PSYCHOSOCIAL ASPECTS OF LIVING WITH DIABETES MELLITUS BASIS

PSYCHOSOCIAL ASPECTS OF LIVING WITH DIABETES MELLITUS: BASIS FOR AN ENHANCED DIABETIC PROGRAM OF PRIMARY HEALTH CARE IN DOHA, QATAR KHALID ALI SHAMS, MD JOYCE J. ESPINOSA, RN, MAN LUZ L. ROVIRA, RN ALI BADER ALBADER, MD ABDULLA ALNAAMA, MD PERRY PAUL J. ESPINOSA, RN, Ph. D

Background of the Study Diabetes Mellitus (DM) is one of the major health and development challenges of the 21 st century (International Diabetes Association, 2017)

Globally, an estimated 422 million adults were living with diabetes mellitus in 2014, compared to 108 million in 1980. It is expected to reach 438 million by the year 2030, with two-thirds of all diabetes cases occurring in low-tomiddle income countries (International Diabetes Federation, 2017).
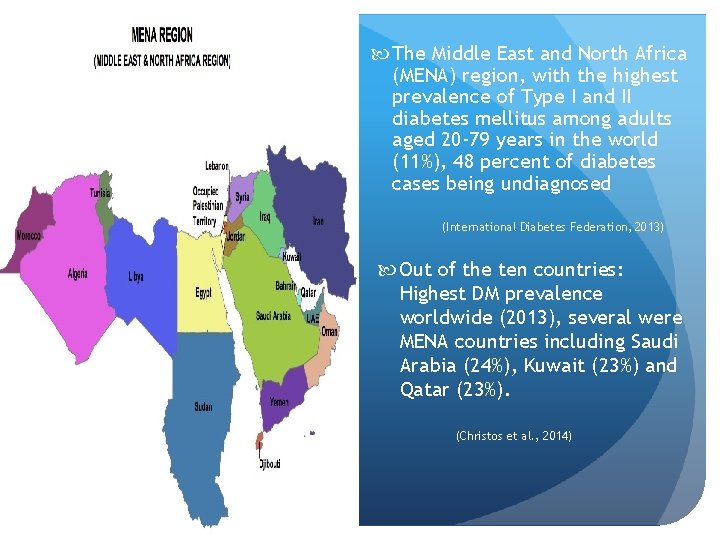
The Middle East and North Africa (MENA) region, with the highest prevalence of Type I and II diabetes mellitus among adults aged 20 -79 years in the world (11%), 48 percent of diabetes cases being undiagnosed (International Diabetes Federation, 2013) Out of the ten countries: Highest DM prevalence worldwide (2013), several were MENA countries including Saudi Arabia (24%), Kuwait (23%) and Qatar (23%). (Christos et al. , 2014)

This situation has prompted the Ministry of Public Health (2017) in the State of Qatar to strengthen their strategies to ensure proper lifestyle advice, education, and counseling be available to diabetic patients and those at risk of developing type 2 diabetes, which in the long term will lead to a modification of risk factors, improving rates of diabetes prevalence and morbidity. Promoting awareness of diabetes and its prevention throughout the population (Qatar Diabetes Association, 2016).

Earlier studies have found that patients with diabetes mellitus: Ø High risk of decreased psychological well-being (Gask, Macdonald, & Bower, 2011; Stuckey et al. , 2014) Ø Detrimental impact on well-being and psychological functioning (Brands et al. , 2007) Ø More likely to experience depression (Almeida, 2015) Ø Psychological morbidity (Al-Madhaki & Al-Kuwari, 2017).

Psychological and social problems are common among diabetic patients worldwide (Peyrot, Rubin, Lauritzen, Snoek, Matthews, & Skovlund, 2005) ü Non-adherence to medications, poor quality of life, and lack of interest in managing disease resulting in poor glycemic control and long-term complications (Gupta, Bhadada, Shah, & Mattoo, 2016) ü Poor psychosocial outcome by 44. 6% of the DM patients (DAWN Study, Nicolucci et al. , 2013)

Psychological and social issues are important concern in the overall health of patients with diabetes mellitus, however, in Qatar, this area is understudied. Moreover, doctors, nurses, and other health care professionals should need to emphasize the psychological and social health aspects of patients with diabetes mellitus. It is important therefore, to look into the psychological and social issues of patients with diabetes mellitus.

Objective of the Study To determine the psychological and social well-being of patients with diabetes mellitus in Doha, Qatar.
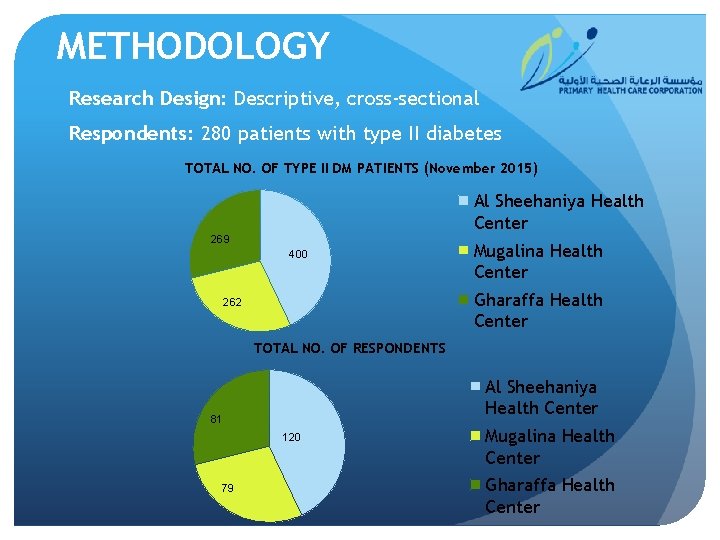
METHODOLOGY Research Design: Descriptive, cross-sectional Respondents: 280 patients with type II diabetes TOTAL NO. OF TYPE II DM PATIENTS (November 2015) Al Sheehaniya Health Center 269 400 Mugalina Health Center Gharaffa Health Center 262 TOTAL NO. OF RESPONDENTS Al Sheehaniya Health Center 81 120 79 Mugalina Health Center Gharaffa Health Center

N = 280 Al Gharaffa (n = 81) Mugalina (n = 79) Al Sheehaniya (n = 120)

Ethical Considerations Ethical Board and Research Section of the Department of Clinical Affairs, Primary Health Care Corporation, Doha, Qatar (PHCC/IEC/16/01/001) Permission to conduct the study was also obtained from the Medical Directors of the 3 Health Centers. Bioethical principles of the Declaration of Helsinki. Consent letter was included as a part of the questionnaire which stated the purpose of the study.

Research Instrument Psychological Well-being (10 -item, researcher-made- checklist) Social Well-being (10 -item, researcher-made- checklist) Validated by 3 Experts Reliability: Cronbach’s Alpha (. 873 and. 815)
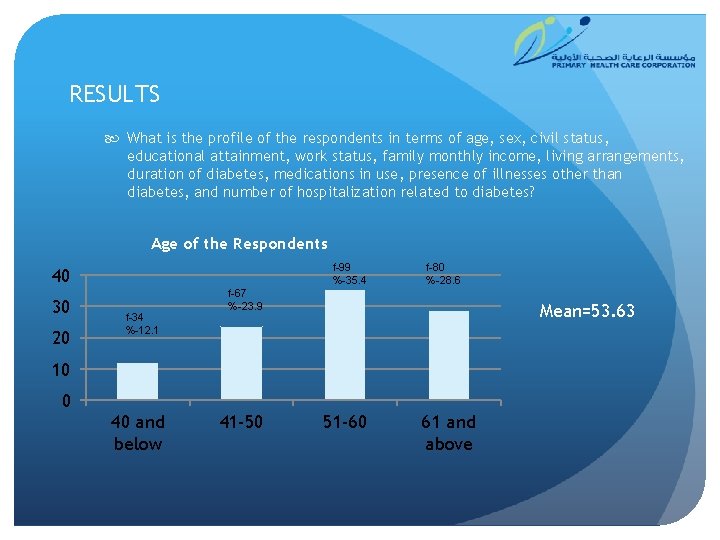
RESULTS What is the profile of the respondents in terms of age, sex, civil status, educational attainment, work status, family monthly income, living arrangements, duration of diabetes, medications in use, presence of illnesses other than diabetes, and number of hospitalization related to diabetes? Age of the Respondents f-99 %-35. 4 40 30 20 f-34 %-12. 1 f-80 %-28. 6 f-67 %-23. 9 Mean=53. 63 10 0 40 and below 41 -50 51 -60 61 and above

Sex Educational Attainment Male f-120 %-42. 9 f-160 %-57. 1 f-70 %-25. 0 Female Total: f-280 Total: %-100 f-59 %-21. 1 f-95 %-33. 9 Civil Status f-20 %-7. 1 f-260 %-92. 9 Single Married Total: f-280 Total: %-100 f-56 %-20. 0 None Elementary Total: f-280 Total: %-100
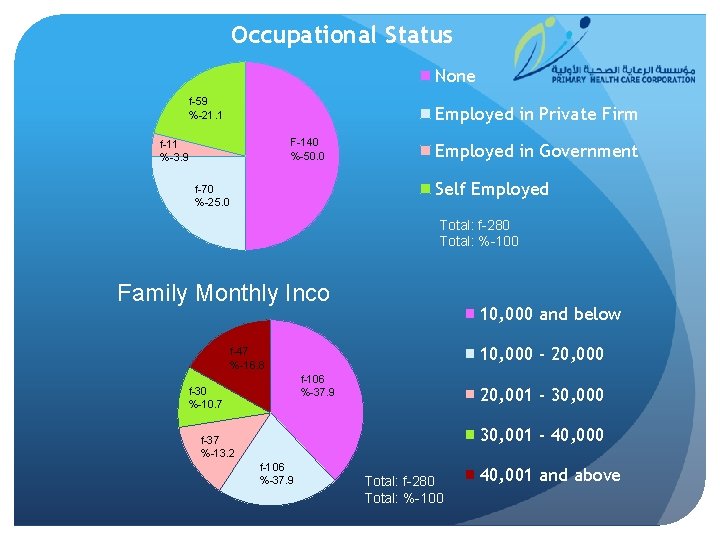
Occupational Status None f-59 %-21. 1 Employed in Private Firm F-140 %-50. 0 f-11 %-3. 9 Employed in Government Self Employed f-70 %-25. 0 Total: f-280 Total: %-100 Family Monthly Income 10, 000 and below 10, 000 - 20, 000 f-47 %-16. 8 f-106 %-37. 9 f-30 %-10. 7 20, 001 - 30, 000 30, 001 - 40, 000 f-37 %-13. 2 f-106 %-37. 9 Total: f-280 Total: %-100 40, 001 and above
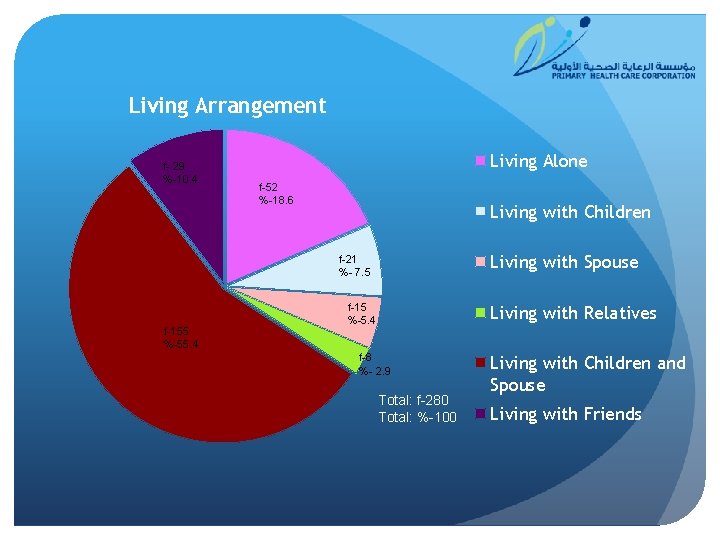
Living Arrangement f- 29 %-10. 4 Living Alone f-52 %-18. 6 Living with Children Living with Spouse f-21 %- 7. 5 f-155 %-55. 4 f-15 %-5. 4 Living with Relatives f-8 %- 2. 9 Total: f-280 Total: %-100 Living with Children and Spouse Living with Friends
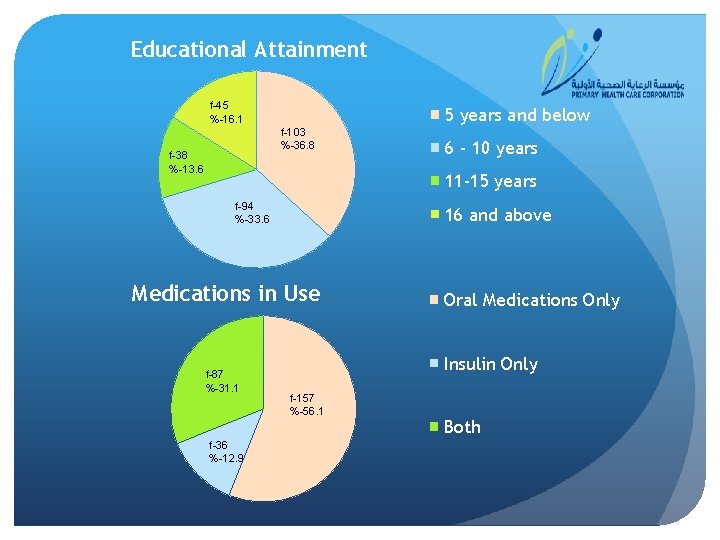
Educational Attainment f-45 %-16. 1 5 years and below f-103 %-36. 8 f-38 %-13. 6 6 - 10 years 11 -15 years f-94 %-33. 6 16 and above Medications in Use f-87 %-31. 1 f-36 %-12. 9 Oral Medications Only Insulin Only f-157 %-56. 1 Both
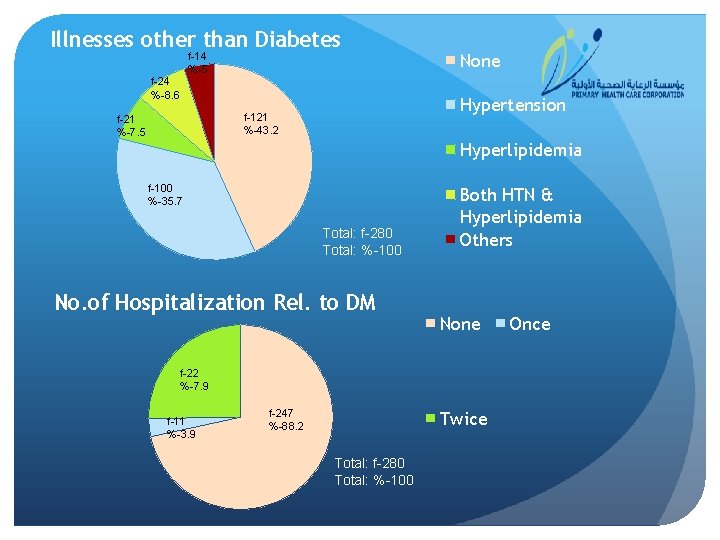
Illnesses other than Diabetes f-14 %-5 f-24 %-8. 6 Hypertension f-121 %-43. 2 f-21 %-7. 5 None Hyperlipidemia f-100 %-35. 7 Total: f-280 Total: %-100 No. of Hospitalization Rel. to DM Both HTN & Hyperlipidemia Others None f-22 %-7. 9 f-11 %-3. 9 f-247 %-88. 2 Twice Total: f-280 Total: %-100 Once
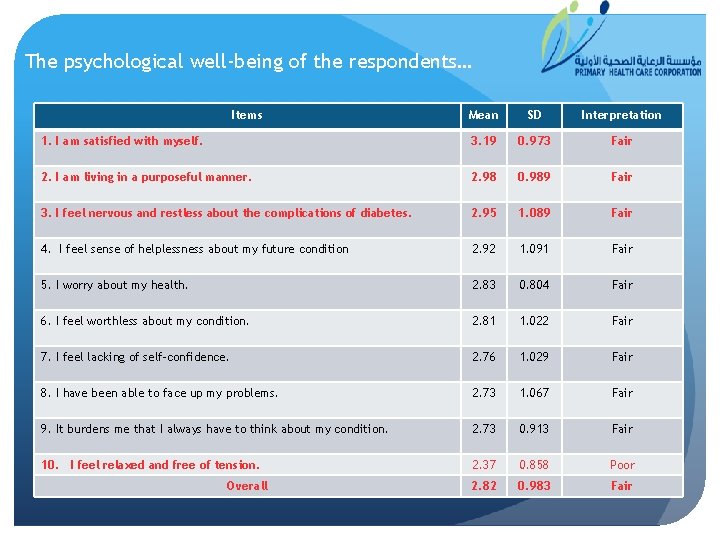
The psychological well-being of the respondents… Items Mean SD Interpretation 1. I am satisfied with myself. 3. 19 0. 973 Fair 2. I am living in a purposeful manner. 2. 98 0. 989 Fair 3. I feel nervous and restless about the complications of diabetes. 2. 95 1. 089 Fair 4. I feel sense of helplessness about my future condition 2. 92 1. 091 Fair 5. I worry about my health. 2. 83 0. 804 Fair 6. I feel worthless about my condition. 2. 81 1. 022 Fair 7. I feel lacking of self-confidence. 2. 76 1. 029 Fair 8. I have been able to face up my problems. 2. 73 1. 067 Fair 9. It burdens me that I always have to think about my condition. 2. 73 0. 913 Fair 10. I feel relaxed and free of tension. 2. 37 0. 858 Poor 2. 82 0. 983 Fair Overall
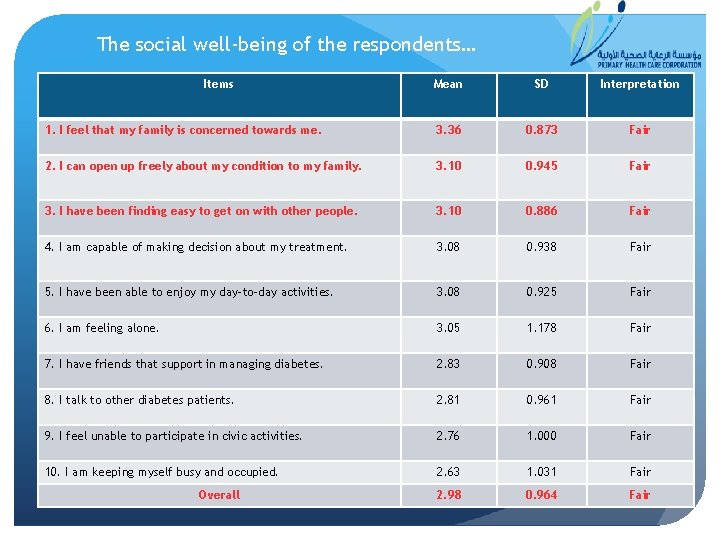
The social well-being of the respondents… Items Mean SD Interpretation 1. I feel that my family is concerned towards me. 3. 36 0. 873 Fair 2. I can open up freely about my condition to my family. 3. 10 0. 945 Fair 3. I have been finding easy to get on with other people. 3. 10 0. 886 Fair 4. I am capable of making decision about my treatment. 3. 08 0. 938 Fair 5. I have been able to enjoy my day-to-day activities. 3. 08 0. 925 Fair 6. I am feeling alone. 3. 05 1. 178 Fair 7. I have friends that support in managing diabetes. 2. 83 0. 908 Fair 8. I talk to other diabetes patients. 2. 81 0. 961 Fair 9. I feel unable to participate in civic activities. 2. 76 1. 000 Fair 10. I am keeping myself busy and occupied. 2. 63 1. 031 Fair 2. 98 0. 964 Fair Overall
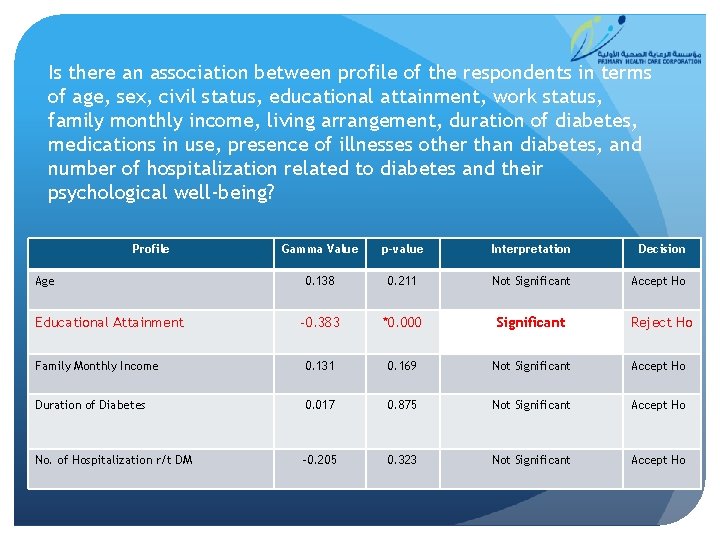
Is there an association between profile of the respondents in terms of age, sex, civil status, educational attainment, work status, family monthly income, living arrangement, duration of diabetes, medications in use, presence of illnesses other than diabetes, and number of hospitalization related to diabetes and their psychological well-being? Profile Gamma Value p-value Interpretation Decision 0. 138 0. 211 Not Significant Accept Ho -0. 383 *0. 000 Significant Reject Ho Family Monthly Income 0. 131 0. 169 Not Significant Accept Ho Duration of Diabetes 0. 017 0. 875 Not Significant Accept Ho No. of Hospitalization r/t DM -0. 205 0. 323 Not Significant Accept Ho Age Educational Attainment
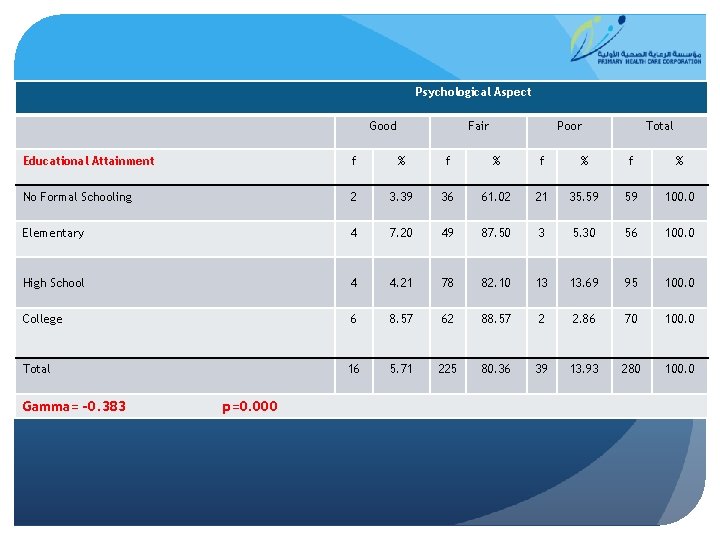
Psychological Aspect Good Fair Poor Total Educational Attainment f % f % No Formal Schooling 2 3. 39 36 61. 02 21 35. 59 59 100. 0 Elementary 4 7. 20 49 87. 50 3 5. 30 56 100. 0 High School 4 4. 21 78 82. 10 13 13. 69 95 100. 0 College 6 8. 57 62 88. 57 2 2. 86 70 100. 0 Total 16 5. 71 225 80. 36 39 13. 93 280 100. 0 Gamma= -0. 383 p=0. 000
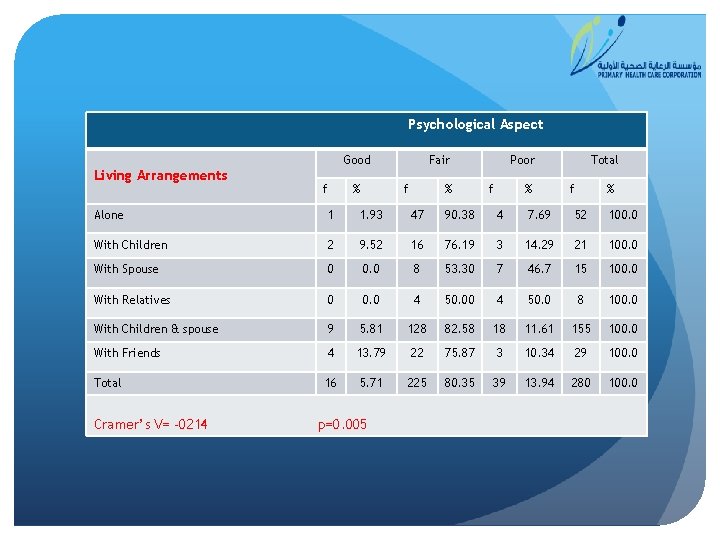
Psychological Aspect Good Living Arrangements f % Fair f % Poor f % Total f % Alone 1 1. 93 47 90. 38 4 7. 69 52 100. 0 With Children 2 9. 52 16 76. 19 3 14. 29 21 100. 0 With Spouse 0 0. 0 8 53. 30 7 46. 7 15 100. 0 With Relatives 0 0. 0 4 50. 0 8 100. 0 With Children & spouse 9 5. 81 128 82. 58 18 11. 61 155 100. 0 With Friends 4 13. 79 22 75. 87 3 10. 34 29 100. 0 Total 16 5. 71 225 80. 35 39 13. 94 280 100. 0 Cramer’s V= -0214 p=0. 005

Profile Cramer’s V Value p-Value Interpretation Decision Sex 0. 103 0. 230 Not Significant Accept Ho Civil Status 0. 070 0. 501 Not Significant Accept Ho Work Status 0. 108 0. 364 Not Significant Accept Ho -0. 214 *0. 005 Significant Reject Ho 0. 054 0. 805 Not Significant Accept Ho -0. 190 *0. 010 Significant Reject Ho Living Arrangement Medication in Use Illnesses Other than Diabetes
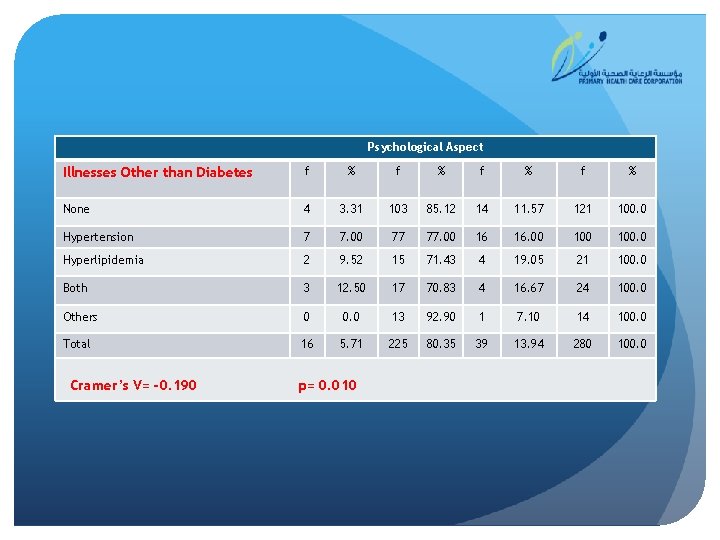
Psychological Aspect Illnesses Other than Diabetes f % f % None 4 3. 31 103 85. 12 14 11. 57 121 100. 0 Hypertension 7 7. 00 77 77. 00 16 16. 00 100. 0 Hyperlipidemia 2 9. 52 15 71. 43 4 19. 05 21 100. 0 Both 3 12. 50 17 70. 83 4 16. 67 24 100. 0 Others 0 0. 0 13 92. 90 1 7. 10 14 100. 0 Total 16 5. 71 225 80. 35 39 13. 94 280 100. 0 Cramer’s V= -0. 190 p= 0. 010
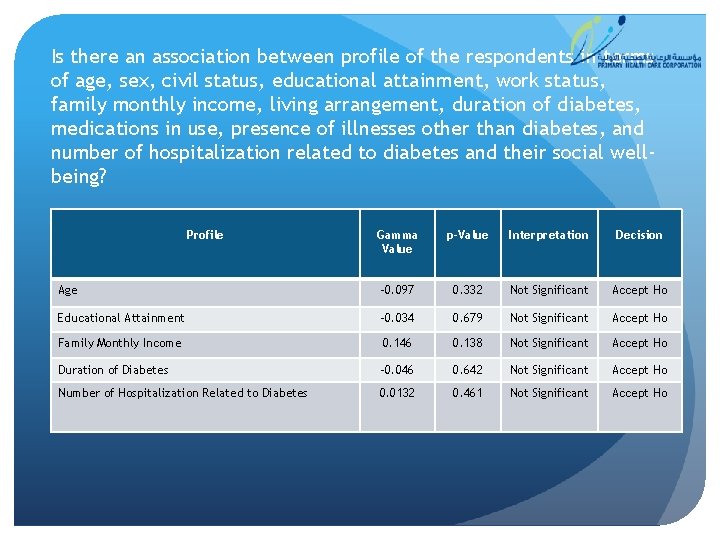
Is there an association between profile of the respondents in terms of age, sex, civil status, educational attainment, work status, family monthly income, living arrangement, duration of diabetes, medications in use, presence of illnesses other than diabetes, and number of hospitalization related to diabetes and their social wellbeing? Profile Gamma Value p-Value Interpretation Decision Age -0. 097 0. 332 Not Significant Accept Ho Educational Attainment -0. 034 0. 679 Not Significant Accept Ho Family Monthly Income 0. 146 0. 138 Not Significant Accept Ho Duration of Diabetes -0. 046 0. 642 Not Significant Accept Ho Number of Hospitalization Related to Diabetes 0. 0132 0. 461 Not Significant Accept Ho
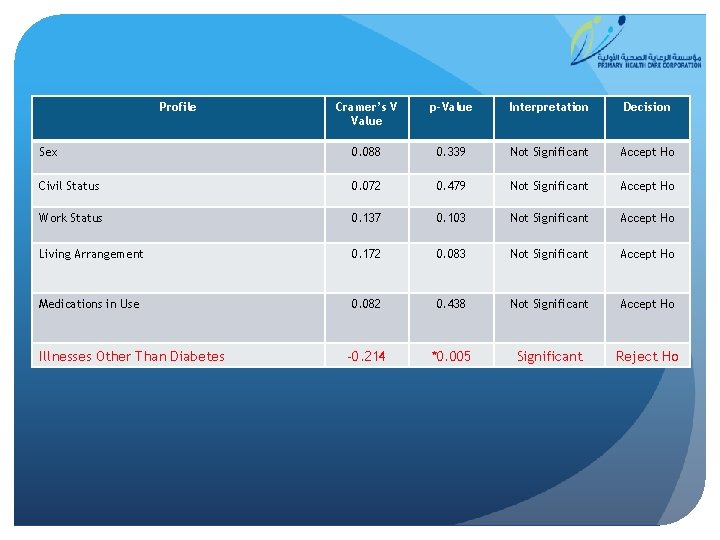
Profile Cramer’s V Value p-Value Interpretation Decision Sex 0. 088 0. 339 Not Significant Accept Ho Civil Status 0. 072 0. 479 Not Significant Accept Ho Work Status 0. 137 0. 103 Not Significant Accept Ho Living Arrangement 0. 172 0. 083 Not Significant Accept Ho Medications in Use 0. 082 0. 438 Not Significant Accept Ho -0. 214 *0. 005 Significant Reject Ho Illnesses Other Than Diabetes
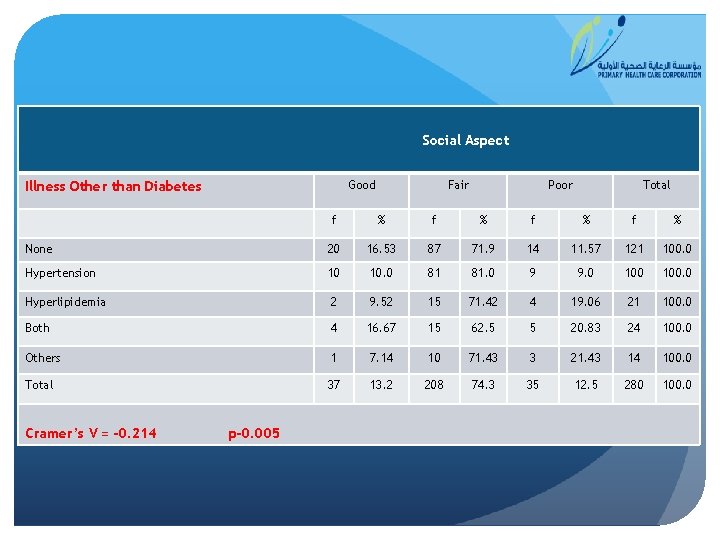
Social Aspect Good Illness Other than Diabetes Fair Poor Total f % f % None 20 16. 53 87 71. 9 14 11. 57 121 100. 0 Hypertension 10 10. 0 81 81. 0 9 9. 0 100. 0 Hyperlipidemia 2 9. 52 15 71. 42 4 19. 06 21 100. 0 Both 4 16. 67 15 62. 5 5 20. 83 24 100. 0 Others 1 7. 14 10 71. 43 3 21. 43 14 100. 0 Total 37 13. 2 208 74. 3 35 12. 5 280 100. 0 Cramer’s V = -0. 214 p-0. 005

Conclusions This study sheds light the importance of addressing the psychological and social well-being of patients living with diabetes mellitus in Doha, Qatar. The results suggest that self-satisfaction and living purposefully despite the illness, and the support of family members are the factors that could increase the likelihood of positive psychological state and better social well-being. Higher level of education and living with spouse, children, and friends are associated with lesser tendency of having poor psychological health. Respondents with no illnesses other than diabetes were more likely to develop good psychological and social functioning as well. Overall, patients with diabetes mellitus still have the ability to maintain positive psychological health and social functioning.

Recommendations Doctors and nurses should continuously and effectively counsel diabetic patients that would maintain and improve patients’ satisfaction and therapeutic outcomes through appropriate psychological and social interventions such as problem-solving and coping skills, relaxation techniques and stress management, motivational interviewing, and empowerment-based programs. To effectively counsel the patients with diabetes, doctors and nurses should receive appropriate training associated with teaching and counseling techniques. To those patients with poor literacy and poor numeracy skills, diabetes education should be strengthened through interactive modules and should be culturally flexible for diabetic patients of different origin and backgrounds.

Acknowledgement Research Section of the Department of Clinical Affairs, Primary Health Care Corporation, Doha, Qatar (PHCC/IEC/16/01/001) Dr. Khalid Joyce Luz Thank you for your attention!
- Slides: 32