Psychosocial Aspects of Human Aging Successful Aging Gail







































- Slides: 41

Psychosocial Aspects of Human Aging, & Successful Aging Gail M. Sullivan, MD, MPH UConn Center on Aging

Demography ≥ 65 years: • • 50% of MD visits 33% of prescribed meds 90% of long term care beds 60% hospital bed days vs. 13% of population – % increasing to 20% by 2030

Baseline Data • Family Circumstances + 80% elders living alone have close contact w/ a child • Living Arrangements + 41% women live alone vs. 15% men + 2/3+ of nursing home beds occupied by women • • Marital Status- more women are widows Economic Status + Poverty rates decreased with Social Security

What is Normal Aging? • “Successful” • Usual or customary • Diseases associated with aging

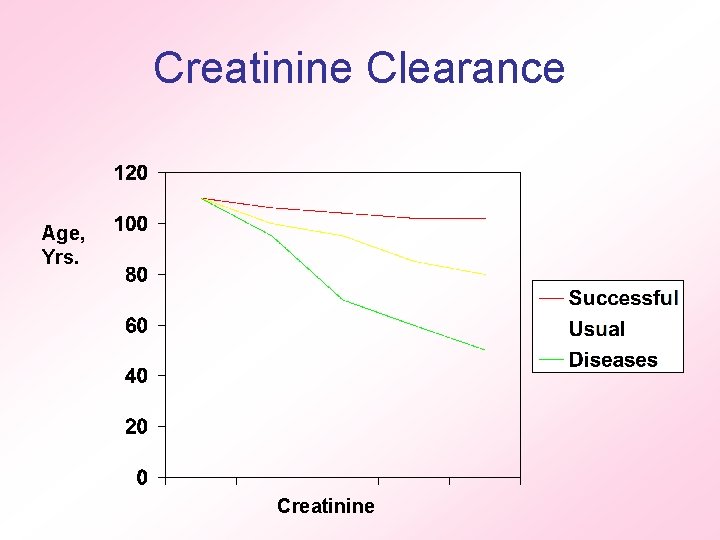
Example 1 • Essentially no change in creatinine clearance (2 S. D. better than mean) • Moderate slow decline - use formula to predict (140 -age) X body wt. (kg) 72 X serum creatinine • Renovascular disease, HTN So what? Important in drug dosing (X. 85 ♀)

Creatinine Clearance Age, Yrs. Creatinine

Example 2 No memory decline (with or w/out training) Slowed information retrieval, slower reaction times Alzheimer’s dementia, vascular dementia So what? “Senile” dementia does not exist

Example 3 Preserved skeletal muscle (older athlete) Decreased skeletal muscle, increased % fat Sarcopenia with cardiac, renal diseases So what? Drug dosing; exercise may reverse declines in strength

Example 4 Height preserved, normal BMD Bone Mineral Density Gradual loss of height (1 -2 inches), osteopenia Osteoporosis, fractures So what? Osteoporosis preventable, treatable, often undetected, not normal

Conclusion: Normal Aging We know: - a lot about customary aging - greater understanding of diseases associated with aging - beginning to understand the prescription for “successful aging”

Ageism Prejudice for or against likelihood of a condition, or any assumption based solely on a patient’s age Example: 88 y/o with decreased walking Patient, family & health professionals all have ageist stereotypes

“Who’d you draw in the jousting tournament? ” “How’d he get to be 97? ”

Tom Lackey, 89, took up wing-walking as a way past the grief of losing his wife. Here, he is flying across the English Channel.

Ilse Telesmanich, 90, hiking in South Africa

Stereotypes • • Wrinkled, leathery skin Fragile bones Sexless Physically weak Blind Deaf Memory impaired Sick

Reality • Tremendous heterogeneity


Functional Assessment • AADL – Driving – Leisure activities, travel • IADL – – Managing finances – Cooking Arranging transportation – Cleaning, laundry Managing meds – Telephone Shopping • ADL – Bathing – Personal hygiene – Toileting, continence – Ambulation, stairs – Transferring OOB, chair – Feeding

Diseases Mr. A • Cardiac disease with congestive heart failure Mrs. A • • Asthma Osteoarthritis Osteoporosis Hip Replacement Non-critical AS Hypertension Diabetes mellitus Cataracts Mild hearing loss Constipation Uterine Fibroids Cholecystectomy Diverticulosis, itis Actinic keratoses Urge incontinence

Function Status Mr. A • • Dependent in AADL, IADL, & ADL Except for feeding & personal hygiene Mrs. A • • Independent in AADL, IADL, ADL Able to travel, play bridge, drive, manage finances, shop, cook, manage meds for both, bathe, dress, walk, transfer, toilet, & eat

Functional Loss in Older Persons Final common pathway for disease First presentation of disease Primary determinant of quality of life Function may be more important than diagnosis

Social Factors - Demographic • Age - functional loss usually due to chronic disease, but lost function may be recovered • Gender- women live longer, but have worse functional status, due to – Osteoporosis, osteoarthritis, sarcopenia, dementia – Heart disease, cancer, CVA • Race - minority status + Worse health, function, survival + Reasons: behaviors, environment, access to health care, but socioeconomic status (SES) most important + If control for SES, race not an independent RF, when aged + 2 most important factors for mortality/dysfunction in late life: + SES & smoking - & smoking prevalence is related to SES


Social Factors & Mortality • Multiple studies show association – but how? – – – Caring network encourages healthful practices Caring network improves adherence to treatments Groups or individuals provide actual physical or financial help Effects on immune function Effects on neuro endocrine function • Social integration (attachments to groups) & social support (attachments to people) – Attendance at church assoc. with better function – Participation in voluntary groups assoc. with ↓ mortality – Social supports associated with improved health outcomes, e. g. , better recovery from MI, CVA • Intervention studies: ↑ self-efficacy (= personal capacity to effect change & control events, i. e. promote ‘can do’) • Maintain sense of well-being, able to adapt to stressors (disease, disability, spouse illness or death, moves) • Live longer • Better health status, better cognitive status

Studies RATS • Social isolation suppresses wound healing and immune response • Timid rats w/ less drive to explore die 6 months earlier than siblings who explore HUMANS • Morbidity assoc. with social isolation equal to that of cigarette smoking

Social Factors- Birth Cohorts • Each successive 5 yr cohort: + More education + More money + Better health + Effects of better environment, nutrition, prevention + Also due to higher SES + Taller

Transitions • Aging brings losses + Spouse, friends, children + Job, income, status + Home, neighborhood + Health, function • But coping skills improve with age

Transitions: Retirement • Gender roles- stereotypic, but may be relevant to current retirees + Men- defined by work and income + Status, identity, social role, friendships are work-dependent; retirement terminates all + Increased mortality if widowed + Women- use outside-of-work activities for all but income + Retired women less likely to be “at a loss”

Transitions: Widowhood Grief versus depression • Grief - appropriate response to death + Sadness, depressed feelings, crying, loss of interest in usual activities + Abates in 4 -8 weeks; sadness & crying persist 6 -12 mo. + Encourage talking, association with friends, family + Norms are culturally-dependent • Grief > 3 mo. + symptoms of major depression - may be depression

Transitions: Relocation effects determined by: • Voluntariness • Nature of new living arrangement: independent, assisted living, nursing home • Predicted, controlled vs. not (determines stress) • Physical & cognitive function

Transitions: Chronic Disease & Disability Chronic disease & disability • Increase with age • But - opportunities to delay and ameliorate losses • NIH study of older disabled women - still have active, involved lives, important social roles – Disability does not equal poor quality of life or depression

Coping Mechanisms (1) Coping - adaptive responses to stress which reduce harm to psychological well-being + Specific coping styles: anger, guilt, denial, accommodation, problem-solving, social involvement + More mature and successful techniques (accommodation, problem-solving, social involvement) - more common with age

Coping Mechanisms (2) Comparisons with peers (rather than to past self) + + How well am I doing vs. my friends Are events expected milestones Shifts in centrality + What roles are central to my identity? shift from: + Breadwinner to volunteer + Parent to grandparent + Head of household to sage dispensing wisdom + Ability to transition to another role is vital to well-being

Psychological Processes in healthy older adults, relevant to care • Attention – maintain performance on a task over time; focus without losing track + Sustained attention very good in healthy older adults + Easier distractibility with age, esp. when irrelevant information presented with relevant + So what? When giving key info, stick to core data, write it down Decreased attention requires eval. , as it is not normal

Learning & Memory • 14 - year longitudinal study, 70 + year-olds + < half had small declines in long term memory + 5 brief training sessions improved decline to baseline + Majority, with no decline, improved after training + Apparently ‘age-obligatory’ losses are modifiable Use it or lose it? • So what? Encourage encoding strategies, refer to reputable memory training, write down instructions or recommendations

Cognitive Training & Function • Large RCT, community elders, av. age 74, 4 groups – – 10 sessions memory training (verbal) 10 sessions reasoning training (inductive) 10 sessions speed of processing (visual search & ID) Controls • All training groups showed improvement in area trained; this persisted 5 yrs later • Reasoning group: less difficulty in IADL vs. controls at 5 yrs • Subgroup with ‘booster’ training at 11 & 35 mos. – Had additional improvement in targeted area • Conclusion: cognitive training improves specific areas trained & reasoning training results in less functional decline

Language • Vocabulary - increases into 50 s & 60 s; occasional errors in naming occur more frequently beginning in mid-life; use encoding strategies • Syntactic skills - combine words in meaningful sequence - no change with age • So what? Write names down; other changes in language require evaluation

Cognitive Function: Bottom Line Normal aging does not cause cognitive loss – Diseases + Dementia, delirium, depression – vs. incorrect assessment or diagnosis + Deafness, aphasia, language barrier Usual change: increase in reaction time, which is modifiable with training So what? Don’t diagnose “senile dementia” or “chronic OBS”

Sensory & Perceptual Processes: Vision • • • Declines with age Acuity, color & brightness discrimination decline Light sensitivity increases (glare) Visual processing speed (reading) declines - ? Modifiable Dynamic vision (scrolling messages on TV screen) declines Depth perception, figure-ground discrimination, visual search (important for driving, e. g. , locating a sign) decline • Clinical points: bright, non-glare light; large, high contrast print; annual OPTOMETRY eval

Hearing • Losses prevalent & >50% are clinically important • Presbycusis is common – progressive, bilateral, mixed sensorineural & central processing loss of hearing • Exacerbated by acoustical trauma • High tones lost: consonants most difficult to hear • Clinical points: screen all, enunciate, don’t shout, low pitch best

Conclusions • • Population aging rapidly & elders use more health services & products • • • Certain diseases associated with aging but not part of usual aging • “Positive” attitude towards aging assoc. with longevity; interventions to boost self-efficacy show better outcomes • • Cohort effects may be important: WWII elders vs. baby boomers • • Insignificant or no changes: attention, learning, memory, language Enormous heterogeneity in elders – in function, diseases, & coping strategies Most elders independent & live in the community, despite chronic diseases Social factors have powerful effects upon function, recovery & mortality (poverty & smoking in mid-life are the worst) Important neuropsychol. changes: hearing & vision decline; reaction time declines Function is primary determinate of quality of life for elders