Public Health Prevention Ahmed Elshafei MD MPHc Seattle

Public Health & Prevention Ahmed Elshafei MD, MPHc Seattle Central College HEA 125

Objectives 1) Definitions & key terms in Public Health 2) Types of prevention (examples) 3) Describe the purpose of public health 4) identify prominent events in the history of public health 5) Recognize the core public health functions and services 6) Describe the role of different stakeholders in the field of public health 7) Recognize how individual determinants of health affect population health

What is Public Health? “The science and art of preventing disease, prolonging life, and promoting health through the organized efforts and informed choices of society, organizations, public and private communities, and individuals. ” Charles Winslow

What are the tools of a public health practitioner?

1) Epidemiology is the study of patterns, causes & effects of different diseases in a defined population So, it is the study of the distribution and determinants of healthrelated states within a population In other words, it is the branch of medicine that deals with the incidence, distribution, and possible control of diseases and other factors relating to health

Epidemiology The tools of epidemiology are numbers. Numbers are ratios converted into rates. Remember: the denominator is key: who is “at risk” for a particular event or disease state. 3

Epidemiology: Key Definitions • Epidemic: occurrence of disease in excess of the expected rate • Pandemic: worldwide epidemic • Epidemic curve: cases plotted against time • Endemic: expected rate of disease over time • Incubation period: period of time from the point of infection to the onset of clinical illness 3

Epidemiology • Disease as distributed within a group • The tools of epidemiology are numbers Numerator Denominator = Actual cases Potential cases = RATE • The denominator is key: Who is “At Risk”? • Rates are events per 100, 000 persons 3 8

Epidemiology Incidence vs. Prevalence

Incidence Vs. Prevalence • Incidence: # of new events in a population • Prevalence: # of all existing cases in a population 4 -6 10

Incidence vs. Prevalence • Incidence is a direct measure of disease risk • Higher incidence implies higher risk • Usually refers to acute conditions • Prevalence is a more relevant when assessing impact of a problem within a community and to assess the subsequent needs 4 -6 11
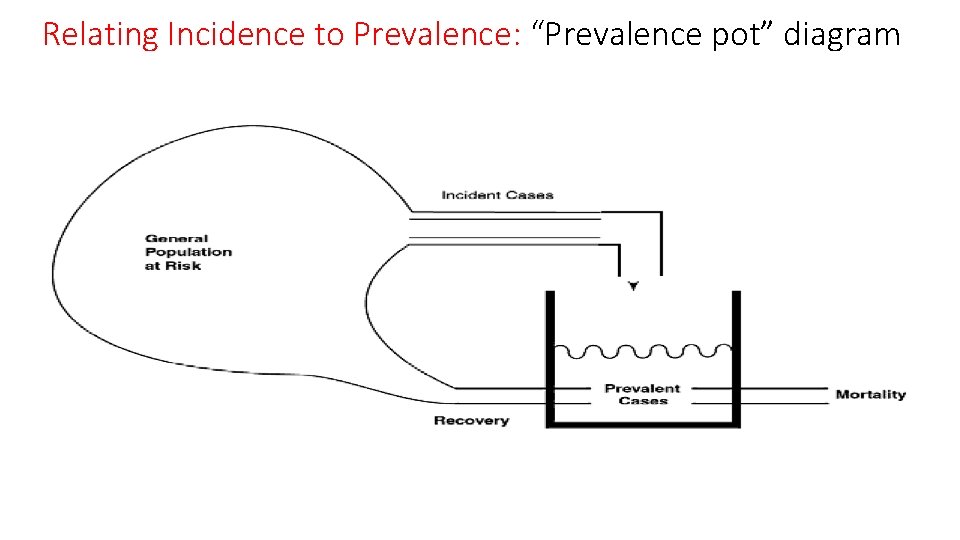
Relating Incidence to Prevalence: “Prevalence pot” diagram 6

2) Statistics Probability Basics “Probability is a branch of mathematics that deals with calculating the likelihood of a given event occurrence, which is expressed as a number. ”

Evidence-based medicine Vs statistics

What is Public Health? “The science and art of preventing disease, prolonging life, and promoting health through the organized efforts and informed choices of society, organizations, public and private communities, and individuals. ” Charles Winslow

WHO “The art and science of preventing disease, prolonging life and promoting health through the organized efforts of society” Public health focuses on the entire spectrum of health and wellbeing, not only the eradication of particular diseases.

Public health key terms Clinical care: prevention, treatment, and management of illness and the preservation of mental and physical well-being through the services offered by medical and allied health professions; also known as health care. Determinant: factor that contributes to the generation of a trait. Epidemic or Outbreak: occurrence in a community or region of cases of an illness, specific health-related behavior, or other health-related event clearly in excess of normal expectancy. Both terms are used interchangeably; however, epidemic usually refers to a larger geographic distribution of illness or healthrelated events. Health outcome: result of a medical condition that directly affects the length or quality of a person’s life. Stedman TL, ed. Stedman’s medical dictionary. 28 th ed. Baltimore, MD: Lippincott, Williams, and Wilkins; 2006. Farlex, Inc. The free dictionary. Huntingdon Valley, PA: Farlex, Inc. ; 2014. Available at: http: //www. thefreedictionary. com/

In other words… - Promotes the welfare of the entire population and ensures its security. - Protects the community from the spread of infectious disease and environmental hazards. - Helps to ensure access to safe and quality care to benefit the population.

Epidemiologic terms • A disease may occur in a country at a regular annual rate, which makes it endemic • If there is a sudden rise in the number of cases in a specific month, we say that there is an epidemic • As the disease continues to rise and spread to other countries, it becomes a pandemic • Thus the terminology is related to both the number of cases and its geographical distribution

What is the importance of “Prevention” in Public Health?

Prevention on individual basis Goals of prevention: • Promote, preserve, and restore health when it is impaired • Minimize suffering and distress • Minimize both morbidity and mortality

How about the goals of prevention on community (aka Public Health) basis?

Primary prevention • Promotes health at both individual and community levels by • Facilitating health-enhancing behaviors • Preventing the onset of risk behaviors • Diminishing exposure to environmental hazards • Decreases disease incidence • Examples include implementation of exercise programs and healthy food programs in schools

Secondary prevention • Screens for risk factors and early detection of asymptomatic or mild disease, permitting timely and effective intervention and curative treatment • Decreases disease prevalence • Examples include recommended annual colonoscopy for patients age > 65 and Hepatitis B & C testing for health care workers with needlestick injuries

Tertiary prevention • Reduces long-term impairments and disabilities and prevents repeated episodes of clinical illness • Prevents recurrence and slow progression • Examples include physical therapy for spinal injury patients and daily low-dose aspirin for those with previous myocardial infarction

Prevention New healthcare bill funded to help wounded war veterans gain access to prosthetic limb replacement • That would be considered “tertiary prevention” • Patients who would have access to the service have already been injured • Prosthetic devices would help reduce complications of amputation and help their rehabilitation • By improving quality of life and reducing morbidity, that is an implementation of tertiary prevention

Prevention • A nursing school student who is asked to wear a nose and mouth mask before entering the room of a patient with meningococcal meningitis • That would be considered “primary prevention” • Because the bacteria in this case can be spread by respiratory contact, the use of the mask will prevent the student from being exposed

History of Public Health Now, let’s review the history of public health. We will take a look at a few historical highlights through four lenses, 1) Sanitation and environmental health, 2) Pandemics, 3) Disaster response and preparedness, and 4) Prevention and policy.

Sanitation and Environmental Health 500 BCE 1840 s Greeks and Romans practice community sanitation measures The Public Health Act of 1848 was established in the United Kingdom 1970 The Environmental Protection Agency was founded
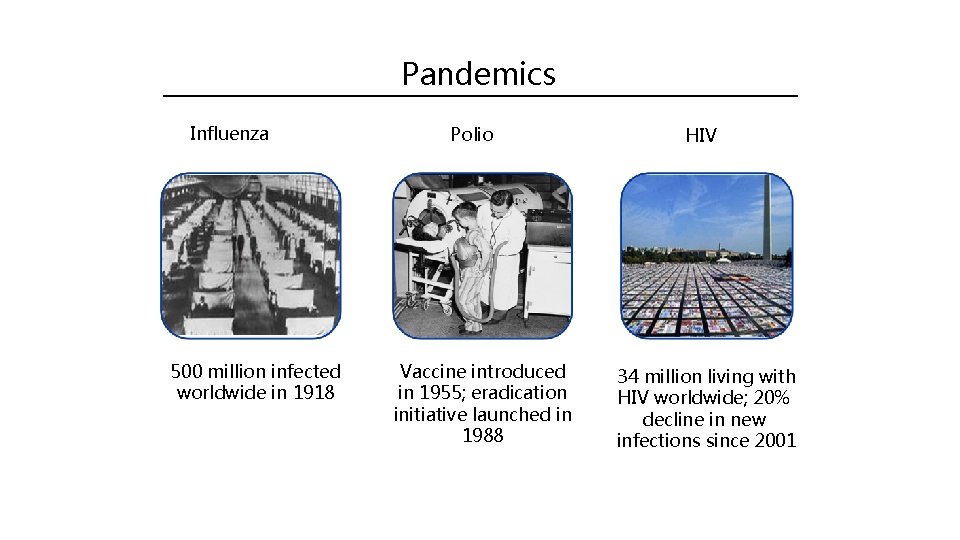
Pandemics Influenza 500 million infected worldwide in 1918 Polio Vaccine introduced in 1955; eradication initiative launched in 1988 HIV 34 million living with HIV worldwide; 20% decline in new infections since 2001

Preparedness for Disaster Response Biologic Warfare Plague used as a weapon of war during the Siege of Kaffa September 2001 Hurricane Katrina Public health surveillance conducted after the 9/11 attacks Emergency services, public health surveillance, and disease treatment provided
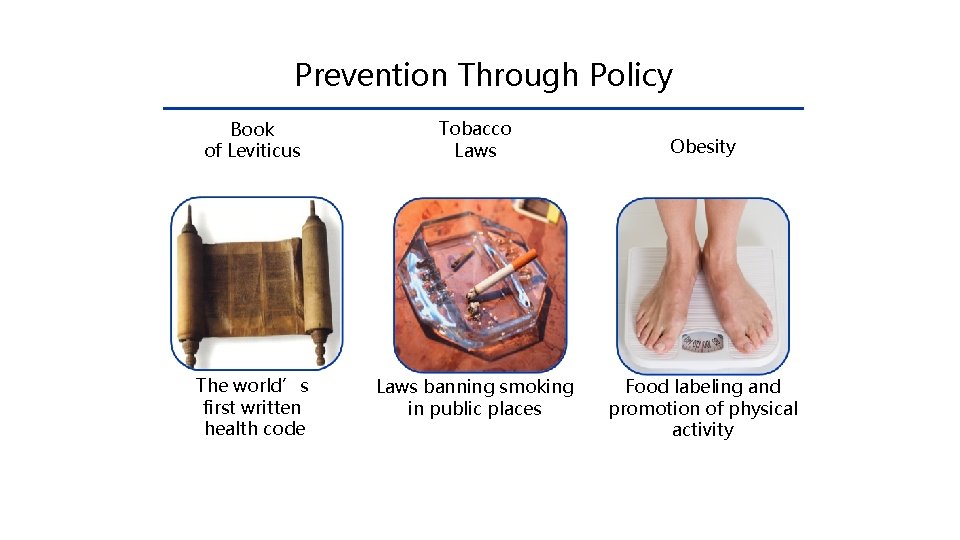
Prevention Through Policy Book of Leviticus Tobacco Laws The world’s first written health code Laws banning smoking in public places Obesity Food labeling and promotion of physical activity

A Public Health Approach
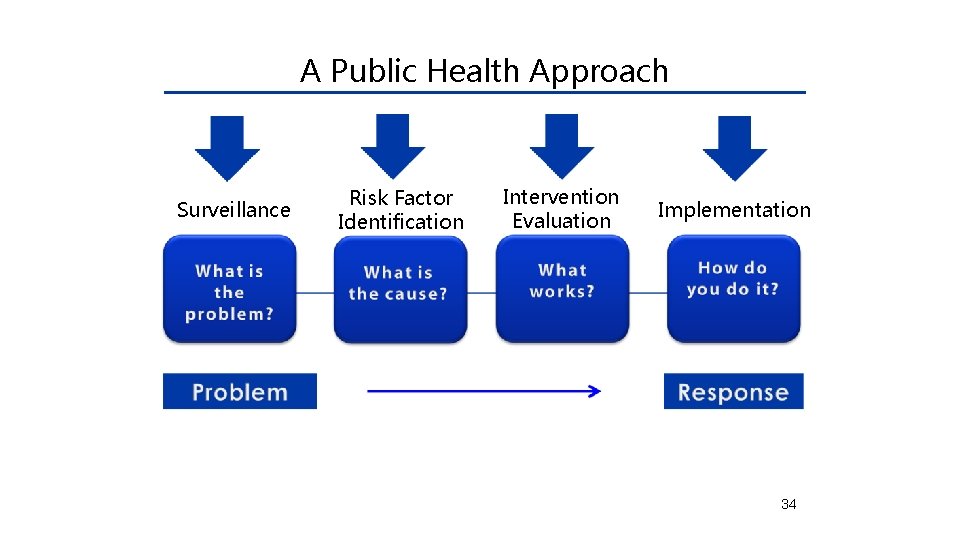
A Public Health Approach Surveillance Risk Factor Identification Intervention Evaluation Implementation 34
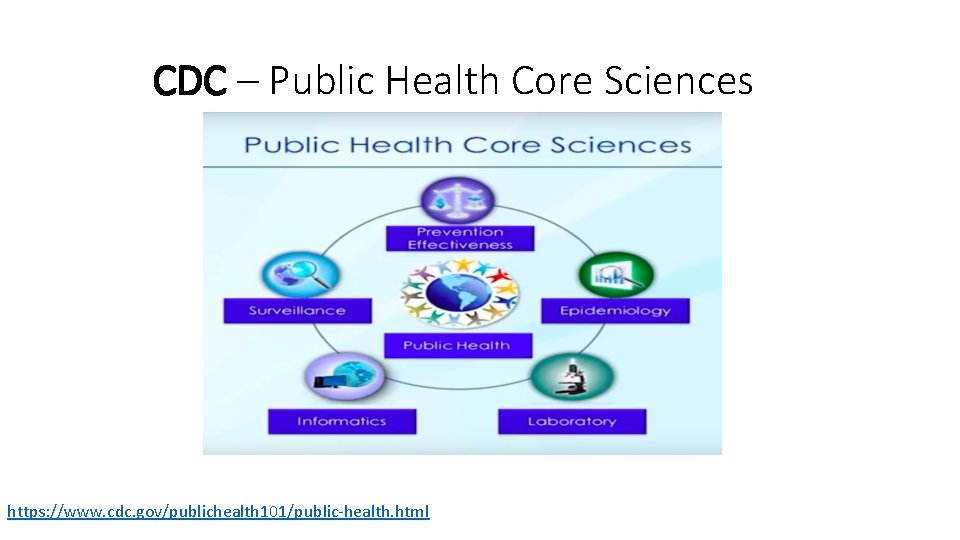
CDC – Public Health Core Sciences https: //www. cdc. gov/publichealth 101/public-health. html

Cholera — A Public Health Approach Cholera, a fatal intestinal disease, was rampant during the early 1800 s in London, causing death to tens of thousands of people in the area. Photo: TJ Kirn, MJ Lafferty, CMP Sandoe, and R Taylor, Dartmouth Medical School Cholera was commonly thought to be caused by bad air from rotting organic matter.

John Snow, Physician John Snow is best known for his work tracing the source of the cholera outbreak and is considered the father of modern epidemiology. Photo: London School of Hygiene and Tropical Medicine

Epidemiology — What is the Problem? Cluster of Cholera Cases, London — 1854 Image: The Geographical Journal

Risk Factor Identification — What Is the Cause? Cluster of Cholera Cases and Pump Site Locations Image: The Geographical Journal

Intervention Evaluation — What Works? Through continuous research, Snow understood what interventions were required to • • stop exposure to the contaminated water supply on a larger scale, and stop exposure to the entire supply of contaminated water in the area 40

Implementation — How Do You Do It? John Snow’s research convinced the British government that the source of cholera was water contaminated with sewage Photo: Justin Cormack 41

Core Functions and Essential Services of Public Health
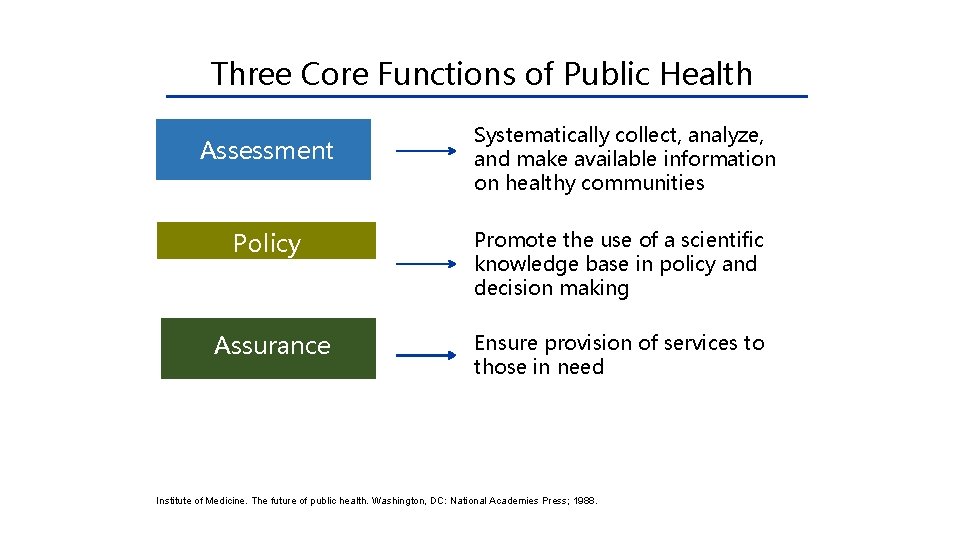
Three Core Functions of Public Health Assessment Systematically collect, analyze, and make available information on healthy communities Policy Development Promote the use of a scientific knowledge base in policy and decision making Assurance Ensure provision of services to those in need Institute of Medicine. The future of public health. Washington, DC: National Academies Press; 1988.

Ten Essential Public Health Services 1. 2. 3. 4. 5. 6. 7. 8. 9. 10. Monitor Health Diagnose and Investigate Inform, Educate, Empower Mobilize Community Partnership Develop Policies Enforce Laws Link to/Provide Care Assure a Competent Workforce Evaluate Research

Governmental responsibilities • Governmental responsibilities for public health extend beyond voluntary activities and services to include additional authorities such as quarantine, mandatory immunization laws, and regulatory authorities. • The state's partnership functions by encouraging residents to do things that benefit their health (e. g. , physical activity) or create conditions to promote good health, and requiring certain actions (e. g. , food safety).

Governmental responsibilities In each State, the community health board shall identify local public health priorities and implement activities to address the priorities and the areas of public health responsibility, which include: 1. Assure an adequate local public health infrastructure 2. Promote health communities and healthy behavior 3. Prevent the spread of communicable diseases 4. Protect against environmental health hazards 5. Prepare and respond to emergencies 6. Assure health services

Governmental responsibilities 1. Assure an adequate local public health infrastructure by: - maintaining the basic foundational capacities to a well-functioning public health system that includes: data analysis and utilization; health planning; partnership development and community mobilization; policy development, analysis, and decision support; communication; and public health research, evaluation, and quality improvement. 2. Promote health communities and healthy behavior 3. Prevent the spread of communicable diseases 4. Protect against environmental health hazards 5. Prepare and respond to emergencies 6. Assure health services

Governmental responsibilities 1. Assure an adequate local public health infrastructure 2. Promote health communities and healthy behavior by: - Engaging communities to change policies, systems, or environments to promote positive health or prevent adverse health; - Providing information and education about healthy communities or population health status; - Addressing issues of health equity, health disparities, and the social determinants to health. 3. Prevent the spread of communicable diseases 4. Protect against environmental health hazards 5. Prepare and respond to emergencies 6. Assure health services

Governmental responsibilities 1. Assure an adequate local public health infrastructure 2. Promote health communities and healthy behavior 3. Prevent the spread of communicable diseases by: - Detecting acute infectious diseases - Ensuring the reporting of infectious diseases - Preventing the transmission of infectious diseases - Implementing control measures during infectious disease outbreaks. 4. Protect against environmental health hazards 5. Prepare and respond to emergencies 6. Assure health services

Governmental responsibilities 1. Assure an adequate local public health infrastructure 2. Promote health communities and healthy behavior 3. Prevent the spread of communicable diseases 4. Protect against environmental health hazards by: - Monitoring air and water quality - Developing policies and programs to reduce exposure to environmental health risks and promote healthy environments - Identifying and mitigating environmental risks such as food and waterborne diseases, radiation, occupational health hazards, and public health nuisances 5. Prepare and respond to emergencies 6. Assure health services

Governmental responsibilities 1. Assure an adequate local public health infrastructure 2. Promote health communities and healthy behavior 3. Prevent the spread of communicable diseases 4. Protect against environmental health hazards 5. Prepare and respond to emergencies by: - Engaging in activities that prepare public health departments to respond to events and incidents and assist communities in recovery, such as providing leadership for public health preparedness activities with a community - Developing, exercising, and periodically reviewing response plans for public health threats - Developing and maintaining a system of public health workforce readiness, deployment, and response. 6. Assure health services

Governmental responsibilities 1. Assure an adequate local public health infrastructure 2. Promote health communities and healthy behavior 3. Prevent the spread of communicable diseases 4. Protect against environmental health hazards 5. Prepare and respond to emergencies 6. Assure health services by: - Engaging in activities such as assessing the availability of health-related services and health care providers in local communities, identifying gaps and barriers in services - Convening community partners to improve community health systems - Providing services identified as priorities by the local assessment and planning process

Stakeholder Roles in Public Health
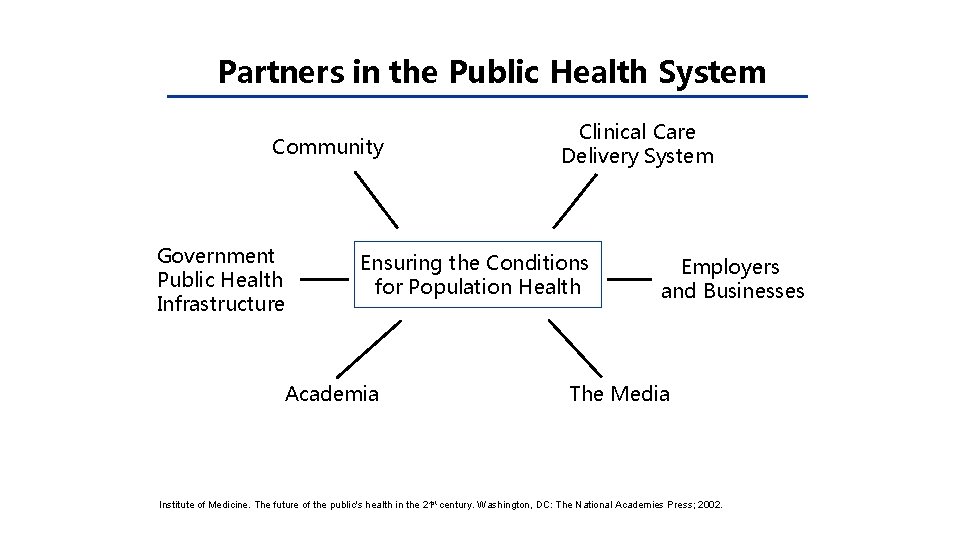
Partners in the Public Health System Community Government Public Health Infrastructure Clinical Care Delivery System Ensuring the Conditions for Population Health Academia Employers and Businesses The Media Institute of Medicine. The future of the public's health in the 21 st century. Washington, DC: The National Academies Press; 2002.

Nongovernmental Organization Examples Organization Type Example Professional membership organizations American Public Health Associations related to a specific health concern American Cancer Society Organizations of citizens focused on health concerns Americans for Nonsmokers Rights Foundations that support health projects and influence public policy development Bill and Melinda Gates Foundation Institute of Medicine. Who will keep the public healthy? Workshop summary. Washington, DC: The National Academies Press; 2003.

Health Care as a Partner in Public Health Care Population focus Individual patient focus Public health ethic Personal service ethic Prevention or public health emphasis Diagnosis and treatment emphasis Joint laboratory and field involvement Joint laboratory and patient involvement Clinical sciences peripheral to professional training Clinical sciences essential to professional training Public sector basis Private sector basis

Other Partners in Public Health • • Serves as vehicle for public discourse Health education and promotion Health communication Social media as catalyst • • • Employer-sponsored health insurance programs Wellness initiatives and benefits Healthy workplaces and communities Government Agencies • • • City planning Education Health in all policies Academia • • Education Training Research Public Service Media Employers and Businesses

Determining and Influencing the Public’s Health

Health Determinants • Genes and biology • Health behaviors • • Social or societal characteristics Health services or medical care Centers for Disease Control and Prevention. Social determinants of health. http: //www. cdc. gov/socialdeterminants/FAQ. html.
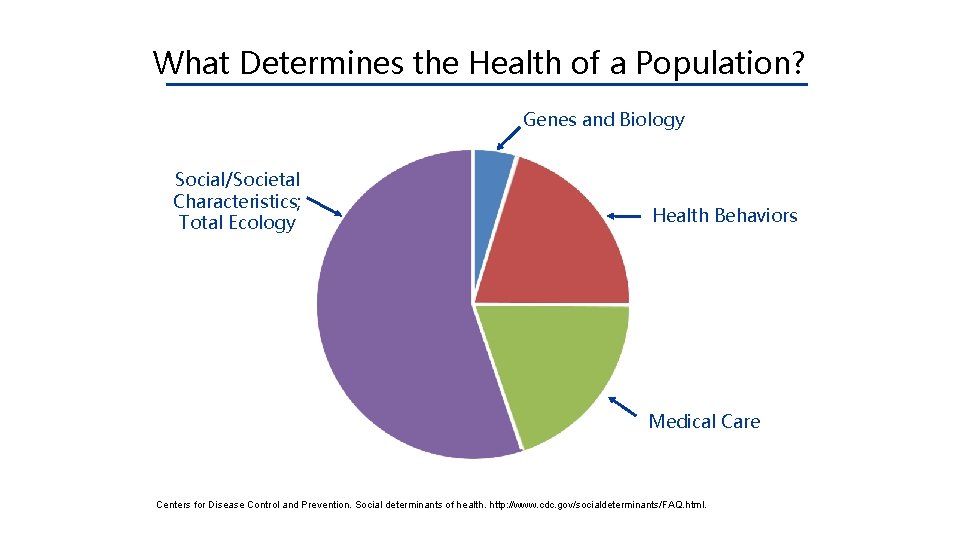
What Determines the Health of a Population? Genes and Biology Social/Societal Characteristics; Total Ecology Health Behaviors Medical Care Centers for Disease Control and Prevention. Social determinants of health. http: //www. cdc. gov/socialdeterminants/FAQ. html.
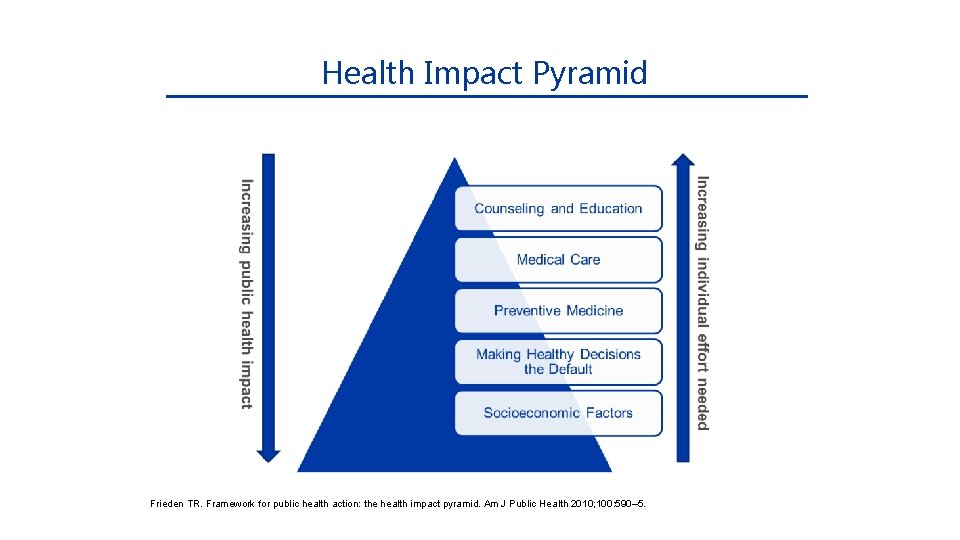
Health Impact Pyramid Frieden TR. Framework for public health action: the health impact pyramid. Am J Public Health 2010; 100: 590– 5.
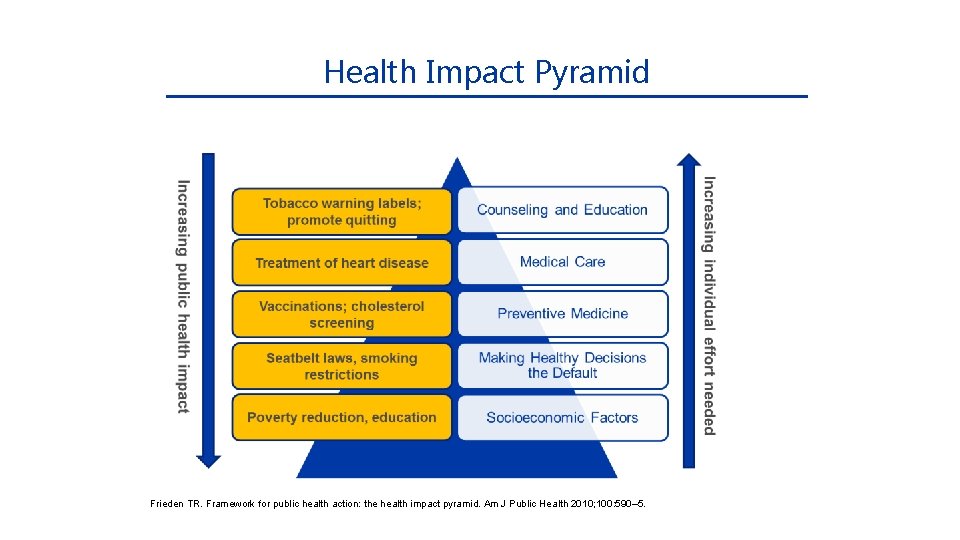
Health Impact Pyramid Frieden TR. Framework for public health action: the health impact pyramid. Am J Public Health 2010; 100: 590– 5.

Resources and Additional Reading • • • American public health Association (APHA). The Prevention and public health Fund: a critical investment in our nation’s physical and fiscal health. APHA Center for Health Policy Issue Brief. Washington, DC: APHA; 2012. http: //www. apha. org/NR/rdonlyres/8 FA 13774 -AA 47 -43 F 2 -838 B 1 B 0757 D 111 C 6/0/APHA_Prev. Fund. Brief_June 2012. pdf. California Department of public health. Tabacco. Free. CA. http: //www. Tobaccofreeca. org. Centers for Disease Control and Prevention. Key facts about seasonal flu vaccine. http: //www. cdc. gov/flu/protect/keyfacts. htm. Centers for Disease Control and Prevention. Overweight and obesity. http: //www. cdc. gov/obesity/index. html. Centers for Disease Control and Prevention. Social determinants of health. http: //www. cdc. gov/socialdeterminants/FAQ. html. Centers for Medicare and Medicaid Services. National health expenditure projections: 2008– 2018. http: //www. cms. gov/Research-Statistics-Data-and-Systems/Statistics-Trends-and. Reports/National. Health. Expend. Data/downloads/proj 2008. pdf. Dean H. Introduction to public health, epidemiology, and surveillance. Presented at the CDC Science Ambassador Program, July 16, 2012. Frieden, TR. Framework for public health action: the health impact pyramid. Am J public health 2010; 100: 590– 5. Kindig D, Stoddart G. What is population health? Am J public health. 2003; 93: 380– 3. Institute of Medicine. For the public’s health: investing in a healthier future. Washington, DC: National Academies Press; 2012. Institute of Medicine. Primary care and public health: exploring integration to improve population health. Washington, DC: The National Academies Press; 2012.

Resources and Additional Reading • • • Institute of Medicine. The future of public health. Washington, DC: The National Academies Press; 1988. Institute of Medicine. The future of the public's health in the 21 st century. Washington, DC: The National Academies Press; 2002. Institute of Medicine. Who will keep the public healthy? Workshop summary. Washington, DC: The National Academies Press; 2003. Pearl R. Tobacco smoking and longevity. Science 1938; 87: 216– 7. Preamble to the Constitution of the World Health Organization as adopted by the International Health Conference, New York, June 19–July 22, 1946. Federal Communications Commission. Texting while driving. http: //www. fcc. gov/guides/textingwhile-driving. UNAIDS World AIDS Day Report, 2012. http: //www. unaids. org/en/media/unaids/contentassets/ documents/epidemiology/2012/gr 2012/JC 2434_World. AIDSday_results_en. pdf. Skelton A. Introduction to public health science and practice. ” Presented at the CDC Steven M. Teutsch Prevention Effectiveness Fellowship Orientation, August 15, 2012. US Department of Health, Education, and Welfare. Smoking and health. Washington, DC: public health Service; 1964. http: //profiles. nlm. nih. gov/ps/access/NNBBMQ. pdf. Winslow CEA. The untilled field of public health. Mod Med 1920; 2: 183– 91. World Health Organization (WHO). World report on violence and health. Geneva: WHO; 2002. http: //www. who. int/violence_injury_prevention/violence/world_report/en/.
- Slides: 64