PULLING BACK THE CURTAIN UNDERSTANDING THE MEDICAL BILLING

PULLING BACK THE CURTAIN: UNDERSTANDING THE MEDICAL BILLING PROCESS Shirley Reitz, Pharm. D Shirley. Reitz@omedarx. com August 10, 2016

Key Take Aways • • Medical billing is different from pharmacy billing A provider = A provider This is a new for the health plans as well Success is possible August 10, 2016 2
Pharmacy Claim ? Rx ? ? Switch Vendor PBM 3
Medical Claim ? ? ? Billing Service Clearinghouse Vendor Payer 4
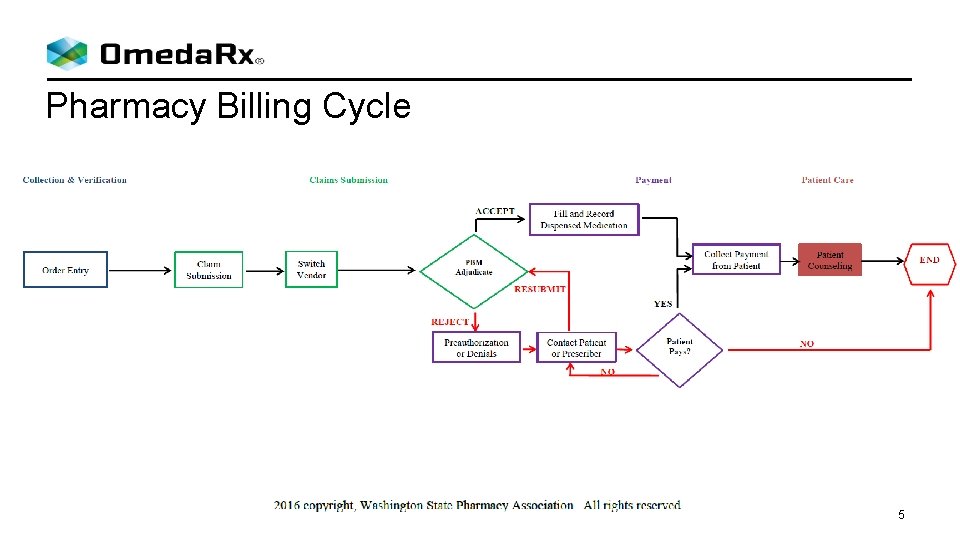
Pharmacy Billing Cycle 5
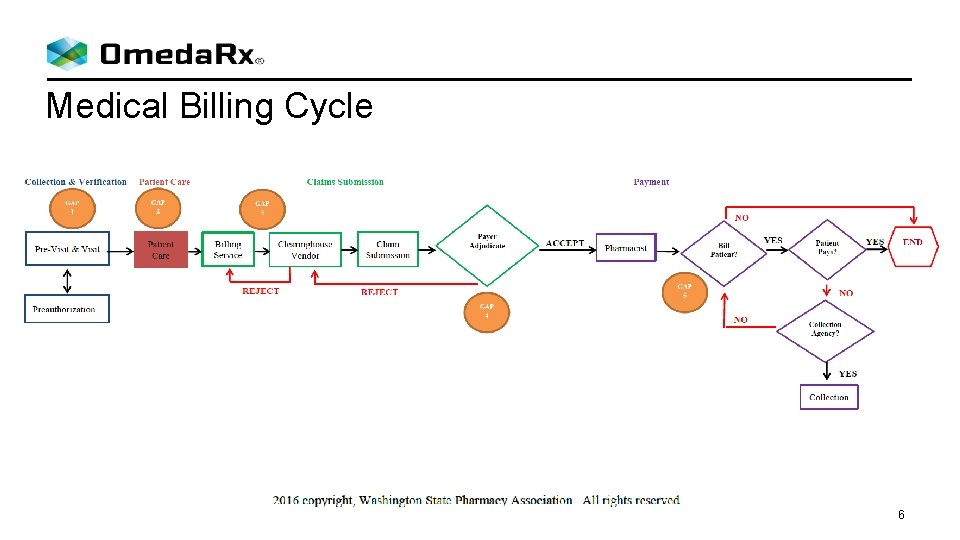
Medical Billing Cycle 6
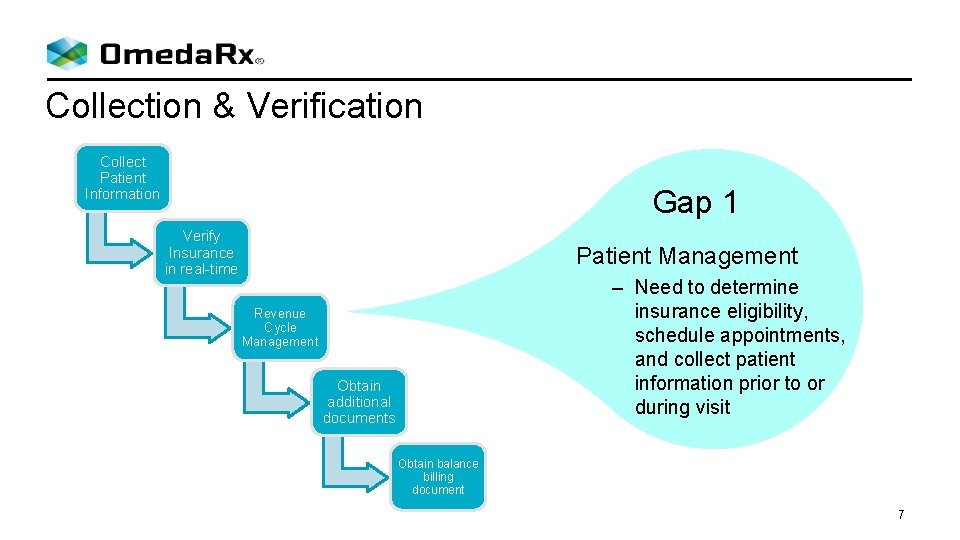
Collection & Verification Collect Patient Information Gap 1 Verify Insurance in real-time Patient Management – Need to determine insurance eligibility, schedule appointments, and collect patient information prior to or during visit Revenue Cycle Management Obtain additional documents Obtain balance billing document 7

Patient Care History Gap 2 Clinical Documentation Examination Medication Decision Making Utilize Pharmacists’ Patient Care Process to improve patient health and outcomes – Need to use industry standards and structured documentation templates to record, receive, and transmit information electronically 8

Medical Billing Cycle 9
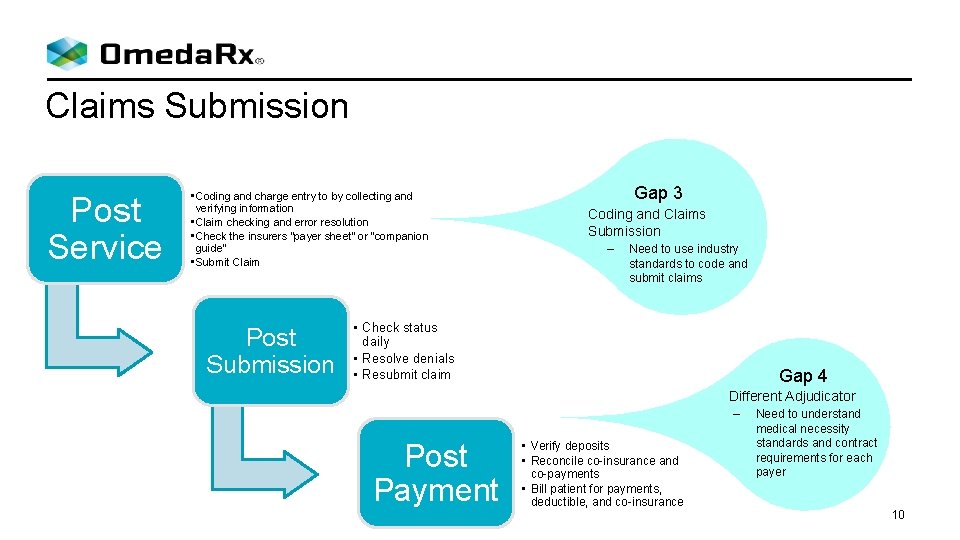
Claims Submission Post Service • Coding and charge entry to by collecting and verifying information • Claim checking and error resolution • Check the insurers “payer sheet” or “companion guide” • Submit Claim Post Submission Gap 3 Coding and Claims Submission – Need to use industry standards to code and submit claims • Check status daily • Resolve denials • Resubmit claim Gap 4 Different Adjudicator – Post Payment • Verify deposits • Reconcile co-insurance and co-payments • Bill patient for payments, deductible, and co-insurance Need to understand medical necessity standards and contract requirements for each payer 10
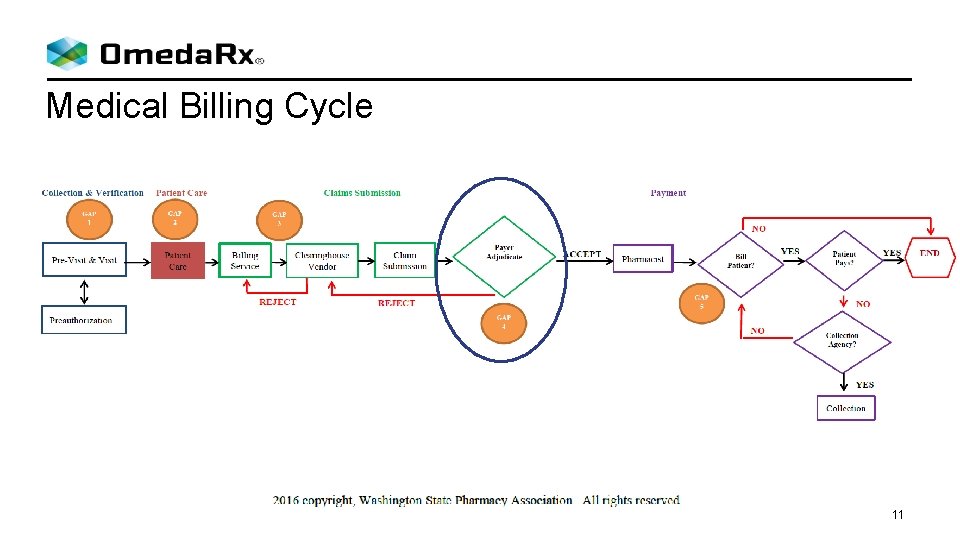
Medical Billing Cycle 11
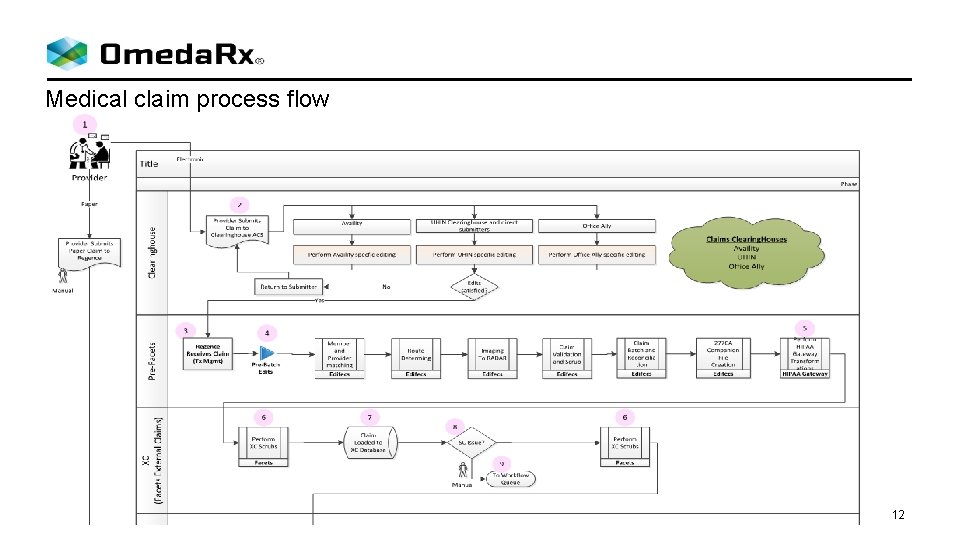
Medical claim process flow 12
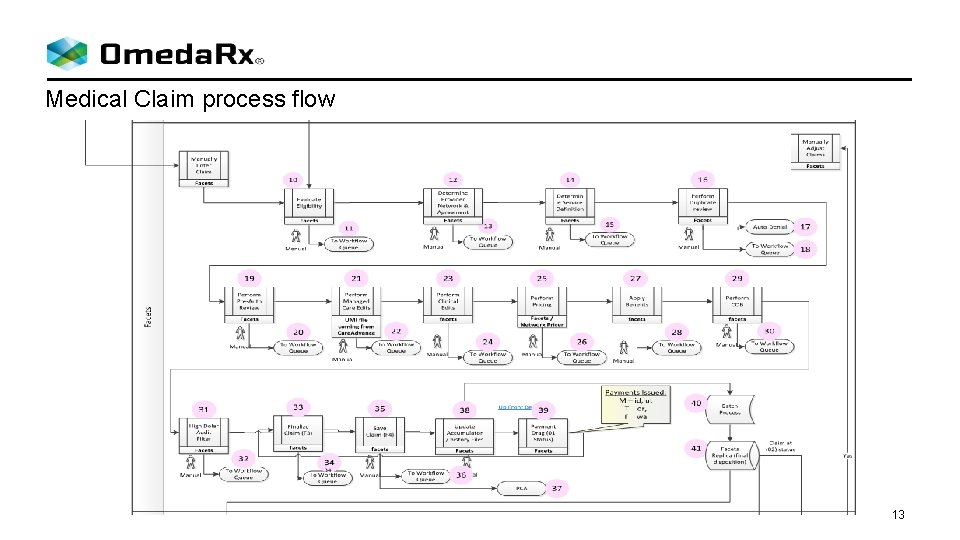
Medical Claim process flow 13

Medical claim process flow 14

Medical Claims information • Regence manages 80 -100, 000 medical claims daily • 82 -86% of medical claims auto-adjudicate • Primary reasons for encountering edits: • Payment generates (in general) within XXXX 15
Payment Review and determine contract limitations and restrictions Gap 5 Payment Collection Patient Follow up – Need to track claims, review denials, and ensure payments – Need to collect payments from patients Provide printed copies of Billing Policy to patients Corrective actions for nonpayments Collection 16
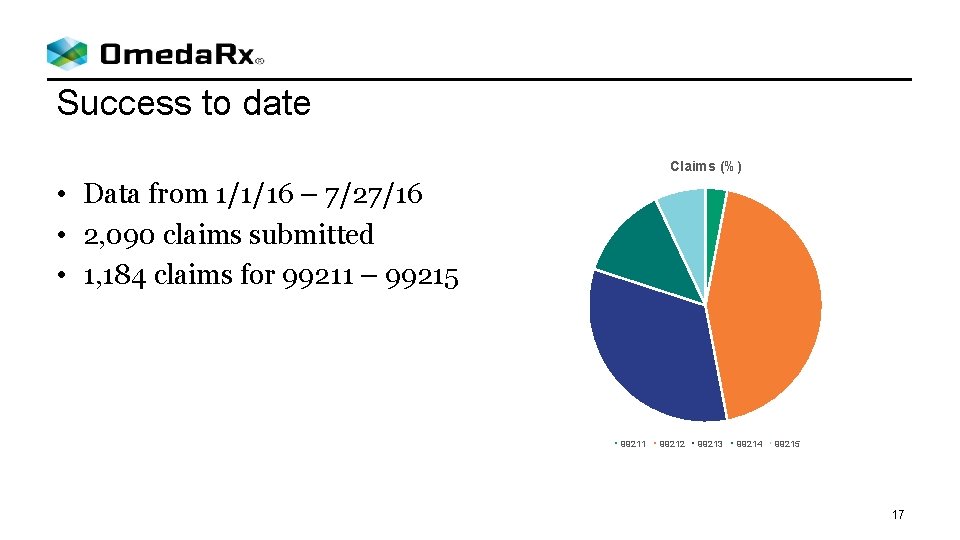
Success to date Claims (%) • Data from 1/1/16 – 7/27/16 • 2, 090 claims submitted • 1, 184 claims for 99211 – 99215 99211 99212 99213 99214 99215 17

Summary 18
- Slides: 18