PTSD and Substance Use Disorders Brian E Lozano

PTSD and Substance Use Disorders Brian E. Lozano, Ph. D. Contributing Collaborator: Sudie E. Back, Ph. D. Medical University of South Carolina Ralph H. Johnson VA Medical Center Lozano@musc. edu Backs@musc. edu

Thank you Colleagues Dr. Kathleen Brady Dr. Therese Killeen Dr. Edna Foa Dr. Colleen Hanlon Dr. Stacia De. Santis Dr. Karen Hartwell Dr. Liz Santa Ana Dr. Brian Lozano Dr. Matt Yoder Dr. Kristy Center Dr. Julianne Flanagan Dr. Jenna Mc. Cauley Ms. Sharon Becker Dr. Megan Moran-Santa Maria Dr. Peter Kalivas Dr. Jacqueline Mc. Ginty Funding Sources NIDA F 31 DA 00607 (Back) NIDA K 23 DA 021228 (Back) NIDA R 01 DA 030143 (Back) J. William Fulbright (Back) NIDA K 24 DA 00435 (Brady) NIH UL 1 RR 029882 (Brady) NIDA T 32 DA 07288 (Mc. Ginty) Do. D 803235 (Kalivas & Back) Do. D 804237 (Mc. Ginty & Back) Staff/Coordinators Mr. Frank Beylotte Ms. Mary Ashley Mercer Ms. Emily Hartwell Dr. Elizabeth Cox Ms. Wendy Muzzy Ms. Alex Jeffery Ms. Virginia Mc. Alister Mr. Scott Henderson Ms. Amanda Federline Ms. Anjinetta Johnson Mr. Drew Teer

Disclosure Statement �No conflicts of interest to disclose �Previous and current research funding from: ◦ National Institute on Drug Abuse ◦ Department of Defense ◦ J. William Fulbright Foreign Scholarship Board

Treatment Models ØSequential Model – SUD first, then PTSD ØSingular Model – Treat the “primary” disorder o Treat only the SUD o Treat only the PTSD ØParallel Model – SUD and PTSD, different clinicians ØIntegrated Model - SUD and PTSD, same clinician
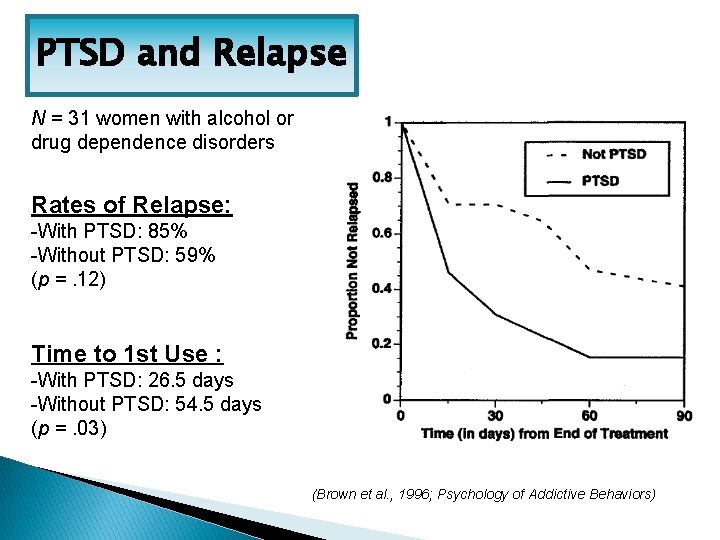
PTSD and Relapse N = 31 women with alcohol or drug dependence disorders Rates of Relapse: -With PTSD: 85% -Without PTSD: 59% (p =. 12) Time to 1 st Use : -With PTSD: 26. 5 days -Without PTSD: 54. 5 days (p =. 03) (Brown et al. , 1996; Psychology of Addictive Behaviors)

The Need to Treat Both PTSD and SUD Untreated PTSD contributes to poorer treatment outcome for substance use, and vice versa. Traditionally, the standard of care = sequential model: (1) SUD treatment first, demonstrate sustained abstinence (3 to 6 months) then… (2) PTSD treatment Clinic #1 Clinic #2

Integrated Model of PTSD/SUD Treatment • Both conditions concurrently, by the same clinician Clinic #1

Integrated Model of PTSD/SUD Treatment • • Both conditions concurrently, by the same clinician Clinic #1 Driven by: o -Hypothesis that substance abuse is result of, in part, PTSD symptoms. o -Reductions in PTSD are more likely to lead to reductions in substance abuse, than the reverse. o -Patient preferences.
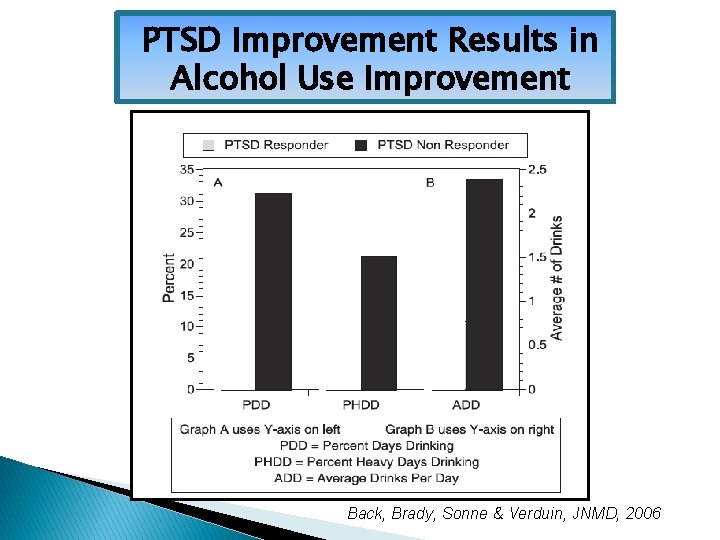
PTSD Improvement Results in Alcohol Use Improvement (N=94) Back, Brady, Sonne & Verduin, JNMD, 2006
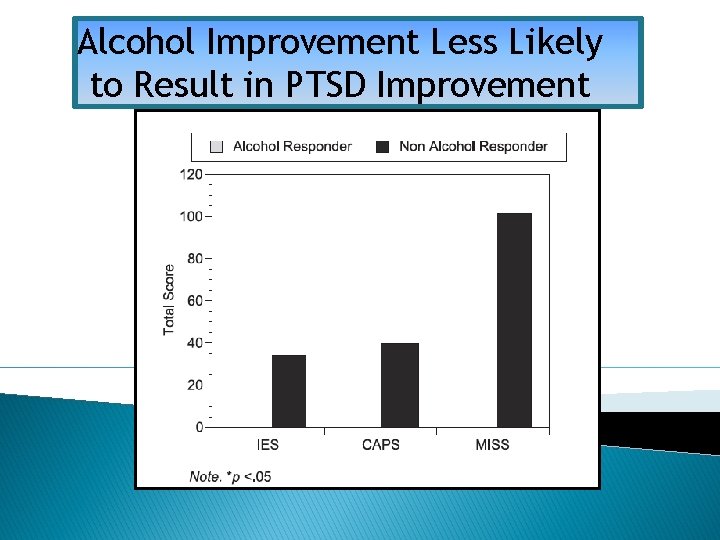
Alcohol Improvement Less Likely to Result in PTSD Improvement
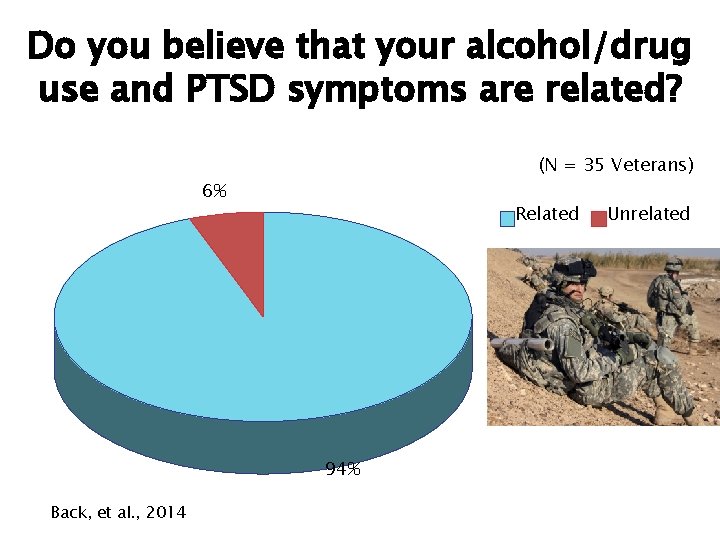
Do you believe that your alcohol/drug use and PTSD symptoms are related? (N = 35 Veterans) 6% Related 94% Back, et al. , 2014 Unrelated
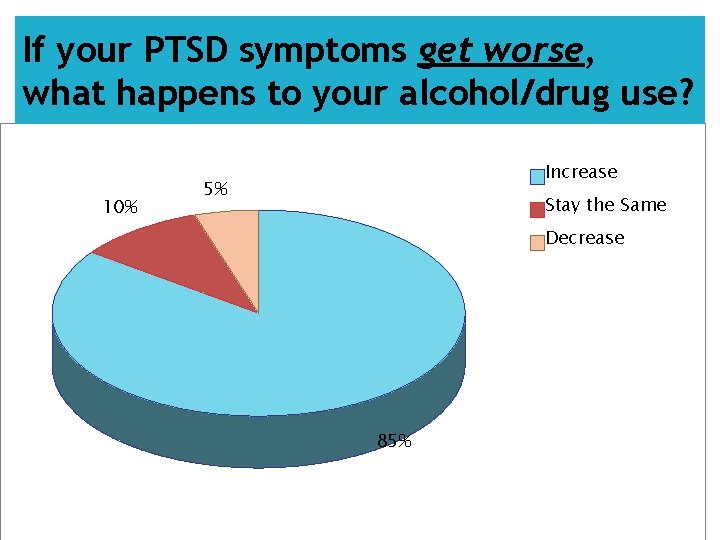
If your PTSD symptoms get worse, what happens to your alcohol/drug use? 10% Increase 5% Stay the Same Decrease 85%
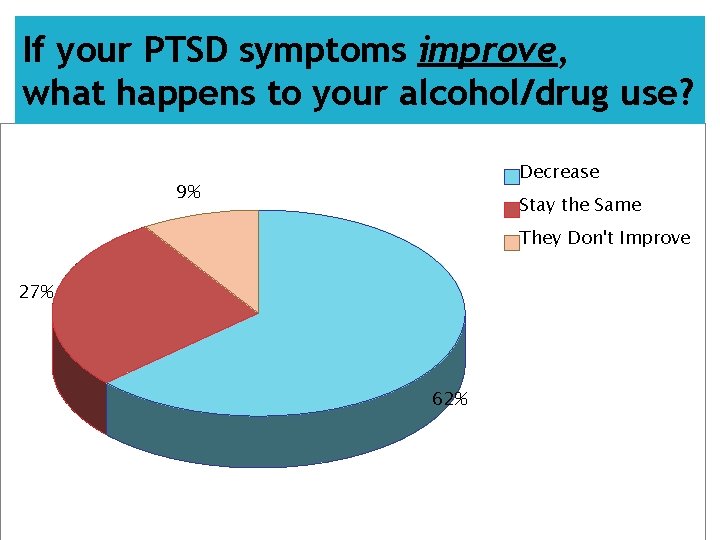
If your PTSD symptoms improve, what happens to your alcohol/drug use? Decrease 9% Stay the Same They Don't Improve 27% 62%
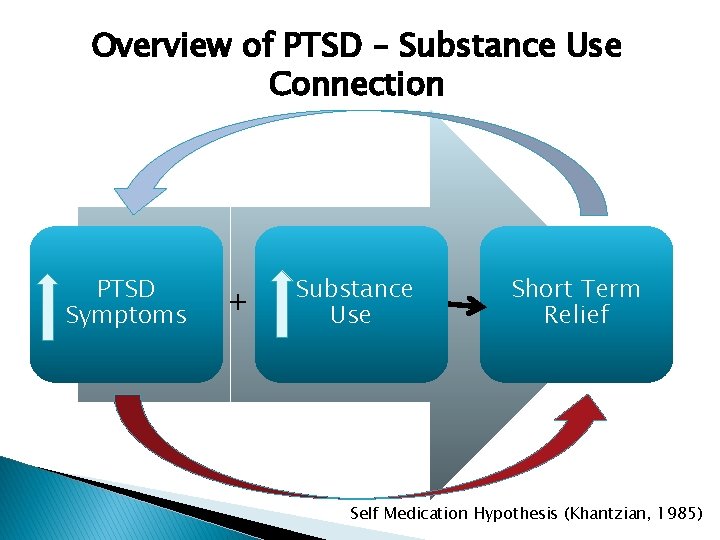
Overview of PTSD – Substance Use Connection PTSD Symptoms + Substance Use Short Term Relief Self Medication Hypothesis (Khantzian, 1985)
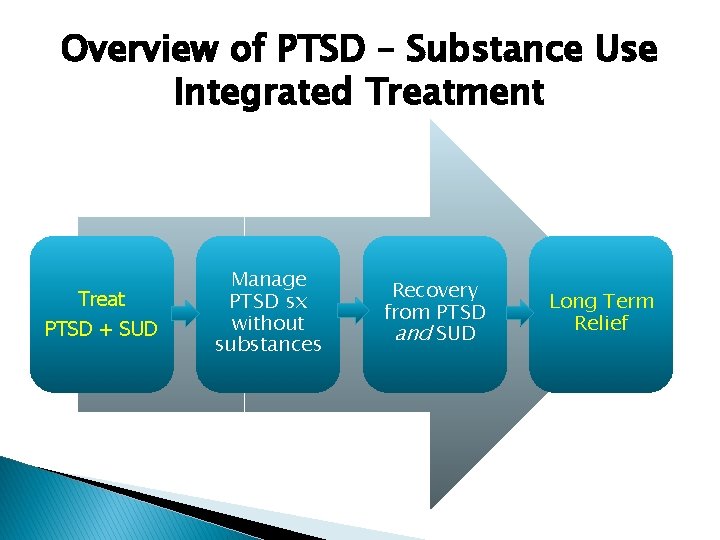
Overview of PTSD – Substance Use Integrated Treatment Treat PTSD + SUD Manage PTSD sx without substances Recovery from PTSD and SUD Long Term Relief

SUD-PTSD Integrated Psychotherapies Najavits (2002) - Seeking Safety. Relapse prevention + education + social skills training. Mostly group. 25 sessions. Back, Foa, Killeen, Brady et al. (in press) – COPE. Relapse prevention + in vivo exposure + imaginal exposure. Individual. 12 sessions.
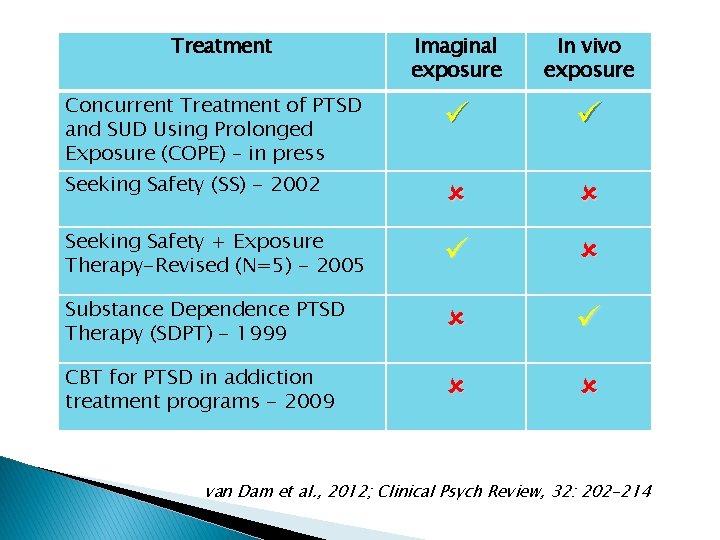
Treatment Imaginal exposure In vivo exposure Concurrent Treatment of PTSD and SUD Using Prolonged Exposure (COPE) – in press Seeking Safety (SS) - 2002 Seeking Safety + Exposure Therapy-Revised (N=5) - 2005 Substance Dependence PTSD Therapy (SDPT) - 1999 CBT for PTSD in addiction treatment programs - 2009 van Dam et al. , 2012; Clinical Psych Review, 32: 202 -214

COPE (Concurrent Treatment of PTSD & SUD using Prolonged Exposure) Synthesis of 2 theory-based and empirically-validated treatments: (1) Prolonged Exposure for PTSD (Foa, Hembree, & Rothbaum, 2007) (2) Relapse Prevention for SUD (Carroll, 1998)

Primary Goals of COPE 1. Educate patients about the functional relationship between substance use and PTSD. 2. Decrease SUD symptom severity, initiate and maintain abstinence. 3. Decrease PTSD symptom severity.

CBT Techniques Used To Treat PTSD Ø Psychoeducation – education about common reactions, normalize symptoms, help understand avoidance & how it maintains PTSD symptoms. Ø Breathing Retraining technique to decrease anxiety. Ø Prolonged Exposure (PE): o In-Vivo Exposure o Imaginal Exposure

In Vivo Exercises ▶ In between therapy sessions ▶ Repeated exposures ▶ Prolonged duration ▶ Common examples: o o o o Walmart (or other crowed store) Sitting in middle of restaurant Going to a sporting event Going to movie theatre Driving during rush hour Being stopped at a stop light Watching or reading the news Group activities (going to AA, church, exercise class)

Imaginal Exposure
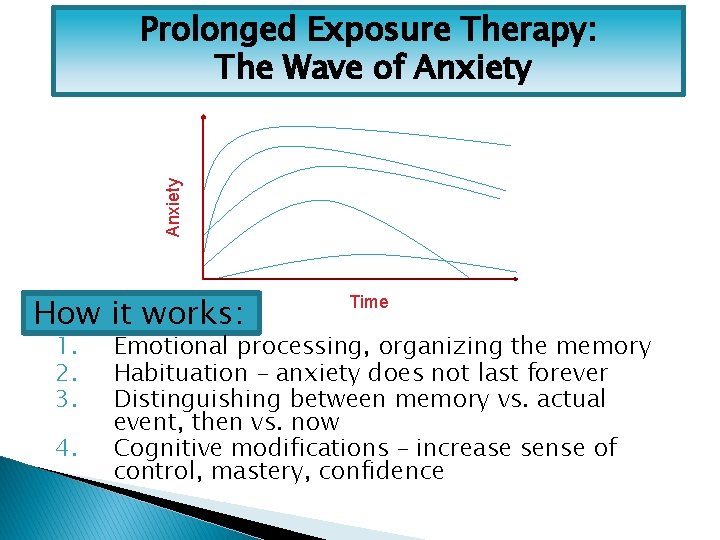
Anxiety Prolonged Exposure Therapy: The Wave of Anxiety How it works: 1. 2. 3. 4. Time Emotional processing, organizing the memory Habituation – anxiety does not last forever Distinguishing between memory vs. actual event, then vs. now Cognitive modifications – increase sense of control, mastery, confidence

Empirical Support for PE Foa et al. (1991) Foa et al. (1999) Foa et al. (2005) Marks et al. (1998) Tarrier et al. (1999) Taylor et al. (2001) Cloitre et al. (2002) Resick et al. (2003) Bryant et al. (2003) Schnurr et al. (2007) Rauch et al. (2009) Resick et al. (2012) *18% with PTSD 5 -10 yrs later

CBT to decrease SUD Symptoms Ø Psychoeducation regarding relationship between substance use and PTSD sx. Ø Effectively manage cravings and thoughts about substance use. Ø Identify triggers for substance use - both PTSD and substance-related triggers. Ø Learn coping skills to help prevent relapse/escalation to substances (e. g. , managing anger, drug refusal skills).

Summary Ø Integrated treatments address both the PTSD and the SUD concurrently. Ø COPE uses Prolonged Exposure (in vivo and imaginal) to treat PTSD, and CBT (Relapse Prevention) to treat SUD. Ø Main Goals: ◦ Psychoeducation ◦ Reduce PTSD symptoms ◦ Reduce SUD symptoms

COPE Session Content

General Session Overview Session # Session Topic 1 Introduction: Psychoeducation, Set Goals, Therapy Contract, Breathing Retraining 2 PTSD: Common Reactions to Trauma SUD: Awareness of Cravings PTSD: In Vivo Hierarchy SUD: Managing Cravings 3 4 PTSD: First Imaginal Exposure SUD: Review coping skills
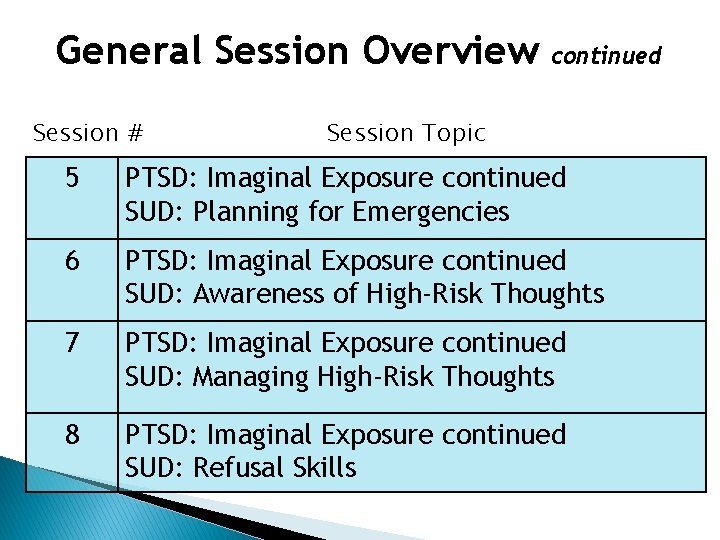

General Session Overview Session # continued Session Topic 5 PTSD: Imaginal Exposure continued SUD: Planning for Emergencies 6 PTSD: Imaginal Exposure continued SUD: Awareness of High-Risk Thoughts 7 PTSD: Imaginal Exposure continued SUD: Managing High-Risk Thoughts 8 PTSD: Imaginal Exposure continued SUD: Refusal Skills

General Session Overview Session # continued Session Topic 9 PTSD: Imaginal Exposure continued SUD: Seemingly Irrelevant Decisions 10 PTSD: Imaginal Exposure continued SUD: Awareness of Anger 11 PTSD: Final Imaginal Exposure SUD: Managing Anger 12 Review and Termination


COPE Studies to Date Ø Brady et al. (2001) and Back et al. (2001): PTSD and cocaine; N=39 Ø Mills et al. (2012): PTSD and mostly heroin; N=103; COPE + TAU vs TAU Ø Back et al. (ongoing): military PTSD and mostly alcohol; COPE vs RP Ø Hien et al. (ongoing): PTSD and mostly alcohol; COPE vs RP Ø Norman et al. (ongoing): military PTSD; COPE vs Seeking Safety

Initial COPE Study Ø Preliminary, Ø N=39 Ø PTSD uncontrolled study and cocaine dependence Ø 16 individual 90 -minute sessions Ø Assessment at weeks 4, 8, 12, and 16, and at 6 months follow up.

Initial COPE Findings (N=39) Cocaine Dependent + PTSD Positive Urine Drug Screen (UDS) Tests § At treatment entry = 12. 8% § First half of treatment = 12. 2% § Second half of treatment = 9. 7% Timing of Attrition The majority (75%) dropped out before PE initiated (e. g. , transportation or employment problems, relocation, scheduling conflicts, unstable living conditions) Brady, Dansky, Back, Foa & Carroll, 2001
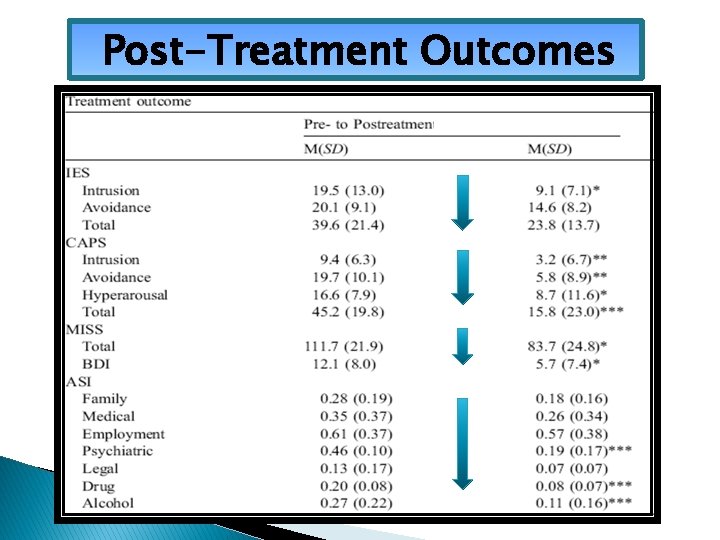
Post-Treatment Outcomes
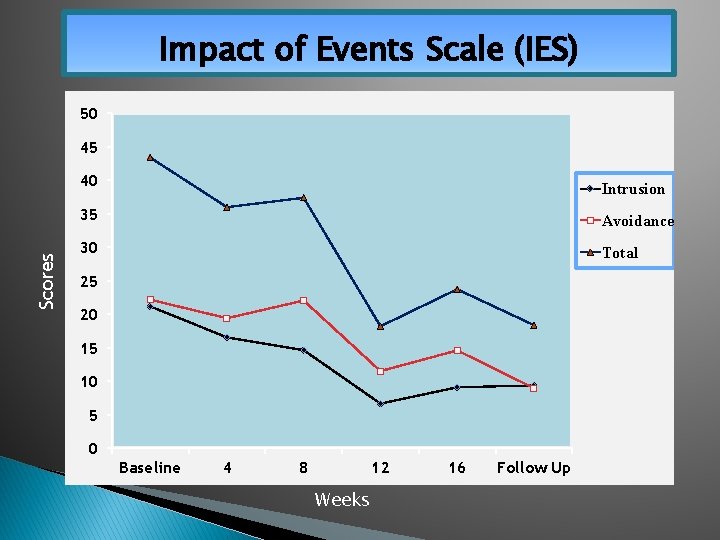
Impact of Events Scale (IES) 50 45 Scores 40 Intrusion 35 Avoidance 30 Total 25 20 15 10 5 0 Baseline 4 8 12 Weeks 16 Follow Up

Considerations Ø Uncontrolled study Ø Small sample size Ø Focused on cocaine dependence Ø High drop-out rate

Study Aims and Design Ø Ø Ø Ø Randomized controlled trial COPE + TAU vs TAU N=103 SUD (mostly heroin) + PTSD Majority (75%) had childhood trauma 62. 1% women 78. 6% unemployed 54. 2% lifetime history of suicide attempt Mills et al. , 2012
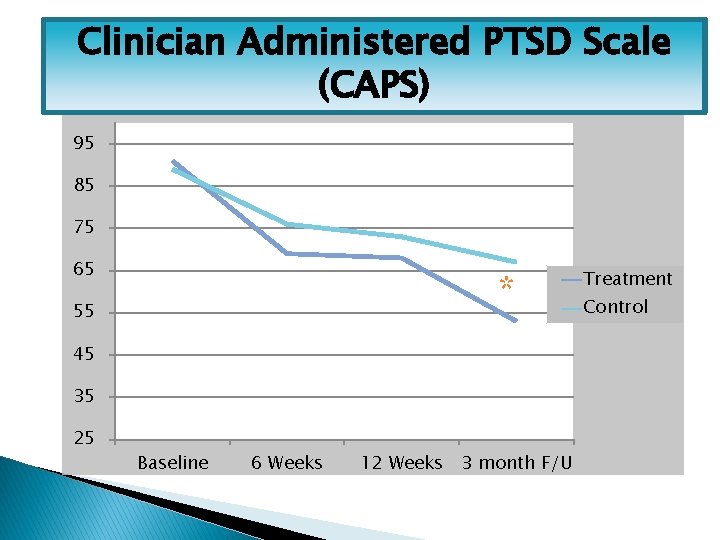
Clinician Administered PTSD Scale (CAPS) 95 85 75 65 * 55 45 35 25 Baseline 6 Weeks 12 Weeks 3 month F/U Treatment Control
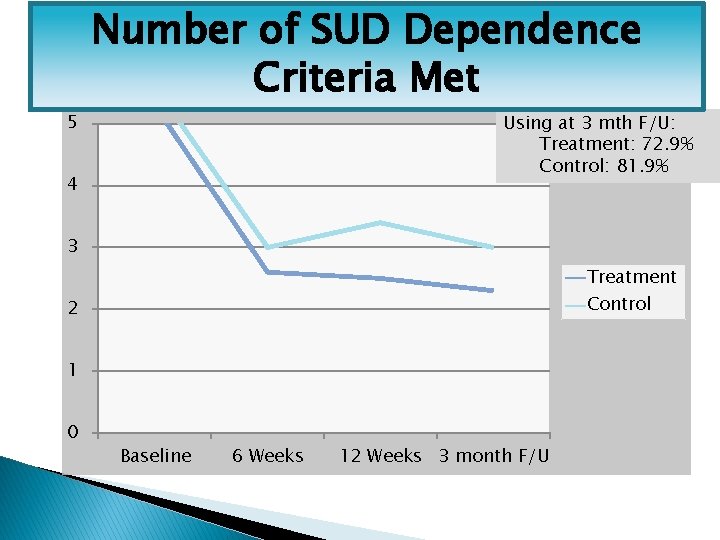
Number of SUD Dependence Criteria Met 5 Using at 3 mth F/U: Treatment: 72. 9% Control: 81. 9% 4 3 Treatment Control 2 1 0 Baseline 6 Weeks 12 Weeks 3 month F/U

COPE among Military Veterans
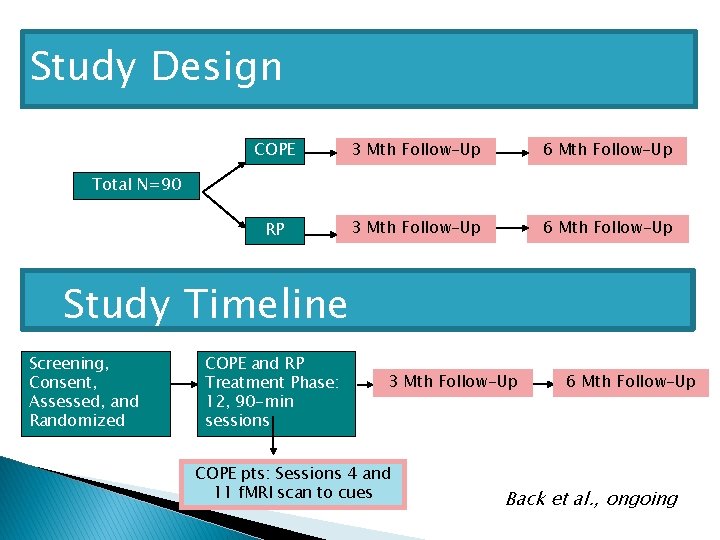
Study Design COPE 3 Mth Follow-Up 6 Mth Follow-Up RP 3 Mth Follow-Up 6 Mth Follow-Up Total N=90 Study Timeline Screening, Consent, Assessed, and Randomized COPE and RP Treatment Phase: 12, 90 -min sessions 3 Mth Follow-Up COPE pts: Sessions 4 and 11 f. MRI scan to cues 6 Mth Follow-Up Back et al. , ongoing

COPE Military Pt 001 ◦ ◦ Single, caucasian, 25 yr old male United States Marine (gunner) Served 3 deployments in Iraq (24 months total) No history of mental health treatment Back, Killeen, Foa et al. Am J Psychiatry 2012; 169: 688 -691

Case Details ØIndex trauma: Combat related. ØPTSD symptoms: Frequent nightmares, intrusive thoughts, isolation/distancing, aggression, extreme difficultly driving, hyperarousal in crowded places (e. g. , Walmart, movies), avoidance of thoughts and memories through alcohol. ØSubstance use symptoms: Consuming 12. 5 beers per day, 83. 3% of the time (50/60 days pre study). ØTx motivation: Initially did not want treatment (“military pride”) but his friend drove him to clinic.
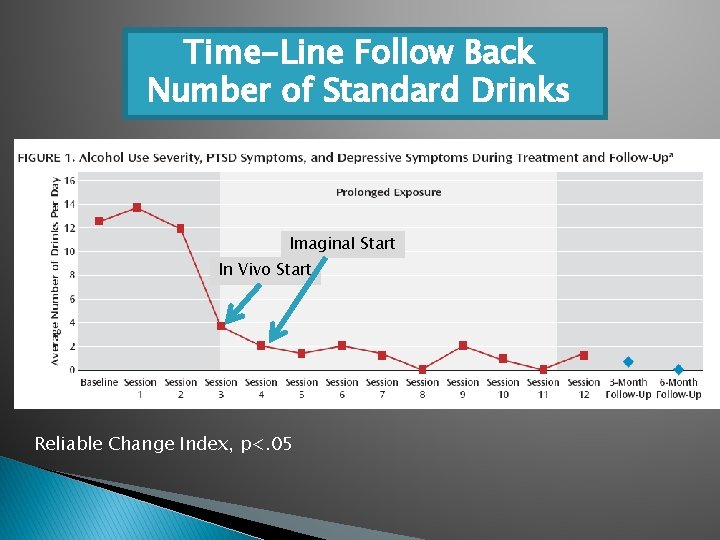
Time-Line Follow Back Number of Standard Drinks Imaginal Start In Vivo Start Reliable Change Index, p<. 05
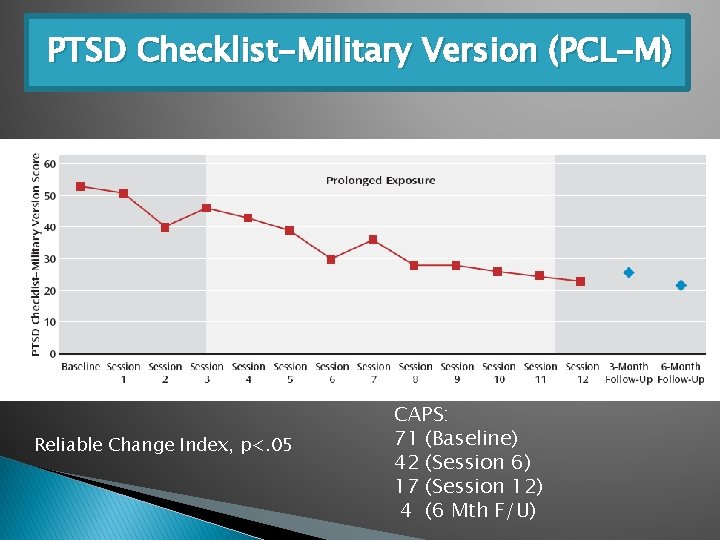
PTSD Checklist-Military Version (PCL-M) Reliable Change Index, p<. 05 CAPS: 71 (Baseline) 42 (Session 6) 17 (Session 12) 4 (6 Mth F/U)
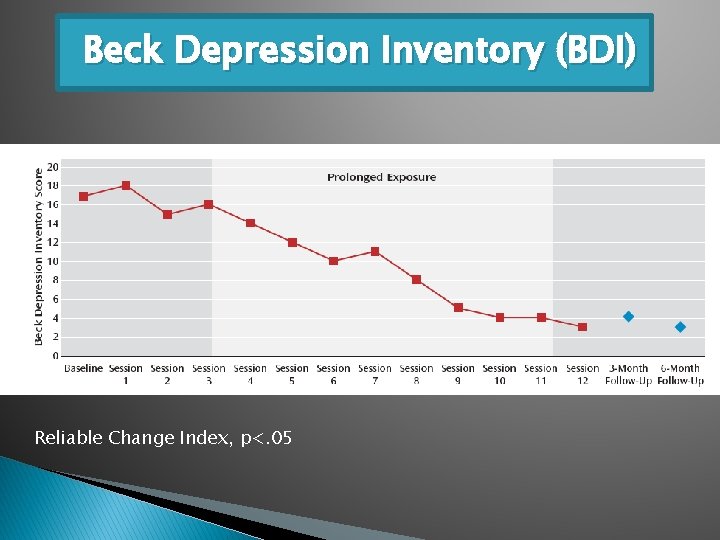
Beck Depression Inventory (BDI) Reliable Change Index, p<. 05

Summary Ø Studies among men and women, civilian and combat-related PTSD, multiple SUD and multiple traumas show: ◦ Feasible ◦ Safe – substance use did not increase with trauma-work ◦ Effective

- Slides: 49