Psychological Pain as a symptom Somatic Symptom Disordersomatization

















- Slides: 19

Psychological Pain as a symptom Somatic Symptom Disorder(somatization) n Illness Anxiety Disorder(hypochondriass) n Functional Neurological Symptom Disorder(Conversion) n Factitious Disorder n Pain Disorder n

Pain Disorder(DSM-5) Prevalence: 5 -12 percent n Is associated with affective and anxiety disorders n Chronic pain most frequently associated with depressive disorders n Acute pain most frequently associated with anxiety disorders n

Pain Disorder Depressive disorders, alcohol dependence, and chronic pain are more common in relatives of individuals with chronic pain disorder n Increased risk for suicide: pain associated with severe depression Pain in terminal illness such as cancer n

Etiology Psychodynamic factors n Behavioral Factors n Interpersonal Factors n Biological Factors n

n Mind n Brain n Body

Psychodynamic Factors: Intrapsychic Conflicts and body language Alexythymia Identification n

n Behavioral and interpersonal factors: Punishment and Reward Secondary gain Manipulation of environment

Depression and pain commonly occur. n n Between 30 -60% of individuals with pain report having comorbid depression. 2, 3, 4 Approximately half of patients with depression report pain. 1 1) Katona et al. Clin Med. 2005; 5: 390 -5; 2) Bair et al. Arch Intern Med 2003; 163: 2433 -45 3) Hassett et al. Curr Pain Headache Rep. 2014; 418: 36; 4) Arnold et al. J Clin Psychiatry 2006; 67: 1219 -25

n Chronic Pain equivalent of depression (Masked depression)

Complexity: Multiple Symptoms Most common complaints: n Chronic widespread pain n Fatigue n Sleep disturbance n Poor mood n Cognitive difficulties n Muscle stiffness Frequently occurring complaints: n Gastrointestinal symptoms n Headache n Genitourinary n Numbness and tingling n Dizziness/loss of balance n Weakness DJ. JAMA 2014; 311; 1547 -55 n Skin. Clauw changes Mease et al. Arthritis Rheum 2008; 59(7): 952 -60

Complexity: High Rates of Co-Morbidity § Comorbidity with other chronic pain states 42 -70% of patients with FM also meet criteria for CFS 32 -80% of patients with FM meet criteria for IBS 42% of back pain patients meet criteria for FM Clauw &Hassett. Aaron & Buchwald. Ann Intern Med 2001; 134: 868– 81 Brummett, Goesling, Tsodikov, Meraj, Wasserman, Arthritis Rheum 2013; 65: 3285 -92. § Co-Morbidity with chronic systemic disease Rheumatoid arthritis, lupus, inflammatory bowel disease 2007; 21: 391 -402 Lee et al. Ann Rheum Dis 2013; 72: 949 -54. Bliddal et al. Best Prac Res Clin Rheumatol Schlesinger, Hassett et al. Ann Rheum 2009 § Psychiatric co-morbidity – mostly anxiety and depression.

Neurobiological perspective. Brain regions associated with physical pain overlap with psychological pain processing: n n Sensory discriminative dimension – Somatosensory cortices (S 1, S 2) – Dorsal posterior insula Affective emotional dimension – Anterior insula – Prefrontal cortex – Anterior cingulate cortex – Thalamus – Amygdala – Hippocampus Goesling, Clauw & Hassett. Curr Psychiatry Rep. 2013; 15: 421

Neurobiological perspective. Neurotransmitters – pain Neurotransmitters depression n. Serotonin n n. Norepinephrine n n. Glutamate n n. GABA n Serotonin Norepinephrine Glutamate GABA Ø Similar neurotransmitter anomalies exist. Ø Both respond to SNRIs, but SSRIs provide little pain relief. Ø SNRIs might be better thought of as “neuromodulators. ” Ø Pain relief with SNRIs is often independent of Buskila & Clauw. Curr Pain Headache Rep 2009; 13: 343 -9 changes Ablin, in depression.

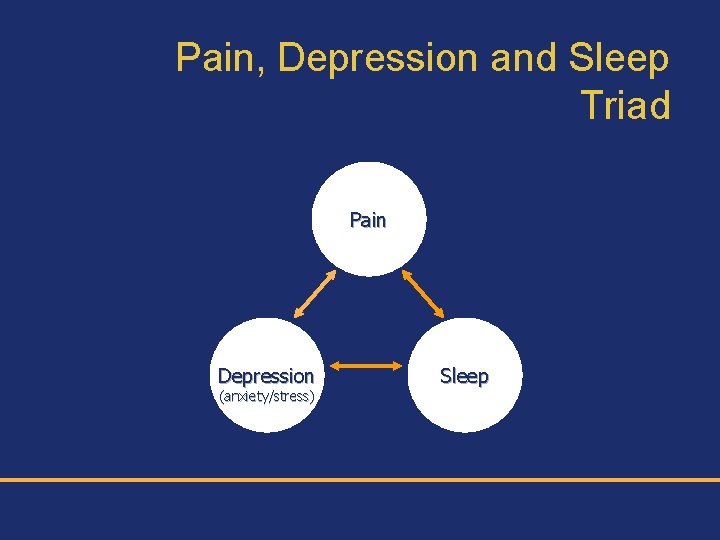
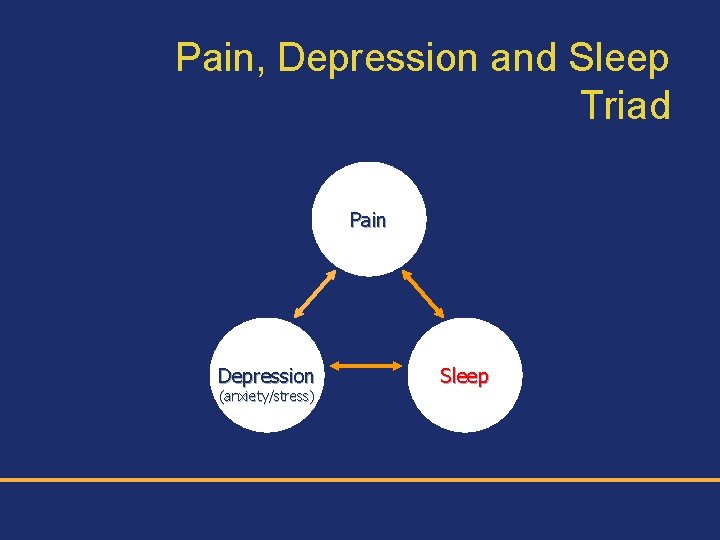
Pain, Depression and Sleep Triad Pain Depression (anxiety/stress) Sleep

Pain, Depression and Sleep Triad Pain Depression (anxiety/stress) Sleep

Sleep Hygiene “Sleep and sleep hygiene” n. DHHS 64 million Americans have chronic insomnia (> 20%) n. Disrupting slow wave sleep over several nights in sedentary middle-aged females (without reducing total sleep efficiency) results in a decreased pain threshold, increased discomfort, and fatigue. Lentz et al. , J Rheumatol 1999, 26(7), 1586 -1592. n. In FM, >75% report sleep disturbances. n. Insomnia up to 65%, snoring and arousals up to 78%, RLS up to 41%, excessive daytime sleepiness up to 93%. n. FM with sleep studies = obstructive sleep apnea ~ 80% Abad et al. , Sleep Med Rev 2008; 12: 211 -28

Non-Pharmacological Interventions

Interventions that enhance positive emotions and resilience!

Acknowledgments Dr Alireza Ahmadi