Ptrme po mikrobech Dl XIV Opakovn doplkov tma

Pátráme po mikrobech Díl XIV. Opakování + doplňkové téma Ondřej Zahradníček K praktickému cvičení pro VLLM 0421 c Kontakty na mne: 777 031 969 zahradnicek@fnusa. cz ICQ 242 -234 -100

Ještě jedna pohádka • Jednou se tři policisté přeli o to, která metoda je nejlepší. • Jeden řekl: Nejdůležitější je snímání otisků prstů, to pomůže určit zločince. • Druhý zas: Ale nejdřív ho musíte chytit! A tak je důležitější pročesávání terénu. • Ale třetí, nejstarší, jim řekl: Nejdůležitější je umět používat metody dohromady, a vědět, kdy kterou použít.

Angličtina v odborném kontextu • Angličtina je mezinárodním jazykem vědecké komunikace, podobně jako kdysi latina. Bez ní se lékař neobejde. • Učitelé jazyků vás mohou naučit konverzaci a základní pojmy, avšak přesné kontextové použití odborných slovíček z jednolivých oborů samozřejmě nemohou znát • Existují i „zrádná slova“ – uvidíte sami • Proto vzniklo toto doplňkové téma

A abychom si zároveň zopakovali, co jsme probrali v tomto semestru • Začneme opakováním v angličtině • Poté si ukážeme některá zrádná slovíčka v mikrobiologické angličtině • Poté si napíšeme zápočtový test • Studenti se splněnými podmínkami zápočtu poté mohou obdržet zápočty

A microbe (microogranism): what does it mean? • It should be living. and grain of dust is not and microbe, although it is microscopical • It should be microscopical. and giraffe is not and microbe, although it is living The secondition is not absolute. For example, and tapeworm can measure 10 m. But the eggs are microscopical, so it belongs to the microbiology.

Main medically important microbes • Viruses (and prions) • Bacteria (e. g. and Streptococcus or an Escherichia) • Fungi (yeasts and molds) • Parasites – not all of them are microbes: – Inner parasites • Protozoa (e. g. Plasmodium malariae) • Flukes (e. g. Schistosoma haematobium) • Roundworms (e. g. Ascaris lumbricoides) • Tapeworms (e. g. Taenia saginata) – Outer parasites (lice, fleas, bugs)

Survey of methods • Direct methods: We search for a microbe, its part or its product (e. g. a bacterial toxin) – Direct detection in specimen – we use the whole specimen (blood, urine, CSF etc. ) – Strain identification – isolate determination • Indirect methods: We search for antibodies. An antibody is neither a part nor a product of a microbe – it is a macroorganism product, after being challenged by a microbe
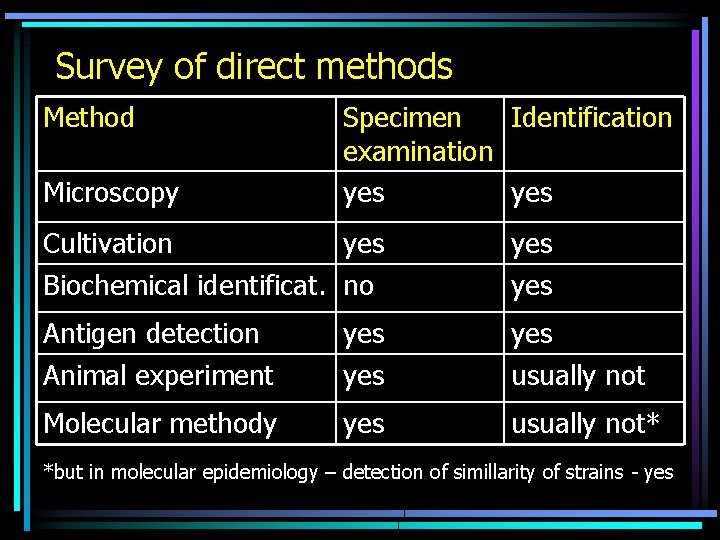

Survey of direct methods Method Microscopy Specimen Identification examination yes Cultivation yes Biochemical identificat. no yes Antigen detection Animal experiment yes yes usually not Molecular methody yes usually not* *but in molecular epidemiology – detection of simillarity of strains - yes

Microscopy

Microscopy • We observe microbes, in specimen also cells of host organism (epitheliae, WBCs etc. ) • Wet mount – for large and/or motile microbes (parasites, fungi, motile bacteria) • Dark field wet mount (mainly spirochets) • Fixated and stained preparations – Gram staining, Giemsa staining, Ziehl Neelsen staining (use for various groups of bacterií, fungi, parasites) • Electron microscopy – in viruses; rather for research than for common virological diagnostics
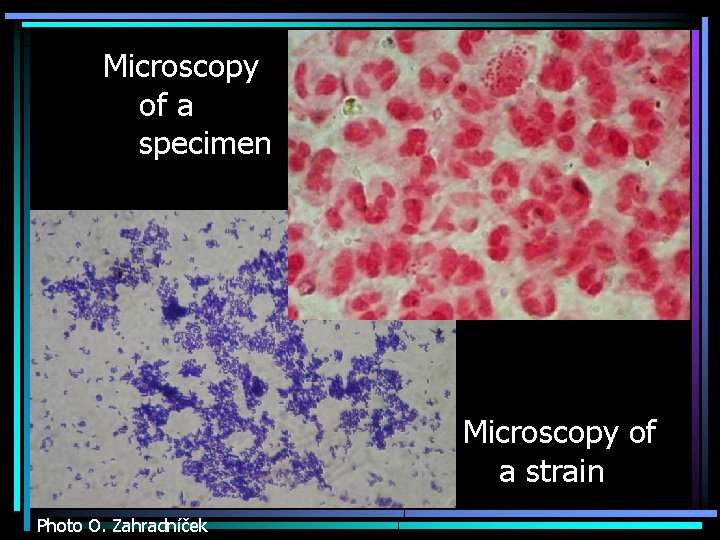
Microscopy of a specimen Microscopy of a strain Photo O. Zahradníček
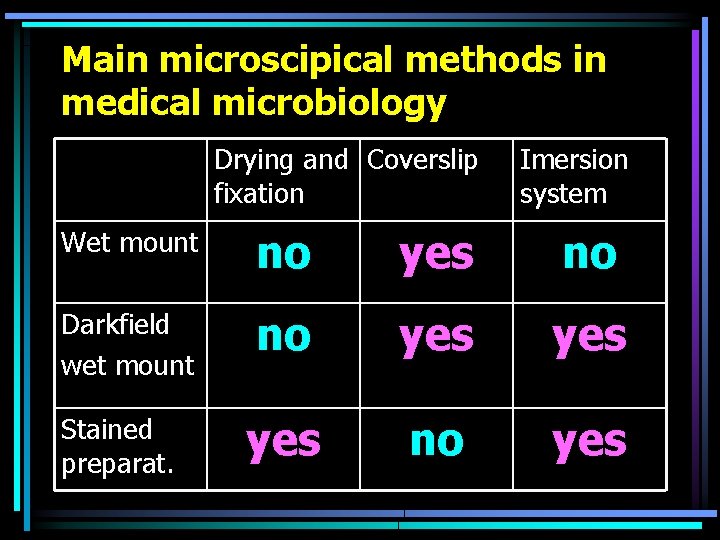

Main microscipical methods in medical microbiology Drying and Coverslip fixation Imersion system Wet mount no yes no Darkfield wet mount no yes yes no yes Stained preparat.

Preparing a microscopical preparation • We make a smear of a swab made by a cotton swab (in stained preparations only) • Liquid specimen are dropped on a slide • If we have a strain, we make a drop of physiological saline onto the slide. We sterilize a microbiological loop in flame and after drying we take a little of bacterial mass. We mix it in a drop of saline.
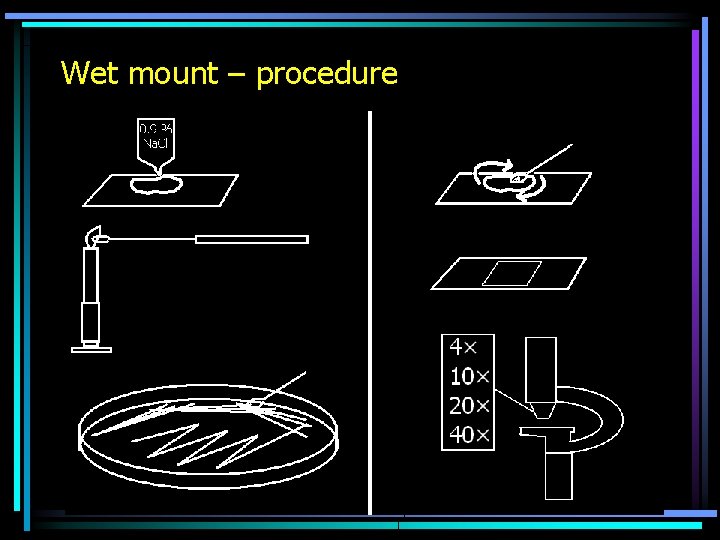
Wet mount – procedure
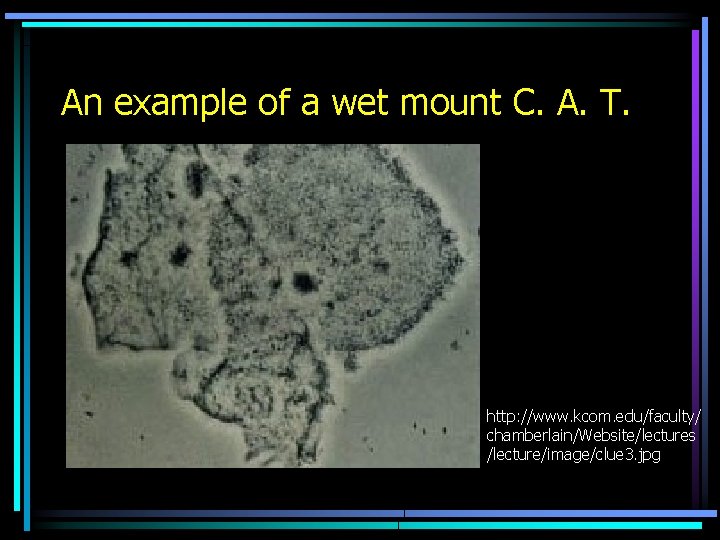
An example of a wet mount C. A. T. http: //www. kcom. edu/faculty/ chamberlain/Website/lectures /lecture/image/clue 3. jpg
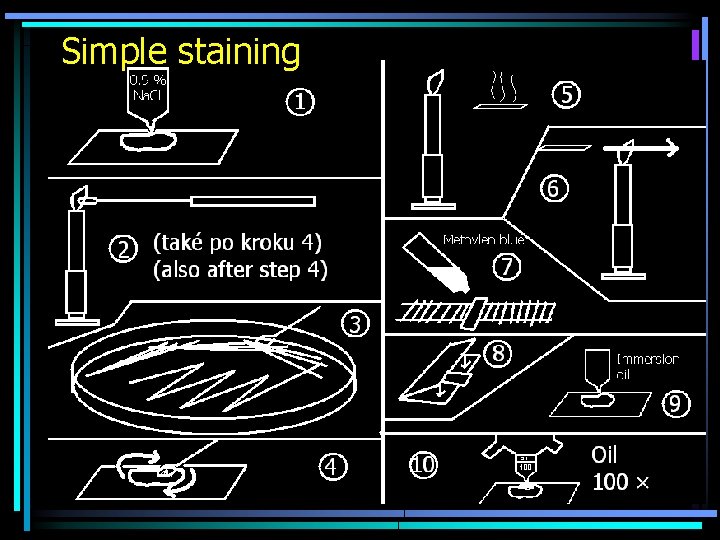
Simple staining
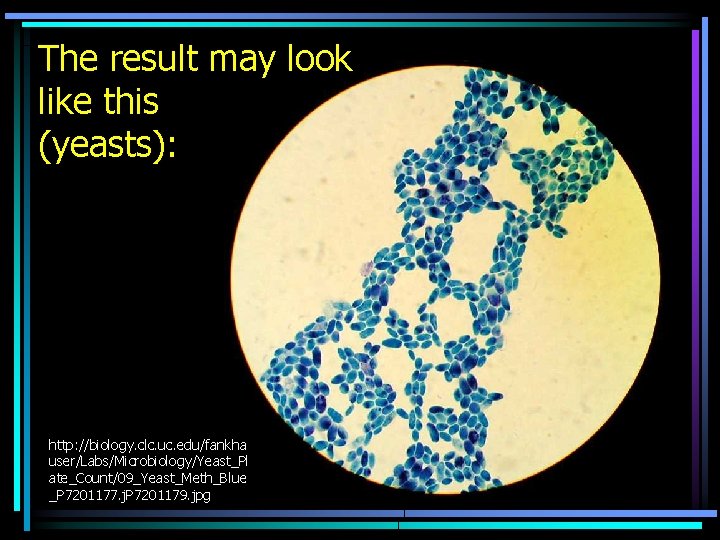
The result may look like this (yeasts): http: //biology. clc. uc. edu/fankha user/Labs/Microbiology/Yeast_Pl ate_Count/09_Yeast_Meth_Blue _P 7201177. j. P 7201179. jpg
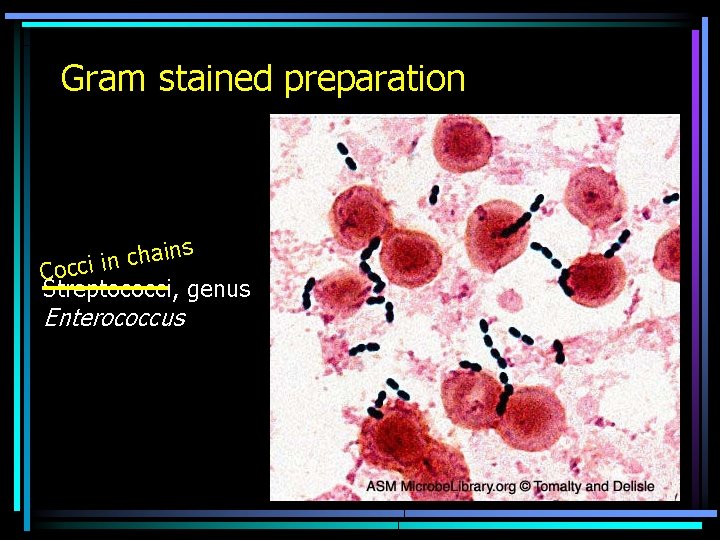
Gram stained preparation ins a h c n i Cocci Streptococci, genus Enterococcus

Bacterial cell wall • There are bacteria, that are mechanically strong, their cell wall is thick and simple. They are called gram-positive bacteria. • There are other bacteria, that are rather chemically strong, their cell wall is tenčí, thin, but more complex. They are called gram-negative bacteria. • Besides these and those, there also so named Gram non-staining bacteria.
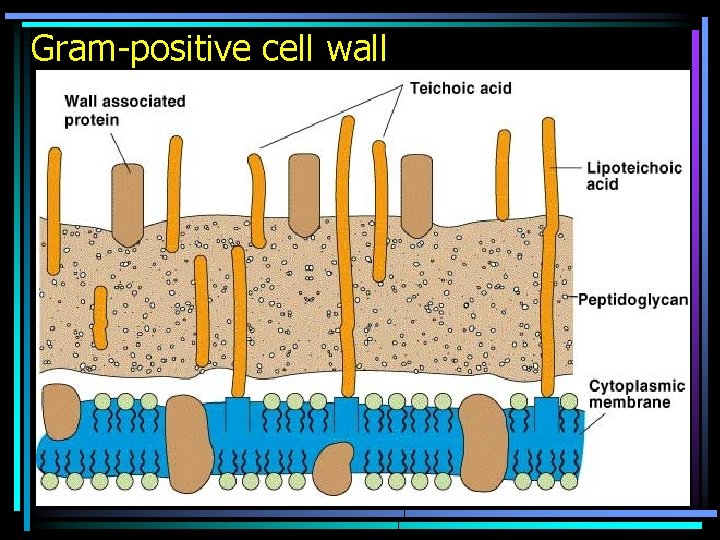
Gram-positive cell wall
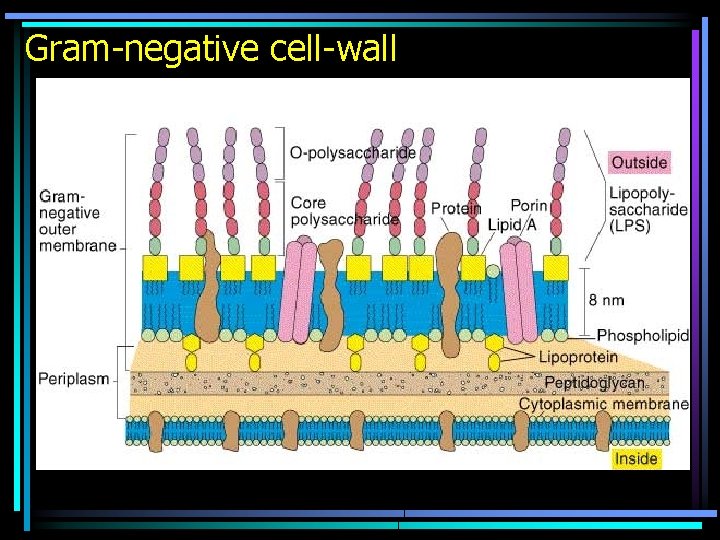
Gram-negative cell-wall

Gram staining – principle • Gram-positive bacteria have thick peptidoglycan layer in the cell wall. So, gentiane/crystallin violet binds more firmly to them, and after confirmation of this bound by Lugol solution even alcohol is not able to decolorize them. Gram-negative bacterie are decolorized by alcohol and thed stained red by safranin. Chemical Gram-positive Gram-negative Crystal. violet Staining violet Lugol iodine Confirmation Less confirm. Alkohol Not decolorized Decolorized Safranin Remain violet Stain to red
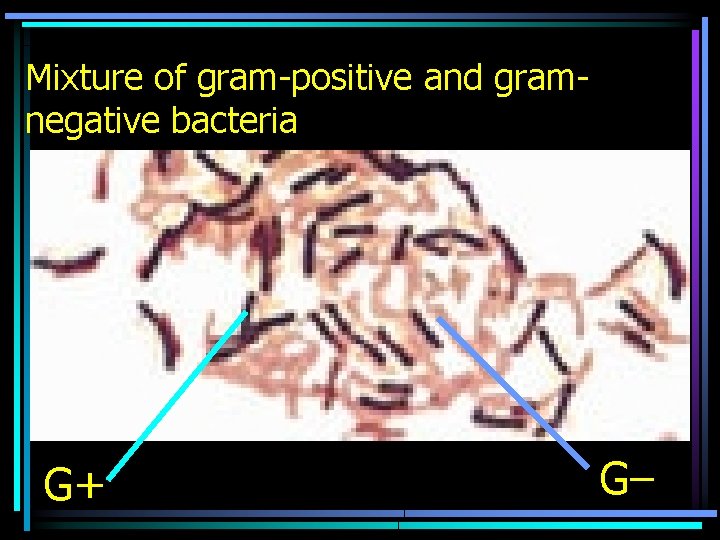
Mixture of gram-positive and gramnegative bacteria G+ G–

Culture

Do matter the conditions for bacterial growth? Of course not! Majority of bacteria need their temperature, moisture, salts concetration and many other characteristics to be in a quite narrow range. lower survival limit lower growth (bactericidal) limit (inhibitory) lower growth upper survival limit (inhibitory) limit (bactericidal) Values, that enable microbial survival, are not sufficient. They should be able to multiply. Various microbes need various conditions!

Medically important bacteria • Temperature usually needed around 37 °C – but bird pathogens more (42 °C), microbes coming from outside less (30 °C) • Value of p. H needed around p. H 7 – but gastric helicobacter by far less • Na. Cl concentration needed around 0, 9 % (physiological saline) – but staphylococci, that have to be able to multiply on sweated skin, multiplies even at 10 % of salt! In practice part of parameters (e. g. temperature) is derived from thermostat settings, and remainder (e. g. Na. Cl concentrations) by composition of the culture medium.

Culture thermostat Besides box thermostats, like this one, our Institute has a chamber thermostat, too. It is a whole room with 37 °C. Majority of bacteria is cultured in a thermostat overnight, so about 24 h.

Relation of bacteria to oxygen • Aerobic and facultative anaerobic (eventually aerotolerant) bacteria can be grown at normal athmosphere • Strictly anaerobic bacteria need athmosphere without oxygen • bacteria with special need for oxygen require special athmosphere (microaerophile and capnophile bacteria)

Why we culture bacteria • Why bacteria are cultured in the laboratory? – To keep them living and to multiply them. This is gained by cultivation in both liquid and solid media (jelly-consistence media, based on agar algae) – To obtain strain – solid media only – To differentiate and divide them mutually – diagnostic and selective media are used, for identification

Specimen and strain • Specimen is taken from a patient. Specimen contains cells macroorganism, various number of microbial species (zero to maybe twenty) and more items • A strain – an isolate – is a population of one bacteria, isolated from a specimen on a solid medium • To gain a strain, we have to grow a bacterium on a solid medium and inoculate carefully

Term „colony“ • A colony is a formation on a surface of a solid media. It is developped from one cell or a small group (couple, chain, cluster) • In some cases number of colonies on an agar shows us number of microbes in the specimen – or more preciselly, number of „colony forming units“ (CFU) • Description of colonies has an important place in. bacterial diagnostics

Liquid media and solid media • Liquid media are based on je meat-peptonic broth (exctract of cooked beef meat + protein hydrolysate). They are used mostly to multiplication. It is difficult to evaluate the result, in fact, only „non turbid broth – turbid broth“ (growth – no growth) • Majority of solid media are based on the same broth, but supplied by an agar alge extract. Bacteria grow slower on solid media, but the result is very variable, and it is possible to get a strain.

Liquid media

Classification of liquid media • Liquid media have two categories only: • multiplying media are common and universal. Example: broth for aerobic culture and VL-broth for anaerobic culture (VL = viande-levure, from french – contains meat-yeas extract) • selectively multiplying media were developped to multilply some bacteria and to supress multiplication of other. Example: selenite broth for salmonella

Solid media

Why an isolated colony is so important • Only ao we can identify larger number of mixed pathogens • But also because only isolated colonies enable to observe typical colony characteristics. The best clown is not able to show you his art, when kept with many other clowns in a small cupboard.
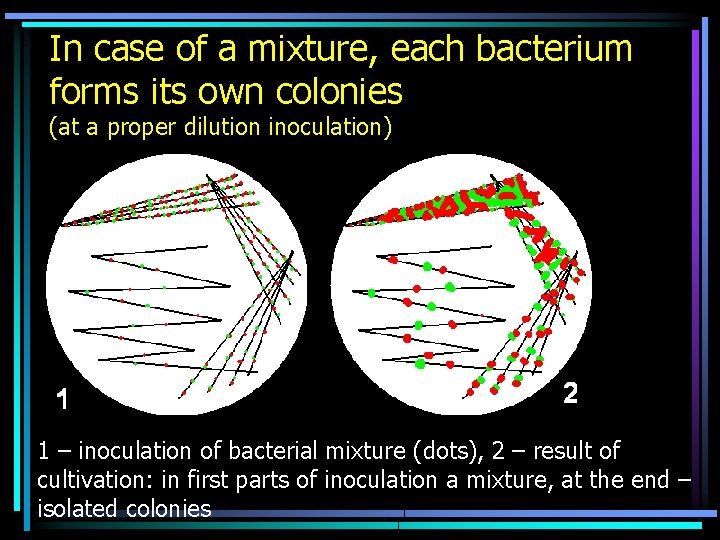
In case of a mixture, each bacterium forms its own colonies (at a proper dilution inoculation) 1 – inoculation of bacterial mixture (dots), 2 – result of cultivation: in first parts of inoculation a mixture, at the end – isolated colonies

What to describe at colonies • • • Size Colour Shape (round…) Profile (convex…) Edges • • • Surface (smooth, rough…) Consistence (dry…) Transparency Smell Colony surroundings* *Definition is related to the medium used. For example, haemolysis is observed around some bacteria grown on media with RBCs.
Solid selective media • They have to select (separate) from a bacterial mixture only one of several groups of genera • An example is blood agar with 10 % Na. Cl used for stafylococci • Sometimes, selectivity is reached by an antibiotic addition. Blood agar with amikacin is selective for streptococci and enterococci Illustration photo: Na. Cl crystals

Diagnostic media • They do not supress growth of any microbe • On the other hand, their composition enable them to differenciate microbes according to some properties • An example is blood agar to observe haemolytical properties, and VL blood agar (simillar, but to anaerobes) • Special case are chromogenic and fluorogenicmedia
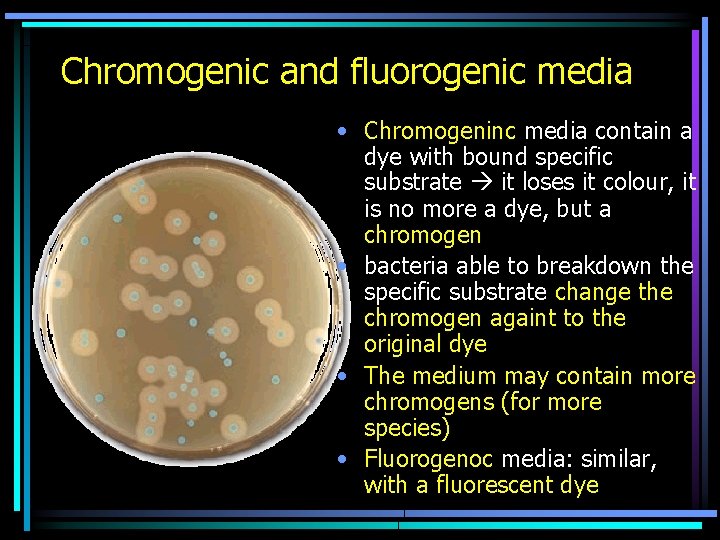
Chromogenic and fluorogenic media • Chromogeninc media contain a dye with bound specific substrate it loses it colour, it is no more a dye, but a chromogen • bacteria able to breakdown the specific substrate change the chromogen againt to the original dye • The medium may contain more chromogens (for more species) • Fluorogenoc media: similar, with a fluorescent dye
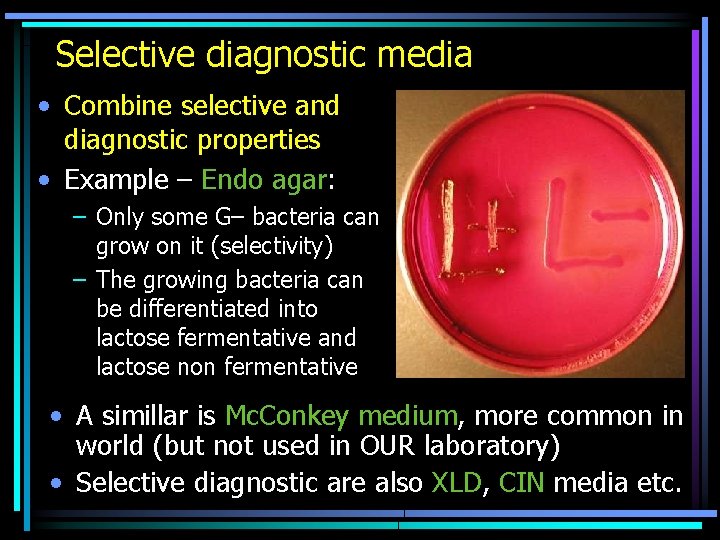
Selective diagnostic media • Combine selective and diagnostic properties • Example – Endo agar: – Only some G– bacteria can grow on it (selectivity) – The growing bacteria can be differentiated into lactose fermentative and lactose non fermentative • A simillar is Mc. Conkey medium, more common in world (but not used in OUR laboratory) • Selective diagnostic are also XLD, CIN media etc.

Selective, diagnostic and selective diagnostic media – review Selective medium Strain A does not grow Diagnostic Strain C medium grows, colonies Selective Strain E diagnostic does not medium grow Strain B grows Strain D grows, colonies Strain F grows, colonies Strain G grows, colonies

Enriched and selective enriched media • For bacteria with specific need for nutrients • They are enriched by different chemicals • Even blood agar is an enriched medium, although shown as a diagnostic medium (it may be considered a member of both groups). • An expample of „pure enriched medium“ is chocolat and Levinthal agar for pathogenous Neisseriae and hemophili (that do not grow even on blood agar) • Media may be selective enriched (e. g. GC agar, – chocolat agar with anibiotics for culture of Neisseria gonorrhoeae)
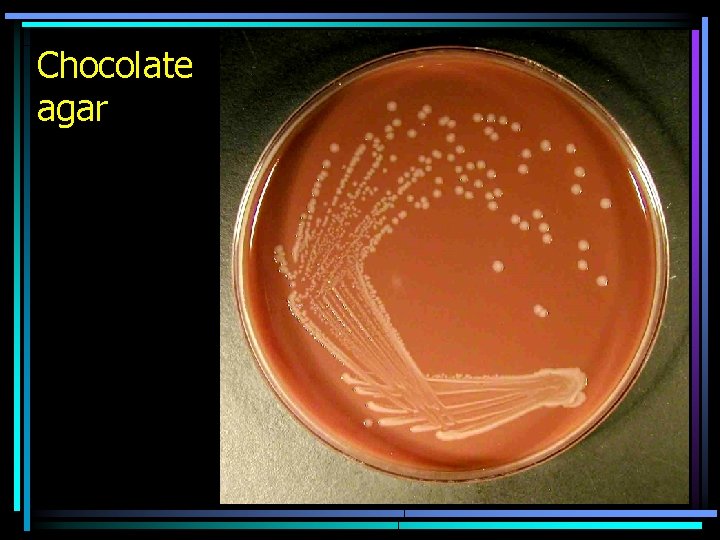
Chocolate agar

Special use media – 1 Observation of virulence factors • Picture shows a medium with Congo red for staphylococcal biofilm • or e. g. yolk agar for histotoxic clostridia Red, wet colonies Dry, black colonies mean no production show biofilm of biofilm production
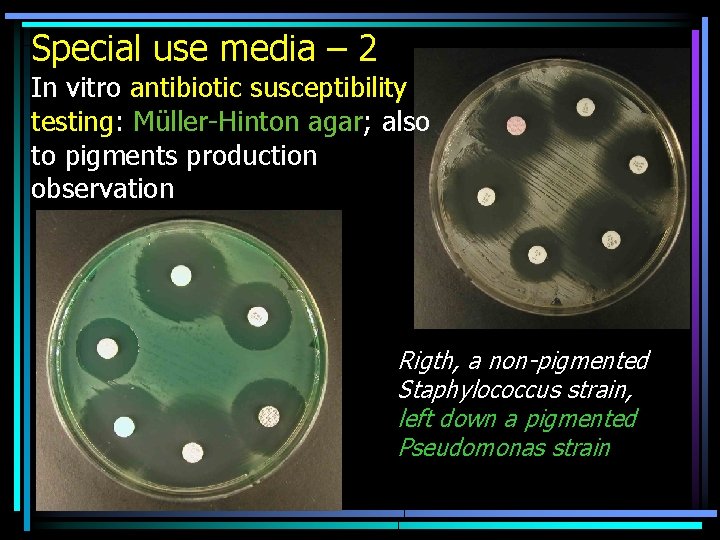
Special use media – 2 In vitro antibiotic susceptibility testing: Müller-Hinton agar; also to pigments production observation Rigth, a non-pigmented Staphylococcus strain, left down a pigmented Pseudomonas strain
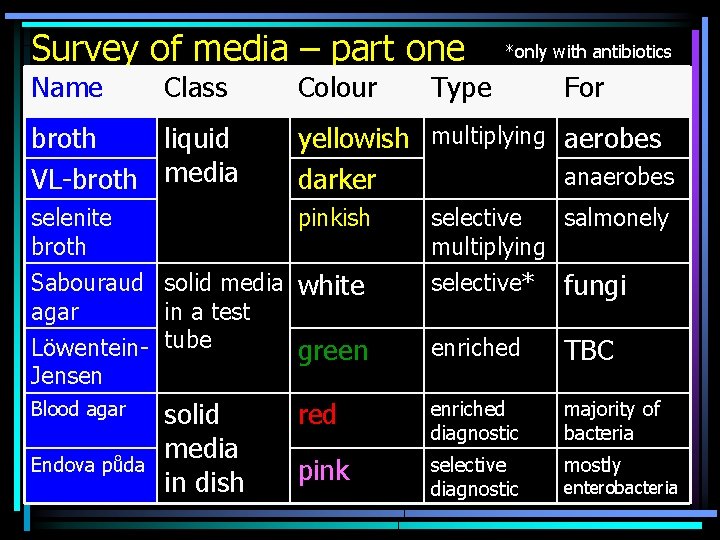
Survey of media – part one Name Class Colour *only with antibiotics Type For broth liquid VL-broth media yellowish multiplying aerobes anaerobes darker selenite broth pinkish Sabouraud solid media white agar in a test Löwentein- tube green Jensen Blood agar Endova půda solid media in. dish selective salmonely multiplying selective* fungi enriched TBC red enriched diagnostic majority of bacteria pink selective diagnostic mostly enterobacteria
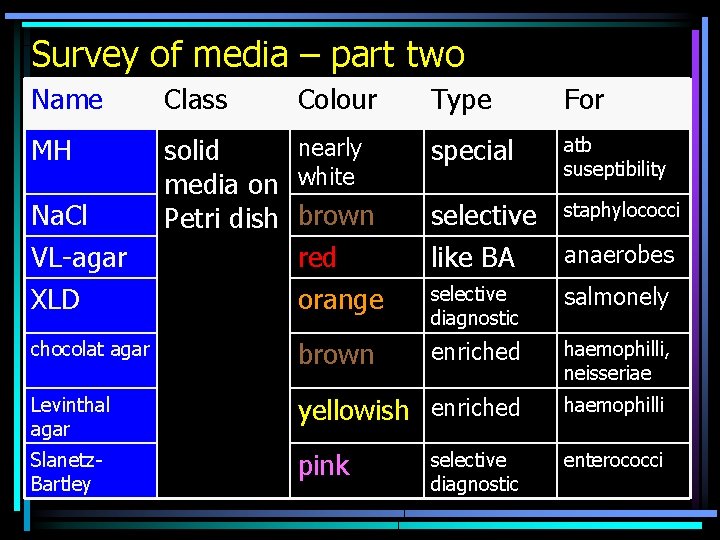
Survey of media – part two Name Class MH nearly solid media on white Petri dish brown red orange Na. Cl VL-agar XLD Colour Type For special atb suseptibility selective staphylococci like BA anaerobes selective diagnostic salmonely enriched haemophilli, neisseriae chocolat agar brown Levinthal agar yellowish enriched haemophilli Slanetz. Bartley pink enterococci selective diagnostic

Biochemical identification

Principle • Even between mammals there are differences. Human body is not able to produce vitamin C, body of some mammals is. • We offer certain substrate to a bacterium, and we search, whether bacteria change it into a product using an enzyme. A product has to be different from substrate by physical phase or colour. If it is not different, we use an indicator • There a lot of ways technical form of this test type.

Practical ways of doing it • Quick tests (seconds to minutes) – Catalase test – Tests s diagnostic strips (oxidase) • Tests with incubation (hours to days) – Simple test-tube tests – Complex test-tube tests – Sests of simple test-tube tests – Tests in microtitration plate (miniaturisation) – Other tests (e. g. Švejcar's plate)

Catalase test • Catalase test: very simple: we mix bacteria with substrate (H 2 O 2 solution). Bubbles = positivity. Principle: 2 H 2 O 2 2 H 2 O + O 2

Tests s diagnostic strips • Tests with dg. strips – We touch colonies by reaction area. If positive, the area changes its colour. The more common are: – oxidase – strip becomes blue – INAC – strip after minutes becomes blue-green – PYR – strip after minutes , addition of a reagent and one more minute of waiting becomes red – betalactamase strip – testing of some resistance factors (see in two weeks)

Oxidase test

Simple test-tube tests • They may be in liquid phase, or in agar. • In both cases, substrate is in a test tube, eventually together with an indicator. Substrate may be also added in form of a strip with reaction area with it (ONPG-test). • Test positivity = colour change (in whole volume, or as a ring at the surface)

Examples of simple test-tube tests • Arabinose – liquid. Turning yellow = positive, remains green = negative (for enterococci) • Simmons citrate – agar. Turning blue = positive, green = negative • ONPG and VPT – with addition of a strip. In ONPG, the liquid turns yellow; in VPT a red ring at the surface is produced

Complex test-tube tests • In one test-tube we have more reactions • For example MIU test. – M = motility (turbidity is spread through a halfliquid agar, not only in site of inoculation) – I = indol (positivity = red ring) – U = urea (breakdown of urea is indicated by the whole medium turning pink) • Or Hajna medium, detecting glucose breakdown, formation of gas from glucose, laktose breakdown and sulphan formation

MIU could be also done as three individual tests: motility…
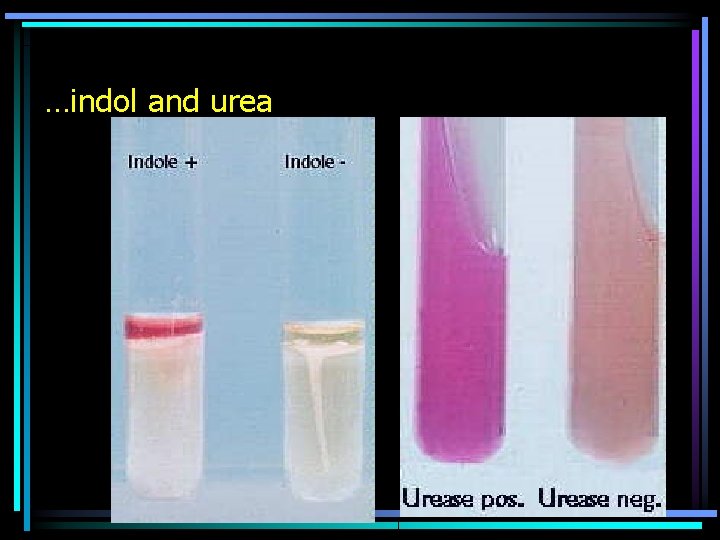
…indol and urea

Sests of test-tubes • Complex test-tube tests have some problems. Often positivity of one test disables to see another one. It is difficult to authomatize them and they require experienced personel. • More simple, although sometimes more expensive solution, is a set of several simple test-tube tests • It is, of course, also possible to combine both simple and complex tests (e. g. Hajna + MIU + Simmons citrate + ornithin dekarboxylase – in our laboratory)

Miniaturisation: tests in microtitration plates • Miniaturisation of a simple test-tube tests set tests in microtitration plate wells. Each test-tube is replaced by a well. • Number of tests in sets is variable from seven (Neisseria Test) to more than fifty • Technical detail are various. Nevertheless, always the substrate is lyofilized, bacteria are mixed with saline of suspensium medium and then it is mixed with the lyofilized substrate
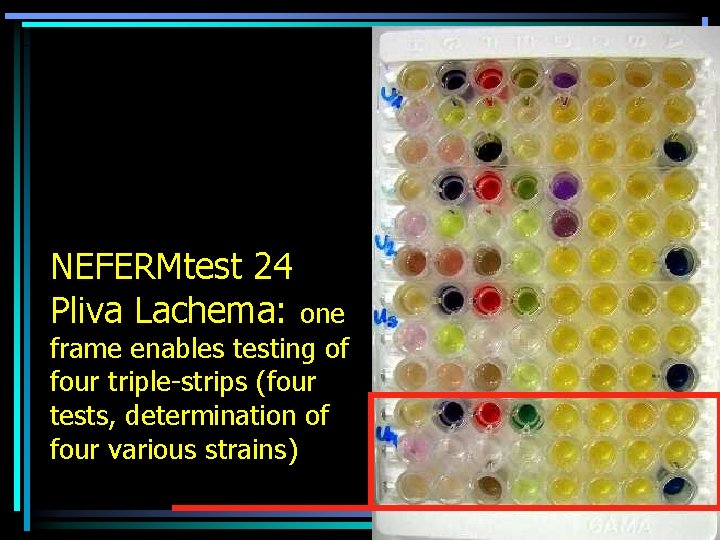
NEFERMtest 24 Pliva Lachema: one frame enables testing of four triple-strips (four tests, determination of four various strains)

Other identification tests • Besides tests based on substrate breakdown, we have also other similar tests, that find presence of some bacterial enzymes or virulence factors. For example: – Test of ability to coagulate rabbit plasma – Test of ability to agglutinate rabbit plasma – Test of ability to decapsulate an encapsulated strain (hyaluronidase test) – Motility testing – we have had it already
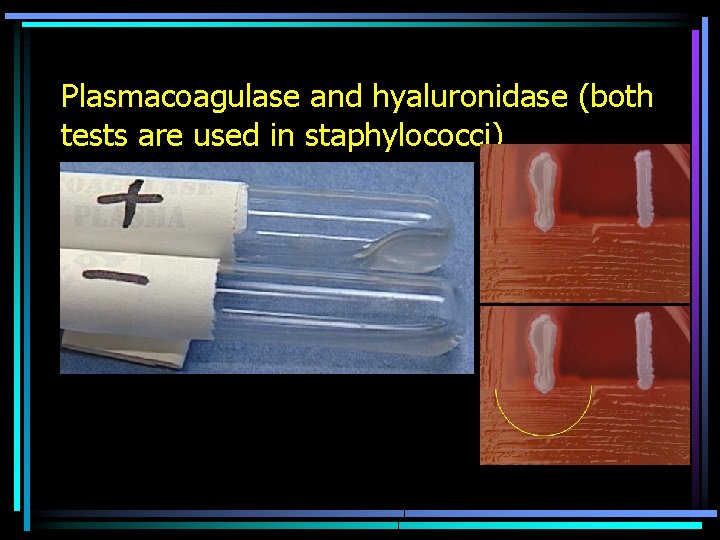
Plasmacoagulase and hyaluronidase (both tests are used in staphylococci)

Outer influences, decontamination

Microbes and outer influences I At decontaminationch methods, it is absolutelly necessary to reach such value of the acting physical or chemical factor, to kill the microbe. lower survival limit lower growth (bactericidal) limit (inhibitory) upper growth upper survival limit (inhibitory) limit (bactericidal) Primarilly, we are interested in survival limit (not growth limit, important for microbial cultivation).
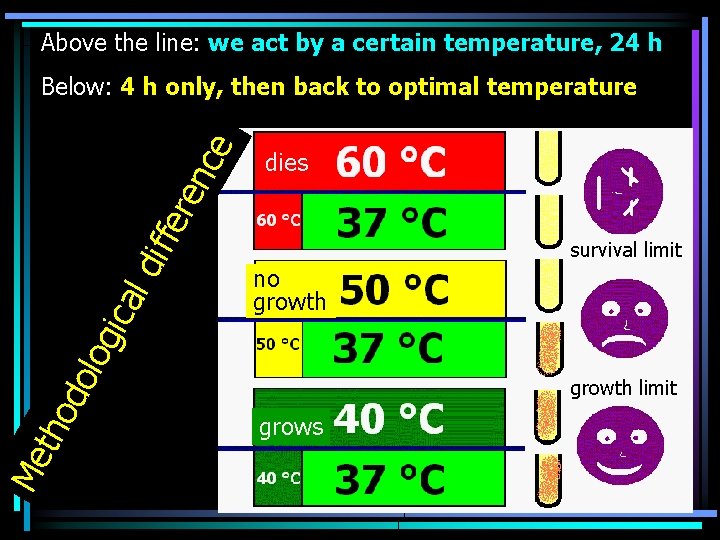
Above the line: we act by a certain temperature, 24 h dies survival limit no growth Me tho do log ica l dif fer en ce Below: 4 h only, then back to optimal temperature growth limit grows

Microbes and outer influences II Sometimes the action of factor combines The factor allways important is the time A resistant, spore 160 °C forming bacterium 170 °C 180 °C 20 min survives dies 30 min survives dies 60 min dies

Checing up, whether sterilisation was done, and its quality assessment • Orientation checking up – e. g. by typical smelling • Assessment of real concentration of disinfectants (chemically) • Chemical check up of sterilization uses indicators that change colour at a certain temperature • Biological way uses resistant strains of Bacillus genus. These absolve the whole cycle and then their survival is assessed.

Antibiotics

Methods of „fight“ with microbes • Immunisation – exploits natural mechanisms of a macroorganism • Decontamination methods – crude physical and chemical influences, action outside the organism (see last practical) • Antimicrobial agents – fine, targeted action inside the organism with aim of maximal effect of the microbe and minimal influence on the host macroorganism

Types of antimicrobial agents • Agents acting to the whole body: – Antiparasital agents against parasites – Antimycotics against yeasts and molds – Antivirotics against viruses – Antituberculotics against mykobacteria – Antibiotics against bacteria (natural origin) – Antibacterial chemoterapeutics also against bacteria, but syntetic In recent period, the last two groups are often put into one group called „antibiotics“ • Locally acting agents: antiseptics

Results of the diffusion disc test CITLIVÝ REZISTENTNÍ n 1 Bacteria are affraid of antibiotics. Large zone (sometimes so large that it is impossible to measure it) n 2 Bacteria are not affraid of antibiotics, they are resistant. A small zone around the disc, or no zone.

Diffusion disc test in practice: zones are measured and compared with reference zohes

Microdillution test • Atb-s are in a row of wells in a plastic microtitration plate, concetration decreases • The lowest concetration, that inhibits the growth, is the MIC value • For interpretation, we need breakpoint values for each antibiotic. MIC < breakpoint => the strain is susceptible. MIC > breakpoint => resistance • One plate is usually used for one strain, e. g. 12 antibiotics, each in 8 concentrations

Microdilution test – example

E-tests • Principially simillar to diffusion disc test • Instead of a disc, a strip is used • The strip has raising atb concentration from one end to another ( grace to a special technology – that is why they are expensive) • The zone is not round, but egg-shaped • The test is quantitative • The strip has a scale – sipmle reeding(see image on the next screen)

E-tests – result We can read the MIC value directly on the strip – in place, where the margins cross the strip

Assessment of resistance factors • Sometimes, instead of susceptibility testing, we should rather assess the presence of individual resistance factors by special methods, e. g. betalactamases • Some of theme are diagnostic strips (chemical detection of a given enzyme) or tests on a different principle. • It is mostly used in situations, where susceptibility tests are not sure enough (for many reasons, e. g. a metabolite is active, l and not the antibiotic itself, etc. )
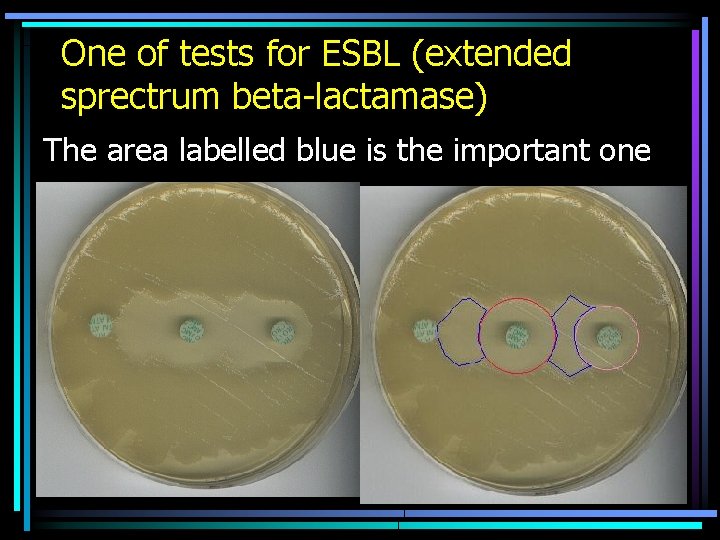
One of tests for ESBL (extended sprectrum beta-lactamase) The area labelled blue is the important one

Serology

Antigen and antibody Antigen = a macromolecule coming from an alien organism: plant, microbe, animal. In microbiology, we are interested in microbial antigens – parts of microbial body, that challenge host body to an antibody response Antibody = an immunoglobuline, formed by the host body as a response to antigen challenge (of course not only by humans, but also by various animals)

Two ways how to use it: Antigen detection: laboratory (animal origin) antibodies + pacient‘s sample or microbial strain. Direct method Antibody detection: laboratory antigen (microbial) + pacient‘s serum (or saliva). Indirect method

Interpretation • Antigen detection: it is a direct method. Positive result means presence of the microbe in the pacient‘s body • Antibody detection: it is an indirect method. Nevertheless, there are some ways how to get the information – when the microbe met the body: – Amount of antibodies (relative – titre) – Class of antibodies: Ig. M/Ig. G – Avidity of antibodies

Titre • After serum dilution, we add the antigen • In relation with the reaction type, either we can se the reaction result directly (aglutinate, precipitate), or we have to visualize it adding other components (complement, RBCs, etc. ) • Anyway, we have to be able to discriminate positive and negative reaction results • The highest dilution, where a positive reaction is still visible, is called titre.

Dynamics of titre 1 first pacient‘s visit 2 after 2 – 3 weeks • Absolute amount of antibodies is not the most sure information: some patients are poor antibody-producers, etc. • Dynamics of titre: better, means how the response gets changed during the time (usually during two or three weeks) 2 1

Precipitation and aglutination – common characteristics • Precipitation and aglutination are the two most simple serological reactions, we work here really with antigen and antibody only without other componenes • Either we decect antigen using animal antibody, or antibody using laboratory antigen • Only in the second example, we count titers!

Precipitation, agglutination on carriers • Precipitation: Antigens act alone, as macromolecules (coloid antigen) • Agglutination: Antigen act being part of its microbial cell (we work with whole microbes, corpuscular antigen) • Agglutination on carriers: Formerly isolated antibodies are bound to an alien particle – latex or RBC
Precipitation

Aglutination
Aglutination on carriers

Complement-fixing test (CFT) • Complement = one component of immunity reaction • For CFT, we use animal (guinea-pig) complement. The patient‘s complement is inactivated before the reaction • Complement is not able to get bound to isolated antigen • Complement is not able to get bound to isolated antibody • Complement is able to get bound to COMPLEX antigen – antibody
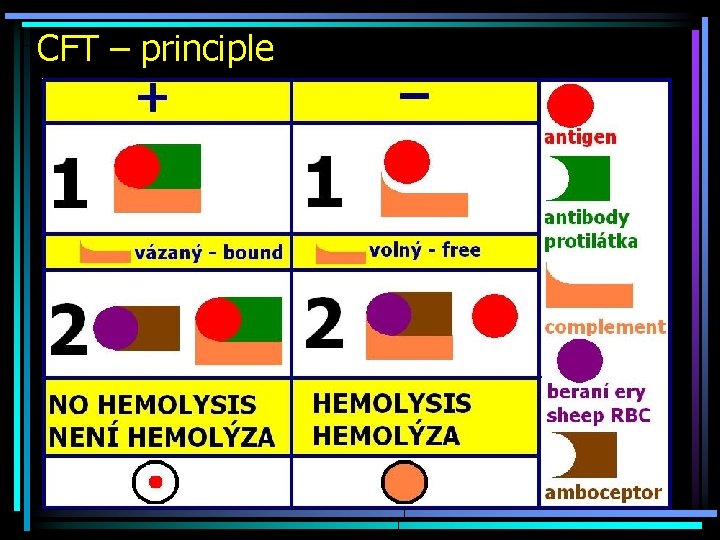
CFT – principle

Problems existing in CFT • Too much complement: false negative results. What to do? Titrate the complement (according to Task 2) • Something in serum binding the complement itself (anticomplementarity component): false positive results. What to do? Perform anticomplementarity test without antigen (A situation like a homeless man sweeping the plant globules from the bench)

Anticomplementarity test

Neutralisation reaction: general principle • There are many ways, how antibodies do work. One of them is direct neutralising effect • This effect is rarely present in whole bacteria. On the other hand, it may be observed in whole viruses, and in bacterial toxins Nevertheless, sometimes antibodies neutralise some characteristic of the whole bacteria, e. g. motility of Treponema in Nelson‘s test

Neutralisation schematically • Antibody (Ig) prevents an effect of a toxin/virus to a cell / red blood cell • Example: ASO (Toxin = streptolysin O, Ig = antistreptolysin O, red blood cell)

Examples of neutralisation reactions Task Neutralised Object Reaction 1 Bacterial toxin RBC (haemolysin) haemolysis ASO 2 Virus RBC agglutination HIT 3 Virus Cell metabolic efect VNT

Reactions with labelled components • Individual components are bound on the previous components, the first of them to the surface. • Instead of one component a specimen from pacient is used. The specimen is suspicious to contain the given component. • If it is true, the component is bound • When all components bind respectivelly, a not-interrupted chain is formed • At the end there is a labelling agent

Washing out and its sense • When also the components that are not bound to the surface would remain, we would not be able to differenciate a positive reaction and a negative one. • That is why after each step washing follows. After such a washing, only bound components remain present. • When the chain is broken, the part after the missing component is washed out.

Types of labelling agent • Fluorescent dye is labelling agent in immunofluorescence • Radioisotope is labelling agent in RIA • Enzyme is labelling agent in ELISA – Western blotting is a special type of an ELISA, where individual antigens are divided electroforetically When an enzyme is used as a labelling agent, the very last component should be the substrate – so one more component.

Importance of the conjugate • Conjugate is used mostly in indirect reactions (detection of antibodies) • It is an antibody that has human antibody (e. g. Ig. M, Ig. A or Ig. G) for an antigen • It can be selective against a certain antibody class • Use of conjugate is the principle of selective diagnostic of individual immunoglobulin classes

ELISA antibody detection: 1. Positive (searching Ig. M, Ig. M present) All components bind step by step. An enzymatic reaction leads to colour change in the well.
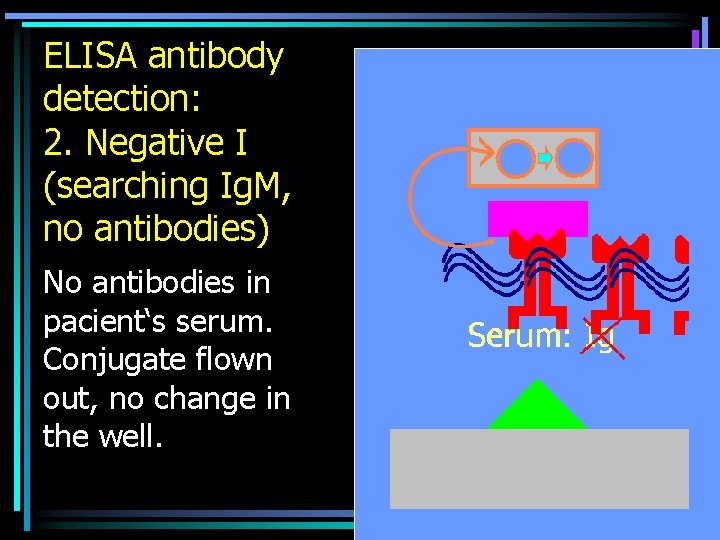
ELISA antibody detection: 2. Negative I (searching Ig. M, no antibodies) No antibodies in pacient‘s serum. Conjugate flown out, no change in the well.
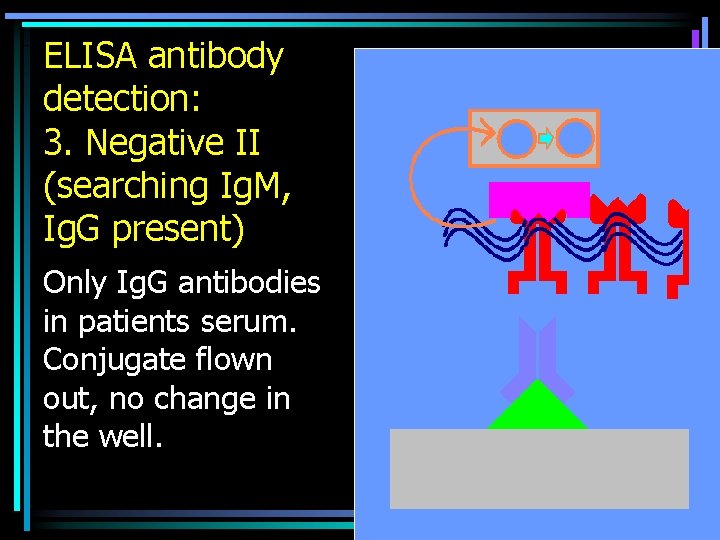
ELISA antibody detection: 3. Negative II (searching Ig. M, Ig. G present) Only Ig. G antibodies in patients serum. Conjugate flown out, no change in the well.

PCR

Basic scheme of PCR reaction • In first phase we have to get isolated DNA. It is a complex process • In second phase proper amplification runs (only if the specimen contains a part of DNA corresponding to a primer) • In third phase amplification product should be detected by – gel electroforesis of by – ELISA method (≠ serologic ELISA!!!)

Use of DNA (RNA) detection in medical microbiology • The methods are used mostly in situations, where microscopic and culture diagnostic is difficult or impossible • It is not very useful for common, ubiquitous pathogens. Because of its sensitivity they would detect accidental molecules comming from environment • The methods are neither useless, as some people think, neither all-problems-solving, as some other people suppose.

Survey of interpretation Proper reaction Internal control Interpretation negative positive negative positive inhibition of reaction positive negative (highly) positive
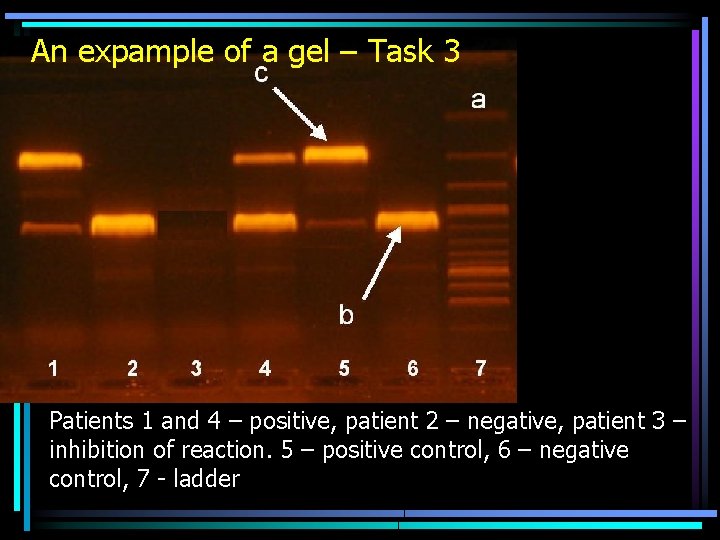
An expample of a gel – Task 3 Patients 1 and 4 – positive, patient 2 – negative, patient 3 – inhibition of reaction. 5 – positive control, 6 – negative control, 7 - ladder

Virology

Virological diagnostics • Culture isolation Requires living cells. • Microscopy: electronoptical, optical only to examination of somenting, that viruses do in vivo / in vitro (inclusions, cytopatic effect) • Biochemical identification is not possible • Animal experiment here equal to izolation • Detection of DNA – in viruses > bacteria • Detection of Ag in specimen – very common • Indirect diagnostics – usually basis of the entire diagnostics
Viral isolation • Animal now less commonly. Typical animal is a suckling baby mouse. • Fertilized egg is a classical method: – Amniotic sac – Alantoic sac – Yolk sac – Chorioallantoic membrane (only here sometimes a visible result – so called pocks) • Tissue cultures: LEP, He. La, monkey kindney and various other. Some viruses perform a cytopathic effect (CPE) on tissue cultures, but some viruses do not.
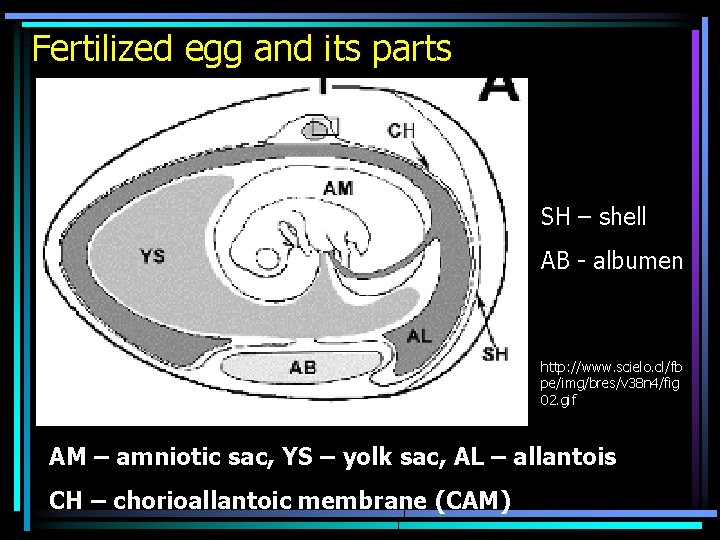
Fertilized egg and its parts SH – shell AB - albumen http: //www. scielo. cl/fb pe/img/bres/v 38 n 4/fig 02. gif AM – amniotic sac, YS – yolk sac, AL – allantois CH – chorioallantoic membrane (CAM)
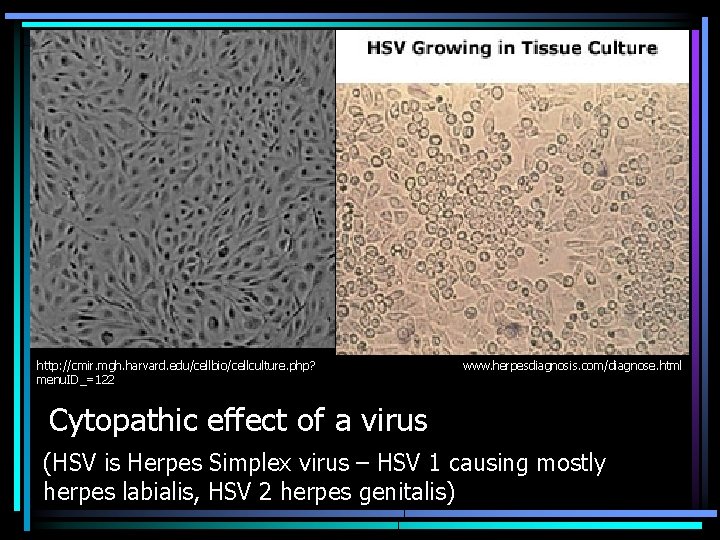
http: //cmir. mgh. harvard. edu/cellbio/cellculture. php? menu. ID_=122 www. herpesdiagnosis. com/diagnose. html Cytopathic effect of a virus (HSV is Herpes Simplex virus – HSV 1 causing mostly herpes labialis, HSV 2 herpes genitalis)

Zrádná slovíčka • • • – a jejich zrádnosti ASLO – ASO (ej es ou; antistreptolyzin O) ASTAL – ASLO (ej es el ou; antistafylolyzin) acidorezistentní – acid fast (méně často acidoresistant) agarová miska (plotna) – agar plate anaerostat – anaerobic jar bakterie (ženský rod) – bacterium (střední rod) (množné číslo: bacteria) barvení – staining barvivo – dye (nepsat s měkkým i!) břišní tyfus – typhoid fever (typhus = skvrnitý tyfus) hemokultura – blood culture (méně často haemoculture) izolovat – to isolate; isolate je ale i podstatné jméno

Zrádná slovíčka • • • – a jejich zrádnosti kmen, izolát – strain, isolate (stem = kmen stromu) kok – coccus (čti: kokəs; množné číslo: cocci – koksáj) kultivace – culture (méně často cultivation) kultivovat – to cultivate, to grow an organism kvasinka (i kvasnice) – yeast legionářská nemoc – legionaire’s disease likvor – cerebrospinal fluid (často zkratkou – CSF) měkký vřed – chancroid nátěr i natírat – smear nativní preparát – wet mount plané neštovice (slov. ovčie kiahne) – chickenpox (chicken pox) plíseň – mold

• • • Zrádná slovíčka – a jejich zrádnosti pravé neštovice (slov. kiahne) – smallpox proužek (např. oxidasový) – strip přenos (infekce) předměty – transfer via fomites (jednotné číslo fomes) příušnice (slov. príušnice i mumps ) – mumps řádek, dvojřádek (například ve STAPHYtestu) – strip sepse – sepsis i septicaemia spála (slovensky šarlach) – scarlatina spalničky (slov. osýpky) – measles tvrdý vřed (u syfilis) – chancre tyčinka – bacillus, rod výtěr i výtěrový tampon na špejli – swab (též jako sloveso – to swab) zarděnky (slov. ružienka) – rubella, rubeola

Zrádná slovíčka – a jejich zrádnosti S. P. Q. R. bičenka poševní blecha morová blecha obecná členovci (mn. č. ) háďátko střevní Trichomonas vaginalis používá se latinský název Pulex irritans bičíkovec pošvový blcha morová blcha ľudská Arthropoda článkonožce arthropodes Strongyloides stercoralis háďatko črevné používá se latinský název Xenopsylla cheopis plague flea (common) flea

Zrádná slovíčka – a jejich zrádnosti S. P. Q. R. klíšťák Argas sp. kliešťak klíště (stř. rod) Ixodes sp. a kliešť koutule flebotomové jiné druhy soft tick (m. (hard) tick rod) Phleboto- kútovky, minae flebotomi měchovec Ancylostoma duodenale / Necator americanus machovec dvanáctnikový měchožil zhoubný Echinococcus granulosus echinokok sandflies, gnats hookworm používá se latinský název
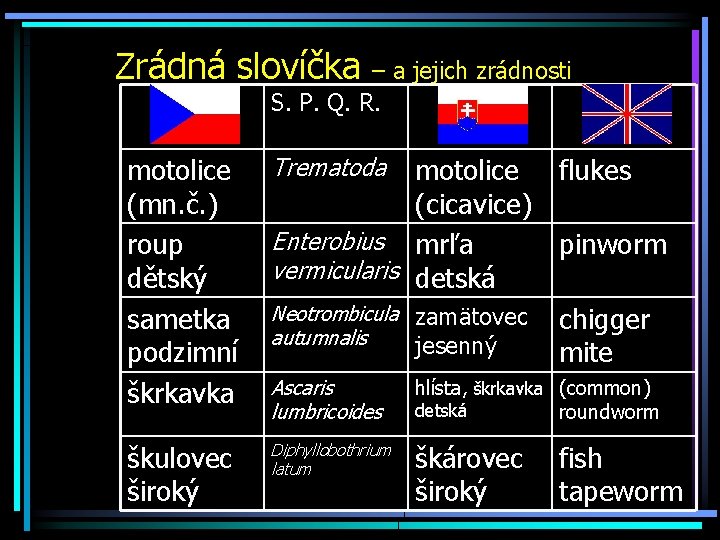
Zrádná slovíčka – a jejich zrádnosti S. P. Q. R. motolice (mn. č. ) roup dětský sametka podzimní škrkavka Trematoda Ascaris lumbricoides hlísta, škrkavka (common) detská roundworm škulovec široký Diphyllobothrium latum škárovec široký motolice flukes (cicavice) Enterobius mrľa pinworm vermicularis detská Neotrombicula zamätovec chigger autumnalis jesenný mite fish tapeworm

Zrádná slovíčka – a jejich zrádnosti S. P. Q. R. štěnice Cimex lectularius šváb Blatta orientalis tasemnice Taeniarhynchus bezbranná saginatus tasemnice Hymenolepis nana dětská tasemnice Taenia dlouhočlenná solium posteľná bed bug, true bug ploštica šváb cocroach (obyčajný) pásomnica beef dlhá tapeworm pásomnica dwarf detská / trpasličia tapeworm pásomnica pork obyčajná tapeworm
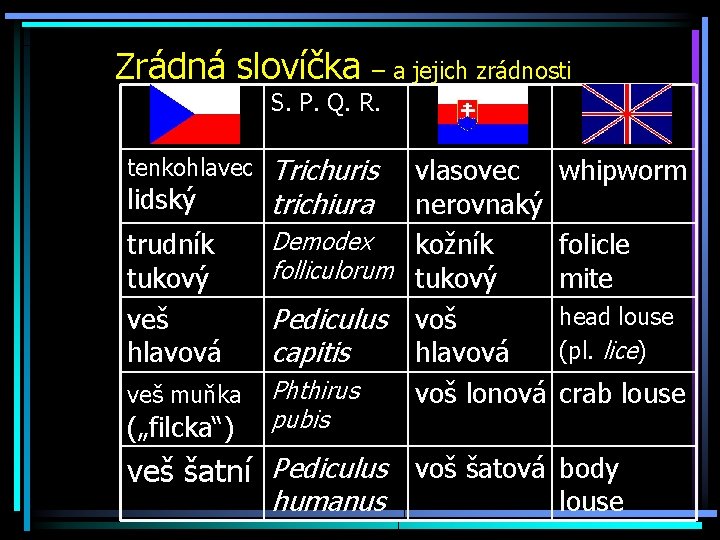
Zrádná slovíčka – a jejich zrádnosti S. P. Q. R. tenkohlavec lidský trudník tukový veš hlavová veš muňka („filcka“) Trichuris trichiura vlasovec nerovnaký Demodex kožník folliculorum tukový Pediculus voš capitis hlavová Phthirus voš lonová pubis whipworm folicle mite head louse (pl. lice) crab louse veš šatní Pediculus voš šatová body humanus louse

Zrádná slovíčka – a jejich zrádnosti S. P. Q. R. vlasovec Dracunculus medinensis medinský Sarcoptes zákožka svrabová scabiei vlasovec medinský používá se latinský název zákožka svrabová/ svrabovec kožný (itch) mite A nyní následuje zápočtový test…
And now, let‘s go to the credit test! Trichomonas vaginalis, photo O. Z.
- Slides: 126