Pulmonary and Extra Pulmonary Tuberculosis NITMED TUTORIALS Chukwuka

Pulmonary and Extra Pulmonary Tuberculosis © NITMED TUTORIALS Chukwuka J C 3/6/2021

outline �Epidemiology �Pathogenesis �Clinical features �Diagnosis �Treatment �Tb/HIV coinfection �Drug resistance Tb Chukwuka J C 3/6/2021

Expectations �Discuss the epidemiology of Tb �Discuss the pathogenesis of Tb �Identify/diagnose Tb �Discuss the treatment of Tb �Discuss factors militating against Tb control Chukwuka J C 3/6/2021

Brief History of Tuberculosis ~60, 000 BCE Earliest unambiguous detection of MTB in bison remains 4000 BCE MTB in skeletal remains of prehistoric humans 3000 -2400 BCE MTB in fragments of spine from Egyptian mummies 460 BCE Hippocrates first used term phthisis (consumption in Greek) 1020 s Ibn Sina; 1 st physician to identify TB as contagious (developed quarantine) 1720 English physician, Benjamin Marten, published A New Theory of Consumption, hypothesizing that TB could be caused by “wonderfully minute living creatures” 1859 First TB sanatorium opened in Germany 1865 V 1865 Villenim communicable 1882 Dr. Robert Koch discovered a staining technique enabling him to see M. tuberculosis 1890 Tuberculin skin test developed by Koch 1908 -1921 BCG vaccine developed by Calmette and Guèrin 1946 Streptomycin first used in TB patient 1949 -1963 Further drug development: p-ASA (1949), INH (1952), PZA (1954), cycloserine (1955), ETH (1962), Rif (1963) Chukwuka J C 3/6/2021

Epidemiology � 1/3 world population are latently infected � 8 - 10 m new active cases per year � 95% in developing countries � 40 -- 50% are communicable � 2– 3 m deaths per year � 98% in developing countries � 13 m co infection with HIV Chukwuka J C 3/6/2021

Epidemiology �Sub saharan Africa, �Indian subcontinent �Asia �Latin America �Pacific rim Chukwuka J C 3/6/2021

Epidemiology � 80% of all new Tb are 22 HBC � 20 of 22 are in Africa and Asia �>50% of all new cases occur in 5 countries India, China, Indonesia South Africa and Nigeria Chukwuka J C 3/6/2021

why �Migration from endemic areas �Relapse of control program �Inadequate drugs esp Rif �Emergence of drug resistant strains & nosocomial transmission �Hiv epidemic Chukwuka J C 3/6/2021

Epidemiology �Overcrowding �Chronic alcoholism �Low socioeconomic status �Malnutrition �Homelessness �Healthcare workers �HIV Chukwuka J C 3/6/2021

Interaction b/w HIV and Tb �Tb most common cause of death in plwha �Among plwha life time risk of Tb 50%- 5 -10% in HIV –ve people �Hiv increas risk of Tb inf—Tb dis (200 X) �Hiv increas likelihood of new Tb inf �Presence of Tb makes HIV to xply more quickly � 40% HIV-Tb/ 28% Tb-HIV Chukwuka J C 3/6/2021

Epidemiology �Mycob bovis/tuberculosis—gm positive, aerophilic, non motile, non spore forming acid/alcohol fast bacilli �Cell wall has high mycolic acid content �Norcardia & Cryptosporidium �Niacin in culture �Doubling time 18 -24 hrs Chukwuka J C 3/6/2021

Transmission of M. tuberculosis • Spread by droplet nuclei • Expelled when person with infectious TB coughs, sneezes, speaks, or sings • Close contacts at highest risk of becoming infected • Transmission occurs from person with infectious TB disease (not latent TB infection) Chukwuka J C 3/6/2021

Probability TB Will Be Transmitted • Infectiousness of person with TB • Environment in which exposure occurred • Duration of exposure • Virulence of the organism Chukwuka J C 3/6/2021

Conditions That Increase the Risk of Progression to TB Disease • HIV infection • Substance abuse • Recent infection • Chest radiograph findings suggestive of previous TB • Diabetes mellitus • Silicosis • Prolonged corticosteriod therapy • Other immunosuppressive therapy Chukwuka J C 3/6/2021

Conditions That Increase the Risk of Progression to TB Disease (cont. ) • Cancer of the head and neck • Hematologic and reticuloendothelial diseases • End-stage renal disease • Intestinal bypass or gastrectomy • Chronic malabsorption syndromes • Low body weight (10% or more below the ideal) Chukwuka J C 3/6/2021

Pathogenesis �Ingestion/inhalation of droplet nuclei----non specific broncho pneumonia or tonsilitis, febrile illnesss gastroenteritis-----1. healing with granuloma formation (75 -80% stable) 2. massive tissue necrosis 3. lymphohaematogenous spread Chukwuka J C 3/6/2021

� Almost all cases are acq thro Person to person contact thro droplet nuclei � For a droplet nucleus to cause infection it must bypass the upper airway defences to reach the alveoli � Deposition of tubercule bacilli in the alveoli causes vasodilation with influx of PMN & macrophages � Macrophages ingest the tubercul process the mycobac ag & present it to. T lymph –release of lymphokines –attract more macroph-cell mediated immunity Chukwuka J C 3/6/2021

�Macroph that ingest the bacilli dev pale foamy cytoplasm rich in lipids �Crowd together as epitheloid cells to form the tubercule or unit lesion of tb �Aggregation of mono nuclear cells fuse to form langerhan giant cells �Lymphocytes surround the outer margin & in the center a zone of caseous necrosis may appear and subseq calcify Chukwuka J C 3/6/2021
�Bacilli xply slowly in the macro �Proliferation of tb bacilli in caseous tissue— softening & liquefaction of caseous material �Discharge-cavity �Extension to blood vessel-hemoptysis/miliary spread �Discharge into major bronchus collapse/suffocation Chukwuka J C 3/6/2021

�In those in whom the initial assault is contained the only evidence is a positive skin test----infected �With clinical disease—tb disease �Point where mycob settles in the lung-ghon focus �Ghon focus+regional lymph node-primary complex Chukwuka J C 3/6/2021

Clinical presentationymptoms Most important symptoms § Cough lasting more than 3 weeks and not responding to § § § usual antibiotic treatment Production of purulent, sometimes blood- stained sputum Evening fevers Night sweats Weight loss Anorexia Extra pul bloody urine, back pains, headache /confusion Chukwuka J C 3/6/2021

Evaluation for TB Chukwuka J C • Medical history • Physical examination • Mantoux tuberculin skin test • Chest radiograph • Bacteriologic or histologic exam 3/6/2021

Medical History • Symptoms of disease • History of TB exposure, infection, or disease • Past TB treatment • Demographic risk factors for TB • Medical conditions that increase risk for TB disease Chukwuka J C 3/6/2021

Test for Mycobacterium infection • Preferred method of testing for TB infection in adults and children is TST useful for - Examining person who is not ill but may be infected. But repeated tests are misleading Inteferon gamma release assays Quantiferon Tb Gold and TB spot test - Chukwuka J C 3/6/2021

Direct detection of Mycobacterium Tests Microscopic examination of specimen of sputum that has been stained by the Ziehl-Neelsen (ZN) method A PTB suspect should submit two sputum samples for microscopy: Chukwuka J C • Sample 1: On first visit, the patient should provide an on-the-spot sputum sample • Sample 2: Give the patient a sputum container to take home for an early morning sample on the following day (day 2) 3/6/2021

Diagnostic tests, continued � An inpatient can provide 2 early morning sputum samples � False negative reports: due to sample being inadequate or faulty smear preparation/interpretation Chukwuka J C 3/6/2021
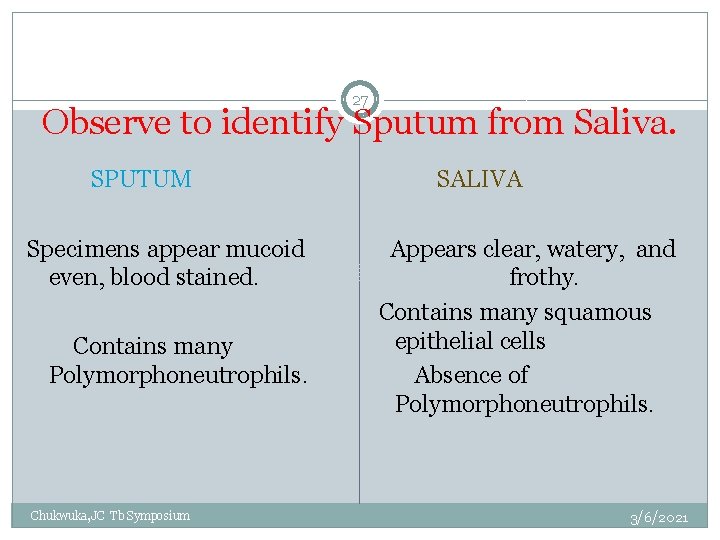
27 Observe to identify Sputum from Saliva. SPUTUM SALIVA Specimens appear mucoid even, blood stained. Contains many Polymorphoneutrophils. Appears clear, watery, and frothy. Contains many squamous epithelial cells Absence of Polymorphoneutrophils. Chukwuka, JC Tb Symposium 3/6/2021
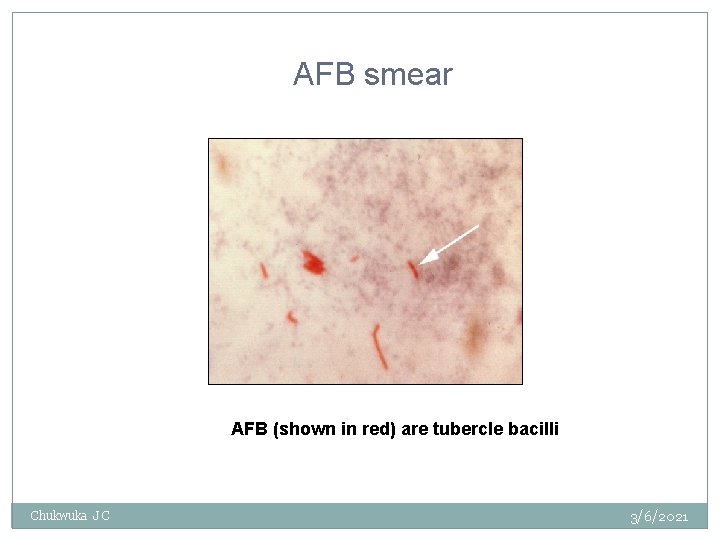
AFB smear AFB (shown in red) are tubercle bacilli Chukwuka J C 3/6/2021

Smear Examination • Strongly consider TB in patients with smears containing acid-fast bacilli (AFB) • Results should be available within 24 hours of specimen collection • Presumptive diagnosis of TB Chukwuka J C 3/6/2021

Limitation of Microscopy for Tuberculosis. �Repeated sample examinations, load on technical staff. �Training and dedication of Microscopist. �The load of bacilli must be more than 10, 000 / ml of sputum. �Low in sensitivity < 50 % �Repeated requests for samples �High drop out by patients, for repeated samples. �Not dependable in pediatric age group. 3/6/2021 Chukwuka, JC Tb Symposium 30

Processing Direct smear negative specimens �Sputum Microscopy can be improved with Sputum liquefaction, concentration and gravity sedimentation. �Popular solvents Sodium hypochlorite. Sodium hydroxide. Ammonium sulphate N-acetyl-L-cysteine –sodium hydroxide. 3/6/2021 Chukwuka, JC Tb Symposium 31

Benefits of Liquefaction and Concentration �Major studies showed processing of sputum with chemicals and centrifugation improved sensitivity up to 18 %. �Incremental yield ( positive with bleach minus positives with Ziehl – Neelsen stain) up to 9 %. �Use of Sodium hypochlorite to treat specimens Mycobactericidal and also kills HIV and improves the safety and acceptability by technical staff. 3/6/2021 Chukwuka, JC Tb Symposium 32

Growing role of Fluorescent Microscopy �There is a growing need for screening for AFB by Fluorescent Microscopy. �Several studies prove fluorescent Microscopy in Diagnosis of Tuberculosis is a priority, �Developing world should opt and initiate fluorescent microscopy. 3/6/2021 Chukwuka, JC Tb Symposium 33

Why we need Fluorescent Microscopy � Useful when few bacilli are present. � Increases the sensitivity in HIV patients with tuberculosis. � Reduces the time needed for testing. � About 15 times as many fields of view can be scanned by fluorescent microscopy than by Ziehl – Neelsen’method in the same period. � Increases the sensitivity by 10 % � Better conclusions with one or two specimens, unlike Ziehl Neelsen’s method needing 3 or > 3 specimens. 3/6/2021 Chukwuka, JC Tb Symposium 34

Acid Fast Bacilli as seen under Fluorescent Microscope 3/6/2021 Chukwuka, JC Tb Symposium 35

Nucleic acid amplification test �Gene. Xpert MTB/RIF early identification, treatment, improved outcome, interruption of transmission and effective public health intervention. Identifies Rif resistance as well. �Unfortunately, presence of blood on the specimen marked diminishes it’s efficacy Chukwuka J C 3/6/2021

Culturing Mycobacterium �Culturing for isolation of Mycobacterium spp continues to be a Gold standard, particularly in Developing countries. �Need only 10 – 100 bacilli / 1 ml of sputum. �BACTEC, MGIT, Versa. Trek , MBBACT 4 -14 days �Solid medium 3 -6 weeks 3/6/2021 Chukwuka, JC Tb Symposium 37

Culturing Most useful in �Surveillance, �Drug sensitivity testing patterns. �Identify treatment failures. � Useful in Patients presenting with respiratory symptoms, X- ray’s suggestive, but smear negative. Can prove culture positive. �Cultures remain suggestive and helpful in early treatment periods, failed drug regimes. 3/6/2021 Chukwuka, JC Tb Symposium 38

Cultures • Use to confirm diagnosis of TB • Culture all specimens, even if smear negative • Results in 4 to 14 days when liquid medium systems used Colonies of M. tuberculosis growing on media Chukwuka J C 3/6/2021

Resistance testing �Drug sensitivity testing �Gene. Xpert MTB/RIF �Line probe assays using PCR �Lucipherase gene Chukwuka J C 3/6/2021

Diagnosis contd Radiology � If TB is still suspected despite negative smears, a chest x-ray should be done. Classical pattern is upper lobe infiltrates with cavitation � However, no chest x-ray is absolutely typical of PTB patients with HIV infection In severe immunosuppression, the appearance is often atypical, as described below Chukwuka J C 3/6/2021
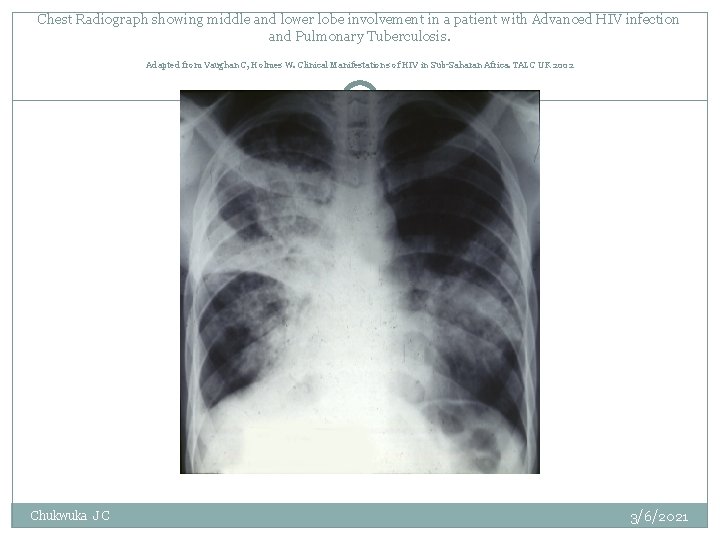
Chest Radiograph showing middle and lower lobe involvement in a patient with Advanced HIV infection and Pulmonary Tuberculosis. Adapted from Vaughan C, Holmes W. Clinical Manifestations of HIV in Sub-Saharan Africa. TALC UK 2002 Chukwuka J C 3/6/2021
Overview, continued With mild immunosuppression: �Typical chest x-ray (CXR) findings include: �upper lobe and or bilateral infiltrates �cavitation �pulmonary fibrosis �shrinkage �Clinical picture often resembles postprimary pulmonary TB (PTB) �Sputum smear is usually positive Chukwuka J C 3/6/2021
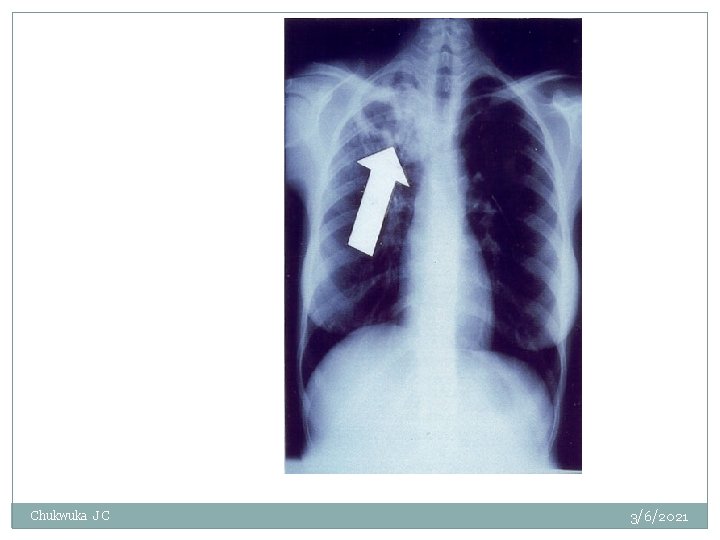
Arrow points to cavity in patient's right upper lobe --typical finding in patient with TB Chukwuka J C 3/6/2021

Overview, continued In severely immunosuppressed patient, the features are atypical, resembling that of primary PTB: § sputum smear often negative § CXR shows interstitial infiltrates especially in lower zones with no features of cavitation and fibrosis § CXR may look exactly like that in bacterial pneumonia § In the setting of an HIV epidemic, it is not possible to look at a CXR and say that it is or is not TB Chukwuka J C 3/6/2021

Diagnosis �CXR /FBC ESR /HIV �ZN for AAFB in sputum, bx specimen �Dovers/lowestein-jensen broth/middlebrook 8/52 �Radiometric detection 14 C 3/52 � direct id pcr, HPLC, HPGC, Nucleic acid hybridization, monoclonal abs �Luciferase phage system Chukwuka J C 3/6/2021

Treatment �C 1 SP Tb, SN wit ext parenchymal involvement, severe EPTb— 2 HRZE+4 HR/4 HR(b) �C 2 previous treatment 3 HRZES 2 5 HRE(b) �C 3 SN, less ext 2 HRZ+6 HE �C 4 Chronic Tb Chukwuka J C 3/6/2021

�R Rifampicin 600 mg daily �E Ethambutol 800 mg daily �H Isoniazid 300 mg daily �Z Pyrazinamide 1 gm daily Chukwuka J C 3/6/2021

Treatment, continued Treatment approaches and strategies � Directly observed treatment, short course (DOT) § § § Chukwuka J C It is difficult to adhere to anti-TB treatment for 6 -8 months or more It is also difficult to predict which patients will adhere to self-administered treatment One certain way to ensure patient adherence is through DOT where a trained supervisor watches the patient swallow the drugs 3/6/2021

Basic principles of DOT, continued § § For patients who need admission, DOT should be started right away and supervised by the nursing staff For patients requiring no admission or for discharged patients, DOT may be supervised by staff of a nearby health facility, a trained community health worker, or a trained family member Chukwuka J C 3/6/2021

Treatment, continued Drug regimens � Initial phase—first 2 -3 months During the initial phase, there is rapid killing of TB bacilli Three or more drugs are used in combination Infectious patients become non-infectious within about 2 weeks and symptoms usually improve Chukwuka J C 3/6/2021

Treatment, continued § Chukwuka J C Continuation phase-additional 4 -6 months • Fewer drugs are necessary (usually 2), but longer time • These drugs eliminate the remaining bacilli 3/6/2021

Treatment, continued Monitoring during treatment � Bacterial monitoring is only possible for patients with smear positive PTB � Sputum smear exam should be done as follows § § At the time of diagnosis At the end of initial phase During the continuation phase—at the end of month 5 On completion of treatment—month 6 or 8 � chest x-ray as appropriate Chukwuka J C 3/6/2021

Treatment of TB for HIV-Positive Persons • Management of HIV/TB is complex • Care for HIV-related TB should be provided by or in consultation with experts in management of both HIV and TB Chukwuka J C 3/6/2021

Treatment of TB for HIV-Positive Persons (cont. ) RIF-based regimens generally recommended for persons On first line therapy who are not on Nevirapine Initial treatment phase should consist of • Isoniazid (INH) • Rifampin (RIF) • Pyrazinzamide (PZA) • Ethambutol (EMB) RIF may be used with some Pls and NNRTIs Chukwuka J C 3/6/2021

Treatment of TB for HIV-Positive Persons (cont. ) • For patients receiving Pis / on SLD, initial treatment phase may consist of - Isoniazid (INH) - Rifabutin (RFB) - Pyrazinamide (PZA) - Ethambutol (EMB) • An alternative nonrifamycin regimen includes Chukwuka J C 3/6/2021 INH,

Candidates for Treatment of LTBI Positive skin test result $5 mm • HIV-positive persons • Recent contacts of a TB case • Persons with fibrotic changes on chest radiograph consistent with old TB • Patients with organ transplants and other immunosuppressed patients Chukwuka J C 3/6/2021

Prevention �Treatment of latent infection esp high risk patients �INH 9/12; 6/12 �Rif 4/12 �Rif/PZA 2 -3/12 �Bacilli calmette guerin BCG �Infection control Chukwuka J C 3/6/2021

Working Definitions & Concepts - 1 � Drug Resistant TB: A patient is determined to have drug resistant TB only if there is a laboratory confirmation of invitro resistance to one or more first-line anti-TB drugs. � Confirmed mono-resistance: TB in patients whose infecting isolates of Mycobacterium tuberculosis are confirmed to be resistant to in vitro one first-line anti-TB drug. � Confirmed poly-resistance: TB in patients whose infecting isolates of M. tuberculosis are resistant in vitro to more than one first-line drug other than isoniazid and rifampicin. Chukwuka J C 3/6/2021

Working Definitions & Concepts - 2 �Confirmed multi-resistance (MDR-TB): TB in patients whose infecting isolates of M. tuberculosis are resistant in vitro to both isoniazid and rifampicin. �Extensive drug resistance (XDR-TB): MDR plus Resistance to: A fluoroquinolone : Ciprofloxacin, Ofloxacin, Levofloxacin, Moxifloxacin, Gatifloxacin, etc + One or more of the following injectable agents: Kanamycin, Amikacin, Capreomycin Chukwuka J C 3/6/2021

Background - 1 � Drug resistance to Streptomycin (1 st anti-TB drug) identified in 1944 � With the advent of rifampicin in the 70 s, resistance soon began to occur � By the mid-1990 s, most countries involved in global survey of anti-TB drug resistance registered cases of MDR-TB � In 2006, a more severe form of drug resistance, extensive drug resistance (XDR) TB emerged � Globally, about 500, 000 MDR-TB cases occur annually � About 58, 000 MDR-TB cases occur annually in Africa Chukwuka J C 3/6/2021

Background - 2 � Burden of MDR-TB in Nigeria is 4. 8% overall, 2. 9% and 14. 3% among new and retreatment cases respectively. � WHO estimates MDR-TB rates of 1. 8% and 9. 3% among new and re-treatment cases respectively � About 5 -10, 000 of MDR-TB cases believed to occur annually � Available but limited institution-based DST reports show MDR-TB rate of 60 -80% among re-treatment cases Chukwuka J C 3/6/2021

� The result of the National MDR survey (2009 -2010) no gender difference in �Economically active age group is most involved �All the 6 geopolitical zones of the country have MDR cases �Highest occurrence is the SWZ. �Important to have DST before instituting treatment in Retreatment cases as per the new WHO guidelines. �HIV positive 2. 9% and negative 5, 7% Chukwuka J C 3/6/2021

Causes of Drug Resistant TB – Programmatic Factors - 1 � Absence of and/ or inappropriate guidelines � Poor regulatory policy on anti-TB drugs � Poorly organized or funded TB control programmes/no DOTs/payment for ant-TB drugs � Unavailability of certain drugs (stocks-outs or delivery disruptions) � Supply of poor quality drugs � Poor training � Poor or no monitoring of treatment Chukwuka J C 3/6/2021

Causes of Drug Resistant TB – Provider Related Factors - 2 �Non compliance with guidelines �Inappropriate or inadequate prescription of anti-TB drugs (i. e. wrong dose or combination) �Adding single drugs to a failing regimen �Poor drug storage conditions. Chukwuka J C 3/6/2021

Causes of Drug Resistant TB – Patient Related Factors - 3 � Poor adherence or poor DOT � Lack of and/or inadequate patient & family education on TB � Lack of money (especially) if treatment is not free) � Lack of transportation (if facility is far) � Adverse drug effects � Social barriers � Malabsorption � Drug or substance dependency disorders Chukwuka J C 3/6/2021

Issues in DR-TB control in the African Region �Poor DOTS programme performance generating DR-TB cases �Unknown burden of DR-TB cases �Limited laboratory capability for TB culture and anti-TB DST �Unavailability of SLD for treating MDR & XDR-TB cases �High TB/HIV co-infection and Infection control challenges �Inadequate human resources & Health worker /community awareness about DR-TB �Poor / non existent DR-TB monitoring and evaluation systems Chukwuka J C 3/6/2021

Possible Forces Driving DR-TB in Nigeria -2 �Inadequate DOTS coverage and implementation �Sub-optimal treatment outcomes: treatment success still below 85%; high defaulter/transfer out rates (>10%); re-treatment rates averages 8% of case finding �Poor drug and logistics management resulting in recurrent outages �Limited access to mycobacateria culture and drug susceptibility testing: delayed diagnosis and hence on-going transmission Chukwuka J C 3/6/2021

Possible Forces Driving DR-TB in Nigeria - 2 �Use of non-standardized second-line anti-TB drugs including fuoroquinolone mono-therapy in the management of MDR-TB cases �Poor regulatory policy on marketing of anti-TB drugs in the country �Poor infection control measures and practices Chukwuka J C 3/6/2021

�SLD from GLC are available �Treatment available at UCH, Lagos and Calabar �Nnewi is being set up now. Chukwuka J C 3/6/2021

Conclusions: Tuberculosis �Preventable disease �Curable disease �Basic public health control essential Adherence Follow up �HIV co-infection complicates �Diagnostics essential Culture Resistance testing Chukwuka J C 3/6/2021

3/6/2021 Chukwuka J C

Expectations �Discuss the epidemiology of Tb �Discuss the pathogenesis of Tb �Identify/diagnose Tb �Discuss the treatment of Tb �Discuss factors militating against Tb control Chukwuka J C 3/6/2021

� THANK YOU! Chukwuka J C 3/6/2021
- Slides: 74