Prostate Cancer Causes Diagnosis and Treatment Options Bruce

Prostate Cancer: Causes, Diagnosis, and Treatment Options Bruce B. Garber, MD, FACS Clinical Associate Professor, Drexel University College of Medicine. Urologist, Chestnut Hill Hospital Philadelphia, PA www. garber-online. com 215 -247 -3082

Introduction The prostate: -is a gland located below the bladder -is only present in men -surrounds the urethra -can undergo benign or malignant change
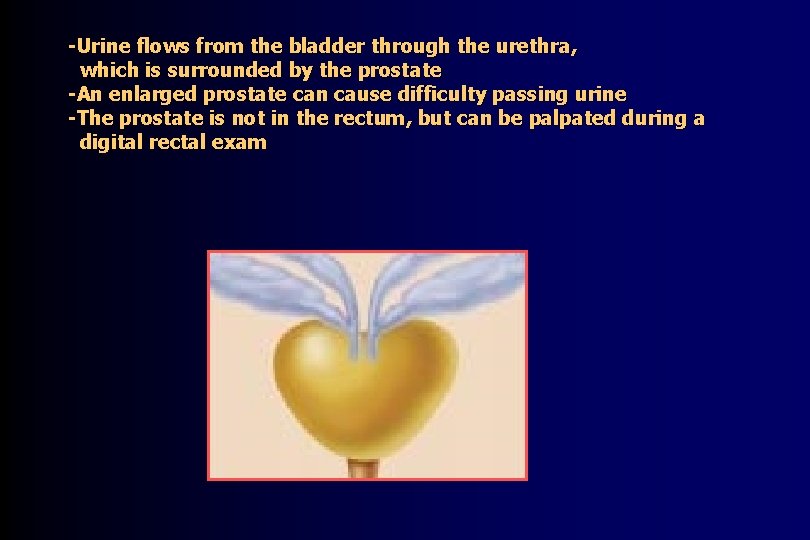
-Urine flows from the bladder through the urethra, which is surrounded by the prostate -An enlarged prostate can cause difficulty passing urine -The prostate is not in the rectum, but can be palpated during a digital rectal exam

Incidence -Lung, colon, breast, and prostate cancer are the most common solid organ cancers -Over 200, 000 men are diagnosed with prostate cancer each year in the U. S. -African-American men have the highest incidence

Prostate Cancer: Causes Risk Factors Currently Under Investigation: ä Racial origin: African American > all other races ä Dietary factors: fatty foods implicated ä Genetic factors: familial prostate cancer; prostate cancer genes have been discovered

Prostate Cancer: Diagnosis Methods of Detection: 1. Prostate exam (digital rectal exam, DRE) 2. Prostate-specific antigen (PSA) blood test (free, total, complexed, velocity) ä If either is abnormal: – Ultrasound-guided prostate needle biopsy
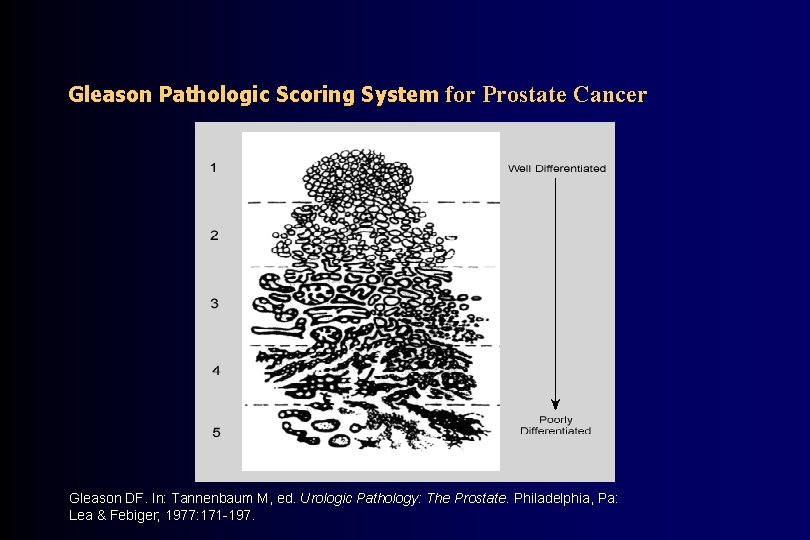
Gleason Pathologic Scoring System for Prostate Cancer Gleason DF. In: Tannenbaum M, ed. Urologic Pathology: The Prostate. Philadelphia, Pa: Lea & Febiger; 1977: 171 -197.

Prostate Cancer Staging Systems ä Stages A, B, C, D ä TNM system (stage T 1 C is most common)

Whitmore-Jewett Classification Stage A Microscopic cancer confined to the prostate and too small to be felt by digital rectal exam A 1 Cancer well differentiated and confined to one site A 2 Cancer moderately or poorly differentiated or present in more than one site
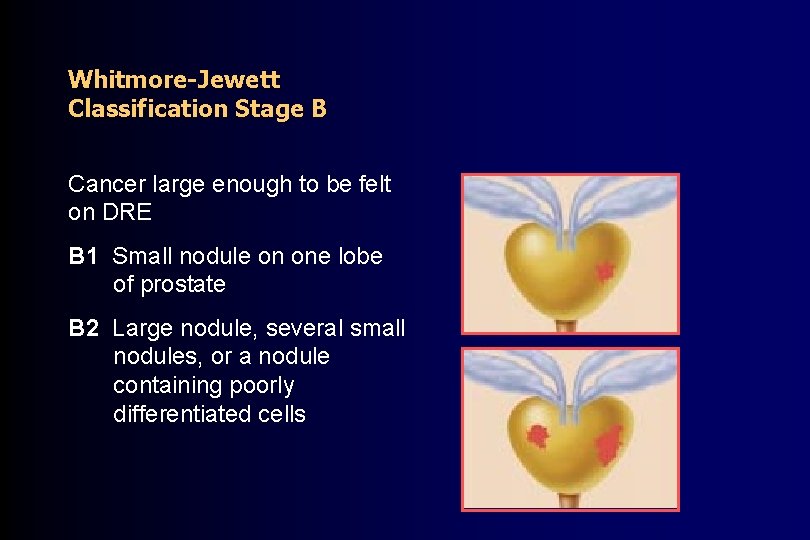
Whitmore-Jewett Classification Stage B Cancer large enough to be felt on DRE B 1 Small nodule on one lobe of prostate B 2 Large nodule, several small nodules, or a nodule containing poorly differentiated cells

Whitmore-Jewett Classification Stage C A large cancer involving nearly the entire gland C 1 Cancer may have spread a small distance beyond the gland C 2 Cancer has invaded the neighboring tissue
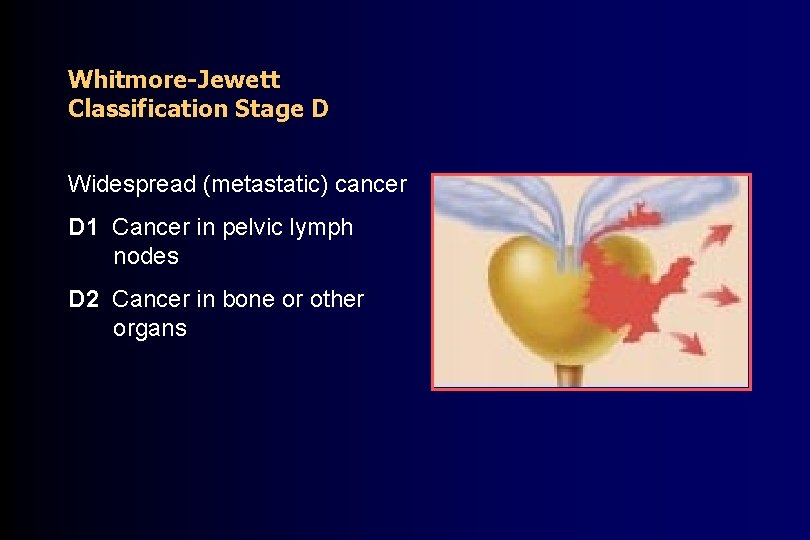
Whitmore-Jewett Classification Stage D Widespread (metastatic) cancer D 1 Cancer in pelvic lymph nodes D 2 Cancer in bone or other organs

Prostate Cancer: Treatment Options Non-curative therapies: 1. Androgen deprivation -LHRH-agonists -Bilateral orchiectomy -Antiandrogens 2. Chemotherapy 3. Observation Potentially curative therapies: 1. Radical prostatectomy • Retropubic • Perineal • Laparoscopic/Robotic 2. Radiotherapy • External beam radiation • Brachytherapy (radioactive seed implant, high dose brachytherapy) 3. Cryo (freezing)

Non-curative Hormonal Therapy: Currently Available Agents LHRH-agonists: ä Zoladex® (goserelin acetate implant) ä Lupron Depot® (leuprolide acetate for depot suspension) ä Viadur™ (leuprolide acetate implant) ä Eligard® ä Vantas® Antiandrogens: ä Casodex® (bicalutamide) ä Eulexin® (flutamide) ä Nilandron (nilutamide) Lupron Depot® is a registered trademark of TAP Pharmaceuticals, Inc. Copyright© 2001 Bayer Corporation. Viadur™ is a trademark of ALZA Corporation under license to Bayer Corporation. Eulexin® is a registered trademark of Schering-Plough Pharmaceuticals. Nilandron is a registered trademark of Aventis.

Therapies of Curative Intent: ä Radical prostatectomy (total prostate removal) – Retropubic (abdominal incision) – Perineal (incision under scrotum) – Laparoscopic/Robotic (multiple ports) ä Radiotherapy – External beam radiation (IMRT, IGRT) – Brachytherapy (radioactive seed implant; high dose brachytherapy) ä Cryoablation (freezing)

Radical Prostatectomy Advantages ä Can remove all the cancer Disadvantages ä Major operation ä Erectile dysfunction ä Incontinence ä Scar tissue ä Rectal injury ä Wound infection, blood clots, heart attack, etc. ä Often doesn’t remove all of the cancer

External Beam Radiation (EBRT) Advantages ä Efficacy similar to prostatectomy ä Outpatient Disadvantages Ø Erectile dysfunction Ø Chronic bowel and bladder irritation (cystitis, proctitis) Ø Requires roughly 7 weeks of daily treatment Ø Increased risk of rectal & bladder cancer

Brachytherapy (radioactive seed implant) Advantages ä Efficacy similar to EBRT or surgery ä Outpatient; one treatment Disadvantages ä Chronic bowel & bladder irritation ä Erectile dysfunction ä Seed migration ä Can’t treat large prostates ä Increased risk of rectal & bladder cancer

Cryoablation of the Prostate (Cryosurgery, Cryotherapy) CRYO = GREEK WORD FOR COLD ABLATION = DESTRUCTION

What is Cryoablation? ä Cryoablation: cancer treatment by freezing to -40º Centigrade ä No surgical incision, minimal blood loss, no radiation ä Immediate cancer cell death ä Dead cells are slowly reabsorbed by the body ä Outpatient procedure, with rapid return to normal activities ä FDA-approved, covered by Medicare & most carriers ä New technology: <2% of Urologists currently offering Cryoablation
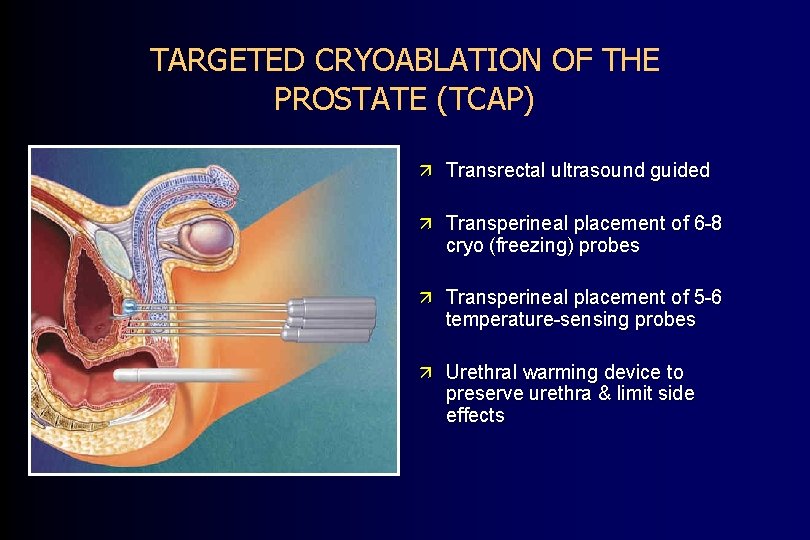
TARGETED CRYOABLATION OF THE PROSTATE (TCAP) ä Transrectal ultrasound guided ä Transperineal placement of 6 -8 cryo (freezing) probes ä Transperineal placement of 5 -6 temperature-sensing probes ä Urethral warming device to preserve urethra & limit side effects

Technology • Computer creates “map” of the prostate • Provides real-time guidance • Identifies and guides probe placement • Temperatures shown in real time • Argon gas freezes prostate rapidly with excellent control • Two freeze/thaw cycles immediately kill cancer cells • Total procedure time about 60 -90 minutes
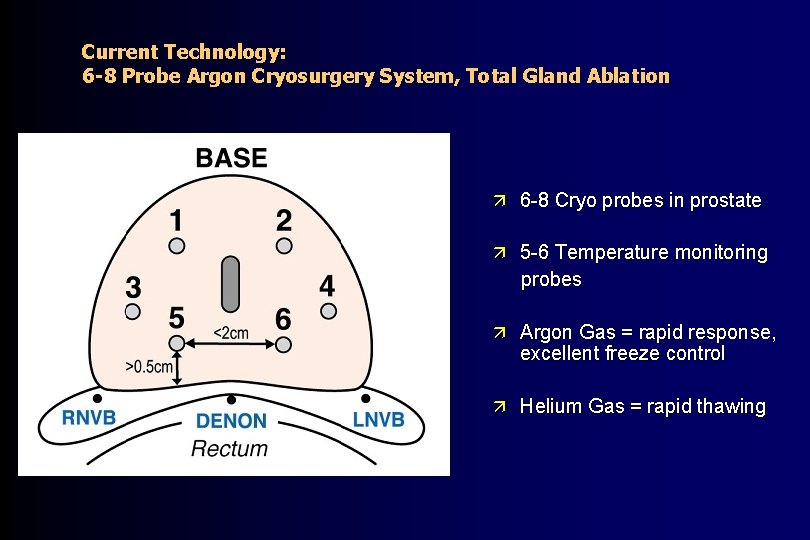
Current Technology: 6 -8 Probe Argon Cryosurgery System, Total Gland Ablation ä 6 -8 Cryo probes in prostate ä 5 -6 Temperature monitoring probes ä Argon Gas = rapid response, excellent freeze control ä Helium Gas = rapid thawing
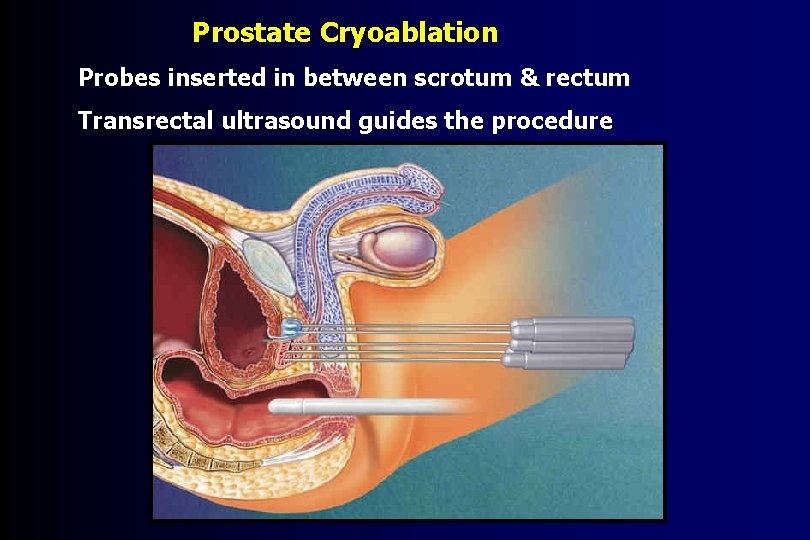
Prostate Cryoablation Probes inserted in between scrotum & rectum Transrectal ultrasound guides the procedure
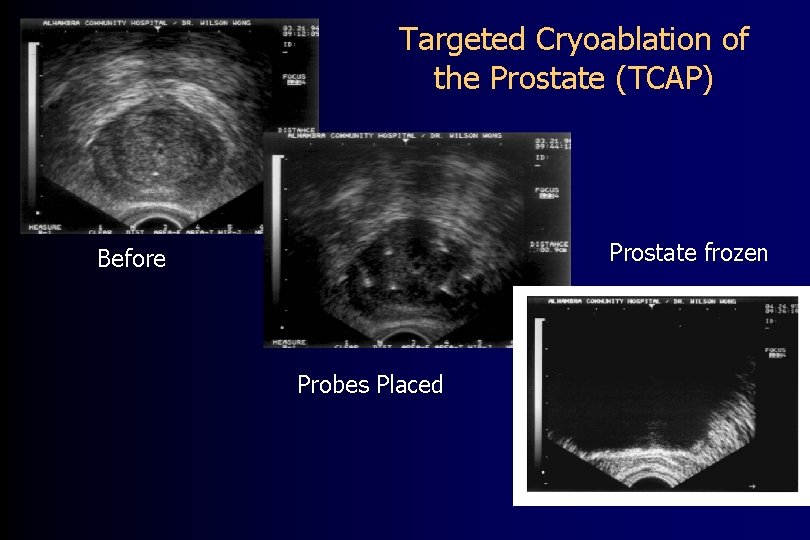
Targeted Cryoablation of the Prostate (TCAP) Prostate frozen Before Probes Placed
Prostate Cryoablation Techniques ä Total Gland Ablation ä Nerve-Sparing ä Focal
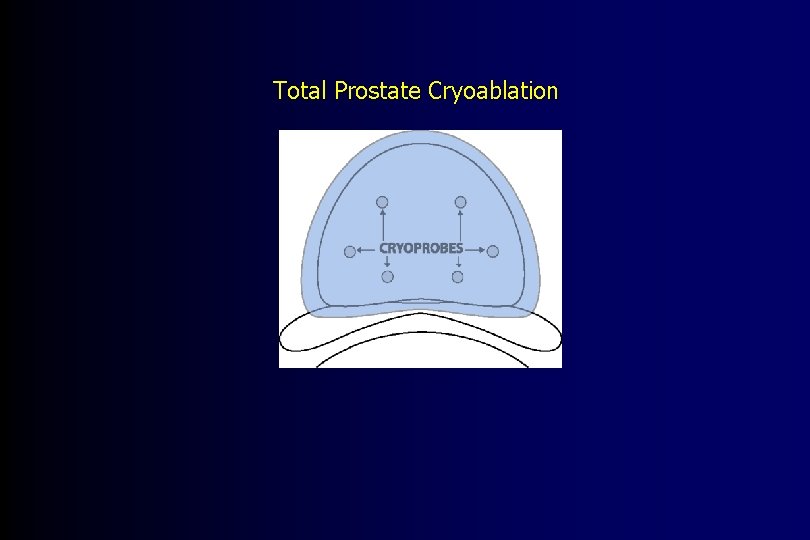
Total Prostate Cryoablation
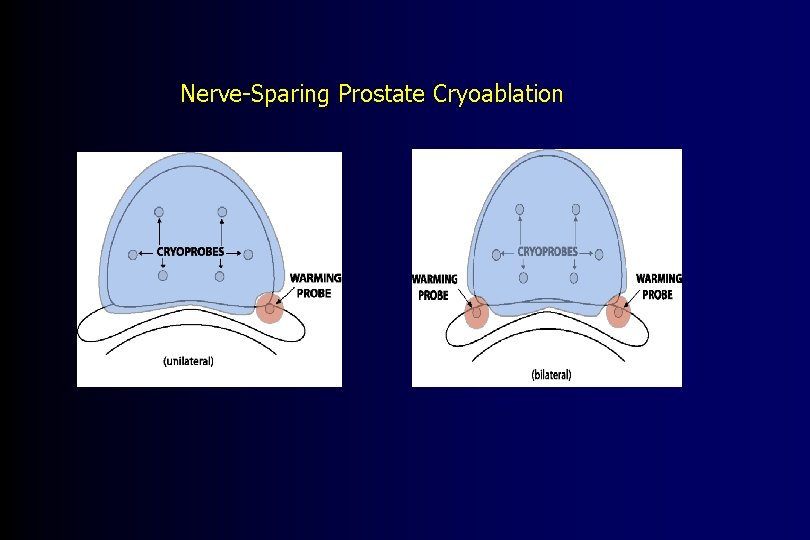
Nerve-Sparing Prostate Cryoablation
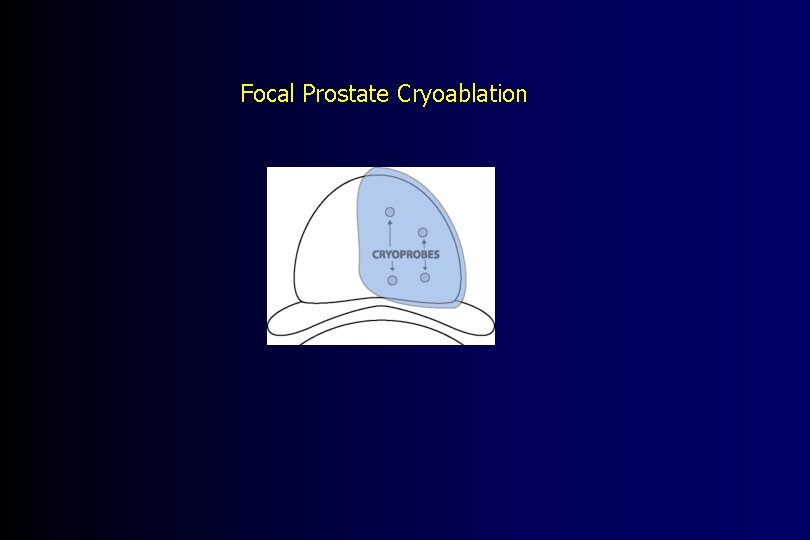
Focal Prostate Cryoablation

Results of Whole Gland Primary Prostate Cryoablation J. Urol 180: 554 -558 (2008) ä 1, 198 patients 5 -year biochemical disease-free status: ä ASTRO Phoenix -low risk pts. : 84. 7% 91. 1% -moderate risk pts. : 73. 4% 78. 5% -high risk pts. : 75. 3% 62. 2% -all pts. : 77. 1% 72. 9% ä Rectal fistula rate: 0. 4% ä Urinary incontinence rate: 4. 8% ä Erectile dysfunction common, but can be successfully treated in most men ä ä ASTRO definition of biochemical failure: 3 consecutive increases in PSA Phoenix definition of biochemical failure: nadir PSA level +2

Results of Salvage Prostate Cryoablation J. Urol 180: 559 -564 (2008) ä 279 patients ä 5 -year biochemical disease-free status: ASTRO Phoenix 58. 9% 54. 5% ä Rectal fistula rate: 1. 2% ä Urinary incontinence rate: 4. 4% ä Erectile dysfunction common, but can be successfully treated in most men

Cryoablation Advantages ä Outpatient ä Minimally-invasive ä Can treat radiation failures ä Can be repeated ä Better than radiation for high grade cancer (Gleason 7 -10) Disadvantages ä Erectile dysfunction ä Urinary problems (short-term) ä Shorter track record than surgery or radiation

Summary: Prostate Cryoablation ä A well-established treatment for localized prostate cancer ä Covered by Medicare & most carriers ä Minimally invasive: no surgical incision ä Minimal blood loss--blood transfusion not needed ä Better than radiation for high risk (e. g. high Gleason score) disease ä Can treat cancer recurrence after radiation therapy ä Does not increase risk of rectal or bladder cancer ä Avoids radiation cystitis and proctitis ä Avoids seed migration seen with brachytherapy ä Can be combined with hormonal therapy ä Outpatient procedure for most men ä Unlike any other treatment, can be repeated if necessary ä Rapid return to normal activities ä More rapid recovery than after radical prostatectomy ä Erectile dysfunction frequent but treatable
- Slides: 33