PROVIDING NUTRITION SUPPORT AFTER BARIATRIC SURGERY Presented by

PROVIDING NUTRITION SUPPORT AFTER BARIATRIC SURGERY Presented by: Aja Stokes 12/19/14
Outline of Presentation Overview of nutrition support Overview of different bariatric surgeries Need for nutrition support after bariatric surgery Medical complications of weight loss procedures Nutritional complications after bariatric procedures Estimating nutrition needs for the obese bariatric patient Indicators to assess nutrition support tolerance Conclusion

Nutrition Support Nutrition support therapy is needed when patients are unable to eat or take adequate nutrition by mouth, or have GI complications that inhibit the use of the intestinal tract for feeding over an extended amount of time
Nutrition Support cont’d Enteral Nutrition EN involves nutrition therapy via nasogastric tube, orogastric tube, gastrostomy, nasoduodenal or nasoenteric, or jejunostomy Parenteral Nutrition PN involves nutrient admixture administered via an IV into the blood with a catheter placed in a vein

Bariatric Surgery Bariatric procedures promote weight loss through restriction and/or malabsorption Approved for individuals whose BMI >/= 40 � BMI between 35 -40 if accompanied by at least one severe obesity-related comorbidity (i. e. , HLD, DM, HTN) Benefits from surgery include: reduced mortality, increased DM remission, improved beta-cell function, and improved pulmonary function

Bariatric Surgeries cont’d Roux-en-Y-gastric bypass (RYGB) � Surgeon creates a small gastric pouch with the capacity of 20 -30 m. L from the proximal and attaches it to the roux limb of the jejunum
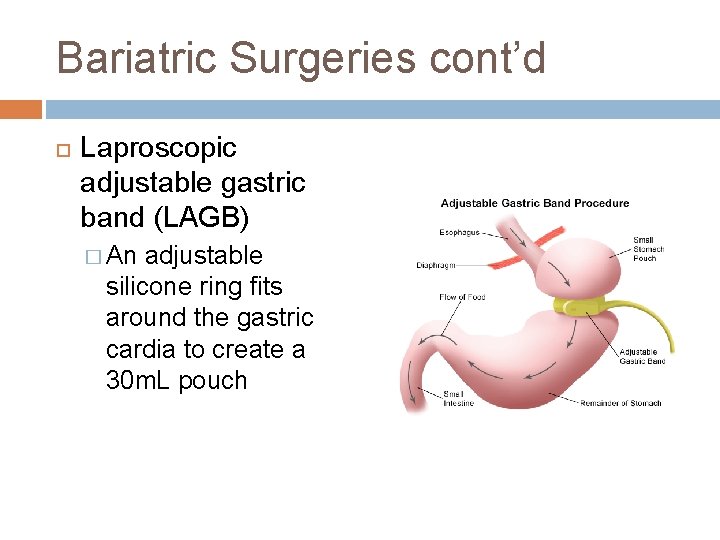
Bariatric Surgeries cont’d Laproscopic adjustable gastric band (LAGB) � An adjustable silicone ring fits around the gastric cardia to create a 30 m. L pouch

Bariatric Surgeries cont’d Vertical Sleeve gastrectomy � Cutting the antrum of the stomach 2 -6 cm away from the pylorus and forming a tubular pouch � Stomach capacity is reduced by about 80 percent through the removal of the fundus and body
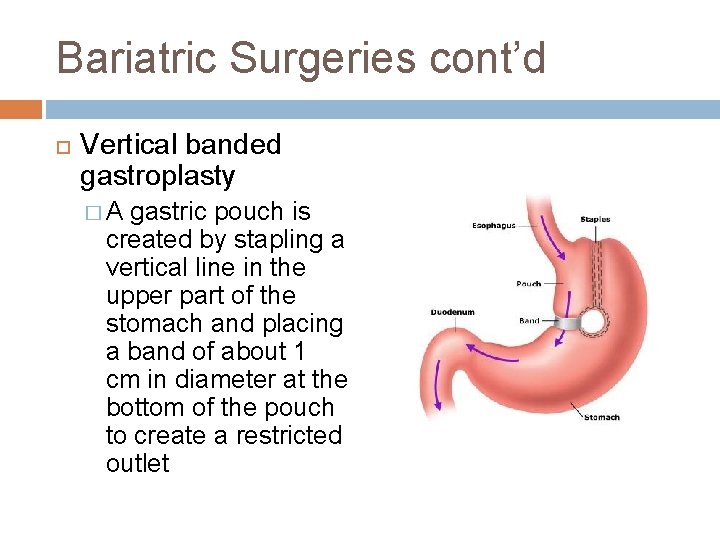
Bariatric Surgeries cont’d Vertical banded gastroplasty �A gastric pouch is created by stapling a vertical line in the upper part of the stomach and placing a band of about 1 cm in diameter at the bottom of the pouch to create a restricted outlet
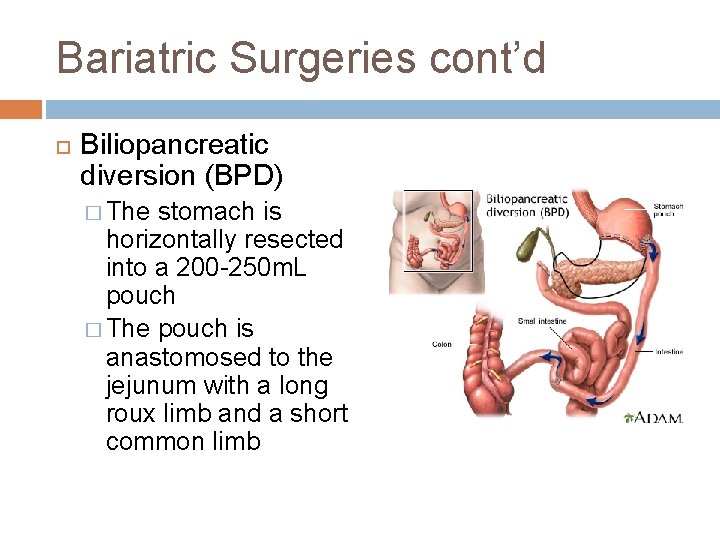
Bariatric Surgeries cont’d Biliopancreatic diversion (BPD) � The stomach is horizontally resected into a 200 -250 m. L pouch � The pouch is anastomosed to the jejunum with a long roux limb and a short common limb
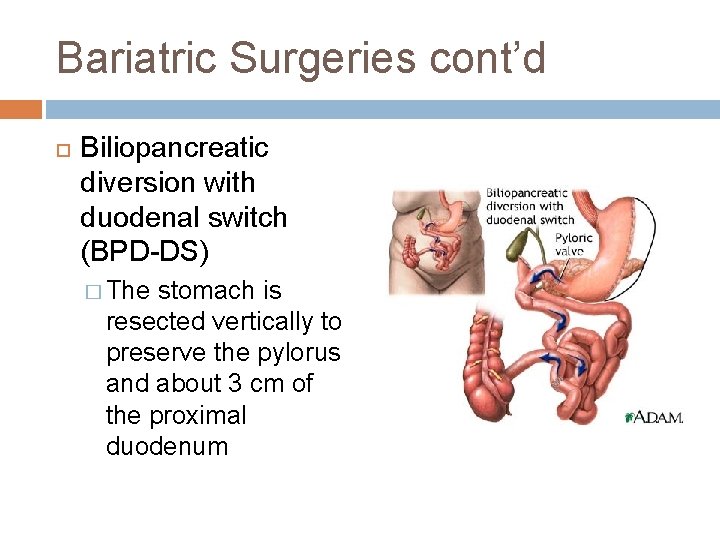
Bariatric Surgeries cont’d Biliopancreatic diversion with duodenal switch (BPD-DS) � The stomach is resected vertically to preserve the pylorus and about 3 cm of the proximal duodenum
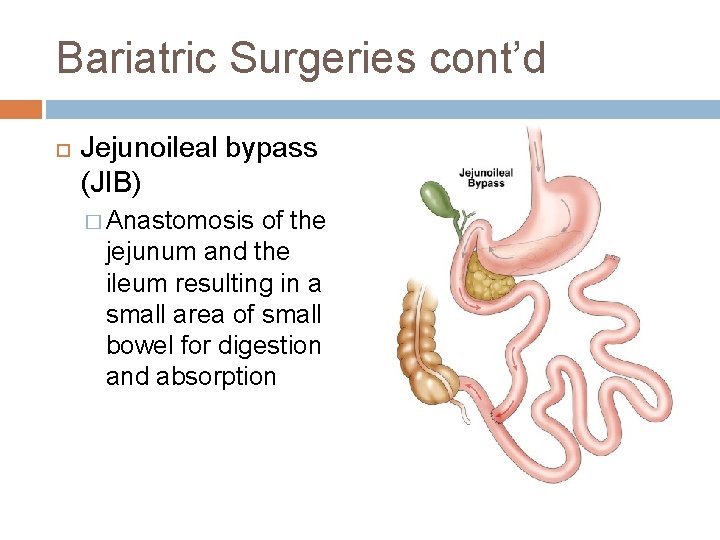
Bariatric Surgeries cont’d Jejunoileal bypass (JIB) � Anastomosis of the jejunum and the ileum resulting in a small area of small bowel for digestion and absorption

Need for Nutrition Therapy after Bariatric Surgery Indications for EN: � During first 7 days of admission (in wellnourished patients) � Must have functional gastrointestinal tract and ability to safely insert an enteral feeding tube � Enterocutaneous fistula where the enteral feeding tube can be inserted distal to the fistula � Inadequate oral intake to meet metabolic demands (i. e. , trauma, burn, or other critically -ill patients) � Significant malnutrition

Need for Nutrition Therapy after Bariatric Surgery cont’d Indications for PN: � Inability to take oral or enteral nutrition for >710 days (5 -7 days in ICU setting) � Entercutaneous fistula where the enteral feeding tube can not be inserted distal to the fistula � Ileus � Intestinal obstruction � Intractable vomiting � Intractable diarrhea � Severe gastrointestinal bleeding � Severe malabsorption � Severe malnutrition with inability to obtain enteral access � Contraindication to enteral nutrition � Poor tolerance to enteral nutrition
Medical Complications EN Nutrition Complications Abdominal bloating Aspiration Constipation Dehydration Diarrhea Electrolyte disturbances Feeding tube clog High gastric residuals Hyperglycemia Infection around tube insertion site Vitamin and mineral deficiency

Medical Complications cont’d PN Nutrition Complications Catheter-related blood stream infection Dehydration Electrolyte disturbances Essential fatty acid deficiency Hyperglycemia Hypoglycemia Intestinal atrophy Metabolic bone disease Parenteral nutritionassociated liver disease Volume overload Vitamin and/or trace element deficiencies or excess
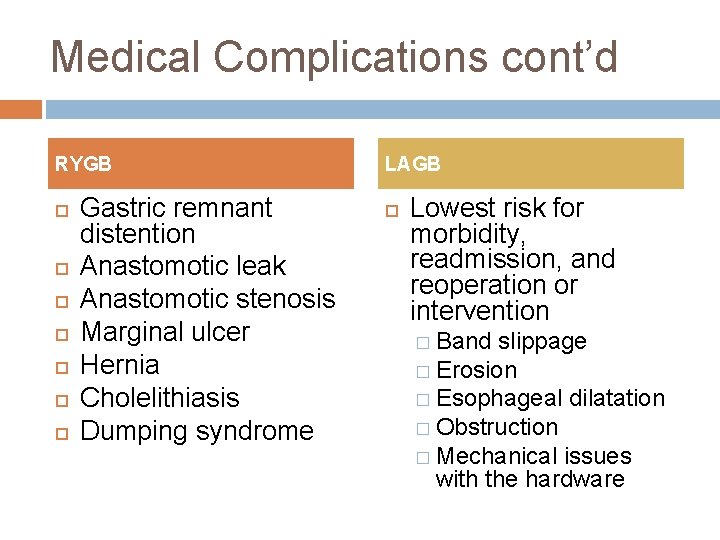
Medical Complications cont’d RYGB Gastric remnant distention Anastomotic leak Anastomotic stenosis Marginal ulcer Hernia Cholelithiasis Dumping syndrome LAGB Lowest risk for morbidity, readmission, and reoperation or intervention � Band slippage � Erosion � Esophageal dilatation � Obstruction � Mechanical issues with the hardware
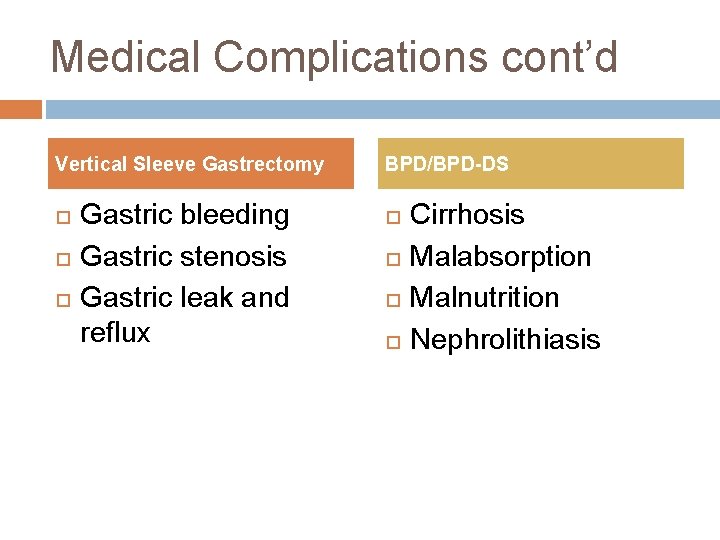
Medical Complications cont’d Vertical Sleeve Gastrectomy Gastric bleeding Gastric stenosis Gastric leak and reflux BPD/BPD-DS Cirrhosis Malabsorption Malnutrition Nephrolithiasis

Nutritional Complications Nutrition-related complications occur in about 30% of patients
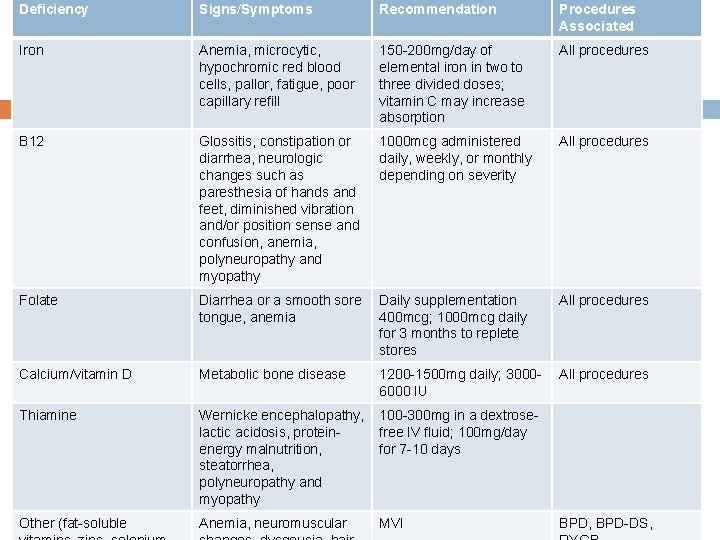
Deficiency Signs/Symptoms Recommendation Procedures Associated Iron Anemia, microcytic, hypochromic red blood cells, pallor, fatigue, poor capillary refill 150 -200 mg/day of elemental iron in two to three divided doses; vitamin C may increase absorption All procedures B 12 Glossitis, constipation or diarrhea, neurologic changes such as paresthesia of hands and feet, diminished vibration and/or position sense and confusion, anemia, polyneuropathy and myopathy 1000 mcg administered daily, weekly, or monthly depending on severity All procedures Folate Diarrhea or a smooth sore tongue, anemia Daily supplementation 400 mcg; 1000 mcg daily for 3 months to replete stores All procedures Calcium/vitamin D Metabolic bone disease 1200 -1500 mg daily; 30006000 IU All procedures Thiamine Wernicke encephalopathy, lactic acidosis, proteinenergy malnutrition, steatorrhea, polyneuropathy and myopathy 100 -300 mg in a dextrosefree IV fluid; 100 mg/day for 7 -10 days Other (fat-soluble Anemia, neuromuscular MVI BPD, BPD-DS,

Estimating Nutrition Needs Calculating energy needs � Hypocaloric 11 feeding to 14 kcals/kg ABW 22 to 25 kcals/kg IBW

Estimating Nutrition Needs cont’d Calculating protein needs � 2. 0 g/kg IBW if BMI= 30 to 39. 9 � 2. 5 g/kg IBW if BMI >/= 40 Calculating fluid needs � No recommendations provided by SCCM/A. S. P. E. N. � Minimum requirement is generally 1. 5 L/day
Indicators to assess nutrition support tolerance Lab measures � Fasting glucose � CRP � Prealbumin � Electrolytes � Nitrogen balance Weight Trends Gastric residuals Adequate wound healing Functional status

Conclusion EN and PN are not often used in the bariatric surgery patient In general, � Protein intake between 2 -2. 5 g/kg (depending on BMI) Wound healing Builds muscle Maintain lean body mass Muscle burns calories May help prevent hair loss Fights infection � Daily supplementation (MVI, iron, B 12, calcium, vitamin D)

Conclusion cont’d Nutrition intervention should be individualized for patients who have undergone bariatric surgery not only in consideration of obesity, but also due to altered gastrointestinal anatomy RD should work with surgical team to create a nutrition plan to stabilize the patients nutrition status
References Fujioka, K. , Di. Baise, J. K. , and Martindale, R. G. (2011). “Nutrition and Metabolic After Bariatric Surgery and Their Treatment. ” Journal of Parenteral and Enteral Nutrition; 35, 52 S-59 S Kerner, Jennifer. (2014). “Nutrition Support After Bariatric Surgery. ” Support Line: A Publication of Dietitians in Nutrition Support; 36(3), 9 -21 Mogensen, Kris M. (2010). “Nutrition Support Therapy for the Bariatric Patient. ” Weight Management Matters; 7(3), 8 -16
- Slides: 26