Properties of skeletal muscle Electrical properties RMP90 mv





















- Slides: 35

Properties of skeletal muscle

• Electrical properties • • • RMP=-90 mv Refractory period =1 -3 msec CV 5 m/sec Chronaxie longer Duration of AP=2 -4 ms

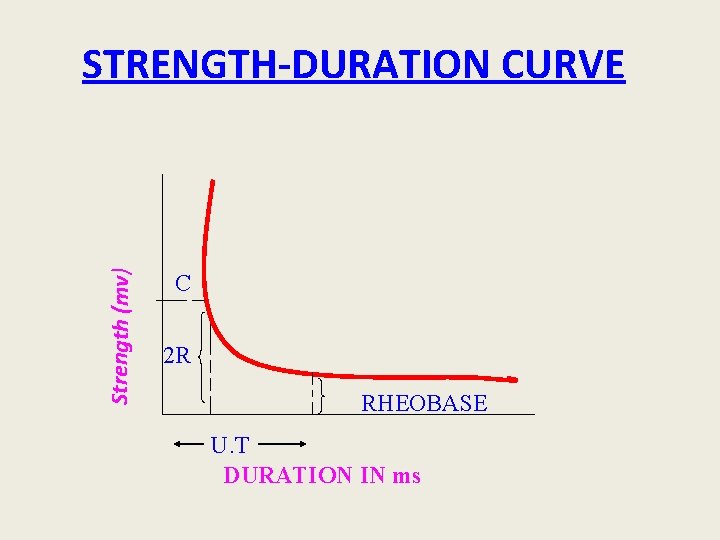
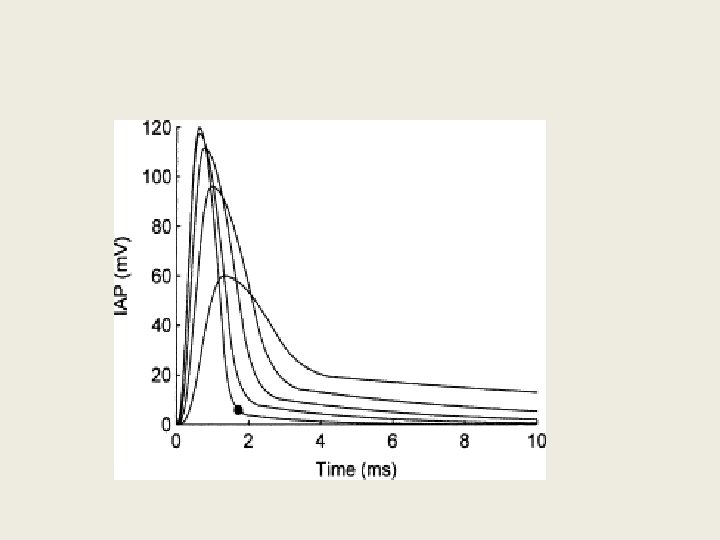
Strength (mv) STRENGTH-DURATION CURVE C 2 R RHEOBASE U. T DURATION IN ms

• Rheobase: the minimum strength of the current acting on the muscle for a variable period that can bring about a response. • Utilization time: the minimum duration for which a current of rheobase strength is applied to excite an excitable tissue • Chronaxie: is defined as the shortest duration of stimulus required to excite a tissue by a current strength equal to twice of rheobase voltage. • Chronaxie of a tissue is a definite measure of its excitability.

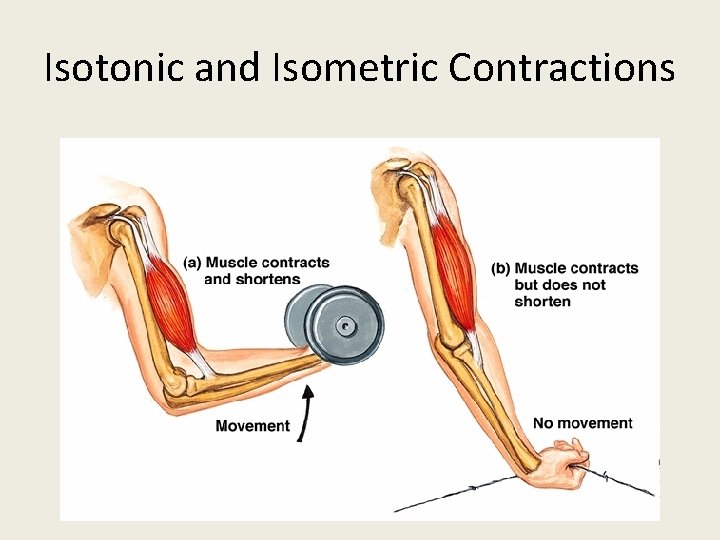
Mechanical properties • Isometric contraction – Muscle exerts force without changing length – Tension increases. – Pulling against immovable object – No external workdone – Postural muscles – Pushing a wall • Isotonic (dynamic) contraction • shortening occurs • No change in the tension • External work is done • Lifting a load

Isotonic and Isometric Contractions

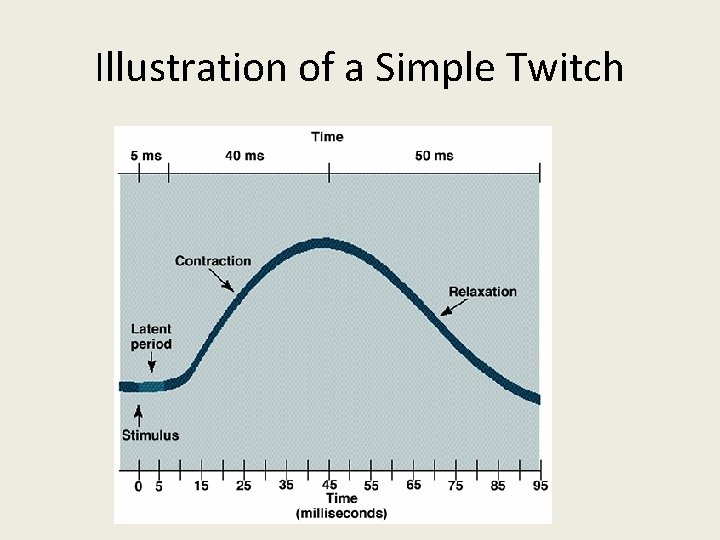
Illustration of a Simple Twitch

• • • Chemical changes ATP --- immediate source Creatine phosphate (CP) ADP+CP creatine +ATP Anaerobic glycolysis Areobic oxidation of glucose Oxidation of FA Oxygen debt Increase oxygen consumption after muscular work which is proportional to oxygen deficit.

Sources of ATP 1. ATP present in sarcoplasm- suffice for 1 -2 sec 2. Creatine phosphate- suffice for 5 -8 sec. Lohman’s reaction CP+ADP=Creatine+ATP 3. Glycolysis- suffice for 1 min 4. Oxidation of cellular foodstuff- for longer periods

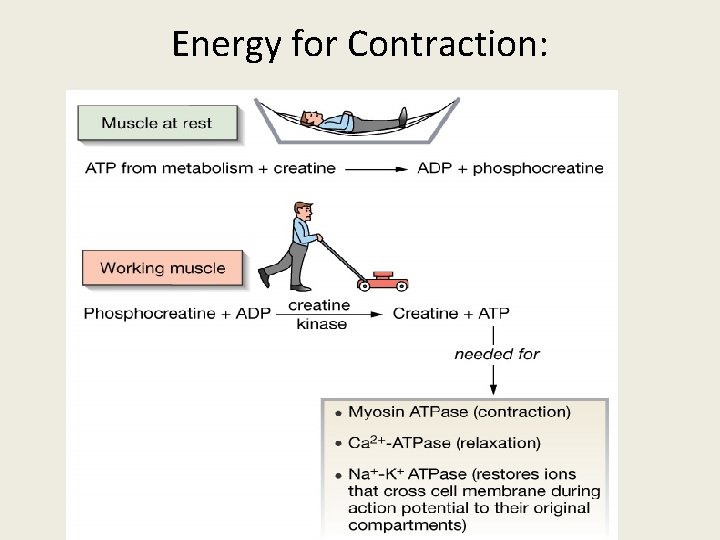
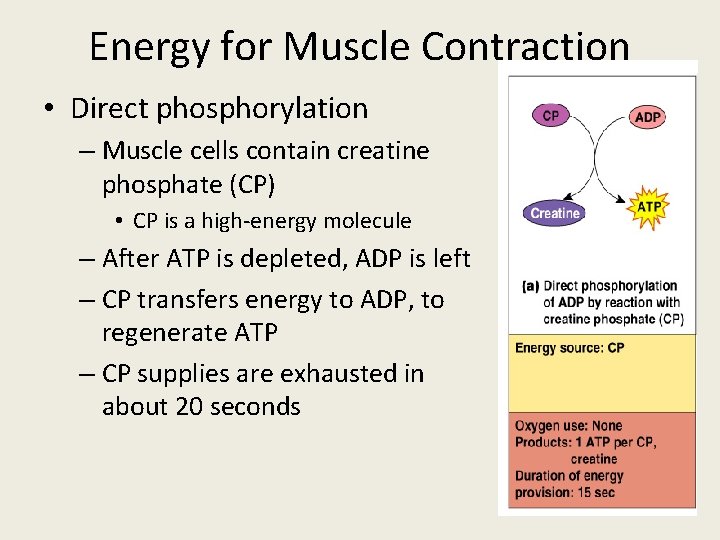
Energy for Contraction: Figure 12 -13: Phosphocreatine

Energy for Muscle Contraction • Direct phosphorylation – Muscle cells contain creatine phosphate (CP) • CP is a high-energy molecule – After ATP is depleted, ADP is left – CP transfers energy to ADP, to regenerate ATP – CP supplies are exhausted in about 20 seconds

Energy for Muscle Contraction • Aerobic Respiration – Series of metabolic pathways that occur in the mitochondria – Glucose is broken down to carbon dioxide and water, releasing energy – This is a slower reaction that requires continuous oxygen

Energy for Muscle Contraction • Anaerobic glycolysis (continued) – This reaction is not as efficient, but is fast • Huge amounts of glucose are needed • Lactic acid produces muscle fatigue

Muscle Fatigue and Oxygen Debt • When a muscle is fatigued, it is unable to contract • The common reason for muscle fatigue is oxygen debt – Oxygen must be “repaid” to tissue to remove oxygen debt – Oxygen is required to get rid of accumulated lactic acid • Increasing acidity (from lactic acid) and lack of ATP causes the muscle to contract less

• Thermal changes • Resting heat • Initial heat • Recovery heat Resting heat Heat produced at rest=BMR Initial heat 1. 2. 3. Heat of activation Heat of shortening Heat of relaxation

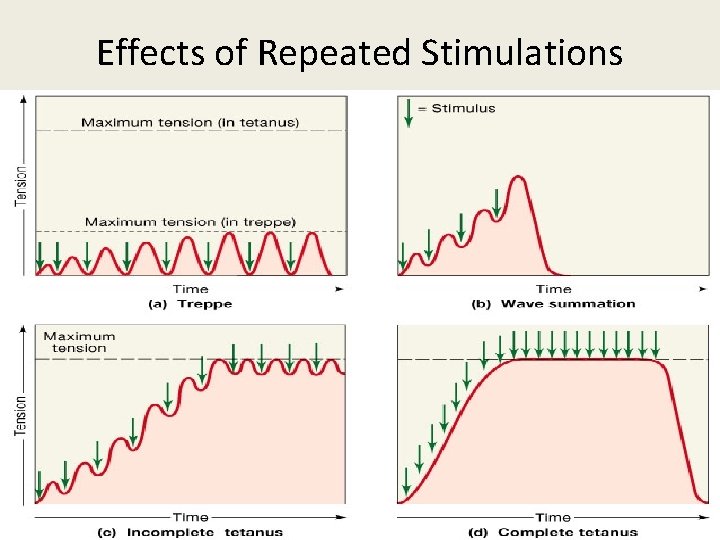
Other important properties of skeletal muscle 1. 2. 3. 4. 5. Summation of contraction Staircase phenomenon Tetanization Length tension relationship Load velocity relationship Repeated stimulus • Tetanus • Muscle is stimulated repeatedly at a very high frequency there is sustained contraction. • Incomplete clonus • Incomplete relaxation between contraction.

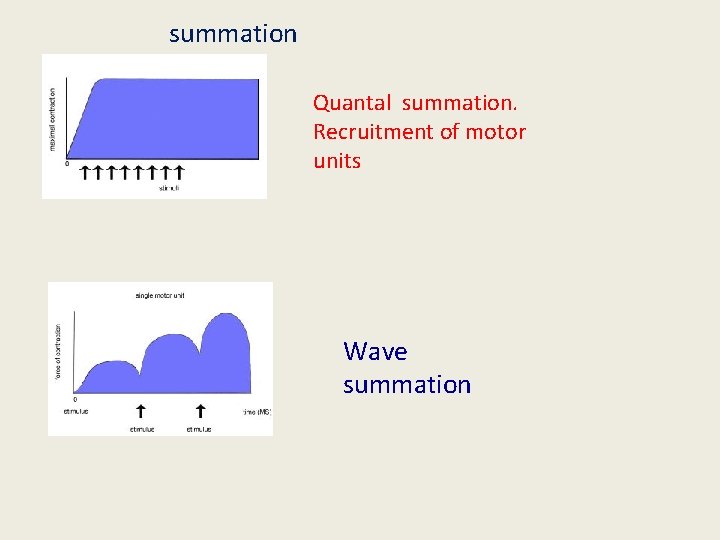
FACTORS AFFECTING CONTRACTION a) Effect of multiple stimuli: 1)effect of 2 successive stimuli: i) beneficial effect ii) superposition iii) summation 2) more than two stimuli: i) clonus ii) tetanus iii) treppe iv) fatigue

– - Increase in the temperature – Decrease in the viscosity – Availability of more Ca++ – Ca ++ from the first contraction is not completely pumped into the saroplasmic reticulum – Second stimulus releases Ca ++ and adds to the remaining Ca ++ from the first contraction

FATIGUE • Definition: it is a decrease in the performance due to continuous and prolonged activity • Nerve is indefatigable


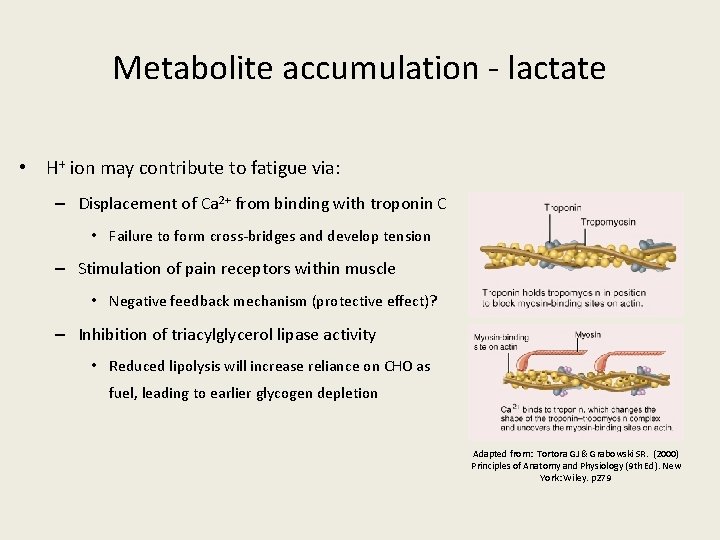
Metabolite accumulation - lactate • H+ ion may contribute to fatigue via: – Displacement of Ca 2+ from binding with troponin C • Failure to form cross-bridges and develop tension – Stimulation of pain receptors within muscle • Negative feedback mechanism (protective effect)? – Inhibition of triacylglycerol lipase activity • Reduced lipolysis will increase reliance on CHO as fuel, leading to earlier glycogen depletion Adapted from: Tortora GJ & Grabowski SR. (2000) Principles of Anatomy and Physiology (9 th Ed). New York: Wiley. p 279

• The presence of lactic acid is what leads to muscle fatigue (when contraction can not occur despite the presence of a continued neural stimulation) when doing short, intense bouts of work. • All causes of muscle fatigue include the depletion of all glycogen, amino acid, lipid reserves. – This occurs after hours of exertion.

Effect of load on muscle contraction 1. Free-load 2. After-load Effect of temperature on muscle contraction • 1. Heat rigor • 2. Calcium rigor • 3. Rigor mortis • •

Effects of Repeated Stimulations

summation Quantal summation. Recruitment of motor units Wave summation

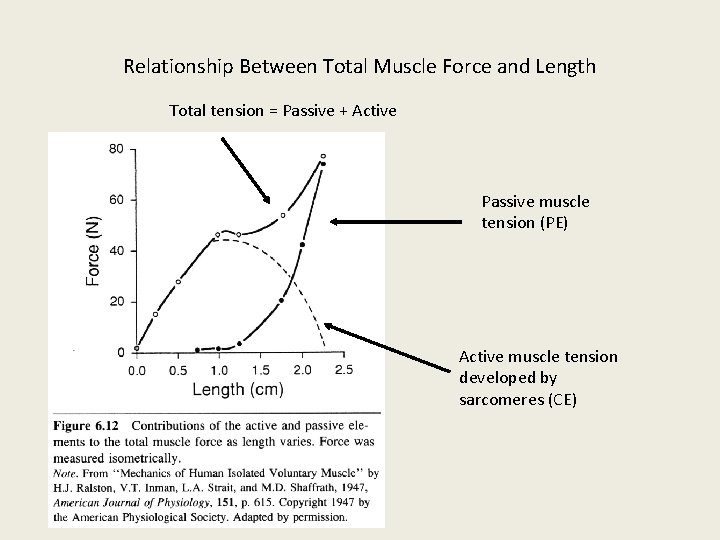
Relationship Between Total Muscle Force and Length Total tension = Passive + Active Passive muscle tension (PE) Active muscle tension developed by sarcomeres (CE)


• Passive tension When the muscle fiber is stretched the tension developed is called passive tension. • Total tension Stretched muscle when stimulated is called total tension. • Active tension Tension created by cross bridge movements is called active tension.

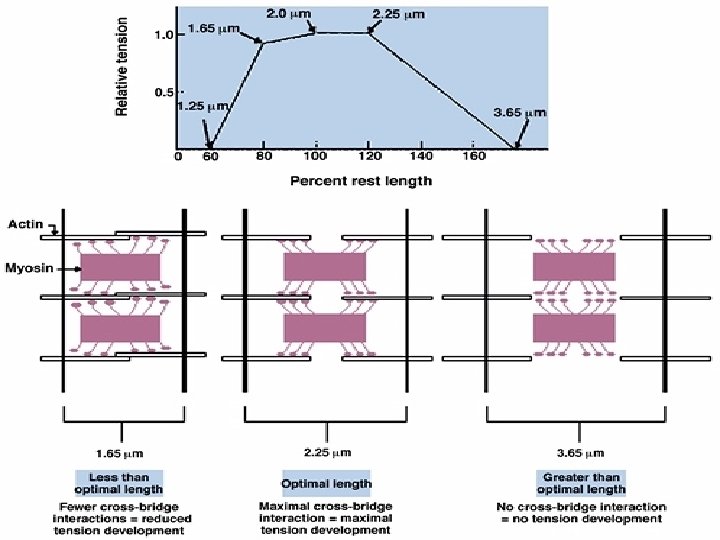
• Length tension relationship shows that within physiological limits the tension in the muscle increases as the length is gradually increased. • Initial length Length of the muscle prior to contraction • Resting length Maximal isometric tension developed is at optimum length.

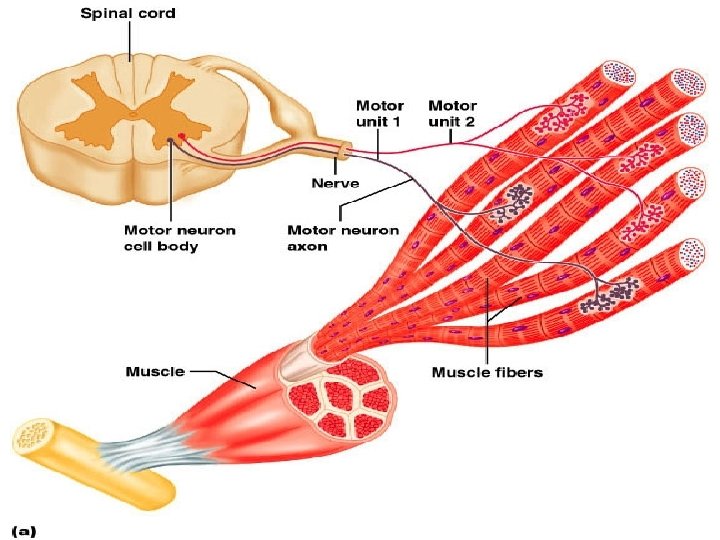
Motor Unit: The Nerve-Muscle Functional Unit • A motor unit is a motor neuron and all the muscle fibers it supplies • The number of muscle fibers per motor unit can vary from a few (4 -6) to hundreds (1200 -1500) • Muscles that control fine movements (fingers, eyes) have small motor units • Large weight-bearing muscles (thighs, hips) have large motor units


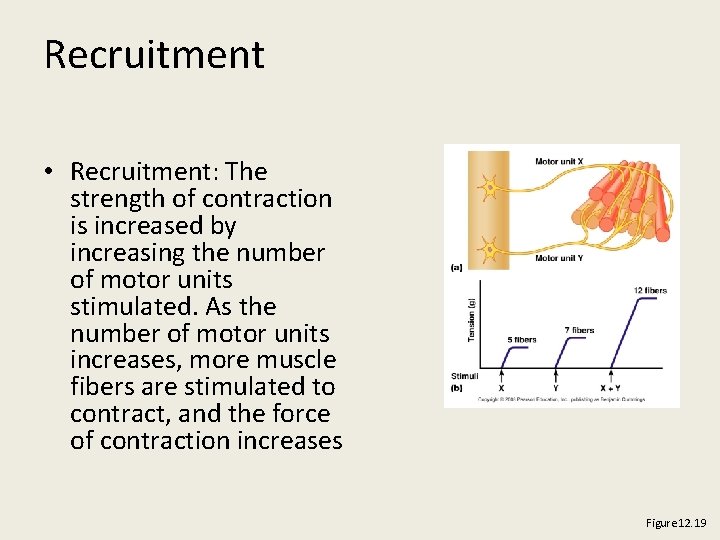
Recruitment • Recruitment: The strength of contraction is increased by increasing the number of motor units stimulated. As the number of motor units increases, more muscle fibers are stimulated to contract, and the force of contraction increases Figure 12. 19

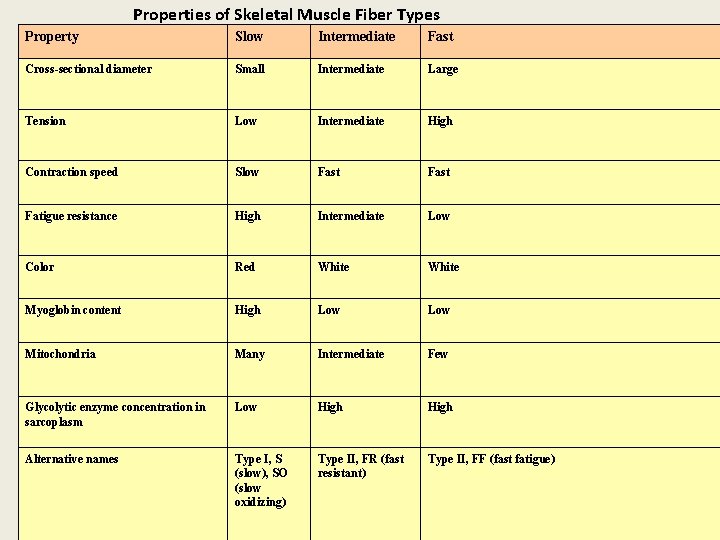
Muscle fibers vary in the body • Fast fibers (white, fast twitch, fast glycolytic) • Slow fibers (red, slow twitch, slow oxidative) • Intermediate fibers (fast twitch, fast oxidative)

Properties of Skeletal Muscle Fiber Types Property Slow Intermediate Fast Cross-sectional diameter Small Intermediate Large Tension Low Intermediate High Contraction speed Slow Fast Fatigue resistance High Intermediate Low Color Red White Myoglobin content High Low Mitochondria Many Intermediate Few Glycolytic enzyme concentration in sarcoplasm Low High Alternative names Type I, S (slow), SO (slow oxidizing) Type II, FR (fast resistant) Type II, FF (fast fatigue)
