Provider Directory Subject Matter Expert Workgroup Meeting 3

Provider Directory Subject Matter Expert Workgroup Meeting #3 April 2, 2014 1
Welcome, March meeting review, agenda review Karen Hale and Susan Otter 2

Agenda Review & March meeting recap � Agenda Review � Direct Secure Messaging � Federated HPD/Common Credentialing data presentation � Breakout session – Key Provider Directory Uses (HIE/Analytics/Operations) � Group discussion of use cases � Wrap up and next steps � March meeting recap � Questions 3 or any other updates from group?

Direct Secure Messaging Presentation Lisa Parker 4

Direct Secure Messaging Overview � Direct secure messaging is a secure, encrypted webbased communication system for healthcare practitioners to share protected health information (PHI) � Allows structured data to be shared from an Electronic Health Record (EHR) (or web portal) that can be ingested directly into an EHR to become part of the patient’s health record data � Allows messages to only be shared between trusted, vetted parties across organizational boundaries and EHR vendors � HIPAA 5 compliant

Elements to achieve statewide Direct secure messaging 1. Organizations must use a Health Information Service Provider (HISP) to communicate with providers outside their organization and/or their specific EHR 2. An organization’s HISP must be a member of a “trust community” to connect with providers participating in a different HISP 3. Direct secure messaging addresses must be known, made available or searchable: • Directories are sometimes a part of a HISP or “trust community” • currently no statewide directory available in Oregon; OHA is developing an interim solution 6
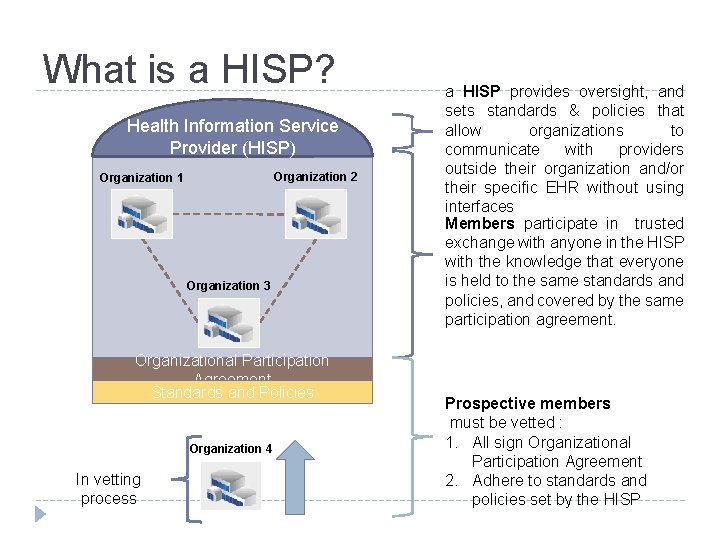
What is a HISP? Health Information Service Provider (HISP) Organization 2 Organization 1 Organization 3 Organizational Participation Agreement Standards and Policies Organization 4 In vetting process a HISP provides oversight, and sets standards & policies that allow organizations to communicate with providers outside their organization and/or their specific EHR without using interfaces Members participate in trusted exchange with anyone in the HISP with the knowledge that everyone is held to the same standards and policies, and covered by the same participation agreement. Prospective members must be vetted : 1. All sign Organizational Participation Agreement 2. Adhere to standards and policies set by the HISP
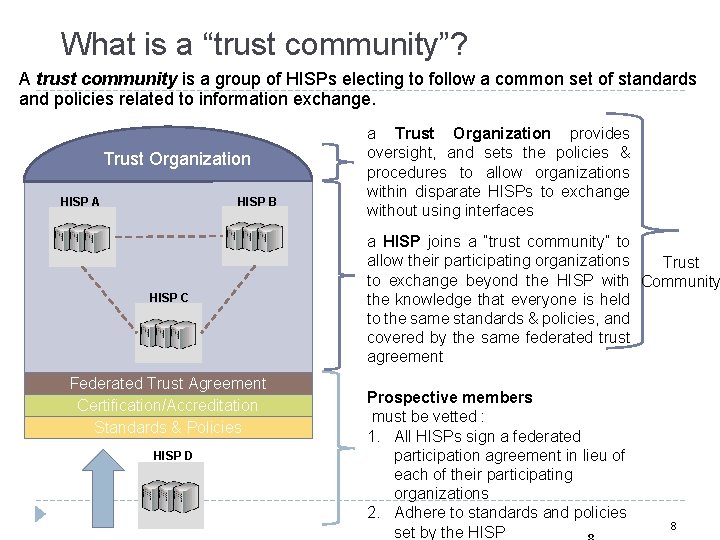
What is a “trust community”? A trust community is a group of HISPs electing to follow a common set of standards and policies related to information exchange. Trust Organization HISP A HISP B HISP C Federated Trust Agreement Certification/Accreditation Standards & Policies HISP D a Trust Organization provides oversight, and sets the policies & procedures to allow organizations within disparate HISPs to exchange without using interfaces a HISP joins a “trust community” to allow their participating organizations Trust to exchange beyond the HISP with Community the knowledge that everyone is held to the same standards & policies, and covered by the same federated trust agreement Prospective members must be vetted : 1. All HISPs sign a federated participation agreement in lieu of each of their participating organizations 2. Adhere to standards and policies set by the HISP 8
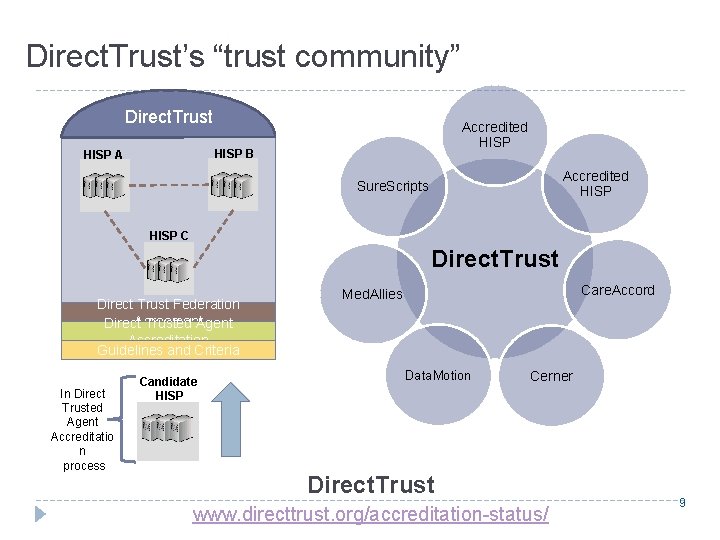
Direct. Trust’s “trust community” Direct. Trust Accredited HISP B HISP A Accredited HISP Sure. Scripts HISP C Direct. Trust Direct Trust Federation Direct. Agreement Trusted Agent Accreditation Guidelines and Criteria In Direct Trusted Agent Accreditatio n process Candidate HISP Care. Accord Med. Allies Data. Motion Cerner Direct. Trust www. directtrust. org/accreditation-status/ 9
Direct. Trust Fully Accredited HISPs 0 EHNAC – Electronic Healthcare Network Accreditation Commission DTAAP – Direct Trusted Agent Accreditation Program 4/2/14 as of

Direct. Trust Candidates for Accreditation EHNAC – Electronic Healthcare Network Accreditation Commission DTAAP – Direct Trusted Agent Accreditation Program 4/2/14 as of

Why does Oregon need a state level provider directory for Direct secure messaging? Direct secure messaging addresses must be known, made available or searchable • • • directories are sometimes a part of a HISP or “trust community” currently no statewide directory available in Oregon OHA is developing an interim solution • Piloting flat file solution for 2014 for Oregon entities with a Direct. Trust accredited HISP Value of Direct secure messaging supported with provider directory Care coordination across organizational boundaries Interoperability of information (exchange without interfaces) • Electronic exchange of structured clinical information • • Policy Levers • Federal: Support Stage 2 Meaningful Use requirements • State: Statewide goal to promote Direct secure messaging; State 12 contracts promoting HIT/HIE; Oregon’s Patient-Centered Primary Care
Federated HPD and Common Credentialing Data Crosswalk John Hall 13

The Big Picture – Where we end up in 2015 � Federal Healthcare Provider directory (HPD) standards are in place that place criteria on how these data are stored and shared in EHRs � Common credentialing database is beginning to capture credentialing data (fully functional in January 2016) � Stand-alone healthcare directories are connected via federated provider directory services Web Portal � Orchestrator “Hub” � Centralized database for some components � � Those with HPD capabilities can connect to the network of Oregon directories and Interstate Directories � Those without HPD capabilities can interact via flat-file exchange with the centralized components of the directory 14
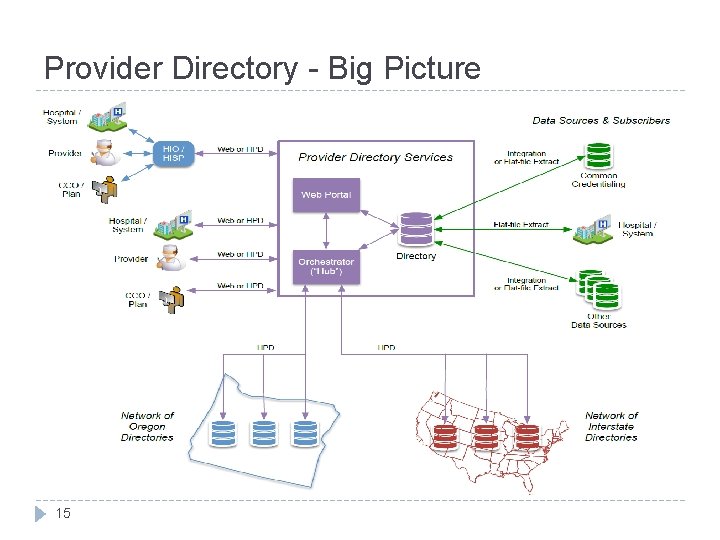
Provider Directory - Big Picture 15
Leveraging state and federal efforts Emerging Federated HPD standard for provider directories 16 Common credentialing efforts underway that ensure data accuracy

Background on OPCA � Oregon Practitioner Credentialing Application Practitioner demographics � Medical specialty � Practice information � � Primary/Additional � practices Hospital/Healthcare affiliations � Starting point for implementing the Oregon Common Credentialing Solution Analysis of RFI responses completed � Rules to be effective June 2014 � RFP to be issued by June 2014 � � Decision � 17 point for possible data elements included in the OCCS Award contract by October 2014

Background on Federated HPD � Federated Healthcare Provider Directory (HPD) is a technology standard for how to “talk” to healthcare directories and describes a minimum set of data supported by those directories Emerging version of HPD � Builds upon HPD Plus v 1. 1 protocol and data model � Adds capabilities supporting federated directory networks � � ONC and Integrating the Healthcare Enterprise (IHE) are collaborating to advance Federated HPD, with the final specification to be published in 2014 18

National Adoption of Federated HPD � Adoption of Federated HPD is anticipated to be widespread Federated HPD seen as the strongest contender enabling a nationwide directory infrastructure � Some vendors are already building to (draft) Federated HPD – Federated HPD Demonstration at HIMSS 2014 conference included Surescripts, Verizon, and other directory vendors � Products supporting Federated HPD could be available as early as 2014, but broad support more likely will be 2015 to early 2016 based on typical vendor product development cycles. � 19

Federated HPD Data Model Credentials • Information about where a provider is credentialed (includes credentialed date and expiration) • Can also represent professional qualifications (e. g. , degrees, certifications) Memberships • Indicates affiliations between individuals and organizations • Includes contact and Services information for the individual specific to the affiliation Organizations • Represents organizational entities • Includes identifying information such as name, legal address, and contact, plus items such as languages supported pointers to Services Providers • Represents individual healthcare professionals • Includes identifying information such as name, profession, specialization, addresses (legal, billing, postal), and contact information, plus items such as status (primary, other, inactive) Services • Contains health information exchange information for an individual or organization, including Direct address and query endpoint 20

Expressing OPCA data in Federated HPD � Initial analysis indicates most of the OPCA data can be expressed using the Federated HPD data model. � Some gaps appear to be indicated, but analysis continues. � Any indicated gaps do not necessarily mean particular data cannot be stored in the statewide Provider Directory Services. More on this after the next slide… 21
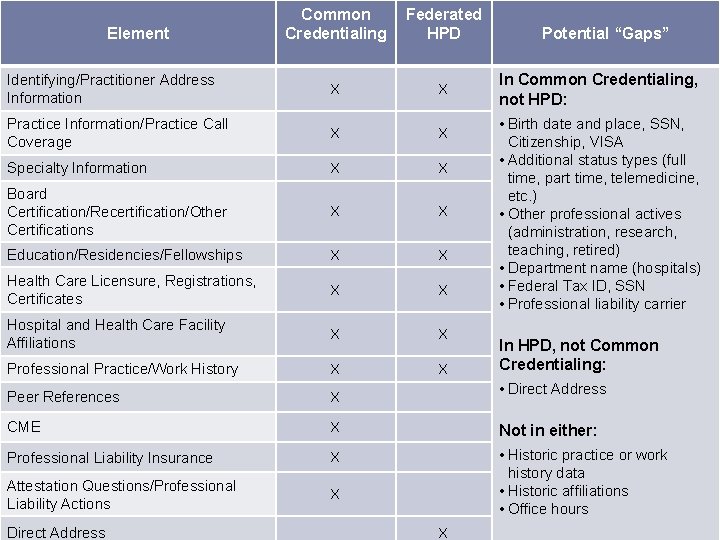
Common Credentialing Federated HPD Identifying/Practitioner Address Information X X Practice Information/Practice Call Coverage X X Specialty Information X X Board Certification/Recertification/Other Certifications X X Education/Residencies/Fellowships X X Health Care Licensure, Registrations, Certificates X X Hospital and Health Care Facility Affiliations X X Professional Practice/Work History X X Peer References X CME X Not in either: Professional Liability Insurance X Attestation Questions/Professional Liability Actions X • Historic practice or work history data • Historic affiliations • Office hours Element In Common Credentialing, not HPD: • Birth date and place, SSN, Citizenship, VISA • Additional status types (full time, part time, telemedicine, etc. ) • Other professional actives (administration, research, teaching, retired) • Department name (hospitals) • Federal Tax ID, SSN • Professional liability carrier In HPD, not Common Credentialing: • Direct Address 22 Direct Address Potential “Gaps” X

Operations and Limitations for Federated HPD � � Querying for and accessing data beyond the standard data model using Federated HPD may pose challenges. � Products used to access directories via Federated HPD may not have the necessary capabilities enabling its users to query for data outside the standard data model. � If a product does allow queries for non-standard data, users may not be aware that such data exists to be queried in the first place or how to use their product to make such queries. � No guarantees that products will be able to display (properly or at all) data received that falls outside the standard Federated HPD data model. Oregon could advocate and work through the Federated HPD standards process to extend the potential of the standard data model. In the meantime, however, other options supporting query and access of such data include: � Web portal of the statewide Provider Directory Services � Extracts for data subscribers � Integration with data subscribers � 23 Use cases will determine which options make sense and when.

A word on historical data. . . Directories are data repositories for “point in time” data � As such, no applicable standards or data models support versioning of information or provide time indicators delimiting applicability of data (i. e. , no directory standards enable queries for relationships in place or data values that were “good” at a given time or time period) � Oregon’s statewide Provider Directory Services could still support queries for historical data via one or more options: � � Periodic repository snapshots Parallel “read only” directories containing data and relationships as they were at defined times Better understanding of use cases in this area will help target the right approach(es). 24
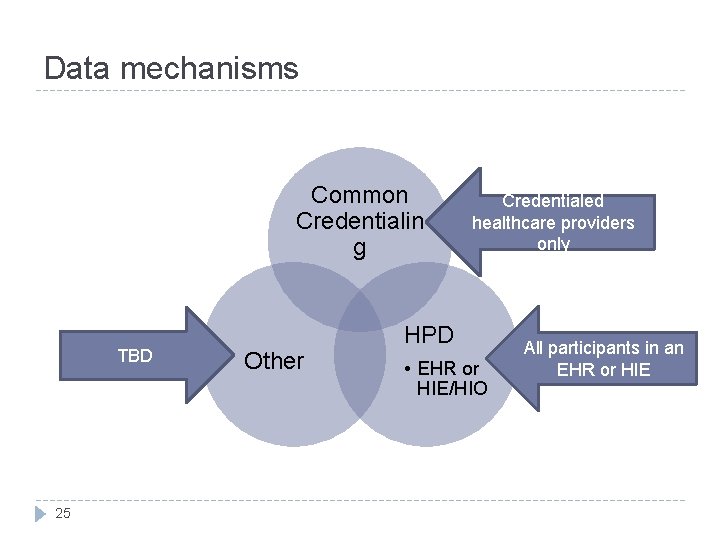
Data mechanisms Common Credentialin g TBD 25 Other Credentialed healthcare providers only HPD • EHR or HIE/HIO All participants in an EHR or HIE

Provider Directory Uses Karen Hale, Susan Otter, and Group 26
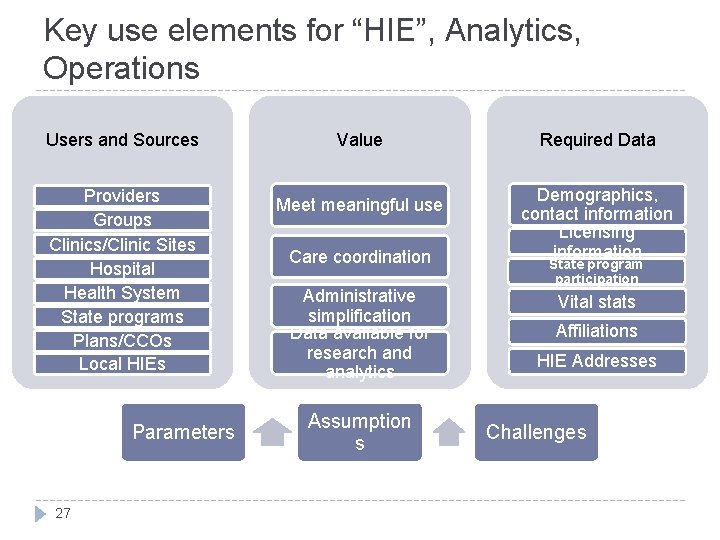
Key use elements for “HIE”, Analytics, Operations Users and Sources Value Providers Groups Clinics/Clinic Sites Hospital Health System State programs Plans/CCOs Local HIEs Meet meaningful use Parameters 27 Care coordination Administrative simplification Data available for research and analytics Assumption s Required Data Demographics, contact information Licensing information State program participation Vital stats Affiliations HIE Addresses Challenges
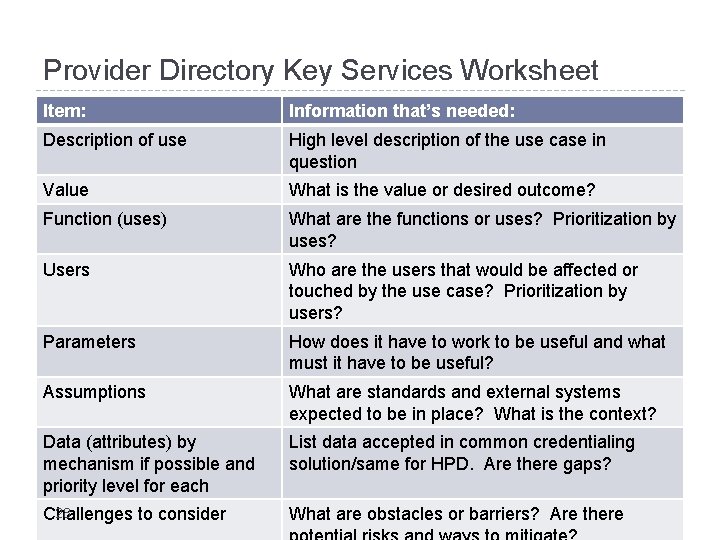
Provider Directory Key Services Worksheet Item: Information that’s needed: Description of use High level description of the use case in question Value What is the value or desired outcome? Function (uses) What are the functions or uses? Prioritization by uses? Users Who are the users that would be affected or touched by the use case? Prioritization by users? Parameters How does it have to work to be useful and what must it have to be useful? Assumptions What are standards and external systems expected to be in place? What is the context? Data (attributes) by mechanism if possible and priority level for each List data accepted in common credentialing solution/same for HPD. Are there gaps? 28 Challenges to consider What are obstacles or barriers? Are there
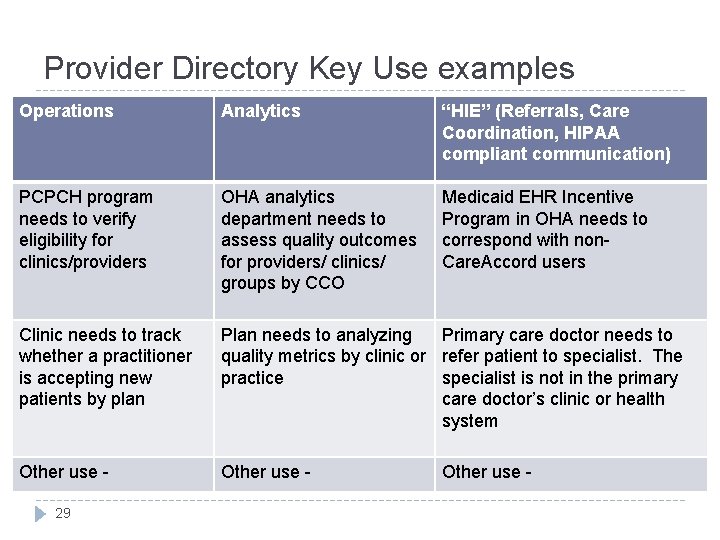
Provider Directory Key Use examples Operations Analytics “HIE” (Referrals, Care Coordination, HIPAA compliant communication) PCPCH program needs to verify eligibility for clinics/providers OHA analytics department needs to assess quality outcomes for providers/ clinics/ groups by CCO Medicaid EHR Incentive Program in OHA needs to correspond with non. Care. Accord users Clinic needs to track whether a practitioner is accepting new patients by plan Plan needs to analyzing Primary care doctor needs to quality metrics by clinic or refer patient to specialist. The practice specialist is not in the primary care doctor’s clinic or health system Other use - 29 Other use -
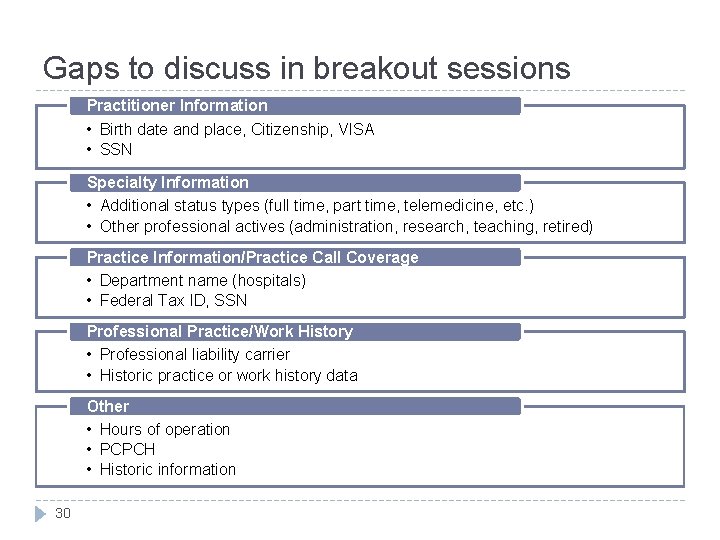
Gaps to discuss in breakout sessions Practitioner Information • Birth date and place, Citizenship, VISA • SSN Specialty Information • Additional status types (full time, part time, telemedicine, etc. ) • Other professional actives (administration, research, teaching, retired) Practice Information/Practice Call Coverage • Department name (hospitals) • Federal Tax ID, SSN Professional Practice/Work History • Professional liability carrier • Historic practice or work history data Other • Hours of operation • PCPCH • Historic information 30
Group Breakout Session “HIE” • Gina, Erick, Bob, Hongcheng Analytics • Jessica, Stephanie, Christopher, Ray Operations • Mary Kaye, Tina, Rebecca, Liz 31

Group Discussion of Use Cases Karen Hale, Susan Otter, and Group 32

Wrap up and next steps Karen Hale & Susan Otter 33

Next Meeting Date Location April 23 rd Salem – State Library 250 Winter Street NE, Conference Room 103 May 14 th Portland – State Office Building 800 NE Oregon Street, Conference Room 1 C 34
- Slides: 34