Pseudomonas and Related Nonfermenters Introduction l Obligate aerobic

Pseudomonas and Related Nonfermenters

Introduction l Obligate aerobic nonfermenters, representing a mixture of opportunistic pathogens of plants, animals and humans. l Genera of significance are (out of 15): Pseudomonas (aeruginosa) Acinetobacter (baumannii) Moraxella (catarrhalis) Burkholderia (cepacia) Alcaligenes (fecalis) Stenotrophomonas (maltophilia) l l l

Pseudomonas l Pseudomonads are ubiquitous organisms found in soil, decaying organic matter, vegetation and water. l The broad environmental distribution of pseudomonas is afforded by their simple growth requirements. l More than 30 organic compounds can be used as a source of carbon and nitrogen, and some strains can even grow in distilled water by using trace nutrients.

l They are also found throughout the hospital environment; in moist reservoirs such as food, cut flowers, sinks, toilets, floor mops, respiratory therapy equipment, and even disinfectant solutions. l Persistent carriage as part of the normal microbial flora in humans is uncommon unless the individual is hospitalized or immunocompromised.

l Pseudomonas also possess a number of structures and toxins that enhance the virulence potential of the organism, as well as render them resistant to most commonly used antibiotics. l Indeed, it is surprising that these organisms are just opportunistic pathogens.

Physiology and structure l Gram-negative, motile (one polar flagellum), nonfermenters and use relatively few carbohydrates (glucose, ribose, gluconate) by oxidative metabolism. l Oxygen is the terminal electron acceptor, and the presence of cytochrome oxidase is used to differentiate this group from Enterobacteriaceae.

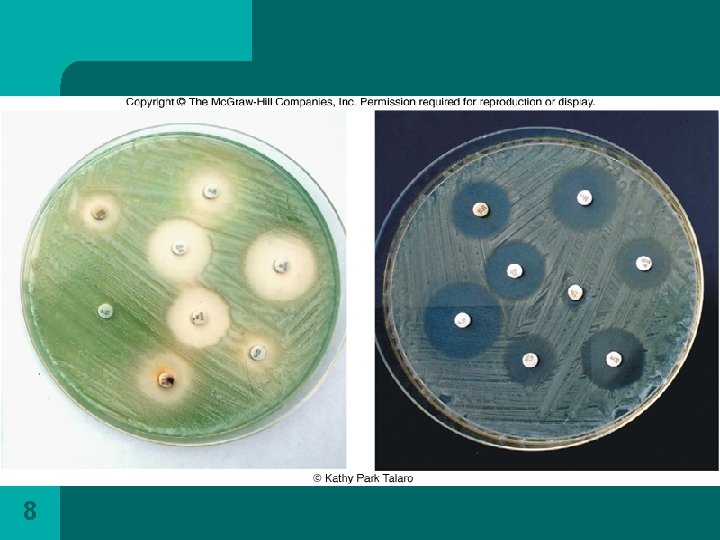
l Some strains appear mucoid because of the abundance of a polysaccharide capsule. l Some strains produce a sweet grape like odor and diffusible pigments as pyocyanin (bluish), pyoverdin (greenish), pyorubin (dark red) or pyomelanin (black). l Pseudomonas aeruginosa is the most common clinically significant and best characterized species of the genus which includes about 30 species.
8

Pathogenesis l Pseudomonads have a number of virulence factors, including structural components, toxins, and enzymes. l Structures: Pili, polysaccharide capsule, and endotoxin. l Exotoxin A: blocks eukaryotic cell protein synthesis.

l Exoenzyme S: heat-stable, can inhibit protein synthesis. l Elastase: can catalyze the destruction of the elastic fiber in blood vessel walls resulting in hemorrhagic lesions. l Phospholipase C: breaks down lipids and lecithin. l Proteases: tissue destruction, inactivation of antibodies, and inhibition of neutrophils.

Clinical Syndromes of Pseudomonas aeruginosa l Bacteremia and endocarditis: similar to that of gram negative but mortality is higher (due to host factors). Originate from other infections. l Pulmonary Infections: range from colonization or benign tracheobronchitis to severe necrotizing bronchopneumonia common in those with cystic fibrosis and chronic pulmonary disease.

Ear Infections - External otitis is most frequent with swimming as a significant risk factor (swimmer's ear). l - A more virulent form of disease (malignant external otitis) can invade the underlying tissue and be life threatening. Also associated with chronic otitis media. l Burn Infections l Ecthyma gangrenosum l Others: UTI, eye infections, CNS infections, GI infection.

Burkholderia l Burkholderia cepacia : common in hospitals causing necrotizing pneumonia and bacteremia. l Burkholderia mallei : causes glanders, a disease of animals that may be transmitted to humans. It usually begins as an ulcer of the skin and mucous membranes followed by lymphangitis and sepsis. l Burkholderia pseudomallei : causes meliodosis; a localized suppurative infection that may lead to septicemia. The most common form is pulmonary which could be chronic.

Stenotrophomons Maltophilia l A free living oxidase negative rod. l Second most commonly isolated nonfermenter as an opportunistic pathogen. l Multiresistant to antimicrobials (except cotrimoxazole).

Acinetobacter l Most commonly responsible for nosocomial respiratory infections. l Thrive in moist environments and have been found as common contaminants of respiratory therapy equipment and monitoring devices.

Pasteurellaceae l The family consists of three genera; Hemophilus, Actinobacillus and Pasteurella. l Hemophilus is the most common human pathogen of the family. l Small, gram –negative, non motile bacilli that are aerobes or facultative anaerobes. l Most are fastidious requiring enriched media for isolation.

Hemophilus l Small, sometimes pleomorphic gram-negative bacilli that are obligate parasites. l They are present on the mucous membranes of humans. l H. influenzae is the species most commonly associated with disease. l Most species require supplementation of media with growth- stimulating factors, specifically x factor (hemin) and/or v factor (NAD).

l Although both factors are present in blood enriched media, the blood must be gently heated to release the factors and destroy inhibitors of V factor. l For this reason heated blood agar (chocolate agar) is used for the in vitro isolation of Hemophilus spp. l Many strains are encapsulated with six antigenic types (a-f) and the most important of which is type b.

Pathogenesis l Hemophilus species, particularly H. parainfluenzae and non encapsulated H. influenzae colonize the upper respiratory tract in virtually all individuals within the first few months of life. l These organisms can spread locally and cause otitis media, sinusitis, bronchitis and pneumonia.

l In contrast, encapsulated H. influenzae (esp. type b) is infrequently present in the upper respiratory tract but has been a common cause of epiglottitis and pediatric meningitis. l In the absence of an opsonic antibody, high grade bacteremia can develop with dissemination to the meninges or other distal foci. l The major virulence factor is the capsule (Polyribitol phosphate-PRP) the antibody to which is protective.

Clinical Syndromes l Meningitis: Peak incidence is between 3 and 18 months of age. l Epiglottitis: characterized by cellulitis and swelling of the supraglottic tissues. It represents a life –threatening emergency. l Cellulitis: seen in very young children ( fever and cellulitis characterized by a reddish – blue color of the cheek or periorbital area)

l Arthritis : infection of a single large joint secondary to bacteremic spread. l Conjunctivitis and Brazilian Purpuric Fever. l Otitis, Sinusitis and lower Respiratory tract disease. l Dental abscesses.

Actinobacillus l Slow growers (2 -3 days) and require carbon dioxide. l A. actinomycetemocomitans is the only significant human pathogen. l The cumbersome name is derived from the fact that this organism is frequently associated with actinomyces. l It is part of the normal oropharyrgeal population detectable in about 20% of healthy individuals. l It is associated with juvenile and adult periodontitis and subacute endocarditis (following dental procedures or from periodontitis)

Pasteurella l P. multocida is the most common human pathogen of the genus. l It causes: 1 - localized infection (dog / cat scratch or bite). 2 - chronic pulmonary disease in those with underlying pulmonary dysfunction. 3 - systemic infection in immunocompromised patients.

Bordetalla l Very small, strictly aerobic gram-negative coccobacilli. Three species have been associated with human disease: - Bordetella pertussis: ( Latin for severe cough ) the agent of pertussis or whooping cough. - Bordetella parapertussis (like pertussis). - Bordetella bronchiseptica: primarily an animal pathogen but an occasional human pathogen. l l They are fastidious requiring supplementation with many nutritional factors.

Pathogenesis l Virulence is mediated by filamentous hemagglutinin, toxins, and LPS. l Filamentous hemagglutinin : agglutinates erythrocytes of a variety of animals and is believed to be important in attachment to ciliated epithelium. Antibodies to it interfere with attachment and are protective. l LPS : consists of two lipids; X and A. Major toxicity is associated with lipid X.

Toxins l Pertussis toxin - Histamine sensitizing factor, lymphocytosis promoting factor, islet cell activating protein and pertussigen. - The heat labile toxin is an A-B toxin consisting of six protein subunits. Subunit A is the active portion of the toxin whereas the pentameric B subunit is the binding portion. - It inhibits transfer of signals from cell surface receptor to intracellular mediator system. Antibodies to it confer immunity.

l Adenylate cyclase toxin - Activates conversion to AMP form ATP. - It inhibits CMI, chemotaxis, phagocytosis and killing. - It protects bacteria in the early stage of disease.

Tracheal cytotoxin - A cell wall peptidoglycan monomer that has a specific affinity for ciliated epithelial cells. l - It inhibits movement of cilia (ciliostasis ) and it interferes with DNA synthesis leading to impaired regeneration of damaged cells. - This disrupts the normal clearance mechanisms in the respiratory tree and leads to the characteristic cough. l Dermonecrotic toxin: can cause vasoconstriction of peripheral blood vessels in animals.

Clinical Picture l Infection is acquired by inhalation of infectious aerosol droplets. l Incubation of 7 -10 days and three clinical stages; - Catarrhal stage: The patient is highly infectious (1 -2 weeks). - Paroxysmal stage: Corresponds to the extrusion of ciliated epithelial cells from the respiratory tract and impaired clearance of mucus. Whooping cough paroxysm (40 -50/day) and marked lymphocytosis. (2 -4 weeks). - Convalescent stage: Paroxysms diminish in number and severity

Diagnosis - Nasopharyngeal aspirates should be immediately inoculated onto special media. - Direct fluorescent antibody test may be used. l Epidemiology - Worldwide endemicity. - No reservoir except the human host. - Decreased vaccine acceptance led to increased incidence. Whole cell inactivated vaccine has been replaced by the acellular vaccines. l

Treatment - It is primarily supportive. l - Antibiotics do not ameliorate the clinical course because convalescence is correlated with regeneration of ciliated epithelial cells. - Erythromycin is effective in eradicating the organisms and can reduce the stage of infectivity but the illness is usually unrecognized during the height of contagiousness.

Brucella l Aerobic, nonmotile, nonencapsulated, gram- negative cocobacilli that grow slowly. l Four species can infect humans; B. abortus, B. melitensis, B. suis and B. canis. l They are intracellular parasites of the RES. l Able to evade the host humoral immune response and inhibit leukocyte degranulation. l B. melitensis is the most virulent.

Clinical Picture l The disease spectrum is influenced by the infecting organism. l B. abortus and B. canis tend to produce mild disease, in contrast B. melitenis and B. suis cause severe disease with a high incidence of serious complications. l Subclinical, subacute or acute disease.

l l Diagnosis isolation of organism and serology. Treatment - Tetracycline and streptomycin or gentamicin. - Risk of relapse Epidemiology - Worldwide distribution. - Direct contact with infected animals. - Consumption of contaminated milk or cheese. - Control of disease in animals leads to its control in humans. l

Vibrionaceae l Curved or Straight bacilli that are facultative anaerobes, oxidase positive and non sporeforming. l They are primarily found in water and are well known for their ability to produce gastrointestinal disease. l Three Genera: Vibrio, Aeromonas and Plesiomonas.

The Vibrios l Gram negative, curved bacilli with a polar flagellum. l They are among the most common bacteria in surface waters worldwide. l They grow on alkaline media (p. H 8. 5 -9. 5). l V. cholerae is the most important species.

l Serogroups OI and O 139 cause classic cholera (epidemics) whereas non OI/non O 139 cause cholera like disease (sporadic). l Serotypes are Ogawa, Hikojima, and Inaba, and biotypes are classic and El Tor. l Infectious dose is very high if water is the vehicle and low if food is the vehicle in individuals with normal gastric acidity.

l V. cholerae causes cholera by a heat-labile enterotoxin (A-B toxin). l B subunit binds to the receptor promoting entry of subunit A into the cell which activates adenylate cyclase yielding high levels of intracellular c. AMP that results in prolonged hypersecretion of water and electrolytes. l Diarrhea occurs with loss of 20 -30 liters fluid per day leading to dehydration, shock, acidosis, and death.

l 60 -75% of infections are asymptomatic. l The incubation period is 1 -4 days for persons who develop symptoms followed by sudden onset of nausea, vomiting, and profuse diarrhea with abdominal cramps. l Stools, which resemble “rice water” contain mucus, epithelial cells, and large number of vibrios. l Dehydration, circulatory collapse and anuria develop with death in 25 -50% of untreated cases.

Diagnosis: - Stool culture: peptone water and TCBS agar. l • Epidemiology - V. cholerae is found in fresh water ponds and estuaries in Asia, the Middle East, Africa and along the costal areas of south, Central and North America. - Major reservoir is infected humans (carriers). - Pandemic spread (7 in the last century)

l V. parahemolyticus causes acute gastroenteritis following ingestion of contaminated sea food, an illness that is of short incubation and self limited. l V. vulnificus can cause severe wound infections after exposure to contaminated sea water and septicemia after consumption of raw oysters.

Campylobacter l Campylobacter species are curved, comma shaped, oxidase – positive , catalase – positive, microaerophilic gram- negative bacilli that are motile by means of a polar flagellum. l They are commensals of cattle, sheep, dogs, cats, rodents, and fowl. l Humans are infected due to consumption of contaminated food, milk or water. l Contaminated poultry is responsible for >50% infections.

l Presents as acute enteritis with sudden onset of crampy abdominal pain, profuse diarrhea that may be grossly bloody, headache, malaise and fever. l The illness is self limited within few days. l Systemic disease may be caused by C. fetus in immunocompromised individuals.

Helicobacter pylori l Spiral – shaped, motile (one polar flagellum) gram negative rods. l Associated with antral gastritis, duodenal (peptic) ulcer disease, gastric ulcers, and gastric carcinoma. l Most important virulence factor is urease production ( protection from gastric acids ), mucinase and adhernce factors. l It causes gastritis, peptic ulcers, and is associated with gastric cancer.
- Slides: 45