Psychosocial outcome following acquired brain injury in adults

Psychosocial outcome following acquired brain injury in adults: a 5 year follow up study Chalotte Glintborg & Tia G. B. Hansen Center for Developmental and Applied Psychological Science

2

Background • Approx. 19, 500 new ABI incidences per year in Denmark • Approx. 125, 000 people in Denmark live with an ABI • Very few longitudinal studies on psychosocial outcome • Much is known about the prevalence of psychological consequences (e. g. depression), but less is known about the long-term course of psychological symptoms.

This study • A longitudinal study of individuals (N=45) with moderate or severe ABI. • Participants acquired an ABI in 2013/2014 and data collection ended spring 2019. • Participants’ wellbeing was evaluated at 3 different time points: 1) at discharge from hospital 2) one-year post injury 3) 5 -year post injury

Data collection • All clients were admitted to the Regional Neuro-Rehabilitation Centre in Northern Denmark between April 2013 and June 2014 and offered to participate. • Time 1: From a total of 64 ABI clients in the relevant time frame, 45 were included in the study. Exclusion reasons: • very severe cognitive impairments (3) • very severe aphasia (3) • only a short observational stay at the center (6) • another diagnosis than ABI (1) • speaking only another language (Arabic) with no translator available (1), • declining to participate in the research project (5). • Clients who agreed to participate did not differ in mean motor and cognitive functions (FIM) from those who declined or were ineligible. 5

• From time 1 to time 2 • Two clients dropped out. • One died and one declined to participate. • From time 2 to time 3 • 18 clients dropped out. • Dropout reasons: • 11 could not be reached by phone or email • 5 declined to participate • 2 declined because of illness in the family. • The remaining 25 participants’ age, gender, diagnosis, hospitalization time and total FIM score at hospitalization and at discharge, did not differ compared to the total sample (Table 1 next slide) 6
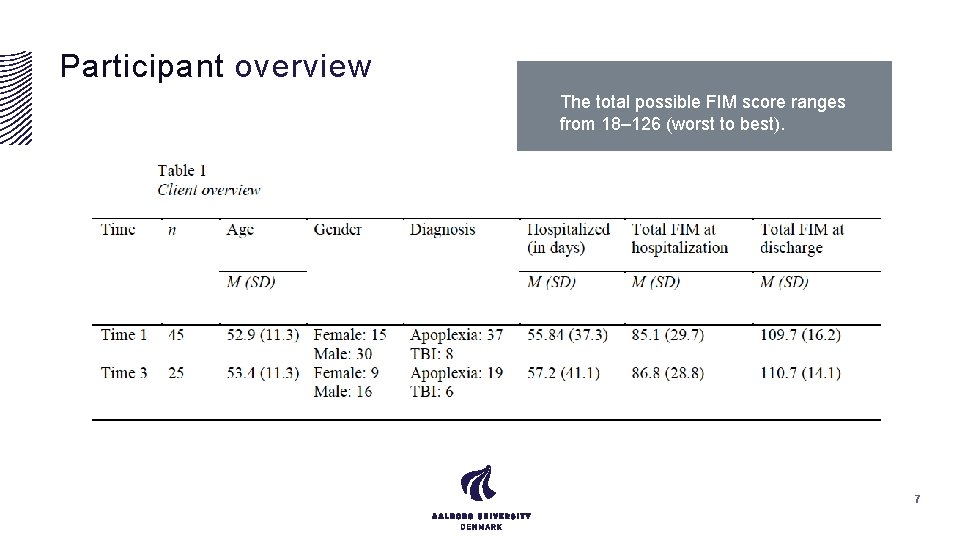
Participant overview The total possible FIM score ranges from 18– 126 (worst to best). 7

Research question Do psychosocial consequences decrease over time? 8

Design Mixed method design: • Multiple measures from more than one source. • A quantitative study of clients’ status at three timepoints: • Depression, Quality of Life, Return to work, Autonomy and Participation • A qualitative study of the clients’ and relatives (will not be presented here) own perspective on the rehabilitation process, based on interviews.

Quantitative measures • Functional Independence Measure (FIM) • Only used to measure motor-functional and cognitive daily life skills at discharge from the Neuro-Rehabilitation Centre. • Quality of Life (WHOQOL-Bref) • Four subscales: physical QOL, psychological QOL, social QOL and environmental QOL (WHO, 1996).

Quantitative measures II • Major Depression Inventory (MDI) • Impact on participation and autonomy questionnaire (IPAQ) • five subscales: “autonomy indoors”, “autonomy outdoors”, “family roles”, “social life and relationships”, and “work and education”). • Return to work • Information given as part of background questionnaire. 11

Analysis • Quantitative analysis • Repeated measures ANOVA with t-test for pairwise comparisons. • Fridman’s Chi-square test when not normal distributed. • Control for missing data bias: Last Observation Carried Forward (LOCF). 12

Results Do psychosocial consequences decrease over time?
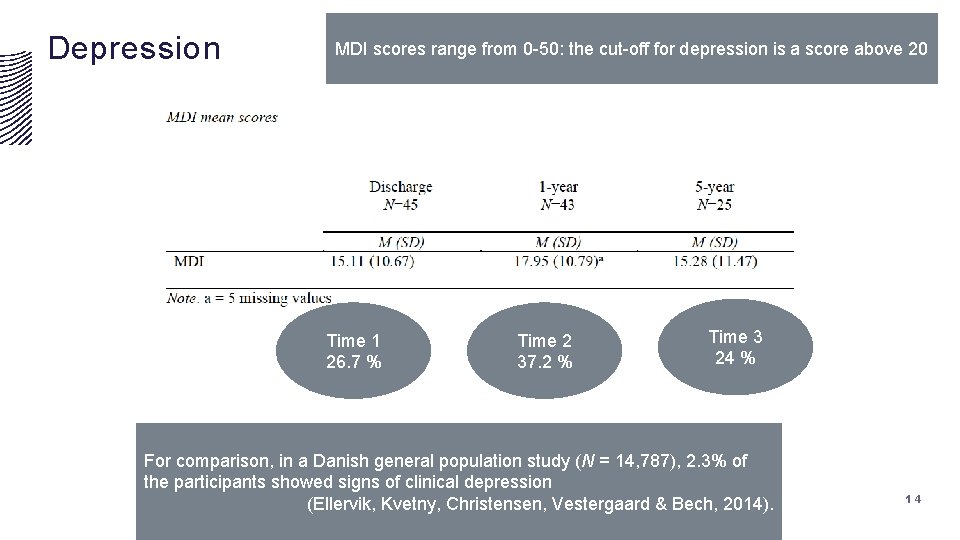
Depression MDI scores range from 0 -50: the cut-off for depression is a score above 20 Time 1 26. 7 % Time 2 37. 2 % Time 3 24 % For comparison, in a Danish general population study (N = 14, 787), 2. 3% of the participants showed signs of clinical depression (Ellervik, Kvetny, Christensen, Vestergaard & Bech, 2014). 14
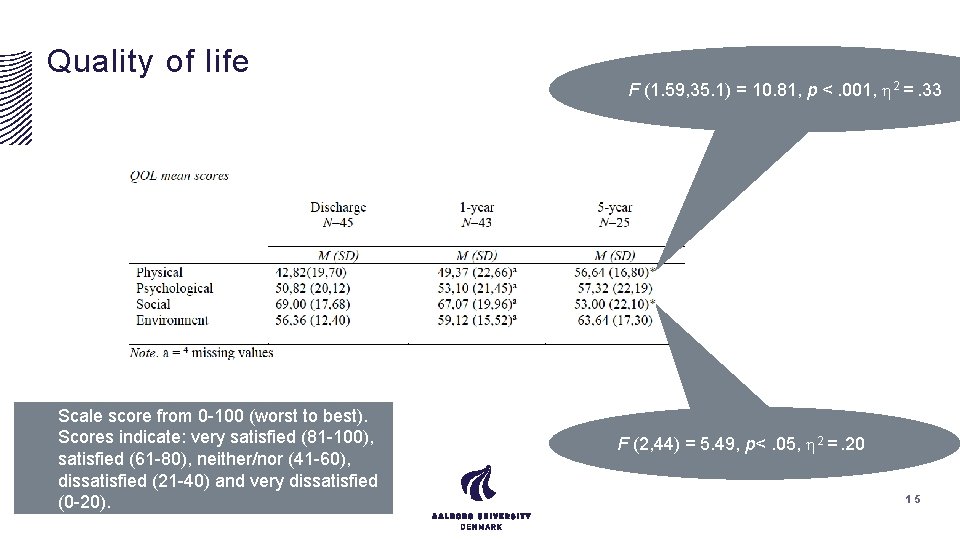
Quality of life Scale score from 0 -100 (worst to best). Scores indicate: very satisfied (81 -100), satisfied (61 -80), neither/nor (41 -60), dissatisfied (21 -40) and very dissatisfied (0 -20). F (1. 59, 35. 1) = 10. 81, p <. 001, 2 =. 33 F (2, 44) = 5. 49, p<. 05, 2 =. 20 15
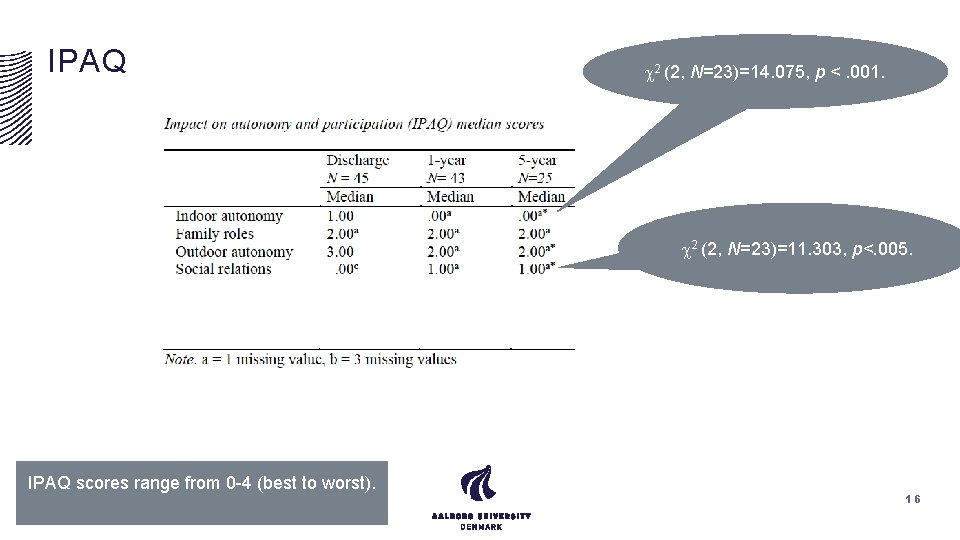
IPAQ 2 (2, N=23)=14. 075, p <. 001. 2 (2, N=23)=11. 303, p<. 005. IPAQ scores range from 0 -4 (best to worst). 16

Participation & Autonomy Four subscales: indoor autonomy, outdoor autonomy, family roles, social relation Challenges in which dimensions • At discharge: Indoor autonomy, outdoor autonomy, and family roles* • At 1 -year follow-up: outdoor autonomy, and family roles • At 5 -year follow-up: outdoor autonomy, family roles, and social relations *Family roles: clients express that they feel different and not able to fulfil the role as a partner or parent anymore.

Return to work • Time 2: 18. 6% had returned to work or education at 1 -year follow-up. • Time 3: 28% had returned to work at 5 -year follow up. • This continuing effort to support clients’ return to work or education can be a result of the new job reform put forward by the Danish Government in 2013. 18

Attrition • To control for attrition, analyses were repeated with N=45 using LOCF. • Results were the same except Social QOL • SOCIAL QOL: For (N = 25) the difference reached statistical significance (p=. 007); for (N = 45 with LOCF) it did not (p=. 078). • Status of all other results remained. • Thus, attrition had neglible impact on results. 19

Main quantitative findings: discussion • Physical QOL increase over time. • Social isolation increases over time • Family roles and identity issues represent a challenge already at discharge and remains a challenge at 5 -year follow up need for identity reconstruction support + family support. • Approx. one third of all clients revels signs of depression at all three timepoints, however, we see an increase from time 1 to 2 after discharge that drops again (time 3). 20

21 Thank you for your attention! cgl@hum. aau. dk
- Slides: 21