Public Health Prevention Bridgend Approach PUBLIC HEALTH WALES

Public Health & Prevention - Bridgend Approach PUBLIC HEALTH WALES ANNUAL GENERAL MEETING Abigail Harris & Peter Mannion 19 th September 2011

Strategic Background ◦ Local Context –Setting the scene Public Health & Prevention Team ◦ Positioning the team – a new focus Example – Weight Management in the Community Overview

Wellbeing Directorate ◦ Adult Social Care ◦ Healthy Living Integration ◦ Joint Locality Director Bridgend Local Care Partnership Service Board Local Context

Bridgend Care Partnership Integrated Referral Management Public Health & Prevention Long Term Care Integrated Operational Teams Integrated Community Networks Community Resource Team Secondary & Community Services

Develop an integrated team which will lead the public health and prevention agenda across Bridgend Team incorporates: ◦ HSCWB Partnership personnel (ABMU/BCBC) ◦ Health Challenge Bridgend Officer (BCBC) ◦ Older Persons Strategy Resources (BCBC) ◦ Local Public Health Team (PHW) ◦ Substance Misuse Service Team (ABMU/BCBC) Public Health & Prevention Team

Strategic Change – from upstream to. . .

Repositioning -Down Stream Pressure Establishing a clear link between PH & P Activity and System pressure ◦ ◦ ◦ Unscheduled Care Residential Care Primary Care Home Carers

CYP & HSCWB Strategies ABMU PH Framework Locality & Wellbeing Business Plans Limited No of Priority Areas Plan Filter
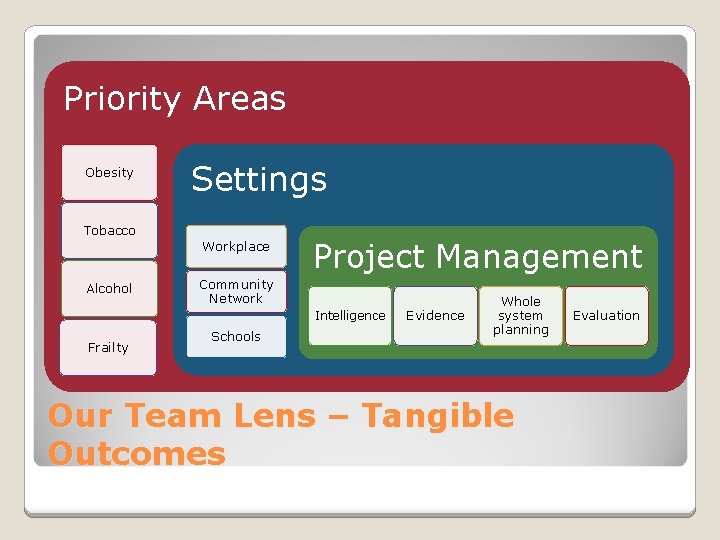
Priority Areas Obesity Tobacco Alcohol Settings Workplace Project Management Community Network Intelligence Frailty Schools Evidence Whole system planning Our Team Lens – Tangible Outcomes Evaluation

Local Context – Bridgend
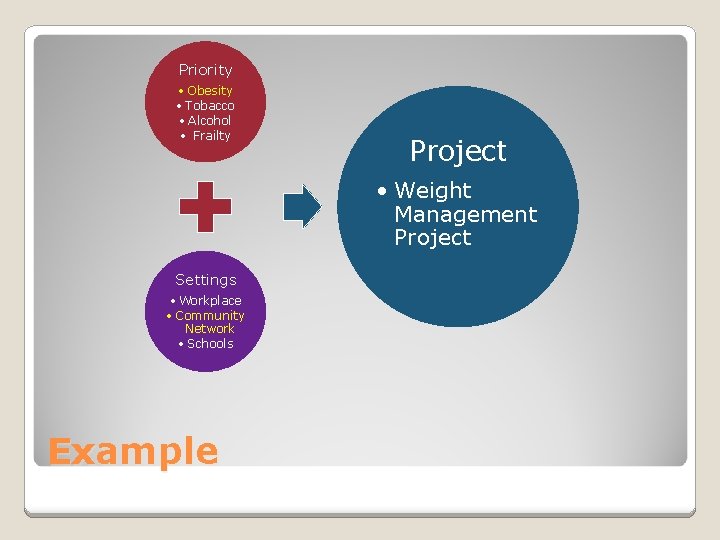
Priority • Obesity • Tobacco • Alcohol • Frailty Project • Weight Management Project Settings • Workplace • Community Network • Schools Example

The North Network has the highest EASR prevalence for Diabetes, CHD and Hypertension within ABMU 25% of adults in Bridgend are reported Obese – higher practice prevalence rates in the North Network If you are clinically obese you are 80 x more likely to develop diabetes than someone of normal weight (Prof Alan Maryon-Davies) Weight Management Project

A non-clinical programme giving individuals support to make sustainable changes to their lifestyle to improve their health and wellbeing. Links up local activities, groups and initiatives that already exist within the community Weight Management Project
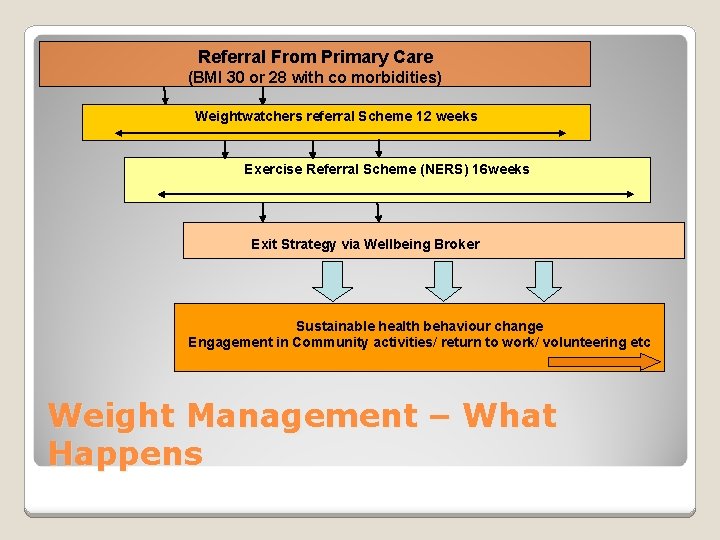
Referral From Primary Care (BMI 30 or 28 with co morbidities) Weightwatchers referral Scheme 12 weeks Exercise Referral Scheme (NERS) 16 weeks Exit Strategy via Wellbeing Broker Sustainable health behaviour change Engagement in Community activities/ return to work/ volunteering etc Weight Management – What Happens

Rolling Program : 147 active referrals since Sept 2010 90% retention rate on WW programme (UK national rate only 57% complete 12 weeks) 90% engaging in Exercise referral (NERS) 51 have achieved 5% weight loss 18 have achieved 10% weight loss Group cumulative loss -154 Stone Average 1 -2 lb per week person Outputs

Quantitative Improved clinical indicators – Hb. A 1 c, BP Medication changes a significant reduction in weight, BMI and waist measurements A significant change in diet and eating habits A significant increase in perceived well-being Qualitative Increased confidence Reduced social isolation Increased activity Economic Cost effectiveness Evaluation
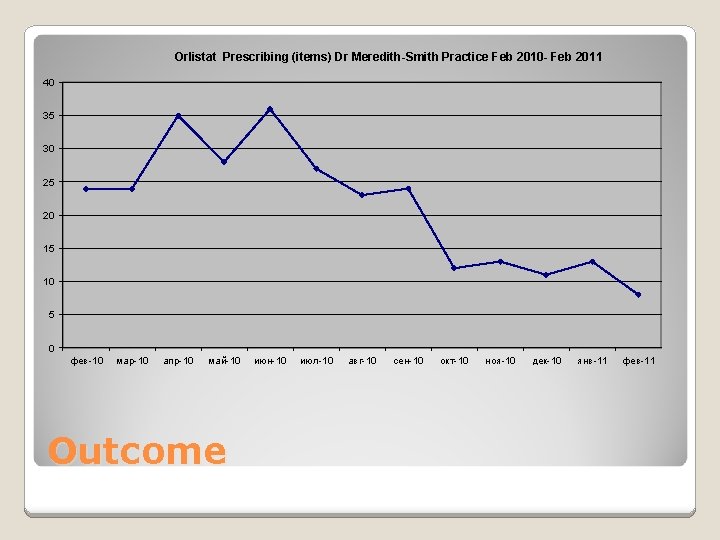
Orlistat Prescribing (items) Dr Meredith-Smith Practice Feb 2010 - Feb 2011 40 35 30 25 20 15 10 5 0 фев-10 мар-10 апр-10 май-10 Outcome июн-10 июл-10 авг-10 сен-10 окт-10 ноя-10 дек-10 янв-11 фев-11
Projects • Public Health / Maintenance Public Health Lens • Priorities • Settings • Process Integrating & Repositioning • Prevention • Workforce • Health Intelligence Value Patient / citizen / service user BCBC Outcome Agreement Unscheduled Care Meeting HSCWB Outcomes Promoting OP Independence Pressure AS Services CCM Priority Integrated Team – The Value
- Slides: 18