Protein Synthesis Inhibitors BY S Bohlooli Ph D

Protein Synthesis Inhibitors BY S. Bohlooli, Ph. D School of Medicine, Ardabil University of Medical Sciences

Protein Synthesis Inhibitors n n n n Tetracyclines Amimoglycosides Macrolides Clindamycin Chloramphenicol Streptogramines Oxazolidinones
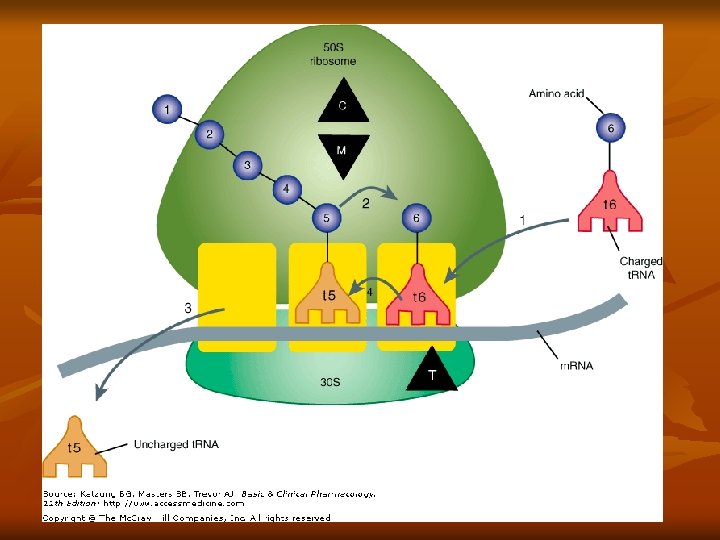

Tetracycline n n First compound, chlortetracycline introduced in 1948 Highly effective against rickettsiae, gm + and – bacteria, chlamydia Inhibit protein synthesis by reversibly binding to 30 S subunit of bacterial ribosome, preventing binding of aminoacyl t. RNA to m. RNA ribosomal complex Bacteriostatic
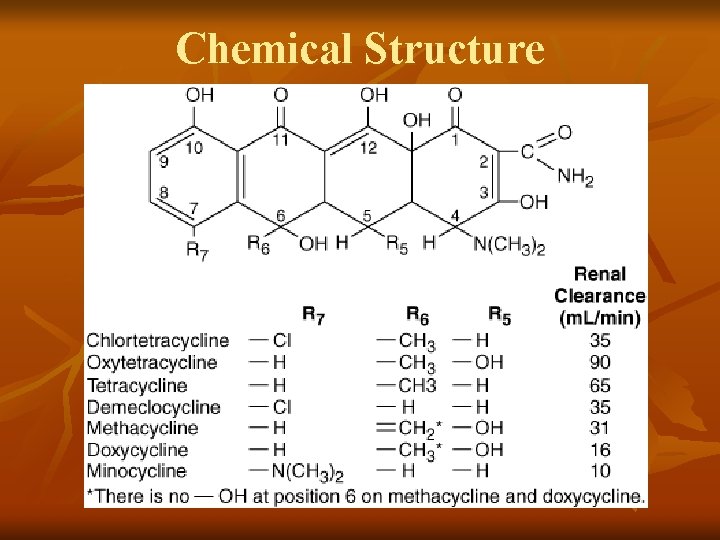
Chemical Structure
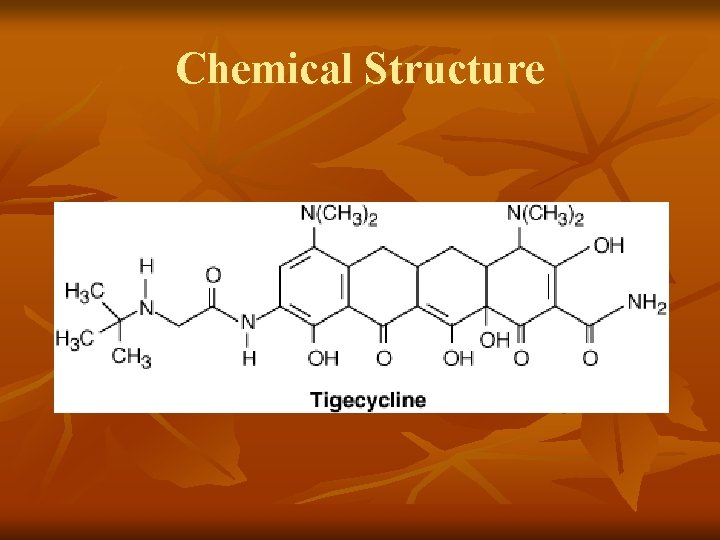
Chemical Structure
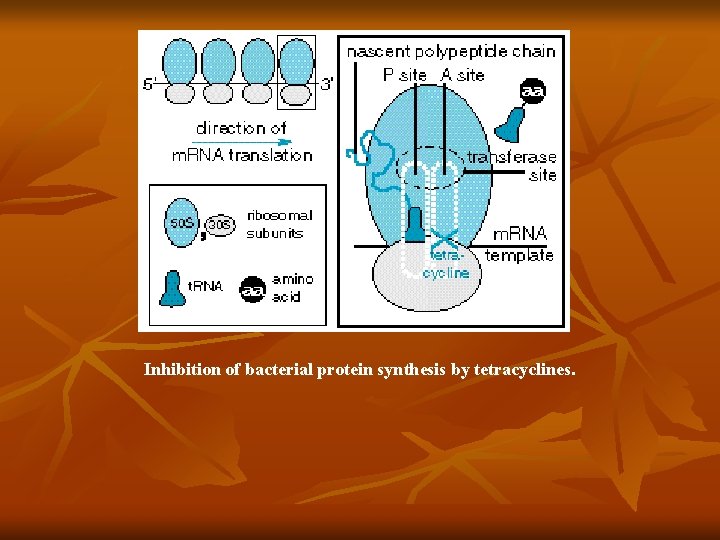
Inhibition of bacterial protein synthesis by tetracyclines.

Resistance n n Wide resistance limits clinical uses Most penicillinase-producing staphylococci are resistant

Absorption n n Incomplete GI absorption: tetracycline (6080%), doxycycline (95%), minocycline (100%) Dairy foods decrease absorption by forming nonabsorbable chelates with calcium ions; also Mg, Fe, Al (antacids)
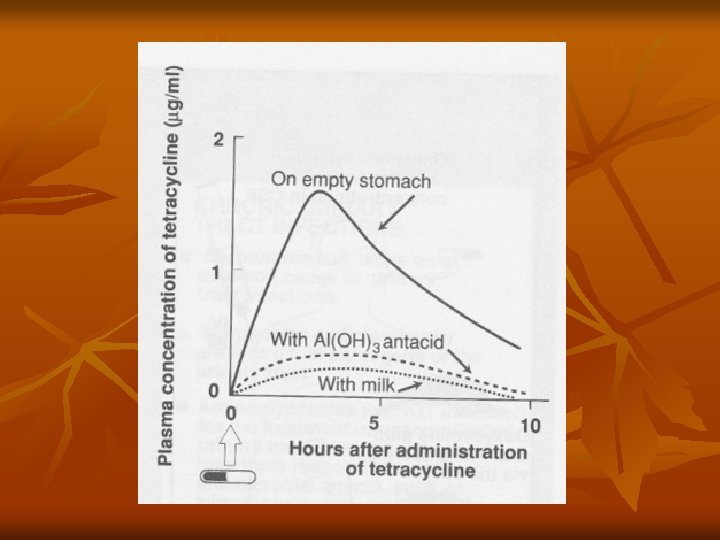

Distribution n n Widely distributed in body Bind in tissues undergoing calcification (teeth, bones) or tumors with high calcium content (gastric carcinoma) All cross placenta and concentrate in fetal bones and teeth Minocycline best CSF penetration n Concentrated in saliva and gingival fluid

Excretion n Concentrate in liver and partially metabolized Secreted into bile and excreted in urine Doxycycline and minocycline largely excreted in feces n Use in renal insufficiency

General Therapeutic Uses n Lyme disease n n n Mycoplasma pneumonia n n Young adult pneumonia Rocky mountain spotted fever n n Spirochete (Borelia burgdorferi) tick bite Skin lesions, headache, fever, meningioencephalitis, arthritis Fever, chills, bone and joint aches Acne

General Therapeutic Uses n Chlamydia n n n Lymphogranuloma venereum- lymph node hypertrophy, obstruction, elephantiasis Psittacosis- pneumonia, hepatitis, myocarditis, coma Cholera n n Ingested fecally contaminated food or water Organism multiplies in GI tract and secretes enterotoxin producing diarrhea Doxycycline reduces organism Fluid replacement

Adverse Effects n GI discomfort n n Hepatic injury n n Anorexia, epigastric pain, abdominal distention, nausea, vomiting, diarrhea, sore mouth, perianal irritation Increased during pregnancy Nephrotoxicity

Adverse Effects n Teeth n n Depression of bone growth n n Deposition in fetal and growing bones, stunted growth Photosensitization n n Discoloration enamel and hypoplasia of teeth Severe sunburn in sun; doxy/demeclocycline Superinfections n Candida or GI staphylococcus

Contraindications n n n Pregnancy Children Renal insufficiency n Can use doxycycline

Drug Interactions n n Do not give with other antibiotics unless establish synergy Increased effects of anticoagulants Not absorbed by cations like Ca, Mg, Fe, Al H 2 blockers may depress tetracycline uptake

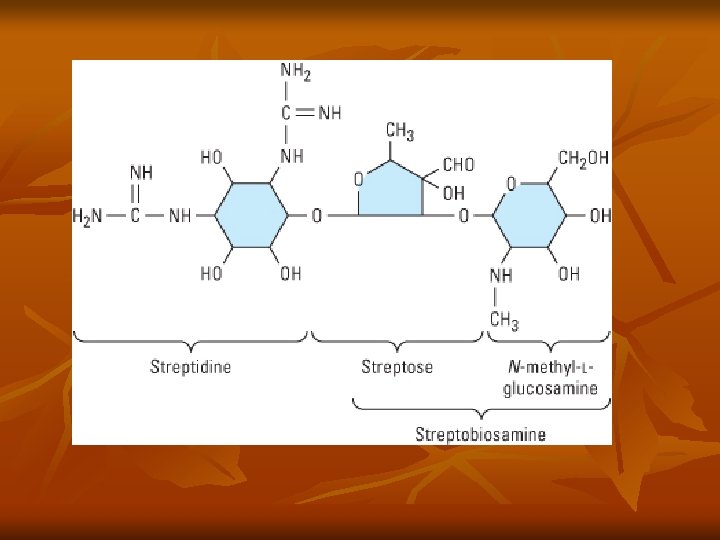
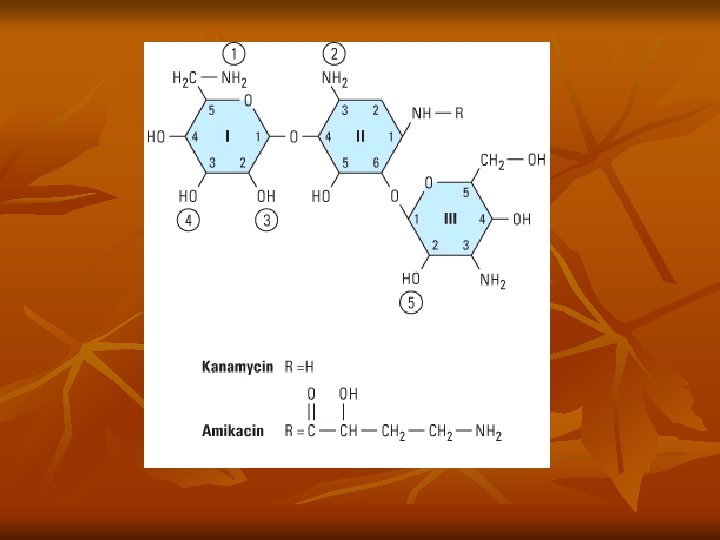
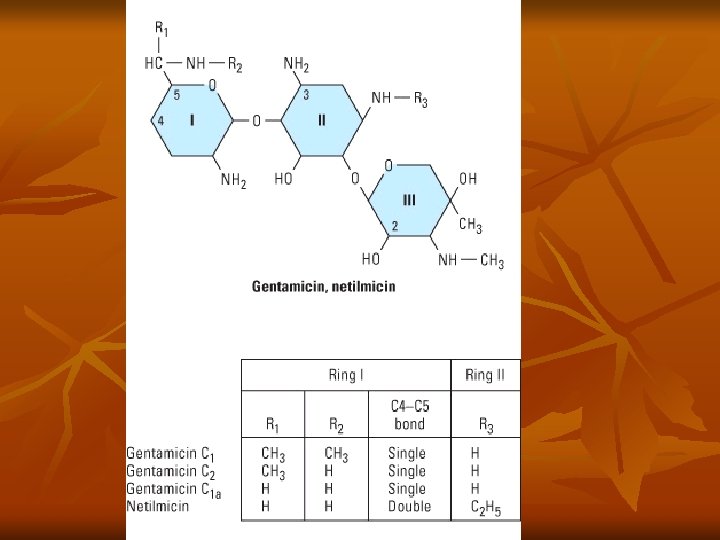
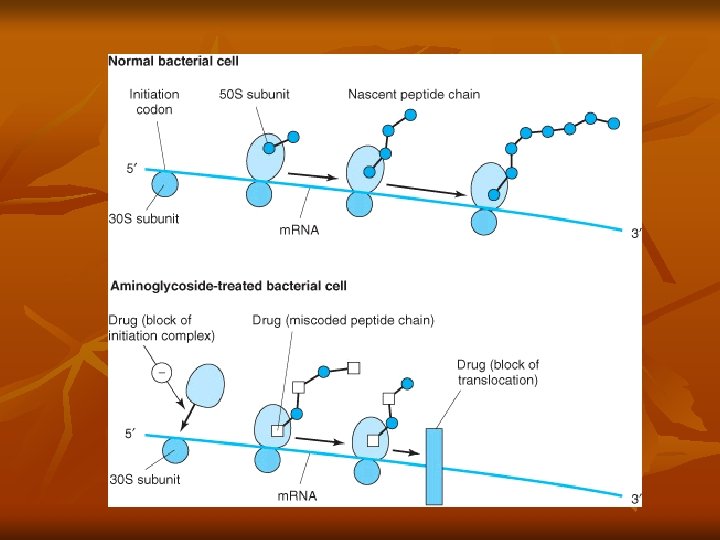
Aminoglycosides n n Contain amino sugars linked to aminocyclitol by glycosidic bonds Binds to 30 S ribosomal subunit (streptomycin) or 50 S (gent/others), interfering with assembly of functional ribosomal apparatus or misreading of genetic code Aerobic gram negative bacteria Bactericidal or static
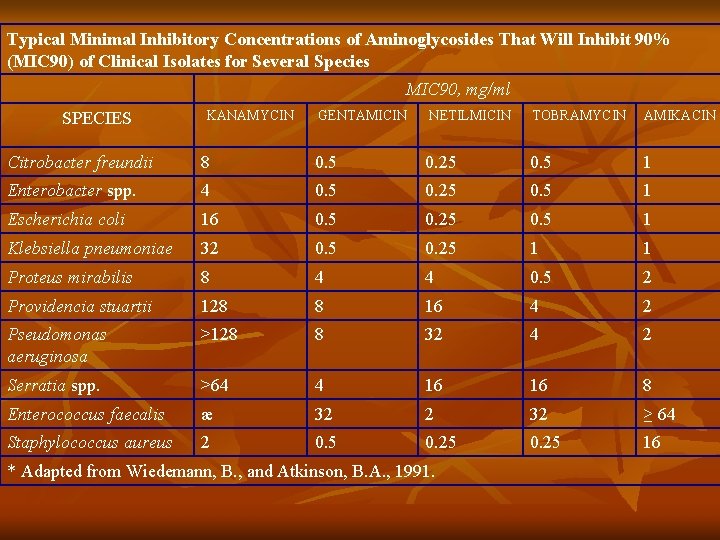
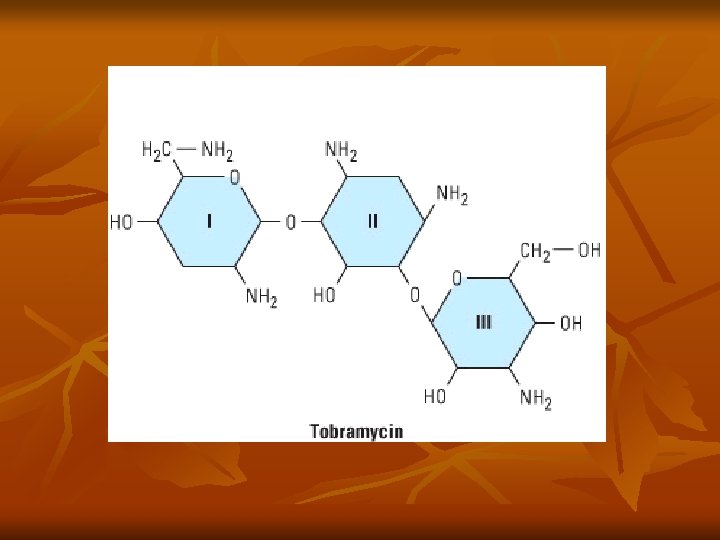

Typical Minimal Inhibitory Concentrations of Aminoglycosides That Will Inhibit 90% (MIC 90) of Clinical Isolates for Several Species MIC 90, mg/ml SPECIES KANAMYCIN GENTAMICIN NETILMICIN TOBRAMYCIN AMIKACIN Citrobacter freundii 8 0. 5 0. 25 0. 5 1 Enterobacter spp. 4 0. 5 0. 25 0. 5 1 Escherichia coli 16 0. 5 0. 25 0. 5 1 Klebsiella pneumoniae 32 0. 5 0. 25 1 1 Proteus mirabilis 8 4 4 0. 5 2 Providencia stuartii 128 8 16 4 2 Pseudomonas aeruginosa >128 8 32 4 2 Serratia spp. >64 4 16 16 8 Enterococcus faecalis æ 32 2 32 ≥ 64 Staphylococcus aureus 2 0. 5 0. 25 16 * Adapted from Wiedemann, B. , and Atkinson, B. A. , 1991.

Resistance n Decreased uptake n n Altered receptor n n Absent oxygen-dependent transport 30 S ribosomal subunit binding site has lower affinity for aminoglycosides Enzymatic modification n Plasmid R factors that synthesize enzymes to modify and inactivate antibiotic

Administration n Inadequate absorption when oral All parenteral, except neomycin Neomycin n n Severe nephrotoxicity Only topical use to reduce intestinal bacteria

Distribution n Good body fluid penetration, except CSF Accumulation in renal cortex and inner ear lymph All cross placenta

Metabolism n n Rapidly excreted into urine Alter dose in renal insufficiency

General Therapeutic Uses n Streptomycin n n Bacterial endocarditis (+ Pen) Tuberculosis (combination) Tularemia- hunters skinning infected animals Gentamycin: combination with Pen/Ceph n n Urinary tract infections (E coli, enterobacter) Pneumonia (pseudomonas, E coli, kleb) Meningitis Peritonitis

General Therapeutic Uses n Tobramycin n Same as gentamycin Poor activity against enterococci Amikacin n Initial treatment of serious nosocomial gram negative bacilli infections when resistance to gentamycin and tobramycin

General Therapeutic Uses n Netilmicin n n Kanamycin n n Serious infections with enterobacteriaceae and other aerobic gram negative bacilli Few indications Neomycin n Topical skin and mucosa infections

Adverse Effects n Ototoxicity n n n Nephrotoxicity Neuromuscular paralysis n n n High peak levels and long duration Intraperitoneal/intrapleural high dose; myasthenia gravis patients at risk Contact dermatitis- neomycin topical Monitor peak and trough plasma levels

Macrolides n n n n Many membered lactone ring where sugars or amino acids are attached Erythromycin Azithromycin Clarithromycin- more strep and staph Dirithromycin Troleandomycin Telithromycin
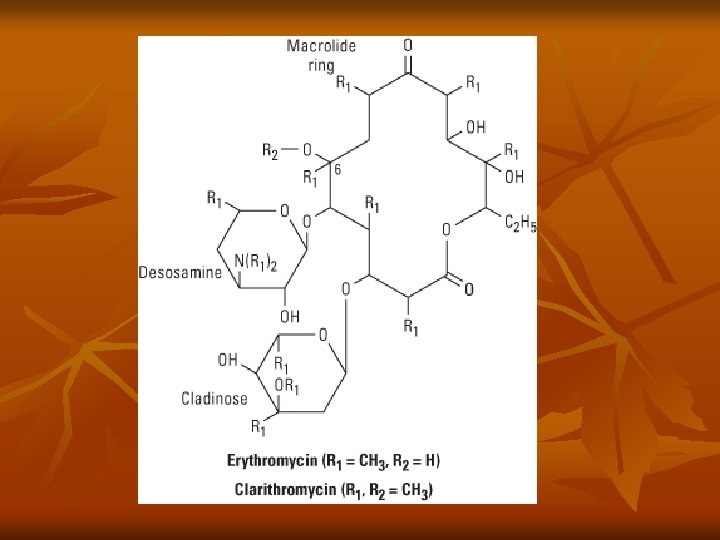

Mechanism of Action n n Bind to 50 S subunit of bacterial ribosome, inhibiting translocation step of protein synthesis Bacteriostatic activity Better intracellular concentration with gram + bacteria Clarithro and Azithro more anaerobic
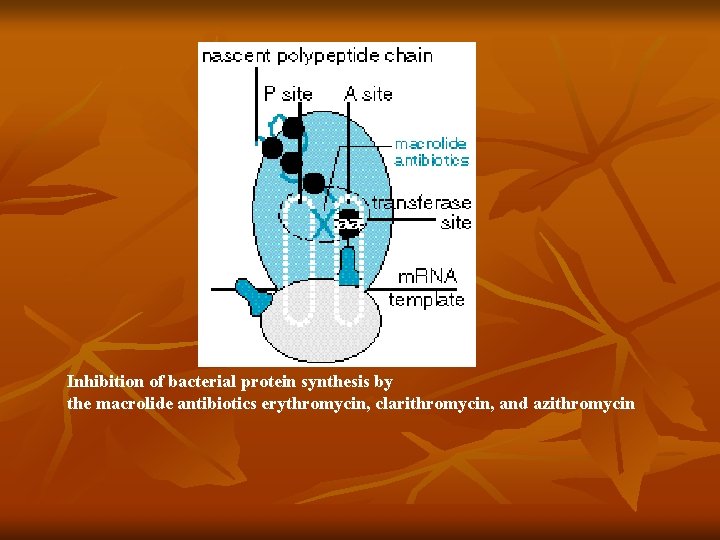
Inhibition of bacterial protein synthesis by the macrolide antibiotics erythromycin, clarithromycin, and azithromycin

Resistance n n Inability of organism to take up antibiotic Decreased affinity of binding site for antibiotic

Administration n Adequate oral absorption Intravenous: thrombophlebitis Intramuscular: painful

Distribution n n Well into body fluids, except CSF Diffuses into prostatic fluids Accumulates in macrophages Concentrated in liver Penetrate well into abscesses

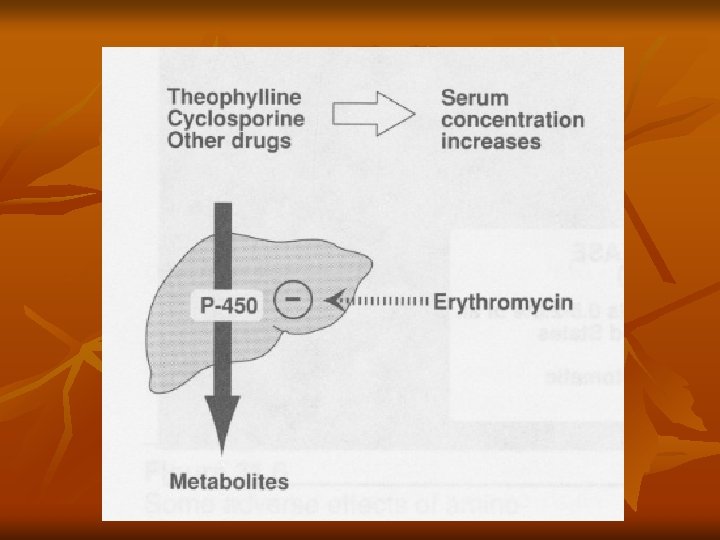
Metabolism n Inhibits oxidation of other drugs through interaction with cytochrome P-450 system

Excretion n n Concentrated and excreted in an active form in the bile Partial reabsorption through enterohepatic circulation

General Therapeutic Uses n n n Mycoplasma pneumonia Syphilis- in penicillin allergic Chlamydia- alternative to tetracycline; during pregnancy Legionellosis pneumonia Corynebacterium diptheriae- carriers Ureaplasma- urethritis

General Therapeutic Uses n n Alternative to penicillin in allergic patients Clarithromycin (Biaxin) and Azythromycin (Zithromax) n n COPD, pneumonia Pharyngitis, tonsillitis Acute maxillary sinusitis Lower respiratory tract infections

Adverse Effects n Epigastric distress n n Cholestatic jaundice n n Nausea, vomiting, pain, diarrhea When estolate form is used Ototoxicity n High doses

Interactions n n Increases plasma concentration of digoxin Inhibits hepatic metabolism of drugs n n n n Theophylin Warfarin Carbamazepine Cyclosporin Methylprednisolone Terfenadine Do not use in liver disease patients

Clindamycin n Introduced in 1970 Semisynthetic derivative of lincomycin, isolated from soil near Lincoln, Nebraska in 1965 Clindamycin produced by exchange of hydroxyl group with chlorine atom at C 7 of lincomycin molecule
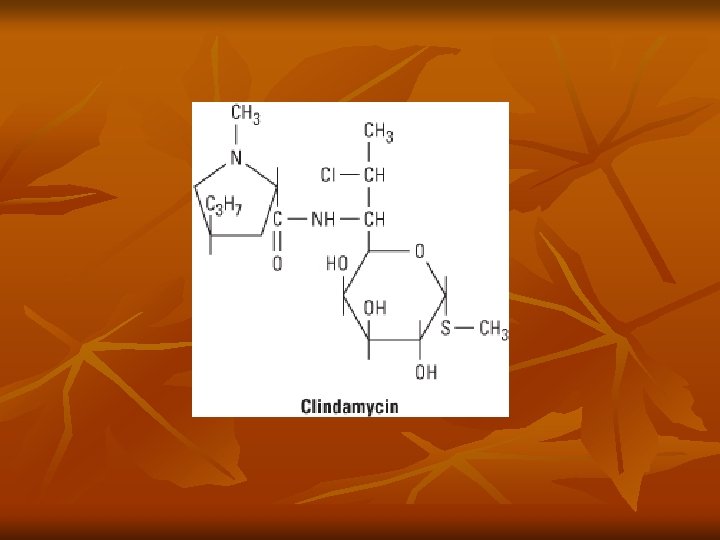

Clindamycin n n Binds to 50 S subunit of bacterial ribosomes to inhibit protein synthesis Bacteriostatic activity, but cidal action against susceptible organisms in vivo

Spectrum n n Similar to erythromycin Increased activity against gram + and anaerobes, staph aureus n Bacteroides fragilis

Pharmacokinetics n n Well absorbed orally Distributes well into body fluids, not CSF Good bone penetration Excreted into bile or urine

Therapeutic Uses n n Strep, Staph, pneumococci, anaerobic infections Purulent osteitis or other bone infection caused by anaerobes

Adverse Effects n GI distress n n n Diarrhea Pseudomembranous colitis- caused by clostridium difficile Superinfections n Fungal overgrowth in oral cavity, intestine, vagina
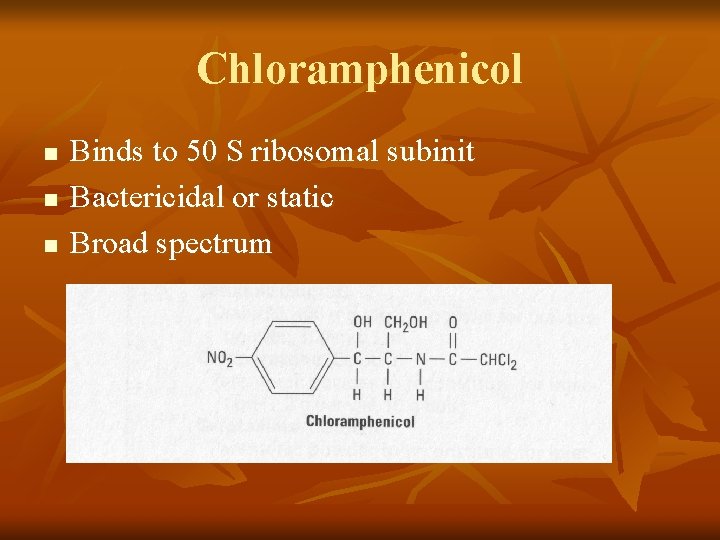
Chloramphenicol n n n Binds to 50 S ribosomal subinit Bactericidal or static Broad spectrum
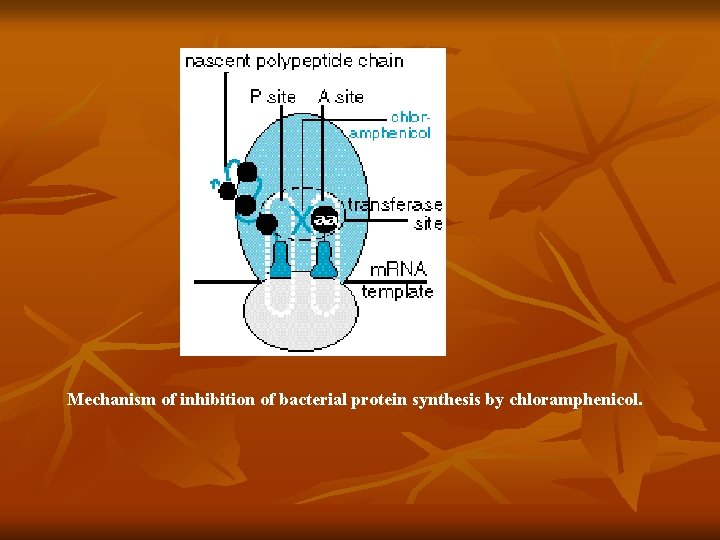
Mechanism of inhibition of bacterial protein synthesis by chloramphenicol.

Pharmacokinetics n n n IV or orally Complete oral absorption Excretion depends on conversion in liver to glucuronide, then secretion in kidney

Therapeutic Uses n n Severe odontogenic infections threatening orbital contents or brain Penetrates well into brain and CSF Typhoid fever- salmonella Refractory meningitis by h. influenza, s. pneumonia, n. meningitidis, rickettsia, brucella, bacteroides

Adverse Effects n Anemias n n Hemolytic, reversible/mild, aplastic Gray baby syndrome n n Neonates if doses not adjusted Low capacity to glucoronidate antibiotic and underdeveloped renal function Decreased excretion ability Poor feeding then cyanosis then death

Streptogramins n n n Quinupristin-dalfopristin Rapidly bactericidal for most organisms except Enterococcus faecium Significantly inhibit CYP 3 A 4

Oxazolidinones n n Linezolid Active against gram-positive organisms Bacteriostatic Inhibits protein synthesis
- Slides: 61