Prospective of Population Aging Problems in Geriatric Care

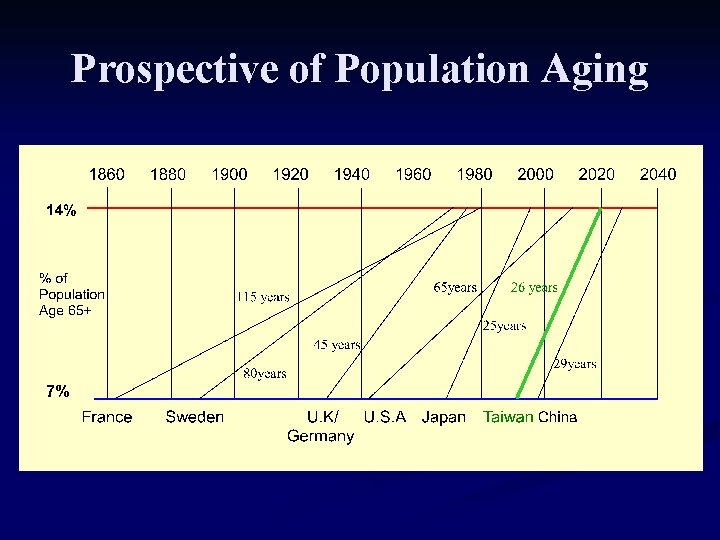
Prospective of Population Aging
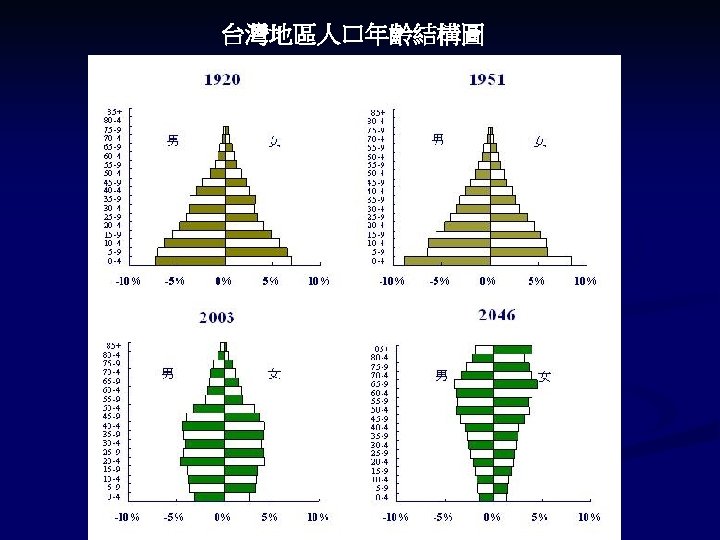
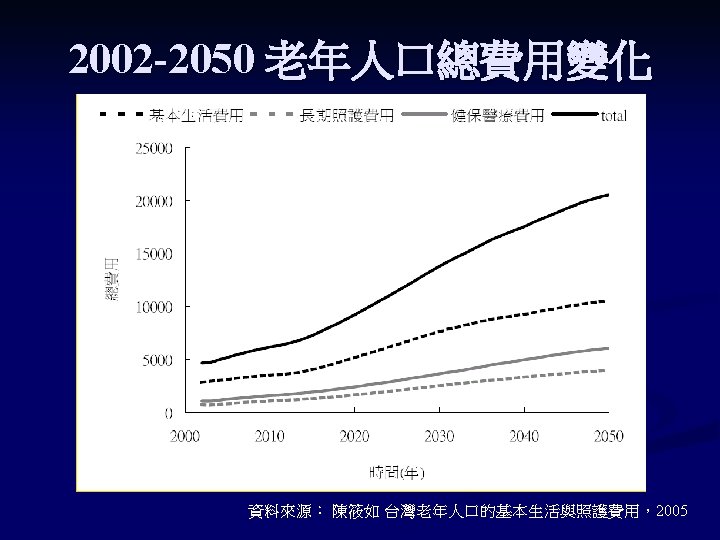
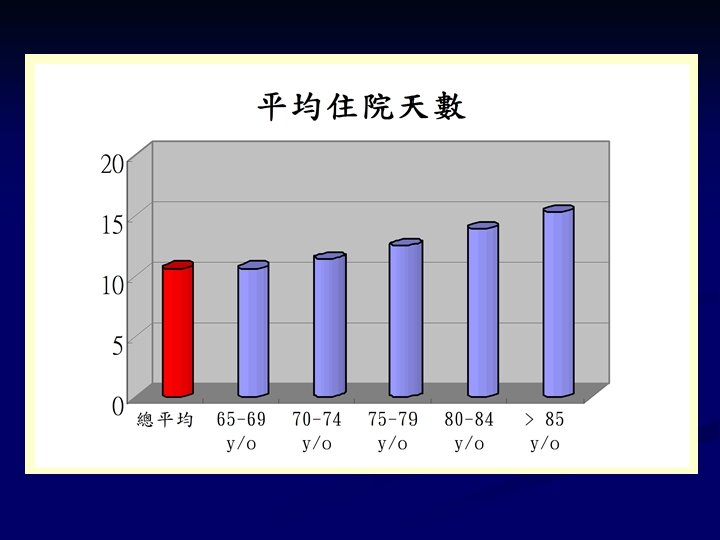
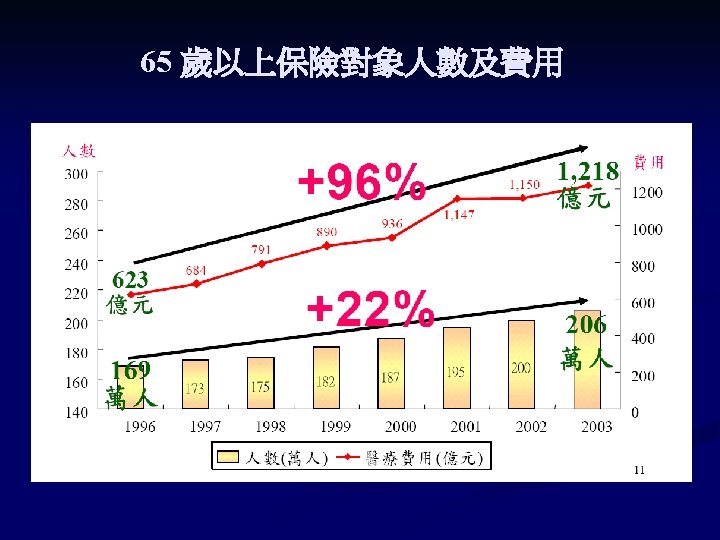

Problems in Geriatric Care n n n n Multiple illness Polypharmacy (drug-drug interaction) Many tubes (restrain) Immobility (pressure ulcer, depression) Nosocomial infection Iatrogenic complications Functional decline Prolong LOS

Characteristics of Geriatrics Biological Psychological Social

Interaction Psychological Biological Social
Geriatric Syndrome

Aging Health Capacity → 成功老化 ( Successful aging ) 正常老化 病態老化 失能 ( Frail ) Age →

Dysfunctional Syndrome Functional elderly • Hospitalization • Hostile environment • Low social support • Depressed mood • Immobility • Malnutrition • Medicines • Physical impairment • Procedures Depressed mood Dysfunctional elderly Physical impairment Negative expectation

Patient factors and function decline older age preadmission functional impairment lower MMSE on admission re-hospitalization Sager M, Franke T, Inouye S, et al. Functional outcomes of acute medical illness and hospitalization in older persons. Arch Intern Med. 1996; 156: 645 -652.

n 31% of elderly patients lose one or more ADL in hospital (at discharge) n 40% of elderly patients declined in IADL function at 3 months after discharge n Negative consequences: death, longer length of stay, institutionalization, rehospitalization, increased comorbidities Sager MA, Arch Int Med 1996 Creditor M, Arch Int Med

Functional decline outcomes Prolonged LOS Higher mortality (almost 2 times risk) Higher rates of institutionalization Higher cost Sager M, Franke T, Inouye S, et al. Functional outcomes of acute medical illness and hospitalization in older persons. Arch Intern Med. 1996; 156: 645 -652.

Elderly functional decline study Hospital based study- Yale Medical inpatients > 70 y/o Looking for those risk of functional decline Functional decline defined as ADL loss Prospective cohort study Inouye S, Wagner R, Acampora D, et al. A predictive index for functional decline in Hospitalized Elderly Medical Patients. J Gen Intern Med. 1999; 8: 645 -652.

Factors studied Demographics Self-reported physical functioning Self report IADL/ADL MMSE Pre-illness social activity Geriatric depressions scale Vision, Jaeger card Hearing- Whisper test Confusion assessment method Skin check for breakdown Overall severity of illness
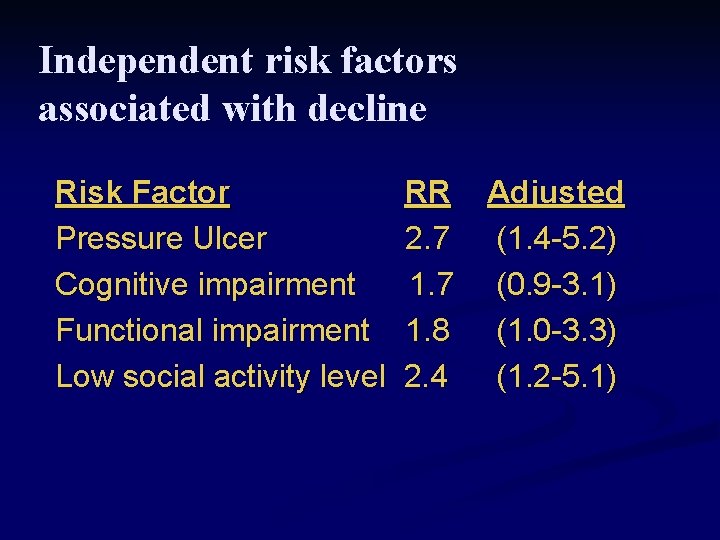
Independent risk factors associated with decline Risk Factor Pressure Ulcer Cognitive impairment Functional impairment Low social activity level RR 2. 7 1. 8 2. 4 Adjusted (1. 4 -5. 2) (0. 9 -3. 1) (1. 0 -3. 3) (1. 2 -5. 1)
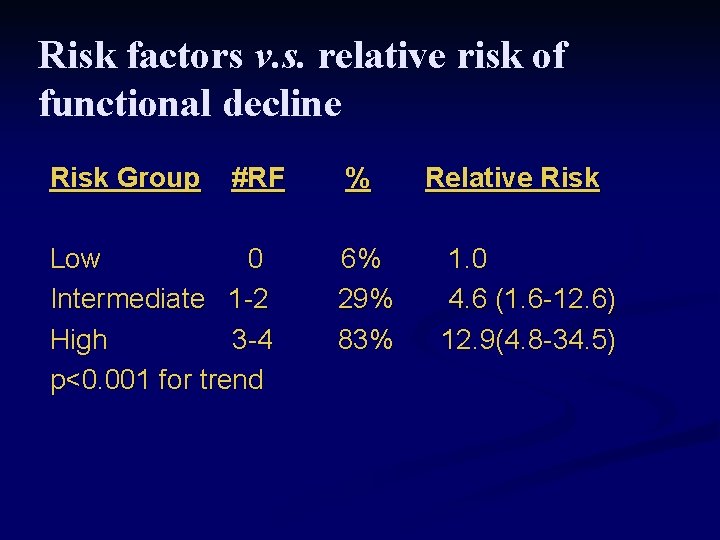
Risk factors v. s. relative risk of functional decline Risk Group #RF Low 0 Intermediate 1 -2 High 3 -4 p<0. 001 for trend % 6% 29% 83% Relative Risk 1. 0 4. 6 (1. 6 -12. 6) 12. 9(4. 8 -34. 5)
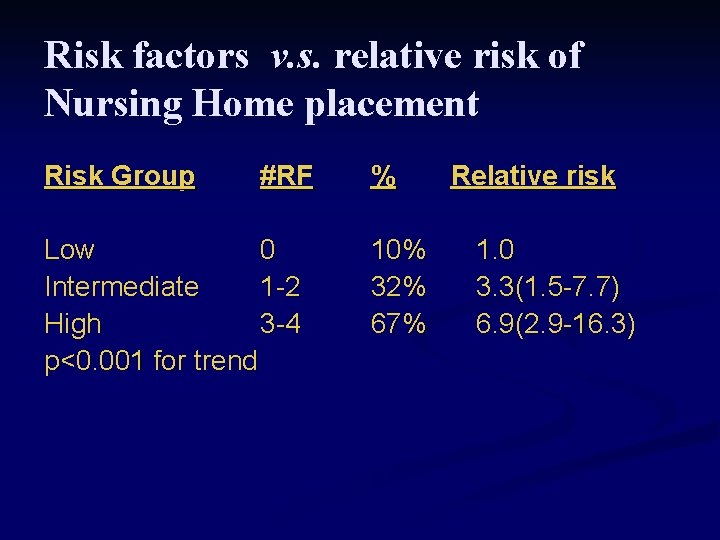

Risk factors v. s. relative risk of Nursing Home placement Risk Group #RF Low 0 Intermediate 1 -2 High 3 -4 p<0. 001 for trend % 10% 32% 67% Relative risk 1. 0 3. 3(1. 5 -7. 7) 6. 9(2. 9 -16. 3)
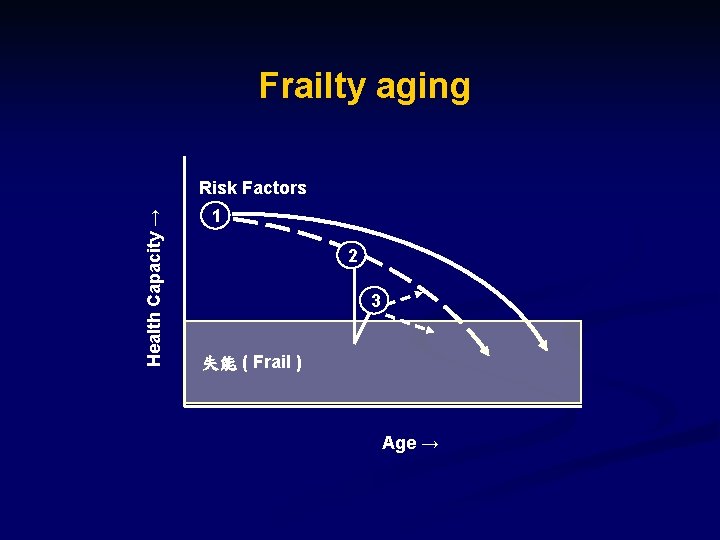
Frailty aging Health Capacity → Risk Factors 1 2 3 失能 ( Frail ) Age →
Strategies prevention Geriatrics intervention deceleration
Different settings of Geriatrics

Geriatric Evaluation and Management Unit (GEMU) n GEMU: Unit designed to perform Comprehensive Geriatric Assessment (CGA) by a hospital based interdisciplinary team( IDT ) n Goals of GEMU Functional status ↑ Mortality↓ Overall medical care cost ↓ Discharge home

GEMU n Results: inpatient : functional decline↓ outpatient : mental health↑ No increase in costs. — Cohen HJ et al. NEJM 2002 mortality ↓in acute sick, frail, older patients — Saltvedt I et al. JAGS 2002

Acute Care for Elders Units n Overall health status at discharge was better — Landefeld CS et al. NEJM 1995 n n More nursing care plans to promote independence Earlier and more frequent SW consult, earlier discharge planning Less days at bed rest, less restraints Higher satisfaction (Staff, family, patients) — Counsell SR et. Al. JAGS 2000

In-Home Geriatric Assessment n n Delay the development of disability Reduce permanent nursing home stays — Stuck AE et al. NEJM, 1995

Prevention Assessment eyes, ears physical performance, fall, pressure ulcer dementia, depression, delirium, drug incontinence, nutrition psychosocial (home safety)

Intervention n SENSORY FUNCTION COGNITION
Sensory interventions Make sure patient has glasses and hearing aid Good lighting Decrease excess noise Visible clock

Functional interventions What to do? Chart orders- walking and range of motion TID Ambulation problem- physical therapy Dressing/bathing/feeding- occupational therapy

Hospital life program at YALE Persons admitted to acute care hospital ≥ 70 y/o One risk factor for cognitive or functional decline ROM and walking TID Minimize restraints (Bladder catheter, restraints) 2 ADL declined : 14% in intervention group 33% in control group

Cognitive interventions Orientation board and cognitive stimulation decreased confusion Use strategies to limit delirium environmental modifications stimulating activities during daytime correction of sensory deficits promote normal sleep avoid restraint

Education! Physician Patient Caregiver Education Administrator Nurse

Path of Geriatrics Control Prevent functional decline n Block vicious cycle n Increase quality of care n Reduce LOS n Cost reduction n


Comprehensive Geriatric Assessment

Cognition screen n. Three item recall at one minute recalls ≦ 2 (1 or 0)--LR-3. 1 recalls 2 --LR-0. 5 recalls 3 items--LR-0. 06 n. Animal naming n n Average performance=18/min Less than 12/min is abnormal --Neurology. 1989; 39: 1159 - 1165. n. Clock completion test Sen/spec for 4 th quadrant predicting dementia 87%/82%
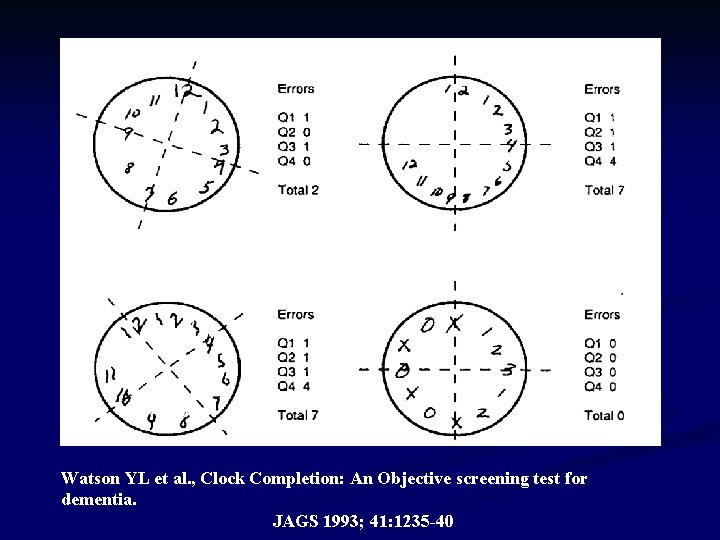
Watson YL et al. , Clock Completion: An Objective screening test for dementia. JAGS 1993; 41: 1235 -40

SPMSQ (short portable mental status questionnaire) n n n n n 1. What is the date today? 2. What day of the week is it? 3. What is the name of this place? 4. What is your telephone number (address)? 5. How old are you? 6. When were you born? 7. Who is the President? 8. Who was the President just before that? 9. What was your mother’s maiden name? 10. Subtract 3 from 20 and keep substracting 3

SPMSQ Fail to n 0 -2: normal n 3 -4: mild n 5 -7: moderate n 8 -10: Severe

Mini-mental status exam (MMSE)

MMSE n n n Time orientation (5) Place orientation(5) Registration (3) Calculation(5) Recall(3) n n n education >6 yrs: 24 no education: 16 Naming(2) Repetition(1) Reading(1) Writing(1) 3 -stage command(3) Drawing(1) education ≦ 6 yrs: 21

Depression screen n. Single Question: Do You Often Feel Sad Or Depressed? (Sen/spe-. 85/. 65) n 5 -Item Geriatric Depression Scale (Sen/spe-. 97/. 85) n 15 -Item GDS (Sen/spec-. 94/. 83)

5 ITEM GDS Yes (1) Are you basically satisfied with your life? (2) Do you often get bored? (3) Do you often feel helpless? (4) Do you prefer to stay at home rather than going out and doing new things? (5) Do you feel pretty worthless the way you are now? No 0 - 1 = not depressed > 2 = depressed *Sens. 97 (. 94)/Spec. 85(. 83) PPV -. 85 (. 82) NPV -. 97 (. 94) Single Question: Sen. 85/Spec. 65 Hoyl, MT et al. Development and Testing of a Five-item Version of the Geriatric Depression Scale. JAGS. 47: 873 -78, 1999.

Delirium Screen Confusion assessment method (CAM) n n Acute onset, fluctuating course Inattention Disorganized thinking Status of unconsciousness Inouye, SK et al, Clarifying confusion: The confusion assessment method. Ann Intern Med 1990; 113(12): 941 -8

Drugs n Any of ≥ 4 Prescribed n the “Anti- ” n Benzodiazepine n Non prescribed, (OTC) n Alternative medicine

Eyes DO YOU HAVE DIFFICULTY WITH. . n. Driving n. Watching TV n. Reading n. Or any daily activity

IF “YES” TO QUESTION THEN n. Test each eye with Snellen Chart while patient wears glasses Inability to read greater than 20/40 on Snellen Chart n

Ears WHISPERED VOICE TEST— n. Explain that you will Whisper some numbers n. Ask senior to close eyes n 12 -18 inches apart n. You exhale and then Whisper 4 random single numbers at 1 sec intervals Fail screen if cannot hear at least 2 numbers (Sen/spec-80 -100%/82 -89%) n

Physical activity Evaluation of general functional mobility n ADL (activity of daily living) Dressing, Eating, Ambulation, Toilet, Hygiene

n IADL ( instrumental activity of daily living) Shopping, Housekeeping, Accounting, Food preparation, Transportation, Telephone, Medication, Laundry

Time Up and Go test Rise chair Walk 10 feet Turn around Walk back and sit in chair n Usual time to complete -- 15 seconds Frail elderly less than 20 seconds n Over 20 seconds on test associated with: poor ADL/IADL performance high falls risk Risk of nursing home placement (Sen/spec-88%/94%) n

Functional reach

Functional reach Question/Test Time to Administer Comments Functional reach If FR < 7” unable to: 1)Leave neighborhood 2)Stand on one foot 3)Do tandem walking 1 min Adjusted Odds Ratio for >2 falls in 6 months 1)8. 1 if unable to reach 2)4. 0 if < 6 inches 3)2. 0 if > 6 inches < 10 inches

Fall M Maladaptive equipment Medical (acute) Medical (chronic) Mental (AD & Depression) Medication E Environment Ethanol Eyes/Ears O Orthostatic signs or symptoms W Weakness

Fall History: SPLATT Symptoms n Prior falls n Location of falls: □outdoor □indoor (□bathroom □bedroom □ kitchen □living room □ others) n Activity during the fall: □slip □trip □weakness □postural change□ reaching □postprandial □ neck flexion n Time of the day the fall occurred: □AM □PM □midnight □Length of time on the ground: □Getting up from falls spontaneously n Trauma/ injury resulting from the falls n

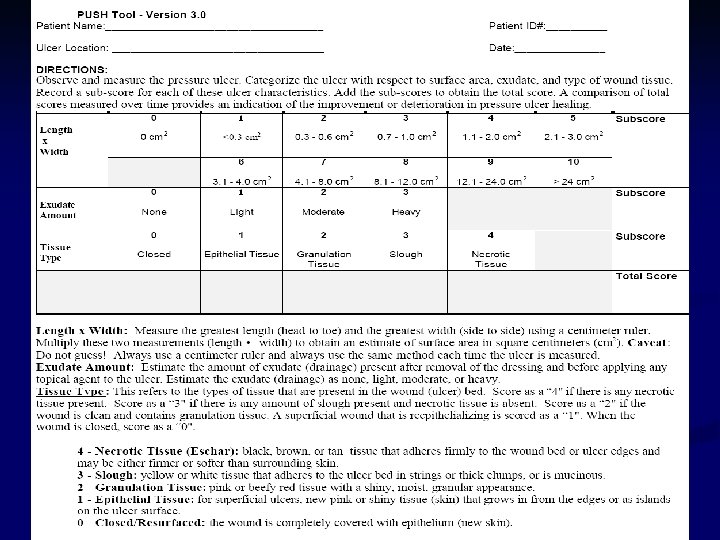
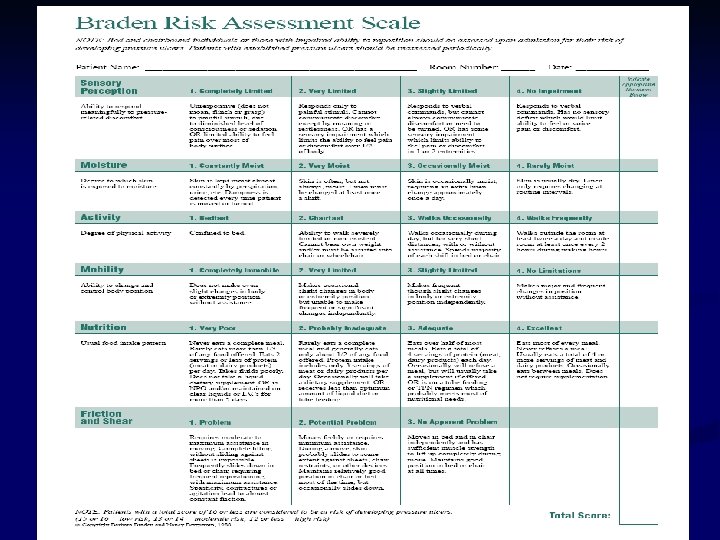
Pressure Ulcer Braden scale: predict risk of pressure ulcer n PUSH: evaluate condition of pressure ulcer n


Psychosocial Assessment of social support n Assessment of caregiver burden n Assessment of elder mistreatment abuse, neglect, exploitation, abandonment n Economic assessment n Assessment of environment- home safety n

Incontinence n Two Questions: 1. In The Last Year, Have You Ever Lost Your Urine And Gotten Wet? 2. Have You Lost Urine On At Least 6 Separate Days? n If Yes To Both, PPV-. 86/NPV-. 96;
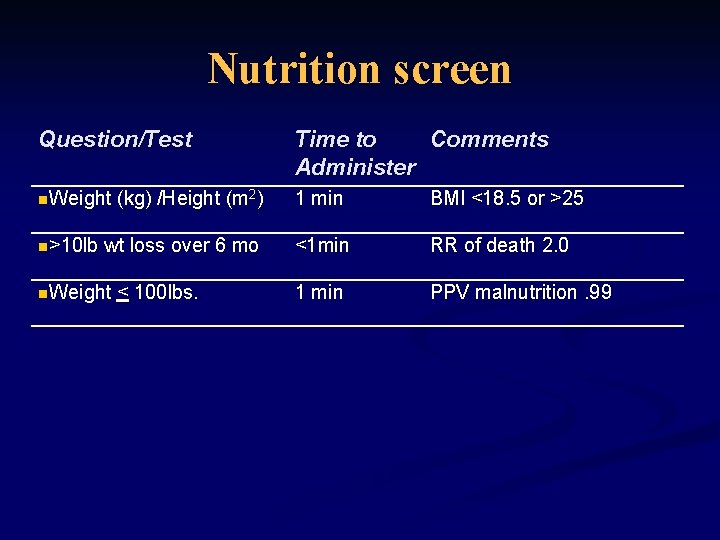
Nutrition screen Question/Test Time to Comments Administer n. Weight 1 min BMI <18. 5 or >25 <1 min RR of death 2. 0 1 min PPV malnutrition. 99 n>10 lb (kg) /Height (m 2) wt loss over 6 mo n. Weight < 100 lbs.
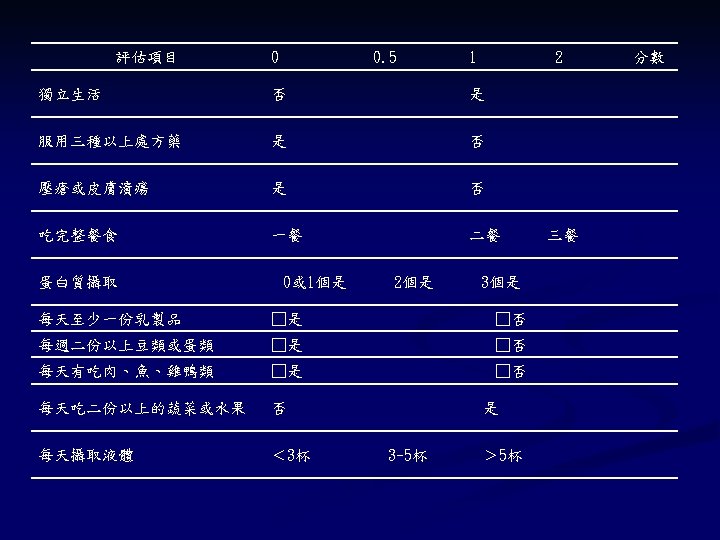

“DEEP IN” FOR QUICK SCREENING D - Dementia, Depression, Delirium, Drugs E - Eyes E - Ears P - Physical Performance, Phall (fall), Pressure ulcer, Psychosocial I - Incontinence N -Nutrition

When we see the patient from different facets, the diamond shines with glamour and draws adoration.

Q&A
- Slides: 69