PSYCHIATRY George Huntington Psychiatry Schizophrenia Obsessive Compulsive Disorders

PSYCHIATRY George Huntington

Psychiatry Schizophrenia Obsessive Compulsive Disorders Depression Functional Illness Bipolar Disorder Body Dysmorphic Disorders Addiction Post traumatic stress disorder Dementia Hysteria Delirium Dissociative Identity Disorder Anxiety Fugue Personality Disorders Sexual disorders Eating Disorders Sleep disorders Attention deficit hyperactivity disorder Autism

Psychiatry Schizophrenia Obsessive Compulsive Disorders Depression Functional Illness Bipolar Disorder Body Dysmorphic Disorders Addiction Post traumatic stress disorder Dementia Hysteria Delirium Dissociative Identity Disorder Anxiety Fugue Personality Disorders Sexual disorders Eating Disorders Sleep disorders Attention deficit hyperactivity disorder Autism

Psychiatry: - All you need for 3 A! Schizophrenia Depression Bipolar Disorder Addiction Dementia Delirium Anxiety Mental Health and Capacity Acts

Psychiatry Schizophrenia Depression Bipolar Disorder Addiction Dementia Delirium Anxiety

SCHIZOPHRENIA Schizophrenia is a chronic mental health problem defined by episodes of psychosis, disordered thinking and social withdrawal. Prevalence of 200 per 100, 000 Prodromal period Predisposing factors: inner-city, childhood abuse, drug and alcohol use, migration. Wide variety of presentations and subtypes. Primarily thought to be due to excess dopaminergic activity, though glutamate, microglia and deficient CNS glucose metabolism also play a role. May be aggressive though this is rare.

SCHIZOPHRENIA - FEATURES Negative symptoms: apathy, social withdrawal, self-neglect, blunting affect, catatonia (rare), Positive symptoms: paranoia, auditory hallucinations (auditory most common), thought disorder, delusions, passivity phenomena Diagnosis based on presence of symptoms and distinguished from a psychotic episode or other causes. Thought disorder: echo, insertion, broadcast, withdrawal. Delusions: Cotard’s, Othello, Capgras, Fregni, De Clerambault’s, wide variety here too.

PSYCHOSIS Psychosis is an abnormal cognitive state Wide variety of causes: schizophrenia, depression, mania, drugs, withdrawal Hallucinations are percepts in the absence of an external corresponding stimulus. Delusions are fixed beliefs held without external evidence. Treated with anti-psychotic (olanzipine) and sedative (lorazepam) Reserve Haloperidol for extreme cases, not to be used for remission therapy.

SCHIZOPHRENIA - MANAGEMENT Antipsychotic drug therapy, can be depot. First line: Olanzipine, Risperidone, (usually atypicals first) Second line: Quetiapine, Aripiprazole, chlorpromazine, Third line: Haloperidol or clozapine (plenty of unpleasant side effects) Usually discuss with patient. Assess risk of side effects in each. Psychological therapies of no use against simple human contact and understanding.

ANTI-PSYCHOTICS 1 st Generation (typical): zuclopenthixol, chlorpromazine, haloperidol, Side effects usually extrapyramidal movement problems: dry mouth, muscle stiffness, movement disorders (tardive dyskinesias and parkinsonism) 2 nd Generation (atypical): olanzapine, risperidone, quetiapine, aripiprazole Side effects usually endocrine and cortisol related: weight gain, increased appetite, cardiovascular disease. Evidence says most effective. Beware Neuroleptic Malignant Syndrome and Agranulocytosis with clozapine.

Psychiatry Schizophrenia Depression Bipolar Disorder Addiction Dementia Delirium Anxiety

DEPRESSION Depression is a mood disorder It is characterised by low mood, lack of enjoyment and poor sleep patterns. Many, many causes. Genetics, poor social situation, substance misuse, abuse, unemployment, loneliness, perinatal, chronic disease It is the most common GP diagnosis (probably incorrectly) Numerous screening tools (Beck Depression Inventory, Hospital Anxiety and Depression score, Patient Health Questionnaire) Most people have reduced serotonin, drug therapy aims to correct this Most people have poor life circumstance, talking therapy aims to correct this Grief and bereavement are normal, healthy processes. Do not treat them!

DEPRESSION - FEATURES Symptoms of depression include anhedonia, persistent low mood, guilt, worthlessness, poor concentration, weight change, difficulty sleeping, early morning waking, agitation. More severe may have psychomotor retardation, nihilistic delusions, mood congruent hallucinations. Symptoms worse in morning and at nightfall. Suicide: ALWAYS ASK

DEPRESSION - MANAGEMENT Good prognosis. Same therapy for remission as in acute treatment. 1 st line: psychotherapy such as cognitive behavioural therapy. Add an SSRI such as fluoxetine if moderate to severe. 2 nd line: consider a different SSRI or a tricylic antidepressant 3 rd line: try an ‘exotic’ antidepressant: venlafaxine, monoamine inhibitor etc. Continue talking therapy! Electroconvulsive therapy very effective in severe depression. Consider if not eating/sleeping. Consent is a must. Very humane, ignore the films. Not to be used for remission.

SUICIDE 5000 deaths a year in the UK and rising (mostly young men). Risks: middle age, male, unemployed, mental illness, recent divorce or bereavement, single, substance abuse, previous self-harm, recent psych admission, Men choose more violent and successful techniques. ASK!

Psychiatry Schizophrenia Depression Bipolar Disorder Addiction Dementia Delirium Anxiety

BIPOLAR DISORDER Bipolar disorder is a psychiatric condition involving manic and depressive episodes with normal functioning in between. Many varieties, probably not important to know. Prevalence of about 1500 in 100, 000. More common in women. Usual onset with end of puberty. Genetic component: afflicted family member increases risk.

MANIA Mania is a period of mental illness characterised by excessive excitement and overactivity. Different from hypomania: more psychotic features such as delusions. Symptoms of mania include euphoria, increased feelings of self-worth, overactivity, decreased appetite, increased energy, irritability, fast speech, flight of ideas. May include delusions of grandiosity and mood congruent hallucinations. May be aggressive

BIPOLAR DISORDER - MANAGEMENT Manage mania with acute anti-psychotic (olanzapine, risperidone, quetiapine), try lithium or sodium valproate if unsuccessful. In depressive episodes avoid non-SSRI antidepressants, be aware or inducing mania or rapid cycling. Consider anti-psychotics as above. For maintenance use lithium as a mood stabiliser (blood test of levels to avoid kidney damage). Control of eating and sleeping patterns. Talking therapy is ineffective but is often provided if requested.

Psychiatry Schizophrenia Depression Bipolar Disorder Addiction Dementia Delirium Anxiety

ADDICTION Addiction is a strong uncontrollable desire to consume a particular substance or engage in a certain behaviour. Distinct from misuse and psychological dependence. More common in men, young people, people with other psychiatric problems, certain jobs. Genetic factors predisposing to addiction exist, probably in relation to dopamine receptor variations.

ADDICTION - FEATURES Dependence syndrome includes behaviours such as: hoarding, binging, craving, withdrawal, ignoring negative consequences, rituals, tolerance, seeking behaviours, loss of control, rituals of consumption and narrowing of repertoire and putting primacy in obtaining. Behaviours may be initially enjoyment but soon turns to a ‘need’. Tolerance is diminished response to a drug following prolonged use. Withdrawal is the group of symptoms which occur due to suddenly stopping a substance.

SUBSTANCES + BEHAVIOURS Alcohol, Nicotine, Heroin, Sugar, Caffeine, Benzodiazepines, Shopping, Crack Cocaine, Vicodin, Zopiclone, Amphetamine, GHB, Sex, Cocaine, Opioids, Methylphenidate, Valium, Hypnotics, Buprenorphine, Muscle relaxants, Aerosols, Cannabis, Barbiturate Gambling, Tramadol, Morphine, Ketamine, Methadone, Self-harm, Methaqualone, Oxycodone, Work, Masturbation, Sedatives, Painkillers, Krokodil, Pornography, Crystal Meth, Food, Exercise, Seconal, Internet, PCP, Ecstasy, (video games? ) Diuretics? Metoclopramide?

ALCOHOL DEPENDENCE Ethanol is a CNS depressant. Short term risks of arrhythmia, hypoglycaemia, violence, decreased libido, blackout, Long term risks of IHD, CVA and stroke, oesophageal varices, Wernicke’s and Korsakoff’s, pancreatitis, infertility, depression, fatty liver disease, CAGE questionnaire.

ALCOHOL DEPENDENCE - MANAGEMENT Total abstinence is recommended. Disulfiram - inhibits acetaldehyde dehydrogenase. Pabrinex – replace B vitamin deficiencies Psychotherapy and programmes such as 12 step are recommended for motivation. May need treatment for other problems: liver disease needing a transplant etc.
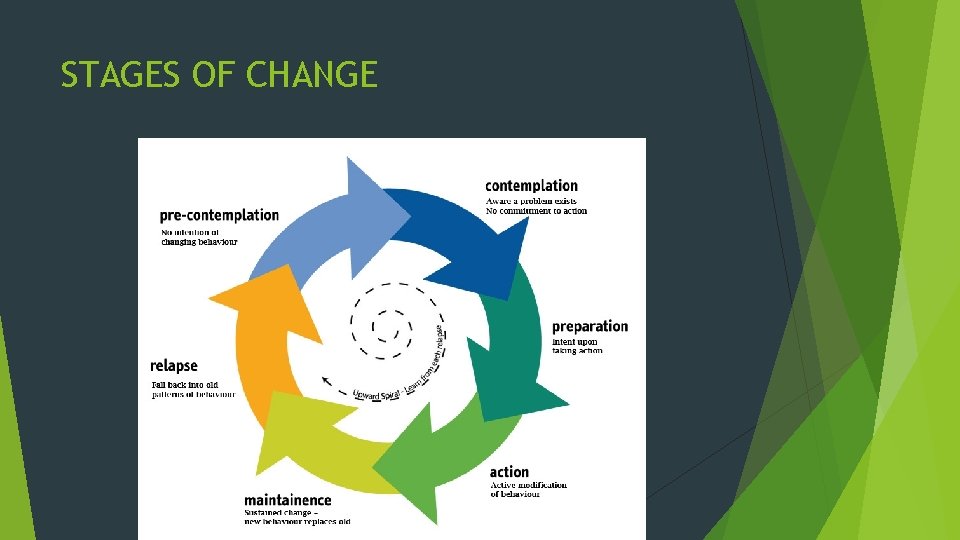
STAGES OF CHANGE
ALCOHOL WITHDRAWAL Produced by abruptly discontinuing alcohol use. Short term: sweating, tremor, nausea, agitation, tachycardia, hypertension. Followed by: delusions, confusion, auditory hallucinations, seizures, diarrhoea May produce delirium tremens: Lilliputian hallucinations, panic attacks, diaphoresis, ataxia, confusion and death, Treat with chlordiazepoxide (benzodiazepine) for sedation and as an anticonvulsant. Fluid and electrolyte replacement are essential (incl. dextrose). Consider long term therapy as with alcohol dependence.

WERNICKE’S Nystagmus Ataxia Confusion Treat quickly with thiamine to avoid Korsakoff’s!

Psychiatry Schizophrenia Depression Bipolar Disorder Addiction Dementia Delirium Anxiety

DEMENTIA Dementia is the progressive decline in cognitive functioning. Four most common types: Alzheimer’s disease, vascular dementia, Lewy-body dementia and fronto-temporal dementia. Often associated with increasing age. Genetic predisposition, few environmental factors proven. Treatment is scant and ineffective. Usually characterised by early memory loss (not always the case). Followed by self-neglect, sundowning, anxiety, wandering behaviours and incontinence Wide variety, is a specialty unto itself.

ALZHEIMER’S DISEASE Atrophy of brain tissue due to accumulation of amyloid protein plaques. Chronic slow progression. Cerebellum preserved. Death usually from bronchopneumonia. Treatment most effective in this type of dementia: anticholinesterase drugs (donepezil, galantamine, rivastigmine), NMDA receptor antagonists (currently only memantine, but watch this space) Drug therapy ensures longer lucid period and reduced cognitive decline but outcomes are the same.

VASCULAR DEMENTIA Clinically appears very similarly to Alzheimer’s. Result of many small vascular infarcts (lacunar strokes) over time. Step-wise progression. Risk: those with cardiovascular and cerebrovascular disease with repeated insult. Smoking and diabetes don’t help much either. Preventable with aspirin therapy in those at risk and managing lifestyle risk factors. Other treatments are ineffective.

LEWY-BODY DEMENTIA Accumulation of Lewy bodies in brainstem and neocortex. Fluctuating symptoms, associated with symptoms and sleep disturbance. Memory usually spared until later. Presence of hallucinations WHICH DO NOT TROUBLE THE PATIENT Similar pathogenesis to Parkinson’s disease. Rivastigmine MAY help, but probably not.

FRONTO-TEMPORAL DEMENTIA Atrophy of fronto-temporal area of brain without the protein deposits seen in Alzheimer’s. Behaviour and personality are destroyed in the early stages with memory and spatial awareness preserved. Produces massive frontal disinhibition which is very unpleasant for family members.

Psychiatry Schizophrenia Depression Bipolar Disorder Addiction Dementia Delirium Anxiety

DELIRIUM Delirium (aka acute confusional state) is acute disturbance in cognition, behaviour and consciousness. Umbrella term. Many causes: stroke, drugs, thyroid disease, anaesthesia, infection, CNS malignancies, subdural haematoma, electrolyte disturbance, sleep deprivation, drug withdrawal, normal pressure hydrocephalus. Most common in very old and very young. May be aggressive Rule out other causes

DELIRIUM - FEATURES Disorientation Reduced level of consciousness Inattention Hallucinations Fluctuating mood Altered personality Symptoms fluctuate and are worse at night.

DELIRIUM - MANAGEMENT Try talking the patient down. Treat underlying condition Best managed with lorazepam (oral or iv) Haloperidol is usually contraindicated. May have to resort to restraints or seclusion, though this is difficult in a non-psych setting. Prevent by minmising sensory deficits and maintaining orientation (i. e. nurse in a well-lit room)

DELIRIUM vs DEMENTIA DELIRIUM DEMENTIA Acute onset Chronic illness Fluctuating course Progressive, slow Impaired attention Attention preserved Decreased consciousness Consciousness preserved Usually reversible Usually irreversible Often accompanies physical illness Usually without physical problems Hospital acquired Community acquired

Psychiatry Schizophrenia Depression Bipolar Disorder Addiction Dementia Delirium Anxiety

ANXIETY Anxiety is a persistent unpleasant feeling of concern or unease disproportionate to actual circumstances and events. Prevalence of about 300 in 100, 000. Common reason to visit GP. More common in women. Closely related to depression. Often caused by distressing life events, but may exist for no apparent reason (free -floating). Many varieties.

GENERALISED ANXIETY DISORDER Generalised Anxiety Disorder is an anxiety disorder characterised by excessive fear and irrational worry. Focuses of anxiety include family, finance, social situations, eschatology, friendship, health and employment. Symptoms include apprehension, sweating, tachycardia, palpitations, rashes, hot flushes, somatisation, insomnia. Cognitive behavioural therapy is more effective than long term medications Drugs used include SSRIs (fluoxetine) and BZDs (lorazepam), though the latter has diminishing returns.

PANIC DISORDER Characterised by recurring panic attacks (more than 4 a month) Panic attacks are brief intensive episodes of extreme anxiety and fear. Symptoms include sweating, palpitations, dizziness, a feeling of impending doom, difficulty breathing, chest pain, hyperventilation, sensation of choking. Often mistaken for MIs. Triggers include embarrassment, stimuli and settings Treated with SSRIs. May also use propranolol to reduce ANS symptoms. Therapy is best, CBT.


PHOBIA Anxiety disorder only provoked in specific situations. Phobias: spiders, snakes, moths, rats, flying, closed spaces, open spaces, clowns, 13, heights, dogs, germs, holes, birds, needles, the ocean, beards, blood, cats, balloons, darkness, vomiting, bridges, bugs, frogs, fire, ducks, bees, sleep, doctors, dolls, fish, bananas, choking, hospitals, loud noises. Leads to unhealthy avoidance behaviours, which re-enforce the disease. Best treatment is confrontation and therapy.


MHA and MCA

MENTAL HEALTH ACT 1983 Amended 2007. For compulsory treatment of the severely mentally ill. If involuntary, known as ‘sectioning’ In practice, try for a voluntary admission. Civil and forensic sections. Also defines which conditions it can be used on and also who can section. Unable to force treatment for physical illness.

SECTION 2 Assessment order Admission for 28 days for assessment. Requires one Section 12 approved psychiatrist (must be trained and F 2 and above) and one other doctor. Cannot be renewed Doesn’t go on record Can treat against patient’s will

SECTION 3 Treatment order Admission for treatment, 6 months. Requires an AMP, a ST 4+ psychiatrist, a GP who is familiar with the patient. Can be renewed. Can treat involuntarily but not with ECT or psychosurgery (not amended currently for t. DCS or TMS).

EMERGENCY ORDERS + HOLDING POWERS Section 4 is the emergency order. Lasts 72 hours. A doctor and an AMP, gives time to find another doctor. No treatment under this order. Converted to a section 2. The holding powers are section 5: 2 and 5: 4. 5: 2, Doctor's holding power. Detain anyone admitted to hospital consensually for 72 hours. Holds a patient for further assessment. 5: 4, Nurse’s holding power. Same as above but for 6 hours.

PLACE OF GREATER SAFETY Section 135: Police section. Enter a patient’s premises and remove to a place of safety for 72 hours. Can use force. Social worker must obtain a warrant. Cannot treat against patient’s will. Section 136: same as above but for a public place. Don’t need a warrant.

COMMUNITY TREATMENT ORDER Basically a Section 3 in the community. Patient must turn up to appointments and take their treatment or will be returned to hospital (if Section 2) or remanded in police custody (if a forensic section).

MENTAL CAPACITY ACT 2007 Applies to everyone over the age of 16. Provides the legal framework to make decisions for those who lack capacity to do so themselves Protects people who lack capacity Empowers individuals who may have reduced capacity to still make decisions for themselves. Allows creation of advanced directives and power of attorney.

PRINCIPLES OF THE MCA Assume capacity until proven otherwise Judge by a time and decision basis: - just because someone has capacity for one decision doesn’t mean this applies to all situations. Poor decisions are still valid. Maximise decision making capabilities Act in patient's best interests

CRITERIA OF CAPACITY Is the patient able to understand information needed to make the decision? Are they able to retain this information long enough to make the decision? Are they able to weight up the pro’s and con’s of a decision? Are they able to communicate their decision?

ANY QUESTIONS?

THANK YOU!
- Slides: 58