Psychosocial Aspects of PCD Tamara Vance MSW LICSW




















- Slides: 25

Psychosocial Aspects of PCD Tamara Vance, MSW, LICSW Anne Griffiths, MD Children’s Minnesota, PCDF Clinical and Research Network Accredited Center

No disclosures. © 2017

Learning Objectives • Present a case highlighting psychosocial needs/interventions • Review mental health issues in chronic medical conditions and impact • Discuss psychosocial issues in PCD patients and caregivers • Share our center’s process and experience screening for anxiety/depression • Future directions for the PCD community © 2017

Case Example: Meet Jack • 14 year old male • Clinical: NRD, chronic sinusitis, OM, bronchiectasis, SA, anxiety, depression • PCD suspected @ age 3, however diagnosis not confirmed until age 12 • Multiple school transfers, 504 plan in place, missed days, homebound program • Nonadherent to PCD medical therapy or psych f/u © 2017

Mental Health Issues in Chronic Medical Conditions • Elevated levels of stress, anxiety and depression found in patients and families with multiple chronic diseases • Chronic medical illness is a risk factor for psychiatric disorders • CF TIDES Study [Quittner, et al. 2014] • Depression: 10% of adolescents, 19% adults, 37% of mothers, 31% of fathers • Anxiety: 22% of adolescents , 32% of adults, 48% of mothers, 36% of fathers • HIGHEST anxiety and depression in CF caregivers increased risk in adolescents © 2017

Mental Health Issues with Chronic Medical Conditions • Increased medical symptoms and diminished health status • Lower health-related quality of life (HRQol) • Increased healthcare costs • Poor treatment adherence and symptom management • Increased hospitalizations © 2017

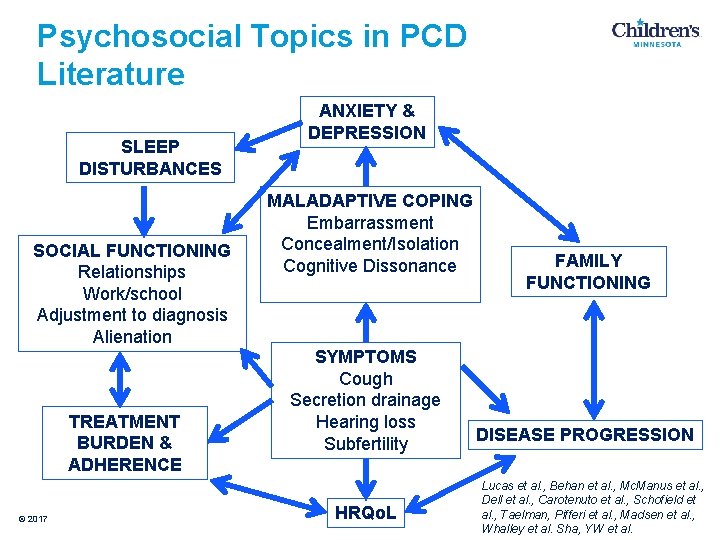
Psychosocial Topics in PCD Literature SLEEP DISTURBANCES SOCIAL FUNCTIONING Relationships Work/school Adjustment to diagnosis Alienation TREATMENT BURDEN & ADHERENCE © 2017 ANXIETY & DEPRESSION MALADAPTIVE COPING Embarrassment Concealment/Isolation Cognitive Dissonance SYMPTOMS Cough Secretion drainage Hearing loss Subfertility HRQo. L FAMILY FUNCTIONING DISEASE PROGRESSION Lucas et al. , Behan et al. , Mc. Manus et al. , Dell et al. , Carotenuto et al. , Schofield et al. , Taelman, Pifferi et al. , Madsen et al. , Whalley et al. Sha, YW et al.

Psychosocial Topics in PCD Parents/Caregivers • Disease inheritance guilt • Grief and fear of future • Isolation due to rare disease and limited community/social media support • Increased anxiety and depression? • No data in PCD • Treatment burden, financial concerns and resources, care coordination • Increased PCD parental distress, parent-child stress • (n=10, Carotenuto 2013) • Stress of family planning • No data in PCD, but common discussion © 2017

Social Work Role in our PCD Center • Member of multidisciplinary team • Ability to see patients outpatient and inpatient • Attend rounds and monthly team meetings to discuss patient needs • Meet with patients annually (minimum) for psychosocial assessment, anxiety/depression screening • Provide ongoing therapeutic services • Provide resources, referrals, and ongoing support to manage care © 2017

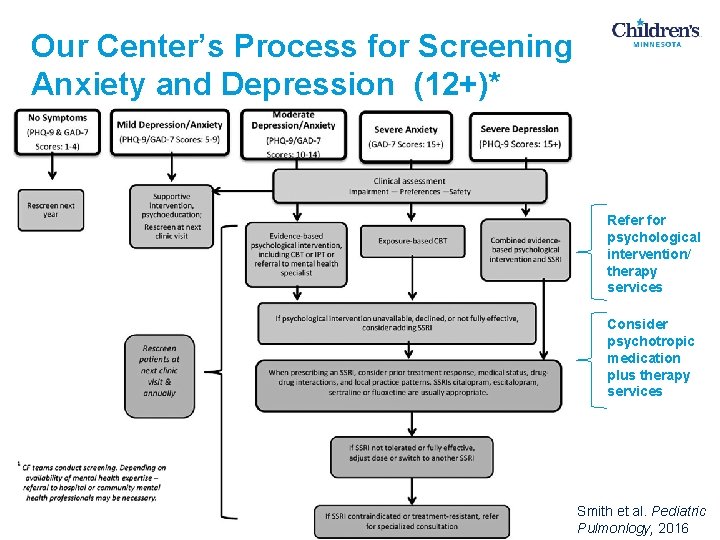
Our Center’s Process for Screening Anxiety and Depression (12+)* Refer for psychological intervention/ therapy services Consider psychotropic medication plus therapy services © 2017 Smith et al. Pediatric Pulmonlogy, 2016

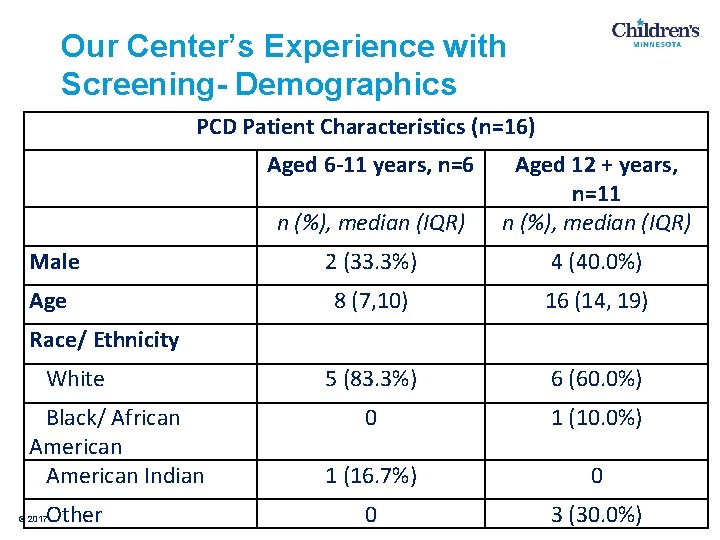
Our Center’s Experience with Screening- Demographics PCD Patient Characteristics (n=16) Aged 6 -11 years, n=6 n (%), median (IQR) Aged 12 + years, n=11 n (%), median (IQR) Male 2 (33. 3%) 4 (40. 0%) Age 8 (7, 10) 16 (14, 19) 5 (83. 3%) 6 (60. 0%) 0 1 (10. 0%) 1 (16. 7%) 0 0 3 (30. 0%) Race/ Ethnicity White Black/ African American Indian Other © 2017

Our Center’s Experience Screening Depression/Anxiety, 6 -11 yo Depression Measures CES-DC % with some depression symptoms present CES-DC score ≥ 15 Aged 6 -11 years, n=6 n (%), median (IQR) 4 (3, 6) 0% Anxiety Measures © 2017 Scared 24 (13, 36) % with some anxiety symptoms present Scared score ≥ 25 3 (50. 0%)

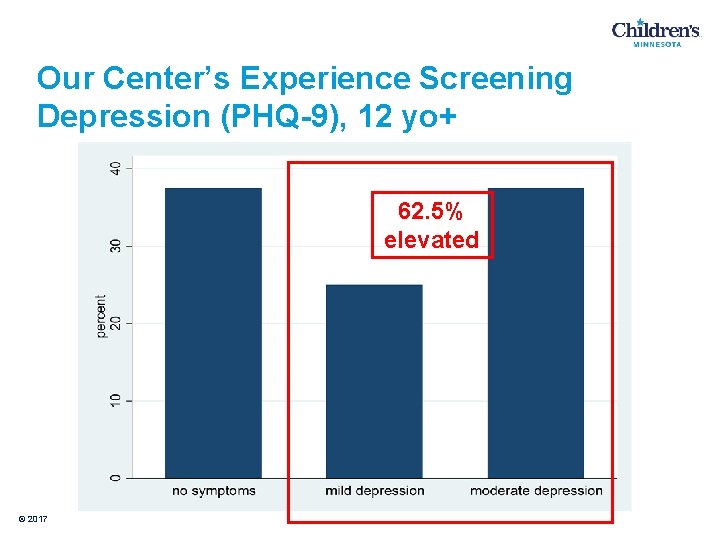
Our Center’s Experience Screening Depression (PHQ-9), 12 yo+ 62. 5% elevated © 2017

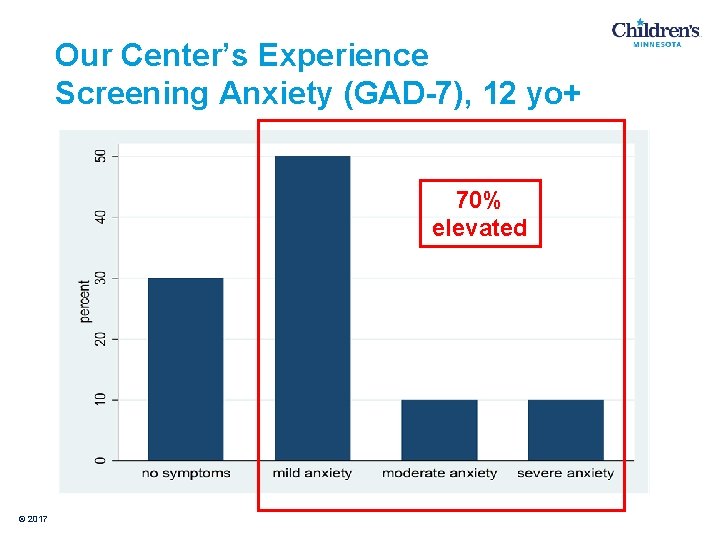
Our Center’s Experience Screening Anxiety (GAD-7), 12 yo+ 70% elevated © 2017

Sleep Disturbance: Somatic Mental Health Symptom or Sleep Apnea in PCD? • Sleep apnea by polysomnogram: highly variable • Santamaria et al: (n=16) all had obstructive sleep apnea (OSA). 19% mild, 50% moderate and 31% severe (by AHI). • All had CRS, FEV 1 103 (58 -117). 2: adenoidectomy, 50% no AH. • Symptoms underestimated by parent questionnaire. • Dehlink E et al: (n=84) 1% moderate OSA, 23% mild • Oktem S et al: (n=29) 52% +OSA (14 mild, 1 moderate) • 37% self-reported as “poor sleepers. ” © 2017

Our Center’s Experience. Sleep/Somatic Overlap, 6 -11 yo Table 1. Summary of Responses to Specific Depression/ Anxiety Scores Related to Sleep Quality in Children Aged 6 -11 years, n=6. Scared Q 2. I get headaches when I’m at school. CES-DC Q 5. I felt like I couldn’t pay attention to what I was doing. CES-DC Q 7. I felt like I was too tired to do things. © 2017 % Answered in affirmative 5 (83. 3%) 1 (16. 7%) 5 (83. 3%) CES-DC Q 11. I didn’t sleep as well as I usually sleep. 0 (0%) CES-DC Q 20. It was hard to get started doing things. 1 (16. 7%)

Our Center’s Experience. Sleep/Somatic Overlap, 12 yo+ Table 2. Summary of Responses to Specific Depression/ Anxiety Scores Related to Sleep Quality in Children Aged 12+ years, n=4 a. PHQ-9 Q 3. Trouble falling asleep or sleeping too much. PHQ-9 Q 5. Feeling tired, or having little energy % Answered in affirmative 4 (100%) 2 (100%), n=2 b PHQ-9 Q 7. Trouble concentrating on things like school work, reading, or watching TV? 3 (75%) GAD Q 5. Being so restless that it is hard to sit still 3 (75%) a. Only 4 patients had complete data (vs. summary scores) for their initial PHQ-9 and GAD assessments b. Two patients did not complete question 5 on the PHQ-9 © 2017

Case Example: Back to Jack • First PCD team meeting with MD, SW, RT, and GC • Medical management adjustments made • Psychosocial assessment completed • GAD 7 and PHQ 9 mental health screens administered: severe anxiety, moderate depression • Returned 1 month: Psychological intervention with PCD SW • Provided referrals for ongoing therapy and med management • Collaborated with school to address needs © 2017

Case Example: Jack today © 2017 • Attending new school that better meets his needs • Reconnected with psychiatrist- on new psychotropic medication • Learned coping skills to better manage PCD, stress and wellness • Anxiety and depression is stable • Engaged with PCD team and adherent to treatment regimen including daily airway clearance and sinus rinses • Increased activity level and social participation • Best FEV 1 !!

Future Directions in PCD • Clinical care • Expand SW role in multidisciplinary team • Assess mental health early therapeutic interventions • Consider impact of family mental health and functioning • Opportunities for research • Further validation of HRQo. L PCD tool in pediatrics • Multicenter evaluation of anxiety & depression: gather data to direct screening recommendations • Further evaluation of sleep, given role in mental health • Role of social media: support and shared experience, driver of care, psychosocial impact? © 2017

Children’s Minnesota PCD Center Pulmonary PCD Center Director and Associate Director: Bill Wheeler and Anne Griffiths Pulmonologists: Cindy Brady, Keith Cavanaugh, Julie Herda, Paul Kubic, Steve Kurachek, John Mc. Namara, Christina Mikesell, Brooke Moore, Mike Pryor, Mike Shreve, and Daniela Zgherea Genetics: Renee Temme Respiratory Therapy: John Plante Pulmonary Diagnostics: Julie Griffin, Kay Kufahl, Katie Johnson Social Worker: Tami Vance RN CNP Center Coordinator: Mary Sachs Patient Care Coordinator: Sarah Bevin © 2017 PCD Nursing Staff: Rachel Scholz and Rachel Barrett Clinical Research: Anne Mills, Elizabeth Thompson, Christine Benoit, and Mike Finch Otolaryngology: Bob Tibesar Pathology: Megan Dishop Specialty Care Division Senior Medical Director: Nancy Mendelsohn Radiology: Bill Mize Neonatology: Jane Barthell, Anastasia Ketko Cardiology: Charles Baker Immunology: Tamara Pozos Adult Pulmonology: Joanne Billings and Jordan Dunitz

References Behan L, Leigh MW, Dell SD, et al. Validation of a health related quality of life instrument for primary ciliary dyskinesia (QOL-PCD). Thorax 2017; 0: 1 -8. doi: 10. 1136/thoraxjnl-2016 -209356 Behan L, et al. The patient’s experience of primary ciliary dyskinesia: a systematic review. Qual Life Res. 30 March 2017 doi: 10. 1007/s 11136 -017 -1564 -y Boat, TF, Filigno, S and RS Amin. Wellness for Families of Children With Chronic Health Disorder. JAMA Pediatr. 2017. doi: 10. 1001/jamapedatrics. 2017. 1682. Carotenuto M, Esposito M, Di Pasquale F, De Stefano S, Santamaria F. Psychological, Cognitive and Maternal Stress Assessment in Children with Primary Ciliary Dyskinesia. World J Pediatr. 2013; 9: 312 -7. Compas, BE, et al. Coping with Chronic Illness in Childhood and Adolescence. Annu Rev Clin Psychol. 2012; 8: 455 -80. Dell SD, et al. Primary Ciliary Dyskinesia: First Health-Related Quality-of-Life Measures for Pediatric Patients. Ann Am Thorac Soc. 2016; 13: 1726 -35. De. Coster, VA. Challenges of type 2 diabetes and role of health care social work: a neglected area of practice. Health Soc Work. 2001; 26: 26 -37. Dehlink E et al. Sleep disordered breathing in children with primary ciliary dyskinesia (PCD). Eur Respir J 016; 48: PA 376. Di. Matteo MR, Lepper HS, and TW Croghan. Depression is a Risk Factor for Noncompliance with Medical Treatment: meta-analysis of the effects of Anxiety and Depression on Patient Adherence. Arch Intern Med. 2000; 160: 2101 -7. Ede LV, et al. Prevalence of depression in patients with chronic obstructive pulmonary disease: a systematic review. Thorax 1999; 54: 688 -92. Garber, J. and Weersing, VR. Comorbidity of Anxiety and Depression in Youth: Implications for Treatment and Prevention. Clin Psychol (New York). 2010 December; 17(4): 293 -306. © 2017

References Hosie P, et al. Primary ciliary dyskinesia: Overlooked and undertreated in children. J Pediatr Child Health. 2014; 50: 952 -8. Katon W, Lin EH and K Kroenke. The Association of Depression and Anxiety with Medical Symptom Burden in Patients with Chronic Medical Illness. Gen Hosp Psychiatry. 2007; 29: 147 -55. Kuehni CE, et al. Factors influencing age at diagnosis of primary ciliary dyskinesia in European children. Eur Respir J. 2010; 36: 1248 -58. Lucas JS, et al. A Quality-of-Life Measure For Adults With Primary Ciliary Dyskinesia: QOL-PCD. Eur Respir J 2015; 46: 375 -83. Mackner LM et al. Psychosocial Issues in Pediatric Inflammatory Bowel Disease: a clinical report of the North American Society for Pediatric Gastroenterology, Hepatology and Nutrition. J Pediatr Gastroenterol Nutr. 2013; 56: 449 -58. Mc. Manus IC, Stubbings GF, & N. Martin. Stigmatization Physical Illness and Mental Health in Primary Ciliary Dyskinesia. J Health Psychol, 2006; 11: 467 -82. Mc. Manus IC, et al. Primary ciliary dyskinesia (Siewert’s / Kartagener’s Syndrome): Respiratory symptoms and psycho-social impact. BMC Pulm Med, 2003; 3: 4 Nathan, AM, et al. Review: Quality of Life in Children with Non-cystic Fibrosis Bronchiectasis. Front. Pediatr. 5: 84. doi: 10. 3389/fped. 2017. 00084. O’Connor MG, et al. Early Diagnosis of Primary Ciliary Dyskinesia: The Role of the Pediatrician. Clin Pediatr. 2017; 1 -4. Oktem S, et al. Sleep disordered breathing in patients with primary ciliary dyskinesia. Pediatr Pulmonol 2013; 48: 897 -903. Pao M and A Bosk. Anxiety in Medically Ill Children/Adolescents. Depress Anxiety. 2011; 28: 40 -9. Pifferi M et al. Health-Related Quality of Life and Unmet Needs in Patients with Primary Ciliary Dsykinesia. Eur Respir J. 2010; 35: 787 -94. © 2017

References Polsky D, et al. Long-term Risk for Depressive Symptoms After a Medical Diagnosis. Arch Intern Med. 2005; 165: 1260 -6. Rich, TA, et al. Comparison of Attitudes Regarding Preimplantation Genetic Diagnosis Among Patients with Hereditary Cancer Syndromes. Fam Cancer. 2014; 13(2)291 -99. Santamaria F, et al. Sleep disordered breathing and airway disease in primary ciliary dyskinesia. Respirology. 2014; 19: 570 -5. Schofield LM and Horobin, HE. Growing up with Primary Ciliary Dyskinesia in Bradford, UK: exploring patients experiences as a physiotherapist. Physiother Theory Pract. 2014; 30(3): 157 -64. Sha YW, Ding L, Li P. Management of primary ciliary dyskinesia/Kartagener’s syndrome in infertile male patients and current progress in defining the underlying genetic mechanism. Asian J Androl 2014; 16: 101 -6. Shapiro et al. Diagnosis, Monitoring, and Treatment of Primary Ciliary Dyskinesia: PCD Foundation Consensus Recommendations Based on State of the Art Review. Ped Pulmonol 2016; 51: 115 -132. Smith BA, Georgiopoulos AM, Quittner, AL. Maintaining Mental Health and Function for the Long Run in Cystic Fibrosis. Pediatr Pulm. 2016; DOI: 10. 1002/ppul. 23522. Smith, BA et al. Depressive Symptoms in Children With Cystic Fibrosis and Parents and Its Effects on Adherence to Airway Clearance. Pediatr Pulm. 2010; 45: 756 -63. Taelman A. , et al. Living with primary ciliary dyskinesia. Eur Respir J 2014; 44: 3676 Quittner AL, Saez-Flores E, Barton JD. The psychological burden of cystic fibrosis. Curr Opin Pulm Med. 2016; 22: 187 -91. Quittner AL, Goldbeck L, et al. Prevalence of Depression and Anxiety in Patients with Cystic Fibrosis and Parent Caregivers: results of The International Depression Epidemiological Study across nine countries. Thorax. 2014; 69: 1090 -7. Wagner EH. The role of patient care teams in chronic disease management. BMJ. 2000; 320: 569 -572. Whalley, S and Mc. Manus, IC. Living with primary ciliary dyskinesia: a prospective qualitative study of knowledge sharing, symptom concealment, embarrassment, mistrust, and stigma. BMC Pulm Med. 2006; 6: 24 © 2017

© 2017