Pulmonary Embolism Pulmonary Embolism Thrombotic Nonthrombotic Fat Embolism

Pulmonary Embolism

Pulmonary Embolism – Thrombotic – Nonthrombotic • Fat Embolism • Amniotic Fluid Embolism • IVDA (Talc, cotton, etc)

• Venous thromboembolism (VTE), which encompasses deep venous thrombosis (DVT) and pulmonary embolism (PE), is one of the three major cardiovascular causes of death, along with myocardial infarction and stroke.

• PE is the most common preventable cause of death among hospitalized patients • Approximately three of four symptomatic VTE events occur in the community, and the remainder are hospital acquired

• In the United States, the Surgeon General • estimates there are 100, 000 to 180, 000 deaths annually from PE

• Approximately 14 million (M) hospitalized patients are at moderate to high risk for VTE in the United States annually: 6 M major surgery patients and 8 M medical patients with comorbidities such as heart failure, cancer, and stroke.

• The long-term effects of nonfatal VTE lower the quality of life. Chronic thromboembolic pulmonary hypertension is often disabling and causes breathlessness. A late effect of DVT is postphlebitic syndrome, which eventually occurs in more than one-half of DVT patients

PE • Epidemiology – Five million cases of venous thrombosis each year – 10% of these will have a PE – 10% will die – Correct diagnosis is made in only 10 -30% of cases – Up to 60% of autopsies will show some evidence of past PE

PE – 90 -95% of pulmonary emboli originate in the deep venous system of the lower extremities – Other rare locations include • • Uterine and prostatic veins Upper extremities Renal veins Right side of the heart
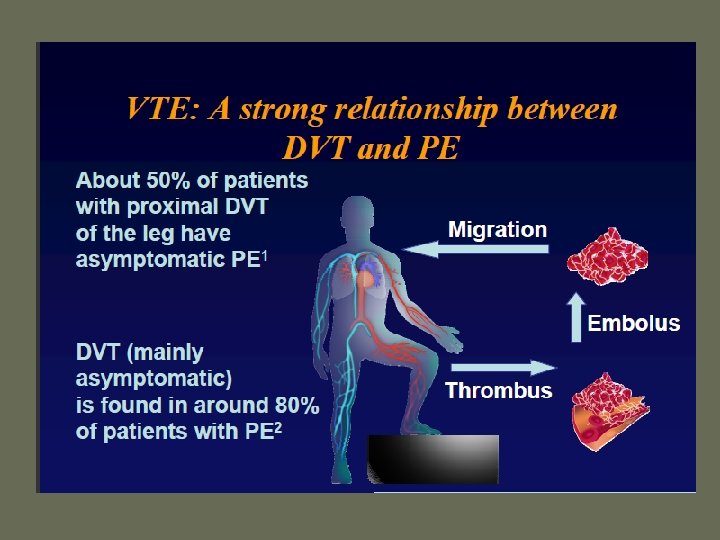
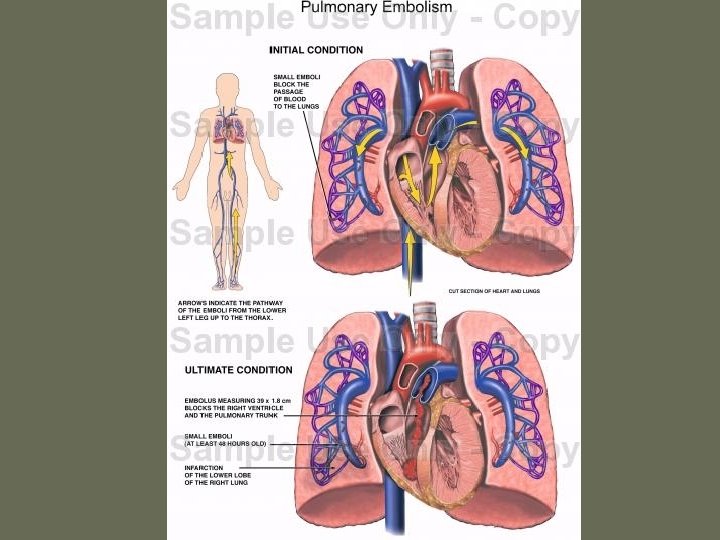
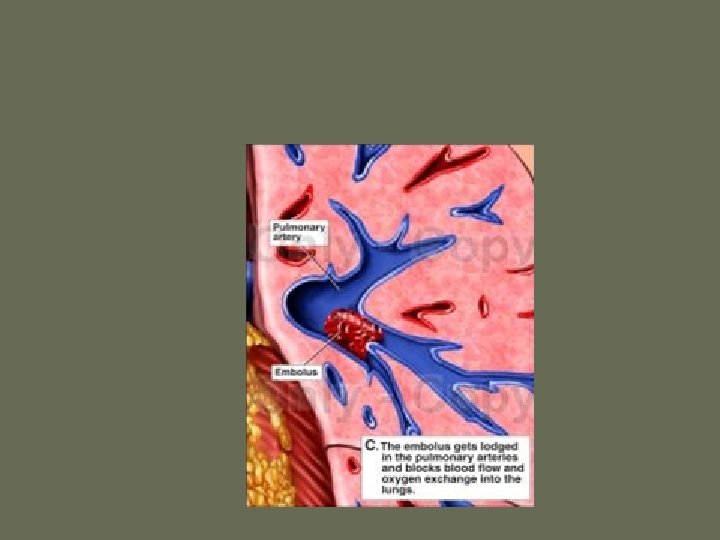

Virchow’s Triad • Rudolf Virchow postulated more than a century ago that a triad of factors predisposed to venous thrombosis – Local trauma to the vessel wall – Hypercoagulability – Stasis of blood flow • It is now felt that pts who suffer a PE have an underlying predisposition that remains silent until a acquired stressor occurs

predisposing factors • • cancer obesity cigarette smoking, hypertension COPD Surgery and trauma chronic kidney disease • • blood transfusion, long-haul air travel , air pollution, oral contraceptives, pregnancy , • postmenopausal hormone replacement,

• • Factor V Leiden mutation Prothrombin gene mutation A 20210 Protein C deficiency Protein S deficiency Antithrombin deficiency Anticardiolipin antibodies Lupus anticoagulant

Factor V Leiden • Most frequent inherited predisposition to hypercoagulability • Resistance to activated Protein C • Single point mutation (Factor V Leiden) • Single nucleotide substitution of glutamine for arginine • Frequency is about 3% in healthy American male physicians participating in the Physicians’ Health Study

PE • When venous emboli become dislodged from their site of origin, they embolize to the pulmonary arterial circulation or, paradoxically to the arterial circulation through a patent foramen ovale – About 50% of pts with pelvic or proximal leg deep venous thrombosis have PE – Isolated calf or upper extremity venous thrombosis pose a lower risk for PE

Pathophysiology • Increased pulmonary vascular resistance • Impaired gas exchange – increased alveolar dead space from vascular obstruction, – hypoxemia from alveolar hypoventilation relative to perfusion in the nonobstructed lung, right-to-left shunting, or impaired carbon monoxide transfer due to loss of gas exchange surface. • Alveolar hyperventilation • Increased airway resistance • Decreased pulmonary compliance

Clinical Syndromes • Pts with massive PE present with systemic arterial hypotension and evidence of dyspnea, syncope, hypotension, and cyanosis • Pts with moderate PE will have right ventricular hypokinesis on echocardiogram but normal systemic arterial pressure • Pts with low risk PE have both normal right heart function and normal systemic arterial pressure

• Clinical Syndromes – Pulmonary Infarction usually indicates a small PE, but is very painful, because it lodges near the innervation of the pleural nerves

Diagnosis • H&P • Always ask about prior DVT, or PE – Family History of thromboembolism – Dyspnea is the most frequent symptom of PE – Tachypnea is the most frequent physical finding – Dyspnea, syncope, hypotension, or cyanosis suggest a massive PE – Pleuritic CP, cough, or hemoptysis
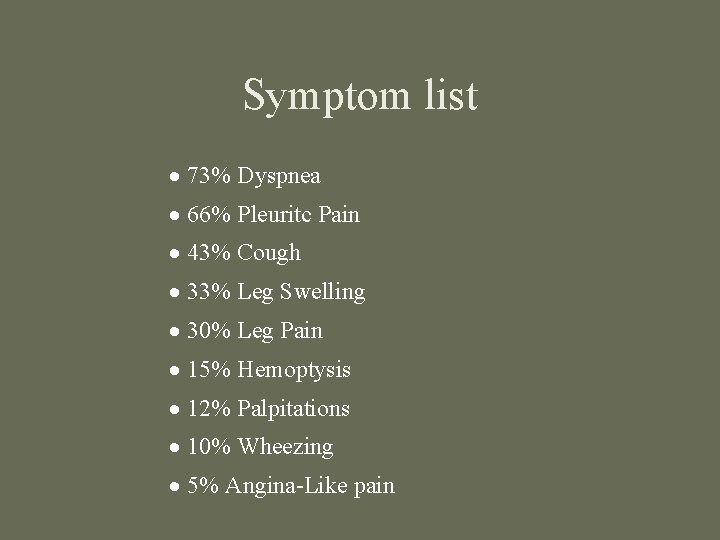

Symptom list · 73% Dyspnea · 66% Pleuritc Pain · 43% Cough · 33% Leg Swelling · 30% Leg Pain · 15% Hemoptysis · 12% Palpitations · 10% Wheezing · 5% Angina-Like pain
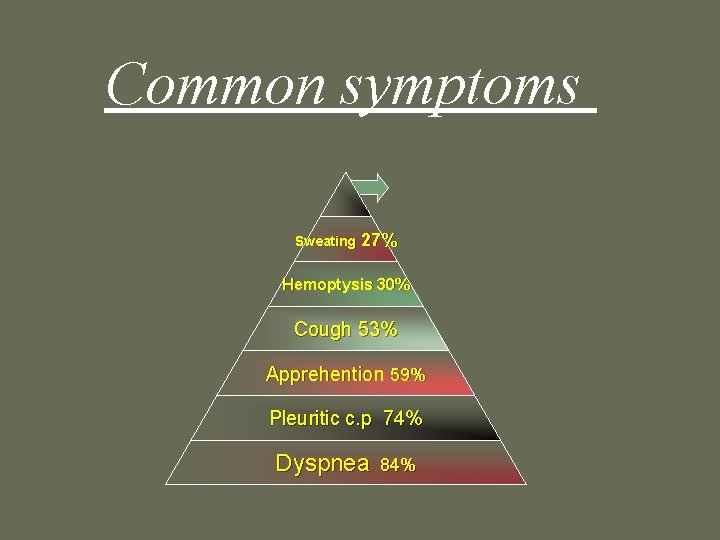
Common symptoms Sweating 27% Hemoptysis 30% Cough 53% Apprehention 59% Pleuritic c. p 74% Dyspnea 84%

Common physical signs Cyanosis 19% Cardiac murmur 23% Thrombophlebitis 32% S 3 OR S 4 34% Fever 43% Tachycardia 44% Rales 58% Tachypnea 92%

Physical Signs & Symptoms · Dyspnea 73% · Pleuritc Pain 66% · Cough 43% · Leg Swelling 33% · Leg Pain 30% · Hemoptysis 15% · Palpitations 12% · Wheezing 10% · Angina-Like pain 5%

Differential Diagnosis • • PE is known as “the great masquerader” Unstable angina , MI Pneumonia, bronchitis CHF Asthma Costochondritis , Rib Fx, Pneumothorax PE can coexist with other illnesses!!

A Summary so Far… • History alone is unreliable • Physical exam is close to useless • However, studies have shown that our clinical suspicion of PE is useful in interpreting diagnostic tests

WELLS CRITERIA • • Suspected DVT 3 An alternative diagnosis is less likely than PE 3 Heart rate > 100 beats / min 1. 5 Immobilization or surgery in pervious 4 week 1. 5 Pervious DVT / PE 1. 5 Hemoptysis 1 Malignancy(on treatment or treated in past 6 1 months )

• Low clinical Likelihood of DVT if Point Score Is Zero or Less; • Moderate Likelihood if Score Is 1 to 2; • High Likelihood if Score Is 3 or Greater

Estimation of Pretest Clinical Probability of Pulmonary Embolism Pretest Clinical Probability Clinical Findings • • • Low-probability (unlikely)1. Symptoms incompatible with pulmonary embolism or compatible symptoms (see below; high-probability section) that can be explained by an alternative process, such as pneumonia, pneumothorax, or pulmonary edema 2. No radiographic or electrocardiographic abnormalities compatible with pulmonary embolism, or findings that can be explained by an alternative diagnosis 3. Absence of risk factors for venous thromboembolism Intermediate-probability (possible/probable)1. Symptoms compatible with pulmonary embolism, but no associated radiographic or electrocardiographic findings 2. Constellation of findings not consistent with low or high clinical probability High-probability (very likely)1. Symptoms compatible with pulmonary embolism (sudden-onset dyspnea, pleuritic chest pain, tachypnea, or syncope), not explained otherwise 2. Radiographic or electrocardiographic findings compatible with pulmonary embolism, or widened alveolar-arterial oxygen gradient, not explained otherwise 3. Presence of risk factors for venous thromboembolism

Diagnosis • Serum Studies – D-dimer • Elevated in more than 90% of pts with PE • Reflects breakdown of plasmin and endogenous thrombolysis • Not specific: Can also be elevated in MI, sepsis, or almost any systemic illness • Negative predictive value – ABG-contrary to classic teaching, arterial blood gases lack diagnostic utility for PE

A-a Gradient – Alveolar arterial oxygen gradient – 148 -1. 2(Pa. CO 2) - Pa. O 2 – Gradient > 15 -20 is considered abnormal. – Done at Room air.

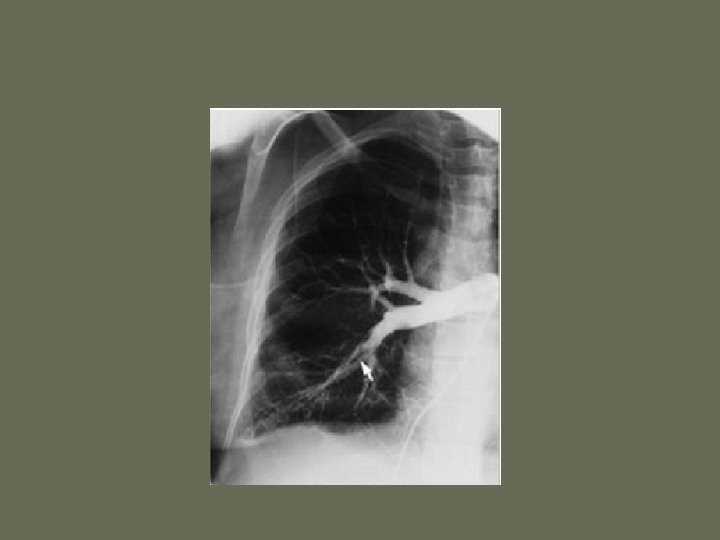
Diagnosis • CXR – Usually reveals a non specific abnormality. 14% normal – Classic abnormalities include: • Westermark’s Sign - focal oligemia • Hampton’s Hump - wedge shaped density • Enlarged Right Descending Pulmonary Artery (Palla’s sign)
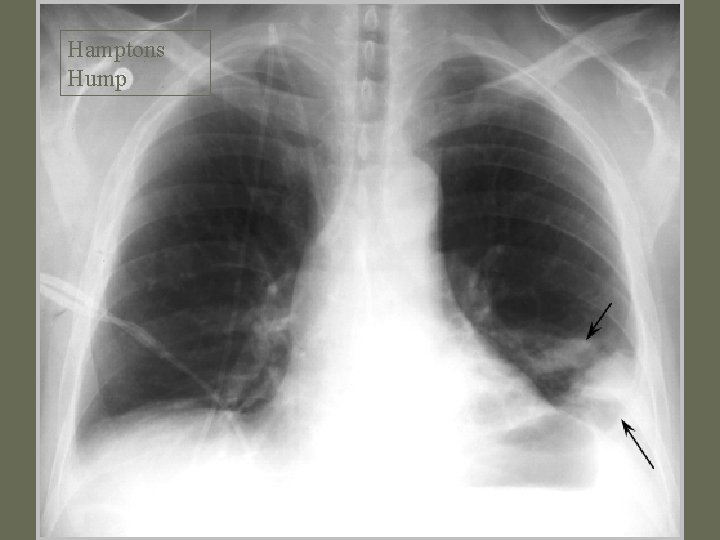
Hamptons Hump PE
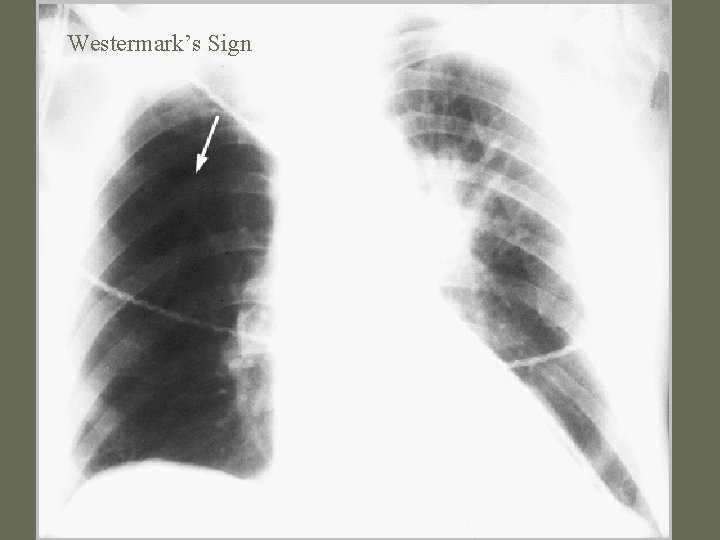
Westermark’s Sign PE
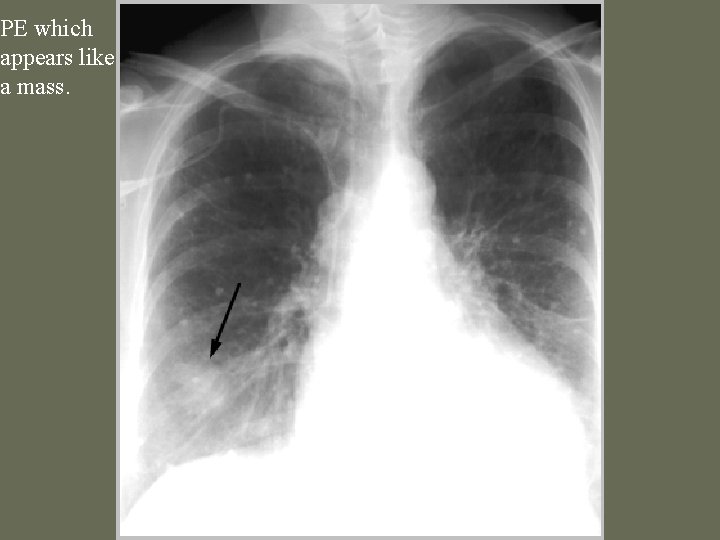
PE which appears like a mass.
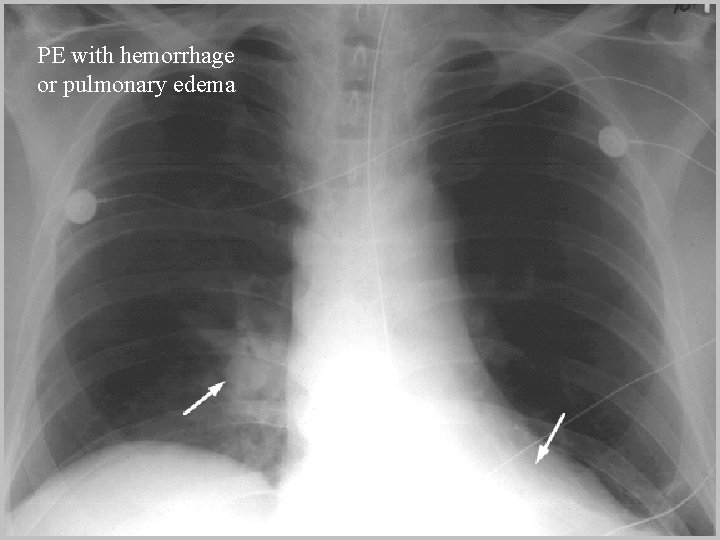
PE with hemorrhage or pulmonary edema
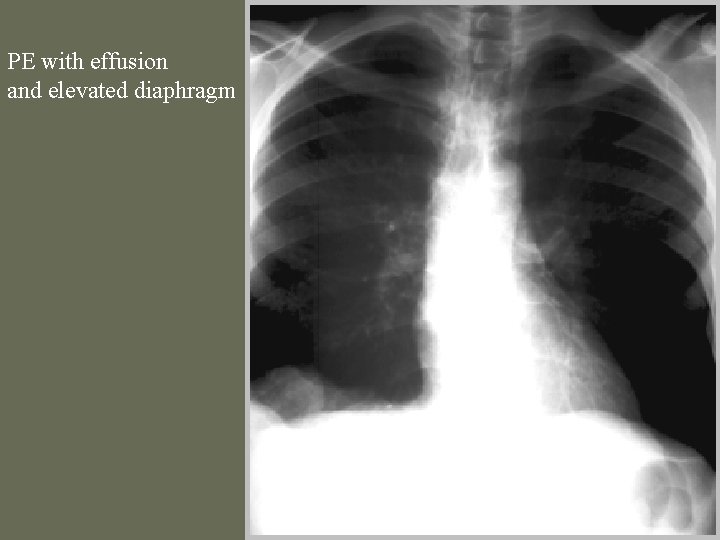
PE with effusion and elevated diaphragm

Venous Ultrasonography • Relies on loss of vein compressibility as the primary criterion • About 1/3 of pts will have no imaging evidence of DVT • Clot may have already embolized • Clot present in the pelvic veins (U/S usually inadequate) – Workup for PE should continue even if dopplers (-) in a pt in which you have a high clinical suspicion
V/Q Scan • Historically, the principal imaging test for the diagnosis of PE – A perfusion defect indicates absent or decreased blood flow – Ventilation scan obtained with radiolabeled gases – A high probability scan is defined as two or more segmental perfusion defects in presence of nl ventilation scan
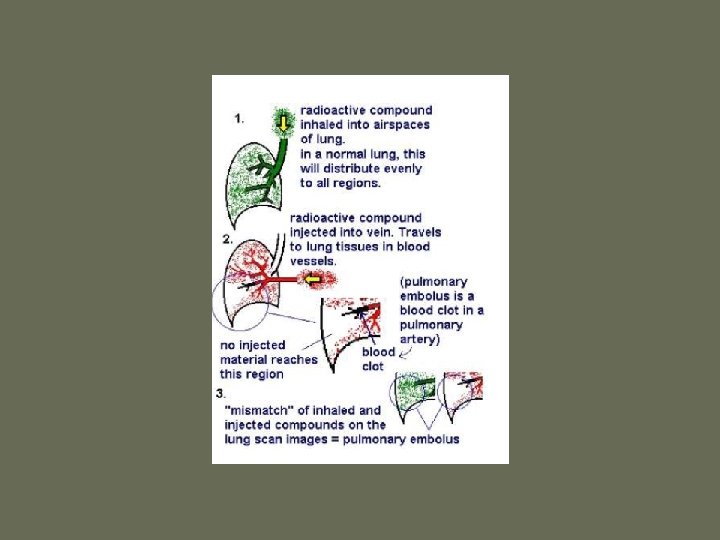

V/Q Scan • Useful if the results are normal or near normal, or if there is a high probability for PE – As many as 40% of pts with high clinical suspicion for PE and low probability scans have a PE on angiogram
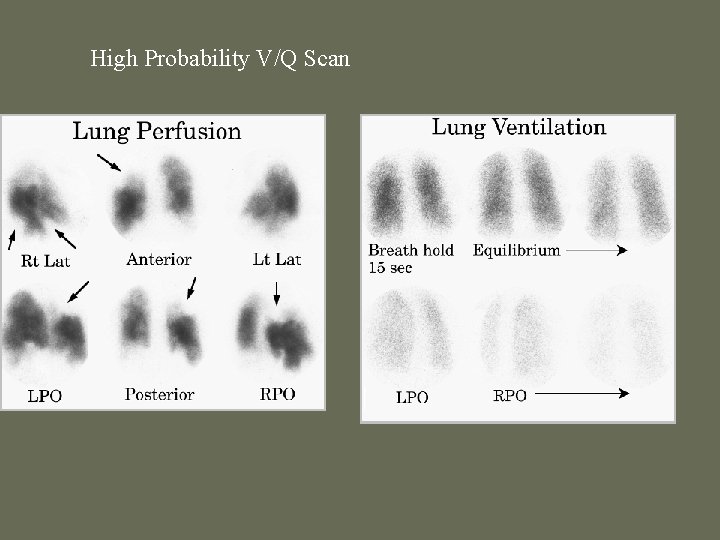
High Probability V/Q Scan

Pulmonary Angiogram • Most specific test available for diagnosis of PE • Can detect emboli as small as 1 -2 mm • Most useful when the clinical likelihood of PE differs substantially from the lung scan result or when the lung scan is intermediate probability

Echocardiogram – Useful for rapid triage of pts – Assess right and left ventricular function – Diagnostic of PE if hemodynamics by echo are consitent with clinical hx

Spiral CT Scan • Identifies proximal PE (which are the ones usually hemodynamically important) • Not as accurate with peripheral PE
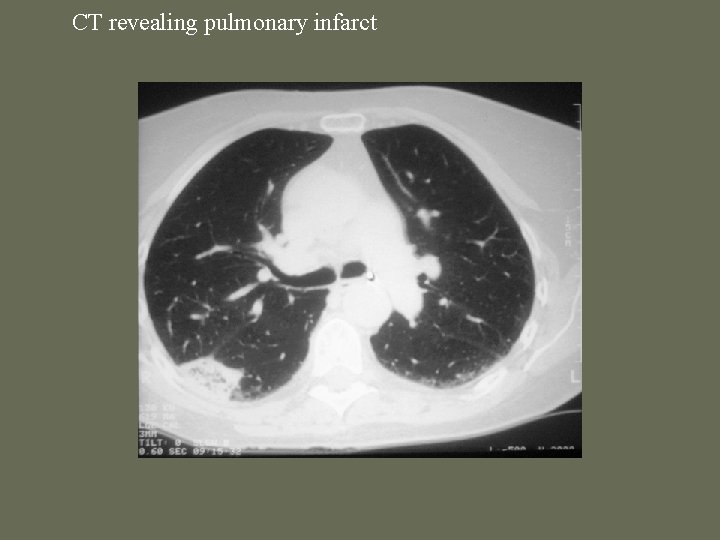
CT revealing pulmonary infarct
DIAGNOSIS OF VENOUS THROMBOEMBOLISM Spiral chest CT scan
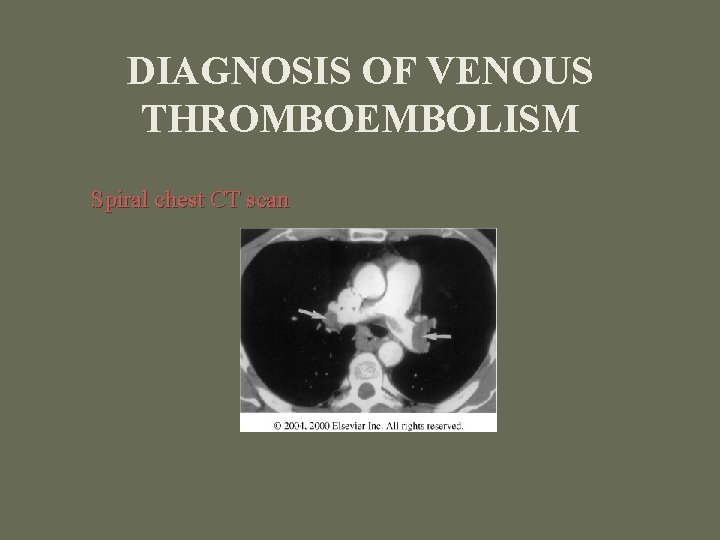
DIAGNOSIS OF VENOUS THROMBOEMBOLISM Spiral chest CT scan

Treatment • Begin treatment with either unfractionated heparin or LMWH, then switch to warfarin (Prevents additional thrombus formation and permits endogenous fibrinolytic mechanisms to lyse clot that has already been formed, Does NOT directly dissolve thrombus that already exists) • Warfarin for atleast 3 months, INR 2 -3

Treatment • Pain Relief • Supplemental Oxygen • Dobutamine for pts with right heart failure and cardiogenic shock • Volume loading is not advised because increased right ventricular dilation can lead to further reductions in left ventricular outflow

Treatment • Thrombolysis 1. Hemodynamically compromised by PE – definitie indication 2. Pulmonary hypertension or right ventricular dysfunction detected by echocardiography, pulmonary arterial catheterization, or new electrocardiographic evidence of right heart stain. (controversial) • Embolectomy – Reserved for pts at high risk for death and those at risk for recurrent PE despite adequate anticoagulation, contraindication for thrombolytics

Adjunctive Therapy • Duration of Anticoagulation – Dependent upon the clinical situation • Cancer, and Obesity most likely will need indefinite treatment • For other pts with isolated calf vein thrombosis (3 mos), proximal leg DVT (6 mos) and PE (1 year) • Inferior Vena Caval Filter • When anticoagulation cannot be undertaken • Recurrent thrombosis despite anticoagulation

Conclusion • PE is often a misdiagnosed clinical disorder. • Rapid identification and appropriate treatment may often prevent unnecessary morbidity and mortality.

• The two principal indications for insertion of an IVC filter are • (1) active bleeding that precludes anticoagulation • (2) recurrent • venous thrombosis despite intensive anticoagulation
- Slides: 56