Public Meeting and Healthcare Exhibition 27 th January

Public Meeting and Healthcare Exhibition 27 th January 2015 ‘The best possible health outcomes for our local community’

Dr John Guy OBE Chair Welcome ‘The best possible health outcomes for our local community’

You said …. we did Progress since September (warts and all……. ) Nicola Airey Director of Planning and Delivery ‘The best possible health outcomes for our local community’

Integrated Care Teams and access to General Practice
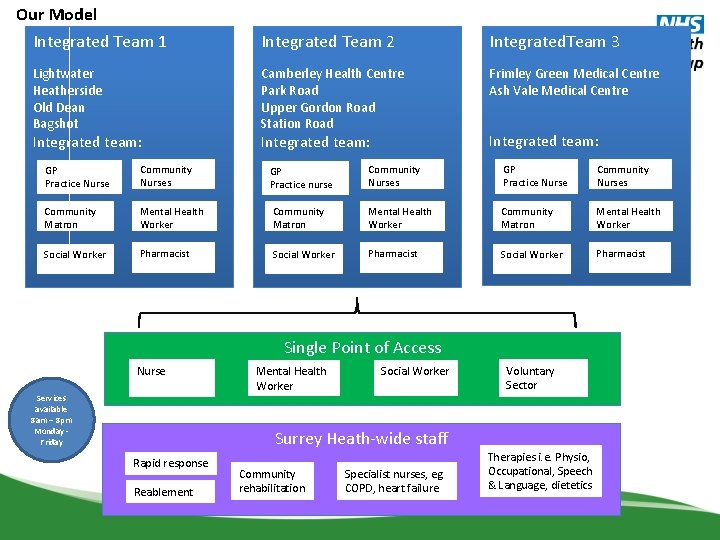
Our Model Integrated Team 1 Lightwater Heatherside Old Dean Bagshot Integrated team: Integrated Team 2 Integrated. Team 3 Camberley Health Centre Park Road Upper Gordon Road Station Road Frimley Green Medical Centre Ash Vale Medical Centre Integrated team: GP Practice Nurse Community Nurses GP Practice nurse Community Nurses GP Practice Nurse Community Nurses Community Matron Mental Health Worker Social Worker Pharmacist Single Point of Access Nurse Services available 8 am – 8 pm Monday Friday Mental Health Worker Social Worker Voluntary Sector Surrey Heath-wide staff Rapid response Reablement Community rehabilitation Specialist nurses, eg COPD, heart failure Therapies i. e. Physio, Occupational, Speech & Language, dietetics

Integrated Care Teams • Delay from December “go live” until April • Will be first community in Surrey to receive • Estates –you said……. . use surgeries as health hub for communities • Investment made – 2/3 staff recruited • Leadership in place • Working through practicalities eg care plans. • Volunteers wanted for patient reference group

Access to General Practice • Practices now open until 8. 00 p. m. Monday to Friday • An additional 75 hours Practice time per week including GP, Practice Nurse and healthcare assistant services (you said…use whole team) • 3 sites are delivering services across Practices a) Lightwater Surgery, Park House Surgery & Heatherside Surgery b) Park Road Surgery & Old Dean Surgery c) Camberley Health Centre & Station Road Surgery* • *Some difficulties sharing data causing restrictions • CCG funded bank holiday openings over Xmas/New year.

Access to General Practice Specific investment in access for over 75 years. • Since October the following activities have been delivered: – Longer Consultations – Healthchecks – Early Support on Discharge – Proactive Home Visits – Practice Care Co-ordinators – Care Co-ordinator role to support patients >75 and act as single point of contact in the Practice •

What’s next? • As part of the Quality Premium Payment GP Practices will be providing support to families of children aged 2 and under that have experienced an emergency episode in hospital • The local GP Practices have submitted an application to the Prime Ministers Challenge Fund to propose a weekend working model and thereby extend current working to 7 days • GP Practices are currently reviewing the invitation to apply for national premises funding (15/16 £ 250 m). The criteria for this funding is: – Extend access to General Practice and associated Community Services – Improve services for the frail and elderly – Building the foundations for more integrated care in the community

Planned Care

‘The best possible health outcomes for our local community’ Slide 11

Care Closer to Home Community Skin • Waiting times reduced • Positive patient feedback • See and treat reducing attendances for patients & carers Community pain • Waiting times reduced • Pain and quality of life scores improved (before & after) • Positive feedback on multi-disciplinary & personalised approach

Mental Health

Mental health services Since September • Additional investment access to psychological therapy (adults) – Group therapy & self referral • MH nurses for elderly as part of ICT (Inc dementia) • Befriending project • Dementia friendly communities • Early dementia diagnosis Working on now for 2015/16 • CAMHS (children and adolescent MH services) – Behavioural pathway – Access to psychological therapies • Crisis café • Acute hospital services & psychiatric liaison • MH expertise in NHS 111 • Suicide awareness training

Dr Andy Brooks Chief Officer Update and Where We Are Now ‘The best possible health outcomes for our local community’

The Forward View into action Planning for 2015/16 Published December 2014 Key Points ‘The best possible health outcomes for our local community’

• 2015/16 NHS extra £ 1. 83 bn. Still significant financial challenge • Dependent on new care models – Urgent and emergency care, maternity services, cancer and specialised services • Remove artificial barriers: – Prevention/treatment, physical/mental health, primary/community/acute care • Whilst delivering significant structural change must deliver core standards • Getting serious about prevention: National action on prevention – and actions for local areas – alcohol, fast food, tobacco, diabetes prevention ‘The best possible health outcomes for our local community’ Slide 17

Empowering patients • Fully interoperable digital health records (2018) • Expansion in personal health budgets in areas where evidence shows benefits. Can be across health & social care. • Concept of “year of care” budgets • Promote choice: mental health & maternity services specifically mentioned ‘The best possible health outcomes for our local community’ Slide 18

Engaging communities - CCG/LA plans to identify and support carers. Voluntary sector and General Practice, young & >85 yrs. - Community volunteering and new roles for volunteers - Grant agreements used for charitable and voluntary sectorless time and complexity than NHS contract. - NHS employers to be progressive – reflect the communities they serve & meet race equality standard ‘The best possible health outcomes for our local community’ Slide 19

Engaging communities 1. CCG/LA plans to identify and support carers. Voluntary sector and General Practice, young & over 85 yrs. 2. Community volunteering and new roles for volunteers 3. Grant agreements used for charitable and voluntary sector- less time and complexity than NHS contract. 4. NHS employers to be progressive – reflect the communities they serve. All employers and boards must meet race equality standard ‘The best possible health outcomes for our local community’ Slide 20

Improving patient quality, outcomes & safety • Published outcomes data this year: 13 medical and surgical specialties • Clinical priorities: Sepsis and acute kidney injury (AKI) • Improve antibiotic prescribing in primary and secondary care. Overuse and incorrect use major drivers of resistance & threat to safe and effective healthcare. ‘The best possible health outcomes for our local community’ Slide 21

Achieving parity for mental health Standards • Deliver existing standards around dementia diagnosis & IAPTS (improving access to psychological therapies) • New access and waiting time standards introduced and delivered from April 2016: – 50% experiencing first episode of psychosis treatment started in 2 weeks – IAPTs 75% first treatment in 6 weeks, 95% in 18 weeks ‘The best possible health outcomes for our local community’ Slide 22

Achieving parity for mental health Services • Develop adequate liaison psychiatry in Hospitals • Crisis Care Concordat – describes the actions required to ensure that those experiencing a mental health crisis are properly supported. Includes: MH as part of NHS 111, 24/7 Crisis Care Home treatment teams, enough capacity for assessment not in police cells • Investment in Child and Adolescent Mental Health Services (CAMHS) • Reducing reliance on inpatient care for people with LD ‘The best possible health outcomes for our local community’ Slide 23

Co-creating new models of care • Different starting points for local health economies • Four prototypes: – Multispecialty community providers (MCPs) includes variants – Integrated Primary and acute care systems (PACs) – Viable smaller hospitals (franchises or chains) – Models of enhanced health in care homes ‘The best possible health outcomes for our local community’ Slide 24

Co-creating new models of care Building the foundations • The future direction for CCGs and providers will be developed by its own leadership in conjunction with partners, patients, communities and staff • All local areas encouraged to develop a local vision, look at medium term strategies and take steps now for rapid adoption. For example, rather than proceed with a stand alone re-procurement of community services, consider how to integrate into MCP model. ‘The best possible health outcomes for our local community’ Slide 25

New models of care 1) Multispecialty Community Providers (MCPs) Will permit groups of GPs to combine with nurses, other community health services, hospital specialists and perhaps mental health and social care to create integrated out-ofhospital care. 2) Integrated Primary and Acute Care systems (PACs) An integrated hospital and primary care provider combining for the first time general practice and hospital services. What do you think? Pros & Cons ‘The best possible health outcomes for our local community’ Slide 26

Aline Poulter Community Services, Surrey Heath Borough Council Being a Dementia Friend Surrey Heath Health & Wellbeing Centre ‘The best possible health outcomes for our local community’

Break ‘The best possible health outcomes for our local community’

Andrew D’Souza Janet Cohen Surrey School Service Young People’s Mental health & Wellbeing ‘The best possible health outcomes for our local community’

Andy D’Souza & Janet Cohen Young people’s mental health & advice for parents School Nursing Service Role of the Camhs Community Nurse for Schools

One in ten children between the ages of one and 15 has a mental health disorder. (The Office for National Statistics Mental health in children and young people in Great Britain, 2005) Estimates vary, but research suggests that 20% of children have a mental health problem in any given year, and about 10% at any one time. (Lifetime Impacts: Childhood and Adolescent Mental Health, Understanding The Lifetime Impacts, Mental Health Foundation, 2005)

Rates of mental health problems among: children: increase as they reach adolescence Disorders affect 10. 4% of boys aged 5 -10 Rising to 12. 8% of boys aged 11 -15 5. 9% of girls aged 5 -10 Rising to 9. 65% of girls aged 11 -15. (Mental Disorder More Common In Boys, National Statistics Online, 2004)

Worried about your Child • Their struggles last longer than would be expected • They have a cluster of things to cope with & several signs they are struggling • They experience these feelings so strongly they interfere with everyday life • Prolonged Unwanted Behaviour

Stay calm Avoid Labelling Use less emotion and less Language when dealing with them “I” Language is very powerful Acknowledge your Child – I can see you have been really down, I can see your really angry all the time, I want to help Contain – I need you to stop and calm down, I need you to take a few breaths, I need you to stop this behaviour Distract – Once you have calmed down I would like you to come and have a sit down here and talk to me.

Wealth of support Nationally & locally for Emotional, Psychological & Behaviour Needs Available to you as parents. Parent Line Adhd – addis website / frimley park website ADHD Specialist Nurse Child. Line Anxiety UK Young Minds National Autistic society Surrey Camhs Website Young Carers Home School Link worker Parent infant Mental Health Support – Via your Health Visitor NCPCC website on parenting behaviour Youth Counselling www. firststeps-surrey. nhs. uk

We are a small team offering a unique and accessible service across Surrey, working alongside 0 -19 teams (School Nurses & Health Visitors). In addition to supporting the 0 -19 teams we offer short term interventions for school aged children attending state primary, secondary or academy schools with Mild to Moderate Emotional , Behavioural and mental health needs
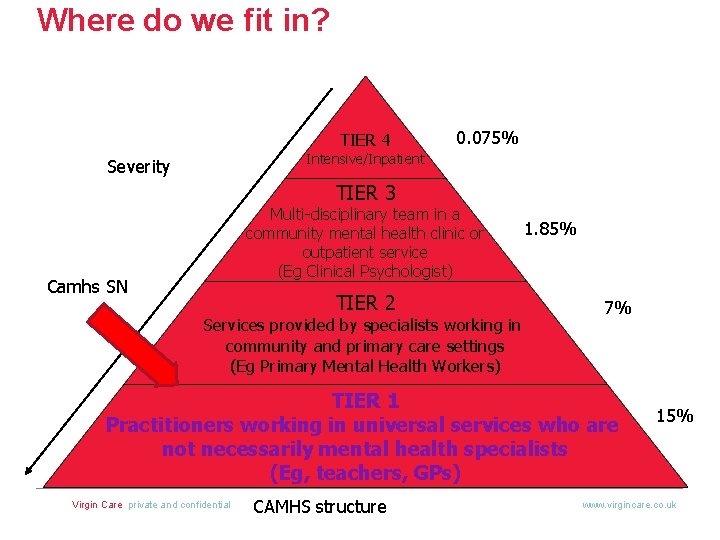
Where do we fit in? TIER 4 0. 075% Intensive/Inpatient Severity TIER 3 Multi-disciplinary team in a community mental health clinic or outpatient service (Eg Clinical Psychologist) Camhs SN TIER 2 Services provided by specialists working in community and primary care settings (Eg Primary Mental Health Workers) 1. 85% 7% TIER 1 Practitioners working in universal services who are not necessarily mental health specialists (Eg, teachers, GPs) Virgin Care private and confidential CAMHS structure 15% www. virgincare. co. uk

SURREY CAMHS 2012

CAMHS Community Nurse for Schools • Strengthening Tier 1 CAMHS provision • Promoting awareness of psychological and emotional health of children and families to other professionals • Enhancing accessibility and equity for all children and families in NW & SW Surrey • Working across agency boundaries to develop a co-ordinated response to children’s emotional and psychological health needs in schools • Providing a short term intervention service to children and their families • Consultation advice service to Schools (via. TAMHS) • Camhs School Nurses main Focus is to support 0 -19 team. • Promote & support Secondary Drop in via School Nurses • Ensure schools are accessing their E. P. & Behaviour Support effectively • Transition support from primary school to secondary school • Cognitive behavioural / solution focused therapeutic approaches • Parenting Advice for Complex Behaviours • Support Surrey & Borders NHS Trust with TAMHS • Working links with HSLW & PMHW (SABP) • Sign Posting to Other Services or Support in referring into Tier 3 Virgin Care private and confidential www. virgincare. co. uk

Ta. MHS Role to support Schools • Staff training (whole school, support staff) • Staff support and on-going consultation • 1: 1 with children and their families (short term intervention) • Group work with children (with Schools) • Support with transition to secondary school (Complex parenting support) • Strong working links with Schools & HSLW Virgin Care private and confidential www. virgincare. co. uk

HOW DO WE GET INVOLVED? REFERRAL PATHWAY to CAMHS COMMUNITY NURSE FOR SCHOOLS Parent Young Person GP School (sencos, HSLW) Advice & support to child/young person/family 0 -19 Team member (Health visitor/ School Nurse) Joint work between Initial Meeting with family / Health Assessment 0 -19 team member and CAMHS Community Nurse Accepted for Direct work by CAMHS Community Nurse Virgin Care private and confidential Completed with Child/ young person and family to identify need for Emotional or Mental Health Support (Mild/ Moderate) CAMHS Community Nurse Other Professional Recommend Referral to other Agency Resource Provision by CAMHS Community Nurse Direct referral to CAMHS (support with referral if required by CAMHS Community Nurse for Schools www. virgincare. co. uk

Example 14 year old girl School notice child low self esteem, low mood – discussed issues with parents(? ) • School Nurse contacted and they complete FHNA with child and family • Identified mild moderate need for support • Identify a possible referral to Camhs Community Nurse for Schools • Up to 6 sessions with girl (and parents) on self-esteem/listening ear /support visits Virgin Care private and confidential www. virgincare. co. uk

Questions Thank you for coming Please complete the feedback forms ‘The best possible health outcomes for our local community’
- Slides: 43