng/ml, in 90% of PE, (latex test 50%) negative test: exclude PE - LDH-3 - Bi
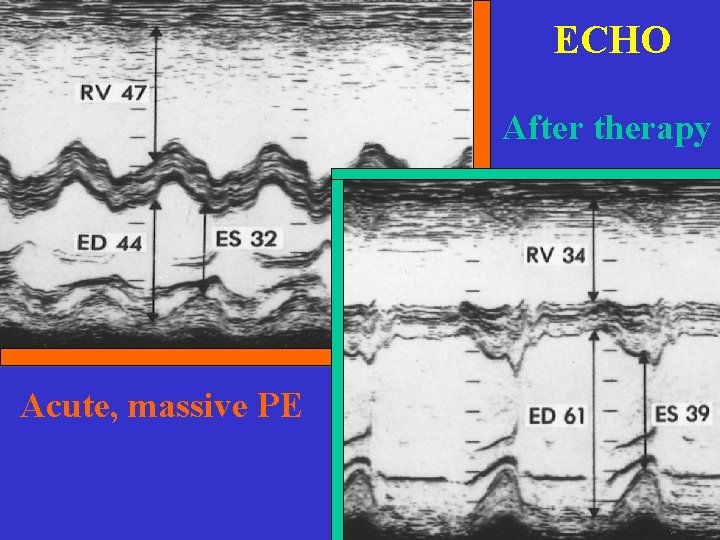
ECHO After therapy Acute, massive PE
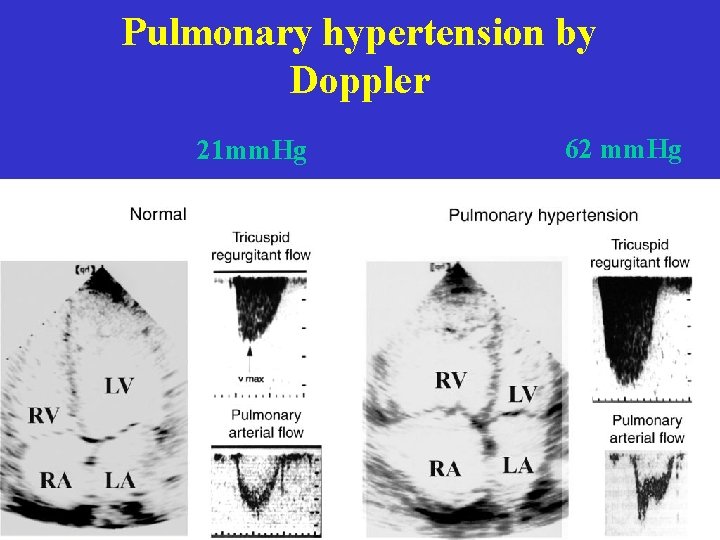
Pulmonary hypertension by Doppler 21 mm. Hg 62 mm. Hg
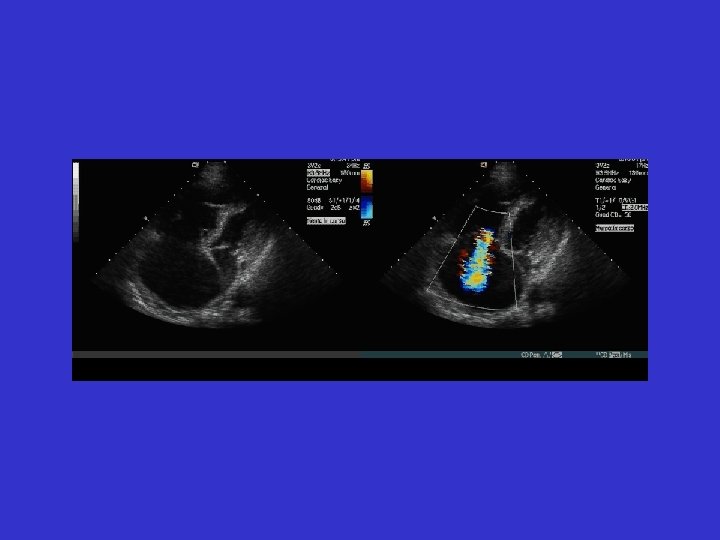
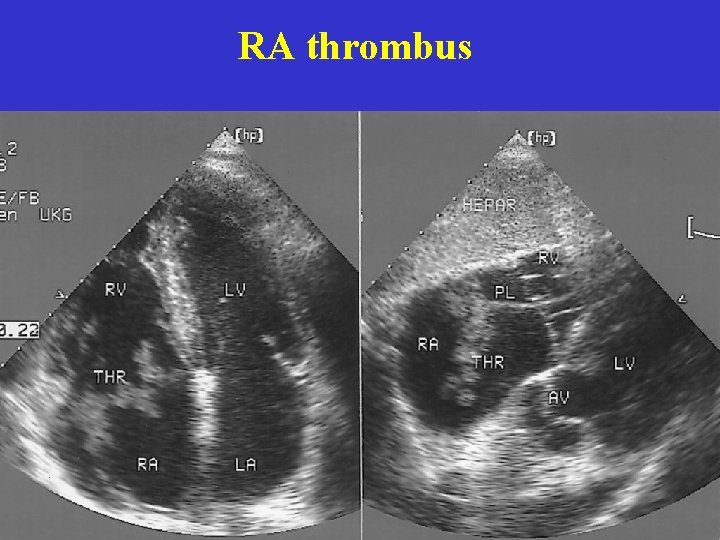
RA thrombus
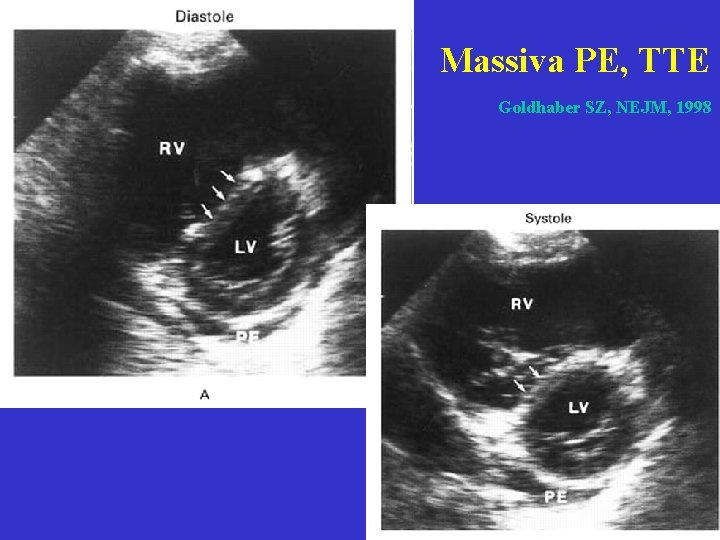
Massiva PE, TTE Goldhaber SZ, NEJM, 1998

Other diagnostic tests • Vascular Doppler of the leg • Inhalation-perfusion scintigraphy: V/Q mismatch • CT angio: central - segmental – subsegmental • Angiography (gold standard)
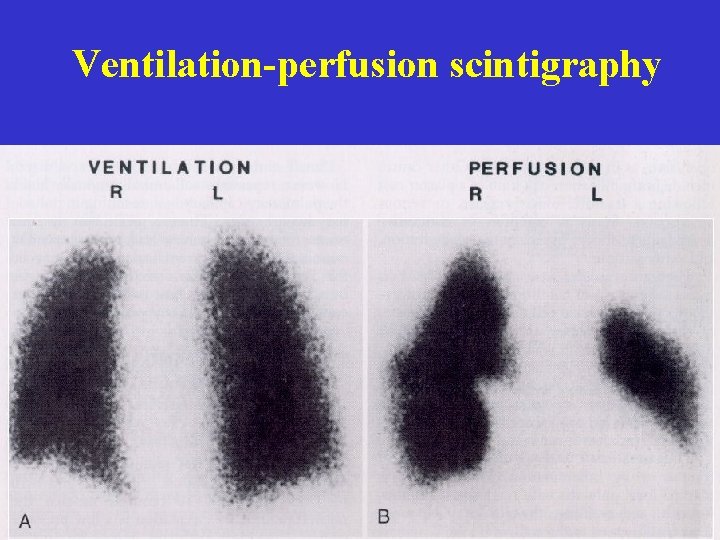
Ventilation-perfusion scintigraphy
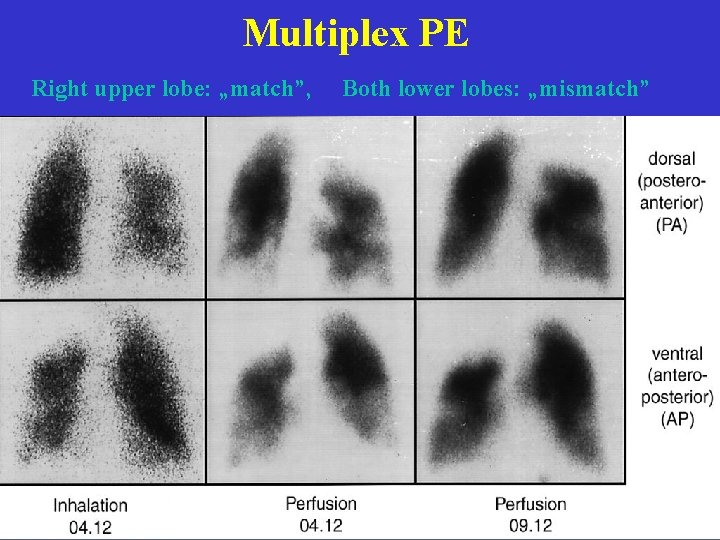
Multiplex PE Right upper lobe: „match”, Both lower lobes: „mismatch”
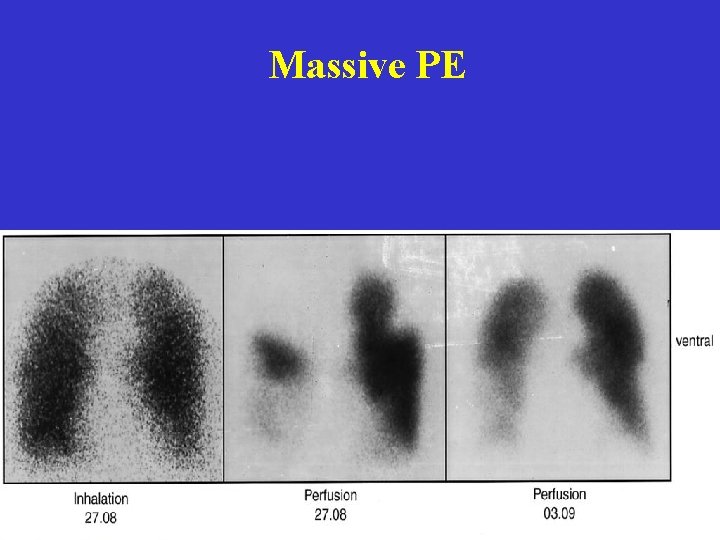
Massive PE
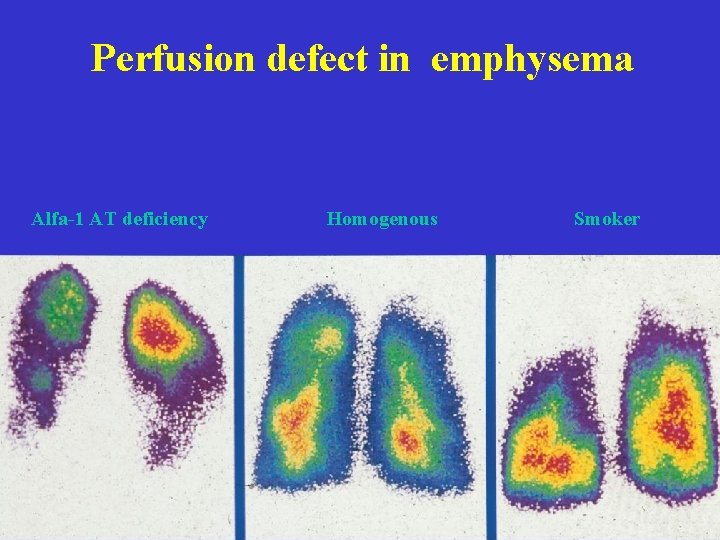
Perfusion defect in emphysema Alfa-1 AT deficiency Homogenous Smoker
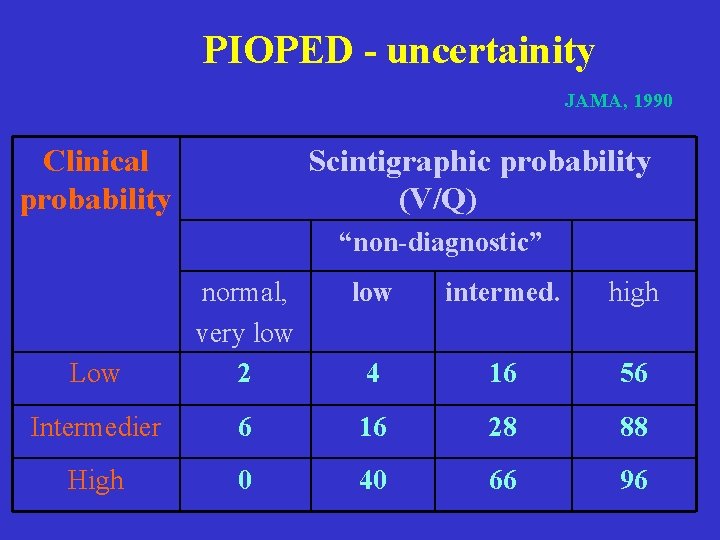

PIOPED - uncertainity JAMA, 1990 Clinical probability Scintigraphic probability (V/Q) “non-diagnostic” low intermed. high Low normal, very low 2 4 16 56 Intermedier 6 16 28 88 High 0 40 66 96
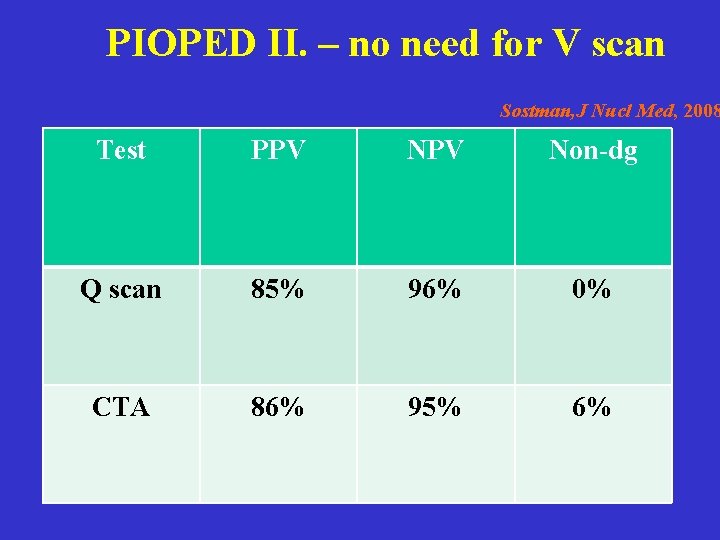
PIOPED II. – no need for V scan Sostman, J Nucl Med, 2008 Test PPV Non-dg Q scan 85% 96% 0% CTA 86% 95% 6%
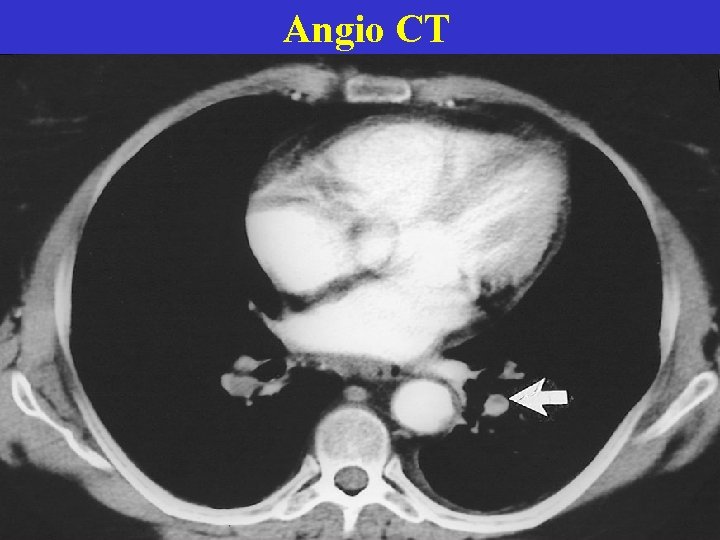
Angio CT
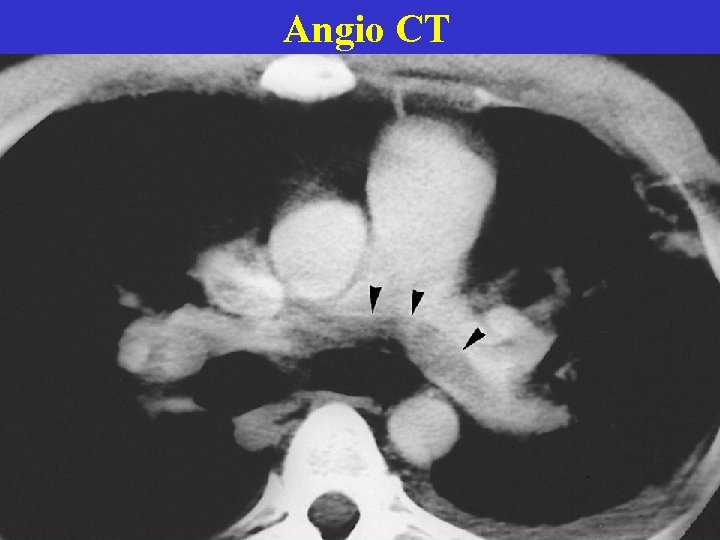
Angio CT
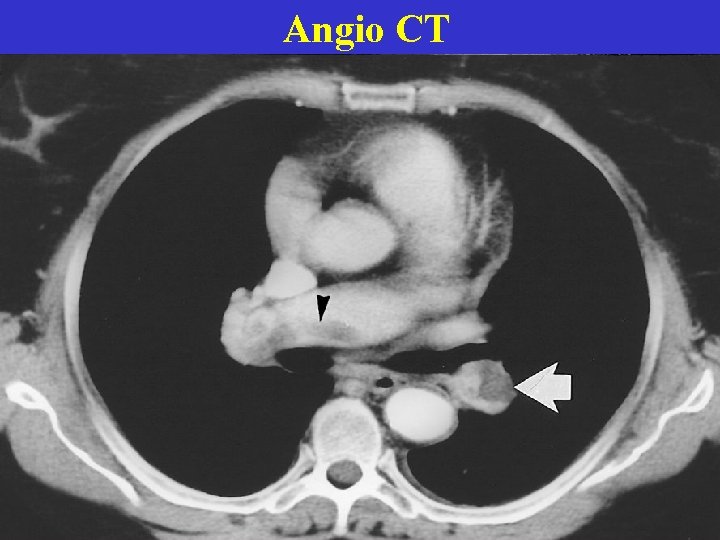
Angio CT
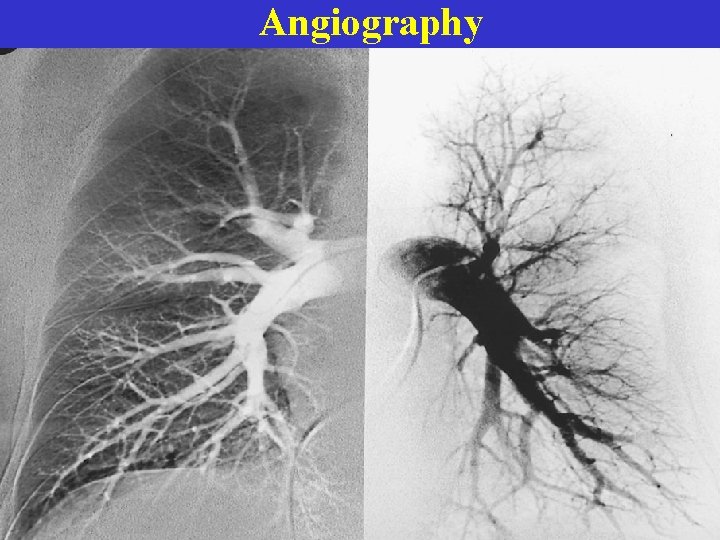
Angiography
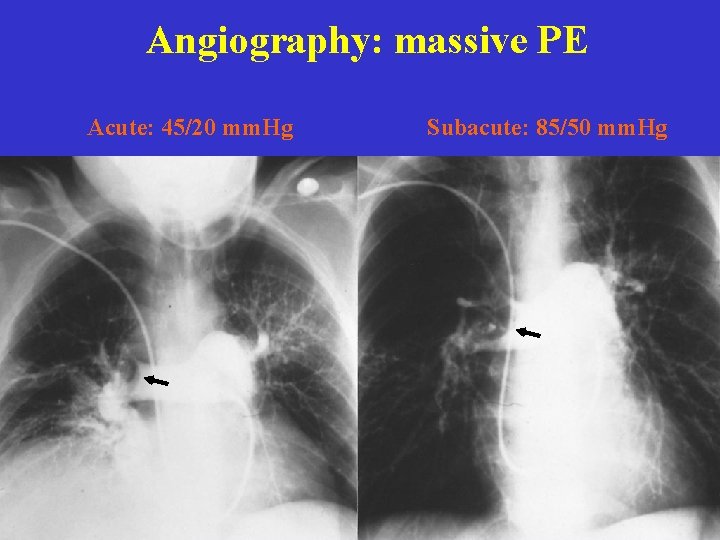
Angiography: massive PE Acute: 45/20 mm. Hg Subacute: 85/50 mm. Hg
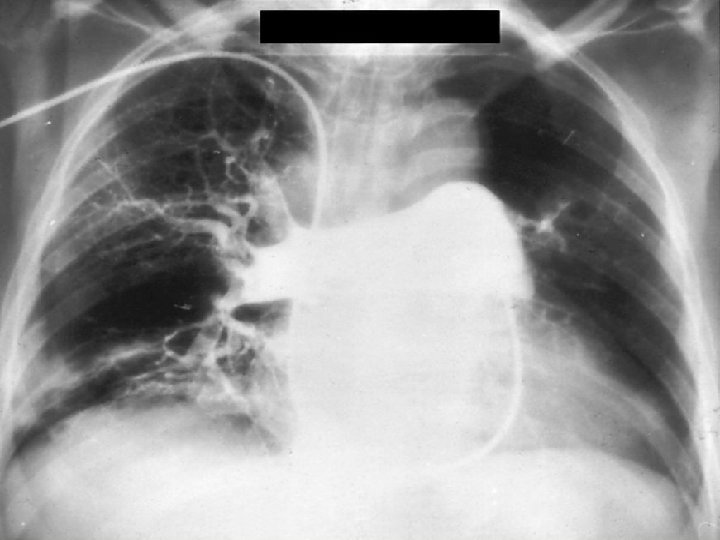
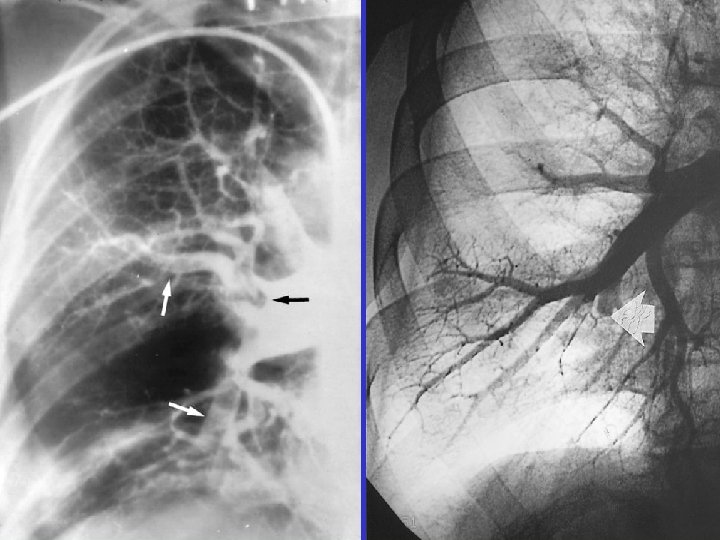
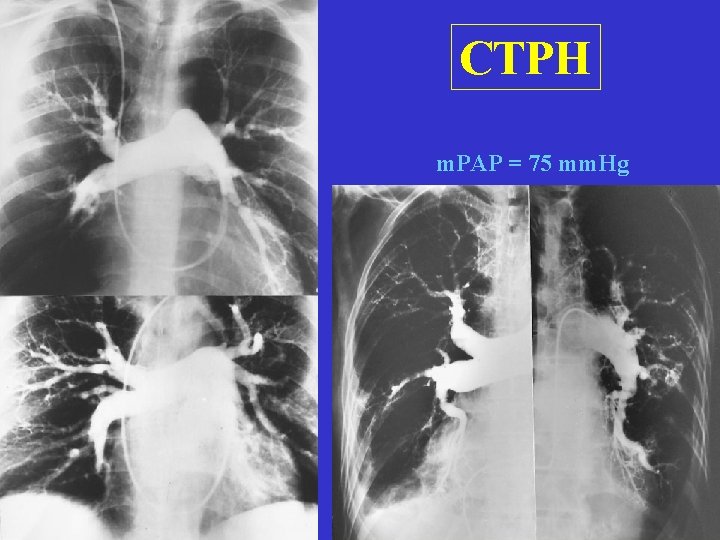
CTPH m. PAP = 75 mm. Hg

Low clinical probability D-dimer (ELISA v. aggl. ) < 500 g/L: - Normál: Nem dg-cus: Magas val. : Ther. (? ) >500 g/L VUS DVT neg. DVT: Ther. V/Q or CT angio

Intermedier clinical probability D-dimer (ELISA) < 500 g/L: - >500 g/L VUS Normál: Non dg: Angio or CT angio: High porbab. : Ther. DVT neg. DVT: Ther. V/Q or CT angio

High clinical probability VUS DVT neg. DVT: Ther. Normal: Non dg: Angio or CT angio: High probab. . : Ther. V/Q or CT angio
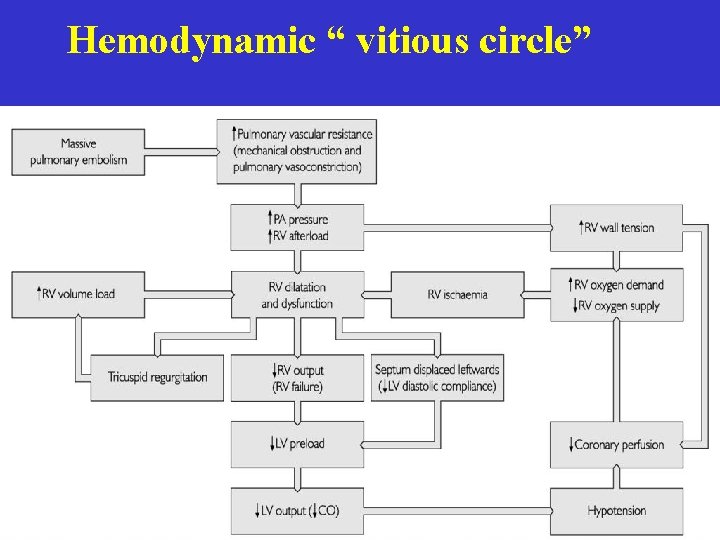
Hemodynamic “ vitious circle”
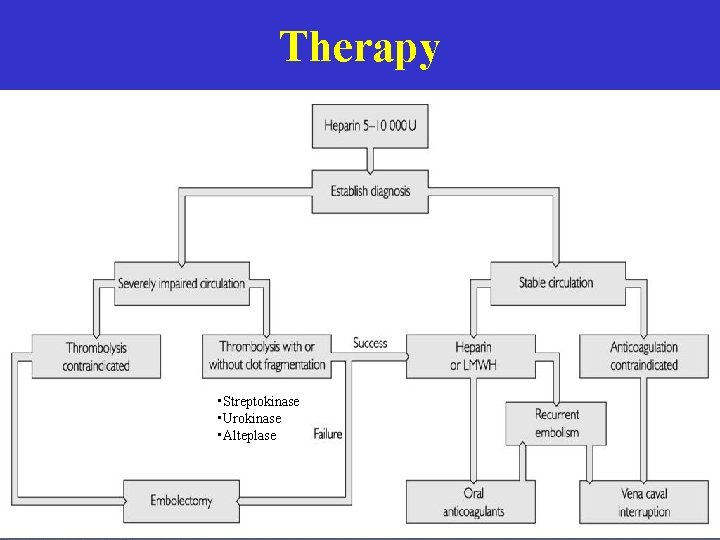
Therapy • Streptokinase • Urokinase • Alteplase

Treatment • Sodium-heparin iv. bolus (5 -10 000 U) followed by either - continouos infusion (control with a. PTI) or - low molecular weight (ultrafractionated) heparin (LMWH) s. c. • Coumarin for 6 -12 months (if irreversible or unknown etiology: lifeterm anticoagulation) therapeutic level: INR: 2 -3

New therapy (NOAC) • Oral thrombin inhibitor - dabigatran (Pradaxa) • Xa inhibitor - rivaroxaban (Xarelto), apixaban (Eliquis) edoxaban (Lixiana) • No need to control coagulability • Side effect: bleeding • Disadvantage: no antidotum, expansive

Rare forms of PE • Fat (trauma, surgery - diffuse alveolar infiltrates) • Septic (osteomyelitis, tricuspid valve endocarditis) • Air (canulla insertion, gynecological intervention) • Amniotic fluid (delivery)

Classification of PH • Postcapillary - LV systolic or diastolic dysfunction - pericardial constriction - LA disease (MS, MI, thrombus), veno-occlusive disease • Precapillary – cor pulmonale - i. PAH - airway or parenchyma disease (COPD, fibrosis, collagen diseases, cancer, resection) - embolism - vasculitis (Wegener-GPA, Churg-Strauss sy -EGPA, CRESTsy, SLE, PN) - Eisenmenger-sy - Alveolar hypoventilation (chest deformity, pleural callus, SAS, neuromuscular diseases) - other (pulmonal stenosis, high altitude, hemoglobinopathies)

Clinical features - Young, middle-aged women - effort dyspnoe, stenocardia - dilated jugular venes, PII ! Diagnostics - EKG - echocardiography - right heart cath (gold standard): m. PAP>25 Hgmm Therpy (i. PAH) - CA antagonist (in case of reversibility) - PD-5 inhibitor, endothelin antagonist, prostaglandin analog

Treatment of CCP • Treatment of primer disease • Oxygen supplementation • Diuretics, vasodilators with caution – preload ! • New vasodilators for i. PAH (PD-5 inhibitors, Pg analogs, endothelin antagonists) • Venesection, in case of polyglobulia • Anticoagulation (IPAH, CTEPH)
- Slides: 54