Psychotherapy BORDERLINE PERSONALITY DISORDER A PSYCHOLOGICAL PERSPECTIVE Borderline

Psychotherapy BORDERLINE PERSONALITY DISORDER: A PSYCHOLOGICAL PERSPECTIVE

Borderline Personality Disorder: A Psychological Perspective Aims and Objectives (from handbook) • Understand emotionally unstable personality disorder from a psychological /psychotherapy perspective. • To gain a more detailed understanding of at least one of the newer therapy approaches to EUPD.

BPD: A Psychological Perspective To achieve this • • • Case Presentation Journal Club 555 Presentation Expert-Led Session MCQs • Please sign the register and complete the feedback

BPD: A Psychological Perspective Expert Led Session Borderline Personality Disorder: A Psychological Perspective Author: Dr. Adam Dierckx Consultant Medical Psychotherapist

OVERVIEW • • • Personality and PD BPD – background Aetiology NICE Guidance Treatment approaches Clinical traps and tips

PERSONALITY • Self vs • Personality – Self as organizing principle for personality traits or – Self = subjective (how we see ourselves) – Personality = objective (how others see us) • Traits / Dimensions cf. Categories

PERSONALITY DISORDER • Intrapersonal – What goes on inside – e. g. affect regulation • Interpersonal – Between people – e. g. conflict, dependence • Social – Within society – i. e how you fit in and adapt • You can’t have PD on a desert island!
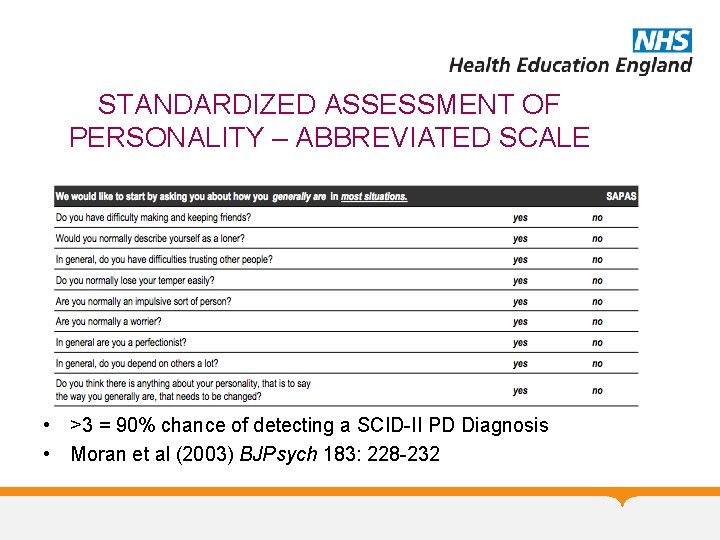
STANDARDIZED ASSESSMENT OF PERSONALITY – ABBREVIATED SCALE • >3 = 90% chance of detecting a SCID-II PD Diagnosis • Moran et al (2003) BJPsych 183: 228 -232

PD DIAGNOSIS: DSM-5 • A: Personality Dysfunction – Self function (Identity &/or self-direction) AND – Interpersonal (empathy &/or intimacy) • B: Pathological Personality Traits • C: A&B stable across time and situations • D: Not normative for development or culture • E: Not due to substances or physical illness

DSM CLUSTERS • Cluster A: Odd / Eccentric • Cluster B: Dramatic / Erratic • Cluster C: Dependent

SEVERITY • Tyrer & Johnson (1996) Am. JPsych 153: 1593 -7 • • • 0 = No PD 1 = Personality Difficulty (PD traits only) 2 = Simple (1 or more PD in same cluster) 3 = Complex (>1 cluster) 4 = Severe (ASPD + another cluster)

BPD DIAGNOSIS: DSM-5 • A: Personality Dysfunction – Self function (Identity &/or self-direction) AND – Interpersonal (empathy &/or intimacy) • B: Pathological Personality Traits – Negative Affectivity – Disinhibition – Antagonism

BORDERLINE PD: DSM-IV • • • Intense anger Unstable mood Chronic emptiness Unstable self-image Paranoia & suspicion • • Feeling abandoned Suicidal & DSH Impulsive acts Intense & unstable relationships

BPD: EPIDEMIOLOGY • Prevalence – ΨIP 15 -25% > ΨOP 10% > GP 7 -8% > Gen pop ½ -5% • Gender: M=F – No supporting evidence for gender difference – Social construct: • Male BPD ASPD diagnosis • Female ASPD BPD diagnosis • Co-morbidity – 85% have Axis I diagnosis (40% have PTSD) – 75% have another Axis II diagnosis
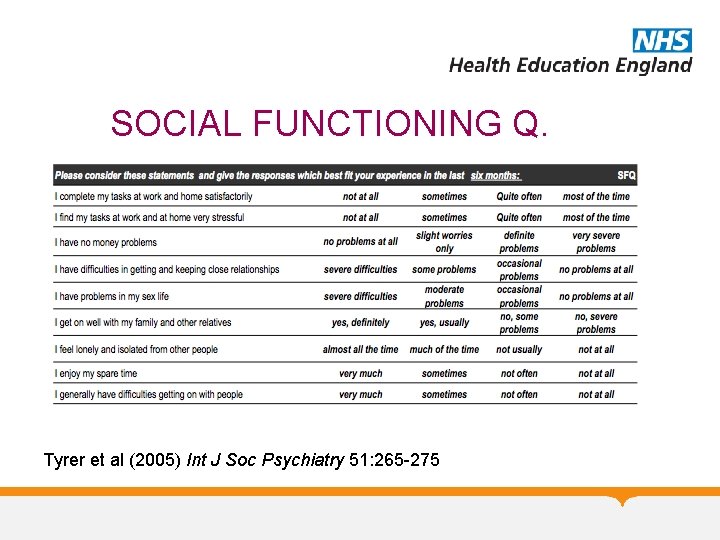
SOCIAL FUNCTIONING Q. Tyrer et al (2005) Int J Soc Psychiatry 51: 265 -275

BPD: PROGNOSIS • Untreated – Remitting – up to 80% diagnosis free by 10 y – Remission unaffected by co-morbid MDD • [MDD prognosis is adversely affected by co-morbid BPD] • Treatment as usual – Terrible prognosis – up to lifelong – Prolonged admission increases recovery time – Mortality by suicide 8 -10% • Specialist intervention – More rapid remission – Remission / recovery maintained
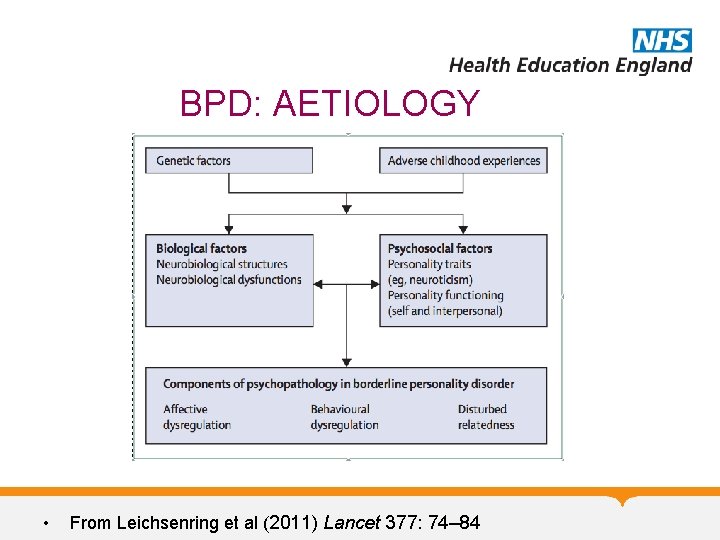
BPD: AETIOLOGY • From Leichsenring et al (2011) Lancet 377: 74– 84

NEUROBIOLOGICAL THEORIES • • • Genetic Factors Primary emotions: Panksepp Autonomic Dysregulation Hypothalamic-Pituitary-Adrenocortial upregulation Amygdala Pre-frontal – limbic pathways

PSYCHOLOGICAL THEORIES • • Cognitive Psychodynamic Attachment Mentalizing

COGNITIVE BEHAVIOURAL THEORY • Early Maladaptive Schema – broad and pervasive themes or patterns made up of memories, feelings, sensations, and thoughts – regarding oneself and one's relationships with others – develop during childhood or adolescence – dysfunctional in that they lead to self-defeating behavior. – E. g. abandonment/instability, mistrust/abuse, emotional deprivation, and defectiveness/shame

PSYCHODYNAMIC CONCEPTS • • • Projection Idealization / Denigration Splitting Projective identification Envy Acting Out

PSYCHODYNAMIC ‘SCHOOLS OF THOUGHT’ • Object Relations Theory • Kernberg: ‘Borderline Personality Organization’ • Kohut: Self Psychology • Group Dynamic theory – Foulkes – Nitsun’s ‘Anti-group’

ATTACHMENT THEORY

THE ATTACHMENT SYSTEM • Universal human need to form close affectional bonds • Extended period of immaturity attachment as a behavioural system triggered by fear to ensure the safety of offspring. • Reciprocity: attachment behaviours of infants are reciprocated by adult caregiving behaviours creates attachment to particular adult.
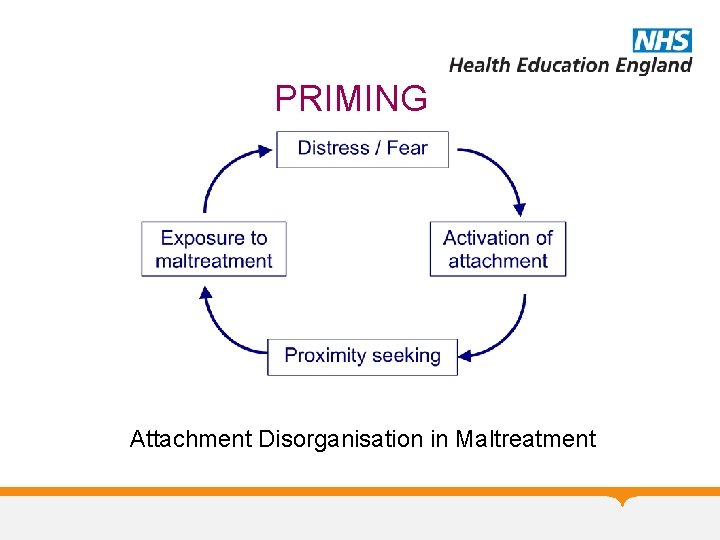
PRIMING Attachment Disorganisation in Maltreatment

EFFECT OF ATTACHMENT TRAUMA • Undermines capacity to think about mental states in oneself and others – Effects on narrative capacity – Poor identification of mental states associated with facial expression

EFFECT OF ATTACHMENT TRAUMA (2) • Defensive inhibition of thinking about mental states in face of genuine malevolence • Trauma arouses attachment, attachment trauma does so chronically • Early excessive stress distorts function of arousal mechanisms inhibiting mentalizing so they trigger at lower levels of risk

DSM CLUSTERS • Cluster A: Odd / Eccentric • Move away • Cluster C: Dependent • Move towards • Cluster B: Dramatic / Erratic • Move against

HYPERACTIVE ATTACHMENT • We assume the attachment system in BPD is “hypersensitive” (triggered too readily) • Indications of this in core symptoms include: – Frantic efforts to avoid abandonment – Unstable and intense relationships – Rapidly escalating tempo from acquaintance to intimacy

PD: AETIOLOGY • Intrapersonal – Observable neuropsychological dysfunction • Interpersonal – Maladaptive enactment of social self-regulation • Social – Social / species vs. Self preservation • All 3 areas interlink

NICE GUIDANCE: CG 78 • Mostly concern good quality relationships – – Equality of access to services Optimistic, trusting relationships Autonomy & choice Managing endings and transitions • Comments on good quality care – Theoretically coherent and shared framework – Training and support for staff; service planning – CPA, other NICE CG (e. g. Self harm) • Don’t use medication for BPD • Some therapies work, most need more research

PHARMACOTHERAPY • • Not recommended by any guidelines Most BPD patients prescribed antipsychotics Little evidence for effectiveness of medication At best Rx gives improvement in 1 -2 symptom areas • 1 RCT of adjunctive Olanzepine + DBT • Significant SE (e. g. Price et al (2009) BJPsych 195: 211 -217) • Tom Main ‘The Ailment’

PSYCHOLOGICAL THERAPIES • ‘Simple’ BPD get (almost) as much benefit from Structured Clinical Management – therapy doesn’t add much. • ‘Complex’ BPD (co-morbidity, several PDs) benefit from adding PD specific therapy. • ‘Severe’ BPD (extremely chaotic) need SCM to stabilize before having therapy.

PSYCHOLOGICAL THERAPIES • Traditional therapies • Psychodynamic • Cognitive – Behavioural • Milieu / Systemic

PSYCHOLOGICAL THERAPIES • Adapted therapies Mentalization Based Treatment Transference Focused Psychotherapy Cognitive Analytic Therapy Schema Focused Therapy Dialectical Behaviour Therapy Therapeutic Communities Structured Clinical Management *

MENTALIZATION BASED TREATMENT

WHAT IS MENTALIZING? • New word for an ancient concept • Implicitly and explicitly interpreting the actions of oneself and others as meaningful on the basis of intentional mental states – (e. g. desires, needs, feelings, beliefs, & reasons)

WHAT IS MENTALIZING? • • A focus on mental states. Oneself or others. Especially in explaining behaviour. It can be: – Automatic or Controlled – Internal or Externally based – Self or Other orientated – Cognitive or Affective

CHARACTERISTICS OF MENTALIZING • • Central concept is internal states are opaque We make inferences about them But inferences are prone to error Overarching principle is to take the ‘inquisitive stance’ = • Others’ minds may change our own

WHAT IS MENTALIZING? • To see ourselves from the outside and others from the inside • Understanding misunderstanding • Having mind in mind • Past present and future

WHERE DOES MENTALIZING OCCUR? • Pre-frontal cortex • Right hemisphere lateralization (slightly) • Other areas are important – Temporal lobe – Amygdala – Anterior Cingulate Gyrus • Dependant on optimal levels of stimulation

HOW DOES IT DEVELOP? • • • Maternal attunement ‘Discovering’ the infant’s mind Marked mirroring Internalisation Play & Safety = • ATTACHMENT
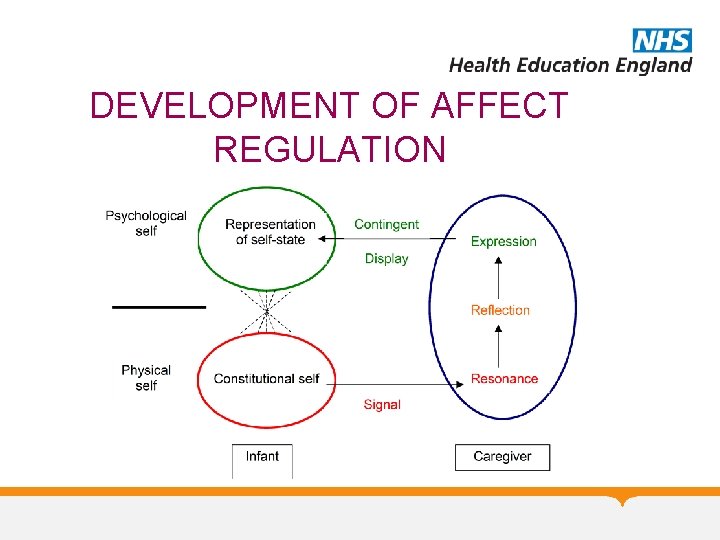
DEVELOPMENT OF AFFECT REGULATION

WHAT STOPS PEOPLE MENTALIZING? • Over-arousal • Past attachment trauma

AROUSAL • Mentalizing systems require optimal levels of arousal. • Too little arousal leads to under-activation of the system and failure to start mentalizing • Excessive arousal leads to over-activation of the system and inhibition of mentalizing

BPD: DISORGANIZED ATTACHMENT Inaccurate judgement of facial affects Delayed theory of mind understanding Failure to understand the situational determinants of emotions

NON-MENTALIZING IN BPD • States of mind that pre-date mentalizing • Psychic Equivalence • Pretend Mode • Teleological Mode

PSYCHIC EQUIVALENCE • Mind-world isomorphism – Mental reality = outer reality – Internal has power of external • Experience of mind can be terrifying • Intolerance of alternative perspectives • Self-related negative cognitions are too real • “Psychic Mode”

PRETEND MODE • Inner and outer reality not linked by ideas • Mental world decoupled from external reality • Linked with emptiness, meaninglessness and dissociation in wake of trauma • Permits DSH & suicide • Endless inconsequential talk in therapy • “Pretend Mode”

TELEOLOGICAL MODE • Expectations concerning the agency of the other are present but are formulated in terms restricted to the physical world • A focus on understanding actions in terms of their physical cf. mental outcomes • Only actions with physical outcomes alter mental states • “Action Mode”

NON-MENTALIZING IN BPD • Psychic Equivalence – If it’s in my mind, that’s the reality of it… • Pretend Mode – Self-report is disconnected from external reality – “In a bubble”, “psychobabble”… • Teleological Mode – It only counts if you do … – Doing that means …

NON-MENTALIZING IN BPD • BPD patients CAN mentalize • Mentalization becomes ‘switched off’ by overarousal in attachment relationships • This is linked to destabilisation of self • When this occurs, pre-mentalizing modes prevail and these determine behaviour • This behaviour has a stabilizing effect on self representation which restores equilibrium

VICIOUS CIRCLE OF NONMENTALIZING • • Over-aroused / intense encounter Poor reality testing e. g. facial expressions Lapse into non-mentalizing state Behaviour that creates reaction in other Other’s non-mentalized actions = iatrogenic Patient’s behaviour deteriorates / escalates Other person even more unable to mentalize

THERAPY IN MBT • Training ground for mentalizing – Mentalizing conditions • Introductory (psycho-education) group • Combined therapy – Individual - intrapsychic – Group - interpersonal

IATROGENIC HARM • Iatrogenic – adj. caused by doctors • • Doctors are human too Acting in a non-mentalizing way Preventing the patient from mentalizing Reinforcing non-mentalizing states

TAU • Treatment as ‘usual’ • The ‘Good Enough’ doctor • Framework for mentalizing – NICE Guidance – Structured Clinical Management • Clinical Skills – Mentalizing – Alert to traps …

TEN TRAPS FOR PD WORKERS • • • Trust Distance Boundaries Limits Responsibility • • • Control Denial Projection Idealization Motivation

ANY QUESTIONS?

TAKE HOME MESSAGE • • • BPD is common and serious Genetic AND environment are important We are potentially keeping people unwell! We can avoid this through psychological psychiatry Basic mental heath skills can make a difference

Psychotherapy: EUPD MCQs 1. The following are symptoms of Emotionally Unstable Personality Disorder (EUPD): A. B. C. D. E. Unstable or unclear self-image Callous unconcern for others Increased impulsivity Intense anger and aggression Unstable and intense relationships

Psychotherapy: EUPD MCQs 1. The following are symptoms of Emotionally Unstable Personality Disorder (EUPD): A. B. C. D. E. Unstable or unclear self-image Callous unconcern for others Increased impulsivity Intense anger and aggression Unstable and intense relationships

Psychotherapy: EUPD MCQs 2. EUPD is group in ‘Cluster B’ of DSM-IV along with: A. B. C. D. E. Antisocial PD Schizotypal PD Narcissistic PD Dependent PD Histrionic PD

Psychotherapy: EUPD MCQs 2. EUPD is group in ‘Cluster B’ of DSM-IV along with: A. B. C. D. E. Antisocial PD Schizotypal PD Narcissistic PD Dependent PD Histrionic PD

Psychotherapy: EUPD MCQs 3. The following have been recommended by NICE in the treatment of EUPD: A. B. C. D. E. Brief Dynamic Psychotherapy Mentalization Based Treatment Mindfulness Based Therapy Olanzepine Dialectical Behaviour Therapy

Psychotherapy: EUPD MCQs 3. The following have been recommended by NICE in the treatment of EUPD: A. B. C. D. E. Brief Dynamic Psychotherapy Mentalization Based Treatment Mindfulness Based Therapy Olanzepine Dialectical Behaviour Therapy

Psychotherapy: EUPD Any Questions? Thank you.
- Slides: 66