Psychotropic Medication Advocacy 1 Result of concerns about

Psychotropic Medication Advocacy

1. Result of concerns about the use of psychotropic medications for people with MR/DD. 2. Represents a coming together of seven professional disciplines: neurology, nursing, pharmacy, pediatrics, psychiatry, psychology, and special education from 11 nations as well as consumers and families 3. Intended uses include: • Consumers-to help formulate questions to physicians and service providers • Agencies-to provide a copy of the book to consulting physicians as a means of strengthening the information on which decisions are made • Physicians-to learn about the observations and opinions of the consensus panel and various committees that wrote the book.

Chapter 4 Guidelines for the Use of Psychotropic Medication John E. Kalachnik, Bennett L. Leventhal, David H. James, Robert Sovner, Theodore A. Kastner, Kevin Walsh, Steven A. Weisblatt, Margaret G. Klitzke 11 -16 -09 Updates via personal contact with John E. Kalachnik

#1 -Psychotropic Medication Definition A psychotropic medication is any drug prescribed to stabilize or improve mood, mental status, or behavior.

#1 -Psychotropic Medication Definition This includes medications typically classified as • antipsychotic, • anti-anxiety, • anti-depressant, • anti-mania, • stimulant, or • sedative-hypnotic, but only if they are prescribed to improve mood, mental status, or behavior.

#1 -Psychotropic Medication Definition This includes other medications not typically classified as psychotropic when such medication is prescribed to improve or stabilize mood, mental status, or behavior, e. g. Benadryl for sleep

#1 -Psychotropic Medication Definition This includes herbal or nutritional substances when such substances are used to stabilize or improve mood, mental status, or behavior.

#2 -Inappropriate Use Psychotropic medication shall not be used �excessively, �as punishment, �for staff convenience, �as a substitute for meaningful psychosocial services, �or in quantities that interfere with an individual’s quality of life.

#2 -Inappropriate Use When this guideline is not followed, psychotropic medication becomes chemical restraint or is not being used in the best interest of the individual.

#2 -Inappropriate Use Excessive includes: inappropriately high doses or inappropriately long periods of time relative to the diagnosis or condition of concern.

#2 -Inappropriate Use Punishment includes the use of psychotropic medication in response to an individual who is exercising his or her legal rights or appropriately responding to inappropriate staff or peer behavior (e. g. striking out at a staff member who is improperly confiscating the individual’s possessions or fighting with a peer who is attempting to assault the individual).

#2 -Inappropriate Use Staff convenience includes the use of psychotropic medication to compensate for poorly trained staff, staff shortages, poor environmental conditions, or non addressed medical or health concerns.

#2 -Inappropriate Use Substitute for meaningful psychosocial services includes the use of psychotropic medication to replace more appropriate or necessary therapeutic, behavioral, or educational interventions.

#2 -Inappropriate Use Interference with quality of life Means that while a specific behavior or condition may be improved, a decline in functional status or learning ability compromises the individual to a greater degree than does the behavior or condition.

#3 -Multidisciplinary Care Plan Psychotropic medication must be used within a coordinated multidisciplinary care plan designed to improve the individual’s quality of life.

#3 -Multidisciplinary Care Plan Psychotropic medication alone is not a care plan. A number of professional and responsible parties may be involved in an overall plan to: • teach skills • alter environmental stressors • provide otherapy • provide patient and family education

#3 -Multidisciplinary Care Plan Multidisciplinary care members must not work in isolation. Med changes must be communicated to other team members and coordinated with changes in life activity or therapy. Similarly, these changes should be coordinated with med changes.

#3 -Multidisciplinary Care Plan This does not include stat orders that by definition constitute emergency intervention. This guideline applies to PRN orders.

#4 -Diagnostic and Functional Assessment The use of psychotropic medication must be based on: 1) a psychiatric diagnosis, or 2) a specific hypothesis if a psychiatric diagnosis is unclear at the time resulting from a diagnostic and functional assessment.

#4 -Diagnostic and Functional Assessment A diagnostic & functional assessment address: 1) Organic and medical pathology 2) Psychosocial & environmental conditions 3) Health status 4) Current medications 5) Presence of a psychiatric condition 6) History, previous interventions/results 7) Functional analysis of behavior

#4 -Diagnostic and Functional Assessment Functional analysis of behavior addresses: 1) what, if any, antecedents or consequences affect/control a behavior, 2) whether behavior represents a deficit or excess, or is situationally inappropriate, 3) whether different patterns occur in different situations, 4) possible schedule of reinforcement effects.

Functional Assessment examples: Systematic Manipulation of Variables: Functional Analysis of Behavior Interviews: Functional Assessment Interview Contextual Assessment Inventory

#5 -Informed Consent Written informed consent (or documented verbal consent until written consent can be obtained) must be obtained from the individual, if competent, or the individual’s guardian before the use of any psychotropic medication and must be periodically renewed.

#5 -Informed Consent If not competent, the individual must be included to the degree possible. Information must be presented orally, in writing, in layperson’s terms, in an educational manner, and in a manner ensuring communication.

#5 -Informed Consent Informed consent does not have to be obtained before the emergency use of psychotropic medication, provided the facility has obtained general consent for medical emergencies.

#5 -Informed Consent As long as the guardian has provided written informed consent, the appropriate use of psychotropic medication should not be affected by a guardian who will not return telephone calls or attend properly announced reviews. The time interval for renewing informed consent depends on the individual treatment phase, but is at least once per year or anytime the risk: benefit ratio changes.

#5 -Informed Consent Information provided to the person/guardian includes: 1) 2) 3) 4) 5) 6) 7) 8) Diagnosis or hypothesis Signs or symptoms expected to be changed How they will be monitored Proposed medication Risks and side effects (get website) An explanation of right to refuse treatment An explanation of right to change one’s mind Identity of the medication prescriber and how to contact them.

#6 -Index Behaviors and Empirical Measurement Index behaviors & quality of life outcomes must be: 1) objectively defined 2) and tracked using an empirical measurement method(s) in order to evaluate and monitor psychotropic medication efficacy.

#6 -Index Behaviors and Empirical Measurement Index behaviors are also referred to as “target behaviors, ” “signs, ” (observable evidence) or “symptoms” (subjective sensations reported by the patient).

#6 -Index Behaviors and Empirical Measurement Recognized empirical measurement methods include one or more of the following: • frequency count, • duration recording, • time sample, • interval recording, • permanent products, and • rating scales as well as • other information and the • subjective observations of an individual who has the ability to provide such information.

#6 -Index Behaviors and Empirical Measurement A baseline quantification must occur before the non emergency initiation or addition of any psychotropic medication. Although a baseline period will vary depending on the severity of the situation, a reasonable period is 2 to 4 weeks.

#6 -Index Behaviors and Empirical Measurement must occur on an ongoing (not necessarily daily) and consistent basis after the initiation of any psychotropic medication, especially before and after any dose or drug change.

#7 -Side Effects Monitoring The individual must be monitored for side effects on a regular and systematic basis using an accepted methodology which includes a standardized assessment instrument.

#7 -Side Effects Monitoring Regular basis means every person receiving drug therapy must be assessed: • at least once every 3 -6 months and • after initiation of a new psychotropic medication. Systematic basis means some coordinated procedure to conduct, review, record, and act on assessment information.

#7 -Side Effects Monitoring A standardized assessment instrument is used in addition to any recommended physiological laboratory assessment, e. g. lithium level, white blood cell count, etc. Standardized assessment instruments mean: 1) A published or recognized scale 2) A checklist constructed from standard pharmaceutical or medical references. A direct examination should accompany the use of the assessment instrument.

#8 -Tardive Dyskinesia Monitoring If antipsychotic medication or other dopamine-blocking drugs are prescribed, the individual must be monitored for tardive dyskinesia on a regular and systematic basis using a standardized assessment instrument.

#8 -Tardive Dyskinesia Monitoring Tardive dyskinesia (TD) is a side effect of antipsychotic medication and metoclopramide (Reglan). The early detection of TD is critical to maximize the chances for reversal and to minimize its impact for individuals for whom long-term antipsychotic medications continues to be necessary.

#8 -Tardive Dyskinesia Monitoring A standardized assessment instrument means: • Monitoring on a regular basis means at least one every 6 months. the use of a published or recognized scale, such as the AIMS, DISCUS, TDRS, or TRIMS. • Systematic basis mean some coordinated procedure to conduct, review, record, and act on assessment information.

#8 -Tardive Dyskinesia Monitoring If a TD causing drug is discontinued, assessments should occur 1 and 2 months after discontinuation to check for withdrawal TD.

#9 -Regular and Systematic Review Psychotropic Medication must be reviewed on a regular and systematic basis.

#9 -Regular and Systematic Review The review schedule should be outlined in the care plan. Regular means at least once every 3 months and within 1 month of drug or dose changes. Systematic review means a coordinated procedure between all parties to: 1) share, review, document, and act on information such as index behavior, quality of life, and side effects data and 2) communicate drug, dose, and non-pharmacological changes.

#9 -Regular and Systematic Review Clinical Review: The prescriber must see the individual at each clinical review. Data Reviews: Appropriate team members may vary depending on factors such as the setting, case, and type of review. May be done via telephone, reports, etc.

#10 -Lowest Optimal Effective Dose Psychotropic medication must be reviewed on a periodic and systematic basis to determine whether it is still necessary or, if it is, whether the lowest optimal effective dose is prescribed.

#10 -Lowest Optimal Effective Dose Lowest optimal effective dose (OED) means the least amount of medication required to improve or stabilize the problem. If several psychotropic medications are prescribed, it may be possible to reduce the number of drugs, although a medicationfree status is not possible.
#10 -Lowest Optimal Effective Dose Periodic means every medication review with in-depth risk: benefit analysis provided at least once per year Systematic means a review of variables such as the 1) views of the individual/guardian 2) pattern of index behavior and quality of life data, 3) results of previous properly conducted reductions, 4) comparison of current drugs and dose levels to norms appropriate for the age group, population, diagnosis and treatment phase, 5) new variables since drug initiation or last reduction attempt, 6) current drugs and dose levels compared to previous levels.

#10 -Lowest Optimal Effective Dose Although there are exceptions, most reductions to determine the lowest OED must be gradual in nature including the dose amount and the length of time at dose level. An annual reduction does NOT need to occur, but review and justification as to the reasons must occur.

#11 -Frequent Changes Frequent drug and dose changes should be avoided.

#11 -Frequent Changes Medications can take varying times to work, e. g. antidepressant drugs may take 2 -8 weeks before the full effect is seen. Drugs and doses should not be changed in a reactive manner to index behavior fluctuation, without consideration of the disorder being treated, or simply for change’s sake.

#13 -Practices to Minimize Longterm use of PRN orders. Long-term is more than a few weeks. PRN orders should be reserved for behavior that occurs sporadically, or unpredictably and does not abate quickly. Regular use of a PRN beyond a few weeks indicates a need to consider an environment al cause or to review the treatment plan. This does not mean the practice may not help a specific individual.

#13 -Practices to Minimize Long-term use of benzodiazepine anti anxiety medications, such as diazepam (Valium). Longterm is more than 3 months. Long-term use of these may lead to diminishing effectiveness, tolerance, and pronounced withdrawal reactions.

#13 -Practices to Minimize Use of long-acting sedative hypnotic medications, such as chloral hydrate. These are associated with behavioral disinhibition (sudden worsening of behavior) in persons with developmental disabilities.

#13 -Practices to Minimize Long-term use of shorteracting sedativehypnotics, such as temazepam (Restoril) Long-term is more than 14 days. This does not mean longer use may not be necessary in some cases. Although preferred over longer-acting sedative hypnotics, it is generally recommended to avoid the longterm use of any sedative hypnotic medication if possible.

#13 -Practices to Minimize Anticholinergic use, such as benztropine (Cogentin), without signs of extra pyramidal side effects (EPSE). Anticholinergic medication is associated with unpleasant side effects such as dry mouth, constipation, blurred vision, and urinary retention; memory loss; and other disadvantages such as cognitive disturbance. Although, prophylactic use may be necessary in some cases.

#13 -Practices to Minimize Long-term use of anticholinergic medication. Long-term is more than 3 -6 months. Long-term may be necessary in some cases. Anticholinergic medication may no longer be required • as the body adapts to EPSE or • when lower antipsychotic medication maintenance levels are reached.

#13 -Practices to Minimize Use of antipsychotic medication at high doses, e. g. above typical package insert maintenance dose range. This does not mean some persons may not respond to high doses, however, this must be empirically demonstrated. Individuals who require high-dose therapy should not be under medicated, but close review of such cases should occur because high doses are generally not required on a longterm basis and may increase the risk of side effects.

#12 -Polypharmacy Keep psychotropic medication regimens as simple as possible in order to enhance compliance and minimize side effects.

#12 -Polypharmacy Intraclass polypharmacy (the use of two psychotropic medications from the same therapeutic class at the same time) should be avoided. Is also referred to as “duplicate therapy. ” There may be infrequent exceptions.

#12 -Polypharmacy Interclass polypharmacy (the use of 3 or more psychotropic medications from different therapeutic classes at the same time). There may be exceptions… …such as during the period when a new drug is being added and a prior one is being eliminated.

Let’s look at some examples of each.
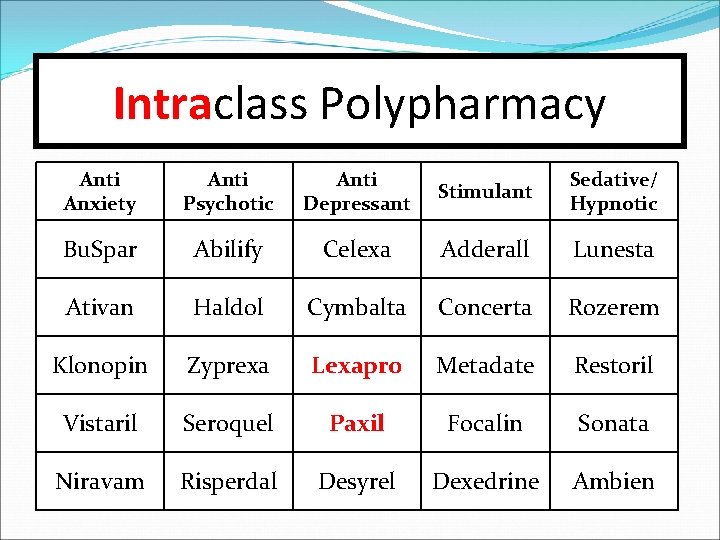
Intraclass Polypharmacy Anti Anxiety Anti Psychotic Anti Depressant Stimulant Sedative/ Hypnotic Bu. Spar Abilify Celexa Adderall Lunesta Ativan Haldol Cymbalta Concerta Rozerem Klonopin Zyprexa Lexapro Metadate Restoril Vistaril Seroquel Paxil Focalin Sonata Niravam Risperdal Desyrel Dexedrine Ambien
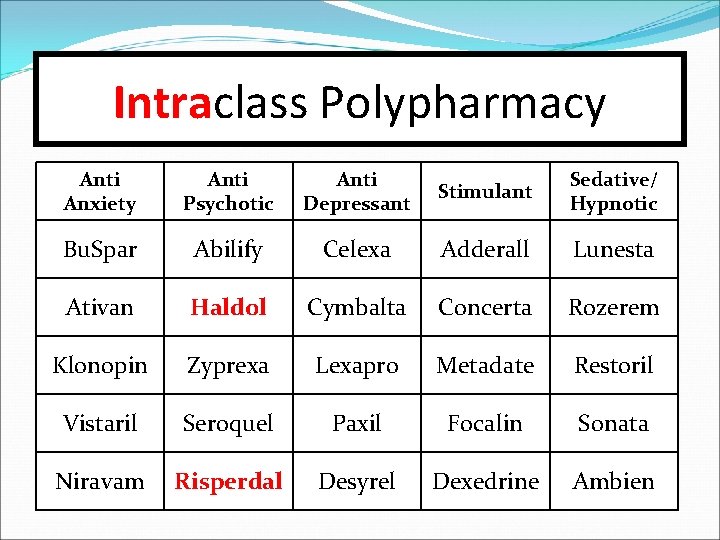
Intraclass Polypharmacy Anti Anxiety Anti Psychotic Anti Depressant Stimulant Sedative/ Hypnotic Bu. Spar Abilify Celexa Adderall Lunesta Ativan Haldol Cymbalta Concerta Rozerem Klonopin Zyprexa Lexapro Metadate Restoril Vistaril Seroquel Paxil Focalin Sonata Niravam Risperdal Desyrel Dexedrine Ambien
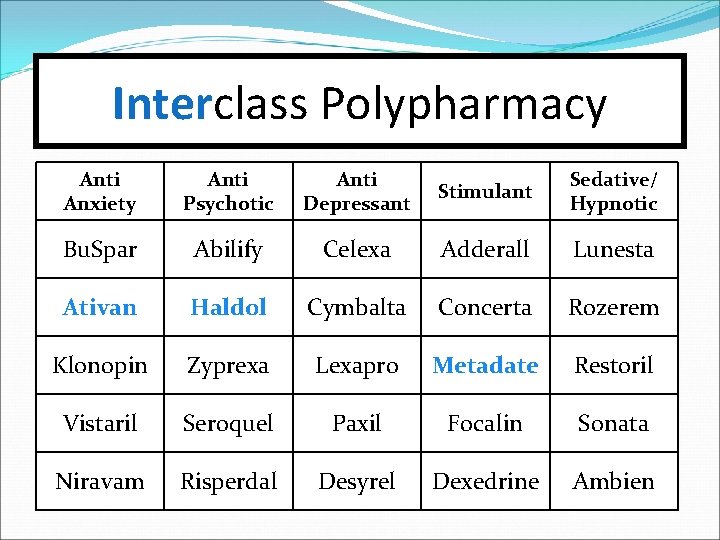
Interclass Polypharmacy Anti Anxiety Anti Psychotic Anti Depressant Stimulant Sedative/ Hypnotic Bu. Spar Abilify Celexa Adderall Lunesta Ativan Haldol Cymbalta Concerta Rozerem Klonopin Zyprexa Lexapro Metadate Restoril Vistaril Seroquel Paxil Focalin Sonata Niravam Risperdal Desyrel Dexedrine Ambien
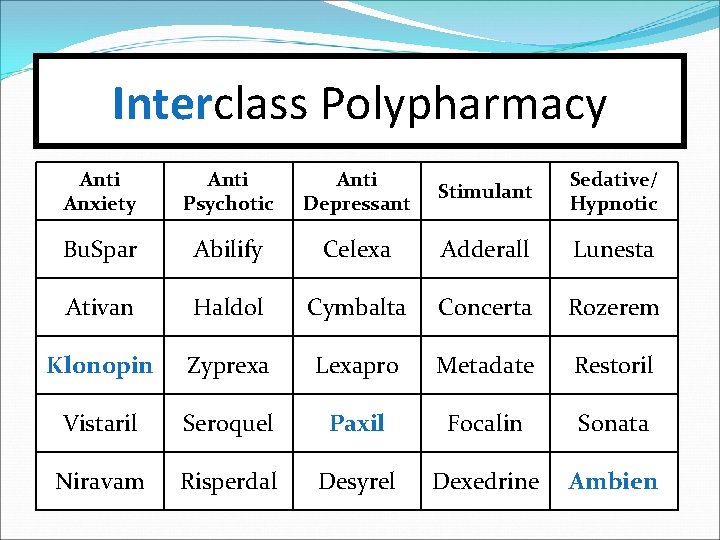
Interclass Polypharmacy Anti Anxiety Anti Psychotic Anti Depressant Stimulant Sedative/ Hypnotic Bu. Spar Abilify Celexa Adderall Lunesta Ativan Haldol Cymbalta Concerta Rozerem Klonopin Zyprexa Lexapro Metadate Restoril Vistaril Seroquel Paxil Focalin Sonata Niravam Risperdal Desyrel Dexedrine Ambien

Chapter VI Pathways to and from Polypharmacy “…major clinical pitfalls that contribute to unnecessary psychiatric polypharmacy…. ”

#1 -Failure to Determine Efficacy “In my experience, a primary contributor to the use of multiple psychopharmacological agents in individuals with ID is the failure to empirically determine the efficacy for existing medication before adding additional agents. ”
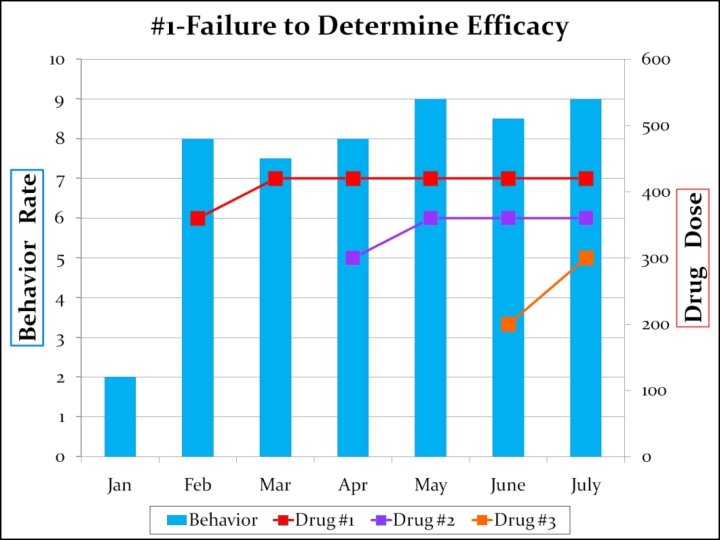

#1 -Failure to Determine Efficacy “It is difficult to imagine how an individual could be receiving 4, 5, or more psychotropic medications and still be exhibiting high rates of aggression and/or selfinjurious behavior if they were all effective for the individual’s underlying disorder. ” Chapter 3 identifies statistical methods to go about challenging the efficacy of medication. These methods are beyond the scope of this presentation. However, advocates can easily inquire from the prescriber, about how this may apply to any person(s) to which services are being provided.

#2 -Reluctance to Accept a Partial Response “In most cases, the symptoms of major mental illness will diminish when the appropriate psychotropic medication is utilized, but the symptoms will NOT entirely disappear. ”
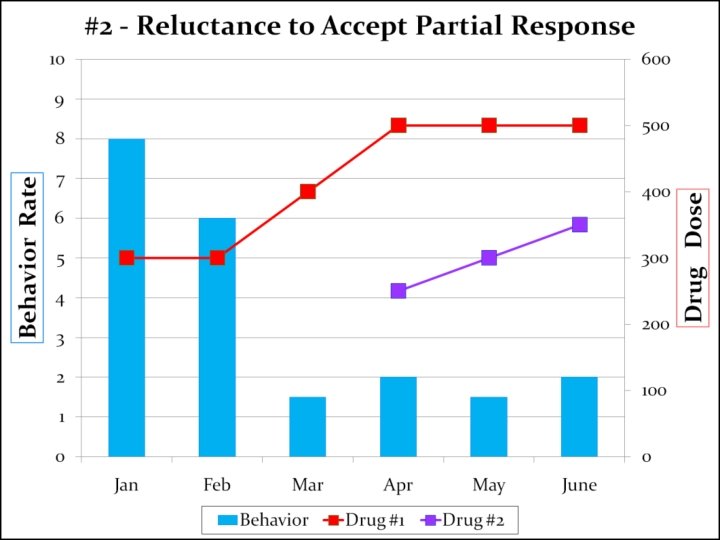

#2 -Reluctance to Accept a Partial Response “…clinical teams often do not appreciate the chronicity of these disorders and may advocate for additional medications in the belief that the total eradication of symptoms is possible. ”

#3 -Bipolar “The diagnostic hallmark of bipolar disorder is a significant change in mental status involving periods of euthymia, depression, and mania or hypomania. This fluctuating course can easily contribute to polypharmacy. ” “…manic-depressive illness …rarely goes into complete remission as a result of pharmacological treatment. ”
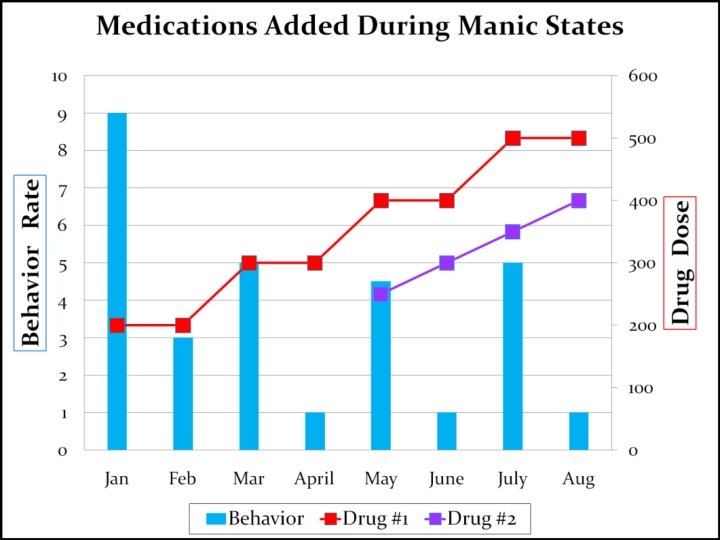

#3 -Bipolar “If an individual with this diagnosis ceases to manifest any symptoms of their cyclical disorder, it is probably more likely that there has been a spontaneous remission of the disorder. ”

#3 -Failure to Distinguish Between Signal and Noise “…a failure to distinguish between signal and noise can lead the clinical team to respond to “blips” and “clusters” of behavior as if they represented a significant trend that could represent a change in the underlying disorder. “ Signal (trend) = steady increase or decrease in the frequency of a monitored symptomatic behavior that occurs over a period of several weeks or months. Noise (blips) = a noticeable change in frequency which occurs for no observable reason and is transient.
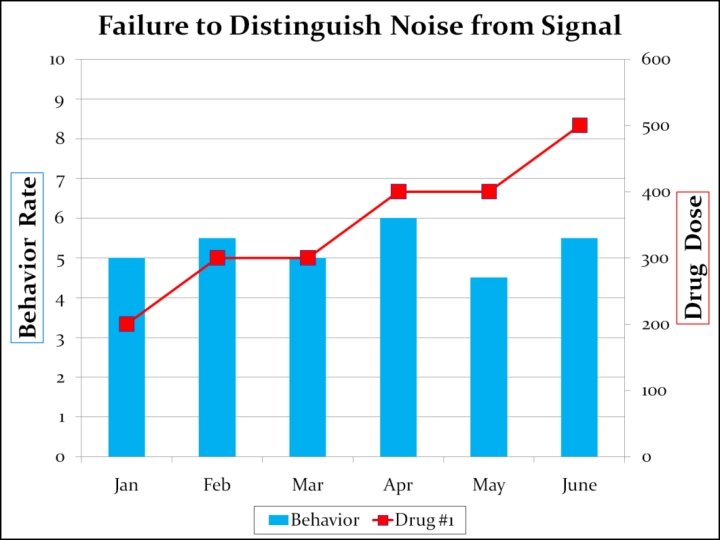

#3 -Failure to Distinguish Between Signal and Noise Mikkelsen’s remedy for this type of error is to develop a data collection system that provides a lengthy historical perspective, specifically one that identifies the degree of variation that has occurred in the past.

#4 -Failure to Address Environmental Issues “Turning a blind eye to environment factors and/or failing to fully investigate them before prescribing psychotropic medication will only perpetuate the problem. ”

#4 -Failure to Address Environmental Issues “You cannot solve fundamentally flawed environmentally precipitated behavior problems with psychotropic medications. ” What the prescriber should know: • Number of housemates with which that the person lives • Characteristics of those people • Size and/or configuration of the person’s home • Staff ratios and rate of staff turnover Is a team member who knows the person well present?

#5 -Failure to Reassess the Psychiatric Diagnosis �…physicians frequently formulate their diagnosis quickly and on relatively little clinical information. � A cognitive bias is then formed. �This leads to the exclusion or minimization of symptoms and other data that would contraindicate the original diagnosis. This process contributes to polypharmacy, as it leads to the implementation of psychopharmacological interventions that may not be effective. The problem is then compounded by the addition of subsequent multiple medications from the same class, rather than a reevaluation of the validity of the psychiatric diagnosis.

#6 Inaccurate or Biased Reporting of Data “If a clear, concise visual presentation of the behavioral data is not available, the prescriber may default to an acceptance of the subjective opinion of whichever staff member happens to accompany the patient on that day. ”
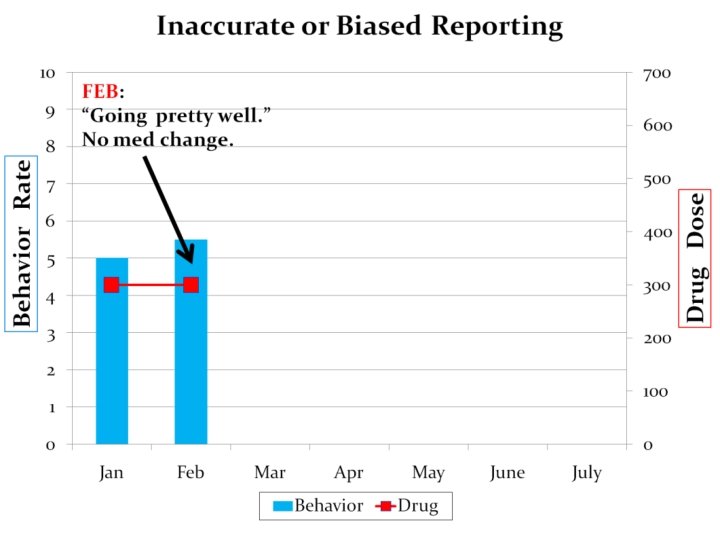
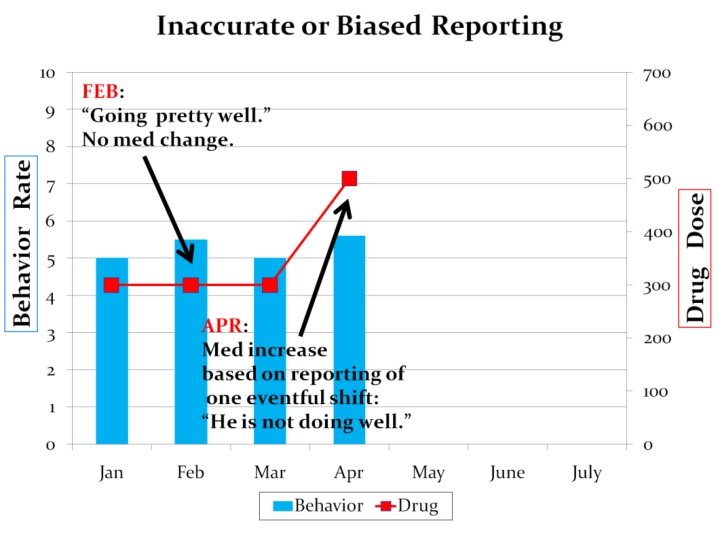
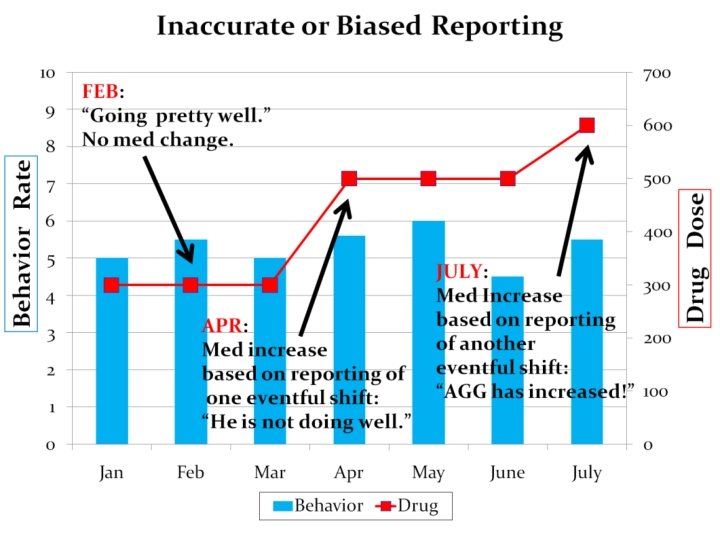

#5 Inaccurate or Biased Reporting of Data Provide the medication prescriber the information she needs in a straight forward manner that is easy to interpret: Medication History Chart
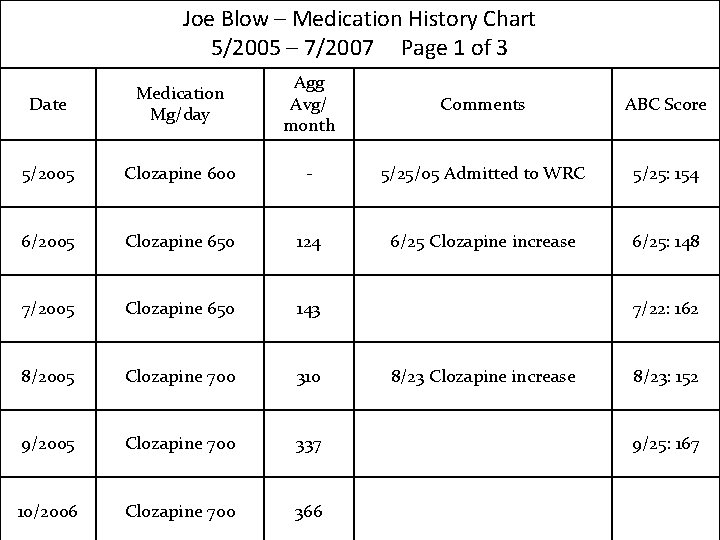
Joe Blow – Medication History Chart 5/2005 – 7/2007 Page 1 of 3 Date Medication Mg/day Agg Avg/ month Comments ABC Score 5/2005 Clozapine 600 - 5/25/05 Admitted to WRC 5/25: 154 6/2005 Clozapine 650 124 6/25 Clozapine increase 6/25: 148 7/2005 Clozapine 650 143 8/2005 Clozapine 700 310 9/2005 Clozapine 700 337 10/2006 Clozapine 700 366 7/22: 162 8/23 Clozapine increase 8/23: 152 9/25: 167
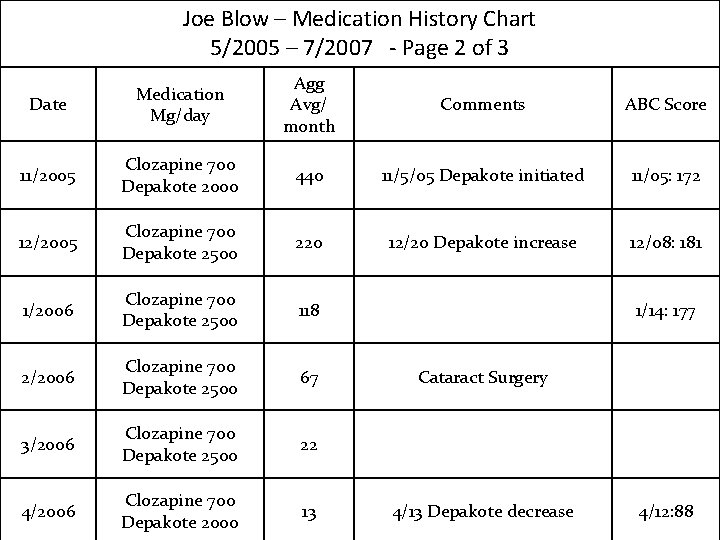
Joe Blow – Medication History Chart 5/2005 – 7/2007 - Page 2 of 3 Date Medication Mg/day Agg Avg/ month Comments ABC Score 11/2005 Clozapine 700 Depakote 2000 440 11/5/05 Depakote initiated 11/05: 172 12/2005 Clozapine 700 Depakote 2500 220 12/20 Depakote increase 12/08: 181 1/2006 Clozapine 700 Depakote 2500 118 2/2006 Clozapine 700 Depakote 2500 67 3/2006 Clozapine 700 Depakote 2500 22 4/2006 Clozapine 700 Depakote 2000 13 1/14: 177 Cataract Surgery 4/13 Depakote decrease 4/12: 88
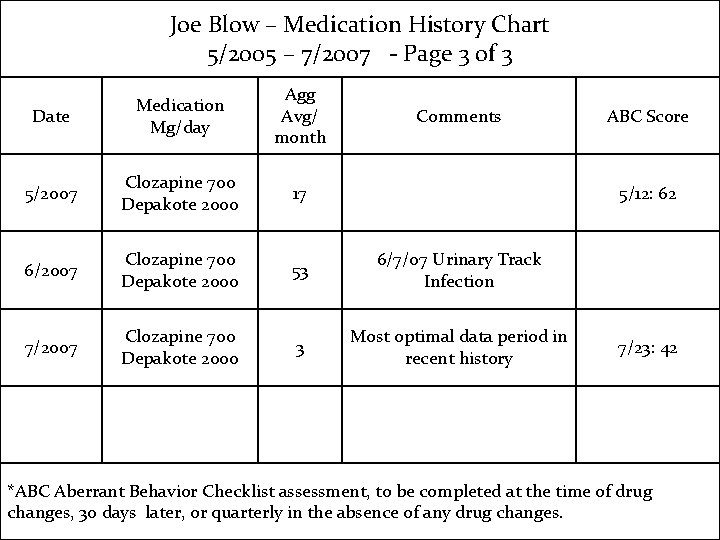
Joe Blow – Medication History Chart 5/2005 – 7/2007 - Page 3 of 3 Date Medication Mg/day Agg Avg/ month 5/2007 Clozapine 700 Depakote 2000 17 6/2007 Clozapine 700 Depakote 2000 53 6/7/07 Urinary Track Infection 7/2007 Clozapine 700 Depakote 2000 3 Most optimal data period in recent history Comments ABC Score 5/12: 62 7/23: 42 *ABC Aberrant Behavior Checklist assessment, to be completed at the time of drug changes, 30 days later, or quarterly in the absence of any drug changes.

Take Home Message: Be familiar with these guidelines. Consider how they apply to the persons you serve. Provide the prescriber with information that will allow him/her to make data based decisions. .
- Slides: 88