Public Health Module Venue Date Unit Public Health

Public Health Module Venue Date Unit: Public Health Aspects of Stroke © 2010

Aims of Unit WB 4 This unit of study will: • Explore how common strokes are and the evidence of their impact on quality and length of life • Familiarise students with the major risk factors for stroke • Explore the efficacy and ethics of interventions for the prevention and management of strokes 2 LTPHN/JH/HB © 2010 2

WB 6 What is health? 3 WHO Definition ‘a state of complete physical, mental and social well-being and not merely the absence of disease or infirmity’ Antonovosky: Salutogenic model ‘sense of coherence’ Seedhouse and Duncan: Achievement of potential Empirical Lack of health LTPHN/JH/HB © 2010

WB 7 What is public health? ‘the science and art of preventing disease, prolonging life and promoting health through the organized efforts of society’ C. E. A. Winslow, 1920 4 LTPHN/JH/HB © 2010

The wider determinants of health Source: Dahlgreen and Whitehead, G and Whitehead M (1991) 5 LTPHN/JH/HB © 2010 WB 7

The challenge for public health 6 LTPHN/JH/HB © 2010 WB 7

WB 8 Statistical description of nation’s health Census data Health Inequalities data Infant Mortality Rates 7 LTPHN/JH/HB © 2010

What is a stroke? • • • A stroke is an interruption in the blood supply to the brain. Also known as cerebrovascular accident or CVA Usually because 1. Blood vessel has ruptured 2. Blood vessel blocked by a blood clot Reduced blood supply results in • Decreased oxygen/nutrient supply to the brain • 8 WB 8 Damage to the brain tissue LTPHN/JH/HB © 2010 8

Types of stroke WB 9 There are two main types of stroke: 1. Ischaemic – caused by a blockage (80% of all strokes) 2. 9 Haemorrhagic – caused by a bleed (20% of all strokes) LTPHN/JH/HB © 2010 9
Ischaemic Stroke WB 9 • Result of an obstruction blocking an artery carrying blood to the brain • Causes include: – Cerebral thrombosis – blood clot (thrombus) forms in a main artery – Cerebral embolus – obstruction caused by a blood clot, air bubble or globule of fat (embolism) formed elsewhere in the body and carried to the brain 10 LTPHN/JH/HB © 2010 10

Haemorrhagic Stroke WB 9 • Results of a burst blood vessel, causing haemorrhage into the brain • Haemorrhagic stroke may result from: – Intra-cerebral haemorrhage where a blood vessel bursts within the brain – Sub-arachnoid haemorrhage when a blood vessel on the surface of the brain bleeds into the sub-arachnoid space between the brain and the skull 11 LTPHN/JH/HB © 2010 11

Epidemiology of Stroke WB 10 • Around 111, 000 people have a stroke each year in the UK • Second most common cause single cause of death in UK • Significant numbers left with moderate or severe disabilities • Stroke consumes 5% of all NHS costs • Incidence has fallen by 40% over the past 20 years 12 LTPHN/JH/HB © 2010 12

WB 12 Risk Factors for Stroke Modifiable • • • 13 Non-modifiable Diet • Raised cholesterol • Physical inactivity • Alcohol High blood pressure Smoking Sleep apnoea Obesity Diabetes mellitis Atrial Fibrillation Previous Transient Ischaemic Attack LTPHN/JH/HB © 2010 Age Gender Ethnicity

Preventing Stroke WB 14 In order to prevent stroke, we need to: 1. 2. 3. Understand factors associated with stroke Know how individual causal factors contribute to the aetiology of stroke Understand these issues at both an individual and population level Primary prevention: preventing disease in healthy individual and population Secondary prevention: preventing the onset of stroke in patients with risk factors Tertiary prevention: preventing the recurrence of stroke in patients who have previously had a stroke or TIA 14 LTPHN/JH/HB © 2010 14

Methods of Prevention WB 15 Methods include: • Controlling high blood pressure • Monitoring elevated blood cholesterol and controlling this where appropriate • Prescribing drugs to thin the blood • Stopping smoking • Dietary improvements including avoiding excess fat, and avoidance of excess alcohol intake • Maintaining a healthy weight • Exercising regularly • Optimising control of diabetes 15 LTPHN/JH/HB © 2010 15

Epidemiological data and prevention WB 16 • Studies have demonstrated that the incidence of major stroke has fallen by 40% over the past 20 years (OXVASC) • Stroke registers also hold a wealth of data on the descriptive epidemiology of stroke, as well as its natural history and impact • Adequate data coverage and accuracy are crucial 16 LTPHN/JH/HB © 2010 16

NHS Health Checks WB 16 • Preventative checks for those aged 40 -74 • Assess risk of vascular disease, including stroke – Objective measurements (e. g. weight) – Self-reporting of lifestyle characteristics (e. g. smoking) • Patients advised how to reduce their risk Can an intervention like this really change behaviour? 17 LTPHN/JH/HB © 2010 17

Symptoms of a stroke WB 20 Symptoms may include any of the following: • Problems with speech • Weakness or sensory loss on one side of the body • Dizziness, nausea, balance and coordination problems • Visual problems: loss or double vision 18 LTPHN/JH/HB © 2010 18

Diagnosis of Stroke • • 19 WB 20 Head CT or MRI ECG Echocardiogram Carotid Duplex Heart Monitor Cerebral angiography Blood tests for cholesterol, glucose, clotting tendency etc LTPHN/JH/HB © 2010 19
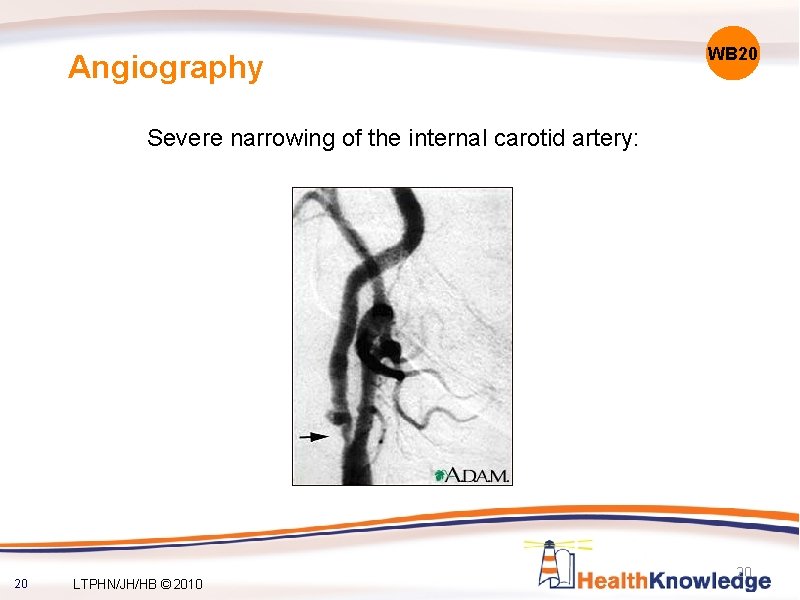
Angiography WB 20 Severe narrowing of the internal carotid artery: 20 LTPHN/JH/HB © 2010 20

Emergency Management WB 21 • Effectiveness of emergency management directly impacts outcome • Ideally, patients transported direct to stroke unit – Rapid triage – Specialist clinicians – Rapid brain imaging • Thrombolysis for ischaemic strokes – use of thrombolysis units 21 LTPHN/JH/HB © 2010 21

Determinants of Prognosis WB 21 • Long term outcome depends on: – – 22 Effectiveness of emergency intervention Extent of damage to brain Associated medical problems Predisposition to recurrence (i. e. risk factors) LTPHN/JH/HB © 2010 22

WB 21 23 LTPHN/JH/HB © 2010 23

Economic Cost of Stroke WB 21 • Stroke care costs the NHS approximately: – £ 7 billion per year in total – £ 2. 9 billion in direct care costs • 1 in 5 acute hospital beds and 1 in 4 long-term beds are occupied by stroke patients • For each stroke patient, the cost to the NHS is around £ 15, 000 over five years 24 LTPHN/JH/HB © 2010 24

Economic Cost of Stroke WB 22 • Total societal costs (treatment + productivity losses) = £ 8. 9 billion a year – 50% direct care costs – 27% informal care costs – 24% indirect costs • Human, personal cost to stroke survivors and their families 25 LTPHN/JH/HB © 2010 25

Quality of Life WB 22 • Individual’s perception of position in life in cultural, social, + environmental context • Influenced by: – Physical – Material – Social – Emotional well-being – Personal development – Purposeful activity 26 LTPHN/JH/HB © 2010 26

Quality of Life after a Stroke WB 22 • 1/3 will be left with significant disabilities • Measurement of health status must include an estimation of well being • Important factors include disability, depression, age and social support • Depression is also a common consequence of stroke 27 LTPHN/JH/HB © 2010 27

WB 23 Government strategies for stroke Targets for 2010: under 75 rates met National Stroke Strategy 10 point plan for action 28 LTPHN/JH/HB © 2010

WB 26 Summary • Stroke is declining but still big killer and disabler in UK • Stroke is preventable and treatable but requires: • Reliable data • Focus on prevention and risk reduction as well as treatment with healthprofessionals able to identify modifiable risk factors and support lifestyle behaviour change • A fully engaged public health workforce – including the ‘wider’ workforce/third sector etc 29 LTPHN/JH/HB © 2010
- Slides: 29