PSEUDOMONAS INTRODUCTION Pseudomonad group Aerobic nonspore forming Gram

PSEUDOMONAS

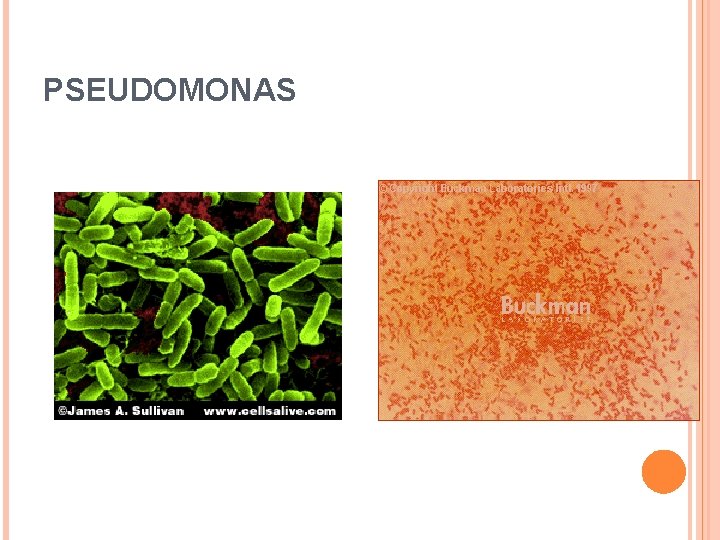
INTRODUCTION Pseudomonad group � Aerobic, non-spore forming � Gram negative straight or slightly curved rod (1 to 3 um in length), polar flagella � Term ‘aeruginosa” stems from green-blue hue � Opportunistic Pathogens of Plants, Animals, and Humans Based on Molecular analysis : - Pseudomonas species reallocated to new genera Burkholderia, Stenotrophomonas and others. •

Pseudomonas aeruginosa (formerly P. pyocyanea : bacillus pyocyaneus) Morphology Slender, Gram-negative bacilli Motile with polar flagella. Non capsulated but many strains have mucoid slime layer Isolates from Cystic fibrosis patients have abundance of extracellular polysaccharides composed of alginate polymers Escape the defence mechanisms by loose capsule in which micro colonies of bacillus are enmeshed and protected from host defences
PSEUDOMONAS

CULTURAL CHARACTERISTICS Obligate aerobe. Temp – 5 to 42 o. C. ORDINARY MEDIA : large, opaque, irregular colonies, with a distinctive, musty, mawkish or eathy smell. NA : iridscent patches with a metallic sheen, with crystals beneath the patches. Mac. Conkey : NLF BA: haemolytic Broth : dense turbidity with surface pellicle
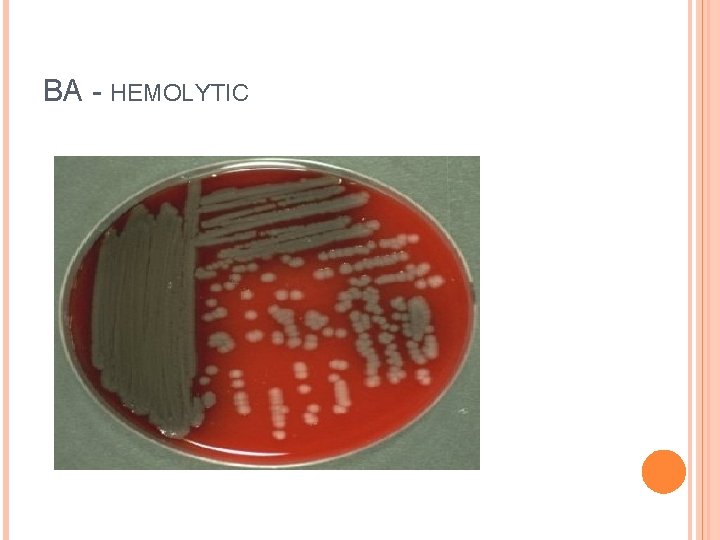
BA - HEMOLYTIC
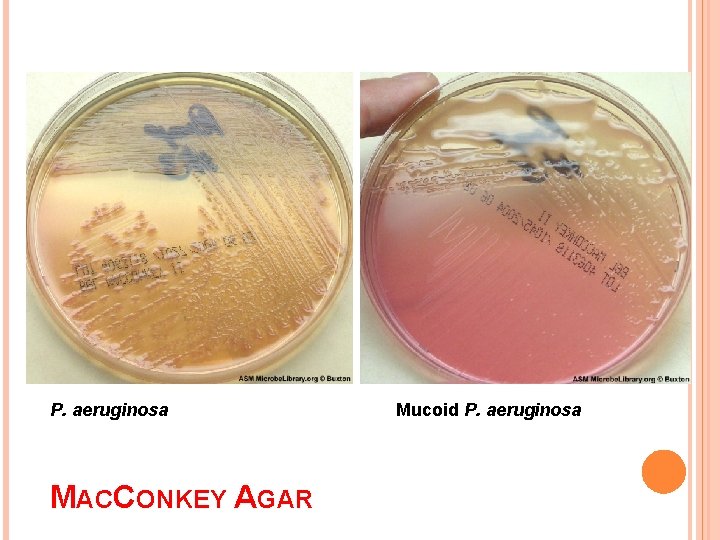
P. aeruginosa MACCONKEY AGAR Mucoid P. aeruginosa

PIGMENT PRODUCTION Pyocycanin Pyorubin Pyomelanin Pyoverdin

PIGMENT PRODUCTION Pyocycanin Bluish green phenazine pigment Produced only by p. aeruginosa Soluble in water and chloroform Pyoverdin (flourescein) Greenish yellow pigment Soluble in water & chloroform Pyorubin (red) Pyomelanin (brown)

BIOCHEMICAL REACTIONS Oxidative and fermentative Catalase, Oxidase, and Arginine tests are positive. Nitrates reduced to nitrites

CLASSIFICATION Serotyping Bacteriocin typing Bacteriophage typing All the methods of typing are replaced by molecular methods due to lack of discrimatory power.

RESISTANCE Killed at 55 oc in on 1 hour High resistance to chemical agents Resistance to quaternary ammonium compounds. Chlorxylenol Resistant to Hexchlorophenes Grows also in antiseptic bottles Dettol as cetrimide as selective medium Sensitive to acids silver salts, beta glutaraldehyde 12
EPIDEMIOLOGY Community acquired Health care associated

COMMUNITY ACQUIRED Common infection – suppurative otitis Which is a major cause of res. tract infection in cystic fibrosis patients.

HEALTH CARE ASSOCIATED Produces localised or generalised infection in hospitals. Localised Generalised

INFECTION PRODUCED BY PSEUDOMONAS IN HOSPITALS wounds, bedsores, eye infections. burns infection. iatrogenic meningitis post tracheostomy pulmonary infection Septicemia, endocarditis Ecthyma gangrenosum

PRE EMINENT ROLE OF P. A IN HOSPITALS due to its resistance to common antibiotics Its ability to establish itself widely in hospitals Extremely adaptable organism Survive and multiply with minimal nutrients and moisture.

ANTIGENIC STRUCTURE AND TOXINS Pili – adhesion Exopolysaccharide alginate – mucoid colonies seen in cultures from patients with cystic fibrosis Lipopolysaccharide – endotoxic activity Extracellular enzymes – elastases, proteases and two hemolysins Exotoxin A - Tissue necrosis, injected - lethal for animals - Blocks protein sysnthesis - Mechanism of action – diptheria toxin - Anti exotoxin A – after infection

ANTIGENIC STRUCTURE AND TOXINS - Exoenzyme S and T Bi functional enzymes GTP ase and ADP- ribosyl transferase - Exoenzyme U – Phospholipase - membrane degradation leads to lysis - Exoenzyme Y – adenyl cyclase -

FACTORS PROMOTING INFECTION Breach in primary body defences Bacterial pili (favour adhesion) Bacterial exoproducts (elastase, exotoxin A, exoenzyme S) Lipopolysaccharide (cellwall) and alginate glycocalyx. Ability to form biofilms.

PATHOGENESIS Pathogenic – areas devoid of normal defenses Examples : Disruption of mucous membrane burn wounds IV or urinary catheter usage Neutropenia Cancer chemotherapy Attachment and colonisation Invades locally, produce systemic disease

P. aeruginosa Clinical Diseases Infection of wounds and burns Ear infections (blue-green pus). Patients with Otitis externa: mild in severe burns may develop into swimmers; malignant bacteriemia. (invasive) in diabetic patients. Skin and nail infections Chronic otitis media Meningitis (when introduced by Osteochondritis of the foot. lumbar puncture). Pulmonary infection Tracheobronchitis Necrotizing pneumonia in CF patients: diffuse, bilateral bronchopneumonia with microabscess and necrosis. Eye infections: corneal ulcer. Urinary tract infection Sepsis: most cases originate from infections of lower RT, UT, and skin and soft tissue. Ecthyma gangrenosum (hemorrhagic necrosis of skin) may be seen in some patients.
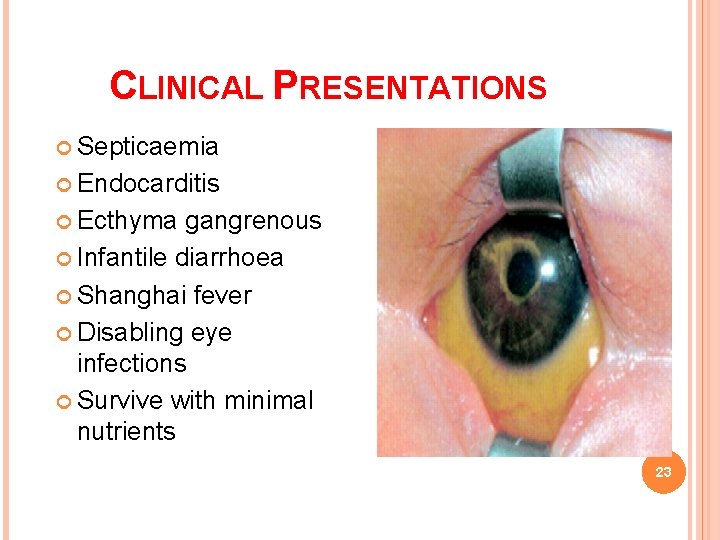
CLINICAL PRESENTATIONS Septicaemia Endocarditis Ecthyma gangrenous Infantile diarrhoea Shanghai fever Disabling eye infections Survive with minimal nutrients 23
PSEUDOMONAS AND CYSTIC FIBROSIS Pseudomonas aeruginosa is the most frequently encountered lung pathogen in patients with cystic fibrosis (CF). Following initial, often intermittent, episodes of infection, it becomes a permanently established component of the chronically infected lung in more than 80% of patients and confers an adverse prognosis 24

INFECTION OF EQUIPMENT'S Respirators Endotracheal tubes Can be Infected All equipment's to be sterilized 25

PSEUDOMONAS AND URINARY TRACT INFECTIONS Pseudomonal UTIs are usually hospitalacquired and are associated with catheterization, instrumentation, and surgery. These infections can involve the urinary tract through an ascending infection or through bacteriuic spread. In addition, these infections are a frequent source of bacteraemia. No specific characteristics distinguish this type of infection from other forms of UTI. 26

Laboratory Diagnosis- P. AERUGINOSA Specimen: skin lesions, pus, urine, blood, spinal fluid, sputum. Culture: blood agar plate and differential media. Identification of P. aeruginosa is described above. Several subtyping methods, including phage typing and molecular typing, are available for epidemiologic purposes.
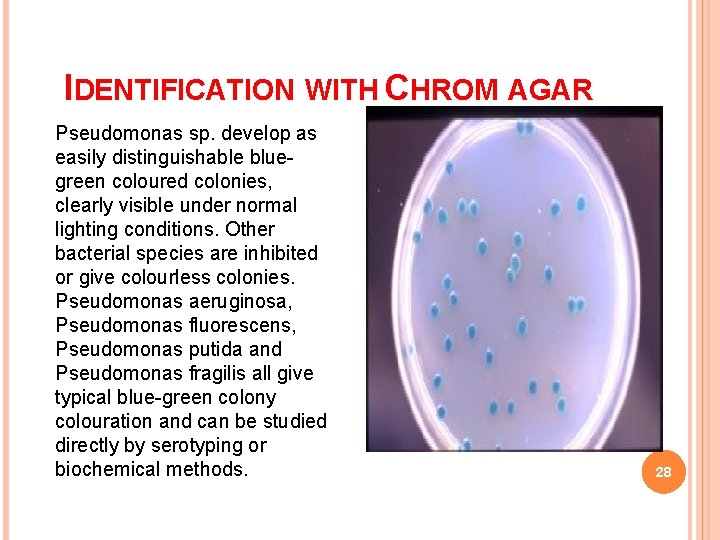
IDENTIFICATION WITH CHROM AGAR Pseudomonas sp. develop as easily distinguishable bluegreen coloured colonies, clearly visible under normal lighting conditions. Other bacterial species are inhibited or give colourless colonies. Pseudomonas aeruginosa, Pseudomonas fluorescens, Pseudomonas putida and Pseudomonas fragilis all give typical blue-green colony colouration and can be studied directly by serotyping or biochemical methods. 28

PSEUDOMONAS AERUGINOSA A RESISTANT PATHOGEN Susceptible to gentamicin, tobramycin, colistin, and amikacin The combination of gentamicin and carbenicillin is frequently used to treat severe Pseudomonas infections. 29

Prevention and Control 1. Patients at high risk should not be admitted to a ward where cases of pseudomonas infection are present. 2. Patients infected with P. aeruginosa should be isolated. 3. Sterilize all instruments, apparatus, and dressing; antimicrobial and otherapeutic substances. 4. Monitor clinically relevant isolates of P. aeruginosa by a suitable typing system to identify epidemic strains.

STENOTROPHOMONAS MALTOPHILIA (P. MALTOPHILA) Saprophyte and opportunistic pathogen BA – Lavendar green or gray colour Positive – lysine decarboxylase, Dnase, oxidation of glucose Health care settings – UTI, Wound infection, Septicemia

BURKHOLDERIA CEPACIA Formerly p. cepacia Opportunistic environmental pathogen Particularly in cystic fibrosis or chronic granulomatous disease Can grow in disinfectants and also in pencillin G using carbon as its sole source. Urinary , respiratory and wound infections, peritonitis, endocarditis and septicemia. Inherently resistant to all antibiotics.

BURKHOLDERIA MALLEI Causative agent of glanders. Disease primarily of equine animals Capable of transmitting to other animals and humans Human infection is occupational ( ostlers, grooms and vetenerians) Infection is acute or chronic Acute glanders – fever, muco purulent nasal discharge and severe prostration.

MORPHOLOGY Slender, non motile, GNB Beaded appearance Aerobe and facultative anaerobe Wide temperature Colony morphology : small and translucent, initial – yellow, ageing – opaque.

BURKHOLDERIA PSEUDOMALLEI Causative agent of melidiosis Melis , a disease of asses (glanders), edios – resemblance Motile , liquefy gelatin and form acid from several sugars Source of infection : Contamination of abrasion wounds with soil

Types : Acute and chronic Acute : Generalised infection presenting as acute septicemia Subacute typhoid like disease or pneumonia Hemoptysis resembling tuberculosis. Chronic : Multiple caseous or suppurative foci Abscess formation – skin, subcutaneous tissues, bones and internal organs.

Lab diagnosis : Microscopy : GNB, typical, bipolar, safety pin appearance with methylene blue stain Culture : isolation from sputum, pus, Blood or urine Serology : ELISA for Ig. G and Ig. M antibody, indirect haemagglutination, PCR. Drug of choice : Prolonged treatment for many months Ceftazidime along with COT, tetracycline, amoxycillin clavulanate or chloramphenicol.
- Slides: 37