PULLING FEMORAL SHEATHS Shannon Haskett RN BSN June

PULLING FEMORAL SHEATHS Shannon Haskett, RN, BSN June 30, 2015 5 Main Nursing Staff

Learner Centered Objectives ◦ The learner will able to identify procedures and reasons why a sheath may be placed. –Cognitive Domain ◦ The learner will be able to list the different sizes of sheaths that are placed in the artery during a cath lab procedure. Cognitive Domain ◦ Staff nurses will be able recognize when to pull the sheath. -Cognitive Domain ◦ Staff nurses will state the reasoning in palpating the femoral and pedal pulse before sheath removal. -Cognitive Domain ◦ Staff nurses will be able to explain all the steps involved in pulling an arterial sheath. ◦ Staff nurses will be to discover if there is internal or external bleeding during or post sheath pull. -Cognitive Domain ◦ Staff nurses will be able to apply their knowledge from this lesson with future sheath pulls and groin complications. Cognitive Domain ◦ Staff nurses will have less anxiety about pulling sheaths on future patients. -Affective Domain ◦ Staff nurses will have alleviated fear about taking care of patients with sheaths or post sheath removal. -Affective Domain ◦ Staff nurses will be competent in pulling arterial sheaths after being checked off during three sheath pulls by another competent RN. –Psychomotor Domain

Introduction ◦ What is a sheath? ◦ Hollow tube placed in the blood vessels of the arms or legs (Cleveland Clinic, 2014). ◦ Used to make a puncture incision by a physician for catheterization lab procedures ◦ Femoral artery is the preferred placement
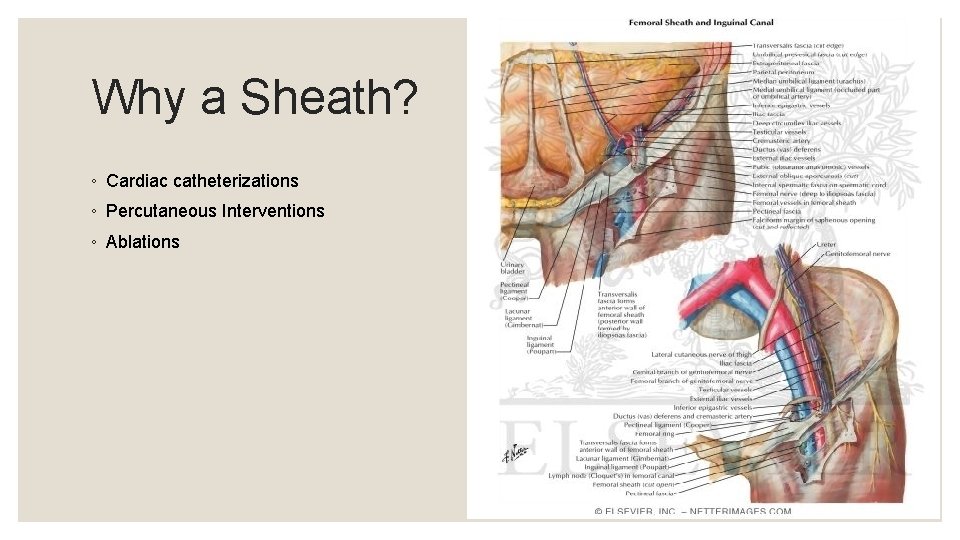
Why a Sheath? ◦ Cardiac catheterizations ◦ Percutaneous Interventions ◦ Ablations

Why a Sheath? : Heart Catheterizations and Interventions ◦ Used for access for a wire to get to the heart ◦ Guided through radiographies and contrast dye ◦ Heart caths can diagnose heart disease, measure heart function, perform hemodynamic monitoring, and measure lung pressures ◦ Left heart catheterizations can lead to an intervention ◦ Interventions require anticoagulation ("Centre for Education and Practive Development, " 2008)
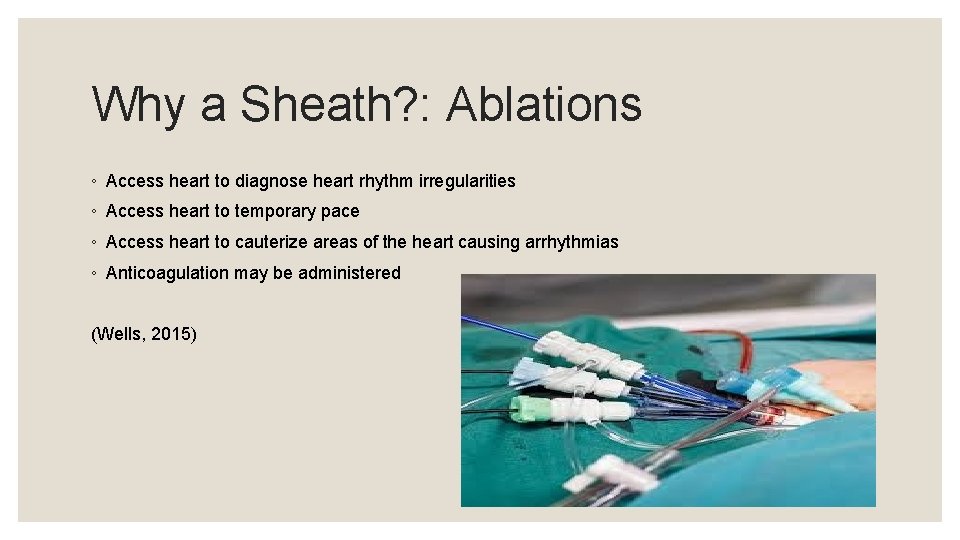
Why a Sheath? : Ablations ◦ Access heart to diagnose heart rhythm irregularities ◦ Access heart to temporary pace ◦ Access heart to cauterize areas of the heart causing arrhythmias ◦ Anticoagulation may be administered (Wells, 2015)
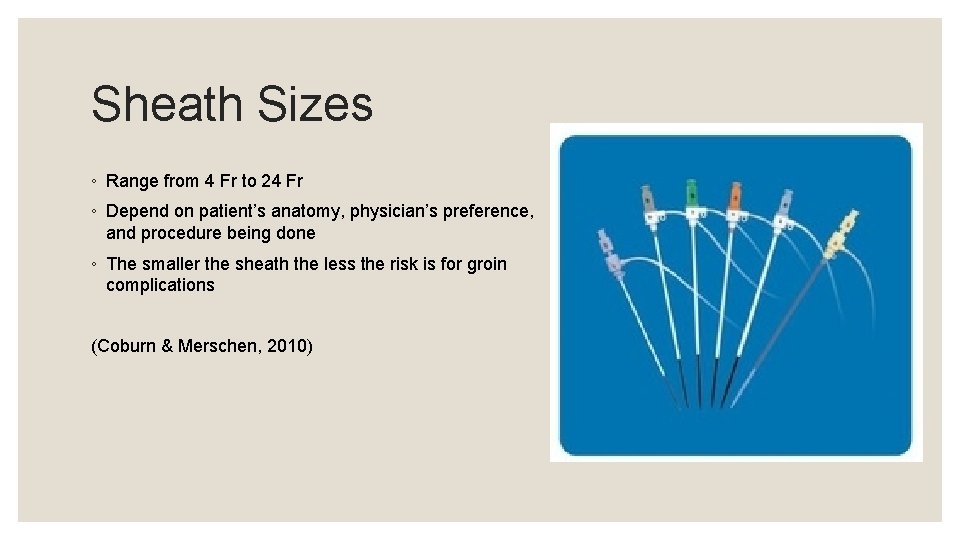
Sheath Sizes ◦ Range from 4 Fr to 24 Fr ◦ Depend on patient’s anatomy, physician’s preference, and procedure being done ◦ The smaller the sheath the less the risk is for groin complications (Coburn & Merschen, 2010)

When Should the Sheath be Removed? ◦ Physician Order ◦ Dependent of the use of coagulation ◦ Checking an ACT
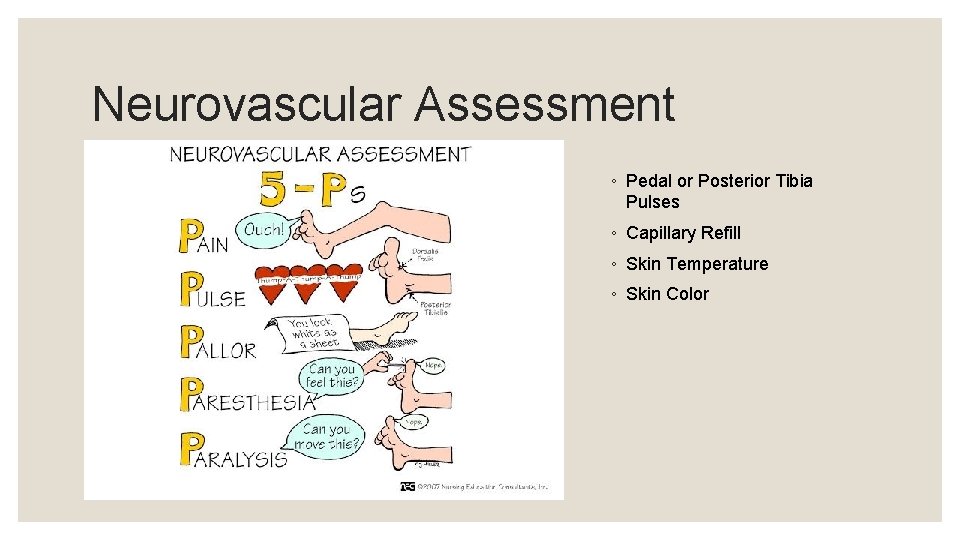
Neurovascular Assessment ◦ Pedal or Posterior Tibia Pulses ◦ Capillary Refill ◦ Skin Temperature ◦ Skin Color
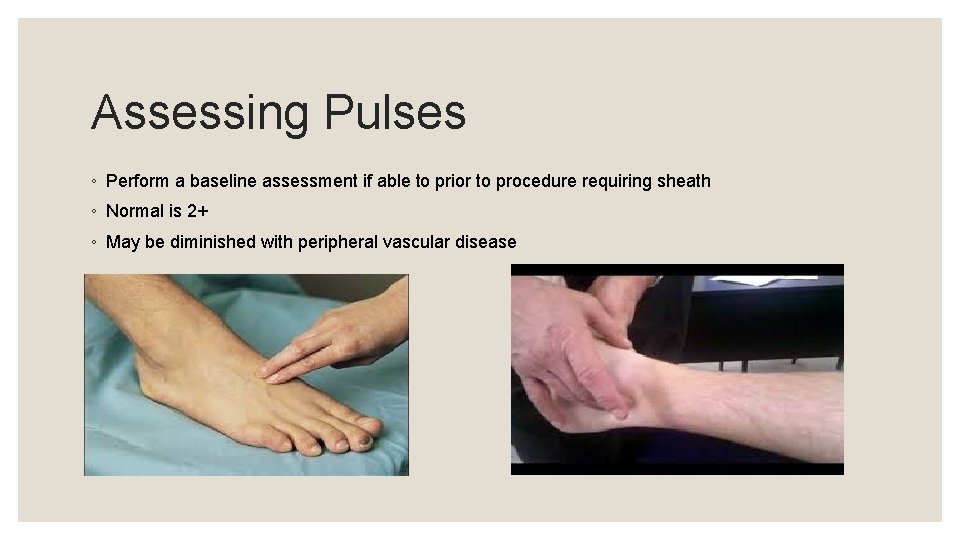
Assessing Pulses ◦ Perform a baseline assessment if able to prior to procedure requiring sheath ◦ Normal is 2+ ◦ May be diminished with peripheral vascular disease
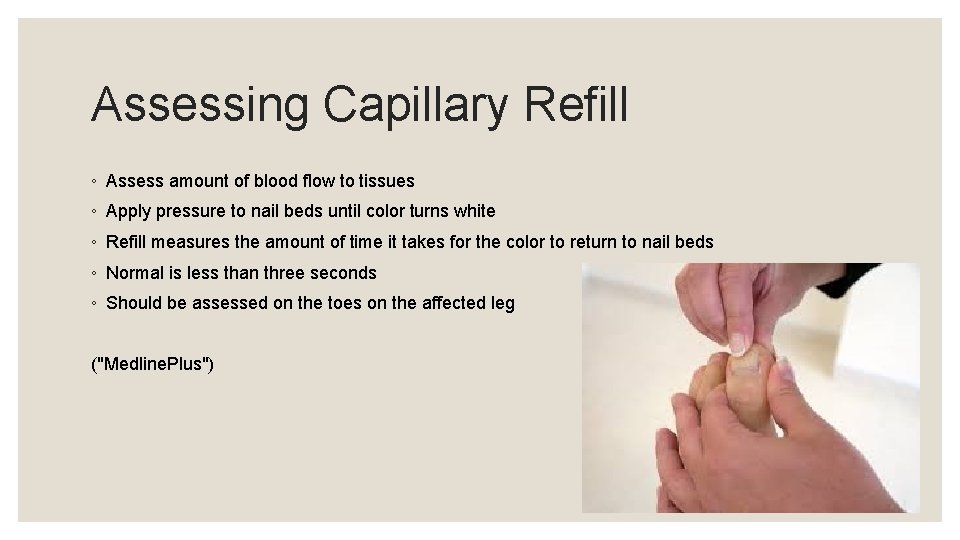
Assessing Capillary Refill ◦ Assess amount of blood flow to tissues ◦ Apply pressure to nail beds until color turns white ◦ Refill measures the amount of time it takes for the color to return to nail beds ◦ Normal is less than three seconds ◦ Should be assessed on the toes on the affected leg ("Medline. Plus")

Assessing Skin Temperature ◦ Normal skin should be warm ◦ Assess baseline temperature before sheath placement ◦ Cool skin can be a sign of peripheral vascular disease or a loss in circulation
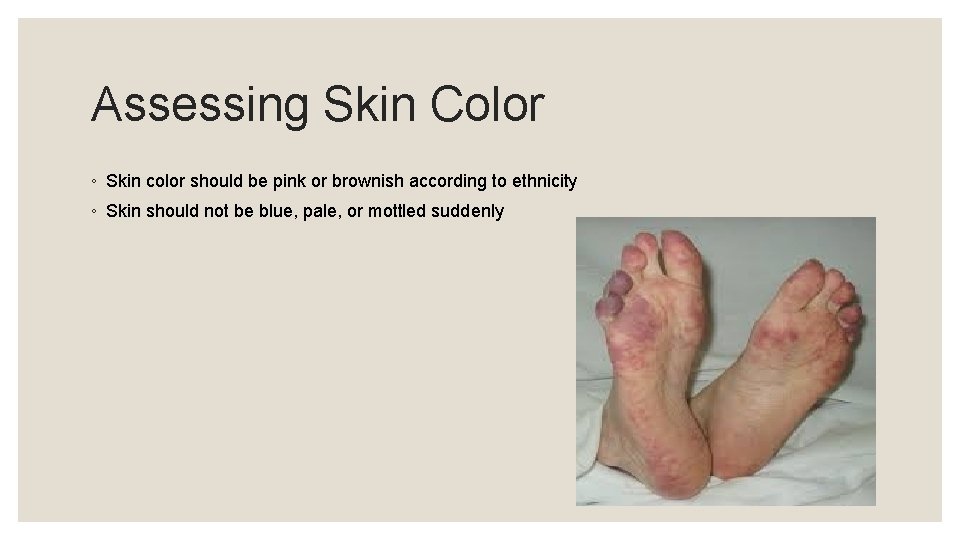
Assessing Skin Color ◦ Skin color should be pink or brownish according to ethnicity ◦ Skin should not be blue, pale, or mottled suddenly
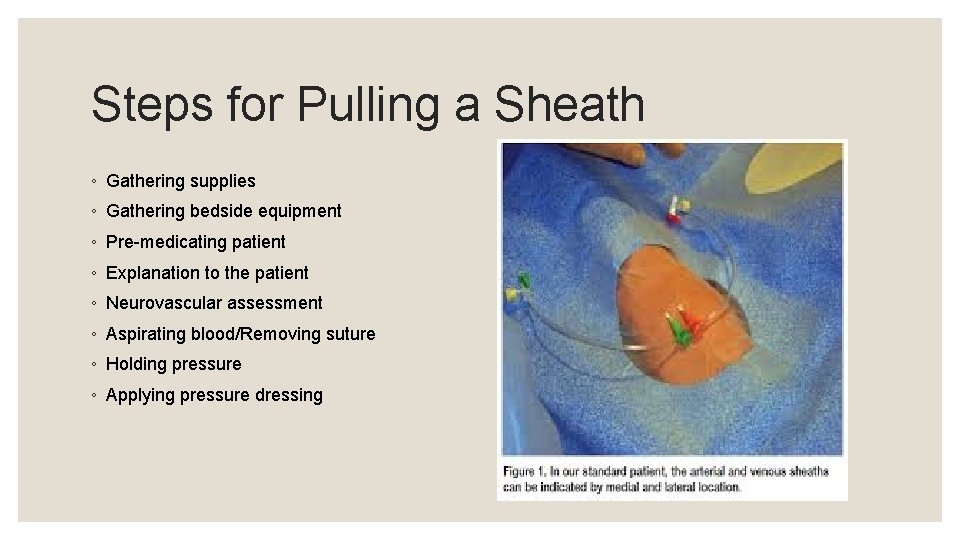
Steps for Pulling a Sheath ◦ Gathering supplies ◦ Gathering bedside equipment ◦ Pre-medicating patient ◦ Explanation to the patient ◦ Neurovascular assessment ◦ Aspirating blood/Removing suture ◦ Holding pressure ◦ Applying pressure dressing

Supplies ◦ Gloves ◦ 10 cc syringe ◦ Box of 4 x 4 sterile gauze ◦ Kerlex ◦ Tegraderm ◦ Xeroform tape ◦ Antibiotic ointment ◦ Atropine ◦ IV fluids

Bedside Equipment ◦ Two nurses at the bedside ◦ Vital sign machine ◦ Telemetry ◦ Bedside heart monitor

Pre-Medicating Patient ◦ Assess need for pain medication ◦ Assess allergy or sensitivity of medications ◦ Physician order ◦ PO or IV medications

Explanation to Patient ◦ Alleviate fear and anxiety ◦ Comfort measures ◦ Involve the patient

Neurovascular Assessment ◦ Pedal or Posterior Tibia Pulses ◦ Capillary Refill ◦ Skin Temperature ◦ Skin Color

Aspiration and Suture Removal ◦ Aspirate blood from sheath or sheaths ◦ Approximately 10 cc ◦ Aspirate to remove clots ◦ Remove sutures with a blade or suture removal kit if present

Removal and Holding Pressure ◦ Locate femoral pulse ◦ Hold at the pulse for arterial sheaths ◦ Hold at the puncture or below the puncture for venous sheaths ◦ Use 4 x 4 guaze ◦ 10 -20 minutes ◦ Assess for groin complications

Applying Pressure Dressing ◦ Hemostasis achieved ◦ Apply antibiotic ointment ◦ Folded 4 x 4 ◦ Apply tegraderm ◦ Place kerlex on top ◦ Place xeroform tape hip to hip or hip to inner thigh ◦ Sandbag ◦ Bedrest

Vasovagal Response ◦ Vagal nerve stimulation ◦ Patient “bearing down” or tensing up ◦ Bradycardia ◦ Hypotension ◦ Nausea/Vomiting ◦ Pallor ◦ Diaphoresis ◦ IV fluid bolus ◦ 0. 5 mg Atropine IV push ("Centre for Education and Practive Development, " 2008)

Complications ◦ Hemorrhaging ◦ Hematoma ◦ Psuedoaneurysm ◦ Retroperitoneal Bleed ◦ Loss of Circulation ◦ Infection
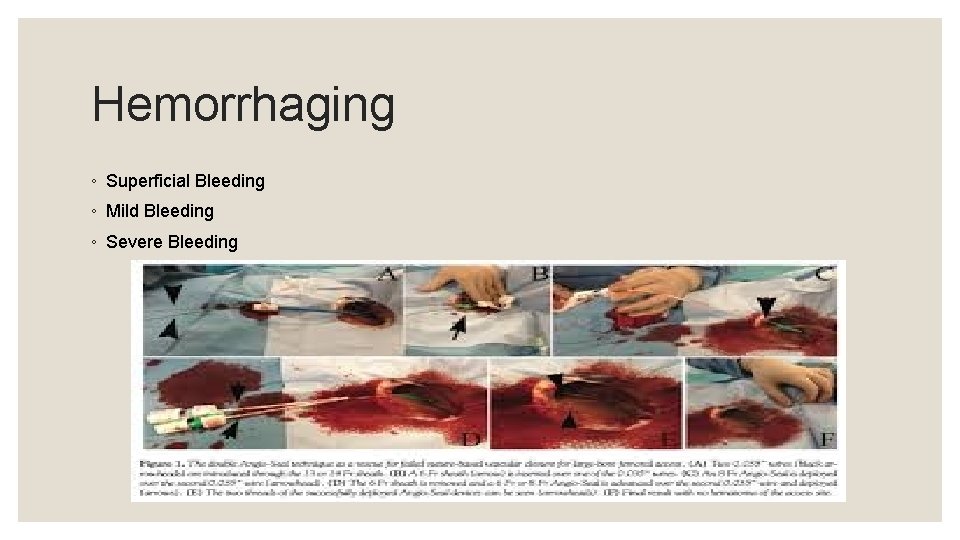
Hemorrhaging ◦ Superficial Bleeding ◦ Mild Bleeding ◦ Severe Bleeding
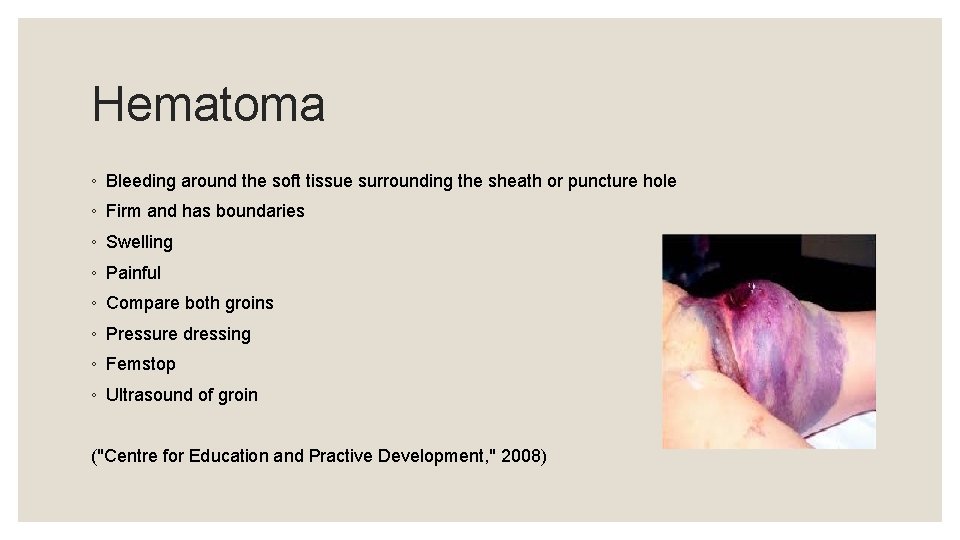
Hematoma ◦ Bleeding around the soft tissue surrounding the sheath or puncture hole ◦ Firm and has boundaries ◦ Swelling ◦ Painful ◦ Compare both groins ◦ Pressure dressing ◦ Femstop ◦ Ultrasound of groin ("Centre for Education and Practive Development, " 2008)
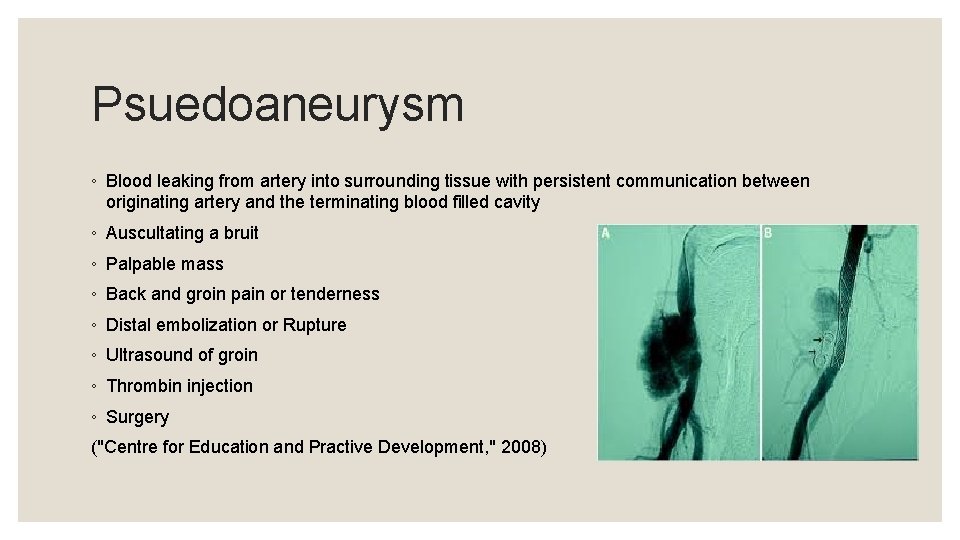
Psuedoaneurysm ◦ Blood leaking from artery into surrounding tissue with persistent communication between originating artery and the terminating blood filled cavity ◦ Auscultating a bruit ◦ Palpable mass ◦ Back and groin pain or tenderness ◦ Distal embolization or Rupture ◦ Ultrasound of groin ◦ Thrombin injection ◦ Surgery ("Centre for Education and Practive Development, " 2008)
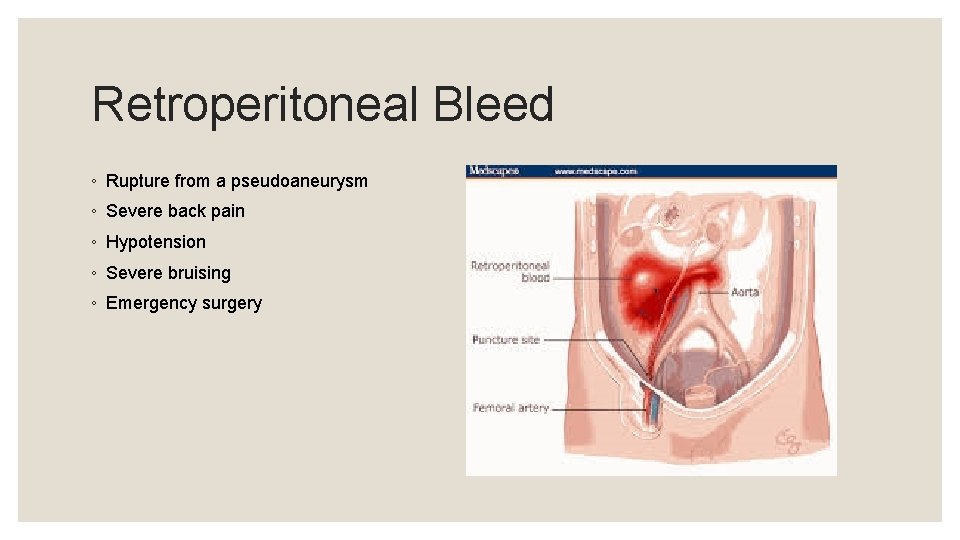
Retroperitoneal Bleed ◦ Rupture from a pseudoaneurysm ◦ Severe back pain ◦ Hypotension ◦ Severe bruising ◦ Emergency surgery
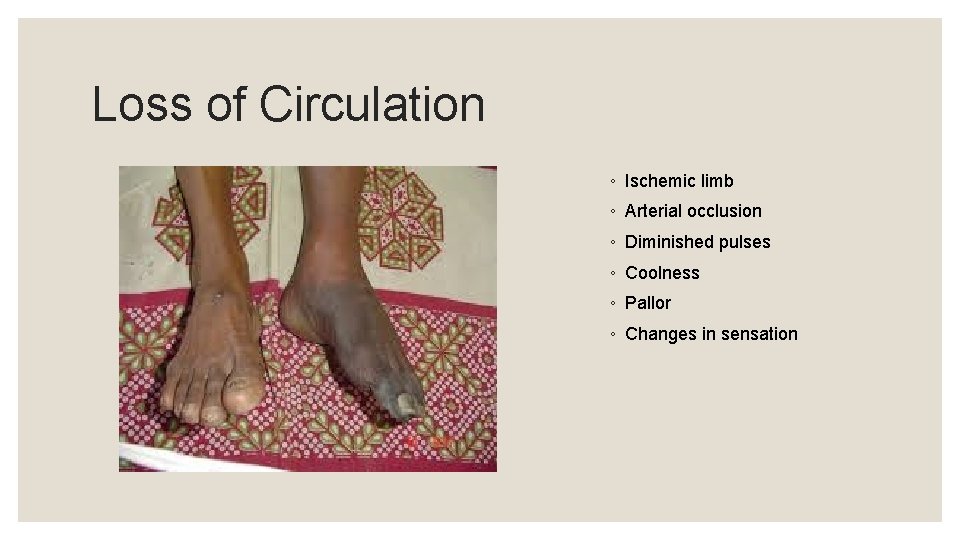
Loss of Circulation ◦ Ischemic limb ◦ Arterial occlusion ◦ Diminished pulses ◦ Coolness ◦ Pallor ◦ Changes in sensation
Infection ◦ Day of sheath removal or several days later ◦ Warmth ◦ Redness ◦ Drainage ◦ Fever ◦ Chills ◦ Pain ◦ Antibiotic ointment ◦ IV or PO antibiotics

Assessing Groin Post Sheath Removal ◦ Lie flat/ Bedrest ◦ Keep affected leg straight ◦ Groin assessment ◦ Neurovascular assessment ◦ Ambulation ◦ Next day wound care

Discharge Education ◦ Activity restrictions ◦ Lifting restrictions ◦ Driving restrictions ◦ Incision care ◦ When to contact MD ◦ Complications ◦ When to start taking anticoagulation again

Questions ◦ Why is it important to check femoral and pedal pulses during sheath removal? ◦ What can you do if a patient vagals during the sheath removal? ◦ What is a hematoma? How can it be expressed? What kind of tests can the doctor order to diagnose a hematoma? How do you treat a hematoma? ◦ What can you do for excessive bleeding? ◦ How often should a nurse check the groin with the sheath in place and after removal?

Conclusion In conclusion, pulling femoral sheaths is a skill not every nurse has received competence in, but should have an idea about. Just because you do not work on a heart floor does not mean you will never have a groin to assess post procedure. Knowing what to observe for and the complications that can occur can keep a patient from crashing fast.

References ◦ Capillary Refill Nail Test. (). Retrieved from https: //www. google. com/search? newwindow=1&q=capillary+refill+&oq=capillary+refill+&gs_l=serp. 3. . 0 i 67 l 3 j 0 l 7. 640 7. 8147. 0. 8845. 11. 0. 0. 0. 3. 221. 1146. 8 j 2 j 1. 11. 0. . . 1 c. 1. 64. serp. . 7. 8. 873. r 6 lg. C 4 F 7 Pgc ◦ Cleveland Clinic (2014). Cardiac Catheterization. Retrieved from http: //my. clevelandclinic. org/services/heart/diagnostics-testing/invasive-testing/cardiac-catheterization ◦ Coburn, M. , & Merschen, R. J. (2010). A Perspective of Sheath Selection and Access Sites for Coronary Angiography. Retrieved from http: //www. cathlabdigest. com/articles/Perspective-Sheath-Selection-Access-Sites. Coronary-Angiography ◦ Femoral Artery Sheath Management. (2008). Retrieved from http: //www. cathlabdigest. com/images/fa. pdf. ◦ Practical-Heamostasis. com (2012). Activated Clotting Time (ACT). Retrieved from http: //practicalhaemostasis. com/Miscellaneous%20 Tests/act. html ◦ Wells, MD, P. (2015). Percutaneous Cardiac Ablation. Retrieved from http: //www. heartracing. com/physicians/percutaneous. cardiac. ablation. asp
- Slides: 35