PSHCS SEATTLE VA HOSPITAL NEUROSURGERY PROGRAM Mikhail Gelfenbeyn

PSHCS SEATTLE VA HOSPITAL NEUROSURGERY PROGRAM Mikhail Gelfenbeyn, MD, Ph. D, Chief of Neurosurgery Ali Ravanpay, MD, Ph. D, Associate Residency Program Director

AMERICA’S COMMITMENT TO HER VETERANS 1951 – a new Veterans Hospital opens in Seattle - only site where medical students “could touch a patient” 1985 – Seattle VA Hospital expansion - currently 200 beds

SEATTLE VA MISSION AND CAPACITY -Excellence in clinical care • Excellence in clinical care -Continuing thethe education • Continuing educationlegacy • Research – enhancing. Veteran care science and quality -Research – enhancing carethrough science and th improvement (5 largest research program) quality improvement Seattle VA hospital is one of two tertiary centers for VISN 20 • Spinal Cord and TBI center of excellence – national referral • Spectrum of surgery (including cardio-thoracic surgery, neurosurgery, gynecology and robotics) • Bone Marrow Transplant (only high risk BMT for US) • Lung Transplant (one of two in US) • Designated cancer center with Tele-tumor Board • Hybrid room (soon) to expand endovascular work and build new programs (e. g. TAVR) • Homeless Veteran Program (9 grant-funded transitional housing programs located across four counties)

OVERVIEW OF PROGRAM • VA resident rotation is 4 months during their 4 th year • VA team: two attendings, a resident, 2. 5 PAs, two nurse-coordinators, a scheduler

VOLUMES AND HOW THIS IMPROVES RESIDENT TRAINING • Total 250 OR cases a year • 60 cases per resident 4 months rotation • Mix of degenerative cervical and lumbar spine • Also peripheral nerve, spinal cord stimulators, intrathecal pumps, and craniotomies for brain tumors, SDH, shunts
VOLUMES AND HOW THIS IMPROVES RESIDENT TRAINING • 2600 outpatient NS clinic visits per year • Designated resident clinic for postoperative patients • Patient referrals from 5 states – WA, AK, OR, ID, MN • 60% growth in unique population in last 10 years Largest integrated health care system in the country, perhaps the world. Provides care for over 9 million veterans at 1, 243 facilities. 170 Medical Centers and 1, 063 outpatient sites of varying complexity.

FOCUS ON EDUCATION • Weekly Journal Club • Weekly Neuroradiology conference for clinic and OR cases review • Biweekly Rounds with Spinal Cord Injury Team • Introductory seminars to common Pain procedures (Pain service) and EMG/NCS (Neurology) for each resident rotation
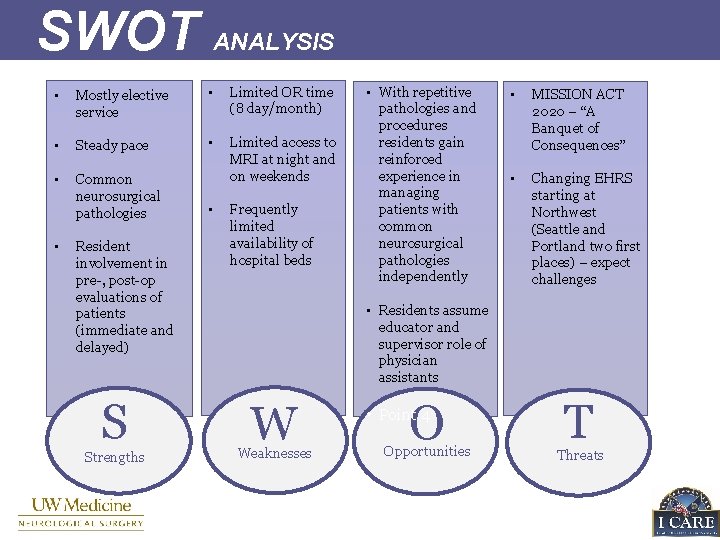
SWOT ANALYSIS • Mostly elective service • Limited OR time (8 day/month) • Steady pace • • Common neurosurgical pathologies Limited access to MRI at night and on weekends • Resident involvement in pre-, post-op evaluations of patients (immediate and delayed) S Strengths • Frequently limited availability of hospital beds • With repetitive pathologies and procedures residents gain reinforced experience in managing patients with common neurosurgical pathologies independently • MISSION ACT 2020 – “A Banquet of Consequences” • Changing EHRS starting at Northwest (Seattle and Portland two first places) – expect challenges • Residents assume educator and supervisor role of physician assistants W Weaknesses O • Point 4 Opportunities T Threats

LEARNING POINTS FROM SWOT Fertile clinical environment for residents to evolve into confident practitioners of common neurosurgical pathologies System intransigence Protracted hiring and equipment acquisition process
KEY INITIATIVES NEXT 1 -3 YEARS Local goals: -Increase the team by hiring another attending for complex spine surgeries and another PA -Expand surgeries to UW North to have more OR time -VA undergoing transition in the near future – MISSION ACT

SUMMARY/CONCLUSIONS • VA rotation is instrumental for resident outpatient evaluation skills and surgical experience • Helpful transitional phase to Chief residency
- Slides: 11