Public Health in Simcoe Muskoka Dr Charles Gardner

Public Health in Simcoe Muskoka Dr. Charles Gardner, Medical Officer of Health Dr. Lisa Simon, Associate Medical Officer of Health Dr. Colin Lee, Associate Medical Officer of Health

Presentation Overview • An overview of Public Health in Simcoe Muskoka • Environmental Health – Rabies Control • Chronic Disease, Family Health, SDOH • Clinical Service Programs – Vaccine Preventable Diseases – Communicable Disease – Sexual Health

Public Health Is… • A 160 year old movement • Strategies focused on populations • To prevent disease and injury, and protect and promote health

Taking Action On The Things That Make Us Healthy • Environment – physical, social, political, economic • Behavior – smoking, diet, physical activity, injuries, sexual health • Human Biology – age, gender, family history • Health Care – prevention, treatment, rehabilitation
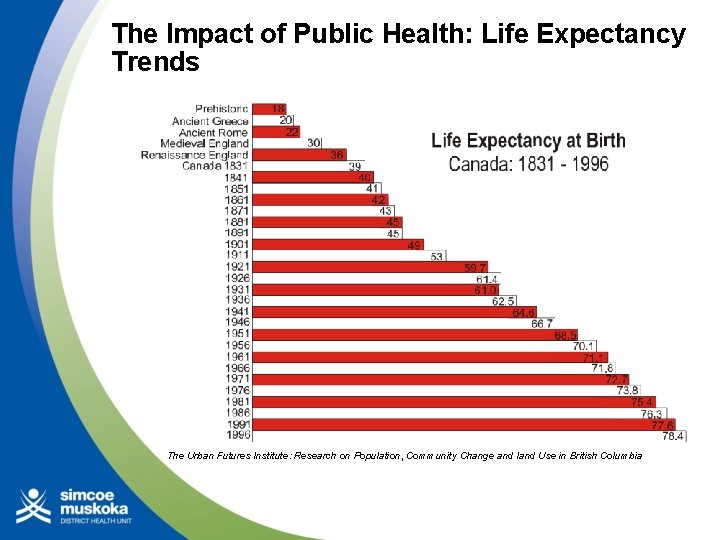
The Impact of Public Health: Life Expectancy Trends The Urban Futures Institute: Research on Population, Community Change and land Use in British Columbia

The Impact of the Public Health Movement • Beginnings of public sanitation movement in the 19 th century – Municipal water sanitation and sewage systems – Improving incomes, housing, nutrition, – Working conditions – Infection control practices: • Water and food safety • Health care – Vaccination (smallpox) Dr. John Snow, cholera and the Broad St. pump
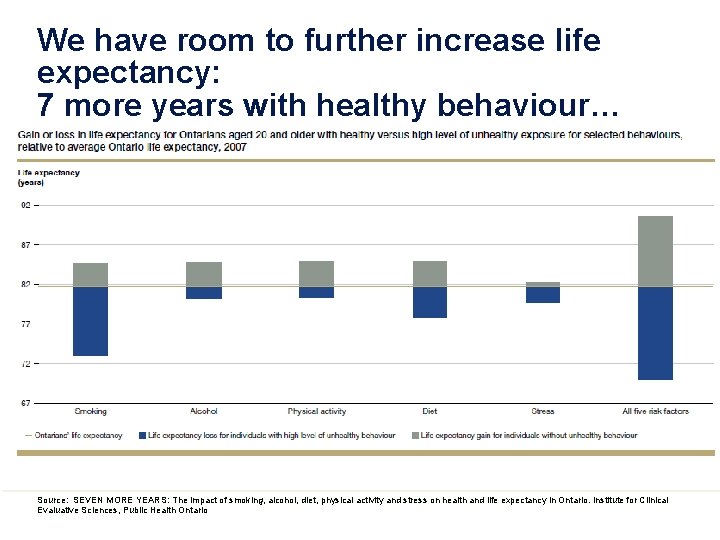
We have room to further increase life expectancy: 7 more years with healthy behaviour… Source: SEVEN MORE YEARS: The impact of smoking, alcohol, diet, physical activity and stress on health and life expectancy in Ontario. Institute for Clinical Evaluative Sciences, Public Health Ontario
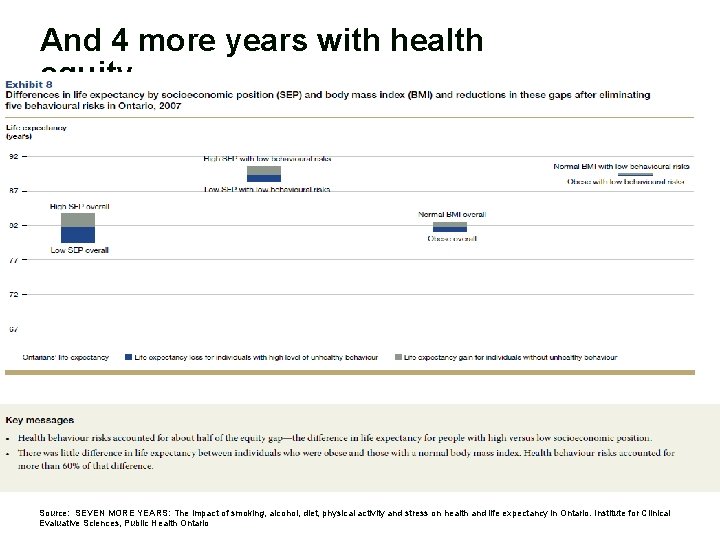
And 4 more years with health equity. Source: SEVEN MORE YEARS: The impact of smoking, alcohol, diet, physical activity and stress on health and life expectancy in Ontario. Institute for Clinical Evaluative Sciences, Public Health Ontario
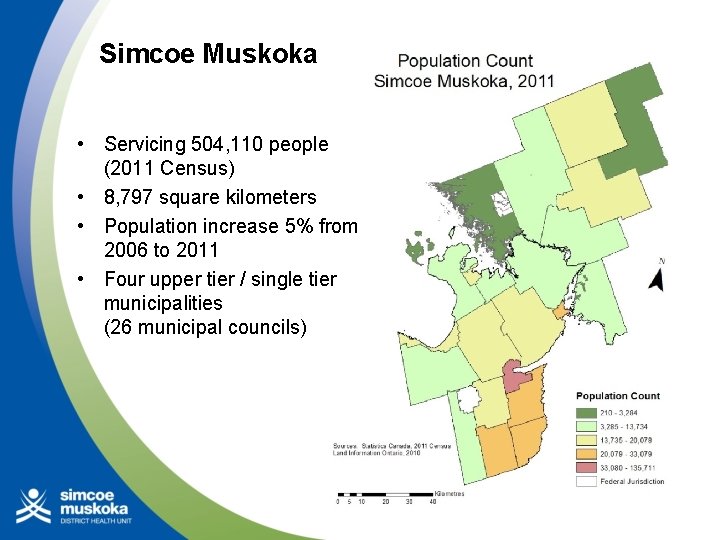
Simcoe Muskoka • Servicing 504, 110 people (2011 Census) • 8, 797 square kilometers • Population increase 5% from 2006 to 2011 • Four upper tier / single tier municipalities (26 municipal councils)

The Ontario Public Health Standards & Protocols

Water • Drinking – To ensure the drinking water the public has access to is potable by: • assessing risk in reports of adverse results • responding to identified risks and hazards • informing and educating the public • Inspection of drinking water systems

Food Safety Program • 2011 Highlights – Over 6000 inspections of high, medium and low-risk premises – Responded to 398 consumer complaints – 21 charges laid under Food Premises Regulation – 1200 food handlers pass food safety certification course – Food safety calendar printed for distribution to over 1900 high and mediumrisk premises in Simcoe Muskoka – Issued over 700 Special Event Permits

Emergency Management • External emergency planning with partnerships/committees: – municipalities, health sector coordination, other health units, Red Cross & Social Service Agencies. • Response experiences: – H 1 N 1 influenza pandemic, G 8 Summit, train derailment, tornadoes/storm events, floods, power outages, chemical fires.

Immunization Provision and Promotion • 7, 629 vaccinations delivered in 7 health unit office clinics (i. e. multiple clinics offered in each of our offices) • 11, 517 influenza vaccinations delivered in 53 public clinics • 20, 252 HBV, HPV and Meningococcal vaccinations delivered in school clinics • Thus 39, 398 total vaccinations delivered by SMDHU staff in 2011 • Most early childhood vaccines provided by family physicians (supplied and guided by public health)

Dental services provided in Simcoe Muskoka • Healthy Smiles Ontario clinics provide full dental services to lowincome families and others on government-funded dental benefits. • Full treatment services at the health unit’s Barrie clinic location. • Healthy Smiles Ontario bus visits communities throughout Simcoe Muskoka. • Oral health surveillance in schools, and community reporting.

Reproductive Health Program • Preconception Health – An increased proportion of individuals in their reproductive years are physically, emotionally, and socially prepared for conception • Healthy Pregnancies and Birth Outcomes – An increased proportion of pregnant women and their families adopt practices to support a healthy pregnancy • Preparation For Parenthood – An increased proportion of expectant parents are physically, emotionally, and socially prepared to become parents

HBHC Program Mandate & Scope • Province-wide voluntary prevention/early intervention program • Goals: – To promote optimal physical, cognitive, communicative and psychosocial development in children who are at risk prenatal to age 6 years – To act as a catalyst for a coordinated, effective, integrated system of services and supports for healthy child development and family wellbeing through the development of a network of service providers and participation in community planning activities

Child Health Program • Positive Parenting – E. g. Triple P Positive Parenting Program • Breastfeeding – E. g. Breastfeeding promotion and supports • Growth and Development – E. g. Enhanced 18 month well baby visit – E. g. Child nutrition, physical activity, etc.

Injury and Substance Misuse Prevention Program • Injury – Road and off road safety – Falls across the lifespan, Regional Falls Prevention Strategy for older adults – Concussion • Substance Misuse – Work with all levels of government on alcohol control measures – Promote Low Risk Drinking Guidelines and clinical screening, brief intervention and referral – Collaborating on an Alcohol and Other Drug Strategy for Simcoe and Muskoka
Chronic Disease Prevention Program • Tobacco Program – Preventing young people from smoking – Protecting people from exposure to second-hand smoke – Supporting people to quit smoking – Enforcing the Smoke Free Ontario Act • Healthy Lifestyle Program – Promoting healthy eating and food security – Promoting physical activity, active transportation – Reviewing official and other municipal plans related to health

Healthy Schools • Work with School Boards and community partners in Simcoe Muskoka to enhance the physical, emotional, mental, and social health of the whole school community. • Implement specific initiatives in partnership: – E. g. Roots of Empathy

Primary Care Portal www. smdhu. org/pcportal

Final Thoughts • Improving the health of the public is achieved through joint work with many partners in and out of the health care system – most commonly with family physicians. • The Simcoe Muskoka District Health Unit continues to be committed to excellence in public health.

RABIES PREVENTION AND CONTROL IN SIMCOE MUSKOKA Charles Gardner, MD, CCFP, MHSc, FRCPC

CLINICAL SCENARIOS • Case 1: Facial Bite by Dog in Guatemala § Dog unavailable § Dog known to be vaccinated § Victim previously immunized 5 years ago • Case 2: Bat Found in Bedroom § Husband awoke to something touching him, he grabbed bat and threw it across room § Wife reports not being touched by bat § Bat killed… awaiting testing for rabies
RABIES VIROLOGY • Zoonotic disease of mammalian • species – humans are incidental hosts RNA virus § Single strand, negative-sense § Rhabdoviridae family, genus Lyssavirus • Most severe acute viral infection of • • humans, with a case fatality rate of almost 100%. Transmitted by percutaneous or mucous membrane exposure to infected saliva – a bite, scratch, (organ transplants) Migration of virus to CNS via the peripheral nerves - encephalomyelitis

RABIES TRANSMISSION CHARACTERISTICS • Likelihood of transmission post bite of a rabid animal is 15% (up to 60% with deep wounds) without rabies post exposure prophylaxis • Completely prevented with timely vaccination – pre or post exposure § failure rates (with a delay or breach in protocol) range from 1 in 80, 000 in developed countries to 1 in 12, 000 in developing countries • Incubation period 3 to 8 weeks after exposure – can range from a few days to several years § Depends on wound severity, innervation of location, distance from CNS • Period of communicability § Only known reliably for dogs, cats, ferrets • 3 -7 days before onset of clinical signs § Longer in other species (skunks, bats)

HUMAN CASES IN CANADA / ONTARIO • In Canada, 9 human cases occurred between 1960 and 2009 (NACI, 2012). • In Ontario, 1 human case occurred in 2012 that was acquired while travelling outside of Canada • The last case of human rabies that was acquired in Ontario occurred in 1967. • Historically, skunks, foxes and raccoons are the main reservoirs in Ontario. Arrival from northern Ontario in the 1950’s • In Ontario, bats currently pose the biggest threat of transmitting the virus to humans. • Dog exposures are the greatest risk for returning travelers – other mammalian species also a risk Source: Based on PHO Grand Rounds , Tuesday April 21, 2015

RABIES CONTROL STRATEGIES In Ontario, four main strategies have been used to prevent rabies cases in humans: 1. Public Health messaging informing people to avoid contact with wild animals. 2. Wildlife rabies control programs targeting skunks, raccoons and foxes. (note: no program for bat rabies) 3. Vaccinating bridge vectors such as dogs, cats, other pets, and farm animals. 4. Human Rabies Post-Exposure Prophylaxis (RPEP), and Pre. Exposure Prophylaxis Source: PHO Grand Rounds , Tuesday April 21, 2015

MANY PARTNERS TO CONTROL RABIES Hospitals/ ER Rooms Primary Care Providers Other Health Units Police Animal Control SMDHU MOHLTC Municipalities PHO Humane Society OAVT OMAFRA Veterinarians CFIA MNR
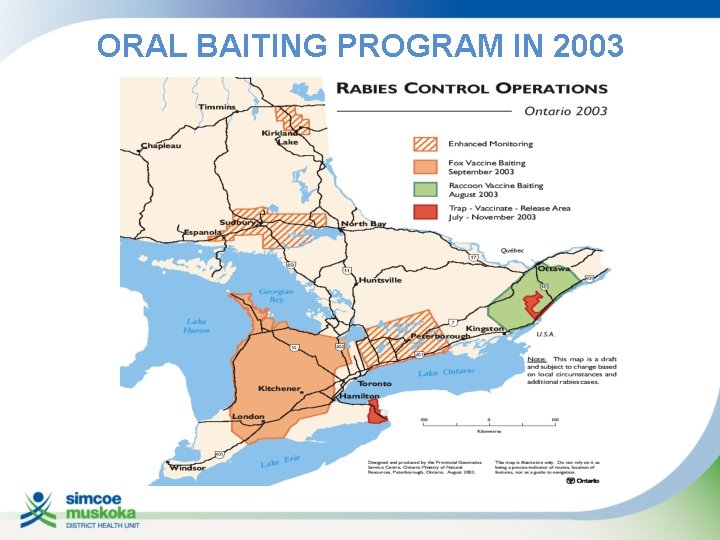
ORAL BAITING PROGRAM IN 2003
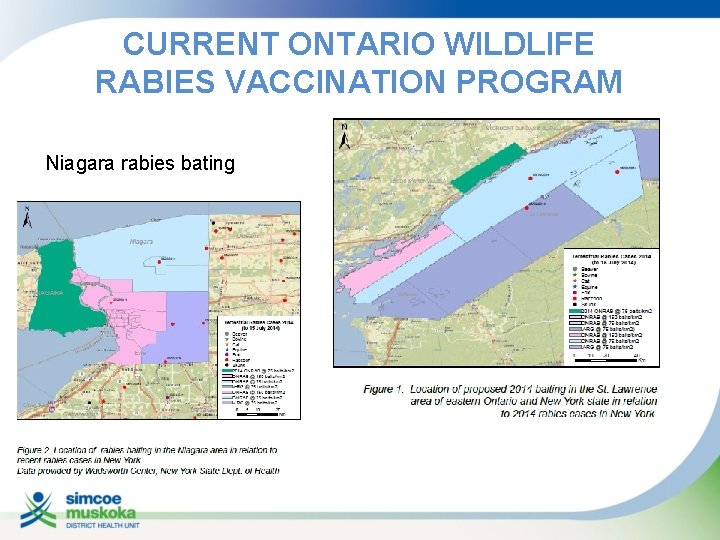
CURRENT ONTARIO WILDLIFE RABIES VACCINATION PROGRAM Niagara rabies bating St. Lawrence River rabies bating
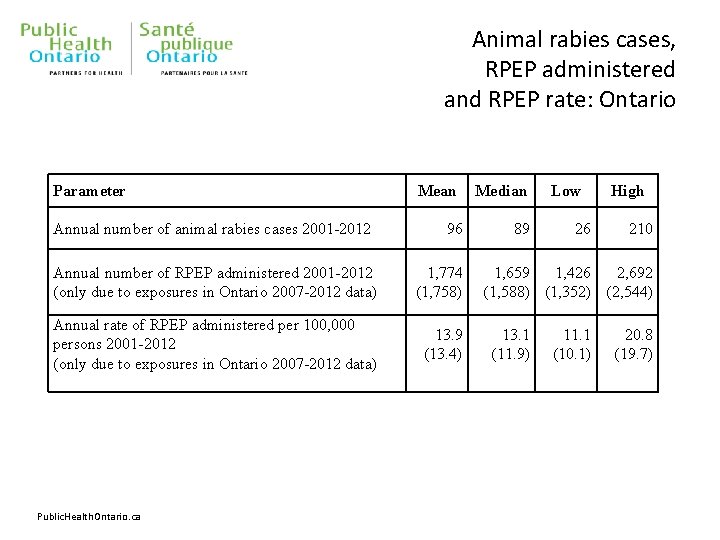
Animal rabies cases, RPEP administered and RPEP rate: Ontario Parameter Annual number of animal rabies cases 2001 -2012 Mean 96 Annual number of RPEP administered 2001 -2012 (only due to exposures in Ontario 2007 -2012 data) 1, 774 (1, 758) Annual rate of RPEP administered per 100, 000 persons 2001 -2012 (only due to exposures in Ontario 2007 -2012 data) 13. 9 (13. 4) Public. Health. Ontario. ca Median 89 Low 26 High 210 1, 659 1, 426 2, 692 (1, 588) (1, 352) (2, 544) 13. 1 (11. 9) 11. 1 (10. 1) 20. 8 (19. 7)
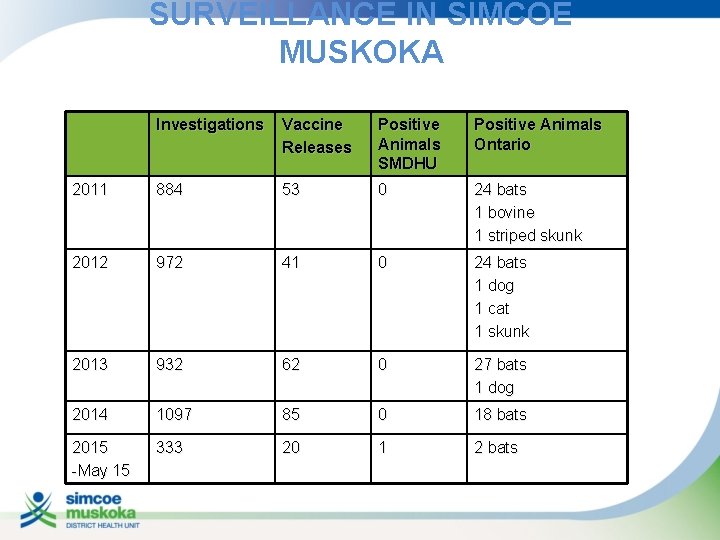
SURVEILLANCE IN SIMCOE MUSKOKA Investigations Vaccine Releases Positive Animals SMDHU Positive Animals Ontario 2011 884 53 0 24 bats 1 bovine 1 striped skunk 2012 972 41 0 24 bats 1 dog 1 cat 1 skunk 2013 932 62 0 27 bats 1 dog 2014 1097 85 0 18 bats 2015 -May 15 333 20 1 2 bats
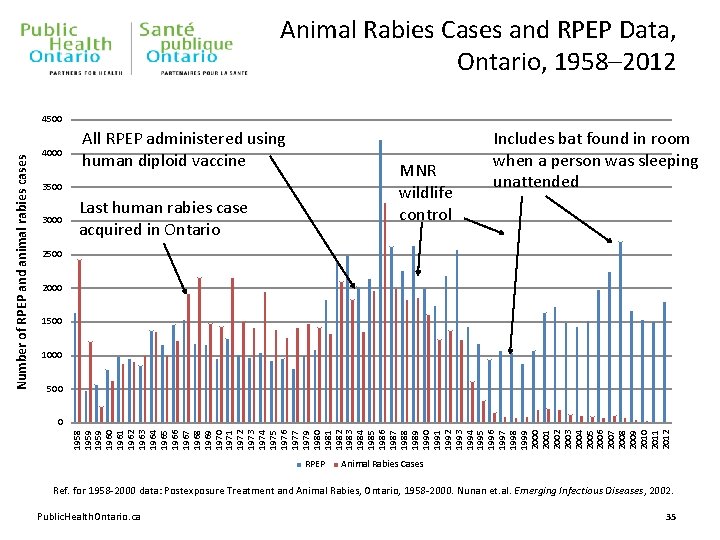
Animal Rabies Cases and RPEP Data, Ontario, 1958– 2012 4000 All RPEP administered using human diploid vaccine MNR wildlife control 3500 3000 Last human rabies case acquired in Ontario Includes bat found in room when a person was sleeping unattended 2500 2000 1500 1000 500 0 1958 1959 1960 1961 1962 1963 1964 1965 1966 1967 1968 1969 1970 1971 1972 1973 1974 1975 1976 1977 1979 1980 1981 1982 1983 1984 1985 1986 1987 1988 1989 1990 1991 1992 1993 1994 1995 1996 1997 1998 1999 2000 2001 2002 2003 2004 2005 2006 2007 2008 2009 2010 2011 2012 Number of RPEP and animal rabies cases 4500 RPEP Animal Rabies Cases Ref. for 1958 -2000 data: Postexposure Treatment and Animal Rabies, Ontario, 1958 -2000. Nunan et. al. Emerging Infectious Diseases, 2002. Public. Health. Ontario. ca 35

RABIES POST-EXPOSURE MANAGEMENT APPROACH 1. Wound care – irrigation (15 minutes), tetanus prophylaxis and antibiotics as appropriate, delayed wound closure 2. Report animal bites to local Public Health (requirement of the HPPA). § Public health staff role includes assessing human exposures to animals to advise on the need for RPEP. • Dogs, cats and ferrets may be observed for 10 days postexposure. • Testing of animals (wild or ill domestic) 3. A course of four rabies vaccines as well as rabies immune globulin (RIG). • Decision based on risk assessment – Canadian Immunization Guidelines, and the Guidance Document for the Management of Suspected Rabies Exposures (Public Health Division, MOHLTC 2013) Source: PHO Grand Rounds, Tuesday April 21, 2015

EXPOSURE INDICATIONS FOR VACCINATION • Species and local prevalence of rabies (exposing animal and in other species) • The type of exposure - bite, non-bite (e. g. salivary contact with open skin or mucous membrane, transplant of infected organs), or direct contact with a bat. • Provoked versus unprovoked bite (not helpful for wild animals) • The vaccination status and behaviour of a domestic animal. • The age of the exposed person (children higher risk) • The location and severity of the bite (hands and face) • Source animal for observation (cats, dogs, ferrets) or testing • Resources § Table 1: Risk Assessment Related to the Exposure to the Potentially Rabid Animal – Canadian Immunization Guide § Table 1: Summary of Post-Exposure Prophylaxis (PEP) for Persons Potentially Exposed to Rabies - Guidance Document for the Management of Suspected Rabies Exposures, MOHLTC

EXPOSURE RISK RECOMMENDATIONS: BATS • Current bat exposure recommendation: Post-exposure rabies prophylaxis following bat contact is recommended when: § There has been direct contact with a bat (touching or landing on a person), AND § A bite, scratch, or saliva exposure into a wound or mucous membrane cannot be ruled out. • Revision of NACI recommendation from 1998 to 2009, that people who may not be aware of or able to report a bat bite (e. g. , sleeping person, young child, cognitively impaired) receive vaccination : § expected to prevent a case in Canada once every 84 years § 314, 000 people would need to be treated (cost of $2 billion) to prevent 1 case § therefore revised recommendation in 2009

POST-EXPOSURE PROPHYLAXIS PROTOCOL: RABIES VACCINE § Rabies vaccines (Rab) • Human Diploid Cell Rabies Vaccine). (HDCV) IMOVAX® Rabies • Purified Chick Embryo Cell Rabies Vaccine), (PCECV) Rab. Avert® § Not Previously Immunized • Immunocompetent – 4 doses (Day 0, 3, 7, 14) – 1 ml IM (never gluteal, as risking reduced immune response) • Immunocompromised (including corticosteroids, chloroquine) – 5 doses (Day 0, 3, 7, 14, 28) – 1 ml IM § Previously immunized • 2 doses – 1 ml IM (Day 0, 3) • 4 doses if previous vaccination was not with HDCV or PCECV

POST-EXPOSURE PROPHYLAXIS PROTOCOL: RABIES IMMUNE GLOBULIN • Post Exposure Prophylaxis § Rabies Immune Golbulin [Human] Hyper. Rab ® S/D § Human Rabies Immunoglobulin- Imo. Gam ® • Not Previously Immunized § To achieve prompt levels of neutralizing antibodies in the wound during the initial phase of management § 20 IU/kg - Day 0 (can be up to 7 days post onset of PEP series, if not immediately available) § If possible, entire volume to be given at the wound site(s) – remainder IM (away from first dose of rabies vaccine) • Previously Immunized - not indicated

PRE-EXPOSURE PROPHYLAXIS • Efficacy § Adequate antibody titres for up to 2 years after immunization – may wane after • 7 days after a booster dose 100% are adequately protected • Indications: § Laboratory workers who handle rabies virus. § Veterinarians, veterinary staff, animal control and wildlife workers. § Travelers to high risk locations – WHO (http: //www. who. int/rabies/Global_Rabies_ITH_2008. png ) § Hunter and trappers in areas with confirmed rabies. § Spelunkers (cavers). • Rabies Vaccine § 3 doses – 1 ml IM (days 0, 7 and 21 or 28) • Rabies Immune Globulin § Not indicated

VACCINATION SAFETY • HDCV risk is estimated to be minor; § Pain, erythema, swelling and itching at the injections site in 30% to 74%; § Headache, nausea, abdominal pain and dizziness in 20%. § Immune complex-like allergic reactions in up to 6% of persons receiving booster doses of HDCV. Few hospitalizations and no deaths. § Anaphylaxis in up to 1 in 10, 000 § In 2012 in Ontario, of the 9812 doses administered, there were 4 adverse events, none with serious outcomes (PHO) • RIG § Local pain, erythema and induration are common. Headache and low-grade fever may follow administration. § Made from human plasma – potential risk of undetected infectious agents (CDC)

CONTRAINDICATIONS AND PRECAUTIONS • No contraindications to the use of rabies vaccine or RIG after significant exposure to a proven rabid animal § Pregnancy not a contraindication for post exposure prophylaxis • Caution re compartment syndrome with wound infiltration • Seek expert consultation if hypersensitive to any ingredient in the formulation or container: § IMOVAX® Rabies: neomycin, phenol red § Rab. Avert®: amphotericin B, chick protein, chlortetracycline, neomycin, polygeline § (gelatin) § IMOGAM® Rabies: latex in vial stopper § HYPERRAB® S/D: • RIG: § Potential anaphylaxis with subsequent serum products for patients with specific Ig. A deficiency § Postpone live vaccinations 3 months afterward

POST VACCINATION SEROLOGIC TESTING • Serologic testing is not routinely indicated with vaccination (pre or post exposure prophylaxis) for healthy persons • Indications for serology testing: § Vaccination given by the ID route – check serology at least 2 weeks after completion of series. § Ongoing high risk of exposure to rabies (every 6 / 12 for continuous risk, to every 2 years for frequent risk). § Substantial deviation from the recommended postexposure schedule – check serology 7 to 14 days after completing the series. § Immunization with a vaccine other than HDCV or PCECV – check serology at least 7 to 14 days after completing the series – can be day 0, and discontinue RPEP after 2 doses HDCV or PCECV if sufficient titre § Immunocompromised persons, or if taking chloroquine - check serology 7 to 14 days after completing the series. Revaccination with a second rabies vaccine series if unacceptable response, followed by serologic testing

PUBLIC HEALTH MANDATE / SERVICES • Animal Bite Investigation § Receive reports of all animal bites (1097 in 2014) § Animal Management • Specimen testing (102 in 2013; 13 in 2014) • Quarantine animal (dogs, cats, ferrets) – Normal 10 days – Follow up on animal vaccination • Companion animal vaccination § Low cost vaccination clinics § Animal vaccination enforcement (HPPA) • Vaccine consultation and provision (62 in 2013; 83 in 2014) • Public and health care provider communication

HOW TO CONTACT US • Website resources – Primary Care Professionals’ Portal (Environmental Health) § http: //www. simcoemuskokahealth. org/JFY/PCPortal. aspx • Rabies email: rabies. program@smdhu. org • New Rabies Program Phone Line 705 -721 -7520 ext. 8894 § For physician consult and vaccine release • Animal exposure reporting § Rabies fax line 705 -725 -8132 § Reporting form: http: //www. simcoemuskokahealth. org/Libraries/JFY_Health_Care_Professio nals/150203 Rabies_and_Animal_Exposure_Report_Form. sflb. ashx • After Hours 1 -888 -225 -7851

CLINICAL SCENARIOS REVISITED • Case 1: Facial Bite by Dog in Guatemala § Dog unavailable § Dog known to be vaccinated § Victim previously immunized 5 years ago • Case 2: Bat Found in Bedroom § Husband awoke to something touching him, he grabbed bat and threw it across room § Wife reports not being touched by bat § Bat killed… awaiting testing for rabies

Chronic Disease Prevention, Family Health, and the Social Determinants of Health Lisa Simon MD, MPH, CCFP, FRCPC Associate Medical Officer of Health

WHY? • Majority of current burden of disease is attributable to chronic disease and injuries (CDP) • Prenatal and early childhood are most vulnerable developmental periods, with lifelong implications (FH) • Social determinants of health are strong, pervasive risk factors, with lifelong implications (SDOH)

HOW? CORE FUNCTIONS FOR PUBLIC HEALTH • Population health assessment and surveillance • Health Promotion - Ottawa Charter for Health Promotion, 1986: § Build healthy public policy § Create supportive environments (social and physical) § Strengthen community actions § Develop personal skills § Reorient health services • Disease and Injury Prevention • Health Protection • Emergency Response and Preparedness


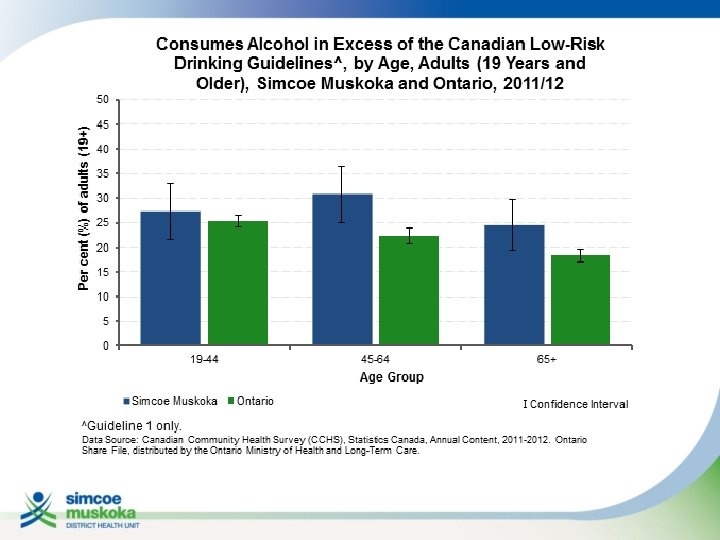
FOCUS ON: ALCOHOL Case: • 60 year old man seeing you for periodic health exam • Known hypertensive • When asked about alcohol consumption, casually states “I enjoy my wine”

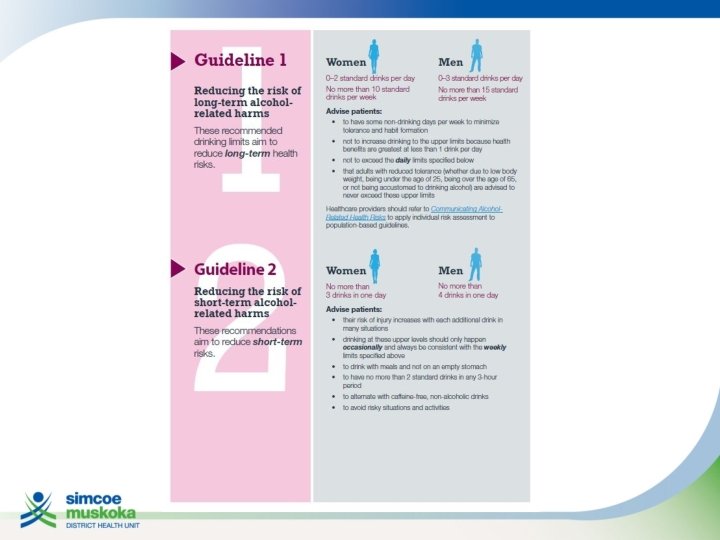

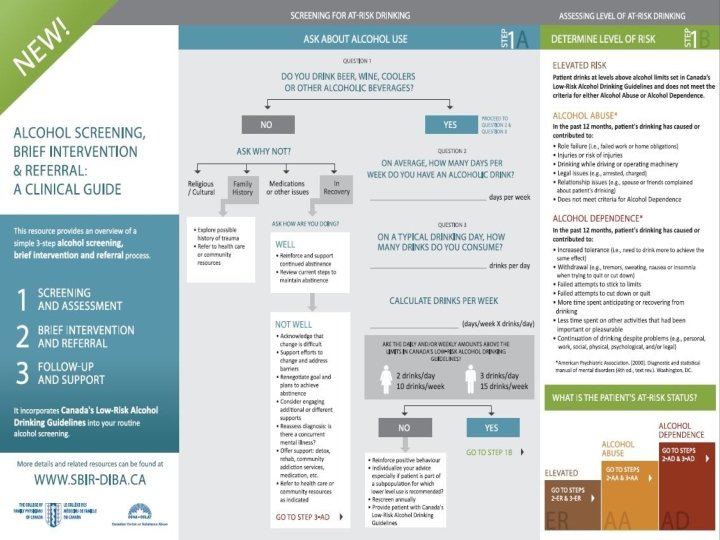

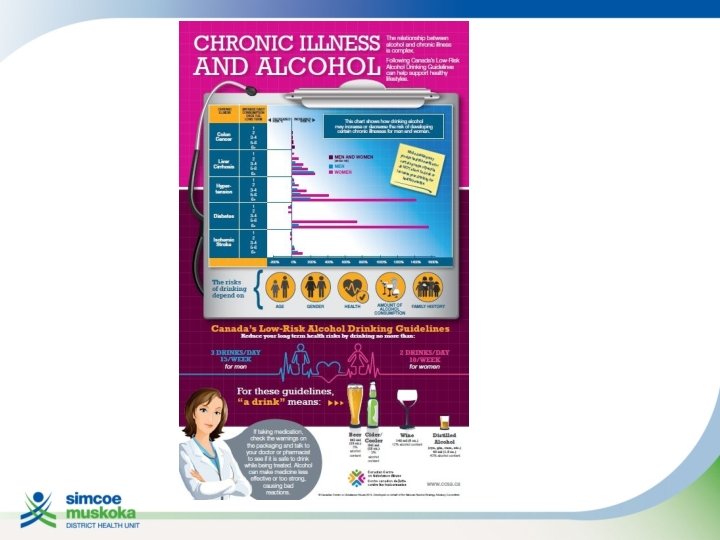


FOCUS ON: EARLY CHILDHOOD DEVELOPMENT Cases: • 1 month well baby visit, healthy infant, mother experiencing post-partum depression, lack of social support • 18 month enhanced well baby visit, parenting challenges

1 MONTH WELL BABY VISIT: PPD • In addition to managing her PPD, consider referral to Healthy Babies Healthy Children (HBHC) Program • Home visiting programs, such as HBHC: § Parenting after home visiting programs has been shown to have consistent positive movement. (Bull J et al. London: NHS Health Development Agency; 2004. ) § Some home visitation programs have been effective at reducing child maltreatment and associated outcomes such as injuries. (Mac. Millan HL et al. Lancet 2009; 373: 250– 66. )

18 MONTH WELL BABY VISIT: PARENTING • In additional to developmental screening & early intervention as necessary, consider referral to Triple P Positive Parenting Program • Triple P Positive Parenting Program: § Can be effective in preventing child maltreatment (Prinz RJ et al. Population-based prevention of child maltreatment: the U. S. Triple P system population trial. Prev Sci 2009; 10: 1– 12. ) § Positive effects on children's social, emotional and behavioral outcomes; parenting practices; etc. (Sanders et al. The Triple P-Positive Parenting Program: A systematic review and meta-analysis of a multi-level system of parenting support. Clinical Psychology Review 34 (2014) 337– 357. )

SOCIAL DETERMINANTS OF HEALTH (SDOH) • • • • Income and Income Distribution Education Unemployment and Job Security Employment and Working Conditions Early Childhood Development Food Insecurity Housing Social Exclusion Social Safety Net Health Services Aboriginal Status Gender Race Disability Source: Juha Mikkonen and Dennis Raphael, 2010

INCOME AND HEALTH • “There is strong and growing evidence that higher social and economic status is associated with better health. In fact, these two factors seem to be the most important determinants of health. ” (Public Health Agency of Canada)
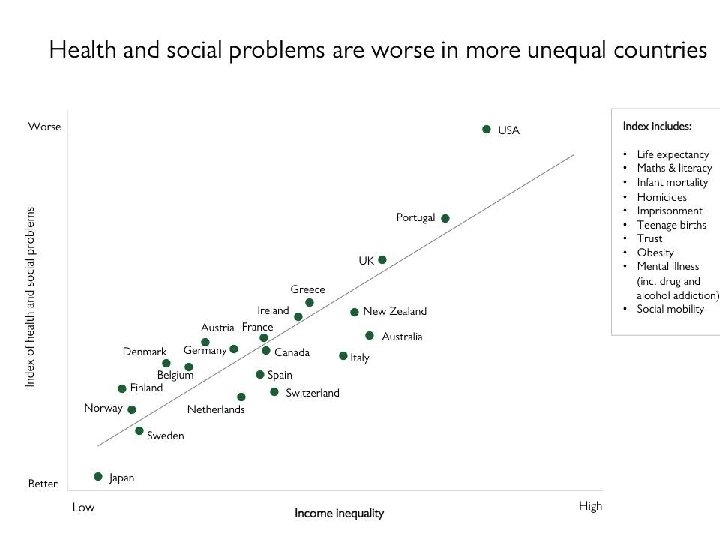
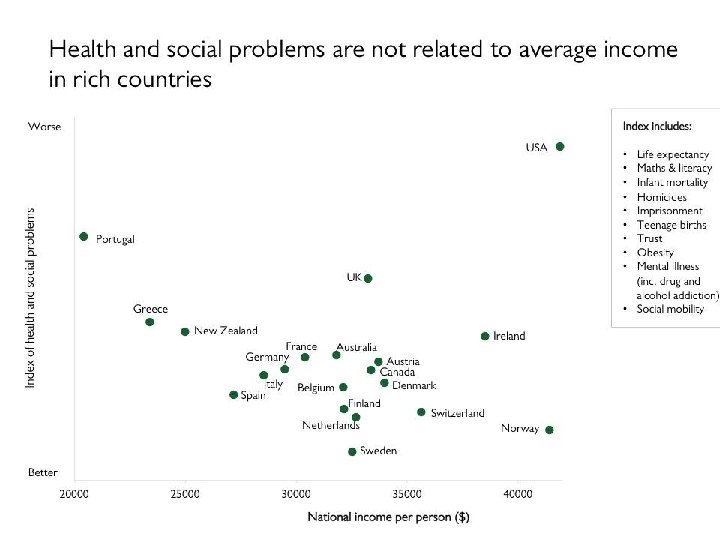

FOCUS ON: INCOME AND HEALTH Case: • 25 year old single mother of two young children, struggling financially
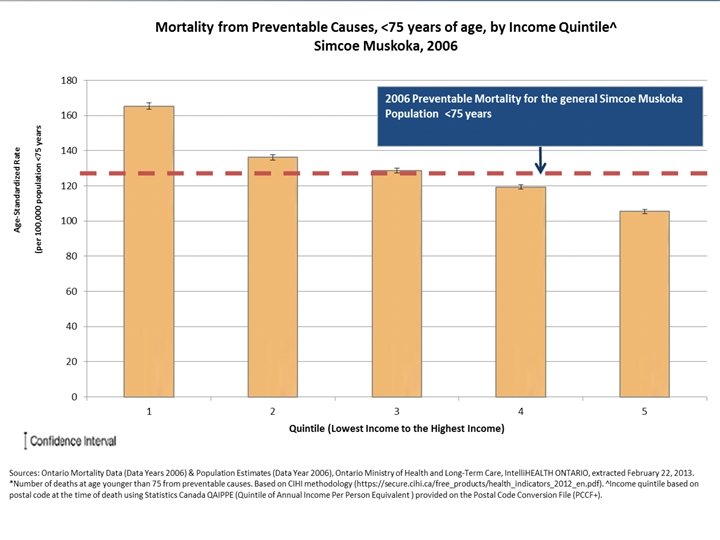

INCORPORATING SDOH INTO FM PRACTICE • Micro: Clinical § 1. Regularly screen patients for poverty, and intervene where necessary. § 2. Ensure your practice is accessible to all patients, especially marginalized populations. § 3. Offer advanced access and same-day scheduling. § 4. Build an antipoverty team that is shaped around your community’s needs. § 5. Understand provide forms for provincial/territorial social assistance programs. • Meso: Community • Macro: Healthy public policy Source: CFPC. Best Advice – Social Determinants of Health. 2015. See related: OCFP. Poverty: a Clinical Tool for Primary Care in Ontario. Access both at SMDHU Portal or http: //ocfp. on. ca/cpd/povertytool

Clinical Services at SMDHU Colin Lee MD, MSc, CCFP(EM), FRCPC Associate Medical Officer of Health

Clinical Services Team Structure • Vaccine Preventable Disease Team – Goal: To reduce or eliminate the burden of vaccine preventable diseases. • Communicable Disease Team – Goal: To prevent or reduce the burden of infectious diseases of public health importance • Sexual Health Team – Goal: To prevent or reduce the burden of sexually transmitted infections and blood-borne infections. – Goal: To promote healthy sexuality.

Examples of Vaccine-Preventable Disease Team Activities
School Immunization Programs • Hepatitis B (Grade 7) – Only 2 immunizations are required vs 3 for the adult schedule • Meningococcal C-ACYW-135 (Grade 7) • HPV (Grade 8 girls) – Uptake remains lower than optimal – multiple reasons, but still impacted by initial negative media and perceived sexual promiscuity associated with being vaccinated – 2013 US estimates of reduction in HPV prevalence following intro of vaccine – What if a parent of one of your male adolescent patients asks you for the HPV vaccine for their son?

Immunizations and school suspensions • Health Unit (HU) required under the Immunization of School Pupil’s Act (ISPA) to collect and maintain up-to-date records of immunization for every child registered in school in Simcoe and Muskoka • Under ISPA, parents required to provide HU with proof of completed immunization for following diseases or with appropriate documentation if choose not to immunize child: – Diseases: Diphtheria, Tetanus, Polio, Measles, Mumps and Rubella – NEW requirement for 2014/15 school year • Meningococcal Disease , Pertussis and Varicella (for children born in 2010 or later) – Documentation: Form 1 - Medical Exemption, or Form 2 - Statement of Conscience or Religious Belief Affidavit – May be suspended if one of the above aren’t provided

Adverse Events Following Immunization (AEFIs)

Vaccine Hesitancy • Understand the specific vaccine concerns of the parent: Use motivational interviewing, ie, questions that are client-centred, semi-directive and aimed at changing behaviour • Stay on message and use clear language to present evidence of vaccine benefits and risks fairly and accurately, e. g. “Vaccines are safe and effective, and serious disease can occur if your child and family are not immunized. ” • Inform parents about the rigour of the vaccine safety system • Address the issues of pain with immunization – Reducing the pain of childhood vaccination: An evidence-based clinical practice guideline. CMAJ 2010; 182(18): 1989 -95. • Do not dismiss children from your practice because parents refuse to immunize Working with vaccine-hesitant parents. Mac. Donald NE, Finlay JC; Canadian Paediatric Society Infectious Diseases and Immunization Committee. Paediatr Child Health 2013; 18(5): 265 -7

VPD Resources for Clinical Practice • Available on SMDHU’s web portal for primary care providers: – MOHLTC publicly funded immunization schedule – Canadian immunization guide (online) and new NACI statements – Patient resources: • SMDHU vaccine fact sheets • SMDHU Focus on Health. STATS 2011 report on vaccines (& references) – And more…

Examples of Communicable Disease Team Activities

Communicable Diseases Reportable to Public Health

Advising on chemoprophylaxis for contacts of select CDs – examples: • Pertussis • Invasive Group A Strep • Invasive meningococcal disease • Haemophilus influenza B • Measles • Hepatitis B • HIV • Influenza outbreaks
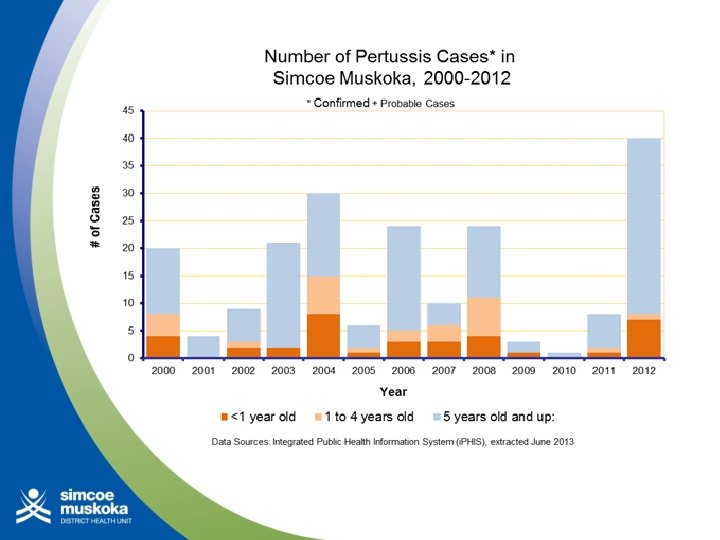

Pertussis: Management of Contacts • Period of Communicability: Highly communicable in the early catarrhal stage and beginning of the paroxysmal stage (first 2 weeks) and then communicability gradually decreases and becomes negligible in about 3 weeks. No longer communicable after 5 days of effective treatment. • There is no evidence that antibiotic prophylaxis of contacts changes the epidemic course of pertussis in the community, therefore, it is only recommended for the following contacts of confirmed pertussis cases who are: – household contacts (including attendees at family daycare centers) where there is a vulnerable person defined as an infant < 1 year of age [vaccinated or not] or a pregnant woman in the third trimester.

Pertussis: Management of Contacts (cont. ) – For out of household exposures, vulnerable persons, defined as infants less than one year of age regardless of immunization status and pregnant women in their third trimester who have had face-to-face exposure and/or have shared confined air for > 1 hour. • The local health unit will identify persons who meet the contact definition above and advise them about chemoprophylaxis and refer them to their physician for prescriptions. Prophylaxis is the same as treatment (macrolide) and should be given within 21 days after exposure.

Public Health - CD Resources Useful for Clinical Practice • General: – Red Book (AAP) – Ontario Public Health Standards (OPHS) ID protocol – Appendix for each reportable disease (free online) – SMDHU communicable disease fact sheets • TB: – Tuberculosis: Information for Health Care Providers (Lung Association, free online) – Canadian TB Standards, 7 th edition (released June 2013) • Key updates on SMDHU website and through Health. FAX – Increased disease activity, emerging infections, etc.

Examples of Sexual Health Team activities

Sexually Transmitted Infections • A 35 y. o. woman is a patient in your practice. During routine prenatal testing, she tests positive for gonorrhea through a cervical PCR swab. • As a family physician in Simcoe-Muskoka, what are your responsibilities to the woman, her sexual contacts and to the public health unit? How can the public health unit assist you?

New: PHO Guidelines for Testing and Treatment of Gonorrhea in Ontario, 2013 Select messages: • Issue: – Emergent multi-drug resistant gonorrhea • Testing: – Culture is preferred option for laboratory testing of symptomatic patients • Treatment: – Oral cefixime is no longer first line therapy for the treatment of gonorrhea in Ontario – New first line therapy: Ceftriaxone 250 mg IM + Azithromycin 1 g PO Anything else, given she’s pregnant?

Information requested from Public Health on a standardized form • Demographic and contact information • Date of positive test: • Reason for testing: – Symptoms – Routine test – Contact of a case – Prenatal Screen • Treatment provided and Date of Treatment: • Check here if patient is pregnant: – E. D. C.

Information requested from Public Health on a standardized form (cont. ) • Partner Notification: • Public Health will contact patient to ensure notification, education, testing and/or treatment of partner(s) is completed unless otherwise indicated by physician. Partner(s) within the last 2 months should be notified for testing and treatment. • Patient informed that a Public Health Nurse will be calling him/her: □ Yes □ No
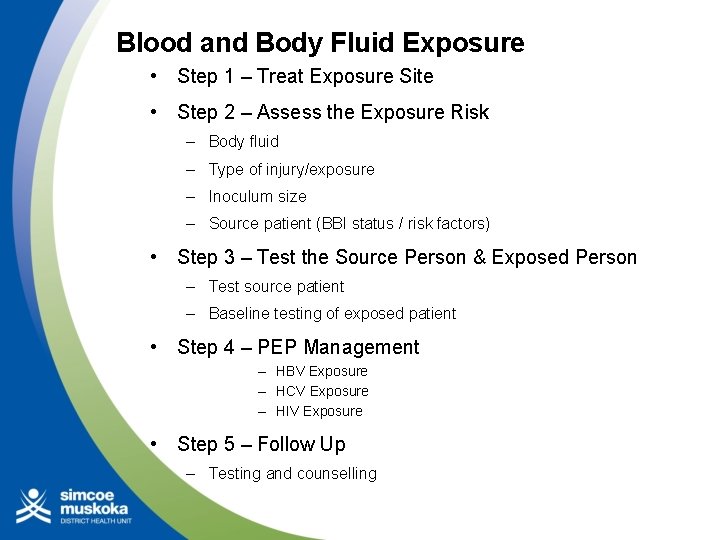
Blood and Body Fluid Exposure • Step 1 – Treat Exposure Site • Step 2 – Assess the Exposure Risk – Body fluid – Type of injury/exposure – Inoculum size – Source patient (BBI status / risk factors) • Step 3 – Test the Source Person & Exposed Person – Test source patient – Baseline testing of exposed patient • Step 4 – PEP Management – HBV Exposure – HCV Exposure – HIV Exposure • Step 5 – Follow Up – Testing and counselling

Public Health – SH Resources Useful for Clinical Practice • Canadian Guidelines on STIs (online) • PHO guidelines on gonorrhea and quick reference (online) • SMDHU post-exposure management documents (online) • SMDHU can provide clinicians with supply of STI medications for free for their patients.

Primary Care Portal www. smdhu. org/pcportal
New resources for primary care providers 1 2 3
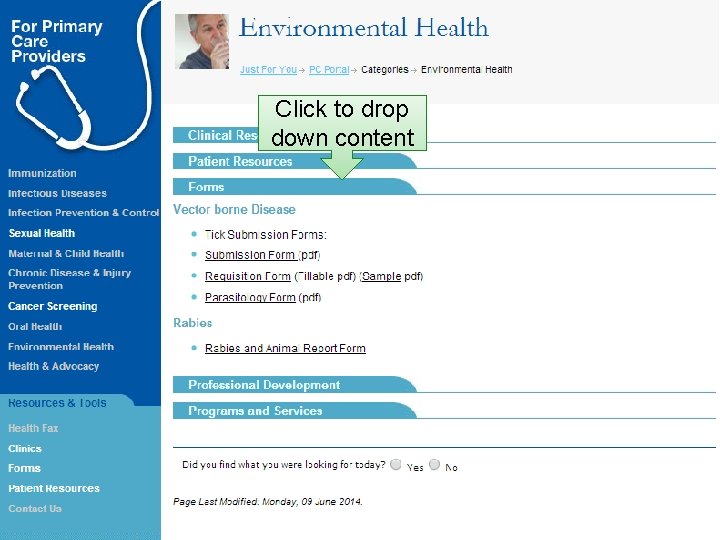
Click to drop down content
- Slides: 96