PTSD Looking Back Looking Ahead Progress and Challenges

PTSD Looking Back & Looking Ahead: Progress and Challenges Matthew J. Friedman, MD, Ph. D. Executive Director National Center for PTSD

Validity of PTSD is Well-Established Ø PTSD has proven to be a very useful and valid diagnosis after 25 years of clinical use Ø Although there have been minor revisions to the diagnostic criteria the core concept has withstood the test of time

The PTSD Concept Ø Inability to cope with overwhelming stress may be followed by a distinctive pattern of symptoms Ø It does not presume that this is the only possible psychiatric outcome

Research Supports the PTSD Concept Ø PTSD and PTSD symptoms rank among the most common new onset posttraumatic clinical problems Ø Before DSM-III, there was no way to identify people so affected

The PTSD Hypothesis Made it Possible to: Ø Predict how affected people react to traumatic reminders Ø Differentiate them from non-affected people or those with depression or other anxiety disorders Ø Develop unique therapeutic approaches (e. g. CBT & medication) that could not have been envisioned without the PTSD model

PTSD is a Disorder of Reactivity Ø Its alterations are best revealed by responses to psychological or pharmacological probes Ø In contrast, depression is a shift in basal state, alterations are best revealed by measurement of tonic activity

PTSD has a Wealth of Animal Models Unequaled in Psychiatry Ø Traumatic stress can be operationalized as uncontrollable or unpredictable stress Ø Laboratory-induced physiological and neurohormonal alterations resemble those seen in PTSD Ø Brain systems affected by uncontrollable stress and fear conditioning resemble those affected in PTSD

PTSD has Provided a New and Powerful Tool for Translational Research Ø Translation of important clinical observations into rigorous experimental protocols Ø Translation of laboratory findings into testable clinical approaches

Is PTSD the Only Post. Traumatic Outcome? No Prospective studies show that people may develop new-onset depression, other anxiety disorders, alcoholism or behavioral alterations without PTSD But that is not what we are here to discuss today

Prevalence of PTSD in the General Population Ø Large national probability sample of US adults (Ns > 5000) l l l Ø National Comorbidity Survey (1995) National Comorbidity Survey-Replication (2005) Benchmark for prevalence of mental disorders in US Lifetime PTSD prevalence 6. 8% (NCS-R) l l 10% women (NCS) 5% men (NCS)

Combat Exposure in the NCS Ø Any combat veteran’s lifetime PTSD prevalence = 39% Ø Male combat > all other male trauma l l Lifetime PTSD prevalence Delayed onset Unresolved symptoms Functional impairment (unemployment, being fired, divorce or separation, spousal abuse)

Changes in the PTSD Diagnostic Criteria Ø Symptom clusters: l Symptoms expanded from DSM-III to III-R and IV Ø Added duration and distress/impairment Ø Revised stressor criterion

Biological Profile Ø The diagnosis has distinguished people with a unique set of biological abnormalities. Ø These include: l l psychophysiological reactivity neurohormonal profiles EKG abnormalities structural and functional brain imaging alternations

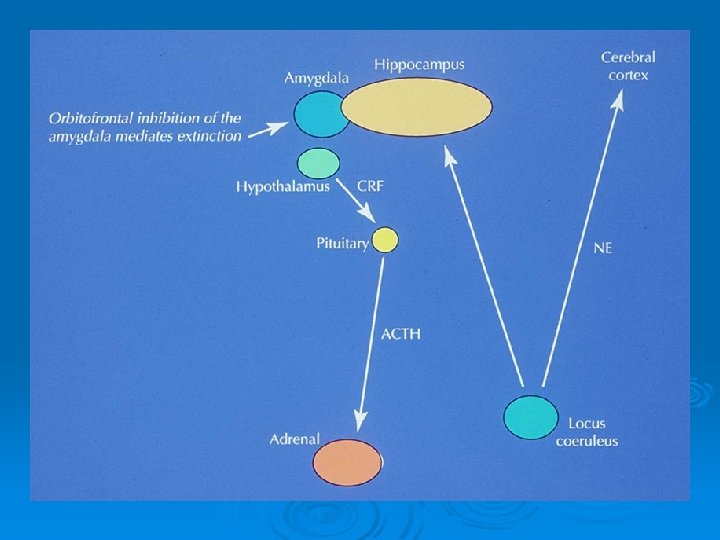
The Stress System The stress system coordinates the generalized stress response which takes place when a stressor of any kind exceeds a threshold The main components are: • HPA system • LC/NE system • Immunological system

Are there structural brain abnormalities associated with PTSD?

Left Right combat childhood abuse combat abused children MVA ? ? trauma combat (% DIFFERENCE BETWEEN PTS AND Controls) abuse + MDD Hippocampal Volume in PTSD Vythilingam 2001 (unpublished)

Are there functional brain abnormalities associated with PTSD?
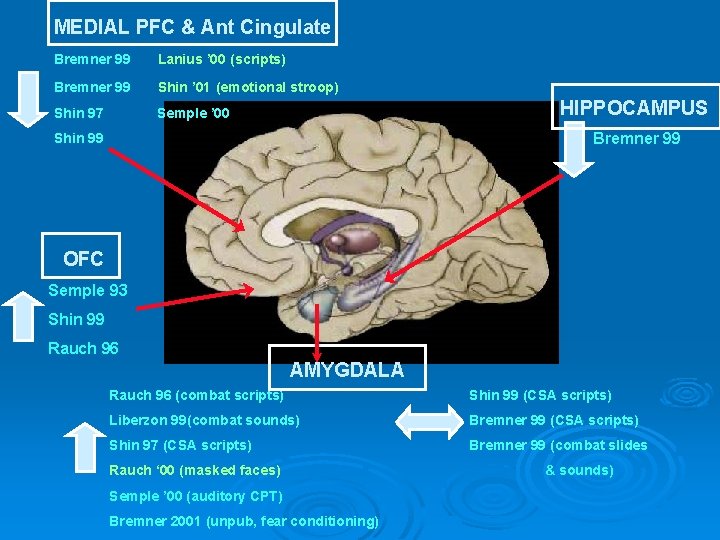
MEDIAL PFC & Ant Cingulate Bremner 99 Lanius ’ 00 (scripts) Bremner 99 Shin ’ 01 (emotional stroop) Shin 97 Semple ’ 00 HIPPOCAMPUS Bremner 99 Shin 99 OFC Semple 93 Shin 99 Rauch 96 AMYGDALA Rauch 96 (combat scripts) Shin 99 (CSA scripts) Liberzon 99(combat sounds) Bremner 99 (CSA scripts) Shin 97 (CSA scripts) Bremner 99 (combat slides Rauch ‘ 00 (masked faces) Semple ’ 00 (auditory CPT) Bremner 2001 (unpub, fear conditioning) & sounds)
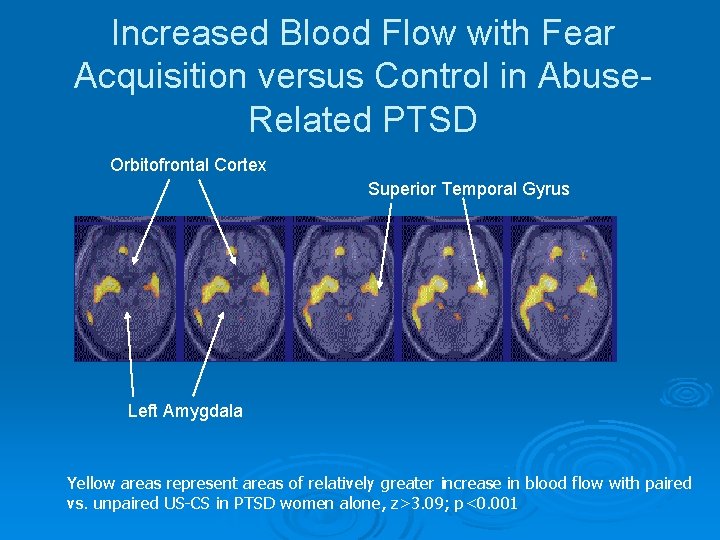
Increased Blood Flow with Fear Acquisition versus Control in Abuse. Related PTSD Orbitofrontal Cortex Superior Temporal Gyrus Left Amygdala Yellow areas represent areas of relatively greater increase in blood flow with paired vs. unpaired US-CS in PTSD women alone, z>3. 09; p<0. 001

Decreased Blood Flow During Recall Of Emotionally Valenced Words In Abuse-Related PTSD Retrieval of Word pairs like “blood-stench” Left hippocampus Medial prefrontal & Orbitofrontal Cortex Fusiform, inferior temporal gyrus

Psychological and Biological Mechanisms We know that: Øa number of psychological mechanisms such as negative cognitions, threat appraisal, coping behaviors, information/memory processing and cognitive strategies predict PTSD; Ø animal models of fear conditioning and neurobiological models concerning the human stress response provide a useful context for understanding acute distress and PTSD; and Ø exposure to stress during crucial developmental periods may produce stable abnormalities in stress response systems.

PTSD Treatment Options Psychosocial Pharmacological Exposure Therapy Cognitive Therapy Anxiety Management Desensitization Hypnotherapy TCAs MAOIs SSRIs Mood Stabilizers Anti-anxiety Agents

Sertraline Flexible-Dose PTSD Study Weeks 0 1 2 3 4 6 8 10 12 0 Adjusted Mean Change in CAPS-2 Total Score -10 -20 -30 * -40 Placebo (N=90) * p <. 001 at week 12 Mean dose for completers = 151. 3 mg Brady K et al. JAMA. 2000; 283: 1837 -1844. Sertraline (N=93)
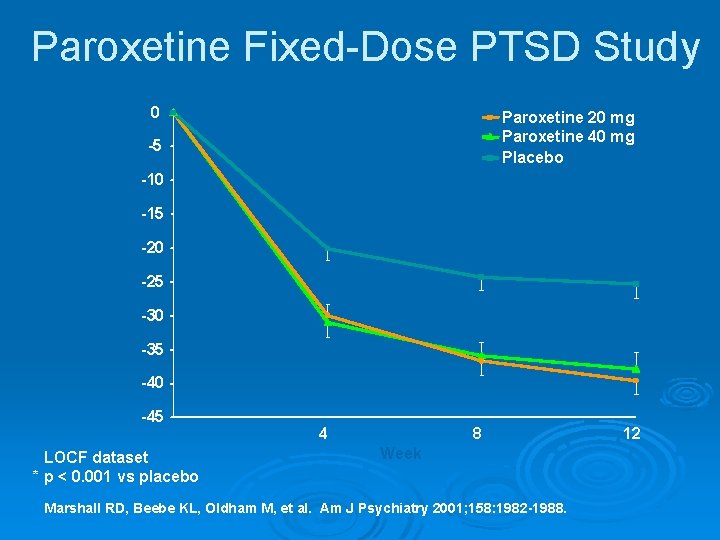
Paroxetine Fixed-Dose PTSD Study 0 Paroxetine 20 mg Paroxetine 40 mg Placebo -5 -10 -15 Adjusted -20 Mean Change in -25 CAPS-2 -30 Total Score * * -35 * * -40 -45 LOCF dataset * p < 0. 001 vs placebo 4 8 Week Marshall RD, Beebe KL, Oldham M, et al. Am J Psychiatry 2001; 158: 1982 -1988. * * 12
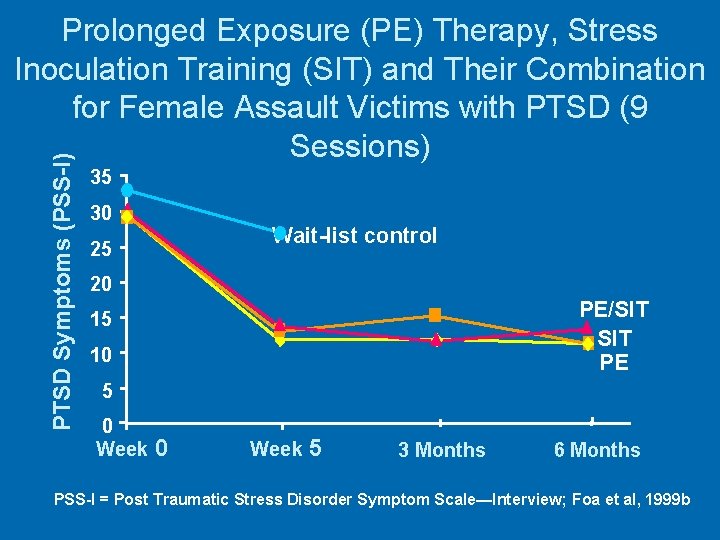
PTSD Symptoms (PSS-I) Prolonged Exposure (PE) Therapy, Stress Inoculation Training (SIT) and Their Combination for Female Assault Victims with PTSD (9 Sessions) 35 30 Wait-list control 25 20 PE/SIT PE 15 10 5 0 Week 5 3 Months 6 Months PSS-I = Post Traumatic Stress Disorder Symptom Scale—Interview; Foa et al, 1999 b



Controversy #1 PTSD is not a Legitimate Diagnosis Ø Battle still wages after 25 years l l Ø Being fought in the media as well as scientific journals Institute of Medicine hearings in U. S. PTSD’s dubious parentage l Emerged from converging social (feminist, veteran) movements rather than traditional scientific and clinical sources

Controversy #1 (continued) Legitimacy of PTSD diagnosis Ø Criticism & negative reception has spurred an outpouring of rigorous research l Clinical phenomenology, cognition, brain imaging, personal dynamics Ø Factor analysis of PTSD symptom clusters has generally validated construct Ø People with PTSD exhibit significant differences from non-affected individuals

Controversy #2 PTSD Needlessly Pathologizes Normal Reactions to Abusive Violence This argument fails to acknowledge that some people cope successfully with traumatic events and manifest normal distress while others exhibit clinically significant symptoms The purpose of any diagnosis is to inform treatment decisions - not to “pathologize”

Controversy #3 PTSD is a Euro-American Culture-Bound Syndrome PTSD has been documented throughout the world 1, 2 Ø Comparable PTSD prevalence in Nairobi embassy and Oklahoma City bombings 3 Ø l l Ø Men: 26% Nairobi, 20% Oklahoma City Women: 35% Nairobi, 34% Oklahoma City Although there may be culture-specific idioms of distress, PTSD appears to encompass a pattern of universal post-traumatic distress 1 de Jong et al. , 2001; 2 Green et al. , 2004; 3 North et al. , 2005

Controversy #4 PTSD primarily serves a litigious rather than a clinical purpose Stressor Causality Liability Ø Geometric rise in PTSD-related civil litigation and disability claims Ø l Ø Great concern about amount of money at stake Big difference between challenging validity of PTSD as a clinical diagnosis and questioning the quality of forensic or disability evaluations

Controversy #5 Traumatic Memories are not Valid When external verification possible - most memories are accurate Ø Recovered Memory Controversy spurred much useful research Ø l l l Accurate memories may be lost and later recovered Some traumatic memories are not accurate The veracity of any specific recovered memory must be judged on a case-by-case basis

Controversy #6 Verbal Reports are Unreliable Ø Excellent structured interviews and assessment tools have been developed Ø Reliability of retrospective self-report data among 260 Vietnam theater veterans was recently confirmed by archival records and other external sources (Dohrenwend et al. , 2006)

Looking Ahead #1 Is PTSD a “Stress-Related Fear Circuitry Disorder? ” Ø Joint APA/WHO initiative being considered for DSM-V/ICD-11 Ø Based on common neurocircuitry, cognitive alterations and neurohormonal changes Ø Would cluster PTSD with panic disorder, simple phobia and social phobia
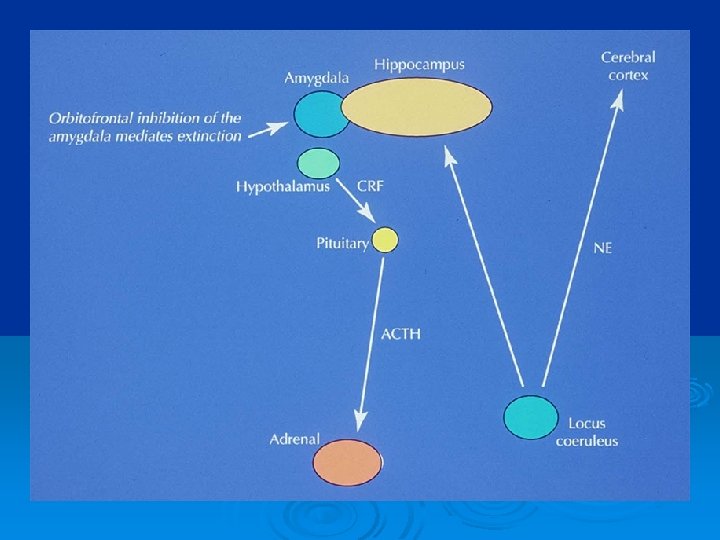

Is PTSD a Fear Circuitry Disorder? Neurocircuitry: Disruption of restraining influence of medial prefrontal cortex (especially ACC) Chain reaction brought about from activation of amygdala by fear stimuli 1 1 Vermetten Charney 2004) & Bremner, 2002;

Is PTSD a Fear Circuitry Disorder? Ø Cognitive / Behavioral: PTSD as a model from Pavlovian Conditioning (Kolb, 1989), and Activated Fear Networks (Lang, 1977; Foa & Kozak, 1986).

Potential Non-Verbal Diagnostic Implications of Stress Related Fear Circuitry Model l l Stimulus-driven paradigms: Auditory / Visual / Narratives: CV / Electrodermal / Electromyographic/ Brain Imaging (Orr et al. , 2004 / Kaufman et al. , 2004) CSFP (Geracioti et al 2006) Pharmacological probes: Super suppression on DST: (Yehuda et al. , 1997) Yohimbine (Southwick 1993; Bremner 1997)

Looking Ahead #1 (continued) Is PTSD a “Stress-Related Fear Circuitry Disorder? ” Ø Other emotions besides fear also often present l Sadness, grief, anger, shame & disgust May not be a nosological problem since the goal is to cluster diagnoses according to a common denominator Ø Would be a conceptual problem since clinical problems often extend beyond fear-based appraisals and reactions Ø l Shame, anger, substance abuse, aggression, horror, helplessness without personal fear (e. g. medical personnel, graves registration, etc. )

Looking Ahead #2 (continued) Should PTSD be Considered a Dimensional Rather Than a Categorical Disorder? Ø Subsyndromal/partial PTSD Ø Chronic non-traumatic stress syndromes Ø Chronic stress-related medical disorders

Subsyndromal/Partial PTSD Affective Disorders: DSM I, III (III-R) and IV DSM-I BAD/Manic-Depression MDD/Psychotic Depression Dysthmia/Depressive Neurosis Cycolthymia/Affective Personality Involuntary Meloncholia (Other) Mood Disorder NOS Atypical Bipolar/NOS Atypical Depressive/NOS Adj Disorder - Depressed Adj Disorder - Mixed Anx/Dep X X DSM-III/ III-R X X X X X X DSM-IV

PSSD - Post-Severe Stress Disorder “Severe” vs. “Traumatic” Stress Are there enduring psychiatric syndromes caused by acute or chronic non-traumatic but severe stress? Divorce, failure, bankruptcy, illness, bereavement Does PSSD differ from PTSD?

Chronic Stress Syndrome Ø PSSD has medical consequences Ø PTSD also has medical consequences Both affect HPA, cardiovascular, immunological, and other systems Should “medical” illnesses precipitated by stress be included with PSSD/PTSD as “stress disorders? ” • Chronic Fatigue Syndrome • Fibromyalgia • Peripheral Vascular Disease • Endocrinopathies • etc

Looking Ahead #3 New Directions for Psychosocial Treatment Ø Despite success of CBT (PE, CT, CPT and EMDR) there is evidence for the efficacy of treatments that do not focus on traumatic material Ø SIT - focuses on symptom management rather than trauma processing Ø Present centered therapies have also been effective Ø SIT and PCT do better in recruitment and retention

Looking Ahead #3 (continued) New Directions for Psychosocial Treatment Ø Need predictors of treatment outcome Ø Case matching - some may be better candidates for trauma processing and others for present-centered approaches or medication

Looking Ahead #3 (continued) New Directions for Psychosocial Treatment Ø EMDR - How does it work? l l Is it CBT in disguise? Does it work through a unique mechanism? Ø Using brain imaging techniques might be a way to approach this issue

Looking Ahead #3 (continued) New Directions for Psychosocial Treatment Ø Third Wave Influenced by Eastern & “mindfulness” approaches that emphasize acceptance l Ø Comorbidity l l Ø Little evidence of efficacy so far Substance abuse (Seeking Safety) Traumatic brain injury Technology l Web based, virtual reality, telehealth

Looking Ahead #4 New Directions for Biological Research Ø Need to expand focus beyond serotonin and norepinephrine l CRF, NPY, GABA, glutamate, dopamine, etc. Ø Is PTSD a final common pathway (like fever or edema) that can be caused by different patterns of psychobiological alterations? Ø Genetic research on resilience and vulnerability

Looking Ahead #5 New Directions for Pharmacotherapy Ø Current medications in use were all initially designed to treat other disorders (antidepressants, antihypertensives, anticonvulsants, antipsychotics, etc. )

Looking Ahead #5 (continued) New Directions for Pharmacotherapy Ø The need is for new medications that preferentially target abnormal psychobiological mechanisms associated with PTSD. l l Medications to interrupt the cascade of stress-related alteratitons (e. g. CRF antagonists, NPY enhancers) Medications to blunt fear conditioning (antiadrenergics, NMDA antagonists) Medications to promote extinction of fear-conditioned reactions (e. g. cycloserine) Medications to target dissociative symptoms (e. g. anticonvulstants such as lamotrigene)

Looking Ahead #5 (continued) New Directions for Pharmacotherapy Ø Combined treatment with CBT l Need augmentation strategies for partial responders Ø Augmentation treatments with different medications Ø Effective and safe approaches for children

Looking Ahead #6 Using Neuroimaging to Understand Therapeutic Mechanisms of Action Ø Does CBT work “top-down” - (pre-frontal) cortical restraint of amygdala Ø Do medications work “bottom-up” - major targets are subcortical Ø Do different psychosocial approaches work in different ways? l CBT vs. SIT or EMDR

Looking Ahead #7 Major Challenges Regarding Memory and Dissociation: Might They Inform Forensic Practice? Studies of traumatic memory will need to be much more rigorous and inventive if they are to reflect the complexity of the processes that have already been demonstrated to occur. Neuroimaging methods will also assist in this understanding.

Looking Ahead #7 (continued) Major Challenges Regarding Memory and Dissociation: Might They Inform Forensic Practice? Ø Should draw more explicitly on concepts developed by cognitive and experimental psychologists Ø Should utilize neuroimaging methods Ø Should distinguish between processing any traumaspecific information from processing information encoded in an emotional context Ø Should be designed to distinguish between ordinary autobiographical memories of trauma and involuntary flashbacks (which have a different neural basis) Brewin, in press

Looking Ahead #8 Developmental Challenges: Children/Adolescents & the Elderly Ø An approach that encompasses the dynamic relationship between experience, neurological processing, and brain development, is necessary for understanding the problems of children who have experienced traumatic events Ø Such an approach must also address selfregulation from a developmental perspective since it has been noted to be a central problem for children with traumatic stress Saxe et al. , in press

Looking Ahead #8 (continued) Developmental Challenges: Children/Adolescents & the Elderly Are the psychological and biological effects of the same trauma (e. g. sexual, accident): • • • different in children than adults different in adults traumatized as children different in adults traumatized as adults

Looking Ahead #8 (continued) Developmental Challenges: Children/Adolescents & the Elderly Unfortunately knowledge in the geriatric field is far from complete. More information is needed regarding the prevalence, symptom expression and course of trauma-related symptoms, particularly age-specific psychosocial and behavioral responses, mediators and moderators of negative and positive consequences, and assessment techniques. Many questions regarding treatment and delivery remain unexamined or only partially answered. Cook & Niederehe, in press
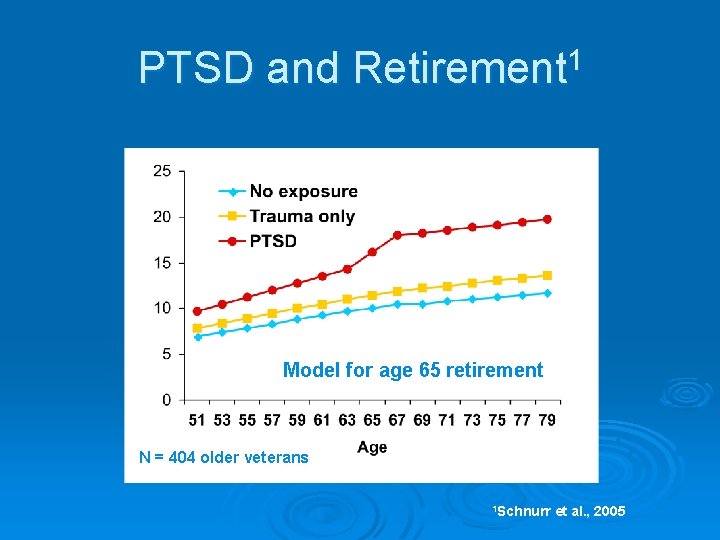
PTSD and Retirement 1 Model for age 65 retirement N = 404 older veterans 1 Schnurr et al. , 2005

Looking Ahead #9 Challenges Regarding Gender The development of testable conceptual models and hypotheses regarding the impact of gender on vulnerability and treatment outcomes in PTSD are sorely needed, as are efficacy trials that can formally assess the potential role of gender as a moderator of treatment efficacy. Kimerling et al, in press

Looking Ahead #10 Cross-Cultural Challenges It is time for the fields of anthropology and mental health to end the debate about the validity of the PTSD diagnosis. A culturally competent model of traumatic stress should address how culture is implicated in the process of appraisal of vulnerable or protective factors. Critical to this field is learning the language-the idioms of distress-that cultural groups use as acceptable means of communicating distress. Equally important is understanding the explanatory models, the attribution of illness and the culturally sanctioned local healing methods. de Jong & Osterman, in press

Looking Ahead #10 (continued) Cross-Cultural Challenges PTSD has been documented throughout the world 1, 2 Ø Comparable PTSD prevalence in Nairobi embassy and Oklahoma City bombings 3 l Men: 26% Nairobi, 20% Oklahoma City l Women: 35% Nairobi, 34% Oklahoma City Ø Although there may be culture-specific idioms of distress, PTSD appears to encompass a pattern of universal post-traumatic distress Ø 1 al. , 2005 de Jong et al. , 2001; 2 Green et al. , 2004; 3 North et
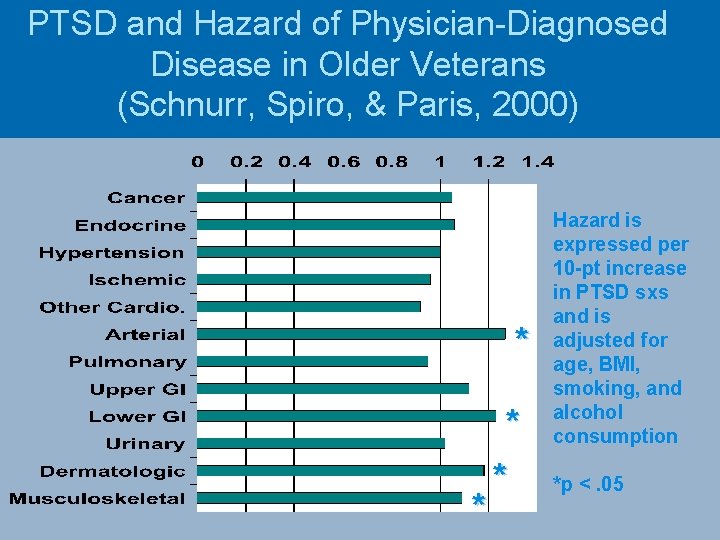

PTSD and Hazard of Physician-Diagnosed Disease in Older Veterans (Schnurr, Spiro, & Paris, 2000) * * Hazard is expressed per 10 -pt increase in PTSD sxs and is adjusted for age, BMI, smoking, and alcohol consumption *p <. 05
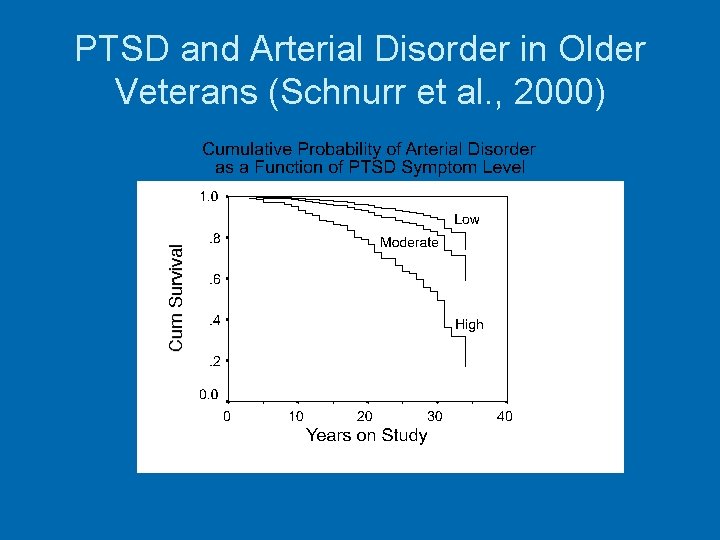
PTSD and Arterial Disorder in Older Veterans (Schnurr et al. , 2000)

Odds of Cardiovascular Problems in Vietnam Veterans with PTSD (Boscarino & Chang, 1999) N = 4, 462 Adjusted for demographic, military, and health risk covariates. *p <. 05.

Looking Ahead #12 Resilience & Prevention Ø Most people exposed to traumatic stress do not develop PTSD Ø It is important to understand resilience in order to promote it in the general population and to use such knowledge to inform the development of new treatments

Gene x Environment-1
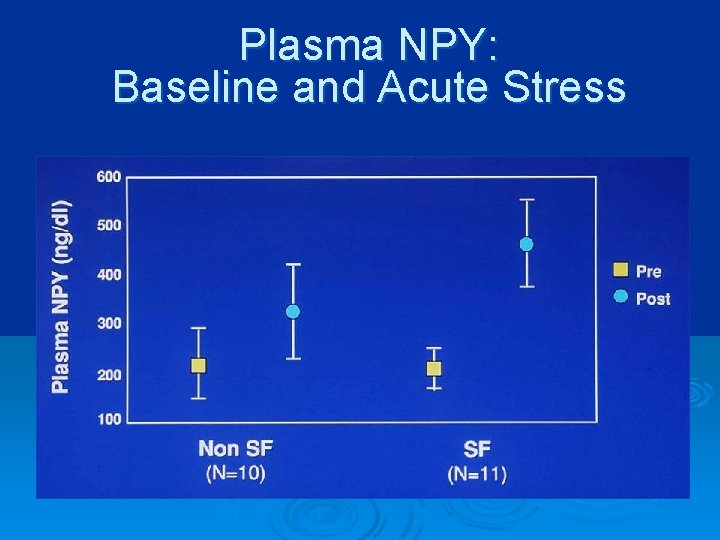
Plasma NPY: Baseline and Acute Stress

Looking Ahead #12 (continued) Resilience & Prevention It is likely that stress-related risk and resilience factors have multiple determinants such as genetic makeup, developmental history, personality, coping style, social support, and history of exposure to traumatic events Southwick et al. , in press

Looking Ahead #12 (continued) Resilience & Prevention A “wellness-oriented” preventive public health approach: Prepare the population-at-large with the expectation of recovery but with the goal of accelerating recovery 1. • 2. psychoeducation, public mental health strategies, foster resilience Identity populations at risk and build capacity for early detection and intervention for those manifesting severe distress or psychiatric symptoms
- Slides: 71